Rheumatology treats musculoskeletal and autoimmune diseases, including arthritis, lupus, gout, and vasculitis.
Send us all your questions or requests, and our expert team will assist you.

Fibromyalgia diagnosis lacks specific lab tests or X-rays, relying on history, exams, and ruling out other conditions. Rheumatologists address overlapping pain and fatigue symptoms thoroughly to exclude treatable alternatives.
Diagnosis of fibromyalgia starts with a detailed medical history focusing on pain patterns consistent with fibromyalgia, such as widespread pain for at least three months. Doctors also assess sleep quality, cognitive issues like “fibro fog,” and other symptoms like headaches or digestive problems to rule out other conditions.
Since fibromyalgia is a “diagnosis of exclusion,” the doctor must verify that no other diseases are causing your pain. Several autoimmune and rheumatic conditions can mimic fibromyalgia. Therefore, the evaluation often involves testing for these “mimics” before confirming fibromyalgia.
Common conditions that must be ruled out include:

While blood tests cannot detect fibromyalgia directly, they are essential for the exclusion process mentioned above. Your doctor will likely order a “rheumatology profile” or a comprehensive panel. These tests check for markers of inflammation and organ function.
Standard blood tests often include:
Normal lab results, lacking elevated inflammation markers, support a fibromyalgia diagnosis as it shows no inflammatory process.
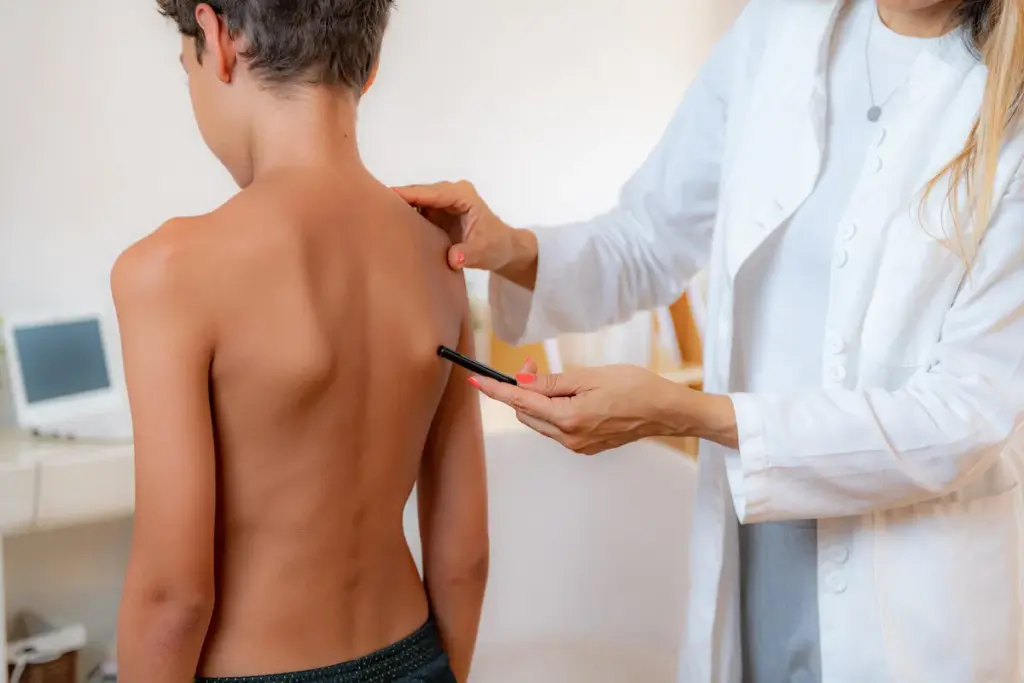
Historically, doctors used a “tender point” test to diagnose fibromyalgia. This involved pressing on 18 specific points on the body to see if it caused pain. While this strict test is no longer the only requirement, a physical exam remains a vital part of the evaluation.
Step-by-Step Exam Process:
Modern diagnosis relies on specific criteria developed by the American College of Rheumatology. These criteria allow doctors to score your symptoms to see if they meet the threshold for fibromyalgia. This moves the diagnosis away from just “tender points” to a more holistic view of how the condition affects your life.
Your doctor will evaluate you based on two main scores:
If your scores on these two scales meet a certain mathematical threshold, and symptoms have persisted for three months, a diagnosis is confirmed.
Imaging is not used to “see” fibromyalgia, as the condition involves the nervous system and does not show up on scans. However, imaging is frequently used to inspect the body for structural damage that could be causing your pain.
Common Imaging Tests:
If you have fibromyalgia, these scans will usually look normal. If an MRI shows a herniated disc, it suggests the pain might be nerve-related rather than fibromyalgia, or that you might have both conditions (comorbidities).
Tracking history aids accurate diagnosis.
Pre-visit Checklist:
It can be confusing for patients when a doctor says, “Your test results are normal,” but the patient is in severe pain. In the context of fibromyalgia, “normal” test results are actually a positive step toward diagnosis.
What the Doctor Looks For:
When all these physical causes are ruled out, the doctor can confidently identify the issue as Central Sensitization—the hallmark of fibromyalgia, where the nervous system amplifies pain signals.
Standard methods diagnose most, but atypical symptoms may require advanced testing for rare conditions.
Advanced Referrals May Include:

Send us all your questions or requests, and our expert team will assist you.
There is no single “fibromyalgia test.” Diagnosis is a clinical process involving a physical exam to check for tenderness, a review of your symptom history (pain, fatigue, sleep issues), and blood tests (like CBC, ESR, and thyroid function) to rule out other conditions like arthritis or lupus.
To prepare, keep a symptom diary for two weeks detailing your pain levels, fatigue, and “brain fog.” Make a list of all medications and supplements you take. Bring copies of any previous medical records, X-rays, or blood test results to the appointment to help the doctor see the full picture.
The examination involves checking for “tender points” by applying mild to moderate pressure on specific areas of your body. This may cause temporary discomfort or a spike in pain at those specific spots, but the exam itself is generally not considered painful and is non-invasive.
Rheumatology tests are highly accurate for excluding other diseases. For example, blood tests are excellent at detecting inflammation or autoimmune markers. When these specific markers are absent, and the patient meets the criteria for widespread pain, the clinical diagnosis of fibromyalgia is considered very reliable.
Advanced imaging, like an MRI or CT scan, is usually only needed if the doctor suspects a structural problem, such as a herniated disc or nerve compression, is causing your pain. If your symptoms are classic for fibromyalgia and your physical exam doesn’t show joint damage, advanced imaging is rarely required.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)