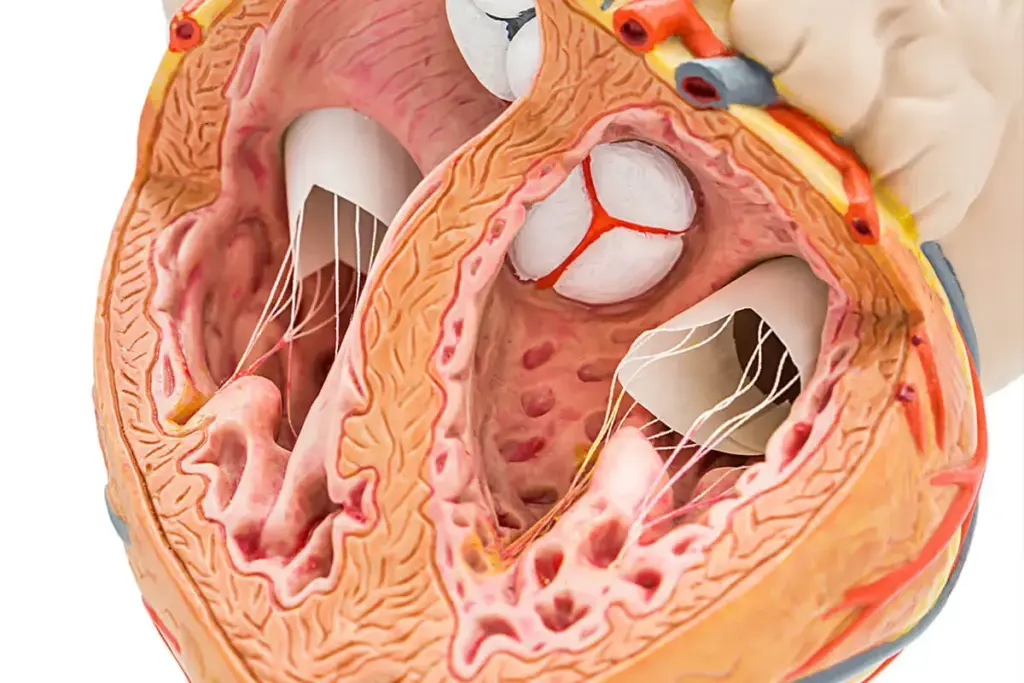
Many patients worried about heart ablation pain. It’s normal to feel scared about medical procedures. We get it, and we’re here to help.
Heart ablation, or cardiac ablation, treats heart rhythm issues. It might sound scary, but it’s a common and effective treatment for many.
We’ll dive into the procedure’s details. You’ll learn about any pain or discomfort you might feel. We’ll also cover what to expect during recovery.
Key Takeaways
- Understanding the heart ablation procedure and its purpose.
- What to expect in terms of pain or discomfort during and after the procedure.
- Overview of the recovery process and post-procedure care.
- Factors influencing the level of pain experienced by patients.
- How heart ablation can improve the quality of life for patients with heart rhythm disorders.
What Happens During a Cardiac Ablation Procedure
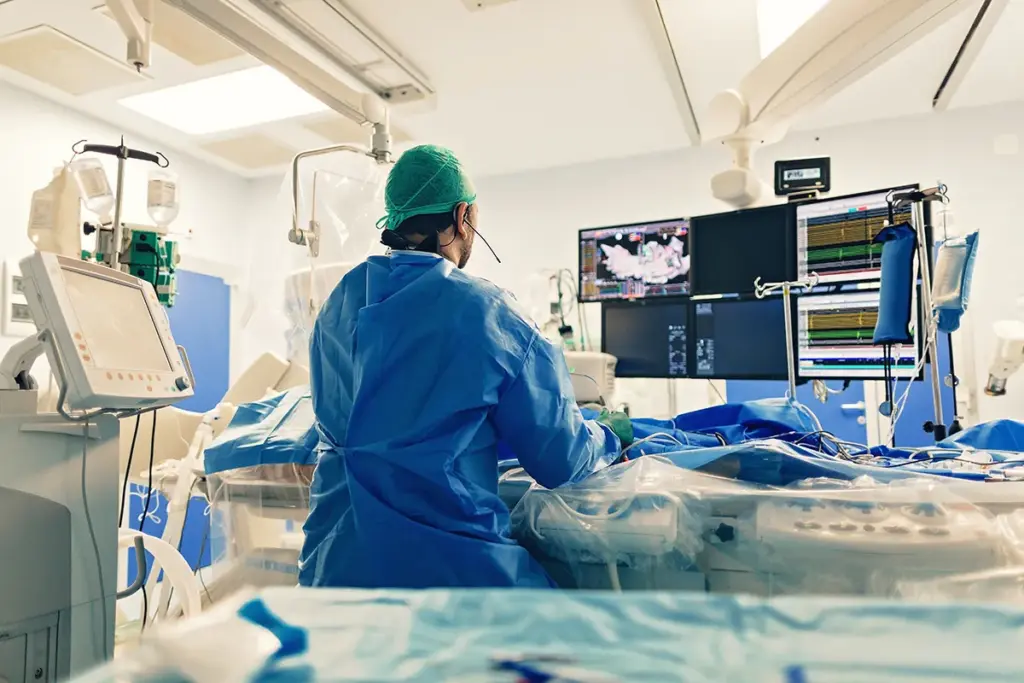
The cardiac ablation procedure is a complex method to fix irregular heartbeats. It uses energy to destroy the abnormal electrical pathways in the heart. This is done to treat arrhythmias that affect millions globally.
Definition and Purpose of Heart Ablation
Heart ablation, or cardiac ablation, is a medical procedure for arrhythmias or irregular heartbeats. Its main goal is to fix the heart rhythm by removing the source of the problem.
We use radiofrequency energy or cryoablation to target the heart areas causing arrhythmias. This blocks the abnormal electrical pathways, helping the heart beat regularly.
Common Heart Conditions Treated with Ablation
Cardiac ablation treats various arrhythmias, including:
- Atrial fibrillation
- Supraventricular tachycardia (SVT)
- Ventricular tachycardia
- Atrial flutter
These conditions can lead to symptoms like palpitations, shortness of breath, and fatigue. Cardiac ablation can greatly improve patients’ lives by addressing the arrhythmia’s root cause.
How Ablation Corrects Abnormal Heart Rhythms
Ablation fixes irregular heart rhythms by targeting the heart tissue causing the problem. The process involves:
- Mapping the heart’s electrical pathways to find the arrhythmia source
- Using energy (radiofrequency or cryoablation) to destroy the targeted tissue
- Checking that the abnormal electrical signals are gone
This method effectively treats arrhythmias, restoring a normal heart rhythm. It improves patients’ health and well-being.
Types of Ablation Techniques for Heart Rhythm Disorders
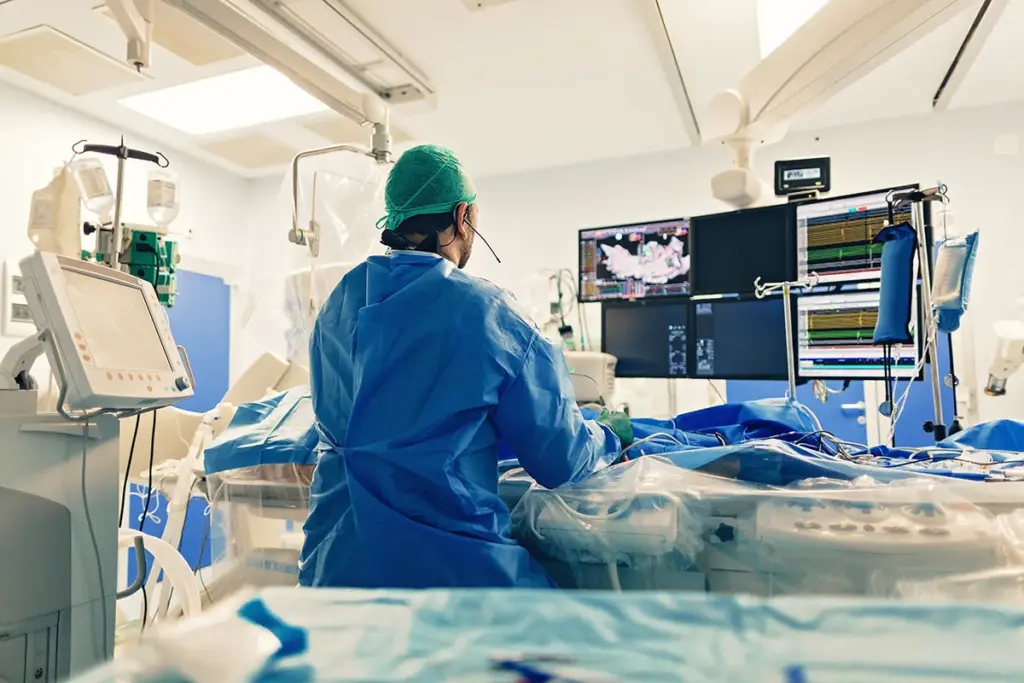
Ablation techniques for heart rhythm disorders have evolved. They provide several effective treatment options. These methods are key for treating various heart rhythm disorders. They offer patients tailored solutions based on their specific conditions.
Radiofrequency Ablation
Radiofrequency ablation uses electrical energy to destroy abnormal heart pathways. It’s widely used for treating arrhythmias like SVT and atrial flutter.
The procedure involves using a catheter to deliver radiofrequency energy. This energy targets and eliminates the arrhythmia source.
- Effective for treating various arrhythmias
- Minimally invasive procedure
- Quick recovery time
Cryoablation (Freezing Method)
Cryoablation, or cryotherapy, uses extreme cold to destroy abnormal pathways. It’s useful for treating certain arrhythmias without harming the heart tissue.
Cryoablation has a lower risk of complications compared to radiofrequency ablation. This makes it a good option for some patients.
Laser Ablation Procedures
Laser ablation uses a laser to destroy abnormal heart tissue. This method is less common but offers an alternative for specific conditions.
The precision of laser ablation can be beneficial in certain cases. Its application is more limited compared to other techniques.
Pulmonary Vein Ablation for Atrial Fibrillation
Pulmonary vein ablation is used mainly to treat atrial fibrillation. It isolates the pulmonary veins from the heart to stop abnormal signals.
This technique is effective in reducing atrial fibrillation symptoms in many patients. It may need multiple procedures for the best results.
Pain Expectations During Cardiac Ablation
Knowing what to expect about pain during cardiac ablation can help ease worries. This procedure treats heart rhythm problems and is usually safe. Yet, many patients worry about pain.
Anesthesia Options and Their Effects
The anesthesia used in cardiac ablation greatly affects pain. You might get local anesthesia, conscious sedation, or general anesthesia. The choice depends on your health, the procedure’s complexity, and your doctor’s advice.
Common Sensations Patients Report
People having cardiac ablation might feel different things. Some feel pressure or discomfort where the catheter goes in. Others might feel a burning or cold sensation from the ablation itself.
Factors That Influence Pain Perception
Many things can change how much pain you feel during cardiac ablation. These include your pain tolerance, the ablation technique, and the anesthesia’s effectiveness. Knowing these can help you prepare better.
|
Factor |
Description |
Impact on Pain |
|---|---|---|
|
Anesthesia Type |
Local, Conscious Sedation, General Anesthesia |
Varies; General Anesthesia typically results in less pain during the procedure. |
|
Pain Tolerance |
Individual’s threshold for pain |
Higher tolerance may result in less reported pain. |
|
Ablation Technique |
Radiofrequency, Cryoablation, Laser |
Different techniques may cause different sensations; e.g., Cryoablation may cause a cold sensation. |
Understanding pain factors and management options can boost confidence for cardiac ablation. It’s key to talk to your healthcare provider about your concerns. This way, you can create a plan for managing pain that’s just right for you.
Preparing for Your Heart Ablation Procedure
Knowing what to expect before your heart ablation can make you feel less anxious. We’ll guide you through the steps to prepare for your procedure.
Pre-Procedure Testing and Evaluation
Before your heart ablation, we do several tests to check your heart. These tests include:
- A cardiac nuclear stress test to see how your heart works under stress
- An echocardiogram to look at your heart’s structure and function
- Blood tests to find any conditions that might affect your procedure
These tests help us find the best way to do your ablation and keep you safe during it.
|
Test |
Purpose |
|---|---|
|
Cardiac Nuclear Stress Test |
Checks how your heart works under stress |
|
Echocardiogram |
Looks at your heart’s structure and function |
|
Blood Tests |
Looks for any underlying conditions |
Medication Adjustments Before Ablation
Some medications might need to be changed or stopped before your procedure. We’ll look at your current medications and tell you what to do. This could mean:
- Stopping anticoagulants a few days before to lower bleeding risk
- Adjusting anti-arrhythmic medications to keep your heart rhythm stable
It’s very important to follow our instructions about your medications. This ensures your safety and the success of your ablation.
Fasting and Day-of-Procedure Instructions
On the day of your procedure, you’ll need to fast for a while. This is usually:
- No food or drink for at least 6-8 hours before the procedure
- Clear liquids might be okay up to 2 hours before, but check with your healthcare team
We’ll also tell you what to bring to the hospital or clinic. This includes:
- A list of your medications and how much to take
- Any important medical records or test results
- A person to drive you home after the procedure
Following these instructions carefully will help make your procedure go smoothly and successfully.
Ablation as a Minimally Invasive Cardiac Procedure
Cardiac ablation is a new, less invasive way to treat heart rhythm problems. It’s a big change from old methods, making it safer than open-heart surgery.
Catheter-Based vs. Surgical Approaches
The main difference is how invasive they are. Catheter-based ablation uses thin tubes through a vein in the leg to reach the heart. This way, you don’t need to open your chest, which means less pain and quicker healing.
On the other hand, traditional surgery is more invasive. It’s done through open-heart surgery. This method is effective but riskier and takes longer to recover from.
Benefits of Minimally Invasive Techniques
Minimally invasive methods, like catheter-based ablation, have many benefits. These include:
- Smaller or no cuts, so less scarring
- Less pain during and after the procedure
- Shorter hospital stays and quicker recovery times
- Lower risk of complications compared to open surgery
These perks make minimally invasive cardiac procedures a great choice for those wanting effective treatment with less impact on their lives.
Recovery Advantages Compared to Open Surgery
The recovery from ablation procedures is much better than open surgery. Patients who get catheter-based ablation usually:
- Get back to normal faster
- Face less risk of infection and other surgery problems
- Need less pain medicine after the procedure
Overall, the recovery advantages of minimally invasive cardiac ablation make it a popular choice for many.
The Step-by-Step Ablation Procedure Experience
Learning about the ablation procedure can ease worries and prepare you. We’ll walk you through each part, from when you arrive to the end of the procedure.
Arrival and Initial Preparation
When you arrive, you’ll go to a prep area to change into a gown. Our team will explain the procedure, answer your questions, and give you sedation or anesthesia if needed. This step is key for a comfortable ablation procedure.
Catheter Insertion and Navigation
Next, we’ll insert catheters through a small cut in your groin or arm. These catheters are guided to your heart using special imaging. Our skilled cardiologists will carefully move the catheters to the right spots.
The Actual Ablation Process
With the catheters in place, we start the ablation. We use energy through the catheters to treat the heart areas. The energy type depends on your condition and needs. Our team watches closely to make sure it’s working right.
Procedure Duration and Monitoring
The procedure can last from 2 to 4 hours, based on the case. We keep a close eye on your heart rhythm and health. This lets us adjust as needed for the best results.
Knowing what to expect from the ablation procedure experience helps. We aim for a safe, effective treatment that eases your discomfort and aids in a quick recovery.
Discomfort Levels During Different Ablation Methods
The discomfort during cardiac ablation varies by method. It’s key to know how each technique affects comfort.
Pain Comparison: Radiofrequency vs. Cryoablation
Radiofrequency ablation uses heat to fix heart issues. Cryoablation uses cold. Each has its own comfort level for patients.
Those getting radiofrequency ablation might feel heat or discomfort. But, sedation helps manage it. Cryoablation causes cold, but some find it less painful than radiofrequency.
Patient Experiences with Various Techniques
Experiences with cardiac ablation differ greatly. The technique, heart area, and pain tolerance matter. Some feel little pain, while others feel more.
- Cryoablation patients might feel cold or pressure.
- Radiofrequency ablation patients might feel heat or burning.
- Most patients find the procedure tolerable, with manageable discomfort.
Factors That May Increase Procedural Discomfort
Several things can make discomfort worse during cardiac ablation. These include procedure complexity, number of ablations, and patient health. Anxiety and stress before the procedure also play a part.
Knowing these factors helps prepare for the procedure. It can reduce discomfort with the right strategies.
Post-Procedure Pain and Immediate Recovery
Knowing what to expect after cardiac ablation can ease worries and make the recovery smoother. The first hours and days are key for managing pain and ensuring a good outcome.
First 24 Hours After Ablation
The first 24 hours are critical for recovery. Patients are watched closely for a few hours after the procedure to catch any immediate issues. Some discomfort, like soreness at the catheter site or feeling tired, is common.
Resting is important during this time. Patients should avoid hard work and heavy lifting. It’s also important to watch for signs like severe chest pain, trouble breathing, or a lot of bleeding.
Common Sources of Post-Procedure Discomfort
Discomfort after cardiac ablation can come from several places:
- Soreness or bruising at the catheter insertion site
- Swelling or redness in the groin or arm where the catheter was placed
- Fatigue or a general feeling of being unwell
- Mild chest discomfort or palpitations
These symptoms usually go away in a few days.
Initial Pain Management Strategies
Good pain management is essential for a comfortable recovery. Strategies include:
|
Pain Management Approach |
Description |
|---|---|
|
Medication |
Over-the-counter pain relievers or prescribed medications to manage pain and discomfort. |
|
Rest |
Avoiding strenuous activities and getting plenty of rest to help the body recover. |
|
Monitoring |
Keeping track of symptoms and reporting any concerns to healthcare providers. |
Effective pain management is key for a smooth recovery. By knowing what to expect and how to handle pain, patients can get through the recovery period more easily.
Potential Complications and Associated Discomfort
Cardiac ablation is usually safe, but complications can happen. It’s important for patients to know these risks to get the right care and recovery.
Minor Complications and Their Symptoms
Minor issues might include soreness where the catheter was, mild chest pain, or short-term heart rhythm problems. These are usually fixed with rest and medicine.
Serious Complications and Warning Signs
Though rare, serious problems like cardiac tamponade, pulmonary vein stenosis, or stroke can occur. Look out for severe chest pain, trouble breathing, or changes in your brain or nerves.
When to Contact Your Doctor or Seek Emergency Care
If you keep feeling bad or have severe symptoms, call your doctor. For severe chest pain, trouble breathing, or other scary signs, go to the emergency room right away.
|
Complication Type |
Symptoms |
Recommended Action |
|---|---|---|
|
Minor |
Soreness, mild chest discomfort |
Rest, medication |
|
Serious |
Severe chest pain, difficulty breathing, neurological changes |
Seek emergency care |
Knowing about possible complications and their signs can help a lot. If you’re worried or notice anything odd after your procedure, talk to your doctor.
Recovery Timeline After Cardiac Ablation
Knowing the recovery timeline after cardiac ablation is key for patients. This procedure treats arrhythmias by destroying bad heart pathways. Everyone recovers differently, but there’s a general pattern.
First Week Post-Procedure
The first week is very important. Patients are watched closely after the procedure and then go home. They might feel tired, sore, and have bruises where the catheter was.
They should not lift heavy things, bend, or do hard activities.
Key Activities to Avoid:
- Lifting objects heavier than 10-15 pounds
- Engaging in strenuous exercise or activities that cause sweating
- Taking a bath or submerging the catheter site in water
Weeks 2-4 Recovery Milestones
By weeks 2-4, most people start to feel better. They get less tired and can do more things. It’s important to listen to the doctor’s advice on when to start exercising again and other activities.
Recovery Milestones:
- Gradual return to light exercise
- Increased energy levels
- Improvement in overall well-being
Long-term Recovery Expectations
How long it takes to fully recover from cardiac ablation varies. Most people can get back to normal in 4-6 weeks. It might take a few months to see the full benefits of the procedure.
Going to follow-up appointments with the cardiologist is important. This helps check how the heart is doing and address any issues.
Long-term Considerations:
- Attending follow-up appointments
- Monitoring heart rhythm and reporting any irregularities
- Maintaining a healthy lifestyle to support heart health
Pain Management Options Following Ablation Therapy
Managing pain well is key to a smooth recovery after ablation therapy. It helps patients get back to their normal life faster. Effective pain management makes a big difference in recovery.
Prescribed Pain Medications
Doctors often give pain meds after ablation therapy. These can be opioids for strong pain or non-opioid meds for less pain. Always follow the dosage and talk to your doctor if you have any questions.
Some common pain meds include:
- Acetaminophen with codeine
- Oxycodone
- Hydrocodone
Over-the-Counter Pain Relief Options
For mild to moderate pain, OTC meds can work well. Acetaminophen (Tylenol) and ibuprofen (Advil, Motrin) are good choices. But, always check with your doctor first, even for OTC meds.
|
Medication |
Dosage |
Side Effects |
|---|---|---|
|
Acetaminophen |
500mg every 4-6 hours |
Liver damage (high doses) |
|
Ibuprofen |
200-400mg every 4-6 hours |
Stomach upset, kidney issues |
Non-Pharmaceutical Comfort Measures
There are also non-medication ways to ease pain and discomfort. These include:
- Resting and avoiding hard activities
- Using heat or cold packs on the area
- Trying relaxation techniques like deep breathing or meditation
“Using a mix of meds and non-medical comfort methods can really help with recovery.” – A Cardiologist
Returning to Normal Activities After Heart Ablation
Patients often wonder when they can go back to normal after heart ablation. The recovery time varies, but knowing the basics helps. It makes the transition back to daily life smoother.
Activity Restrictions and Timelines
Right after the procedure, patients should avoid hard work. Heavy lifting, bending, or exercise should be avoided for at least 24 to 48 hours. The exact time to start activities again depends on health, procedure complexity, and doctor’s advice.
Here’s a general outline of activity restrictions and timelines:
|
Activity |
Recommended Waiting Period |
|---|---|
|
Light walking |
Immediately after procedure |
|
Moderate exercise (e.g., brisk walking) |
3-5 days post-procedure |
|
Strenuous exercise (e.g., running, heavy lifting) |
1-2 weeks post-procedure |
Gradual Return to Exercise Protocol
Coming back to exercise after heart ablation should be slow. Start with short walks and gradually increase the time and intensity. It’s important to listen to your body and not overdo it.
“The key to a successful recovery is patience and a gradual return to normal activities. It’s not just about getting back to where you were before the procedure, but also about ensuring that you’re healing properly.” – A Cardiologist
Long-term Lifestyle Considerations
Keeping a healthy lifestyle is key after heart ablation. This means eating well, exercising regularly, managing stress, and taking medications as prescribed. Regular check-ups with your cardiologist are vital to keep your heart healthy.
By following these guidelines, patients can safely and effectively return to their normal activities after heart ablation.
Real Patient Experiences with Cardiac Ablation
Real patient testimonials give us a peek into what happens during and after cardiac ablation. These stories show the different experiences people have had with this procedure. They help ease worries and give a clear idea of what to expect.
Pain Level Testimonials
People have reported feeling different levels of pain during and after the procedure. Some say it was just a little uncomfortable, while others felt more pain. For example, one patient might say, “I was surprised by how little pain I experienced during the procedure.” Others might feel more pain, showing the need for custom pain plans.
- Some patients experience minimal discomfort.
- Others report more significant pain during the procedure.
- Pain management strategies are tailored to individual needs.
Varying Recovery Experiences
Recovery times after cardiac ablation can differ a lot. Some people bounce back quickly, while others take longer. The speed of recovery depends on the patient’s health, the procedure’s complexity, and following doctor’s orders.
- Most patients can resume normal activities within a week.
- Some may need more time to fully recover.
- Following post-procedure instructions is key for a smooth recovery.
Long-term Satisfaction Rates
Most patients are very happy with the results of cardiac ablation. They often see big improvements in their life quality, with fewer symptoms and better heart function. Doctors might use a stress test with nuclear imaging to check the heart’s function after the procedure.
Key benefits reported by patients include:
- Reduced frequency of arrhythmia episodes.
- Improved overall heart health.
- Enhanced quality of life.
Sharing real patient stories helps us understand the good and bad of cardiac ablation. These testimonials are a great help for those thinking about this procedure. They offer a clear view of what to expect.
Discussing Pain Concerns with Your Cardiologist
Talking about pain with your cardiologist before cardiac ablation is key. This chat helps tailor the procedure to fit your needs. It ensures your comfort and addresses any worries you might have.
Important Questions to Ask Before Your Procedure
It’s smart to prepare questions for your consultation. Ask about:
- What kind of pain or discomfort you might feel during the procedure.
- Your anesthesia options and how they’ll affect your pain.
- How your pain will be managed after the procedure.
- Recommended pain management strategies for cardiac ablation.
These questions help you understand what to expect and how your pain will be managed.
Communicating Your Pain Tolerance and Concerns
Telling your cardiologist about your pain tolerance and concerns is vital. This open talk helps tailor your care. Discuss:
- Your past experiences with pain and how you’ve handled it.
- Any fears or anxieties you have about the procedure.
- Your preferences for pain management, including any effective methods you’ve tried.
Your cardiologist is there to support you. Sharing your concerns can make you more comfortable and satisfied with the procedure.
Creating a Personalized Pain Management Plan
Your cardiologist will create a pain management plan just for you. This plan might include:
- Medications to manage pain and discomfort.
- Alternative pain relief strategies, like relaxation techniques or physical therapy.
- Advice on managing side effects or complications.
Having a clear plan can reduce anxiety and improve your experience. As one patient said, “Knowing my pain management options and having a plan made a big difference in my comfort during recovery.”
“The key to a successful cardiac ablation isn’t just about the technical skills of the cardiologist, but also about how well they address the patient’s concerns and pain.” -A Cardiologist
By discussing your pain concerns and working with your cardiologist, you can have a more comfortable and successful cardiac ablation experience.
Conclusion
Cardiac ablation is a key treatment for heart rhythm disorders. It might cause some discomfort, but there are ways to manage pain. This makes the procedure more comfortable.
Knowing what to expect during recovery is important. Being well-informed helps patients smoothly go through the process. This knowledge prepares them for the therapy.
We’ve talked about different ablation techniques and the role of anesthesia. Post-procedure care is also vital. Working with a cardiologist helps create a pain management plan that fits each patient’s needs.
In summary, cardiac ablation is a powerful treatment for heart issues. Understanding the procedure, possible discomfort, and recovery helps patients make better choices. Good pain management and support can greatly improve the therapy’s success.
FAQ
What is a nuclear stress test?
A nuclear stress test is a test that uses a tiny bit of radioactive material. It shows how the heart and blood flow work when stressed. This stress is usually from exercise or medicine.
How does a nuclear stress test differ from a regular stress test?
A nuclear stress test uses radioactive dye to see the heart. This lets doctors check blood flow and heart function more closely than a regular stress test.
What is the purpose of a cardiac nuclear stress test?
This test is mainly to find and check heart problems like coronary artery disease and heart failure. It looks at how blood flows to the heart muscle.
Is a nuclear stress test painful?
The test itself is not painful. But, some people might feel uncomfortable during the stress part, whether it’s from exercise or medicine.
How accurate is a nuclear stress test?
Nuclear stress tests are very accurate. They can spot coronary artery disease and heart function issues well. They have high sensitivity and specificity.
What is the difference between a nuclear stress test and a cardiac PET scan?
Both tests use radioactive material. But, a cardiac PET scan gives even clearer images of the heart’s blood flow and metabolism. It’s used for more detailed diagnoses.
Can I undergo a nuclear stress test if I have a pacemaker or other implanted devices?
Mostly, having a pacemaker or other devices doesn’t stop you from getting a nuclear stress test. But, tell your doctor about any devices you have before the test.
How long does a nuclear stress test take?
The whole process takes a few hours. This includes getting ready, doing the test, and recovering.
Are there any side effects from the radioactive dye used in a nuclear stress test?
The dye is safe, and side effects are rare. Some people might get a little itching or flushing.
Can I eat or drink before a nuclear stress test?
It’s best to avoid eating or drinking certain things before the test. Your doctor will tell you exactly what to do.
What should I expect during the recovery period after a nuclear stress test?
After the test, you can usually go back to normal activities. The radioactive material will leave your body in a few hours to a day.
How does ablation therapy relate to nuclear stress tests?
Ablation therapy, like radiofrequency ablation, treats heart rhythm problems. A nuclear stress test might be done before or after to check the heart’s function.
What are the benefits of minimally invasive cardiac procedures like ablation?
Procedures like ablation are less invasive. They have less pain, quicker recovery, and fewer complications than open-heart surgery.
How does a nuclear stress test help in diagnosing heart conditions?
A nuclear stress test gives detailed images of the heart’s blood flow and function under stress. This helps doctors diagnose and manage heart conditions, like coronary artery disease.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/25488958/




































