Urology treats urinary tract diseases in all genders and male reproductive issues, covering the kidneys, bladder, prostate, urethra, from infections to complex cancers.
Send us all your questions or requests, and our expert team will assist you.
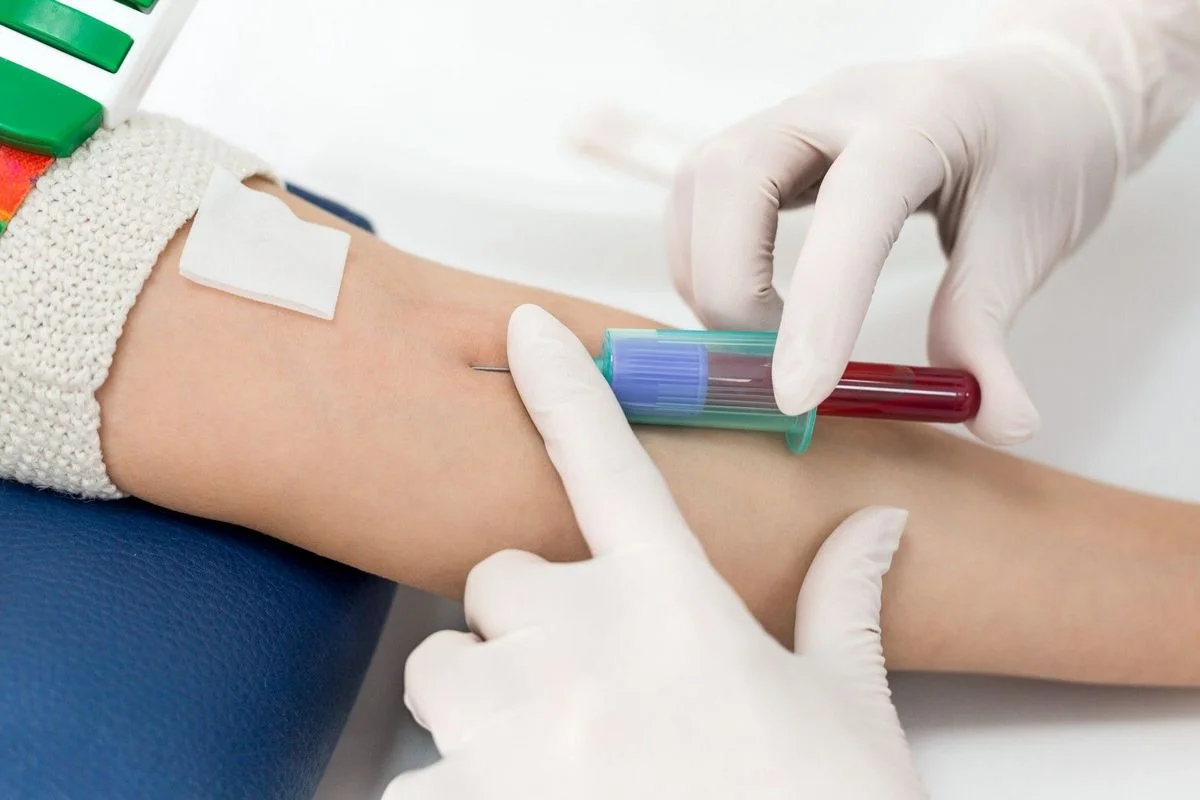
The diagnostic pathway in Interventional Nephrology relies on advanced imaging to visualize the vascular architecture and quantify hemodynamics. Doppler Ultrasound is the first-line modality. It provides a non-invasive, real-time assessment of vessel diameter, depth, and blood flow volume. It can detect stenosis by identifying areas of velocity acceleration and turbulence (aliasing). It also assesses the arterial inflow and can diagnose accessory veins that siphon flow away from the main channel.
Digital Subtraction Angiography (DSA) remains the gold standard for guiding interventions. This technique involves injecting contrast dye into the access while subtracting the background bone and soft tissue images digitally. This provides a high-definition roadmap of the vascular tree. Carbon Dioxide (CO2) angiography is a specialized technique used in patients with residual renal function or contrast allergy. CO2 is a negative contrast agent that is non-nephrotoxic and rapidly dissolved in blood, allowing for safe visualization without the risk of Contrast-Induced Nephropathy.
Intravascular Ultrasound (IVUS) brings the “eye” inside the vessel. A miniaturized ultrasound probe is advanced through the catheter to provide cross-sectional images of the vessel lumen and wall. IVUS is superior to angiography for determining the true vessel diameter and for characterizing the nature of the stenosis (e.g., fibrotic recoil vs. thrombus). It allows for precise sizing of balloons and stents, preventing undersizing (which leads to early failure) or oversizing (which causes rupture).
Optical Coherence Tomography (OCT) is an emerging modality that uses light waves instead of sound to create micron-scale images of the vessel wall. OCT can visualize the endothelial layer, macrophages, and thin neointimal tissue with unprecedented detail. This “optical biopsy” capability allows researchers and clinicians to study the healing response after angioplasty and to identify early signs of restenosis or stent malapposition at the cellular level.
Proactive surveillance is key to preventing thrombosis. Transonic flow monitoring (dilution technique) is performed during dialysis sessions to measure the access blood flow. A drop in flow of greater than 20-25% from baseline or a flow less than 600 mL/min triggers a referral for angiography. Static venous pressure monitoring measures the pressure required to return blood to the patient; high dynamic venous pressures indicate outflow stenosis.
Physical examination, often undervalued, is a potent diagnostic tool. The “arm elevation test” can identify outflow stenosis if the fistula fails to collapse when the arm is raised. Pulse augmentation tests help localize the site of narrowing. Teaching patients to perform self-examination (checking for the thrill, observing for swelling) is an integral part of the diagnostic strategy.
While imaging dominates, biochemical markers are gaining traction. Plasma levels of Matrix Metalloproteinases (MMPs) and their inhibitors (TIMPs) correlate with the rate of vascular remodeling. Elevated levels of asymmetric dimethylarginine (ADMA), an endogenous inhibitor of nitric oxide synthase, serve as a marker of endothelial dysfunction. Monitoring inflammatory markers like High-Sensitivity C-Reactive Protein (hsCRP) and Interleukin-6 can stratify patients based on their risk for access failure and cardiovascular events.
Genetic profiling is also being explored. Polymorphisms in the heme oxygenase-1 gene or the TGF-beta gene may predispose certain individuals to aggressive neointimal hyperplasia. This genomic insight could eventually lead to personalized surveillance protocols and targeted pharmacological therapies.
The diagnosis extends to the systemic impact of the access. A high-flow fistula can act as a significant cardiovascular burden, leading to high-output heart failure. Echocardiography is used to assess cardiac output, right ventricular function, and pulmonary pressures. The ratio of access flow to cardiac output (Qa/CO) is a critical metric; a ratio greater than 0.3 indicates a high risk of cardiac decompensation. Diagnosis in Interventional Nephrology therefore involves a holistic assessment of the “access-heart” axis.

Send us all your questions or requests, and our expert team will assist you.
CO2 angiography is an imaging technique that uses carbon dioxide gas instead of standard liquid contrast dye to visualize blood vessels. Because CO2 is a gas, it displaces blood to create an image and is then harmlessly breathed out by the lungs. It is safe for the kidneys (non-nephrotoxic) and causes no allergic reactions, making it ideal for patients with remaining kidney function or dye allergies.
An ultrasound, or “vessel mapping,” is performed to measure the size and depth of the arteries and veins in the arm. It ensures the vessels are large enough (usually at least 2mm for arteries and 2.5mm for veins) and healthy enough to support a fistula. This precise mapping helps the surgeon choose the best location for the access, increasing the chance of success.
An X-ray (angiogram) shows the silhouette of the blood flow inside the vessel (the lumen). IVUS (Intravascular Ultrasound) uses a tiny probe inside the vessel to show the vessel wall itself. It can reveal the thickness of the scar tissue, the true diameter of the vessel, and whether a stent is fully expanded against the wall. This detail helps ensuring the treatment is perfectly sized.
Steal Syndrome is diagnosed using a combination of physical exam and Digital Plethysmography. The doctor checks the pulse and blood pressure in the fingers. If the finger pressure improves when the fistula is temporarily compressed, it confirms that the fistula is “stealing” flow. Imaging helps visualize the arterial anatomy to plan the correction (e.g., banding or DRIL procedure).
Surveillance monitoring involves regular checks of the dialysis access to detect problems before they cause a blockage. This includes measuring the blood flow rate during dialysis (using ultrasound dilution), monitoring the pressure in the venous return line, and physical exams. If trends show decreasing flow or increasing pressure, an intervention can be scheduled to fix the narrowing before the access clots.

 Interventional Nephrology
Interventional Nephrology
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)