Last Updated on November 25, 2025 by
Doctors often talk about whether ultrasound, CT urogram vs cystoscopy is better for finding bladder problems. We look at the good and bad of each, like how well they work and their accuracy. Studies show that these tools have different strengths, with research showing how they find bladder masses differently.

Cystoscopy is seen as the top choice, but ultrasound is a non-invasive option that works well in some cases. Knowing how each tool works helps us improve care and procedures at leading hospitals.
Getting the right diagnosis for bladder problems is key to good treatment. We use different methods to figure out what’s wrong. This helps us decide the best course of action.
Getting a precise diagnosis is the first step to a successful treatment. It’s very important because it affects how well the treatment works. For example, cystoscopy for hematuria lets doctors see inside the bladder to find problems.
If the diagnosis is wrong or late, the treatment might not work. This could even make things worse. So, using the right diagnostic tools is critical.
There are many ways to check on bladder health. These include cystoscopy, ultrasound, and CT urogram. Each has its own benefits and uses.
Cystoscopy uses a thin tube with a camera to look inside the bladder. It’s great for finding issues like bladder cancer. It’s often used when there’s blood in the urine.
Ultrasound is a non-invasive way to see the bladder using sound waves. It’s good for spotting problems without needing to go inside the body.
Choosing the right test depends on the patient’s condition and history. For example, cystoscopy for hematuria is a good choice when there’s blood in the urine. It lets doctors see the bladder closely.
Knowing about these tests helps doctors pick the best one for each patient. This ensures the best care possible.
Cystoscopy is a key tool in urology, giving a clear view of the bladder’s inside. A thin, flexible or rigid tube with a camera and light is inserted through the urethra into the bladder.
The cystoscope is linked to a monitor. This lets urologists check the bladder’s lining for issues like tumors, stones, or inflammation. The procedure can be done with local anesthesia or sedation, based on the patient’s comfort and the exam’s complexity.
During the procedure, the urologist can also take biopsies or remove small tumors or stones if found. This makes cystoscopy not just for diagnosis but also for treatment.
Cystoscopy is very good at finding bladder tumors, with a 97.9% sensitivity rate. Its high accuracy comes from the direct view it offers, spotting even small lesions.
A leading urologist says, “Cystoscopy is unmatched in accurately diagnosing bladder conditions. Its high sensitivity rate makes it a go-to for healthcare professionals.” –
A trusted diagnostic method, cystoscopy continues to be a cornerstone in urological care.
The cystoscopy table is made for comfort and stability during the procedure.
The table has stirrups and adjustable parts for easy access and comfort. The experience can differ based on the patient’s pain tolerance and the exam’s details.
Ultrasound technology has changed how we diagnose diseases. It’s a non-invasive way to check the bladder. We’ll look at how it works, its effectiveness, and its benefits.
Bladder ultrasonography uses sound waves to see the bladder. It’s non-invasive and painless, which is great for patients. A technician or doctor applies gel to the abdomen and uses a probe to get images.
Ultrasound can spot bladder tumors with a success rate of 71% to 89%. A study on PMC shows its promise as a first test. How well it works depends on the tumor’s size, location, and the operator’s skill.
Ultrasound is non-invasive, which lowers the risk of complications from invasive tests like cystoscopy. It means patients have less recovery time and less discomfort. This makes it a good choice for initial checks and for those at low risk of bladder problems.
When diagnosing bladder problems, two main methods are often used: CT urogram and cystoscopy. Each has its own benefits and drawbacks. It’s important for doctors to know these differences to choose the best option.
A CT urogram uses CT scans to see the urinary system, including the bladder. It’s great for finding bladder tumors, stones, and other issues. Here’s what it can do:
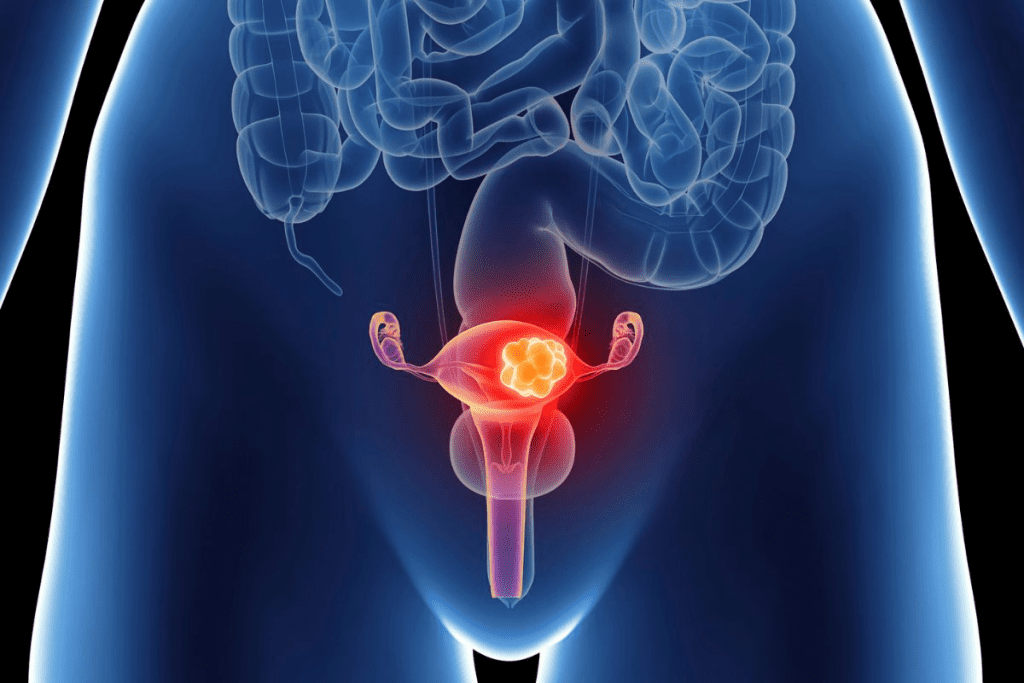
CT urogram involves ionizing radiation. While it’s often worth it, think about the radiation risk. This is more important for young patients or those needing many scans.
CT urogram and cystoscopy are good at different things. Cystoscopy is very good at finding bladder tumors, with a 97.9% success rate. CT urogram is better for the upper urinary tract and finding ureteral obstruction. The right choice depends on the situation and the patient.
Knowing how CT urogram and cystoscopy work helps doctors pick the best test for their patients.
Cystoscopy is key in checking for hematuria, which means blood in the urine. It helps find the cause of this symptom. Hematuria can be tiny or big, and it needs a detailed check to figure out why it’s happening.
To find out why there’s blood in the urine, doctors use several steps. Cystoscopy is very helpful because it lets doctors see inside the bladder and urethra. They can look for tumors, stones, or swelling.
When someone has blood in their urine, doctors first look at their medical history and do a physical check. They also do tests like urinalysis. If the blood keeps coming back or if there’s pain, more tests are needed.
Doctors sort patients with hematuria into risk groups. They look at age, smoking, chemical exposure, and other symptoms. High-risk patients often need more tests, like cystoscopy, because they might have serious problems like bladder cancer.
After finding blood in the urine, it’s important to keep an eye on the patient. This is true for those who had cystoscopy. They might need more cystoscopies, depending on their history and risk.
The timing of these follow-ups depends on the patient’s risk and what the first tests showed. Custom follow-up plans help make sure patients get the right care and catch any new problems early.
In some cases, ultrasound is a better choice than cystoscopy. It’s non-invasive and works well for certain issues. While cystoscopy is great for finding bladder problems, ultrasound has its own benefits.
Ultrasound is perfect for patients at low-to-moderate risk of bladder cancer. It’s easy and doesn’t carry the risks of cystoscopy. Ultrasound shows real-time images of the bladder, helping spot big issues without direct viewing.
It’s also more comfortable for patients. No instruments are needed, making it less scary and less uncomfortable. This makes it great for regular checks or follow-ups in low-risk patients.
For advanced cervical cancer, knowing if it’s spread to the bladder is key. Ultrasound is very helpful here, checking the bladder wall and nearby tissues. It shows how far the cancer has spread, which is important for doctors and surgeons.
Using ultrasound can also skip more invasive tests, lowering risks and improving results. It’s also good for tracking changes in the cancer, helping see how well treatments are working.
The choice between ultrasound and cystoscopy depends on the patient. Factors like medical history, current health, and personal feelings matter. For example, some patients might do better with ultrasound due to their body or past experiences.
Custom care is key in healthcare today. Tailoring treatments to each patient’s needs leads to better care and a better experience. This approach helps doctors make the best choices for each patient.
Using different diagnostic methods together can make bladder condition diagnoses more accurate. This way, doctors get a full picture of a patient’s health. This leads to better treatment plans.
Each diagnostic method has its own strengths and weaknesses. For example, cystoscopy is great for finding bladder tumors but is invasive. Ultrasound is non-invasive but might miss some conditions.
Sequential testing means doing one test and then another to confirm or rule out a diagnosis. This method is helpful when the first test isn’t clear or when more information is needed.
For instance, a patient with blood in their urine might start with an ultrasound. If the ultrasound shows something that needs a closer look, a cystoscopy might follow.
When it comes to healthcare, the cost of tests is important. More tests can give more information but also cost more.
It’s important to think about the cost and benefits of each test. Starting with cheaper tests like ultrasound can be smart. Then, save more expensive tests like cystoscopy or CT urogram for when they’re really needed.
Personalized diagnostic strategies mean tailoring the tests to each patient’s needs. This can make diagnoses more accurate and improve patient care.
For example, people at high risk for bladder cancer might get more tests early on. Those at lower risk might start with less invasive tests.
By mixing different diagnostic methods and tailoring them to each patient, we can get the best results. This approach not only improves accuracy but also leads to better treatment plans and care for patients.
Choosing between ultrasound and cystoscopy for bladder checks depends on several things. These include the patient’s health, risk level, and what the doctor needs to find out. We’ve looked at what each method does well and what it doesn’t.
Ultrasound is a non-invasive way to check the bladder. It’s good for finding tumors in patients at lower risk. But, cystoscopy is the top choice for getting a detailed look at the bladder. It lets doctors take tissue samples for further tests.
Deciding between ultrasound, cystoscopy, or both should be based on knowing their strengths and weaknesses. Healthcare providers need to think about each patient’s needs and the situation. This way, they can choose the best approach for accurate diagnosis and the best care for the patient.
Cystoscopy lets us see inside the bladder with a scope. A CT urogram uses imaging to look at the urinary tract. Both help us check the bladder and urinary system but in different ways.
Yes, cystoscopy is key for checking blood in the urine. It helps find the cause of bleeding, which is important for patients at risk for bladder cancer.
Cystoscopy is the best way to check the bladder because it’s very accurate. Ultrasound is a safer option for a first check or when cystoscopy isn’t needed.
Ultrasound is safer and doesn’t need a scope in the bladder. It’s good for screening and checking bladder issues in some cases.
The cystoscopy table helps make the exam comfortable. It’s adjusted to support the patient during the procedure.
Yes, using ultrasound and cystoscopy together can give the best results. We choose the best tests for each patient based on their needs.
Ultrasound can spot tumors 71% to 89% of the time. It’s not as good as cystoscopy but is useful in some cases.
CT urogram uses radiation, but cystoscopy doesn’t. We think about radiation risks when choosing tests, to protect patients from harm.
Stamatiou, K., et al. (2009). The accuracy of ultrasonography in the diagnosis of bladder tumors: A comparative study with cystoscopy. Journal of Urology. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2813642/
Subscribe to our e-newsletter to stay informed about the latest innovations in the world of health and exclusive offers!