Last Updated on November 27, 2025 by Bilal Hasdemir
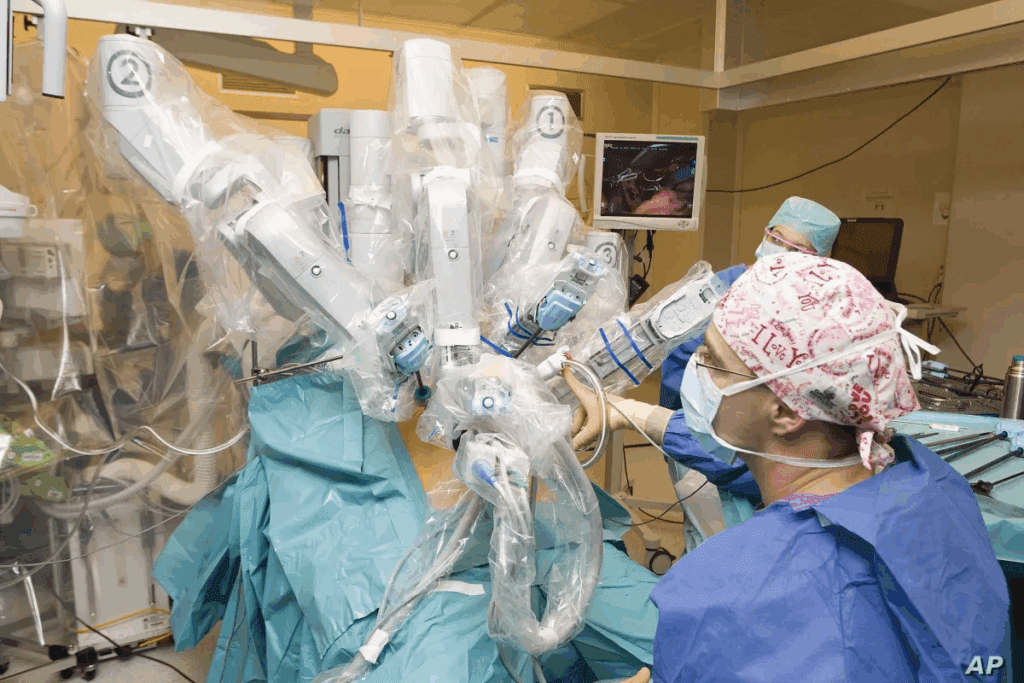
Nearly 500,000 women have hysterectomies every year in the U.S. Many choose robotic-assisted technology. It’s less invasive and cuts down on recovery time. Do you have robotic hysterectomy stitches internally? Learn about dissolvable sutures, healing process, and wound care.
Knowing about robotic hysterectomy and internal stitches is key for those thinking about it.
We’ll dive into the details of internal stitches in robotic hysterectomy. This will help clear up any confusion about this part of the procedure.
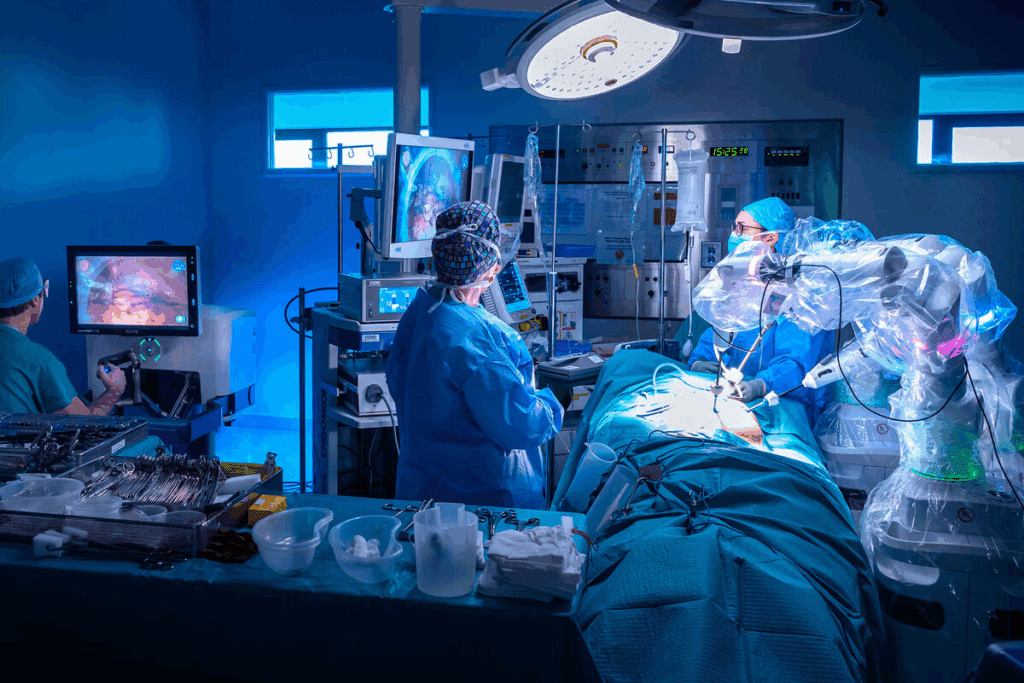
Robotic hysterectomy is changing gynecological surgery with its precision and less invasive method. It’s getting a lot of attention for possibly improving patient results and cutting down recovery times.
Let’s dive into what robotic hysterectomy is all about. We’ll look at its basics, how it works, and the different types of hysterectomies it can do.
A robotic hysterectomy is a surgery to remove the uterus using robotic technology. This minimally invasive surgery lets surgeons do complex operations with better precision and control than old methods.
The robotic system has a console for the surgeon, a cart with robotic arms, and a 3D vision system. This setup helps surgeons see clearly and make accurate movements.
Robotic-assisted technology turns the surgeon’s hand movements into precise robotic actions. The high-definition 3D vision gives a detailed view of the area, making dissection and suturing precise.
The robotic arms have instruments that can move 360 degrees. This flexibility is great for complex surgeries, letting surgeons easily move around delicate areas.
Robotic technology can be used for many types of hysterectomies, like total, subtotal, and radical hysterectomies. The choice depends on the patient’s situation, the surgery’s purpose, and the surgeon’s opinion.
Robotic hysterectomy helps with conditions like fibroids, endometriosis, and uterine prolapse. It offers benefits like less blood loss, lower infection risk, and shorter hospital stays compared to open surgery.

Hysterectomy procedures have changed a lot, moving from big open surgeries to small robotic surgeries. This change is a big step forward in women’s health. Technology has been key in making these surgeries better for patients.
In the past, hysterectomies were performed with large abdominal incisions.This method was good but had big downsides. It took longer to heal, hurt more, and had more risks.
New methods like laparoscopic and robotic surgeries are now common. They use small cuts, causing less damage and pain. This means patients heal faster and have fewer problems.
Robotic surgery has made gynecology better. It lets surgeons do complex tasks with more precision. This tech helps treat many gynecological issues.
Robotic surgery is better than laparoscopy in many ways. It gives surgeons more control and better views. This leads to better results and a smoother surgery.
Robotic hysterectomies have many benefits. They cause less bleeding, fewer problems, and shorter stays in the hospital. Data shows patients recover faster and have fewer complications than with open surgeries.
These improvements show how important new tech and methods are in gynecology. As we keep innovating, robotic surgery will likely be even more important for hysterectomies.
Robotic hysterectomy stitches are a key part of the surgery. Knowing what to expect can ease worries. The kind of stitches used affects recovery, scarring, and results. We’ll look at the different stitches used in robotic hysterectomy.
The sutures in robotic hysterectomy are made from materials safe for the body. Monofilament and multifilament sutures are often used. Each has its own benefits and characteristics.
| Suture Type | Characteristics | Uses |
| Monofilament | Single strand, smooth surface | Ideal for delicate tissues, reduces risk of infection |
| Multifilament | Braided strands, higher tensile strength | Suitable for tissues under tension, provides secure closure |
Robotic hysterectomy uses both internal and external stitches. Internal sutures close incisions inside the body. External sutures close the skin. The choice depends on the procedure and the surgeon’s preference.
Sutures in robotic hysterectomy can be dissolvable or removable. Dissolvable sutures dissolve over time and are absorbed by the body. Removable sutures are taken out once the wound heals.
Knowing about the stitches used in robotic hysterectomy helps prepare for surgery and recovery. It’s important to talk to your healthcare provider about any concerns or questions. This ensures the best results.
Learning about a robotic hysterectomy can ease worries and prepare you. This surgery is complex, with many steps from start to finish.
Before a robotic hysterectomy, patients prepare in several ways. This includes:
The robotic hysterectomy procedure has several key steps:
After removing the uterus, the surgeon focuses on closing the incisions. Robotic technology helps with precise suturing. This can lead to better healing and less scarring.
The suturing techniques depend on the patient’s needs and the surgeon’s judgment.
Some important aspects of closing techniques include:
Robotic surgery brings new levels of precision and control. It changes how surgeons do complex surgeries, like hysterectomies. This is thanks to the advanced robotic-assisted technology.
Robotic systems give surgeons better dexterity and vision. This means they can stitch more accurately. The robotic arms work the suturing tools with great precision, cutting down on mistakes.
Key benefits of precision stitching with robotic assistance include:
Barbed sutures are a big step forward in robotic surgery. They have tiny barbs that hold onto tissue, making knots less necessary. This reduces the chance of suture failure. New suture materials and techniques also make sutures last longer and work better.
“The introduction of barbed sutures has been a game-changer in robotic surgery, simplifying the suturing process and improving patient outcomes.”
Surgeons use a console to control the robotic system. They use hand controls and foot pedals. This lets them move the robotic arms with precision, making complex stitches easy.
The ability to control stitching remotely is a significant advantage of robotic surgery, as it allows surgeons to perform procedures with greater precision and less fatigue.
Robotic hysterectomy is a big step forward in minimally invasive surgery. It uses advanced technology for precise stitching inside the body. This is key for the surgery’s success.
One big plus of robotic surgery is how it looks. It uses internal stitches, so there’s no need for visible ones. This is great for those worried about how they’ll look after surgery.
Internal stitching in robotic hysterectomy also lowers infection risk. It keeps internal tissues away from the outside, cutting down on bacteria. This makes the surgery safer for the patient.
The stitching in robotic surgery helps healing happen faster. It makes sure tissues are stitched together right, which helps them heal better. This can mean patients get back to normal sooner.
People who have robotic hysterectomy with internal stitches often feel less pain after. The surgery is done in a way that hurts less, thanks to the precise stitching. This leads to less discomfort for patients.
In summary, internal stitches in robotic hysterectomy offer many benefits. These include better looks, less chance of infection, faster healing, and less pain after surgery. As robotic surgery keeps getting better, helping patients more is the main goal.
Robotic hysterectomy is a modern and less invasive surgery. Yet, it’s important to know about possible stitch complications. Even with advanced technology, stitches can pose risks.
Stitches from robotic hysterectomy can lead to several issues. We’ll cover these to help you understand what might happen.
Occasionally, the body may react to stitches, causing inflammation or other problems. Though rare, it’s possible for the body to reject the stitches.
Common reactions include:
Infections can happen with any surgery, including robotic hysterectomy. Good wound care and follow-up are key to avoiding this risk.
Signs of infection may include:
Dehiscence is when the surgical wound opens up. This can be due to infection, stress, or suture failure.
| Complication | Description | Typical Management |
| Suture Reaction | Adverse reaction to suture material | Monitoring, possible removal of suture |
| Infection | Bacterial infection of the wound | Antibiotics, wound care |
| Dehiscence | Reopening of the surgical wound | Wound closure, possibly under general anesthesia |
Knowing when to seek medical help is vital. If you notice severe pain, heavy bleeding, signs of infection, or wound dehiscence, call your doctor right away.
Being aware of these complications and watching your recovery closely can greatly improve your healing and outcome.
Robotic surgery for women’s health, like a hysterectomy, has changed recovery. It’s less invasive and can heal faster. Knowing the recovery timeline helps manage expectations and ensures a smooth healing journey.
Right after a robotic hysterectomy, patients usually stay in the hospital or recovery area for a few hours to overnight. Medical staff watch them closely for any immediate problems and help manage pain. Patients go home when they’re stable and can take care of themselves.
In the first week, patients might feel some discomfort, tiredness, and possibly vaginal bleeding or discharge. It’s important to follow the surgeon’s advice on rest, activity, and wound care. Patients can start with short walks and light stretching but should avoid heavy lifting, bending, or strenuous activities.
The long-term healing after a robotic hysterectomy can take several weeks to a few months. Most women can get back to normal activities in 4-6 weeks. But, full recovery, including strength and internal tissue healing, may take longer. It’s key to keep up with follow-up appointments with the healthcare provider to track the healing.
Getting back to normal activities should be slow. Patients are often told to avoid heavy lifting, strenuous exercise, and sexual activity for 6-8 weeks. It’s important to listen to your body and not rush the recovery. As you get stronger and more comfortable, you can slowly start doing your usual things, like work and exercise, with your healthcare provider’s guidance.
By understanding the recovery timeline and following the recommended guidelines, patients can improve their healing process and reduce the risk of complications after a robotic hysterectomy procedure.
Proper care for your incision sites after a robotic hysterectomy is key for a smooth recovery. This period can be tough, but following the right practices helps your body heal right. It also lowers the risk of complications.
Keeping your incision sites clean is vital. We suggest gently washing them with mild soap and water. Stay away from harsh or scented soaps, as they can irritate the skin and increase the risk of infection.
Key steps in wound care:
You can usually shower 24 to 48 hours after surgery, but check with your healthcare provider first. When showering, let water gently run over the incisions. Avoid scrubbing or soaking the area.
Tips for bathing:
It’s normal for incision sites to be slightly red, swollen, or tender at first. But, watch out for signs of complications like increased redness, swelling, or discharge.
Watch for these signs of possible complications:
To protect your stitches and ensure healing, follow activity restrictions. Avoid heavy lifting, bending, or strenuous activities as advised by your healthcare provider.
Recommended activities during recovery:
Looking at the stitches used in different hysterectomy methods shows why robotic hysterectomy stands out.
Traditional open hysterectomy needs a big cut. It uses thick sutures, which can be inside or outside the body. The outside stitches come out after a week or two. The inside ones might stay or dissolve.
Laparoscopic hysterectomy uses small cuts and special tools. It uses thinner, dissolvable stitches. This lowers the chance of problems and helps healing.
Robotic hysterectomy is precise thanks to the robot’s help. It uses thin, precise stitches. This leads to better healing and fewer issues. The robot’s tools allow for detailed work, causing less damage to tissues.
Key Advantages of Robotic Hysterectomy Suturing:
Vaginal hysterectomy takes out the uterus through the vagina. It uses internal stitches that dissolve. This method avoids big cuts, which can make recovery faster and leave less scar.
Let’s look at a table to see how different methods use stitches:
| Surgical Method | Suture Type | Suture Characteristics |
| Traditional Open Hysterectomy | Thicker, external or internal | May be dissolvable or non-dissolvable |
| Laparoscopic Hysterectomy | Finer, often dissolvable | Less risk of complications |
| Robotic Hysterectomy | Fine, precise, dissolvable | Enhanced precision, less tissue trauma |
| Vaginal Hysterectomy | Dissolvable, internal | No external scarring |
Robotic surgery has made hysterectomy stitches more comfortable for women. It has changed surgery for the better, with less pain and quicker healing. This new method means less scarring and faster recovery times.
Women feel different levels of pain after robotic hysterectomy. Some might feel only a little discomfort, while others might feel more pain. It really depends on the person’s health, the surgery’s complexity, and how they handle pain.
Common feelings include:
Healing times after robotic hysterectomy vary. Women usually see improvement over weeks. Knowing what to expect can help manage stress and anxiety.
| Timeframe | Typical Healing Progress |
| 1-2 weeks | Initial recovery; most patients experience significant improvement in pain levels. |
| 2-6 weeks | Gradual return to normal activities; stitches typically dissolve or are absorbed. |
| 6-12 weeks | Full recovery for most patients; significant reduction in discomfort. |
Managing pain well is key to a smooth recovery. Doctors often give a mix of medicines to help with pain. Some women also find relief with relaxation techniques or physical therapy.
Key pain management strategies include:
Most women are very happy with the results of robotic hysterectomy. The surgery is less invasive, leading to fewer problems and a quicker return to life as usual.
Factors influencing long-term satisfaction include:
When you’re getting ready for a robotic hysterectomy, talking about stitches with your surgeon is key. This chat helps you grasp the stitching methods used and what healing will be like.
Before your surgery, ask your surgeon about the stitches they’ll use. You might want to know the material, if they dissolve, and how they’ll affect healing. Also, asking about the stitching method can give you insight into the advanced surgical techniques your surgeon uses.
Some important questions to ask include:
Every case is different, and knowing the details of your robotic hysterectomy can prepare you better. Your surgeon can explain the stitching method, the number of cuts, and how stitches will be handled after surgery. As one surgeon said, “The key to a successful robotic hysterectomy lies in the precision of the suturing technique.”
You can also talk to your surgeon about your stitch preferences. Some might prefer dissolvable stitches to avoid removal. Your surgeon will choose the best method based on your case and health history.
For example, you might ask, “Can we use dissolvable stitches for my procedure?” or “Is there a suturing method that will reduce scarring?” Talking about these options can make the procedure fit your needs better.
After surgery, following your surgeon’s wound care and follow-up advice is vital. Proper care of your incisions can greatly affect healing. Make sure you understand how to manage your stitches and what to watch for that might mean a problem.
Talking about stitches with your surgeon can help you understand your robotic hysterectomy better. It can also make your recovery smoother.
Robotic surgery in gynecology has brought new suturing techniques. Technology keeps getting better, leading to more precise and safe surgeries. This is true for procedures like robotic hysterectomy.
New robotic systems are changing surgery for the better. They have better vision, more flexible arms, and designs that help surgeons. For example, the newest robots have 3D high-definition vision. This helps surgeons see better and make more accurate cuts.
AI is making suturing in surgery smarter. It helps decide the best way to sew, reducing surgeon stress. This technology is new but could change surgery a lot in the future.
Single-site surgery is another big step forward. It means doing the whole surgery through one small cut. This can mean less pain, less scarring, and quicker healing. The robots used for this surgery help with better views and control.
We’re expecting even more from AI, robotics, and surgery soon. Future tools might analyze tissues live, adjust stitches automatically, and give better feedback. These changes will make surgery safer and faster, helping patients recover quicker.
Robotic hysterectomy stitches are key to a successful procedure. They reduce infection risk and speed up healing. The technology’s precision means better suturing, leading to better patient outcomes.
Robotic surgery offers smaller cuts and less pain after surgery. This makes it a great choice for women needing a hysterectomy. As technology improves, we’ll see even better stitching methods, helping patients recover faster and more comfortably.
Knowing about stitches in robotic hysterectomy helps patients prepare better. This leads to higher satisfaction and better results. As robotic surgery gets better, precise stitching will keep being a vital part of successful procedures.
Robotic hysterectomy uses dissolvable sutures for stitching inside the body. This means no need to remove stitches later. These sutures dissolve over time and are absorbed by the body.
Most stitches in robotic hysterectomy are internal. The robotic technology allows for precise stitching inside the body. This reduces the need for stitches on the outside.
The time for stitches to dissolve varies by suture type. Usually, dissolvable sutures start to dissolve in a few weeks. They are fully absorbed in 6-8 weeks.
You might not see the stitches because they are mostly internal. But, there could be a few small stitches on the outside. These are usually not very noticeable.
Yes, you can talk to your surgeon about your preferences. While surgeons usually choose based on medical judgment, they might consider your wishes. This depends on the discussion and implications.
Like any surgery, stitches can have risks. These include reactions, infection, and dehiscence. But, the advanced techniques in robotic hysterectomy lower these risks.
Keep your incision sites clean and dry. Follow your healthcare team’s showering and bathing guidelines. Watch for signs of healing or complications.
Recovery time varies. Most people can start normal activities in 4-6 weeks. Always follow your surgeon’s specific instructions.
Robotic hysterectomy has many benefits. It offers precise stitching, smaller incisions, and fewer complications. This is compared to traditional or laparoscopic methods.
Robotic surgery is getting better. There’s AI-assisted suturing, single-site surgery, and more. These advancements improve minimally invasive gynecological surgery.
PMC Article: Vaginal Cuff Closure in Minimally Invasive Hysterectomy (2017)
Subscribe to our e-newsletter to stay informed about the latest innovations in the world of health and exclusive offers!