Colorectal surgery is a big deal and needs careful thought about anesthesia. Did you know over 1.8 million people worldwide get colorectal surgery each year? Get abdominal surgery with the best amazing care. Learn incredible proven secrets for a successful and safe anesthetic experience today.
The thought of undergoing colorectal surgery and being put to sleep can evoke anxiety for many patients. We get it. Surgery worries are normal, and questions about anesthesia are common.
We’ll walk you through what happens during colorectal surgery. We’ll talk about the different anesthetics and how they’re given. Our aim is to make you understand the process better, easing your worries.
Key Takeaways
- Colorectal surgery often requires general anesthesia or regional anesthesia.
- The type of anesthesia used depends on the specific procedure and patient health.
- Anesthesia is administered by a trained anesthesiologist.
- Patients are closely monitored during and after the procedure.
- Post-operative care includes managing pain and discomfort.
Understanding Colorectal Surgery Basics
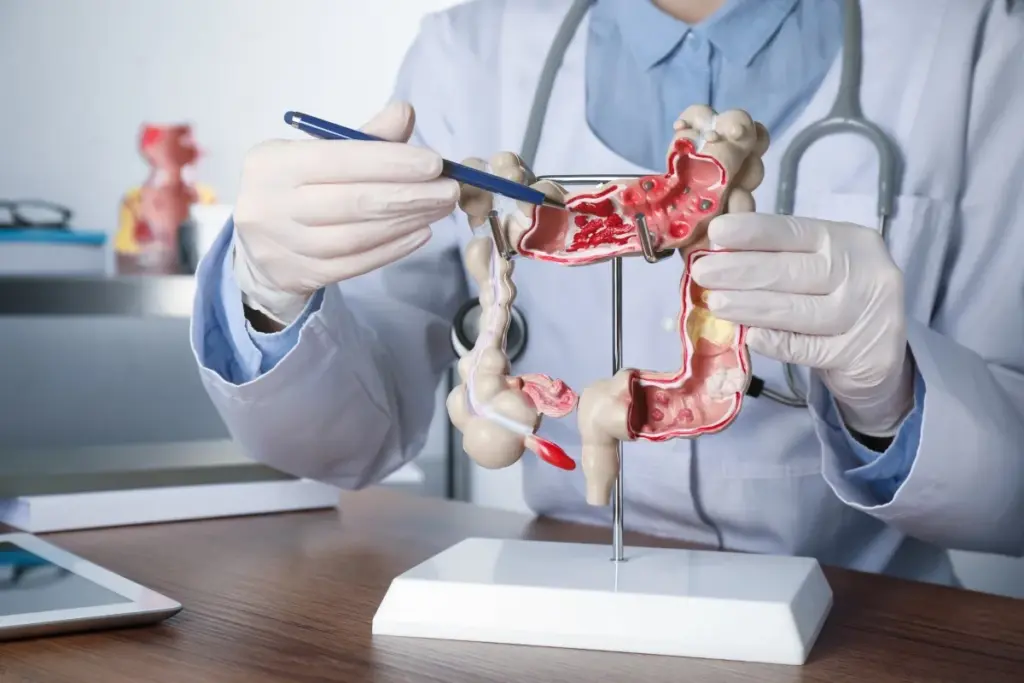
It’s important for patients to know about colorectal surgery basics. This surgery deals with the colon and rectum, parts of the large intestine. Each procedure is unique, depending on the condition being treated.
Common Types of Colorectal Procedures
There are several common types of colorectal surgeries. These include:
- Colectomy: Removal of part or all of the colon.
- Proctectomy: Removal of part or all of the rectum.
- Proctocolectomy: Removal of both the colon and rectum.
- Pouch surgery: Creation of an internal pouch to store waste after removal of the colon and rectum.
These surgeries can be done in different ways. They can be open surgery or minimally invasive surgery.
|
Procedure |
Description |
Typical Indications |
|---|---|---|
|
Colectomy |
Removal of part or all of the colon |
Cancer, polyps, diverticulitis |
|
Proctectomy |
Removal of part or all of the rectum |
Rectal cancer, severe rectal disease |
|
Proctocolectomy |
Removal of both the colon and rectum |
Familial adenomatous polyposis, ulcerative colitis |
Why Colorectal Surgery Is Performed
Colorectal surgery treats many conditions. These include:
- Cancer of the colon or rectum
- Diverticulitis
- Inflammatory bowel disease (IBD)
- Polyps
- Severe constipation or fecal incontinence
As one expert says, “Surgery is often a critical part of treatment. It can cure or greatly improve symptoms.”
The Surgical Team Involved
A colorectal surgical team has many healthcare professionals. These include:
- Colorectal Surgeon: The main surgeon for the operation.
- Anesthesiologist: Gives the anesthesia.
- Nurses and Surgical Technicians: Help during surgery.
- Pathologist: Examines tissue samples.
This team works together to ensure the best results for patients with abdominal issues.
Types of Anesthesia Used in Colorectal Surgery
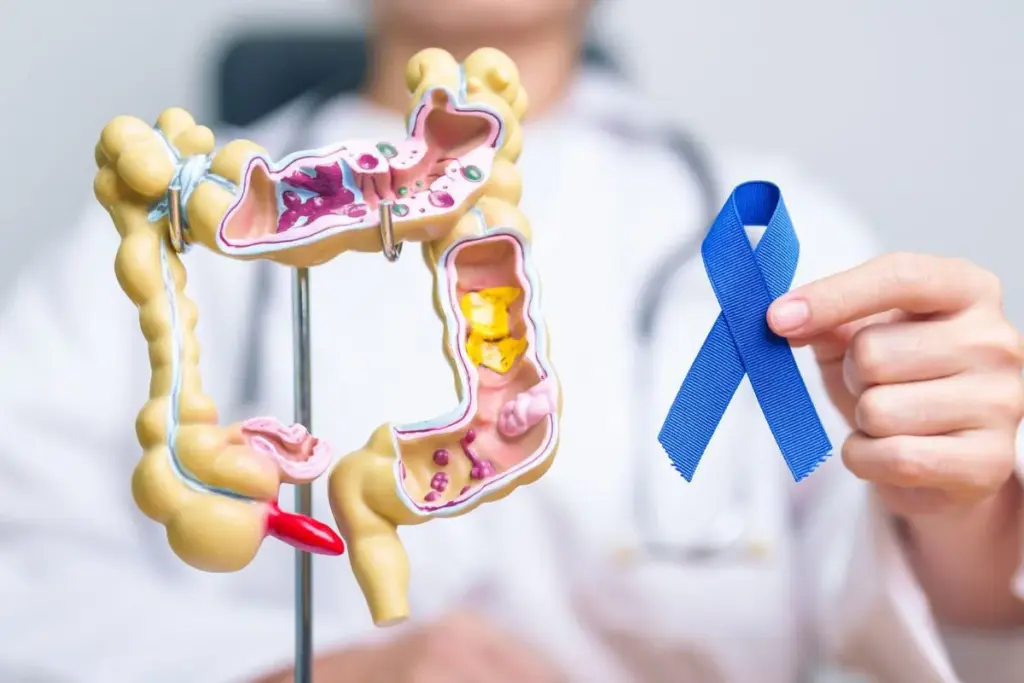
When you have colorectal surgery, the anesthesia matters a lot. Knowing about your options helps you make better choices for your care.
General Anesthesia
General anesthesia is often used for colorectal surgery. It makes you completely asleep and pain-free during the surgery. This anesthesia mix is perfect for complex surgeries. The anesthesiologist keeps an eye on your vital signs to keep you safe.
Regional Anesthesia
Regional anesthesia numbs the abdominal area. This can be epidural or spinal anesthesia. It helps with less pain after surgery and quicker recovery.
Local Anesthesia
Local anesthesia numbs a small area. It’s not as common for big surgeries but works for small ones. It lets you stay awake and recover fast.
Conscious Sedation
Conscious sedation makes you relax and feel calm during procedures. It’s often paired with local anesthesia. You’re not asleep but can respond to commands.
The right anesthesia depends on the surgery, your health, and what you prefer. Our anesthesiologists team up with the surgeons to pick the best anesthesia for you.
- General Anesthesia: Best for complex surgeries, keeps you asleep and pain-free.
- Regional Anesthesia: Numbs the belly, cuts down on pain and speeds up recovery.
- Local Anesthesia: Good for small procedures or with other anesthesia, for quick recovery.
- Conscious Sedation: Makes you relax during procedures, often with local anesthesia.
Is General Anesthesia Always Used for Colorectal Surgery?
The choice of anesthesia for colorectal surgery depends on many factors. These include the type of procedure, the patient’s health, and the professional judgment of the surgeon or anesthesiologist. Knowing about anesthesia options can help ease concerns about surgery.
Factors That Determine Anesthesia Choice
Several key factors influence the decision on the type of anesthesia for colorectal surgery. These include:
- The complexity and duration of the surgical procedure
- The patient’s medical history, including any previous adverse reactions to anesthesia
- The patient’s current health status, including conditions such as heart disease or diabetes
- The patient’s age and overall physical condition
- The preferences of the patient and the surgical team
When Alternative Anesthesia Methods Might Be Used
While general anesthesia is common for colorectal surgery, other methods might be used in some cases. For example, regional anesthesia could be an option for less invasive procedures or for those at high risk for general anesthesia complications. We carefully evaluate each patient’s situation to determine the most appropriate anesthesia plan.
Patient-Specific Considerations
Patient-specific factors are key in choosing the right anesthesia. For instance, patients with certain medical conditions may need special considerations to minimize risks of abdominal surgery and abdominal surgery complications. Our team works closely with patients to understand their unique needs and preferences. We ensure the chosen anesthesia method aligns with their overall care plan.
The Process of Being “Put to Sleep” for Colorectal Surgery
Being “put to sleep” for colorectal surgery involves several steps. It starts with a thorough pre-anesthesia evaluation. This step is key for patient safety and the best anesthesia care.
Pre-Anesthesia Evaluation
Our anesthesiologists do a detailed pre-anesthesia evaluation before surgery. They look at the patient’s medical history, current meds, and past anesthesia experiences. A physical exam is also done to spot any risks or complications.
We talk about the patient’s concerns and what they want for anesthesia. For surgeries like laparoscopic abdominal surgery, we consider the patient’s health, surgery complexity, and special needs.
Administration of Anesthesia
After the pre-anesthesia check, anesthesia starts. We use a mix of intravenous and inhaled drugs. The choice depends on the patient’s needs and the surgery type.
In the operating room, we watch the patient’s vital signs closely. We adjust the anesthesia to keep them stable and pain-free. For laparoscopic surgeries, we focus on their breathing and heart health, as these surgeries can affect pressure inside the abdomen.
Monitoring During Surgery
Our team keeps a close eye on the patient’s vital signs during surgery. We track heart rate, blood pressure, and oxygen levels. Advanced tools help us see how deep the anesthesia is and keep the patient comfortable.
We also watch for surgery-specific factors, like the patient’s position and any complications. Our aim is to provide safe and effective anesthesia. This supports the surgical team and helps the patient recover well.
By managing anesthesia well, we reduce risks. This ensures a smooth recovery for patients, even with laparoscopic or minimally invasive surgeries.
Can You Be Awake During Colorectal Surgery?
Now, thanks to new medical tech and anesthesia, you can be awake during colorectal surgery. This change brings new choices for those having colorectal procedures.
Awake Surgery Options
Thanks to regional anesthesia, you can stay awake during colorectal surgery. This method numbs the area where surgery happens. So, you can stay alert and awake.
There are different ways to get regional anesthesia, like epidural and spinal. These methods are safe and work well for many surgeries, including colorectal ones.
Patient Experiences with Regional Anesthesia
Many patients like being awake during surgery with regional anesthesia. They say it’s better than general anesthesia because it’s safer.
“I was nervous about being awake during my surgery, but the regional anesthesia made it a very comfortable experience. I was able to relax and even watch the procedure on the monitor if I wanted to.” -A patient who underwent colorectal surgery
Benefits and Limitations of Being Awake
Being awake during surgery has many good points. It lowers the risk of anesthesia problems, helps you recover faster, and lets you get back to normal sooner.
|
Benefits |
Limitations |
|---|---|
|
Reduced risk of complications |
Potential discomfort during surgery |
|
Faster recovery times |
Limited suitability for complex procedures |
|
Ability to resume normal activities sooner |
Requires skilled abdominal surgery specialists |
But, it’s not right for everyone or every surgery. Doctors decide based on your health, the surgery’s complexity, and their team’s skills.
As abdominal surgery specialists get better, you’ll have more choices. This includes being awake during colorectal surgery.
Preparing for Anesthesia Before Colorectal Surgery
Before your colorectal surgery, it’s key to get ready for anesthesia. This ensures your safety and comfort during the procedure. Preparing for anesthesia involves several steps to help your medical team provide the best care.
Fasting Requirements
One important step is to follow the fasting rules set by your healthcare provider. Usually, patients must fast for a certain time before surgery. This is to lower the risk of aspiration during anesthesia.
Fasting Guidelines:
|
Food/Drink |
Fasting Period |
|---|---|
|
Clear Liquids |
2 hours |
|
Light Meal |
6 hours |
|
Heavy Meal |
8 hours |
Medication Adjustments
Tell your healthcare provider about all medications you’re taking. Some might need to be adjusted or stopped before surgery. This is to avoid any complications with anesthesia.
“It’s essential to follow your doctor’s instructions regarding medication adjustments before surgery to ensure your safety during anesthesia.”
What to Expect During Pre-Op
During the pre-operative evaluation, your anesthesiologist will check your health and review your medical history. They will also discuss your anesthesia options. This is a chance for you to ask questions and share any concerns.
Mental Preparation for Anesthesia
Mental preparation is as important as physical preparation. Knowing about the anesthesia process and staying positive can make a big difference. Techniques like deep breathing, meditation, or having a supportive friend can help reduce anxiety.
By following these guidelines and working with your healthcare team, you can have a smooth and successful surgery.
The Role of the Anesthesiologist in Colorectal Surgery
The anesthesiologist is key in colorectal surgery, making sure patients are safe and comfortable. They are part of the surgical team. Their job is to give anesthesia and manage pain before, during, and after surgery.
Qualifications and Expertise
Anesthesiologists have a lot of training in anesthesia and pain management. They go to medical school for four years and then do four years of residency in anesthesiology.
They know how anesthesia, surgery, and the patient’s health work together. This helps them make good decisions during surgery.
Responsibilities During Surgery
During surgery, the anesthesiologist’s main job is to give and watch anesthesia. They keep an eye on the patient’s vital signs like heart rate and blood pressure. They adjust the anesthesia as needed.
They also handle any problems that come up during surgery. This could be bleeding or changes in blood pressure. They work with the surgical team to get the best results.
Communication with the Surgical Team
Good communication is very important for colorectal surgery. The anesthesiologist works with the surgeon and others to give the patient the best care.
They talk about the patient’s health, the surgery plan, and any risks. They also work together to care for the patient during and after surgery.
Abdominal Surgery and Anesthesia Considerations
Abdominal surgery is complex and requires careful planning in anesthesia. These surgeries range from simple to very complex, involving many organs.
Special Considerations for Abdominal Procedures
Several factors are key for effective anesthesia in abdominal surgery. These include:
- The type and extent of the surgical procedure
- The patient’s overall health and any comorbid conditions
- The possibility of significant blood loss or fluid shifts
- The need for adequate muscle relaxation
Positioning and Ventilation Challenges
Proper patient positioning is vital in abdominal surgery. It helps ensure good surgical access and reduces the risk of nerve injury. Managing ventilation is also tricky due to diaphragmatic splinting and anesthesia’s effects on breathing.
Key strategies for these challenges include:
- Careful patient positioning to optimize surgical exposure
- Using advanced ventilation techniques to keep oxygen levels up
- Monitoring the patient’s breathing closely during the surgery
Managing Intra-Abdominal Pressure
Intra-abdominal pressure (IAP) affects both the surgery and the patient’s health. High IAP can decrease blood flow, lower heart output, and harm kidney function.
To manage IAP well, anesthesiologists and surgeons work together to:
- Keep a close eye on IAP during the surgery
- Adjust surgical methods to lower pressure
- Use strategies to lessen the effects of high IAP
Understanding these special considerations helps healthcare providers improve outcomes for patients having abdominal surgery.
Minimally Invasive Colorectal Surgery and Anesthesia Options
Colorectal surgery has changed a lot with new, less invasive methods. These include laparoscopic and robotic-assisted surgeries. They offer patients better options than the old open surgery.
Laparoscopic Procedures
Laparoscopic surgery uses small cuts for tools and a camera. It’s less invasive than open surgery, causing less damage and pain.
Studies show laparoscopic surgery leads to quicker healing, less pain, and smaller scars. It needs special anesthesia because of the gas used and how the patient is positioned.
Robotic-Assisted Surgery
Robotic-assisted surgery is a step up from laparoscopic. It uses a robotic system for better control and view. This helps in complex surgeries.
The robotic system makes precise work easier. Anesthesia must consider the patient’s position and how the gas and position might affect blood pressure.
Anesthesia Adaptations for Minimally Invasive Approaches
Anesthesia for these surgeries needs special care. It must handle the gas used and the patient’s position. It also needs to keep the patient comfortable and pain-free.
- Managing pneumoperitoneum and its effects on respiratory and cardiovascular systems
- Addressing patient positioning challenges, such as steep Trendelenburg position
- Ensuring adequate pain control and comfort during the procedure
Recovery Differences from Traditional Surgery
Recovery from minimally invasive surgery is different from open surgery. Key differences include:
|
Recovery Aspect |
Minimally Invasive Surgery |
Traditional Open Surgery |
|---|---|---|
|
Hospital Stay |
Typically shorter (1-3 days) |
Often longer (5-7 days or more) |
|
Postoperative Pain |
Generally less due to smaller incisions |
More significant due to larger incision |
|
Return to Normal Activities |
Faster recovery (within a few weeks) |
Slower recovery ( potentially several months) |
Patients with minimally invasive surgery recover faster and have fewer problems. Knowing these differences helps in caring for patients better.
Waking Up After Colorectal Surgery
Patients start a new chapter in their recovery after colorectal surgery. The first hours after surgery are key for a safe recovery. We’ll guide you through what to expect when you wake up.
The Recovery Room Experience
Patients go to the recovery room after surgery. Here, our medical team watches over them closely. They check vital signs, manage pain, and look for any issues.
Patients might feel confused or forgetful because of the anesthesia. It’s normal to feel a bit mixed up right after surgery. Our staff is ready to help and support you during this time.
Managing Post-Anesthesia Side Effects
Patients may feel sick, shiver, or have other side effects after waking up. Our team knows how to handle these issues with the right medicine and care. We also give tips to help you feel better and recover faster.
Some common side effects include:
- Sore throat
- Dizziness
- Nausea
- Headache
These side effects usually go away within a few hours or days after surgery.
Timeline for Full Anesthesia Recovery
The time it takes to fully recover from anesthesia varies. It usually takes a few hours after surgery for the anesthesia to wear off. But, it can take days for your body to fully get back to normal.
We recommend resting at home for a few days after leaving the hospital. Following our post-operative instructions is key for a smooth recovery.
Potential Risks and Complications of Anesthesia
Anesthesia is usually safe, but it can have risks and complications in colorectal surgery. Knowing these can help patients prepare better for their surgery.
Common Side Effects
Most people have some side effects from anesthesia, but they are usually mild and short-lived. Common side effects include:
- Nausea and vomiting
- Dizziness or feeling groggy
- Sore throat
- Shivering
- Itching
These side effects usually go away within a few hours to a few days after surgery.
Rare but Serious Complications
Though rare, serious complications can happen. These may include:
- Anaphylaxis: A severe allergic reaction that needs immediate treatment.
- Malignant hyperthermia: A rare but dangerous condition caused by certain anesthetics.
- Respiratory or cardiac problems: These can happen in patients with existing conditions.
- Nerve damage: This can be temporary or, rarely, permanent.
Risk Factors for Anesthesia Complications
Some factors can make complications from anesthesia more likely. These include:
|
Risk Factor |
Description |
|---|---|
|
Age |
Older adults may have a higher risk due to decreased physiological reserve. |
|
Chronic Health Conditions |
Conditions like heart disease, diabetes, or lung disease can increase risk. |
|
Obesity |
Obesity can complicate anesthesia administration and recovery. |
|
Previous Adverse Reactions |
A history of adverse reactions to anesthesia can increase risk. |
How Complications Are Managed
Our anesthesiologists are trained to handle complications quickly and effectively. They do this by:
- Continuously monitoring during surgery
- Having emergency medications and equipment ready
- Working closely with the surgical team
- Keeping patients and their families informed
By understanding the risks and complications of anesthesia, patients can prepare better for their surgery and recovery.
Pain Management After Colorectal Surgery
Managing pain well after colorectal surgery is key for a smooth recovery. It helps patients heal faster, lowers the chance of problems, and boosts their overall health.
Immediate Post-Operative Pain Control
Right after surgery, doctors use IV meds or epidural anesthesia to control pain. These methods work well in the first few days of recovery.
IV drugs, like opioids, are often used because they can be adjusted as needed. Epidural anesthesia, which puts medication near the spinal cord, offers great pain relief without the side effects of IV opioids.
Transitioning to Oral Pain Medications
When patients can eat and drink again, they switch from IV or epidural to oral meds. Oral opioids are a common choice for managing pain after surgery.
It’s important to follow the doctor’s advice on taking these meds. They can cause side effects like constipation and addiction.
Non-Pharmaceutical Pain Management Techniques
There are also non-medical ways to manage pain after surgery. These include:
- Breathing exercises and relaxation techniques
- Physical therapy and gentle movement
- Heat or cold therapy
- Transcutaneous electrical nerve stimulation (TENS)
These methods can help with pain relief and reduce the need for opioids.
Expected Duration of Pain
Pain after surgery can last differently for everyone. Pain is usually worst in the first few days and gets better over weeks.
|
Time Frame |
Expected Pain Level |
Recommended Pain Management |
|---|---|---|
|
0-3 days post-op |
Severe |
IV or epidural pain management |
|
3-7 days post-op |
Moderate |
Oral opioids and non-pharmaceutical techniques |
|
1-2 weeks post-op |
Mild to moderate |
Oral pain medications and continued non-pharmaceutical techniques |
|
2-4 weeks post-op |
Mild |
Gradual tapering of pain medications |
Knowing the options for pain management after surgery helps patients prepare for recovery. They can work with their healthcare team to create a good pain management plan.
Special Considerations for High-Risk Patients
High-risk patients face unique challenges during colorectal surgery. They often have health conditions that make surgery and recovery harder. As specialists, we must carefully manage these risks for the best outcomes.
Elderly Patients
Elderly patients have extra challenges due to age and health issues. We consider their decreased strength, possible brain changes, and chronic conditions when planning their care.
For example, elderly patients might need special anesthesia and close monitoring during and after surgery. Our team works with patients and their families to create care plans that meet their unique needs.
Patients with Chronic Conditions
Patients with chronic diseases like diabetes, heart disease, or lung disease need careful management before, during, and after surgery. We help patients control their conditions, adjusting medications as needed to ensure they’re healthy enough for surgery.
Obese Patients
Obese patients face higher risks, such as wound and breathing problems, during colorectal surgery. We manage these risks with nutritional counseling and careful surgical planning.
|
Consideration |
Strategy for Obese Patients |
|---|---|
|
Nutritional Status |
Preoperative nutritional counseling |
|
Surgical Technique |
Use of minimally invasive techniques when possible |
|
Wound Care |
Enhanced postoperative wound care protocols |
Previous Adverse Reactions to Anesthesia
Patients with a history of bad reactions to anesthesia need special care. We review their past experiences and work with anesthesiologists to find safer alternatives.
We might choose different anesthesia types or adjust dosages based on their past reactions. Our goal is to make sure all patients have a safe and comfortable experience, no matter their history with anesthesia.
Costs and Insurance Coverage for Anesthesia in Colorectal Surgery
Many patients wonder about the cost of anesthesia for colorectal surgery. Knowing the financial side can ease your mind and help you heal better. We’ll cover typical costs, insurance, and what to ask your doctor.
Typical Anesthesia Costs
Anesthesia costs for colorectal surgery vary a lot. This depends on the surgery’s complexity, the anesthesiologist’s fees, and the surgery location. On average, costs range from $800 to $2,000 or more. These are separate from the surgeon’s fees and hospital bills.
Insurance Coverage Considerations
Most insurance plans cover anesthesia for colorectal surgery. But, coverage can differ a lot. It’s key to check your coverage before surgery to know what you’ll pay. Also, see if your insurance needs pre-approval for anesthesia.
- Check if your insurance covers the anesthesiologist’s fees.
- Verify if there are any out-of-network charges.
- Understand your deductible and co-pay requirements.
Questions to Ask Your Provider
To get ready for the financial side of your surgery, ask your doctor these questions:
- What are the estimated costs for anesthesia services?
- Are there any additional fees associated with the anesthesia?
- How do I verify my insurance coverage for anesthesia?
- Are there any financial assistance programs available?
Understanding anesthesia costs and insurance for colorectal surgery helps you manage your care’s financial side. This way, you can focus on getting better.
Conclusion
Knowing about anesthesia for colorectal surgery is key for patients to feel ready. We’ve looked at the different types of anesthesia and the role of anesthesiologists. We also talked about special care for high-risk patients.
Colorectal surgery, whether it’s traditional or minimally invasive, needs careful planning. By learning about anesthesia options, patients can better understand their surgery. This helps them make informed choices about their care.
In conclusion, talking about anesthesia with your doctor is very important. It helps patients feel less anxious and more confident in their treatment. Our aim is to offer full support to international patients looking for advanced medical care, including colorectal surgery.
FAQ
What type of anesthesia is typically used for colorectal surgery?
General anesthesia is often used for colorectal surgery. It makes sure you’re asleep and comfortable. But, the choice of anesthesia can change based on the surgery, your health, and the surgeon’s choice.
Will I be asleep during the entire surgery?
Yes, you’ll be asleep and won’t feel the surgery. Our anesthesiologists watch your vital signs to keep you safe and comfortable.
What are the benefits of being awake during colorectal surgery?
Being awake can have benefits like less risk of breathing problems and less nausea. It might also mean a quicker recovery. But, it depends on the surgery and your health.
How is pain managed after colorectal surgery?
We use different medicines to manage pain after surgery. This includes opioids, non-opioid pain relievers, and local anesthetics. We’ll work with you to find the best pain plan for you.
Are there any risks associated with anesthesia for colorectal surgery?
Yes, anesthesia can have risks like allergic reactions and breathing problems. But, our skilled anesthesiologists take steps to reduce these risks and keep you safe.
How long does it take to recover from anesthesia after colorectal surgery?
Recovery time varies based on your age, health, and surgery type. Most people start to feel the anesthesia effects wear off a few hours after surgery.
Can I discuss my anesthesia options with my doctor?
Yes, we encourage talking about anesthesia options with your surgeon and anesthesiologist. They’ll help pick the best anesthesia for you.
Will I experience any side effects from the anesthesia?
You might feel drowsy, nauseous, or have a sore throat after anesthesia. These effects are usually short-term and can be managed with medicine or other treatments.
How do I prepare for anesthesia before colorectal surgery?
Follow the instructions from your healthcare team, like fasting and medication changes. This helps ensure your safety and comfort during the surgery.
Are there any costs associated with anesthesia that I should be aware of?
Anesthesia costs ca n vary. They depend on the type of anesthesia, surgery complexity, and your insurance. Talk to your healthcare provider about costs and insurance to understand your financial responsibilities.
Can patients with chronic conditions undergo colorectal surgery safely?
Yes, people with chronic conditions can have surgery safely. We carefully evaluate and manage their risks. We create a personalized plan to ensure their safety during the procedure.
What is the role of the anesthesiologist during colorectal surgery?
The anesthesiologist is key to your comfort and safety during surgery. They give anesthesia, monitor your vital signs, and handle any complications that might arise.





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News