Urology treats urinary tract diseases in all genders and male reproductive issues, covering the kidneys, bladder, prostate, urethra, from infections to complex cancers.
Send us all your questions or requests, and our expert team will assist you.
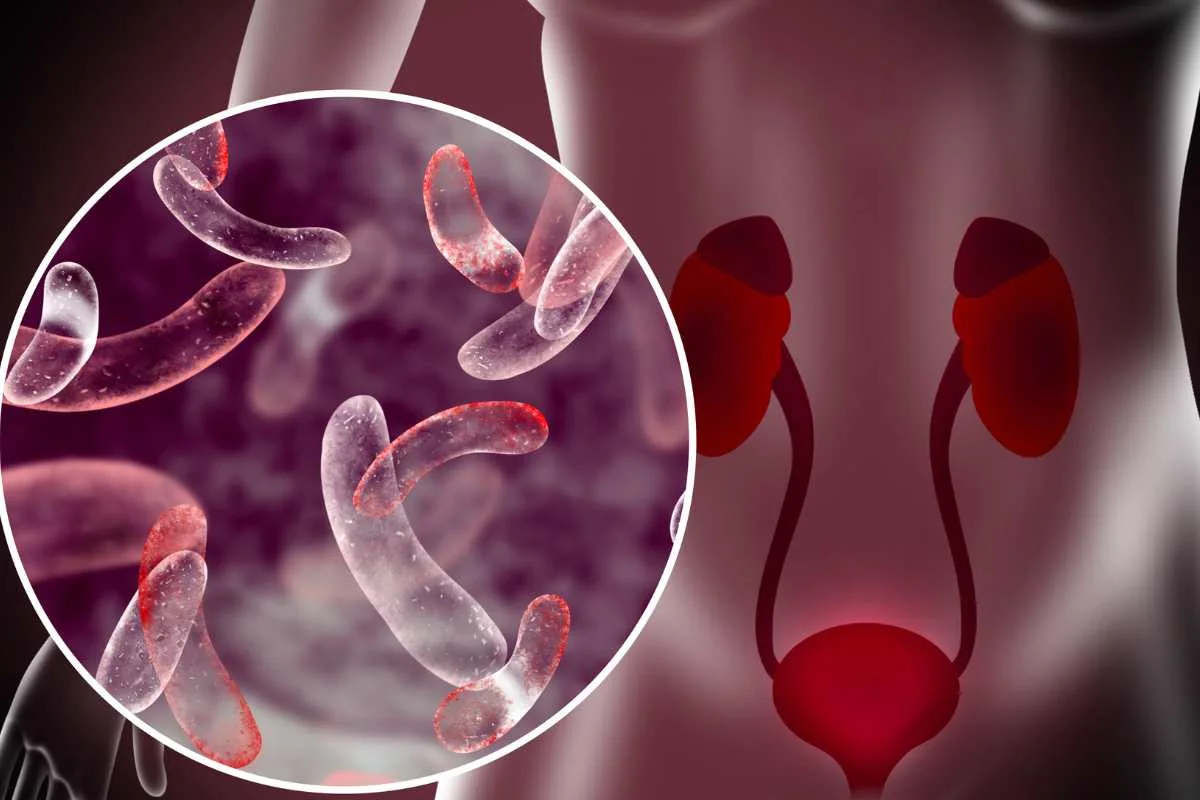
The urethra is the final part of the urinary tract, moving urine from the bladder out of the body. In men, it also carries semen during ejaculation. While it looks like a simple tube, the urethra is made of special tissues that need to stay open for urination but also help hold urine in when necessary.
To understand urethral diseases, it helps to know how male and female anatomy differ. The male urethra is much longer, about twenty centimeters, and passes through the prostate and penis, making it more prone to strictures or injuries. The female urethra is much shorter, about four centimeters, and sits in the front wall of the vagina. Its closeness to the anal canal means women are more likely to get urethral infections.
Urethral diseases include many conditions that affect how the urethra works or is built. These can be caused by inflammation, infection, narrowing (strictures), congenital disabilities, or injuries. When the urethra’s size, stretchiness, or lining is changed, it can make urination difficult and may even affect the bladder and kidneys.

Doctors group urethral problems by their cause. This helps them choose the right treatment, whether it is medicine or surgery.

A key idea in understanding urethral disease, especially strictures, is spongiofibrosis. The male urethra is surrounded by a soft, blood-rich tissue called the corpus spongiosum. When healthy, this tissue cushions and supports the urethra.
If the urethral lining is hurt by injury, infection, or medical tools, urine can leak into nearby tissue. Urine is harsh on tissues outside the urinary tract and causes irritation and swelling. The body tries to fix the damage, but often forms thick, messy scar tissue instead of healthy tissue.
This process changes the soft, blood-rich tissue into stiff scar tissue. The narrowed part of the urethra cannot stretch during urination. How serious the problem is depends on how deep and thick the scar is. Treatment often involves not just widening the urethra, but also removing or covering the scarred area.
The Regenerative Medicine Context: Urothelial Repair
With advances in medical science and regenerative research, the urethra is both a challenge and an opportunity. The best result after a urethral injury is for the lining and supporting tissue to regrow without scarring. The urethral lining can repair itself using stem cells that multiply to cover damaged areas.
However, if the injury is deep or happens many times, the body’s ability to heal is overtaken by scar formation. Current research is looking for ways to help the body regrow healthy tissue instead of scar tissue. Scientists are testing special materials and scaffolds to help bridge gaps in the urethra and encourage new growth.
Currently, doctors use regenerative medicine for the urethra mainly by using Buccal Mucosa Grafts (BMG). They take tissue from inside the patient’s cheek to rebuild the urethra. This tissue is a good choice because it stays moist, has no hair, and heals quickly due to its rich blood supply. In the future, doctors hope to use 3D printing with the patient’s own cells to create new urethral tissue, so they won’t need to take tissue from the mouth.

Urethral diseases are a global health problem and can greatly affect quality of life. In developing countries, untreated infections and injuries often cause severe narrowing of the urethra, sometimes leading to complete blockage and the need for permanent catheters. In developed countries, strictures are more often caused by medical procedures like catheter use or surgery.
Urethral disease affects more than just the ability to urinate. It can cause ongoing pain, repeated urinary tract infections, kidney problems from back-pressure, and sexual issues like trouble ejaculating or erectile dysfunction, especially when there is a lot of scarring. Good urethral health means more than just no blockage—it also means normal urination, healthy anatomy, and good sexual function.

Send us all your questions or requests, and our expert team will assist you.
Both conditions cause difficulty urinating, but the location and cause are different. An enlarged prostate (BPH) squeezes the urethra from the outside at the base of the bladder. A urethral stricture is a narrowing caused by scar tissue inside the urethra itself, which can occur anywhere along its length, not just at the prostate.
Urethritis is inflammation specifically of the urethra, whereas a urinary tract infection (UTI) can affect the bladder, ureters, or kidneys. While urethritis can be a symptom of a UTI, it is often a distinct condition caused by sexually transmitted infections or irritation, presenting primarily with discharge and burning at the tip of the penis or urethra.
Yes, although it is much rarer than in men due to the shorter length of the female urethra. Strictures in women can result from trauma during childbirth, previous vaginal surgeries, or chronic inflammation. They often present with voiding difficulty or recurrent infections that are mistaken for simple bladder issues.
A urethral diverticulum is a pocket or pouch that forms in the wall of the urethra. It acts like a trap for urine. Because the urine in the pouch doesn’t empty properly, it can become infected or form stones. It is most common in women and can cause pain during intercourse or dribbling of urine after voiding.
The lining of the cheek, or buccal mucosa, is ideal for urethral repair because it is rugged, hairless, and used to being wet. It has a rich blood supply and heals quickly. When placed in the urethra, it acts as a patch to widen the narrowed segment and integrates well with the urethral tissue, offering a long-term cure.

 Urethra Diseases
Urethra Diseases Urethra Diseases
Urethra Diseases Urethra Diseases
Urethra Diseases Urethra Diseases
Urethra Diseases
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)