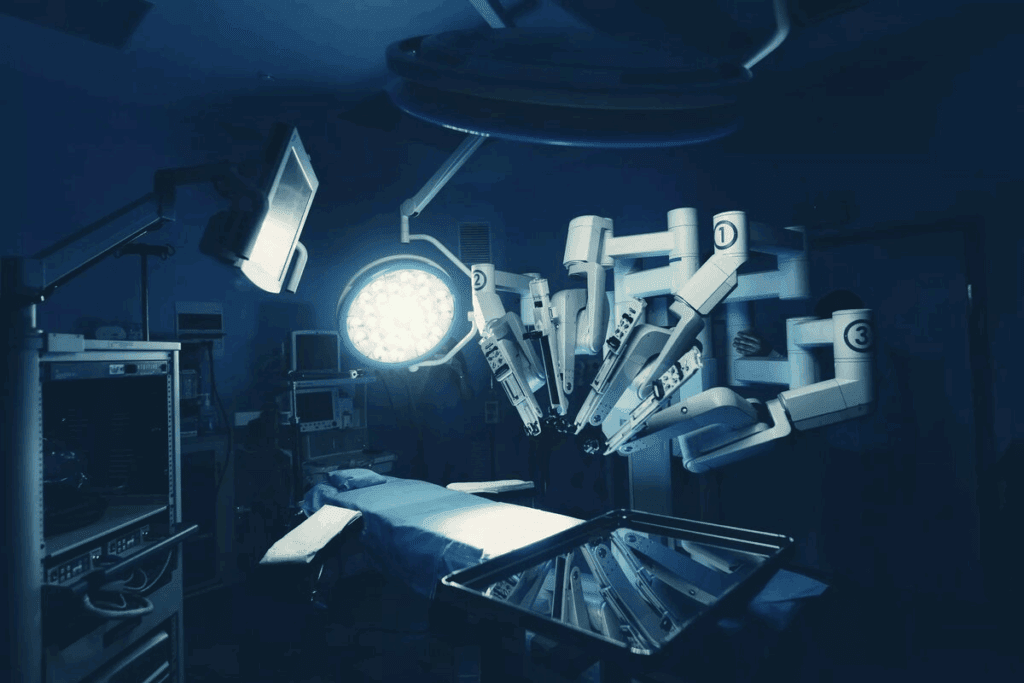
Every year, over 500,000 spine surgeries happen in the U.S. Many of these now use robotic technology. While robotic spine surgery improves precision and reduces recovery time, it’s important to be aware of the Disadvantages of Robotic Spine Surgery.
Robotic technology in spine surgery is a big leap forward in medical tech. It brings improved accuracy and minimally invasive procedures. As this area grows, knowing its advantages and disadvantages is key.
Key Takeaways
- Robotic spine surgery enhances precision and reduces recovery time.
- The technology offers improved accuracy and minimally invasive procedures.
- Understanding the advantages and disadvantages is important for judging its worth.
- Robotic spine surgery is a rapidly evolving field with growing importance.
- The article explores whether robotic spine surgery is better than traditional methods.
The Evolution of Spine Surgery Techniques
Spine surgery has changed a lot over time, thanks to new technology. Before, surgeries were big and hurt a lot, making recovery slow and risky.
From Traditional to Minimally Invasive Approaches
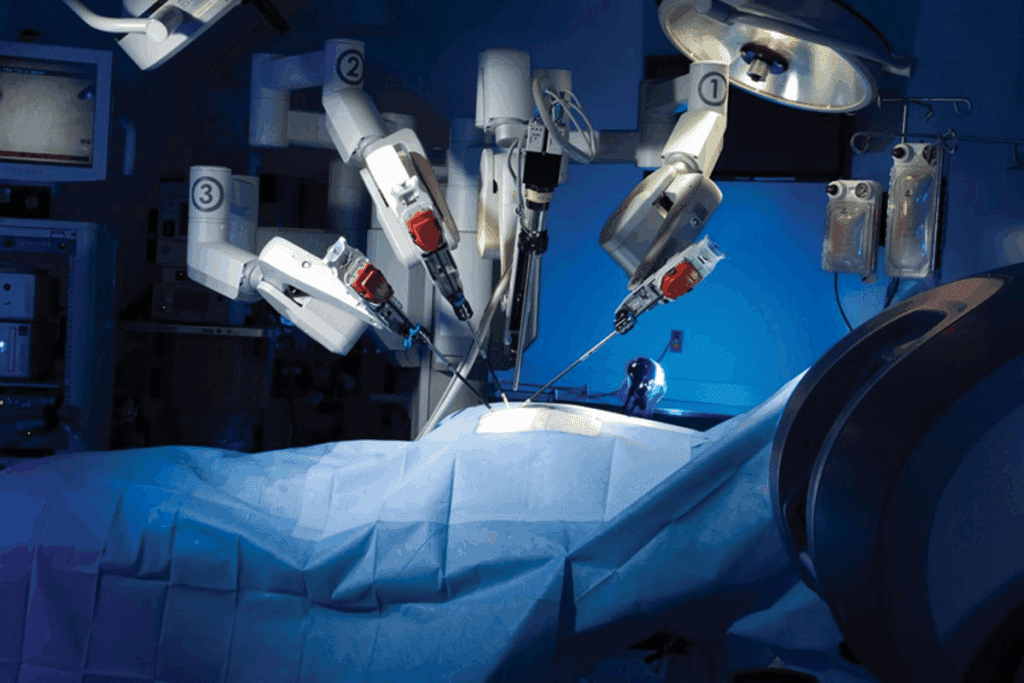
Minimally invasive spine surgery is a big step forward. It uses smaller cuts, less damage, and less blood loss. This means patients heal faster and do better.
“Minimally invasive spine surgery has revolutionized the field, making it safer and more effective than old methods.”
As Spine Surgeon
These new methods are popular because they hurt less and keep patients in the hospital less. But, they need special training and tools.
| Technique | Benefits | Limitations |
| Traditional Open Surgery | Wide exposure, direct visualization | Large incision, significant tissue damage, longer recovery |
| Minimally Invasive Surgery | Smaller incisions, less tissue damage, faster recovery | Specialized training required, limited visualization |
The Emergence of Robotic Assistance
Robotic assistance in spine surgery is a big leap. Robots help with precision, accuracy, and control.
Systems like the Mazor X Stealth Edition help surgeons do better. But, they’re not everywhere yet, and they’re expensive.
Robots help a lot, making surgeries safer and less likely to go wrong. As tech gets better, robots will play a bigger role in spine surgery.
Understanding Robotic Spine Surgery Technology

Spinal surgery has changed a lot with robotic technology. This new tech brings better precision and accuracy to surgeries.
How Robotic Systems Function in Spine Procedures
Robotic systems use advanced tech for better surgery accuracy. They have a robotic arm, a navigation system, and a control console. The arm holds surgical tools for precise movements.
The navigation system guides the arm with real-time images. This ensures implants are placed correctly.
Robotic tech in spine surgery also means better training for surgeons. Training requirements are key. They help surgeons use the tech well and handle technical malfunctions.
Major Robotic Platforms in Current Use
Many robotic systems are used in spine surgery today. The ROSA Spine System and the Mazor X Stealth Edition are among them. They aim to improve surgery results by being more precise and reducing damage.
Robotic systems in spine surgery are set to grow. As tech improves and more surgeons learn to use it, challenges will arise. These include the need for strong training requirements and ways to fix technical malfunctions.
Clinical Applications and Procedure Types
Advanced robotic technology is changing spinal surgery. It brings a new level of precision and success to many procedures.
Robotic spine surgery is used for different procedures. Each one has its own benefits and challenges. Robotic systems help surgeons do complex operations more accurately.
Spinal Fusion Procedures
Spinal fusion joins two or more vertebrae together. Robotic help in spinal fusion makes precision in screw placement better. It also lowers the risk of problems.
A study showed robotic-assisted spinal fusion has better fusion rates and fewer issues than traditional methods.
“The use of robotic navigation in spinal fusion procedures has significantly improved our accuracy rates and reduced revision surgeries.”
NASS (North American Spine Society)
Decompression Surgeries
Decompression surgeries relieve pressure on the spinal cord or nerves. Robotic systems help with minimally invasive approaches. This reduces tissue damage and speeds up recovery.
The precision of robotic technology is key in decompression surgeries. It’s where the difference between relief and injury is very small.
Complex Deformity Correction
Fixing complex spinal deformities needs careful planning and execution. Robotic systems offer the precision and flexibility needed for these tough cases.
Robotic-assisted surgery lets surgeons make adjustments during the procedure. This improves results in complex deformity correction.
| Procedure Type | Robotic Assistance Benefits | Clinical Outcomes |
| Spinal Fusion | Enhanced precision in screw placement | Higher fusion rates, fewer complications |
| Decompression Surgeries | Minimally invasive, reduced tissue damage | Faster recovery, less post-operative pain |
| Complex Deformity Correction | Precision, real-time adjustments | Improved outcomes, better correction |
Potential Benefits of Robotic-Assisted Spine Surgery
Robotic-assisted spine surgery is changing spinal care. It offers enhanced precision and reduced invasiveness. This technology could greatly improve patient outcomes and recovery times.
Enhanced Precision and Accuracy
Robotic-assisted spine surgery boosts precision and accuracy. It uses advanced imaging and navigation. This helps surgeons perform complex tasks with better accuracy.
Research shows it can lead to more accurate screw placement and fewer complications. For example, a study in the Journal of Neurosurgery: Spine found robotic-assisted pedicle screw placement was much more accurate than traditional methods.
| Study | Accuracy Rate – Robotic-Assisted | Accuracy Rate – Traditional |
| Journal of Neurosurgery: Spine | 95.5% | 85.2% |
| Spine Journal | 96.1% | 87.5% |
Reduced Invasiveness and Tissue Damage
Robotic-assisted spine surgery also means less invasiveness and tissue damage. The precision allows for smaller incisions. This could lead to less pain and faster recovery.
Potential for Improved Recovery Times
The precision and reduced invasiveness of robotic-assisted spine surgery may lead to improved recovery times. Patients might experience less trauma. This could mean shorter hospital stays and quicker return to normal activities.
But, robotic-assisted spine surgery also has challenges, like the lack of tactile feedback for surgeons. Despite this, its benefits make it a promising area in spinal care.
Disadvantages of Robotic Spine Surgery
Robotic spine surgery has its challenges and limits. It’s important for doctors and patients to know these. This knowledge helps in making informed decisions.
High Initial and Ongoing Costs
The cost of robotic spine surgery is high. Buying the equipment costs between $1 million and $2.5 million. This price depends on the system’s features.
Cost Breakdown
| Cost Component | Estimated Cost |
| Robotic System | $1,000,000 – $2,500,000 |
| Maintenance (Annual) | $50,000 – $100,000 |
| Training and Support | $20,000 – $50,000 |
Costs don’t stop after buying the equipment. There are yearly expenses for upkeep, updates, and training. These add to the financial load on hospitals.
Technical Limitations of Current Systems
Today’s robotic spine surgery systems have some technical issues. These can affect how well they work. Some of these problems include:
- Limited flexibility and range of motion
- Dependence on pre-operative imaging
- Potential for software glitches
- Limited ability to adapt to complex anatomies
These issues can make surgeries harder. They might also affect how well the surgery goes.
Patient Selection Restrictions
Not every patient can have robotic spine surgery. The criteria for who can have it are strict. This means some patients with complex spinal issues or past surgeries are not eligible.
Key factors influencing patient selection include:
- Spinal anatomy complexity
- Previous surgical history
- Specific condition being treated
These rules mean robotic spine surgery isn’t for everyone. It’s important to check if a patient is a good fit before surgery.
Limited Availability and Access Barriers
Robotic-assisted spinal procedures are not available everywhere. This is due to several reasons. The limited availability of robotic spine surgery is a big problem. It affects patients’ access to this advanced technology.
Geographic Distribution Challenges
The availability of robotic spine surgery systems is not even. Many centers, mainly in rural or underserved areas, don’t have access to this technology. Major metropolitan areas and specialized surgical centers are more likely to have these systems. This creates a big gap in healthcare access.
A study showed that nearly 70% of robotic spine surgeries were performed in urban centers. This leaves a big gap in access for rural populations.
Insurance Coverage and Financial Considerations
Insurance coverage and financial considerations also affect access to robotic spine surgery. Variability in insurance coverage for robotic-assisted procedures can lead to big out-of-pocket expenses for patients.
- Some insurance providers may not cover robotic spine surgery. They might say it’s an experimental or investigational procedure.
- Even when covered, the extent of coverage can vary a lot. This affects patients’ ability to afford the procedure.
The high costs of robotic systems are usually passed on to patients. This makes access even harder. As a result, financial counseling and assistance programs are becoming more important for patients considering robotic spine surgery.
In conclusion, solving the limited availability and access barriers to robotic spine surgery needs a multi-faceted approach. We need to improve geographic distribution and tackle insurance and financial challenges.
Training Requirements and Steep Learning Curve
The use of robotic technology in spine surgery has changed the game. It brings precision and complexity, needing special training for surgeons and staff. With more robotic systems in surgery, training programs are key.
Robotic spine surgery is complex, needing a deep tech and surgical skill understanding. Surgeons must learn the robotic system and how to use it in their practice. They need to know its strengths, weaknesses, and how to fix problems during surgery.
Surgeon Training Protocols and Certification
Surgeon training for robotic spine surgery mixes theory and practice. Programs include classes, simulation, and supervised surgeries to ensure skill. There are also certification programs for a standard of skill before using the system alone.
The training covers everything from basic robotic use to complex surgeries. Surgeons learn to handle different situations, including surgery complications.
Operating Room Team Preparation Needs
The operating room team is vital for robotic spine surgery success. Nurses, techs, and support staff need training on the robotic system. They must know their roles in setup, troubleshooting, and assisting during surgery. The team must work well together with the surgeon.
Team training includes learning about robotic surgery and the specific system used. It also includes simulation and hands-on practice for the demands of robotic-assisted procedures.
Technical Malfunctions and System Failures
Robotic spine surgery has made big strides, but it’s not perfect. Like all complex tech, it can face system failures. These failures can affect how well the surgery goes.
These malfunctions can show up in different ways, like software bugs or hardware breakdowns. It’s key for doctors and staff to know about these issues. This helps keep patients safe and ensures the best results.
Software Glitches During Procedures
Software bugs can pop up during robotic spine surgery for many reasons. This could be because of coding mistakes or problems with how different parts work together. These bugs can make the robotic system act strangely, which might cause problems during the surgery.
“The complexity of robotic systems demands rigorous testing and validation to minimize the risk of software glitches during surgery.”
Expert Opinion
To tackle software problems, makers and healthcare teams need to team up. They should create strong testing plans. Also, they must check software updates carefully before using them.
Hardware Failures and Their Consequences
When robotic spine surgery systems fail, it can lead to big problems. These can include delays or even having to stop the surgery. Issues often come from mechanical parts not working right or sensors not working as they should.
| Hardware Component | Potential Failure | Consequence |
| Robotic Arm | Mechanical failure | Procedure delay or cancellation |
| Sensors | Malfunction | Inaccurate readings, potentially leading to surgical complications |
| Control System | Failure to respond | Loss of control during procedure |
Keeping hardware in good shape is key. Regular checks and maintenance can help avoid failures during robotic spine surgery.
Contingency Planning for System Breakdowns
Having a plan for when things go wrong is vital. This means having backup systems ready and staff trained to handle emergencies.
Key elements of contingency planning include:
- Regular training for surgical staff on troubleshooting and emergency procedures
- Availability of backup hardware and software components
- Established communication protocols for reporting and addressing technical issues
With a solid plan, healthcare teams can deal with technical issues. This keeps robotic spine surgery successful.
Extended Setup Time and Operating Room Efficiency
Robotic spine surgery is changing how we do surgery. It affects how well the operating room works. The good and bad sides of this change are important to understand.
Pre-operative Planning Requirements
Getting ready for robotic spine surgery takes a lot of time. This time is spent on:
- Looking at patient images to plan the surgery
- Setting up the robotic system for the surgery
- Testing the system to make sure it works right
This careful planning is key to a successful surgery. But, it means the surgery takes longer.
Increased Operating Room Time Considerations
Robotic systems in spine surgery can make the surgery longer. This is because of:
- Setting up and calibrating the robotic equipment
- Doing precise checks to make sure everything is right
- Dealing with any technical problems during the surgery
These steps are important for making sure the surgery is safe and accurate. But, they can make the surgery take longer.
Hospitals and surgical teams are finding ways to make things better. They are working on:
- Making pre-operative planning faster
- Getting robotic systems to work better with the operating room
- Training staff to use the robotic systems well
By tackling these issues, healthcare providers can use robotic technology in spine surgery better. They can keep the operating room running smoothly.
Lack of Tactile Feedback for Surgeons
Surgeons doing robotic spine surgery face a big challenge. They can’t feel tactile sensations during the procedure.
This lack of touch can really change how they work. Surgeons usually use both what they see and feel to make decisions.
Impact on Surgical Decision-Making
The lack of touch affects how surgeons make decisions.
They have to rely more on what they see from the robotic system. This can make learning harder and might affect how precise their decisions are.
Switching from feeling and seeing to just seeing is tough. It’s even harder in complex surgeries where feeling is key for checking tissue and finding important details.
Compensatory Techniques and Technologies
To deal with the lack of touch, surgeons and engineers are finding new ways.
Robotic systems are getting advanced imaging technologies. These give more detailed visual feedback, helping without touch.
Surgeons are also learning to use what they see from the robotic system more. They use real-time imaging to help make their decisions.
Researchers are looking into adding haptic feedback technology to robotic surgery. This could bring back the sense of touch for surgeons in the future.
These new steps aim to make robotic spine surgery safer and more effective. This could help more patients get the care they need.
Potential for Conversion to Open Surgery
In some cases, surgeons might switch from robotic spine surgery to open surgery. This is due to complications or unexpected changes in the patient’s anatomy.
Robotic-assisted spine surgery has many benefits. It’s less invasive and can lead to quicker recovery times. Yet, the complexity of the spine and the variability in patient conditions pose challenges. Surgeons must be ready for any situation, including the need for open surgery.
Common Scenarios Requiring Conversion
Several scenarios might require a switch from robotic to open surgery:
- Unexpected Bleeding: Significant bleeding that can’t be managed with the robotic system.
- Anatomical Variations: Unexpected complexities in the anatomy that robotic surgery can’t handle.
- Equipment Malfunction: Failure of the robotic system during the surgery.
Patient Outcomes After Conversion
The effects of switching from robotic to open surgery on patient outcomes can vary:
- Recovery Time: Patients might need a longer recovery period than those who had successful robotic surgery.
- Complications: The risk of complications, such as infection or nerve damage, could be higher in open surgery.
- Surgical Success: Despite the conversion, the surgery can often successfully address the spinal issue.
It’s important for surgeons to talk to patients about the possibility of conversion before surgery. This way, patients understand the risks and possibilities of robotic spine surgery.
Complexity in Emergency Situations
Robotic spine surgery brings unique challenges in emergency cases. It offers precision and quicker recovery times but faces specific hurdles in urgent situations.
Emergency issues can pop up due to tech problems, patient reactions, or surgery complications. The need for quick tech fixes adds to the complexity.
Limitations During Urgent Procedures
Urgent robotic spine surgeries face tech issues as a major hurdle. For example, a system failure during surgery might force a switch to manual or open surgery.
The table below shows common tech problems and their effects:
| Technical Issue | Potential Consequence | Emergency Response |
| Robotic arm malfunction | Delay or complication in surgery | Switch to manual or open surgery |
| Software glitch | Disruption of surgical process | Restart system or use backup |
| Image guidance failure | Inaccurate surgical navigation | Use alternative imaging or manual technique |
Protocols for Emergency Management
Hospitals and surgical teams need strong emergency plans for robotic spine surgery. These plans should cover how to handle tech failures, patient issues, and other emergencies.
Key components of emergency management protocols include:
- Regular maintenance and checks of robotic gear to avoid failures
- Training for staff on open surgery or alternative methods
- Clear communication among the team for quick emergency responses
- Backup systems or alternative gear for critical parts
With these protocols, hospitals can better handle emergencies in robotic spine surgery. This ensures a safer and more effective response.
Radiation Exposure Concerns
Radiation exposure is a big worry in robotic spine surgery. It affects both patients and medical staff. Imaging tech like fluoroscopy is key for robotic surgery’s precision. But, it also means more radiation.
Patient Exposure During Robotic Procedures
Patients in robotic spine surgery face radiation risks, mainly from fluoroscopy. The amount of radiation depends on the surgery’s complexity, the robotic system, and safety protocols. It’s vital to reduce radiation while keeping images clear for surgery success and patient safety.
To cut down patient radiation, doctors and techs work on better imaging plans. They aim for the lowest radiation dose needed and limit image counts during surgery.
Staff Exposure and Protection Strategies
Staff, like surgeons and nurses, also face radiation risks in robotic spine surgeries. The robotic system doesn’t emit radiation, but imaging does. Good protection strategies are key to lower staff exposure.
Staff wear protective gear like lead aprons and glasses. They also stand behind lead barriers or in shielded spots when not needed. Training on radiation safety and using protective gear correctly is important.
Knowing the risks of radiation and using safety steps can make robotic spine surgery safer. This way, its benefits can be enjoyed while keeping risks low.
Comparing Outcomes: Robotic vs. Traditional Approaches
It’s important to compare robotic spine surgery with traditional methods to find the best treatment. Robotic technology in spine surgery has sparked debate about its benefits and effectiveness.
Short-term Clinical Results
Research on short-term results of robotic and traditional spine surgery shows mixed findings. Some studies suggest that robotic surgery can lead to less blood loss and tissue damage. This could mean faster recovery times. Yet, other studies found no significant difference in short-term results.
A review of studies found that robotic spine surgery is more accurate in screw placement. This is key for spinal fusion success. But, the real impact of this accuracy is debated.
Long-term Outcomes and Limited Data
Long-term results of robotic versus traditional spine surgery are not well-studied. There’s limited data on how well these results last and any long-term complications. Some research points to better long-term outcomes with robotic surgery due to precise implant placement and lower revision surgery risk.
But, the lack of long-term data makes it hard to say for sure which method is better over time.
Patient Satisfaction and Quality of Life Metrics
Patient satisfaction and quality of life are key to measuring spine surgery success. Both robotic and traditional surgery can lead to significant improvements in patient outcomes. This includes less pain and better function.
Studies on patient satisfaction show mixed results. Some suggest robotic surgery’s minimally invasive nature leads to higher satisfaction. This is due to less pain and quicker recovery.
Conclusion
Robotic spine surgery is a big step forward in spinal surgery. It brings better precision and less invasion. This tech could lead to better patient results and faster recovery times.
But, it also has its own set of problems. These include high costs, technical issues, and a learning curve for doctors.
The future of robotic spine surgery looks promising. We need to work on its current limits and make it more available. Research and development are key to improving this technology.
As the field grows, we’ll see better robotic systems and their use in spine surgery. This could greatly benefit patients.
To fully use robotic spine surgery, we must consider both its good and bad sides. We need to keep checking how it affects patient care. This way, we can make the most of this technology and help more people with spinal issues.
FAQ
What is robotic spine surgery and how does it differ from traditional spine surgery?
Robotic spine surgery is a new way to do spine surgery. It uses a robot to help the surgeon. This method is less invasive and more precise than old ways.
What are the benefits of robotic spine surgery?
Robotic spine surgery is better because it’s more precise. It also causes less damage and can help you recover faster. Plus, it offers real-time feedback and better views during surgery.
What are the limitations of robotic spine surgery?
There are downsides to robotic spine surgery. It’s expensive and not perfect yet. It’s also not for everyone and needs special training.
How does robotic spine surgery technology work?
This technology uses a robot and special systems to guide the surgeon. It helps make the surgery more precise and accurate.
What kind of training is required for surgeons to perform robotic spine surgery?
Surgeons need special training to use the robot. They learn how to use it and get hands-on practice.
What are the possible risks and complications of robotic spine surgery?
There are risks like technical problems and exposure to radiation. There are also challenges with patient positioning and the chance of needing open surgery.
How does robotic spine surgery compare to traditional spine surgery in terms of outcomes?
Early studies show robotic surgery might have better short-term results. But, we need more research to know for sure.
Is robotic spine surgery available everywhere?
No, it’s not available everywhere. There are issues with where it’s offered and who can afford it.
Can robotic spine surgery be used for complex deformity correction?
Yes, it can be used for complex cases. The robot’s precision is helpful for these tough surgeries.
What measures are taken to minimize radiation exposure during robotic spine surgery?
To reduce radiation, low-dose imaging is used. Fewer images are taken, and patients and staff are protected.
Reference:
Clinical efficacy of robotic spine surgery
PMC, 2023: https://pmc.ncbi.nlm.nih.gov/articles/PMC10646522/



































