A heart attack happens when the heart doesn’t get enough blood. This is usually because of a big blockage. Stenting is a common way to fix heart blockage, but it’s not always the best choice. Doctors decide if a stent is needed based on how bad the blockage is and the patient’s health 70 percent heart blockage symptoms.
It’s important to know the warning signs of heart blockage to get help quickly. Heart blockage signs can be different for everyone. But common ones include chest pain and feeling short of breath. Spotting these signs early can really help with treatment.
Key Takeaways
- The decision to consider stenting is based on the severity of the heart blockage.
- Individual patient health plays a key role in deciding treatment.
- Understanding 70 percent heart blockage symptoms is vital for diagnosis.
- Recognizing heart blockage signs early can improve treatment outcomes.
- The decision to use a stent is based on many factors, including the percentage of blockage.
Understanding Coronary Artery Disease and Heart Blockages
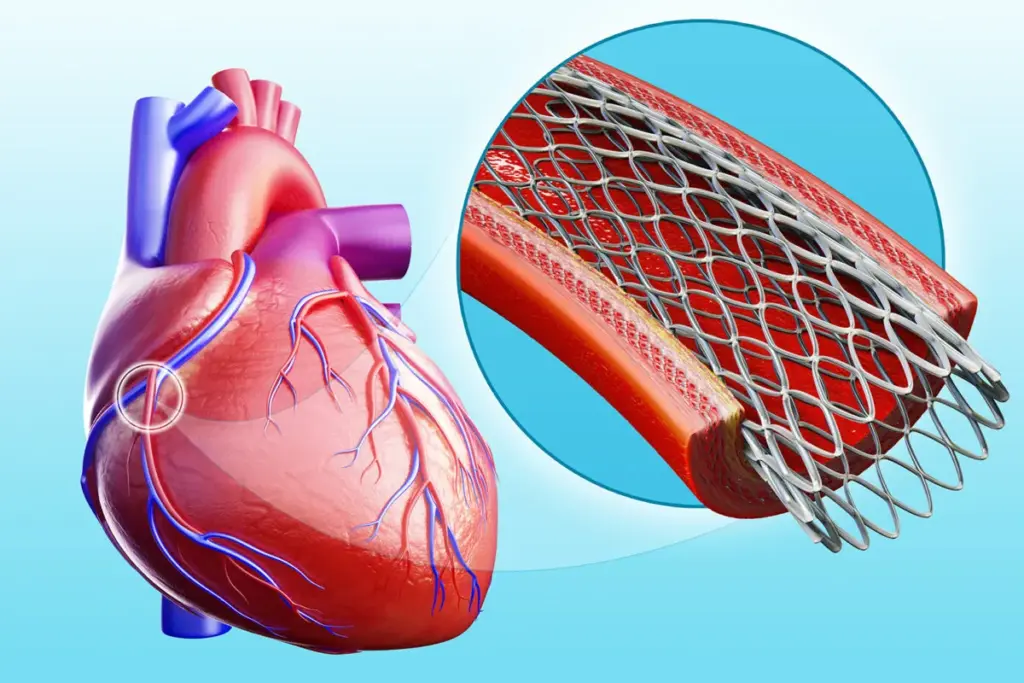
Coronary artery disease is a big problem. It happens when the arteries that carry blood to the heart get narrowed or blocked. This is a major cause of heart problems all over the world.
When the arteries that bring blood to the heart get damaged, it’s called coronary artery disease. This damage often comes from high cholesterol, high blood pressure, and smoking.
How Plaque Builds Up in Arteries
It starts with plaque buildup in the arteries. Plaque is a mix of fat, cholesterol, and other stuff. This buildup, called atherosclerosis, can narrow or block the arteries, cutting off blood to the heart.
As more plaque builds up, the artery walls get hard and narrow. This is called stenosis. It can reduce blood flow to the heart, causing chest pain or angina.
Different Degrees of Arterial Blockage
Arterial blockages can be different in how bad they are. A small blockage might not cause much trouble, but a big one can lead to a heart attack. Doctors measure how bad a blockage is by how much of the artery is blocked.
Blockages are divided into levels based on how much of the artery is blocked. Knowing these levels helps doctors figure out the best treatment.
Measuring Coronary Artery Blockages: The Percentage System

To figure out the right treatment, doctors use a percentage system to measure blockages. This system shows how severe the blockage is. It’s key for choosing the best treatment.
The system looks at how much the arteries are narrowed. This narrowing is due to plaque buildup. The percentage shows how much the artery is blocked.
Mild Blockage: 1-49% Stenosis
A mild blockage is 1-49% stenosis. At this level, the blockage isn’t severe enough to cause big symptoms. But, it’s important to watch it and manage risk factors.
Moderate Blockage: 50-69% Stenosis
Moderate blockage is 50-69% stenosis. This blockage is serious and can lead to symptoms or heart problems. Treatment might include lifestyle changes, medicine, or more serious procedures.
Severe Blockage: 70% and Above
Severe blockage is 70% or more stenosis. At this point, the risk of heart attack or serious heart issues is high. Stenting might be considered for blockages this severe.
|
Blockage Category |
Percentage Stenosis |
Typical Treatment Approach |
|---|---|---|
|
Mild |
1-49% |
Monitoring, risk factor management |
|
Moderate |
50-69% |
Lifestyle changes, medication, possible intervention |
|
Severe |
70% and above |
Stenting or other invasive procedures |
Knowing the percentage system for blockages is key for doctors and patients. It helps in choosing the right treatment.
70 Percent Heart Blockage Symptoms: Warning Signs You Shouldn’t Ignore
Knowing the signs of a 70 percent heart blockage is key for quick medical help. A blockage this big can cause serious health issues, like a heart attack.
Chest Pain and Angina
Chest pain or angina is a common sign of a big heart blockage. It feels like pressure or squeezing in the chest. This pain can spread to the arms, back, neck, jaw, or stomach.
Angina means the heart isn’t getting enough oxygen-rich blood.
Shortness of Breath
Shortness of breath or dyspnea is another important symptom. It happens when the heart can’t pump enough blood. This leads to fluid in the lungs.
This can happen even when you’re sitting or lying down. It’s a sign you need to see a doctor.
Fatigue and Weakness
Feeling very tired or weak is a symptom you shouldn’t ignore. A blockage in the heart can make you feel drained. This tiredness can be very strong and doesn’t get better with rest.
Other Common Symptoms
Other symptoms include:
- Light-headedness or dizziness
- Nausea or loss of appetite
- Rapid or irregular heartbeat
- Cold sweats
These symptoms can differ from person to person. They might not always show up. But if you or someone you know has these signs, getting medical help fast is important.
What level of blockage requires a stent?
Coronary artery disease is a big problem worldwide. It leads to a lot of sickness and death. Many patients need procedures like stenting to fix it.
Determining the level of blockage that necessitates a stent is key for good treatment and results. We look at symptoms, how much the heart is affected, and how complex the blockage is.
Choosing to use a stent depends on each patient. We consider their specific needs and health history.
Key Takeaways
- The level of blockage that requires a stent is determined by multiple factors.
- Severity of symptoms and extent of ischemia are key.
- Stenting is a common fix for coronary artery disease.
- The decision to place a stent is made for each patient.
- We consider each patient’s needs and health history.
Understanding Coronary Artery Disease and Heart Blockages
The coronary arteries carry blood to the heart muscle. They can narrow or block due to plaque buildup, known as coronary artery disease. This happens when cholesterol, fat, and other materials stick to the artery walls.
How Plaque Builds Up in Arteries
Plaque buildup starts early in life and grows slowly. It’s made of cholesterol, fatty substances, and more, hardening the arteries. Inflammation makes it worse.
As plaque grows, arteries become stiff and narrow. This limits blood flow to the heart. Symptoms like chest pain or shortness of breath show the heart isn’t getting enough oxygen and nutrients.
Different Degrees of Arterial Blockage
Blockages can be mild, moderate, or severe. Knowing the blockage’s level helps decide the right treatment.
|
Blockage Severity |
Description |
Percentage Stenosis |
|---|---|---|
|
Mild |
Little impact on blood flow |
1-49% |
|
Moderate |
Noticeable narrowing, possible symptoms |
50-69% |
|
Severe |
Big blockage, high heart attack risk |
70% and above |
It’s key to know the blockage level to manage coronary artery disease well. Mild blockages might not be a big worry. But, moderate to severe ones need serious medical attention to ensure blood flow to the heart.
Measuring Coronary Artery Blockages: The Percentage System
The percentage system helps measure how blocked the coronary arteries are. This is key for figuring out the right treatment. It shows how much the arteries are narrowed.
Mild Blockage
A mild blockage is 1-49% stenosis. At this point, the blockage isn’t too bad, and you might not feel any symptoms. But, it’s important to keep an eye on it to stop it from getting worse.
Moderate Blockage
A moderate blockage is 50-69% stenosis. Here, you might start to feel symptoms. Doctors might suggest lifestyle changes or other treatments.
Severe Blockage
Severe blockage is 70% stenosis or more. This blocks a lot of blood flow to the heart. You could feel severe chest pain and shortness of breath.
To understand coronary artery blockage better, let’s look at a table:
|
Blockage Level |
Percentage Stenosis |
Typical Symptoms |
Recommended Treatment |
|---|---|---|---|
|
Mild |
1-49% |
Minimal or none |
Monitoring, lifestyle changes |
|
Moderate |
50-69% |
May include angina, shortness of breath |
Lifestyle changes, medical management |
|
Severe |
70% and above |
Often includes significant chest pain, shortness of breath |
Medical intervention, potentially stenting or surgery |
70 Percent Heart Blockage Symptoms: Warning Signs You Shouldn’t Ignore
Knowing the symptoms of a 70 percent heart blockage is key to avoiding more heart problems. A blockage this severe can really hurt the heart’s ability to work right.
Chest Pain and Angina
Chest pain or angina is a common sign of a serious heart blockage. It feels like pressure or squeezing in the chest. It might also spread to the arms, back, neck, jaw, or stomach. Angina means the heart isn’t getting enough oxygen-rich blood.
Shortness of Breath
Shortness of breath or dyspnea is another important symptom. It happens when the heart can’t pump enough blood. This leads to fluid in the lungs, even when you’re resting.
Fatigue and Weakness
Feeling fatigued or weak can also be a sign of a serious heart blockage. The heart has to work harder because of the blockage. This can make you feel really tired.
Other Common Symptoms
Other signs include palpitations, dizziness, or nausea. A severe blockage can even cause a heart attack. This is a medical emergency that needs quick attention.
|
Symptom |
Description |
|---|---|
|
Chest Pain/Angina |
Pressure or squeezing in the chest, potentially radiating to other areas. |
|
Shortness of Breath |
Difficulty breathing, potentially at rest, due to fluid buildup in the lungs. |
|
Fatigue/Weakness |
Unusual tiredness or lack of energy due to the heart’s reduced efficiency. |
|
Other Symptoms |
Palpitations, dizziness, nausea, potentially leading to a heart attack. |
Spotting these symptoms early is very important. If you notice any of these signs, get medical help right away.
When Does a Blockage Require Intervention?
Knowing when a blockage needs medical help is key for good treatment. Coronary artery blockages are very serious. They can cause heart attacks if not treated right.
We look at many things to decide if help is needed. The blockage’s size is important, but it’s not everything.
The 70% Threshold for Intervention
A blockage is seen as big when it’s 70% or more stenosis. At this point, the chance of a heart attack goes up a lot. Getting help is often needed to stop more problems.
Factors Beyond Percentage That Influence Treatment Decisions
While blockage size is a big deal, we also look at other important things. These include:
- Symptoms: If you’re feeling chest pain or having trouble breathing, you might need help even with a blockage under 70%.
- Overall Health: People with health issues like diabetes or high blood pressure might get help sooner.
- Blockage Location: Where the blockage is in the artery can also affect the decision for treatment.
By looking at these factors, we can make smart choices about when to intervene. This helps ensure the best results for patients with coronary artery blockages.
Diagnostic Tests to Determine Blockage Severity
Knowing how severe a blockage is is very important. We use different tests to see how bad the blockages in the heart’s arteries are. Each test gives us important information about the heart’s health.
Non-Invasive Tests
Non-invasive tests are often the first step. They include:
- Stress Tests: These tests check how the heart works when it’s stressed, like during exercise or with medicine. They help find blockages.
- Electrocardiogram (ECG): An ECG shows the heart’s electrical activity. It can spot patterns that suggest blockages or other heart issues.
- Echocardiogram: This ultrasound makes pictures of the heart. It lets us see its shape and how well it works, including any blockages.
- Coronary Calcium Scan: This CT scan finds calcium in the heart’s arteries. Calcium buildup means there’s plaque.
Invasive Diagnostic Procedures
If non-invasive tests show a big blockage, we might need more detailed tests.
- Coronary Angiography: This involves putting dye in the arteries to see blockages with X-rays.
- Intravascular Ultrasound (IVUS): IVUS uses a special catheter to make detailed pictures of the arteries. It gives exact measurements of blockages.
- Fractional Flow Reserve (FFR): FFR checks the pressure difference across a blockage. It helps decide if we need to do something about it.
These tests are key to figuring out how bad the blockages are. By using both non-invasive and invasive tests, we get a full picture of the heart’s condition. This helps us make the best treatment plan.
Understanding Stents: What They Are and How They Work
Stents are key in treating coronary artery disease. They help restore blood flow to the heart. This keeps arteries open, improving blood flow and reducing symptoms.
Types of Coronary Stents
There are many types of coronary stents, each for different needs. The main types are:
- Bare-metal stents: These are made from metal mesh and are designed to keep the artery open.
- Drug-eluting stents: These stents release medication that prevents the artery from re-narrowing.
- Bioresorbable stents: These are made from materials that dissolve over time, reducing the risk of long-term complications.
|
Stent Type |
Description |
Benefits |
|---|---|---|
|
Bare-metal |
Made from metal mesh |
Simple design, less expensive |
|
Drug-eluting |
Releases medication to prevent re-narrowing |
Reduces risk of artery re-narrowing |
|
Bioresorbable |
Dissolves over time |
Reduces long-term complications |
How Stents Restore Blood Flow
Stents keep the artery open, improving blood flow to the heart. During a stenting procedure, the stent is placed at the blockage. It expands to support the artery walls, ensuring blood flow continues.
Understanding stents and their types helps patients make informed choices for treating coronary artery disease.
The Stent Placement Procedure: What to Expect
Learning about the stent placement procedure can ease your worries. We’ll walk you through each step, from getting ready to recovering. This way, you’ll know what to expect.
Preparation for the Procedure
Before the procedure, you’ll go through some steps. Your medical team will give you clear instructions on what medications to take or avoid. They’ll also tell you about any food restrictions. It’s important to share any allergies or health conditions with your doctor.
During Stent Implantation
During the procedure, you’ll get local anesthesia to numb the area. The procedure happens in a catheterization lab, and you’ll be watched closely.
- A small incision is made to access the artery.
- A catheter is guided to the blocked coronary artery.
- A balloon angioplasty is performed to open the blockage.
- A stent is placed to keep the artery open.
Immediate Recovery
After the procedure, you’ll go to a recovery area for monitoring. You’ll need to stay calm for a few hours to let the puncture site heal. Your team will guide you on what to do next and any follow-up visits.
Medical Management vs. Stenting: When Each is Appropriate
Choosing between medical management and stenting for coronary artery disease depends on the patient’s health. We’ll look at what makes each choice right for different patients.
Conservative Treatment for Mild to Moderate Blockages
For those with mild to moderate blockages, conservative treatment is often the first step. This includes diet changes, exercise, and medicines to manage symptoms. Our team helps patients create a treatment plan that fits their needs and goals.
Medicines like statins and beta-blockers are used to lower cholesterol and blood pressure. Antiplatelet drugs prevent clots. Lifestyle changes, such as a heart-healthy diet and regular exercise, are also key.
When Stenting is the Preferred Option
Stenting is usually for severe blockages or when medical management doesn’t work. Our cardiologists use imaging to decide the best treatment. They consider the benefits and risks of stenting.
Stenting involves placing a stent in the narrowed artery to improve blood flow. This is done during an angiogram, through a small incision in the wrist or groin.
Comparing Outcomes of Different Approaches
Both medical management and stenting can manage coronary artery disease well. The best choice depends on the patient. Studies look at symptom relief, quality of life, and survival to help decide.
A study found stenting quickly relieves symptoms, but medical therapy works well over time for some. We use this research to choose the best treatment for each patient.
By carefully looking at each patient’s situation and the latest research, we pick the right treatment. This could be medical management, stenting, or both.
Alternatives to Stents for Treating Heart Blockages
Heart blockages can be treated in many ways, not just with stents. Each method has its own benefits and is chosen based on the patient’s needs. This gives both patients and doctors more options.
Surgical Interventions
Coronary artery bypass grafting (CABG) is an alternative to stenting for some. It involves using a graft to bypass the blocked area. This helps restore blood flow to the heart.
Choosing CABG over stenting depends on the blockage’s severity and location. It also depends on the patient’s overall health.
Other Catheter-Based Treatments
Atherectomy is a catheter-based procedure that removes plaque. It’s an alternative to stenting for certain blockages.
Emerging Therapies
New treatments for heart blockages are being researched. Emerging therapies include advanced catheter technologies and new medicines.
Here’s a comparison of different treatment options:
|
Treatment |
Description |
Indications |
|---|---|---|
|
Stenting |
Minimally invasive procedure to place a stent |
Moderate to severe blockages |
|
CABG |
Surgical bypass of blocked artery |
Complex or multiple blockages |
|
Atherectomy |
Catheter-based removal of plaque |
Specific types of blockages |
Life After Stent Placement: Recovery and Rehabilitation
Knowing how to recover after a stent is key for a good outcome. The time after the procedure is important. It helps make sure the stent works right and the patient gets better fully.
Immediate Post-Procedure Care
Right after the stent is put in, patients stay in a recovery area for a few hours. Medical staff watch closely for any problems and make sure the patient is okay. Some patients might feel pain or bruising where the catheter was put in, but it usually goes away.
Important things to do right after the procedure include:
- Resting in bed for a few hours to avoid bleeding at the catheter site
- Watching for signs of trouble, like chest pain or trouble breathing
- Taking pain or discomfort medicine as told by doctors
Cardiac Rehabilitation Programs
Cardiac rehab is a big part of getting better after a stent. These programs help improve heart health with exercise, learning, and lifestyle advice.
Cardiac rehab offers many benefits, like:
- Getting stronger and more fit
- Managing heart disease risk better
- Learning about healthy eating and living
Medication Regimen
After a stent, patients usually take medicines to stop clots and manage heart health. It’s very important to take these medicines as told to make the stent work well and keep the heart healthy.
Some common medicines after a stent include:
- Antiplatelet drugs to stop clots
- Statins to lower cholesterol
- Beta-blockers to control blood pressure and heart rate
Potential Complications and Risks of Stent Procedures
Stent placement has greatly improved heart blockage treatment. Yet, it’s important to know about possible complications. While stent procedures are usually safe, some risks can happen.
Procedure-Related Complications
Complications from the procedure can include bleeding, infection, and damage to blood vessels. Some patients might have an allergic reaction to the stent or the drugs used during the procedure.
- Bleeding or hematoma at the access site
- Infection
- Damage to the blood vessel
- Allergic reactions to stent materials or medications
Long-term Stent Complications
Long-term issues can occur after a stent is placed. A big risk is restenosis, where the artery narrows again. This happens in up to 30% of patients, but drug-eluting stents have lowered this risk.
Other long-term problems include:
- Stent thrombosis, a blood clot inside the stent
- Restenosis, where the treated artery narrows again
Monitoring and Managing Complications
To reduce these risks, close monitoring and management are key. Patients often take antiplatelet therapy to prevent clots. Regular check-ups with healthcare providers are needed to watch the stent’s performance and handle any issues early.
It’s vital for patients to know the signs of complications, like chest pain or shortness of breath. If these symptoms occur, seek medical help right away.
Lifestyle Changes to Maintain Stent Health and Prevent Further Blockages
After getting a stent, it’s key to make big lifestyle changes. These changes help keep your stent working well and prevent heart problems later on.
Heart-Healthy Diet Recommendations
Eating right is very important after a stent. You should eat foods low in bad fats, cholesterol, and salt. Instead, choose foods high in fiber, vitamins, and minerals. Foods like fruits, veggies, whole grains, lean proteins, and healthy fats are great.
Nutritional Tips:
- Eat more omega-3 fatty acids from fish like salmon and sardines.
- Go for whole grains over refined ones.
- Stay away from foods with lots of added sugars and bad fats.
Exercise Guidelines After Stent Placement
Staying active is key for heart health after a stent. Aim for 150 minutes of moderate exercise, 75 minutes of vigorous exercise, or a mix of both each week.
|
Exercise Type |
Intensity |
Frequency |
|---|---|---|
|
Aerobic Exercise |
Moderate |
At least 150 minutes/week |
|
Aerobic Exercise |
Vigorous |
At least 75 minutes/week |
Smoking Cessation and Alcohol Moderation
Quitting smoking is a huge step for better heart health after a stent. Also, drink alcohol in moderation. Women should have no more than one drink a day, and men should have no more than two.
Quitting smoking can greatly lower your risk of heart disease and improve your health.
Stress Management Techniques
Too much stress can hurt your heart health. Try stress-reducing activities like meditation, yoga, or deep breathing every day.
Stress Reduction Tips:
- Do mindfulness meditation every day.
- Do physical activities you love.
- Stay connected with friends and family for support.
When to Seek Emergency Care After Stent Placement
It’s important to know the signs of stent failure to get timely help. After a stent is placed, watch for symptoms that could mean trouble with your stent or heart.
Warning Signs of Stent Failure
Stent failure is rare but can happen for reasons like blood clots or new tissue growth. Symptoms of stent failure include:
- Chest pain or discomfort, known as angina
- Shortness of breath
- Fatigue or weakness
- Pain or discomfort in the arms, back, neck, jaw, or stomach
If you notice these signs, get medical help right away.
Symptoms That Require Immediate Medical Attention
Some symptoms need quick action. If you have any of these, call for emergency help or go to the hospital:
- Severe chest pain or pressure that doesn’t go away
- Severe shortness of breath
- Dizziness or fainting
- Rapid or irregular heartbeat
Acting quickly can make a big difference in your health.
|
Symptom |
Action |
|---|---|
|
Chest pain or discomfort |
Seek immediate medical attention if severe or persistent |
|
Shortness of breath |
Seek immediate medical attention if severe |
|
Dizziness or fainting |
Seek immediate medical attention |
Staying informed and careful about your health after a stent is key. If unsure about your symptoms, always choose caution and see a doctor.
Preventing Coronary Artery Disease and Future Blockages
To prevent coronary artery disease and future blockages, we need a multi-step plan. This plan should tackle different risk factors. By managing these risks, people can lower their chance of heart problems.
Controlling Risk Factors
It’s key to control risk factors to stop coronary artery disease from getting worse. High blood pressure, high cholesterol, diabetes, smoking, and obesity are major risks. Working with your doctor to change your lifestyle and use medicine when needed is important.
Effective management strategies include:
- Managing blood pressure through diet, exercise, and medication
- Lowering cholesterol levels through dietary changes and statins
- Controlling blood sugar levels for diabetic patients
- Quitting smoking and avoiding secondhand smoke
- Maintaining a healthy weight through diet and exercise
Regular Medical Check-ups
Regular doctor visits are key to keeping an eye on your heart health. Your doctor will check your overall health and look for heart disease signs. They will also update your treatment plan if needed.
Recommended check-up frequency:
|
Risk Level |
Recommended Check-up Frequency |
|---|---|
|
Low Risk |
Annual check-ups |
|
Moderate Risk |
Bi-annual check-ups |
|
High Risk |
Quarterly check-ups or as advised by your healthcare provider |
Heart Health Screening Recommendations
Heart health screenings are a must for preventive care. These tests can spot risk factors and find heart disease early. Early detection makes treatment easier.
Recommended screenings include:
- Lipid profiles to check cholesterol levels
- Blood pressure checks
- Fasting glucose tests to screen for diabetes
- Electrocardiograms (ECGs) to assess heart function
- Stress tests to evaluate heart function under stress
Conclusion
It’s important to understand coronary artery disease and how stents help treat it. Stents are often used to open blocked arteries in the heart. This is key for keeping the heart healthy.
Changing your lifestyle and getting regular medical care are also critical. Eating well, exercising, and managing stress can help avoid future heart problems. These steps are important for the success of stent placement.
Don’t forget the importance of regular health check-ups and screenings. They help catch heart issues early. Working with your healthcare team is a great way to keep your heart in good shape and prevent disease.
FAQ
What is considered a significant blockage in the coronary arteries?
A blockage is seen as significant when it reaches 70% or more stenosis. The exact threshold for intervention can vary. It depends on the individual patient’s factors and symptoms.
How is the severity of coronary artery blockage measured?
The severity is measured using a percentage system. It categorizes blockages into three levels. These are mild (1-49% stenosis), moderate (50-69% stenosis), and severe (70% and above).
What are the symptoms of 70% heart blockage?
Symptoms include chest pain or angina, shortness of breath, fatigue, and weakness. Some people may not show any symptoms at all.
Can a pacemaker or defibrillator prevent heart blockage?
No, devices like pacemakers or implantable cardioverter-defibrillators (ICDs) are used to manage heart rhythm issues. They do not prevent or treat coronary artery blockages directly.
Are there lifestyle changes that can help prevent further blockages after stent placement?
Yes, adopting a heart-healthy diet, exercising regularly, quitting smoking, and moderating alcohol consumption can help. Managing stress is also important to maintain stent health and prevent future blockages.
What are the risks associated with stent placement?
Risks include procedure-related complications like bleeding or vascular injury. Long-term complications such as stent thrombosis or restenosis can also occur.
How often should I have medical check-ups after stent placement?
Regular follow-up appointments with your healthcare provider are essential. They help monitor your condition, adjust medications as needed, and address any concerns or symptoms.
Can I use a microwave oven if I have a pacemaker?
Generally, microwave ovens are safe for individuals with pacemakers. It’s best to follow the manufacturer’s guidelines and consult with your healthcare provider.
What is the difference between a pacemaker and an ICD?
A pacemaker helps control the heartbeat at a stable, normal rate. An ICD is designed to prevent sudden death from cardiac arrhythmias. It delivers an electric shock when necessary.
How do I manage stress after stent placement?
Stress management techniques like meditation, deep breathing exercises, or yoga can be beneficial. Maintaining a healthy work-life balance and engaging in enjoyable activities is also helpful.
References
JAMA Network. Evidence-Based Medical Insight. Retrieved from https://jamanetwork.com/journals/jama/fullarticle/193148)





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























