
It’s important to know the signs of a blood clot in a varicose vein. This is because getting medical help quickly is key. We will talk about the common signs and symptoms of this condition.
Identify a blood clot in leg symptoms quickly. Learn vital life-saving tips to ensure a successful and safe recovery from pain.
Signs include sudden pain, swelling, redness, warmth, or tenderness in the affected vein. Experts say about 30% of people with Deep Vein Thrombosis (DVT) don’t show symptoms. But, common symptoms are swelling, pain, tenderness, and redness.
If you have varicose veins, knowing these warning signs is vital. We aim to help you understand the risks and symptoms of blood clots in varicose veins.
Key Takeaways
- Common signs of a blood clot in a varicose vein include pain, swelling, redness, and tenderness.
- Around 30% of individuals with DVT may not show symptoms.
- Recognizing these signs is key for early detection and treatment.
- Varicose veins increase the risk of developing a blood clot.
- Seeking timely medical attention can prevent serious complications.
Understanding Varicose Veins and Blood Clots

Varicose veins are more than just a cosmetic issue. They can also increase the risk of blood clots. To grasp the risks, we need to know what varicose veins are and how they can cause blood clots.
What are varicose veins?
Varicose veins happen when vein valves get weak or damaged. This leads to blood pooling and increased pressure. They are enlarged, twisted veins, usually in the legs. The blood pooling makes the veins look bigger and twisted.
How blood clots form in veins
Blood clots form when blood flow is disrupted. This can happen due to many reasons like not moving much, injury, or genetics. Blood clots in varicose veins can be very painful and may lead to serious problems if not treated.
The connection between varicose veins and clotting
Varicose veins and blood clots are linked because of abnormal blood flow and high pressure. The risk of clotting is higher in varicose veins because of the stagnant blood and inflammation.
“Varicose veins are not just a benign condition; they can lead to serious complications like superficial vein thrombosis. It’s important for patients to be aware of the risks and seek medical attention if they experience symptoms.”
|
Condition |
Risk of Blood Clot Formation |
Complication Rate |
|---|---|---|
|
Varicose Veins |
Moderate |
10% |
|
Deep Vein Thrombosis (DVT) |
High |
30% |
|
Superficial Vein Thrombosis (SVT) |
Moderate to High |
20% |
It’s key to understand varicose veins and their risk of causing blood clots. By knowing the risks and taking steps to prevent them, people can lower their chance of serious complications.
Recognizing Signs of a Blood Clot in Leg Varicose Veins
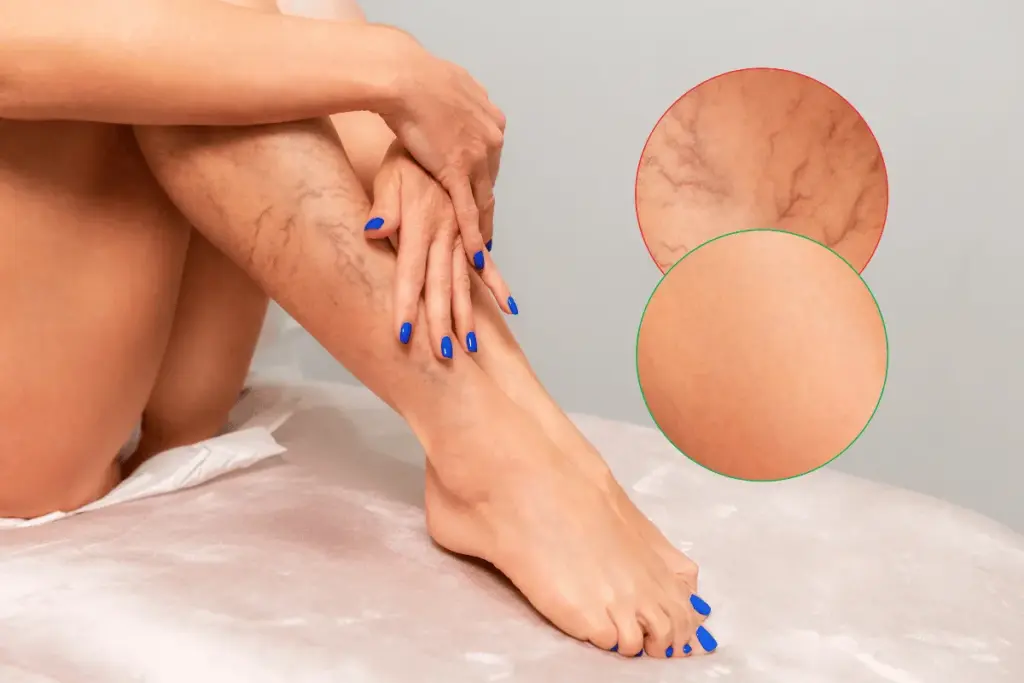
It’s important to know the signs of a blood clot in leg varicose veins. A blood clot in a varicose vein can cause a lot of pain and serious health issues if not treated quickly.
Sudden Localized Pain and Tenderness
Sudden localized pain and tenderness in the leg are key signs of a blood clot. The pain can feel like a dull ache or a sharp stab. It’s important to remember that this pain doesn’t go away on its own and can get worse.
Swelling and Inflammation
Swelling and inflammation are common signs of a blood clot in varicose veins. The area may swell up because of fluid buildup, and the skin might look inflamed. You might also feel like your leg is heavy or tight.
Skin Redness and Warmth
The skin over the vein might turn red and warm because of the clot. This is the body’s way of reacting to the clot. It’s a clear sign that you might have a thrombosis.
Hardening or Cord-like Feeling in the Vein
A blood clot can make the vein feel hard or like a cord under the skin. This happens because the clot causes inflammation in the vein wall. It makes the vein feel different to the touch.
Seeing these signs early is key to getting medical help fast. If you notice any of these symptoms, you should see a doctor right away. They can help figure out what’s wrong and how to treat it.
Superficial Vein Thrombosis (SVT) in Varicose Veins
Varicose veins are more than just a cosmetic problem. They can lead to serious issues like Superficial Vein Thrombosis (SVT). This happens when a clot forms in a superficial vein. We will dive into what causes it, its symptoms, and what it means for your health.
What is Superficial Vein Thrombosis?
Superficial Vein Thrombosis (SVT) is when a blood clot forms in a vein close to the skin’s surface. It often happens in varicose veins, which are swollen and twisted. This clot can cause pain, swelling, and redness in the affected area.
SVT is different from Deep Vein Thrombosis (DVT), which affects deeper veins. While SVT is usually less severe, it’s important to see a doctor to avoid further problems and to feel better.
Common Locations for SVT
SVT most often happens in the legs, in varicose veins. Veins near the surface and affected by varicosity are most at risk. This condition can be quite painful and may cause inflammation and other issues if not treated.
Typical Progression of Symptoms
The signs of SVT can vary but often include pain, swelling, and redness around the vein. The area might feel warm, and you might feel a hard, cord-like structure under the skin. Sometimes, symptoms are mild, but they can get worse if not treated.
It’s important to understand how SVT symptoms progress. If symptoms don’t go away or get worse, see a doctor right away.
Deep Vein Thrombosis vs. Superficial Clots
It’s important to know the difference between deep vein thrombosis (DVT) and superficial vein thrombosis (SVT). Both involve blood clots in veins, but they are different in location, symptoms, and risks. Knowing the difference helps in getting the right treatment.
Key differences between SVT and DVT
SVT happens in veins near the skin’s surface, often in varicose veins. DVT, on the other hand, occurs in deeper veins, usually in the legs. Here’s a table showing the main differences:
|
Characteristics |
SVT |
DVT |
|---|---|---|
|
Location |
Superficial veins |
Deep veins |
|
Symptoms |
Localized pain, redness, and swelling |
Pain, swelling, warmth, and redness in the affected limb |
|
Complications |
Generally less severe, but can extend to deep veins |
Can lead to pulmonary embolism, a potentially life-threatening condition |
How superficial clots can extend to deeper veins
A superficial vein thrombosis can sometimes move into the deep veins, leading to DVT. This happens when the clot in the superficial vein grows and meets a deeper vein. It’s vital to watch SVT closely to stop this from happening.
Warning signs of progression to DVT
If you have SVT, watch for signs that might mean it’s turning into DVT. Look for pain that gets worse, swelling that gets bigger, and warmth or redness spreading. If you notice these, get medical help right away.
We stress the need to tell SVT and DVT apart because of their different impacts on health. DVT is more serious and can cause a life-threatening condition called pulmonary embolism. By knowing the differences, doctors can give better care and lower the risk of bad outcomes.
Risk Factors for Developing Blood Clots in Leg Varicose Veins
Several factors can raise the risk of blood clots in varicose veins. These include age, lifestyle, and medical conditions. Knowing these risks helps people prevent them and get medical help when needed.
Age and Gender Considerations
Age is a big risk factor for blood clots in varicose veins. As we get older, our risk goes up because we move less and our bodies change. Women are more likely to get varicose veins and blood clots, mainly during pregnancy and menopause.
Immobility and Sedentary Lifestyle
Being inactive or sitting for long periods raises the risk of blood clots. Movement helps blood flow better. Without it, blood can pool in veins, making clots more likely.
A vascular specialist says, “Being stuck in one place for too long, like at a job or on a long trip, can lead to blood clots in varicose veins.”
Recent Surgery or Hospitalization
Having surgery or being in the hospital recently also increases the risk. Patients often move less, which can cause clots. Surgery can also hurt veins, making clots more likely.
Medical Conditions that Increase Risk
Some medical conditions raise the risk of blood clots in varicose veins. These include problems with blood clotting and diseases that harm veins. It’s important to manage these conditions to prevent clots.
Many factors can increase the chance of blood clots in leg varicose veins. By understanding these risks, people can lower their chances and get help if symptoms show up.
How Doctors Diagnose Blood Clots in Varicose Veins
Doctors use a mix of checks and scans to find blood clots in varicose veins. Finding these clots right is key to treating them well. We’ll look at how doctors spot blood clots in varicose veins.
Physical Examination Techniques
When someone shows signs of a blood clot in a varicose vein, we start with a detailed check. We look for swelling, redness, and warmth in the affected limb. We also feel for tenderness and a hard, cord-like vein, which might mean a clot is there. Feeling and looking are key parts of this first check.
Duplex Ultrasound Imaging
Duplex ultrasound is a big help in finding blood clots in varicose veins. It uses sound waves to see blood flow and find clots. This method lets us see how big the clot is and where it is, and how it affects blood flow. It’s great for spotting both surface and deep vein clots.
Additional Diagnostic Tests
Even with duplex ultrasound, sometimes more tests are needed. These might include blood tests to check for clotting problems or inflammation. Sometimes, we might need more scans like venography or MRI to be sure. These extra tests help us make a treatment plan that fits the patient.
In short, finding blood clots in varicose veins takes a few steps. We use physical checks, duplex ultrasound, and sometimes more tests. By using all these ways, we can find and treat blood clots in varicose veins well.
What to Tell Your Doctor When You Suspect a Blood Clot
Talking to your doctor is very important if you think you have a blood clot in a varicose vein. Giving them all the details you can is key. This helps them figure out what’s wrong and how to treat it.
Important Symptoms to Report
When you see your doctor, tell them about any symptoms you’re feeling. This includes pain, swelling, redness, or warmth in your leg. Also, mention if your varicose veins look different or if you feel anything strange.
Key symptoms to highlight:
- Pain or tenderness in the leg
- Swelling or inflammation
- Redness or warmth around the affected vein
- Hardening or a cord-like feeling in the vein
Medical History Details to Share
Your medical history is very important for your doctor to know. Tell them about your health, any blood clots or vein treatments you’ve had, and surgeries. Also, let them know about any medicines you’re taking, like blood thinners or hormones.
Important medical history details:
- Previous blood clots or deep vein thrombosis
- Family history of blood clotting disorders
- Recent surgeries or hospitalizations
- Current medications and supplements
Questions to Ask During Your Appointment
It’s good to come with questions to understand your condition better. Ask about the risks of your blood clot, the chance of it becoming worse, and how to manage symptoms at home.
Sample questions:
- What are the immediate risks associated with my condition?
- What treatment options are available for my specific case?
- Are there any lifestyle changes I should make to aid in recovery?
By sharing all the information and asking the right questions, you can get the best care for your condition.
When to Seek Emergency Medical Care
Certain symptoms need immediate action. Knowing these can prevent serious issues from blood clots in varicose veins. If you see any red flag symptoms, get emergency medical care right away.
Red Flag Symptoms Requiring Immediate Attention
Severe symptoms like sudden shortness of breath or severe chest pain need emergency care. Other critical signs include:
- Swelling, pain, or redness in one leg
- Sudden difficulty breathing
- Chest pain or pressure
- Coughing up blood
- Rapid heart rate
- Dizziness or fainting
Act quickly if you see these symptoms. They could mean a life-threatening condition.
Risk of Pulmonary Embolism
Blood clots in varicose veins can be dangerous. They might break loose and travel to the lungs, causing a pulmonary embolism (PE). A PE is very serious and needs immediate medical help.
|
Symptoms |
Description |
|---|---|
|
Sudden shortness of breath |
Feeling winded even when sitting or doing light activities |
|
Chest pain |
Pain or discomfort that gets worse with deep breathing or coughing |
|
Coughing up blood |
Coughing up blood or rust-colored mucus |
What Happens in the Emergency Room
When you go to the emergency room with blood clot or PE symptoms, the staff will quickly check you. They will:
- Do a physical exam
- Ask for your medical history
- Order tests like ultrasound, CT scan, or blood tests
- Give oxygen if you’re having trouble breathing
- Give anticoagulant medication to stop more clotting
Knowing what to expect can make you feel less anxious about emergency care.
Treatment Options for Blood Clots in Varicose Veins
Treating blood clots in varicose veins depends on the clot’s size and where it is. We will look at the different ways to treat them. This will help patients understand their choices and make good decisions about their health.
Conservative Management Approaches
For many, the first step is conservative management. This includes compression therapy to lessen swelling and improve blood flow. It also includes elevation of the affected limb to reduce pain and swelling. Regular checks are also important to see how the clot is doing and adjust treatment as needed.
Anticoagulant Medications
In some cases, anticoagulant medications are used to stop the clot from getting bigger. These drugs make the blood thinner, which helps prevent new clots. We will talk about the different types of these drugs, their side effects, and why it’s important to keep an eye on them while taking them.
Anti-inflammatory Treatments
Anti-inflammatory treatments are key in managing symptoms of blood clots in varicose veins. Nonsteroidal anti-inflammatory drugs (NSAIDs) are often used to lessen pain and swelling. We will explain the benefits and risks of these treatments, so patients know their options.
Surgical Interventions When Necessary
In severe cases or when other treatments don’t work, surgical interventions might be needed. This could include removing the clot or fixing the damaged vein. We will discuss the surgical options, their risks and benefits, and what to expect during recovery.
Knowing the treatment options for blood clots in varicose veins helps patients take charge of their health. By working with healthcare providers, individuals can create a treatment plan that meets their specific needs and aims for the best results.
Home Management of Superficial Blood Clots
Managing superficial blood clots at home involves rest, using compression therapy, and managing pain. These steps help patients deal with their condition and lower the chance of serious problems.
Elevation and Rest Recommendations
It’s important to elevate the affected limb to reduce swelling and improve blood flow. We suggest keeping the leg higher than the heart for 15-20 minutes, three to four times a day. Also, resting comfortably can help ease pain.
Compression Therapy Techniques
Compression therapy is key in managing superficial blood clots. Wearing compression stockings or bandages can boost circulation and lessen pain. Patients should wear these stockings during the day and follow the maker’s guidelines for use.
Safe Pain Management Strategies
Managing pain is vital for those with superficial blood clots. Over-the-counter pain meds like acetaminophen or ibuprofen can help with pain and swelling. But, always check with a healthcare provider before taking any medication to make sure it’s safe.
Activity Modifications During Recovery
Changing daily activities can make recovery easier. It’s best to avoid hard work like heavy lifting or bending. Gentle exercises, like walking, can help blood flow without straining the affected limb too much.
|
Activity |
Recommended Adjustment |
|---|---|
|
Walking |
Continue with gentle walks to promote circulation |
|
Heavy Lifting |
Avoid lifting heavy objects to reduce strain |
|
Standing or Sitting |
Take regular breaks to move and elevate the affected limb |
By using these home management tips, patients can manage superficial blood clots well and aid in their recovery.
Preventing Blood Clots in Varicose Veins
It’s important to prevent blood clots in varicose veins for good vascular health. We suggest a few steps: making lifestyle changes, wearing compression stockings, and managing vein disease.
Regular Exercise and Movement
Exercise is key to stop blood clots. It boosts blood flow, lowering clot risk. Try walking, cycling, or swimming. Also, avoid sitting or standing too long.
- Take breaks to move if your job is sedentary.
- Do leg exercises like toe raises or ankle rotations.
- Yoga or Pilates can also help circulation.
Compression Stockings Use
Compression stockings help prevent blood clots. They apply pressure to improve blood flow. Talk to a doctor to find the right fit for you.
Key benefits of compression stockings include:
- Improved circulation
- Reduced swelling
- More comfort when traveling or standing long
Hydration and Nutrition
Drinking enough water and eating well is key for vascular health. Water keeps blood thin and less likely to clot. Eat fruits, veggies, and whole grains for nutrients.
Some diet tips are:
- Eat more omega-3s from fish and nuts.
- Include vitamin C-rich foods like citrus and greens.
- Don’t eat too much salt to avoid water retention.
Managing Underlying Vein Disease
Managing varicose veins is key to avoid blood clots. This might mean lifestyle changes, medical treatments, or surgery. We help patients with a tailored plan.
Strategies for vein disease include:
- Regular visits to a vascular specialist
- Non-invasive treatments like sclerotherapy or laser therapy
- Lifestyle changes to lessen symptoms and stop disease from getting worse
By following these steps, you can lower your risk of blood clots in varicose veins. We aim to give our patients the best care for their vascular health.
Special Risk Considerations for Blood Clots
Some life situations can raise the risk of blood clots in varicose veins. It’s key to know these factors to protect yourself and get medical help when needed.
Pregnancy and Hormonal Factors
Pregnancy ups the risk of blood clots because of more blood, higher pressure, and hormone changes. The danger grows after giving birth. Women with varicose veins need to watch out closely during these times.
Hormone treatments, like birth control or hormone therapy, also raise blood clot risk. Talk to your doctor about the pros and cons.
Long-Distance Travel Precautions
Traveling far, like by plane or car, can up the risk of blood clots because you’re not moving much. Make sure to get up and stretch often on long trips.
Wearing compression socks and drinking plenty of water can help too. People with varicose veins should take these steps to avoid blood clots.
Occupational Risks and Mitigation
Jobs that make you stand, sit, or lift a lot can increase blood clot risk. Take breaks and do exercises to keep blood flowing.
Wearing compression socks and eating well, with regular exercise, can lower the risk. Employers can help by supporting wellness at work.
Statistics and Outcomes for Varicose Vein Blood Clots
Learning about varicose vein blood clots can help us understand the risks. Varicose veins affect millions worldwide. They are often seen as just a cosmetic issue, but can lead to serious problems like blood clots.
Prevalence of SVT in Varicose Vein Patients
Research shows up to 4% of varicose vein patients get Superficial Vein Thrombosis (SVT). SVT is when a blood clot forms in a vein near the skin. It’s less severe than DVT but can cause pain and lead to bigger problems if not treated.
Rate of Progression to DVT
SVT can turn into DVT, a more serious condition. Studies show SVT can move into deeper veins, causing DVT. The chance of this happening depends on the clot’s size and location, and the patient’s health.
Long-term Prognosis and Recurrence Rates
The future for those with a blood clot in a varicose vein varies. Some fully recover, while others face SVT again or chronic venous insufficiency. The outcome depends on the treatment’s success, the presence of other venous diseases, and following prevention steps. Knowing these stats helps doctors and patients make better choices.
Looking at the stats on varicose vein blood clots helps us grasp the risks and outcomes. This info aids in making treatment choices and improving patient care.
Differentiating Blood Clots from Other Vein Conditions
It’s important to know the differences between blood clots and other vein issues. Varicose veins can cause many symptoms, making it hard to tell what’s wrong. Getting the right diagnosis is key to treating the problem.
Varicose Vein Bleeding vs. Clotting
Bleeding and clotting in varicose veins are two different problems. Bleeding from varicose veins happens when the skin over the vein gets damaged. It shows as blood outside the body. Clotting, on the other hand, is when a blood clot forms inside the vein. This can cause pain, swelling, and redness.
“Knowing the difference between bleeding and clotting is very important,” says a vascular specialist. Quickly figuring out the problem helps in getting the right treatment and avoiding more issues.
Venous Insufficiency Symptoms
Venous insufficiency happens when veins can’t push blood back to the heart because of bad valves. It leads to swelling, pain, and skin changes in the affected limb. While it can raise the risk of blood clots, it’s a separate issue that needs its own treatment plan.
- Swelling in the legs or ankles
- Pain or aching in the legs
- Skin discoloration or ulcers
To diagnose venous insufficiency, doctors use a physical exam and tests like duplex ultrasound.
Cellulitis and Other Skin Infections
Cellulitis is a bacterial infection of the skin that can happen in people with varicose veins. It shows as redness, warmth, swelling, and pain. It’s important to tell it apart from blood clots or venous insufficiency to treat it right.
Dealing with vein problems needs a detailed approach for accurate diagnosis and treatment. By understanding the differences between blood clots, varicose vein bleeding, venous insufficiency, and cellulitis, we can give our patients the best care.
Conclusion
It’s important to know about blood clots in varicose veins to get help quickly. Spotting the signs and symptoms early can make a big difference. We’ve talked about the risks, how to find out if you have a blood clot, and how to treat it.
We aim to provide top-notch healthcare to everyone. We focus on helping international patients too. If you notice any symptoms, don’t wait. Get medical help right away. This can help prevent serious problems and improve your health.
FAQ
What are the common signs of a blood clot in a varicose vein?
Signs include sudden pain, swelling, redness, and a hardening or cord-like feeling in the vein.
How do I differentiate between a blood clot and other vein-related conditions?
Blood clots show pain, swelling, and redness. Varicose vein bleeding has visible bleeding or bruising. Venous insufficiency causes chronic swelling and discomfort.
What is superficial vein thrombosis, and how does it differ from deep vein thrombosis?
Superficial vein thrombosis is a blood clot in a superficial vein, often with varicose veins. It’s different from deep vein thrombosis, which is in deeper veins and more serious.
What are the risk factors for developing blood clots in varicose veins?
Risk factors include age, gender, immobility, recent surgery or hospitalization, and certain medical conditions.
How do doctors diagnose blood clots in varicose veins?
Doctors use physical exams, duplex ultrasound imaging, and sometimes more tests to diagnose.
What should I tell my doctor when suspecting a blood clot in a varicose vein?
Tell your doctor about your symptoms, medical history, and ask questions during your visit.
When should I seek emergency medical care for a suspected blood clot?
Get immediate help if you have severe pain, trouble breathing, or signs of pulmonary embolism.
What are the treatment options for blood clots in varicose veins?
Treatment includes conservative management, anticoagulant medications, anti-inflammatory treatments, and sometimes surgery.
How can I manage superficial blood clots at home?
Manage at home with elevation, rest, compression therapy, safe pain management, and modifying activities.
What preventive measures can reduce the risk of developing blood clots in varicose veins?
Preventive measures include regular exercise, compression stockings, staying hydrated and well-nourished, and managing vein disease.
Are there specific situations that increase the risk of blood clots?
Yes, pregnancy, long-distance travel, and certain jobs can increase the risk.
What is the prevalence of superficial vein thrombosis in patients with varicose veins?
The prevalence varies, but knowing the statistics helps patients and healthcare providers make informed decisions.
Can blood clots in varicose veins lead to complications like deep vein thrombosis?
Yes, superficial vein thrombosis can turn into deep vein thrombosis, so timely medical evaluation is important.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from























