Last Updated on November 4, 2025 by mcelik
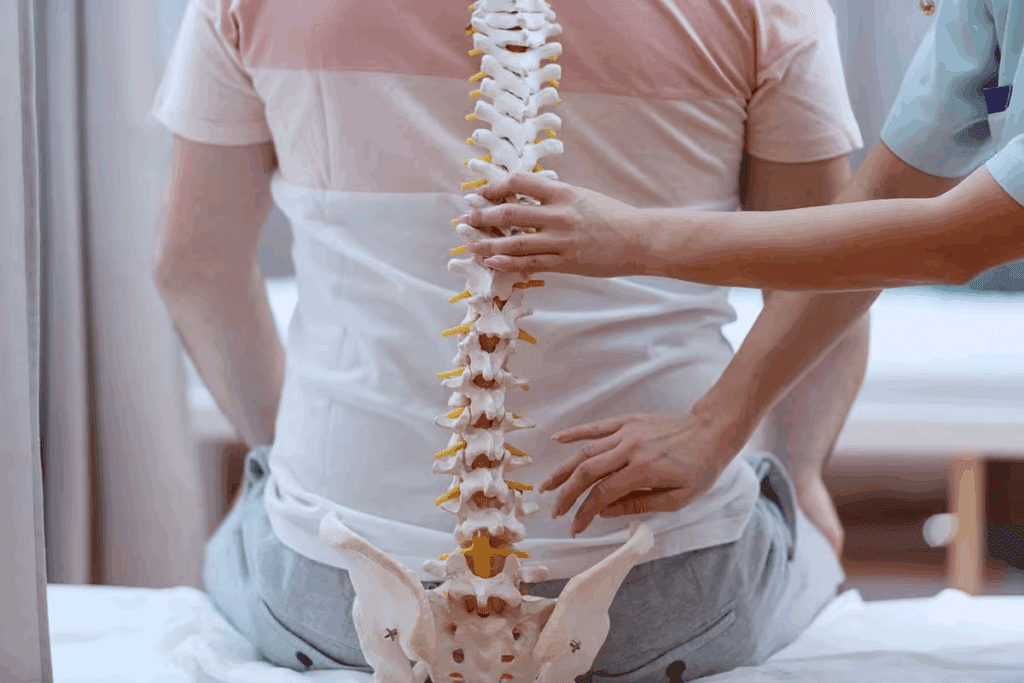
Spinal stenosis affects millions of people worldwide, causing significant discomfort and impacting daily life. Learn how to identify when spinal stenosis worse and when to consult a spine specialist.
Spinal stenosis is a condition where the spinal canal narrows. This puts pressure on nerves, causing pain, numbness, and weakness. It’s important to recognize symptoms and know when they worsen for effective management.
Spinal stenosis happens when the spinal canal gets narrower. This can put pressure on nerves and cause symptoms. It’s important to know how age affects the spine.
The spine has vertebrae, discs, and nerves. The spinal canal is where the spinal cord and nerves go. When this canal narrows, it can press on nerves.
Spinal stenosis can happen anywhere in the spine. But it’s most common in the lumbar and cervical areas. Knowing the anatomy helps us understand how stenosis affects the spine and what symptoms it causes.
Spinal stenosis often comes from aging. With aging, the degeneration of discs may lead to bulging, and ligaments can thicken, contributing to spinal canal narrowing. This narrows the spinal canal. Other causes include:
Some people are more likely to get spinal stenosis. These include:
Knowing who’s at risk and why can help catch spinal stenosis early. This makes it easier to manage the condition.
It’s important to know about the different types of spinal stenosis. This helps doctors diagnose and treat it better. Each type affects a different part of the spine, leading to different symptoms.
Cervical spinal stenosis happens in the neck. It can press on the spinal cord. This might cause numbness, weakness, or tingling in the arms or legs.
Cervical stenosis can also make it hard to balance and walk.
Lumbar spinal stenosis affects the lower back. It’s the most common type. It can cause pain, numbness, or cramping in the legs, mainly when standing or walking.
Lumbar stenosiscan really affect how well you can move and live your life.
Thoracic spinal stenosis is in the mid-back. It’s less common than cervical or lumbar stenosis. But, it can cause a lot of pain and nerve problems because of the spinal cord compression.
Spinal stenosis can be divided into central canal stenosis and foraminal stenosis. Central canal stenosis narrows the central canal of the spine, where the spinal cord or cauda equina is. Foraminal stenosis narrows the foramina, where nerve roots exit the spinal canal.
Both types can cause nerve compression and symptoms.
In summary, spinal stenosis varies by location and the specific spine area affected. Knowing the exact type is key for proper treatment and management.
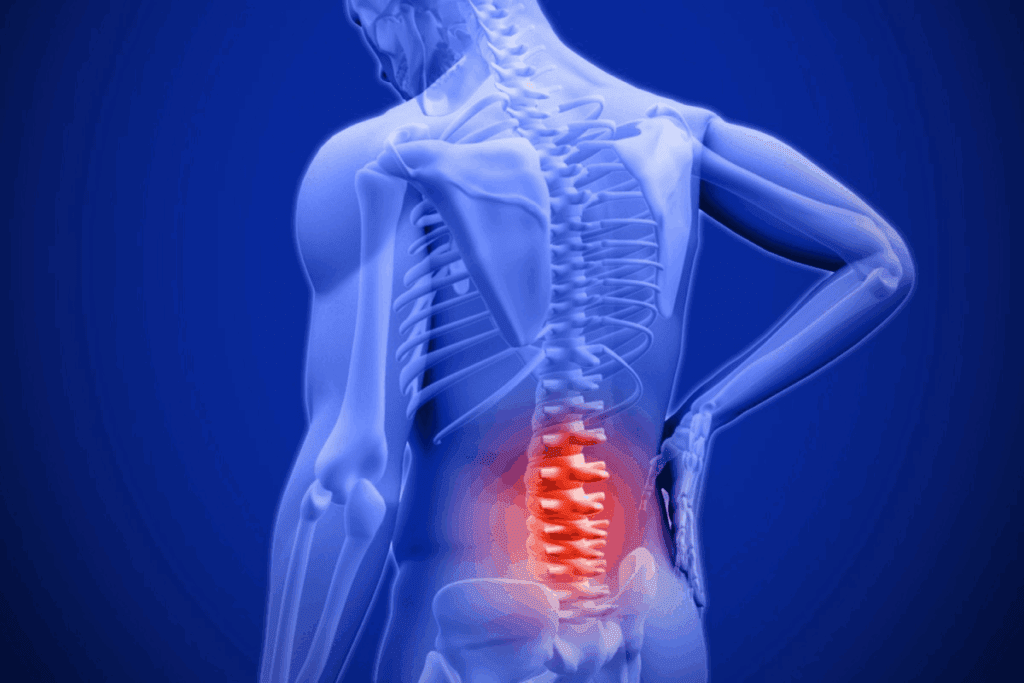
Spinal stenosis develops over time due to age, genetics, and lifestyle. Knowing how it progresses is key to managing it well.
Spinal stenosis gets worse slowly, with the spinal canal narrowing over months or years. This can put more pressure on the spinal cord and nerves, causing symptoms.
It starts with small changes, like a slight narrowing of the spinal canal. Over time, it can become more severe, leading to a lot of pain and trouble moving.
Several things can affect how spinal stenosis gets worse, including:
Knowing these factors can help people take steps to manage their condition better.
How fast spinal stenosis develops can vary a lot. Some people see symptoms get worse quickly, while others notice it more slowly.
Things like how bad the narrowing is, other health issues, and how well you manage your condition can affect how fast it gets worse.
Keeping an eye on your symptoms and working with your doctor can help you understand your own progression. This way, you can make a good plan to manage it.
Knowing when spinal stenosis is getting worse is key. It’s about understanding its symptoms and how they change. Spinal stenosis narrows the spine, causing symptoms that can get worse over time. Spotting these changes is vital for getting the right treatment.
It’s important to know the difference between baseline and progressive symptoms. Baseline symptoms are the first signs, like mild pain or numbness. Progressive symptoms, like more pain or weakness, mean the condition is getting worse.
Baseline symptoms are usually manageable over time. But progressive symptoms need medical attention. For example, if your pain gets worse or you feel new tingling, your stenosis might be getting worse.
There are warning signs that your spinal stenosis might be getting worse. These include:
Knowing these signs can help you get medical help early. This might stop the condition from getting worse.
Tracking your symptoms is important for keeping an eye on spinal stenosis. You can:
Tracking your symptoms helps your doctor make better decisions about your care. It’s a way to stay on top of your condition.
“The key to managing spinal stenosis is early detection of its progression and timely intervention.”
One key sign of worsening spinal stenosis is a change in pain. As it gets worse, the pain can become more intense and hard to handle.
A big sign is more intense pain. This pain can be sharp and severe, making daily tasks hard. Also, pain episodes might increase, happening more often or during certain activities.
For example, people with lumbar stenosis might feel pain more when walking or standing. Resting or bending forward might help. It’s important to watch these changes to understand how the condition is getting worse.
Another sign is new pain locations or changes in how pain spreads. As stenosis gets worse, pain can spread to new areas. For instance, pain might start in the lower back and go to the legs, or start in the neck and go to the arms.
This spread of pain is key to track. It shows which nerves are being compressed and how severe the stenosis is.
Changes in how pain reacts to activities or rest can also signal worsening stenosis. Activities that were once okay might now make the pain worse. Or, rest might not help as much as it used to.
For example, someone with cervical stenosis might find neck pain gets worse with looking up or overhead activities. Those with lumbar stenosis might feel more pain when bending or twisting.
Understanding these changes in pain patterns is key to managing spinal stenosis well. It helps figure out the best treatment.
It’s important to know the signs that spinal stenosis might be getting worse. As it progresses, people may find it harder to move and do everyday tasks.
One big sign is when you can’t walk as far as you used to. You might feel pain or discomfort sooner. This change can really affect your daily life.
Difficulty with daily activities is another warning sign. Even simple tasks like bathing or cooking can become hard. Spotting these problems early can help manage the condition better.
Problems with balance and coordination are also signs of worsening spinal stenosis. Compression of the spinal cord or nerves can cause these issues. It’s key to address them quickly to avoid more harm.
In summary, keeping an eye on changes in mobility and function is critical. Spotting these signs early can help get the right treatment for spinal stenosis.
Neurological symptoms are a big worry for people with worsening spinal stenosis. They affect how we feel and move. As stenosis gets worse, nerves get compressed or irritated, causing many problems.
One common symptom is more numbness or tingling. These feelings can happen in hands, feet, arms, or legs. Numbness and tingling often show up first, warning that nerves are being squeezed harder.
As stenosis gets worse, muscle weakness becomes a problem. This weakness can make it hard to move around and do everyday tasks. For example, weakness in the legs from lumbar stenosis can make walking or standing hard.
Changes in reflexes are another sign of worsening stenosis. These changes can mean nerves are damaged or compressed. Doctors check reflexes to see how much nerve damage there is.
| Neurological Symptom | Description | Possible Impact |
| Numbness or Tingling | Sensory disturbances in extremities | Discomfort, reduced sensitivity |
| Muscle Weakness | Decreased muscle strength | Reduced mobility, difficulty with daily activities |
| Reflex Changes | Altered reflex responses | Indicator of nerve damage or compression |
It’s important to know about these symptoms to manage worsening spinal stenosis. Recognizing these signs early helps patients get the help they need. This can improve their quality of life.
Knowing when spinal stenosis is a medical emergency can save lives. Spinal stenosis usually gets worse over time. But, it can turn into a serious emergency in some cases.
Cauda Equina Syndrome (CES) is a critical emergency linked to spinal stenosis. It happens when nerves in the lower back get compressed. This can cause permanent damage if not treated fast.
Symptoms include:
Seeing a doctor right away is key if you have these symptoms. Waiting too long can lead to permanent nerve damage.
Other severe nerve problems can also mean a medical emergency. These include:
These signs show spinal stenosis is badly affecting the nerves. You need to get checked out right away.
If you’re showing signs of Cauda Equina Syndrome or severe nerve problems, go to the emergency room fast. Don’t wait to see if symptoms get better. Go to the emergency room or call for help.
Acting quickly in a spinal stenosis emergency can make a big difference. Knowing the signs and acting fast can prevent long-term harm.
Diagnostic tests are key in tracking spinal stenosis. They help doctors see how severe the condition is. This information guides treatment choices.
Imaging tests are vital for spotting spinal stenosis. The main ones used are:
“MRI is the best for looking at spinal stenosis because it shows soft tissues well.”
| Imaging Modality | Strengths | Limitations |
| MRI | Excellent soft tissue visualization, high sensitivity for nerve compression | Claustrophobia, pacemaker incompatibility, higher cost |
| CT Scan | Excellent bone detail, quick procedure | Radiation exposure, less sensitive for soft tissue |
| X-rays | Quick, low cost, useful for initial assessment | Limited detail, radiation exposure |
EMG and NCS are vital for checking nerve function in spinal stenosis.
A detailed physical check is key for spinal stenosis tracking. Doctors look at:
Changes in these findings over time show the condition’s progress.
Spinal stenosis gets worse and needs a mix of treatments. This includes non-surgical steps, procedures, and surgery. Each step is chosen based on the patient’s needs.
First, doctors try non-surgical ways to treat spinal stenosis. Physical therapy is key. It helps strengthen muscles, improve flexibility, and correct posture.
Pain management is also important. Doctors use medicines like NSAIDs and muscle relaxants. They also suggest losing weight and quitting smoking to slow the disease.
If non-surgical methods don’t work, doctors try pain procedures. Epidural steroid injections are often used. They put steroids near the spinal cord to reduce pain and swelling.
Nerve blocks are another option. They inject medicine around nerves to stop pain signals. These methods can greatly reduce pain and improve function.
If other treatments don’t help, surgery might be needed. Surgery aims to remove what’s pressing on the nerves or spinal cord.
Laminectomy is a common surgery. It removes part of the bony plate to make more room for nerves. This can greatly reduce symptoms.
Other surgeries include spinal fusion and laminoplasty. The right surgery depends on how bad the stenosis is and the patient’s health.
Making lifestyle changes can help manage spinal stenosis. These changes can slow down the condition’s progress. By adjusting daily habits, people can improve their life quality.
Exercise and physical therapy are key for spinal stenosis management. Gentle exercises like stretching and strengthening keep flexibility and reduce pain. Physical therapy offers tailored exercises to boost mobility and strength.
Some good exercises include:
Good posture and body mechanics are vital for spine health. It’s important to be mindful of posture during daily tasks like sitting, standing, and lifting.
Improving posture and body mechanics can be done by:
Weight management is also critical for spinal stenosis. Extra weight can strain the spine, making the condition worse. A balanced diet and regular exercise help maintain a healthy weight.
Effective weight management strategies include:
Managing spinal stenosis needs a strong team effort with your healthcare providers. It’s all about working together with your medical team to manage your condition well.
Creating a team of healthcare experts is key for full care. Your team might include your primary doctor, an orthopedic specialist, a neurologist, a physical therapist, and a pain management specialist. Each one is important for different parts of your care.
Think about these points when building your team:
Talking about symptom changes with your doctors is critical. Keeping a symptom journal is very helpful. It helps track symptoms, their intensity, and what makes them better or worse.
When you talk about symptoms, be ready to share:
Having questions for your doctor can improve your care. Ask about treatment benefits and risks, symptom progression chances, and lifestyle changes that might help.
Some good questions to ask include:
By working closely with your healthcare team and keeping communication open, you’ll get the best care for your spinal stenosis.
Dealing with worsening spinal stenosis means you need to manage symptoms and stay independent. You’ll have to change your lifestyle, home, and health care plans as the condition gets worse.
Adjusting your home is key when spinal stenosis gets worse. You might put in grab bars and non-slip mats in the bathroom. Also, make sure things you use a lot are easy to get to.
Changing your home might mean moving furniture to make paths clearer. You might also need to install a stairlift or make your bathroom more accessible with a walk-in shower.
Managing pain is vital when spinal stenosis worsens. You might use medication, physical therapy, or try acupuncture or chiropractic care. It’s important to work with your doctor to find the right plan for you.
Doing gentle exercises and stretching can help keep you flexible and reduce pain. Mindfulness and deep breathing can also help manage chronic pain.
Spinal stenosis can affect your mental health. You might feel depression or anxiety as your condition worsens. It’s important to talk to mental health professionals for support.
Staying connected with friends and family can also help. Joining support groups online or in-person can be very helpful.
Connecting with others who face similar challenges is very helpful. Support groups let you share advice and find emotional support. Online forums and local groups offer a sense of community.
There are also many resources to help you deal with spinal stenosis. These include educational materials, advocacy groups, and healthcare services designed for people with spinal stenosis.
Living with progressive spinal stenosis is a big challenge. It affects your daily life in many ways. Understanding the condition is key to managing symptoms and keeping a good quality of life.
Spinal stenosis can progress differently for everyone. Some people may see symptoms get worse slowly, while others might experience a faster decline. Generally, it gets worse slowly, with some periods being better than others.
Key factors influencing the long-term outlook include:
Keeping a good quality of life is very important for those with progressive spinal stenosis. This involves medical care, lifestyle changes, and sometimes, using special equipment for daily tasks.
| Strategy | Description | Benefit |
| Physical Therapy | Tailored exercises to improve mobility and strength | Enhanced functional ability |
| Pain Management | Medications and interventions to control pain | Reduced discomfort and improved daily functioning |
| Lifestyle Modifications | Changes in daily habits to reduce strain on the spine | Slowed progression of stenosis |
Research on spinal stenosis is ongoing. It aims to find better treatments and improve patient outcomes. New treatments include less invasive surgeries and new medicines.
As research improves, people with progressive spinal stenosis have hope for better treatments in the future. Staying updated on new research and working with healthcare providers is important for a positive outlook.
Understanding spinal stenosis is key to managing it well. This article covered its types, symptoms, and treatment options. It’s all about knowing how to handle it.
Recognizing worsening symptoms is vital. This includes pain, mobility problems, and nerve issues. We talked about how to diagnose and treat these problems.
Knowing your condition helps you manage it better. You can make lifestyle changes and work with doctors. This way, you can stay informed and proactive.
In short, managing spinal stenosis needs a full plan. Stay informed and work with your healthcare team. This way, you can slow the disease and keep living well.
Spinal stenosis is a condition where the spinal canal narrows. This can put pressure on the spinal cord and nerves. It leads to pain, numbness, and weakness.
Spinal stenosis can be caused by several factors. These include degenerative changes like osteoarthritis and disc degeneration. Ligament thickening and congenital conditions also play a role. Trauma and infections can also cause it.
Older adults, those with a family history, and people with osteoarthritis are at higher risk. These groups are more likely to develop spinal stenosis.
Symptoms include pain, numbness, tingling, and weakness in the back, legs, or arms. Difficulty walking or standing is also common.
Doctors diagnose spinal stenosis through a medical history, physical exam, and imaging studies. MRI, CT, or X-rays are often used.
Treatment options include physical therapy and pain management. Interventions like decompression or fusion surgery are also available.
There’s no cure for spinal stenosis. But, treatments can manage symptoms and slow disease progression.
Lifestyle changes can help. Regular exercise, maintaining a healthy weight, and good posture are key.
Seek emergency care for sudden or severe symptoms. This includes cauda equina syndrome, severe pain, or bladder and bowel control issues.
Yes, exercise is beneficial. Stretching and strengthening can manage symptoms. Always consult a healthcare provider for a safe plan.
Pain management includes medication, physical therapy, and alternative therapies. Acupuncture or chiropractic care can also help.
The outlook varies based on the condition’s severity and treatment success. With proper management, many can maintain a good quality of life.
Medical News Today. (2024). Spinal stenosis symptoms, progression, and treatments. https://www.medicalnewstoday.com/articles/spinal-stensosis-symptoms
Subscribe to our e-newsletter to stay informed about the latest innovations in the world of health and exclusive offers!