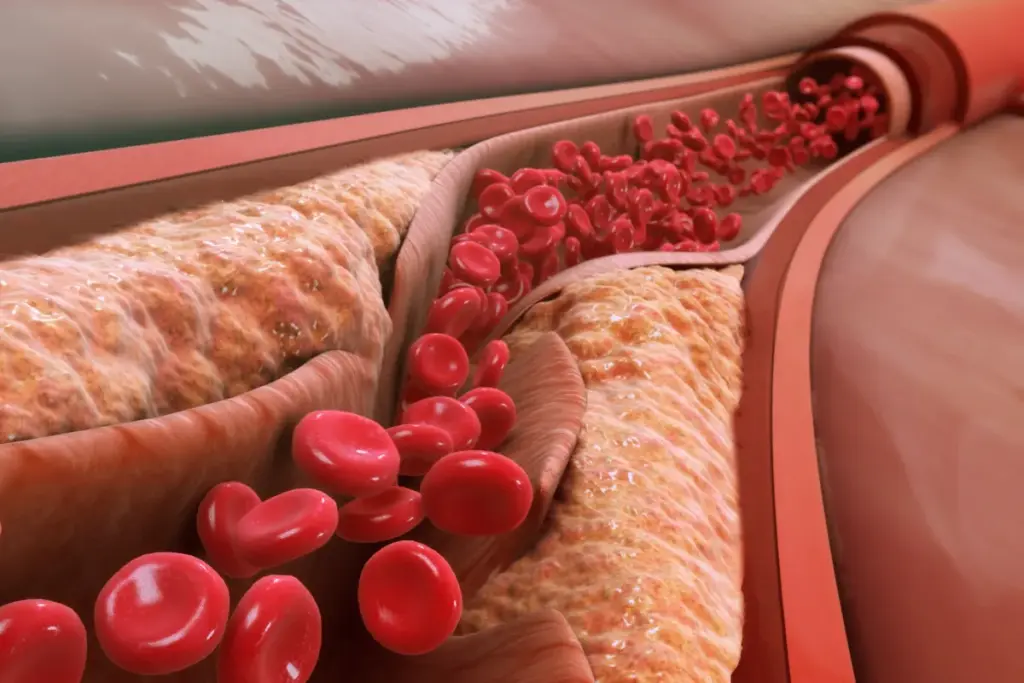
Peripheral artery disease (PAD) is a big problem worldwide. About 8.5 million Americans aged 40 and older have it. It happens when the arteries in your limbs get narrow, cutting off blood flow.
Knowing who is at risk of PAD is key to catching it early. Some groups are more likely to get it. These include older people and those who have had heart disease before.
Key Takeaways
- PAD is a big risk for heart problems.
- Older adults are more likely to get PAD.
- Having heart disease before makes you more likely to get PAD.
- Finding out who is at high risk is important for early detection.
- PAD can cut off blood flow to your limbs, causing mobility issues.
Understanding Peripheral Artery Disease: A Complete Overview

It’s key to understand peripheral artery disease well for early detection and treatment. Peripheral artery disease (PAD) is when the arteries in the limbs get narrowed. This reduces blood flow to the limbs.
What is Peripheral Artery Disease?
PAD is linked to atherosclerosis. This is when plaque builds up in arteries, causing them to narrow. This can greatly cut down blood flow to the limbs, leading to symptoms.
The American Heart Association says PAD needs thorough management. This is to stop it from getting worse and to lower heart disease risks.
How PAD Affects the Body
PAD mainly hits the arteries that carry blood to the legs. It causes symptoms like intermittent claudication (pain when walking) and coldness in the limb. As PAD gets worse, it can make moving around harder and raise the risk of heart problems.
The less blood flow from PAD can cause a lot of pain. In severe cases, it can even lead to gangrene.
Common Symptoms and Progression
Signs of PAD include leg pain when active, feeling cold or discolored in the limb. As the disease gets worse, symptoms can get more severe. This can lead to pain even when not moving and serious complications.
- Leg pain during walking (intermittent claudication)
- Coldness or numbness in the legs
- Pain at rest
- Gangrene in advanced cases
Spotting PAD early and treating it is vital. It helps stop the disease from getting worse and lowers the risk of heart problems.
PAD Risk Factors Demographics: The Complete Picture
It’s key to know the demographics that affect peripheral artery disease (PAD) risk. This knowledge helps in making better prevention and treatment plans. By looking at demographics, healthcare providers can better meet the needs of different groups.
Defining Risk Demographics
Risk demographics are the traits of a group that affect their chance of getting PAD. These traits include age, gender, ethnicity, and socioeconomic status. Knowing these helps healthcare providers focus on high-risk groups.
Age is a big factor, with PAD risk going up after 50. Gender also matters, with studies showing men and women have different PAD risks.
The Importance of Demographic Analysis in PAD
Demographic analysis is key for understanding PAD risk. It helps find out who is most at risk. By studying who gets PAD, researchers and doctors can find out which risk factors are most important for different groups.
This info is critical for making prevention and treatment plans that work. For example, some ethnic groups might be at higher risk because of their genes. Socioeconomic factors can also affect who gets diagnosed and treated for PAD.
How Demographics Influence Treatment Approaches
Demographics shape how PAD is treated. Older adults might need gentler care because of other health issues. Younger patients might get more aggressive treatments to lower their heart disease risk.
It’s vital to understand these differences for personalized care. By considering age, gender, and ethnicity, doctors can create treatment plans that fit each person’s needs and risk level.
Age as a Primary Risk Factor for PAD
As people age, their risk of getting peripheral artery disease (PAD) goes up. Studies show that PAD prevalence increases significantly with age, after 65 years old.
PAD Prevalence by Age Group
The risk of PAD grows with age. Most PAD cases are found in people over 65. This age group faces more risks because of aging and other factors.
Why Aging Increases PAD Risk
Aging brings changes to blood vessels that can lead to PAD. Arteries become less flexible and narrow with age, affecting blood flow. Older adults also face more health issues like diabetes and high blood pressure, making PAD worse.
Age-Related Vascular Changes
Changes in blood vessels with age are key to PAD. These include increased arterial stiffness and reduced vascular function. Stiffer arteries struggle with blood pressure changes, putting more strain on the system. The inner lining of blood vessels also gets less efficient, making it harder to control blood flow.
Knowing about these changes helps spot who’s at risk for PAD. It’s important for early prevention.
Gender Differences in PAD Risk and Presentation
Peripheral artery disease (PAD) affects both men and women. But, there are big differences in how it shows up and how common it is. Knowing these differences is key for the right diagnosis and treatment.
Male vs. Female PAD Prevalence
Research shows PAD is common in both men and women. But, men tend to get it younger than women. Women’s risk goes up a lot after menopause, showing how hormones play a part.
Key statistics on PAD prevalence by gender:
- Men under 50 are more likely to develop PAD than women of the same age group.
- PAD prevalence in women increases after menopause, potentially due to declining estrogen levels.
- Women are more likely to be asymptomatic or have atypical symptoms, making diagnosis more challenging.
Hormonal Influences on PAD Development
Hormonal changes, like the drop in estrogen after menopause, affect PAD risk. Estrogen helps protect blood vessels. Its decrease may raise PAD risk in older women.
Gender-Specific Symptoms and Diagnosis Challenges
Men and women show PAD symptoms differently, making diagnosis tricky. Men usually have clear symptoms like leg pain when walking. Women often have less obvious symptoms, making it harder to catch PAD early.
Common gender-specific symptoms include:
- Men: Intermittent claudication, leg pain during exercise.
- Women: Atypical leg pain, decreased functional capacity without clear claudication symptoms.
Doctors need to know these differences to give the right care and catch PAD early.
Ethnic and Racial Disparities in PAD Diagnosis
Ethnic and racial disparities in PAD diagnosis are a big concern. Some groups face a higher risk of this disease. Peripheral artery disease (PAD) affects blood vessels outside the heart, reducing blood flow to limbs.
The disease’s prevalence varies among ethnic and racial groups. This highlights the need for targeted healthcare approaches.
PAD Prevalence Among Different Ethnic Groups
Studies show African Americans are at a higher risk of PAD. The disease’s prevalence is about 7.8% in African Americans, compared to 4.4% in non-Hispanic whites. This disparity shows the need to understand PAD risk factors in diverse populations.
“The higher prevalence of PAD in African Americans is a critical concern,” said a researcher. “It necessitates further investigation into genetic, environmental, and socioeconomic factors.”
Genetic Factors Contributing to Racial Disparities
Genetic factors are key in PAD development. Certain genetic variations are more common in specific ethnic groups. For example, genetic studies have found variants linked to PAD risk in African Americans.
Understanding these genetic factors helps in developing targeted interventions for high-risk groups.
- Genetic variants associated with PAD risk
- Ethnic-specific genetic markers
- Gene-environment interactions influencing PAD development
Socioeconomic Factors and Healthcare Access
Socioeconomic factors, like healthcare access, education, and income, affect PAD diagnosis and management. People from lower socioeconomic backgrounds often face barriers to healthcare. This leads to delayed diagnosis and treatment.
Addressing these disparities is key to improving health outcomes in diverse populations.
Key socioeconomic factors include:
- Access to healthcare services
- Education and health literacy
- Income level and economic stability
Understanding genetic, socioeconomic, and environmental factors helps healthcare providers. They can then develop more effective strategies for PAD prevention and treatment in diverse groups.
Lifestyle Factors Contributing to PAD Risk
Peripheral artery disease (PAD) risk is tied to lifestyle choices we can change. Knowing and adjusting these factors can lower PAD risk.
Smoking and Tobacco Use
Smoking and tobacco use are big risks for PAD. Tobacco harms artery linings, making them block more easily. The American Heart Association says smoking causes a lot of PAD cases. Quitting smoking greatly lowers PAD risk and boosts heart health.
Key statistics on smoking and PAD:
- Smokers face up to four times the risk of PAD compared to non-smokers.
- Secondhand smoke also raises PAD risk.
- Quitting smoking can cut PAD risk by up to 50% in a few years.
Physical Inactivity and Sedentary Behavior
A sedentary lifestyle is a big PAD risk. Exercise keeps blood flowing and stops plaque buildup. But sitting too much harms circulation and raises PAD risk.
Benefits of regular physical activity for PAD prevention:
- Boosts blood flow and circulation.
- Helps manage weight and lower obesity-related PAD risk.
- Lowers blood pressure and improves heart health.
Dietary Patterns and Nutritional Factors
Diet is key in PAD development. Eating lots of saturated fats, cholesterol, and sodium ups PAD risk. But, a diet full of fruits, veggies, and whole grains can help.
Key dietary recommendations for PAD prevention:
- Eat more omega-3s from fish and nuts.
- Reduce processed and high-sodium foods.
- Focus on whole grains, fruits, and veggies.
By tackling these lifestyle areas, we can lower our chance of getting PAD.
Comorbidities and Their Impact on PAD Development
It’s important to know how comorbidities affect PAD. Comorbidities are other health issues that often happen with PAD. They can change how the disease gets worse and how well treatments work.
Diabetes and PAD: A Dangerous Combination
Diabetes makes PAD worse by speeding up atherosclerosis. This is the main cause of PAD. When diabetes and PAD are together, it raises the risk of heart problems and makes treatment harder.
- Increased risk of foot ulcers and amputations
- Higher likelihood of cardiovascular morbidity
- Challenges in managing blood glucose levels
Hypertension as a PAD Risk Multiplier
Hypertension also plays a big role in PAD. High blood pressure can harm blood vessels more, making PAD symptoms worse. It also raises the chance of heart problems.
Key considerations include:
- Monitoring blood pressure regularly
- Managing hypertension through lifestyle changes and medication
- Assessing cardiovascular risk factors comprehensively
Hyperlipidemia and Atherosclerosis
Hyperlipidemia, or high cholesterol and triglycerides, leads to atherosclerosis. This is the main cause of PAD. It’s key to manage high lipid levels to slow down PAD.
Effective management strategies include diet changes, exercise, and medicines to lower lipids. It’s important to understand how hyperlipidemia and PAD work together. This helps create treatment plans that fit each person’s needs.
Socioeconomic Factors Influencing PAD Prevalence
Socioeconomic factors greatly impact peripheral artery disease (PAD). They affect how well people can get healthcare, know about the disease, and stay healthy.
Education and PAD Awareness
Education is key in understanding PAD. People with more education are more aware of PAD risks. Public health efforts to teach about PAD can lead to better management.
Income Level and Healthcare Access
Income also plays a big role in PAD. Those with less money often can’t get the healthcare they need. More affordable healthcare can help fix this problem.
Geographic Variations in PAD Diagnosis
Some places have more PAD cases than others. This is due to many factors like healthcare access and lifestyle.
Knowing why PAD varies by place is important. It helps us create better plans to fight PAD. By tackling these issues, we can help everyone get better care.
Family History and Genetic Predisposition to PAD
Family history is key in figuring out PAD risk. It’s a big deal in diagnosing the condition. People with a family history of PAD or heart disease are more likely to get PAD.
Hereditary Risk Factors
Studies show that genes can play a part in PAD. Some genetic markers are passed down, raising the risk. Family history is a big risk factor that can’t be changed. But knowing it can help catch PAD early.
Genetic Markers Associated with PAD
Many genetic markers are linked to a higher PAD risk. These markers can spot people at risk early. Genetic testing can show an individual’s risk level.
Family Screening Recommendations
Those with PAD in their family should get checked often. The Ankle-Brachial Index (ABI) test is a simple way to find PAD early. Family members should talk to their doctor about their risk and follow screening advice.
Knowing your family history and genetic risk can help manage PAD risk. Being aware of these factors lets people take steps to prevent and catch PAD early.
High-Risk Occupations and PAD Development
Peripheral artery disease (PAD) is more common in certain jobs. Workers in these jobs often stand or sit for long hours. They may also face harmful environmental factors. Knowing these risks is key to spotting PAD early and preventing it.
Jobs Requiring Prolonged Standing or Sitting
Jobs that make you stand or sit for hours can harm your blood vessels. Prolonged standing puts extra pressure on your legs, making PAD symptoms worse. On the other hand, prolonged sitting can cut down blood flow and raise PAD risk.
Jobs in manufacturing, transportation, and customer service are examples of high-risk jobs. This is because they often involve standing or sitting for long periods.
Occupational Exposure to Environmental Factors
Some jobs expose workers to harmful environmental factors that increase PAD risk. Exposure to pollutants like particulate matter and carbon monoxide can harm blood vessels. For example, workers in construction, mining, or those around secondhand smoke are at higher risk.
Work-Related Stress and Vascular Health
Work-related stress can also lead to PAD. Stress can raise blood pressure and heart rate, straining blood vessels. Jobs with high stress levels, like healthcare, finance, or emergency services, may see more PAD cases.
It’s important to understand how work affects PAD risk. This knowledge helps healthcare providers give better advice and help prevent PAD in different jobs.
PAD Risk Assessment Tools and Screening Recommendations
The Ankle-Brachial Index (ABI) is a key method for PAD screening, mainly for those at high risk. Accurate PAD diagnosis is vital for effective treatment. There are many tools to help doctors spot those at risk.
Ankle-Brachial Index (ABI) Testing
The ABI test compares ankle and arm blood pressure. A lower reading means PAD. It’s great for:
- Diagnosing PAD in symptomatic patients
- Screening asymptomatic individuals at high risk
- Monitoring disease progression
Doctors recommend ABI testing for those with PAD symptoms, like leg pain when walking. It’s also for high-risk groups, like older adults and those with diabetes or a smoking history.
|
ABI Value |
Interpretation |
|---|---|
|
1.00-1.40 |
Normal |
|
0.91-0.99 |
Borderline |
|
0.41-0.90 |
Mild to Moderate PAD |
|
0.00-0.40 |
Severe PAD |
Screening Guidelines for High-Risk Populations
Screening guidelines suggest ABI testing for high-risk groups, including:
- Individuals aged 65 and older
- Those with a history of smoking or diabetes
- Patients with known atherosclerotic disease
Early detection through ABI testing can lead to timely intervention. This can lower the risk of heart problems and improve life quality.
Understanding PAD risk assessment tools and following screening guidelines helps healthcare providers manage PAD better. This improves patient outcomes.
Preventive Strategies for High-Risk Demographics
For those at high risk of peripheral artery disease (PAD), it’s key to take steps to prevent it. Understanding and tackling PAD risk factors is essential. This way, high-risk groups can lower their chances of getting the disease.
Lifestyle Modifications for PAD Prevention
Making lifestyle changes is vital in preventing PAD. Stopping smoking is a big step, as smoking greatly increases PAD risk. Also, exercising more helps improve blood flow and heart health.
Eating well is another important change. A diet full of fruits, veggies, whole grains, and lean meats helps manage weight and blood pressure. These factors are key in lowering PAD risk.
Patient Education and Self-Monitoring
Teaching patients about PAD is critical. Knowing the risks and symptoms empowers them to care for their health. This includes regular doctor visits and screenings, which are important for those at risk.
Keeping an eye on your body is also key. Look out for signs like leg pain when walking. Catching PAD early can stop it from getting worse.
Combining lifestyle changes with education and self-checks can greatly reduce PAD risk. Healthcare teams are essential in guiding these efforts. They offer the support and advice needed by high-risk individuals.
Future Trends in PAD Demographics and Risk Assessment
Research is changing how we see Peripheral Artery Disease (PAD). New trends and tech are set to change how we understand and manage PAD.
Emerging Risk Factors
New studies have found risk factors for PAD. These include biomarkers and genetic markers that could improve risk assessment.
Novel Biomarkers: New biomarkers for PAD have been found. These could help detect and track the disease early.
|
Biomarker |
Description |
Potential Impact |
|---|---|---|
|
C-reactive protein (CRP) |
Indicator of inflammation |
Early detection of PAD risk |
|
Lipoprotein(a) [Lp(a)] |
Genetic marker associated with cardiovascular risk |
Identification of genetic predisposition to PAD |
Personalized Risk Prediction
Personalized medicine is key in managing PAD. Advanced genetic analysis and machine learning help tailor risk predictions and treatment plans.
Using new risk factors in personalized models is a big step in PAD management. It helps target interventions more effectively.
Key Elements of Personalized Risk Prediction:
- Genetic analysis to identify predispositions
- Advanced biomarker testing for early detection
- Machine learning algorithms to analyze complex data sets
Conclusion: Understanding Your Personal PAD Risk Profile
Knowing your PAD risk profile is key to preventing and catching PAD early. By looking at your personal risk factors, you can lower your chance of getting PAD. This also helps avoid heart problems.
A detailed spots risk factors like age, gender, and lifestyle. This info lets doctors create plans to help you stay healthy. It also helps improve your health outcomes.
When you know your PAD risk, you can make better health choices. You can change your lifestyle and get regular check-ups. These steps can greatly lower your risk of PAD and its serious side effects.
It’s important to keep up with new PAD research and guidelines. This knowledge helps both doctors and people at risk. It lets you manage your blood vessel health better, helping you and the healthcare system.
FAQ
What are the primary risk factors for developing peripheral artery disease (PAD)?
PAD risk factors include age, smoking, and diabetes. Also, hypertension, high cholesterol, and family history play a role. Lifestyle choices like not exercising and eating too much saturated fat are also important.
How does age affect the risk of developing PAD?
Age is a big risk factor for PAD. After 65, the risk goes up a lot. This is because arteries get stiffer and work less well with age.
Are there gender differences in PAD risk and presentation?
Yes, men and women show PAD symptoms differently. Hormones can also affect who gets PAD. It’s key to understand these differences for the right diagnosis and treatment.
How do ethnic and racial disparities impact PAD diagnosis?
Some ethnic and racial groups face higher PAD risks. This is due to genetics, money issues, and healthcare access. These disparities lead to health inequalities.
What lifestyle factors contribute to PAD risk?
Smoking, not moving enough, and eating too much saturated fat increase PAD risk. Eating fewer fruits and veggies also plays a part.
How do comorbidities like diabetes and hypertension affect PAD risk?
Diabetes, high blood pressure, and high cholesterol make arteries worse. This speeds up PAD and raises the risk of heart problems.
What is the role of socioeconomic factors in PAD prevalence?
Money, education, and healthcare access affect PAD rates. These factors influence who gets diagnosed and treated.
How does family history influence PAD risk?
A family history of PAD or heart disease increases your risk. Genetic tests can spot those at higher risk.
What occupations are considered high-risk for PAD development?
Jobs that make you stand or sit a lot, or expose you to pollutants, raise PAD risk. So does work stress.
What is the Ankle-Brachial Index (ABI) test, and how is it used in PAD diagnosis?
The ABI test checks for PAD by comparing ankle and arm blood pressure. It’s a simple, non-invasive test.
What preventive strategies can high-risk demographics adopt to reduce PAD risk?
Quit smoking, exercise regularly, and eat well to lower PAD risk. Education and self-checks are also key.
How will future trends in PAD demographics and risk assessment evolve?
New risk factors and personalized tests will shape PAD trends. Genetic research and biomarkers will help predict and prevent PAD better.
References
The Lancet. Evidence-Based Medical Insight. Retrieved from https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(13)61249-0/fulltext


































