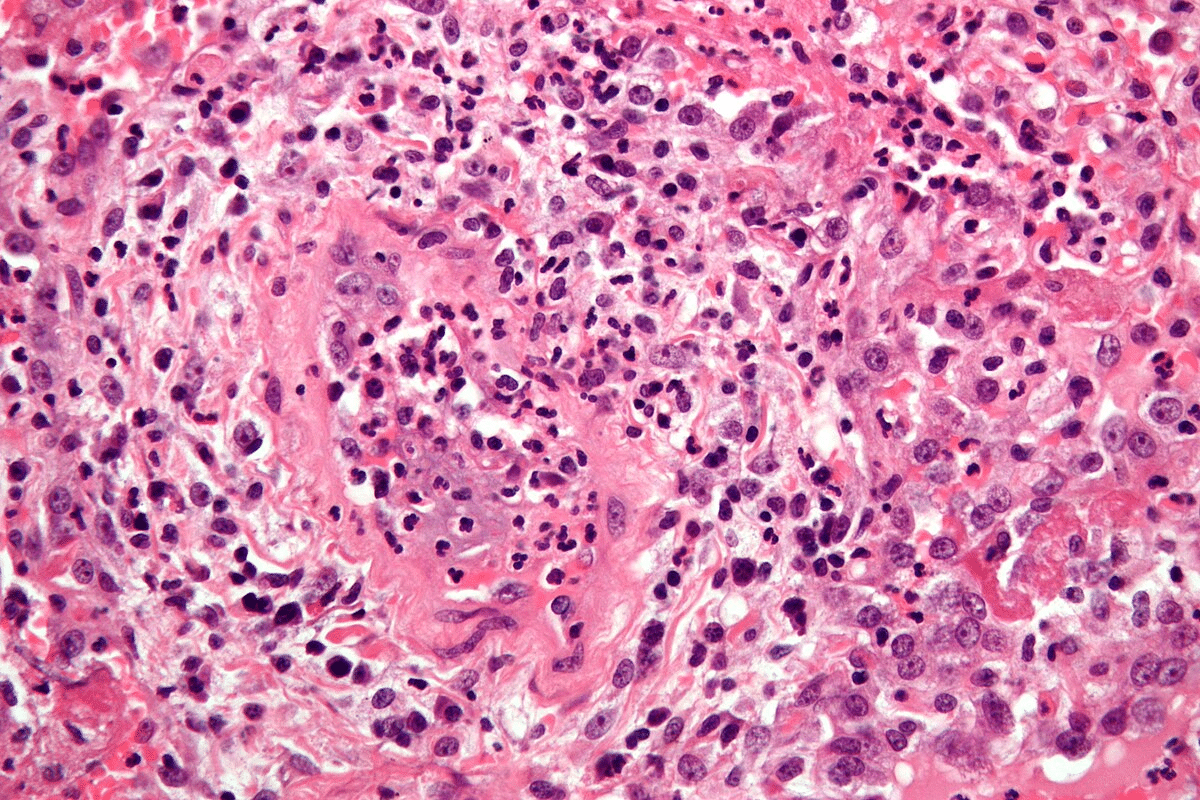
Vasculitis is when blood vessels get inflamed. This can harm tissues and organs because blood flow is blocked. When it hits the skin, it’s called cutaneous vasculitis. Knowing the signs and how to diagnose it is key to helping patients.
Cutaneous vasculitis shows up as different skin problems. These include palpable purpura and petechiae. At Liv Hospital, we use the latest tools and care with kindness to meet each patient’s needs.
Key Takeaways
- Cutaneous vasculitis involves inflammation of blood vessels in the skin.
- Recognizing symptoms such as palpable purpura and petechiae is key.
- Getting a diagnosis quickly is vital for good care and avoiding problems.
- Liv Hospital provides full care for those with cutaneous vasculitis.
- Our advanced tests help diagnose accurately and fast.
What is Cutaneous Vasculitis?
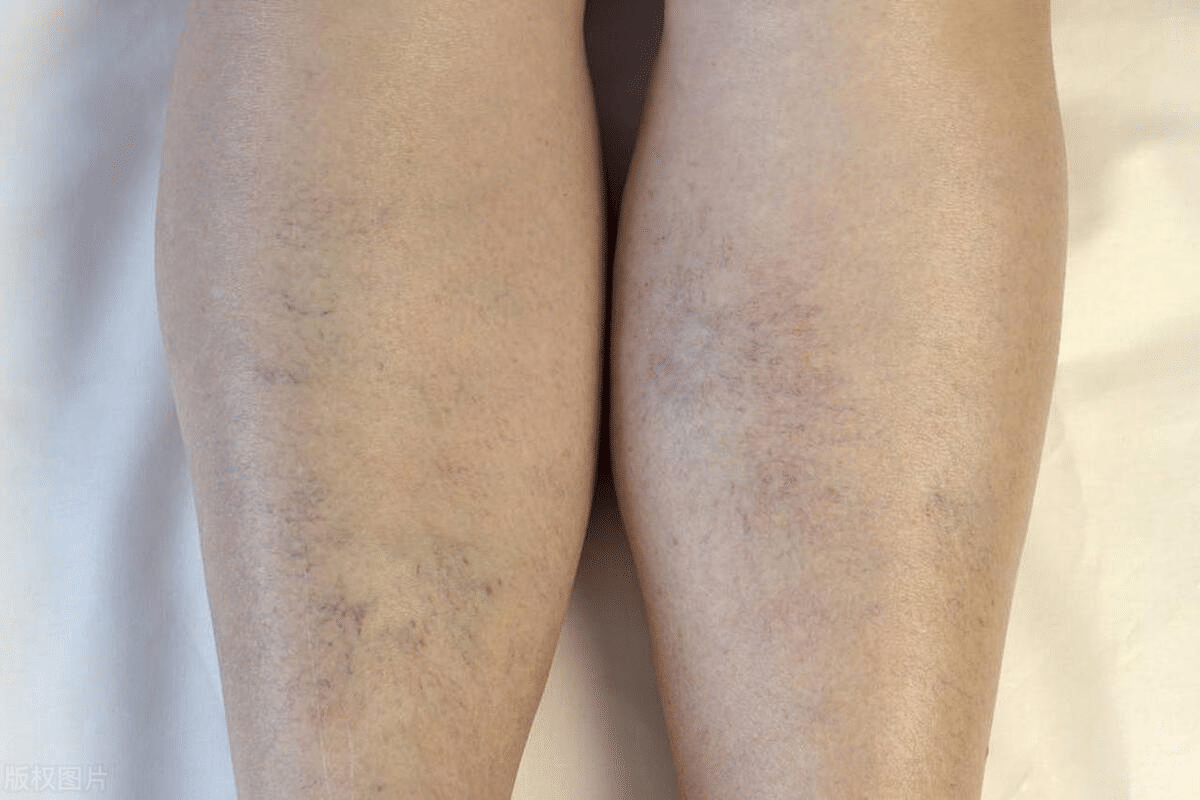
Cutaneous vasculitis is a group of disorders that cause inflammation in the skin’s blood vessels. It can show up in different ways, depending on the blood vessels involved.
Definition and Pathophysiology
Cutaneous vasculitis is when the blood vessel walls get inflamed. This can damage the vessels and lead to skin lesions. It happens when the immune system attacks the blood vessels.
This attack can be caused by infections, medicines, or autoimmune disorders. The inflammation can affect the blood vessels in different ways, from the smallest capillaries to the largest vessels.
Prevalence and Risk Factors
Cutaneous vasculitis can happen to anyone, but some types are more common in certain age groups. IgA vasculitis is the most common in kids, making up about 10% of all cases.
Some types might get better on their own, but most need treatment to control the inflammation. The Medical organization says medicines are often needed to manage it well.
|
Risk Factor |
Description |
|---|---|
|
Infections |
Bacterial, viral, or other infections can trigger cutaneous vasculitis. |
|
Autoimmune Disorders |
Conditions like lupus or rheumatoid arthritis can increase the risk. |
|
Medications |
Certain drugs can induce vasculitis as an adverse reaction. |
Knowing about the prevalence and risk factors of cutaneous vasculitis is key for early diagnosis and treatment.
Common Causes of Cutaneous Vasculitis

Cutaneous vasculitis can be caused by many things. This includes autoimmune disorders, infections, and certain medications. Knowing what causes it is key to treating it.
Autoimmune Disorders
Autoimmune disorders are a big reason for cutaneous vasculitis. Conditions like rheumatoid arthritis and systemic lupus erythematosus make the immune system attack blood vessels.
Other autoimmune conditions that can cause cutaneous vasculitis include:
- Granulomatosis with polyangiitis
- Microscopic polyangiitis
- Eosinophilic granulomatosis with polyangiitis
Infections
Infections are also a common cause. Bacterial, viral, and fungal infections can all lead to vasculitis. For instance, hepatitis B and C infections have been linked to it.
|
Infection Type |
Examples |
Association with Vasculitis |
|---|---|---|
|
Bacterial |
Streptococcal infections |
Can trigger vasculitis through immune complex deposition |
|
Viral |
Hepatitis B and C |
Cryoglobulinemic vasculitis is associated with hepatitis C |
|
Fungal |
Aspergillosis |
Rarely, fungal infections can cause vasculitis in immunocompromised individuals |
Medications and Other Triggers
Some medications can cause cutaneous vasculitis. These include:
- Antibiotics such as penicillins and sulfonamides
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Anticonvulsants
Other triggers include malignancies like lymphoma or leukemia. These can cause vasculitis in different ways.
Key Sign #1: Palpable Purpura
Palpable purpura is a key sign of cutaneous vasculitis. It shows as purple spots on the skin that can be felt when touched.
Characteristics and Appearance
The look of palpable purpura is very important for doctors to diagnose. These spots don’t change color when pressed, which is why they are called non-blanching. They can be different sizes and often appear on the lower legs.
Clinical observations also show that these spots can be with smaller spots called petechiae. Seeing both can mean a more serious problem.
Distribution and Progression
Palpable purpura spots usually show up on the legs and buttocks. Knowing how these spots spread is key for treatment.
A study found that spots like these often mean a more serious disease. This shows why catching it early is so important.
“The presence of palpable purpura is often associated with a more severe disease course.”
How these spots grow can change based on many things. This includes the cause and how well treatment works. Watching how these spots change is vital for managing the condition.
|
Characteristics |
Description |
|---|---|
|
Appearance |
Purple spots on the skin |
|
Palpability |
Can be felt upon examination |
|
Common Locations |
Lower extremities, legs, and buttocks |
Key Sign #2: Petechiae and Skin Lesions
In patients with cutaneous vasculitis, petechiae and other skin lesions are common. Petechiae are small, pinpoint spots that occur due to bleeding from small capillaries. They can be a sign of vasculitis among other conditions.
Identifying Petechiae in Vasculitis
Petechiae are often seen in patients with vasculitis, where small blood vessels are inflamed. To identify petechiae, clinicians should look for small, red or purple spots that do not blanch when pressed. These spots are typically found on the lower extremities but can appear anywhere on the body.
It’s important to differentiate petechiae from other skin conditions. For instance, capillaritis can also present with petechiae-like lesions, making diagnosis challenging. Understanding the differences between capillaritis and vasculitis is essential for accurate diagnosis.
Differentiation from Other Skin Conditions
Differentiating petechiae associated with vasculitis from other skin conditions requires careful examination. Conditions such as thrombocytopenia or trauma can also cause petechiae. A thorough medical history and physical examination are necessary to determine the underlying cause.
As noted by medical professionals, “Petechiae are a critical sign that requires further investigation to determine their cause.” Accurate diagnosis involves a combination of clinical evaluation, laboratory tests, and sometimes skin biopsies.
“The presence of petechiae should prompt a thorough evaluation for underlying vasculitis or other systemic conditions.”
For more information on cutaneous vasculitis and its manifestations, including images, one can refer to medical resources. These resources provide cutaneous vasculitis pictures and vasculitis skin images. They can aid in understanding the visual characteristics of the condition.
Key Sign #3: Urticarial Vasculitis
Urticarial vasculitis is a key sign of cutaneous vasculitis. It has a unique look. The lesions look like urticaria but are different in how long they last and what they look like under a microscope.
Clinical Presentation
Lesions from urticarial vasculitis are itchy or painful. They last more than 24 hours, unlike regular urticaria. They can show up anywhere on the body and might come with fever and joint pain.
Hypocomplementemic vs. Normocomplementemic Forms
Urticarial vasculitis comes in two types: hypocomplementemic and normocomplementemic. The hypocomplementemic form has lower blood complement levels. It can be more serious and affect other organs. The normocomplementemic form is milder, with fewer body-wide symptoms.
Knowing the difference between these types is key to treating it right. The hypocomplementemic form might need stronger treatment because of its risk of affecting other parts of the body.
Key Sign #4: Ulcers and Nodules
Ulcers and nodules are key signs of cutaneous vasculitis. They need careful checking. These signs can tell us a lot about the disease and how serious it is.
Development and Progression
Ulcers and nodules in cutaneous vasculitis come from inflammation and damage to blood vessels. This can cause tissue to die and form ulcers.
Key factors influencing their development include:
- Increased inflammatory response
- Vascular damage and ischemia
- Potential secondary infections
Common Locations and Characteristics
Ulcers and nodules from cutaneous vasculitis often appear on the lower legs.
Characteristics of these lesions include:
- Painful or painless ulcers
- Nodules that may be tender or non-tender
- Variable sizes and depths of ulcers
Looking at the ulcers and nodules is key to diagnosing cutaneous vasculitis. The image below shows what they look like.
Knowing about ulcers and nodules is vital for treating cutaneous vasculitis. We must look for these signs when checking patients. This helps us give them the right care.
Key Sign #5: Livedo Racemosa
Livedo racemosa is a sign linked to different vascular diseases, like vasculitis. It shows up as a mottled, net-like pattern on the skin. This pattern can hint at deeper health issues.
Visual Characteristics and Patterns
The look of livedo racemosa can change, but it often has a branching or net-like appearance. This happens because deeper skin vessels are affected in vasculitis. The pattern gets clearer in cold weather.
Livedo racemosa can show up on different body parts, mainly the extremities. Seeing it should lead to a detailed check for other vasculitis signs.
Association with Systemic Vasculitis
Livedo racemosa is more than just a skin issue; it’s linked to systemic vasculitis. Finding livedo racemosa might mean a serious condition needs a full check-up. Systemic vasculitis can hit many body parts, and livedo racemosa is a sign to look into further.
Spotting livedo racemosa as a sign of systemic vasculitis is key for early treatment. It shows why a team effort is needed to manage vasculitis patients.
Systemic Manifestations of Cutaneous Vasculitis
Patients with cutaneous vasculitis often face systemic symptoms that make their condition harder to manage. The main issue is in the skin, but the inflammation can spread to other parts of the body.
Fever and Constitutional Symptoms
Fever is a common symptom of cutaneous vasculitis. It often comes with other symptoms like fatigue, weight loss, and feeling unwell. These symptoms can really affect a patient’s life and how they feel overall.
When fever and other symptoms show up, it usually means the vasculitis is more serious. It’s important to treat these symptoms well to help patients get better and avoid serious problems later on.
Joint and Muscle Involvement
Many patients with cutaneous vasculitis complain of joint and muscle pain. The inflammation from vasculitis can hurt the muscles and joints, making it hard to move around.
In some cases, the pain in the joints can be very bad, like in other diseases. It’s important to check carefully to figure out if the pain is from vasculitis or something else.
|
Systemic Manifestation |
Frequency |
Clinical Implications |
|---|---|---|
|
Fever |
Common |
Indicates active inflammation |
|
Joint Pain |
Frequent |
May require additional treatment |
|
Muscle Pain |
Frequent |
Can impact mobility and quality of life |
Neurological and Renal Complications
Some patients with cutaneous vasculitis may develop neurological problems, like nerve damage. This happens when the inflammation affects the nerves.
Another serious issue is when the kidneys get involved. This can lead to kidney damage. It’s key to keep an eye on the kidneys to catch any problems early.
It’s vital to understand the systemic symptoms of cutaneous vasculitis for better care. By tackling these symptoms, we can help patients get better and avoid serious problems.
Diagnostic Approaches for Cutaneous Vasculitis
Diagnosing cutaneous vasculitis requires a detailed approach. This includes clinical assessment, lab tests, and histopathology. Let’s dive into each step.
Clinical Evaluation and History
The first step is a thorough clinical evaluation and history. We look at symptoms, medical history, and physical findings. Identifying the characteristic skin lesions is key.
We also examine the patient’s medical history. This helps find possible triggers or underlying conditions. It’s important to check the patient’s medication history too, as some drugs can cause vasculitis.
Laboratory Tests and Biomarkers
Laboratory tests are essential in diagnosing cutaneous vasculitis. They help measure inflammation and identify causes. Common tests include:
- Complete Blood Count (CBC)
- Erythrocyte Sedimentation Rate (ESR) or C-Reactive Protein (CRP)
- Urinalysis
- Serological tests for autoimmune disorders
|
Laboratory Test |
Purpose |
|---|---|
|
CBC |
Assess for anemia, leukocytosis, or thrombocytopenia |
|
ESR or CRP |
Measure inflammation levels |
|
Urinalysis |
Detect renal involvement |
|
Serological tests |
Identify autoimmune disorders |
“Laboratory tests are essential in diagnosing and managing cutaneous vasculitis, providing valuable information on the extent of inflammation and possible causes.”
– Medical News Today
Skin Biopsy and Histopathology
Skin biopsy is the most accurate way to diagnose cutaneous vasculitis. It involves examining the biopsy specimen under a microscope. This confirms vasculitis and identifies the affected vessels.
The biopsy findings also show the inflammation’s severity and any associated conditions. This information helps us decide on treatment and monitor the disease’s progress.
Treatment Strategies for Cutaneous Vasculitis
Cutaneous vasculitis treatment varies based on the condition’s severity and cause. It involves a detailed plan that looks at the patient’s health, skin involvement, and any systemic signs. This approach helps manage the condition effectively.
Mild Cases
For mild cutaneous vasculitis, a gentle approach works well. This includes supportive care like wound care and pain management. We also advise avoiding triggers that worsen the condition. Using compression stockings can help with swelling and improve blood flow.
Therapies for Moderate to Severe Disease
For more severe cases, stronger treatments are needed to control symptoms and prevent complications. Immunosuppressive therapies are used to fight inflammation and protect blood vessels. These may include corticosteroids or cyclophosphamide. For those not responding, intravenous immunoglobulin (IVIG) therapy is considered.
Emerging Treatment Options
New research offers hope for treating cutaneous vasculitis. Biologic agents like rituximab are being explored for their ability to target immune responses. We’re also looking into anti-inflammatory therapies to lessen vasculitis severity and improve patient results.
In summary, treating cutaneous vasculitis requires a personalized plan. Keeping up with new treatments and therapies ensures we offer the best care for those affected by this complex condition.
Conclusion
Cutaneous vasculitis is a complex condition that needs a deep understanding. We’ve talked about its signs and treatment options. Key signs include palpable purpura, petechiae, and ulcers.
Early diagnosis and treatment are key to better outcomes. Recognizing symptoms helps healthcare providers manage the condition well. This includes understanding its systemic effects.
Knowing the causes, diagnosis, and treatment of cutaneous vasculitis is vital. It helps us care for patients better. Timely medical care is essential to avoid complications and improve patient outcomes.
FAQ
What is cutaneous vasculitis?
Cutaneous vasculitis is inflammation of blood vessels in the skin. It can range from mild to severe. Symptoms include palpable purpura, petechiae, and skin lesions.
What are the common causes of cutaneous vasculitis?
It can be caused by autoimmune disorders, infections, and some medications. Knowing these causes helps in diagnosis and treatment.
What is palpable purpura, and how is it related to cutaneous vasculitis?
Palpable purpura is a sign of cutaneous vasculitis. It looks like purple spots on the skin that can be felt. It’s often seen on the legs and buttocks.
How is cutaneous vasculitis diagnosed?
Diagnosis includes a clinical evaluation, lab tests, and skin biopsy. These steps help find the cause and assess the condition’s extent.
What are the treatment options for cutaneous vasculitis?
Mild cases might be treated with supportive care. For more severe cases, immunosuppressive therapies are used. New treatments are also being explored.
Can cutaneous vasculitis affect other parts of the body beside the skin?
Yes, it can affect other parts of the body. Symptoms include fever, joint and muscle issues, and problems with the nervous system and kidneys. It’s important to manage these systemic effects.
What is the difference between hypocomplementemic and normocomplementemic urticarial vasculitis?
Hypocomplementemic urticarial vasculitis has low complement levels and is often more severe. Normocomplementemic urticarial vasculitis has normal complement levels and may be milder.
What is livedo racemosa, and how is it related to cutaneous vasculitis?
Livedo racemosa is a skin pattern that looks like a net. It’s often linked to systemic vasculitis. Recognizing this pattern is key to diagnosing vascular issues.
Are there any specific risk factors for developing cutaneous vasculitis?
Yes, certain factors like IgA vasculitis in childhood increase the risk. Knowing these risk factors helps in early diagnosis.
Can vasculitis skin lesions be confused with other skin conditions?
Yes, vasculitis skin lesions can look like other conditions, such as infections or allergic reactions. Accurate diagnosis requires a thorough evaluation and sometimes a skin biopsy.
References
National Center for Biotechnology Information. Cutaneous vasculitis. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC5533149/


































