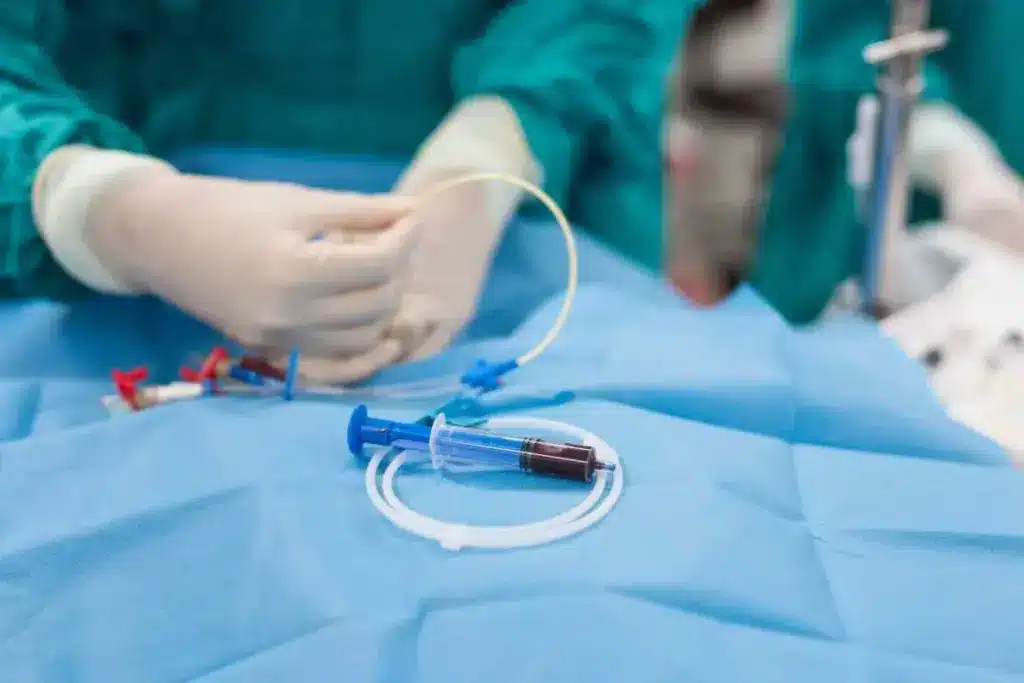
Atrial fibrillation (AFib) is a common heart rhythm disorder affecting millions worldwide. Despite the effectiveness of atrial fibrillation ablation, some patients experience AFib recurrence. Studies indicate that 20–40% of patients may face AFib again after the procedure. What if AFib returns? Discover why afib ablation remains a vital tool and learn about the amazing second chances for a normal heart rhythm.
Experiencing AFib recurrence can be concerning, and understanding the risks and management options is key. We are committed to delivering world-class healthcare. We offer complete support for international patients.
We will explore the reasons behind AFib recurrence after cardiac ablation for afib. We will also discuss effective management strategies. Our goal is to provide you with the necessary information and support. We aim to help you navigate this condition with confidence.
Key Takeaways
- AFib recurrence is a common concern after atrial fibrillation ablation.
- Understanding the risks associated with AFib recurrence is key.
- Effective management strategies are available for AFib recurrence.
- World-class healthcare is essential for managing AFib recurrence.
Understanding AFib Recurrence After Ablation
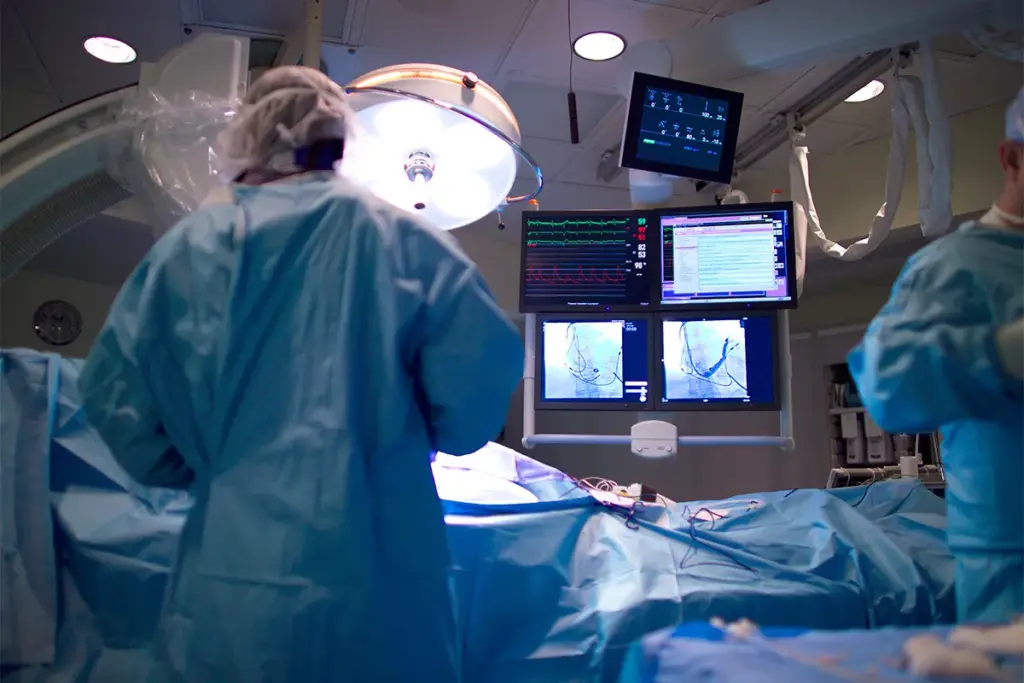
It’s important to understand why atrial fibrillation (AFib) might come back after treatment. AFib recurrence can affect a patient’s health and life quality. Knowing this helps manage what patients expect and their outcomes.
Definition of AFib Recurrence
AFib recurrence happens when atrial fibrillation returns after a treatment called catheter ablation. This can happen for several reasons, like pulmonary vein reconnection and non-pulmonary vein triggers. Studies show that up to 50% of patients might experience recurrence over time.
Timeframes for Recurrence Classification
The time it takes for AFib to come back can vary. It’s key to know the different time frames for recurrence. This helps figure out if the treatment worked and what to do next.
Impact on Patient Health and Quality of Life
When AFib comes back, it can harm a patient’s health. It can raise the risk of stroke by five times and increase the chance of heart failure. So, managing AFib recurrence is vital for better health and life quality. Here are some important points:
- Increased Stroke Risk: AFib raises the stroke risk, making it important for patients to take anticoagulation therapy.
- Impact on Quality of Life: Recurrent AFib can cause symptoms like palpitations, shortness of breath, and fatigue. These symptoms can lower a patient’s quality of life.
- Risk of Heart Failure: AFib can lead to heart failure. This shows why managing recurrence is so important.
Statistics on AFib Recurrence Rates
Looking at AFib recurrence rates after ablation helps us see how well the procedure works. It also shows where we can get better. We look at the data to give you an idea of what to expect.
Short-term Recurrence Rates
Research shows that short-term recurrence rates, or recurrences in the first year, are between 20% to 40%. These numbers can change based on the ablation method and the patient’s health.
Medium-term Recurrence Rates
In the medium term, which is one to three years after the procedure, rates are between 40% to 50%. This time frame is key because it shows how long the ablation lasts.
Long-term Recurrence Rates
Looking at data up to five years after ablation, rates are about 50.3%. A study on Annals of Cardiothoracic Surgery sheds light on long-term results. It shows why keeping an eye on patients is so important.
Factors Affecting Statistical Outcomes
Many things can change AFib recurrence rates. These include the ablation method, the patient’s health, and heart structure issues. Knowing these factors helps us understand the data better and make better care plans.
By looking at AFib recurrence rates, we learn more about managing AFib. We see why treatment plans need to be tailored to each patient.
The Blanking Period: What You Need to Know<SEP-9262_image_4>
Knowing about the blanking period is key for those who’ve had AFib ablation. It shows how the heart heals after the procedure. This time is important for the heart to adjust.
Definition and Duration
The blanking period usually lasts 3 months after the procedure. During this time, the heart is getting used to the changes. It’s common for patients to feel irregular heartbeats or early AFib recurrence.
Early recurrences might not mean the procedure failed. They often show the heart’s healing and inflammation.
Why Early Recurrences May Not Indicate Failure
Early AFib recurrence during the blanking period can be due to temporary reasons. These include inflammation or the heart adjusting to the procedure. These don’t always mean AFib will come back for good.
Studies show the heart keeps improving, even with early recurrences. So, it’s important to be patient and keep monitoring.
Monitoring During the Blanking Period
Keeping an eye on the heart during the blanking period is critical. It helps see how the heart is doing and adjust treatments if needed. This might include regular ECGs, Holter monitors, or other tools to check heart rhythm.
|
Monitoring Method |
Description |
Frequency |
|---|---|---|
|
ECG |
Electrocardiogram to assess heart rhythm |
As directed by physician |
|
Holter Monitor |
Portable device to record heart rhythm over 24-48 hours |
At 1 and 3 months post-ablation |
|
Event Recorder |
Device to record heart rhythm during symptoms |
As needed for symptoms |
Managing other health issues and sticking to lifestyle changes are key during this time. Understanding the blanking period helps patients better manage their recovery.
Mechanisms Behind AFib Recurrence
Understanding why AFib comes back is key to treating it well. AFib can return after treatment, and many things can cause it. Each person’s situation is different.
Pulmonary Vein Reconnection
Pulmonary vein reconnection is a main reason for AFib coming back. It happens when the heart’s electrical isolation is lost. This lets bad electrical signals get back into the heart. Pulmonary vein reconnection often means needing to do the treatment again to keep the heart’s rhythm steady.
Non-Pulmonary Vein Triggers
Sometimes, AFib comes back because of triggers not in the pulmonary veins. These can be in other parts of the heart. Finding and treating these triggers is important to prevent AFib from coming back.
“Advances in medical technology, such as pulsed field ablation, are being developed to improve outcomes and reduce recurrence.”
Structural Remodeling
Changes in the heart’s structure can also lead to AFib coming back. These changes happen when AFib lasts a long time. Fixing the underlying issues that cause these changes is vital for managing AFib.
Inflammatory Responses
Inflammation in the heart can also cause AFib to return. It can change the heart’s electrical and structural functions. Controlling inflammation with the right medicine can help lower this risk.
Knowing how AFib comes back helps doctors give better care. They can make treatments fit each person’s needs. This can lead to better results and less chance of AFib coming back.
Risk Factors for Returning to AFib After Ablation
Knowing the risk factors for AFib coming back is key. It helps us create treatment plans that fit each patient. This way, we can meet their unique needs better.
Age-Related Factors
Getting older raises the chance of AFib coming back after ablation. As we age, we’re more likely to get conditions like high blood pressure. Studies show that people over 65 face a higher risk.
Comorbid Conditions
Having other health issues, like high blood pressure or obesity, can raise the risk of AFib coming back. It’s important to manage these conditions well. For example, keeping a healthy weight and controlling blood pressure can help.
Some key conditions that affect AFib recurrence include:
- Hypertension
- Obesity
- Sleep-disordered breathing
- Diabetes
Structural Heart Disease
Heart problems, like thickened heart muscle or abnormal valves, can also increase the risk. These conditions might need a more detailed treatment plan. This could include medication and changes in lifestyle.
Genetic Predispositions
Genetics also play a part in the risk of AFib coming back. If you have a family history of AFib, you might be more likely to experience it again. While we can’t change genetics, knowing about them helps us plan better treatments.
By tackling these risk factors, we can lower the chance of AFib coming back. A good approach includes managing other health issues, addressing heart problems, and looking at genetics. This way, we can improve patient outcomes.
Symptoms of AFib Recurrence: What to Watch For
After AFib ablation, knowing the signs of recurrence is key. Spotting these symptoms early can help with treatment.
Common Symptoms
AFib recurrence symptoms differ for everyone. But, some common signs include:
- Palpitations: Irregular heartbeats or a fluttering feeling in the chest.
- Shortness of Breath: Feeling winded or having trouble breathing at rest.
- Fatigue: Feeling unusually tired or lacking energy.
- Chest Discomfort: Pain, pressure, or discomfort in the chest area.
- Dizziness or Lightheadedness: Feeling faint or like you might pass out.
Silent Recurrences
Some people have silent recurrences of AFib without symptoms. Regular check-ups with your doctor are vital.
When to Contact Your Doctor
If you notice any severe or worsening symptoms, reach out to your doctor. Also, contact them if symptoms affect your daily life or if you notice anything new or strange.
- Severe or worsening symptoms.
- Symptoms that interfere with daily activities.
- Any new or unexplained symptoms.
|
Symptom Severity |
Action |
|---|---|
|
Mild |
Monitor symptoms; schedule a follow-up if they persist. |
|
Moderate to Severe |
Contact your doctor for guidance. |
Distinguishing Normal Recovery from Recurrence
Telling normal recovery from AFib recurrence can be hard. Symptoms that get worse or last a long time might mean recurrence. Symptoms that get better are likely part of recovery.
Knowing the signs of AFib recurrence helps patients get help quickly. This can lead to better treatment outcomes.
Diagnostic Methods for Detecting Recurrent AFib
Advanced diagnostic techniques are key in tracking AFib recurrence after ablation. Spotting recurrence early is vital for timely action. This allows for better treatment plans, leading to improved patient results.
ECG Monitoring
ECG monitoring is a basic tool for finding AFib recurrence. It records the heart’s electrical activity in real-time. This helps doctors spot irregular heart rhythms linked to AFib.
Holter Monitors
Holter monitors record ECG over 24 to 48 hours. They catch AFib episodes that might miss a standard ECG check.
Implantable Loop Recorders
For those at high risk, implantable loop recorders offer long-term monitoring. They can track AFib episodes for years, giving insights into how often and long they last.
Mobile Health Technologies
Mobile health technologies have changed how we monitor AFib. Smartphones and wearables let patients track their heart rhythm anytime. This gives doctors real-time data for quick treatment changes.
Using these methods, we can better find AFib recurrence. We can then tailor treatments to each patient. This leads to better results for those who’ve had AFib ablation.
The AFib Ablation Procedure: A Brief Review
Knowing about the AFib ablation procedure is key for those thinking about it. This treatment aims to fix AFib by removing bad electrical paths in the heart. It helps stop arrhythmia.
How the Initial Procedure Works
The procedure starts with imaging to see the heart’s layout. Then, catheters are put in through a leg vein and guided to the heart. Next, energy is used to make lesions on the heart, stopping bad signals.
Key Steps in AFib Ablation:
- Imaging and mapping of the heart
- Insertion of catheters through a vein
- Guiding catheters to the heart
- Ablation using energy to create lesions
Success Rates for Different Ablation Techniques
AFib ablation success changes with the method and patient factors. Radiofrequency and cryoablation have different success rates.
|
Ablation Technique |
Short-term Success Rate |
Long-term Success Rate |
|---|---|---|
|
Radiofrequency Ablation |
70-80% |
50-60% |
|
Cryoablation |
80-85% |
60-65% |
Expectations vs. Reality
Patients often have different hopes than what happens with AFib ablation. Some feel no symptoms, but others need more treatment.
It’s important to remember that AFib ablation isn’t for everyone. The length of AFib, health issues, and the ablation method all play a part in success.
Treatment Options for Recurrent AFib
When AFib comes back after ablation, patients and doctors look at many treatment options. The right choice depends on the patient’s health, how bad the symptoms are, and why AFib came back.
Medication Management
Medicine is key in treating recurring AFib. Antiarrhythmic drugs help control symptoms and keep the heart rhythm normal. The right medicine depends on the patient’s health and any other health issues.
Amiodarone is often used because it works well, but it needs careful watching because of side effects. Other medicines like sotalol and flecainide might also be options based on the patient’s situation.
Repeat Ablation Considerations
For some, having another ablation might be a good choice. This decision is made after thinking about how the first procedure went and why AFib came back.
Having another ablation can be more complicated than the first one. It might need to fix more areas of bad electrical activity. How well it works can vary, so talking about the pros and cons with a doctor is important.
Hybrid Approaches
Hybrid methods mix different treatments, like medicine, ablation, and lifestyle changes, to tackle recurring AFib. This all-in-one approach can lead to better results by tackling the condition from different angles.
In a hybrid plan, medicine might be used to manage symptoms while another ablation is done to fix electrical issues. Making lifestyle changes, like losing weight or controlling blood pressure, is also key.
Emerging Therapies
New treatments for AFib are being researched, like pulse field ablation. There are also new medicines and devices being developed.
People with recurring AFib should talk to their doctor about these new options. This is true if usual treatments haven’t worked well.
|
Treatment Option |
Description |
Considerations |
|---|---|---|
|
Medication Management |
Use of antiarrhythmic drugs to control symptoms and maintain normal heart rhythm. |
Potential side effects, monitoring required. |
|
Repeat Ablation |
Repeat procedure to address recurrent AFib, potentially involving new areas of abnormal activity. |
Variable success rate, increased complexity. |
|
Hybrid Approaches |
Combination of treatments including medication, ablation, and lifestyle changes. |
Comprehensive strategy, potentially improved outcomes. |
|
Emerging Therapies |
New techniques and treatments being researched, such as pulse field ablation. |
Potential for improved efficacy, may not be widely available. |
If AFib Ablation Fails: Next Steps
Feeling disappointed when AFib comes back after ablation is normal. But, it’s important to figure out why it happened. Knowing why it didn’t work helps find the best next steps.
Evaluating Why the Procedure Didn’t Work
AFib ablation can fail for several reasons. These include pulmonary vein reconnection, non-pulmonary vein triggers, or structural remodeling of the heart. A doctor needs to check each case carefully to find out why.
“Understanding the reasons behind AFib ablation failure is key,” says a top cardiologist. This helps tailor treatments to fit each person’s needs.
Alternative Treatment Strategies
When ablation doesn’t work, other treatments can help. These might include medication management to control symptoms. Changes in lifestyle, like weight management and blood pressure control, can also help.
- Medication management to control AFib symptoms
- Lifestyle changes, including diet and exercise
- Consideration of repeat ablation or hybrid approaches
Managing Expectations
It’s important to manage what you expect when AFib ablation fails. Remember, AFib management is a long-term process that might need different treatments. Working with your doctor can help create a good plan for managing your condition.
When to Consider More Invasive Options
In some cases, more serious treatments might be needed. This could be repeat ablation procedures or hybrid approaches. Always talk to your doctor before trying these options, considering your health and situation.
By looking into why ablation failed and trying different treatments, you can improve your life and health.
Repeat AFib Ablation: What to Expect
Knowing what to expect from a repeat AFib ablation is key. This procedure is often needed when AFib comes back after the first one.
Differences from the First Procedure
A repeat AFib ablation might be different from the first one. The procedure can get more complex because of changes in the heart or scar tissue from before. We use new technologies to map the heart’s electrical paths better.
Before the procedure, we carefully review the patient’s history, past ablation details, and current heart health.
Success Rates of Subsequent Ablations
The success of repeat ablations can depend on several things. These include how well the first ablation worked and the patient’s health. Even though success rates might be lower, many patients find great benefits from repeat ablations.
- Success can be influenced by heart disease and other health issues.
- The doctor’s skill and experience are also very important.
Recovery Considerations
Recovery from a repeat AFib ablation is similar to the first one. Some patients might recover faster because they know what to expect. It’s important to follow post-procedure care closely to avoid complications.
Patients usually follow the same post-procedure plan as before. This includes watching for symptoms and going to follow-up appointments.
How Many Ablations Can One Safely Undergo?
How many ablations a patient can safely have varies. It depends on their health, the cause of AFib, and any issues from before. Every case is different, and we look at each one carefully.
We weigh the risks and benefits of each procedure. We follow the latest guidelines and consider the patient’s wishes.
Lifestyle Modifications to Reduce Recurrence Risk
Lifestyle changes are key to lowering the chance of AFib coming back after treatment. Making the right changes can greatly improve heart health and outcomes.
Weight Management
Keeping a healthy weight is essential to avoid AFib coming back. Research shows losing weight can greatly improve AFib symptoms. We suggest a mix of healthy eating and regular exercise to keep a good weight.
- Aim for a BMI between 18.5 and 24.9
- Eat a balanced diet full of fruits, veggies, and whole grains
- Do regular physical activities like walking or swimming
Blood Pressure Control
High blood pressure increases the risk of AFib coming back. Managing blood pressure well through lifestyle and, if needed, medicine is key. We advise:
- Check your blood pressure often
- Lower sodium intake
- Eat more foods high in potassium
Sleep Apnea Treatment
Sleep apnea often goes with AFib, and treating it can lower recurrence risk. We recommend:
- Get a sleep study if symptoms don’t go away
- Use CPAP therapy if you have sleep apnea
- Make lifestyle changes like losing weight and avoiding alcohol before bed
Exercise Recommendations
Regular exercise is vital for heart health and lowering AFib risk. Exercise boosts heart fitness and reduces stress. We suggest:
- Do at least 150 minutes of moderate-intensity aerobic exercise weekly
- Add strength training to your routine
- Stay away from very intense exercise if you’re not used to it, as it can trigger AFib
By making these lifestyle changes, people can greatly lower their risk of AFib coming back. This can also improve their overall life quality.
Conclusion
We get how tough it is to deal with AFib coming back after ablation. We’re all in on giving top-notch healthcare and support to patients from around the world. We’ve talked about how to handle AFib coming back, and it’s all about using the right strategies and care.
Knowing how AFib comes back, spotting risks, and using the right tests can help patients stay on top of their heart health. Our team is here to offer personalized care and support. We help patients understand their treatment choices and make smart health decisions.
We aim to give patients the power to manage their AFib. By mixing advanced medical care with healthy lifestyle changes and ongoing support, we help patients get the best results. For more details on our AFib treatment and care services.
FAQ
What is AFib recurrence, and how is it defined?
AFib recurrence happens when atrial fibrillation comes back after treatment. It’s when symptoms of AFib show up again or are found through tests after treatment.
What are the common symptoms of AFib recurrence?
Symptoms of AFib recurrence include heart racing, breathing problems, feeling tired, dizziness, and chest pain. Some people might not notice these symptoms.
How is AFib recurrence diagnosed?
Doctors use ECGs, Holter monitors, and implantable recorders to find AFib recurrence. They also use mobile health apps. These tools help spot AFib episodes and decide on treatment.
What is the blanking period after AFib ablation, and why is it important?
The blanking period is the first few months after treatment. It’s when the heart is adjusting. Early signs of AFib during this time might not mean treatment failed. It’s important to watch closely to see if treatment worked.
What are the risk factors for AFib recurrence after ablation?
Risk factors include age, health conditions, heart structure, and genetics. Knowing these helps doctors tailor treatment plans for each patient.
Can lifestyle modifications reduce the risk of AFib recurrence?
Yes, changes like losing weight, controlling blood pressure, treating sleep apnea, and exercising regularly can lower AFib recurrence risk. They also improve overall health.
What are the treatment options for recurrent AFib?
Treatment options include medications, repeat ablation, and new therapies. The best choice depends on the patient’s situation and needs.
How many times can one undergo AFib ablation?
How many times ablation can be done varies by patient and condition. There’s no strict limit. Decisions are made based on individual risks and benefits.
What happens if AFib ablation fails?
If ablation fails, doctors look into why it didn’t work. They consider other treatments, manage expectations, and might explore more invasive options.
What are the success rates of AFib ablation?
Success rates vary based on the treatment method, patient selection, and follow-up time. Rates range from 50% to 80% or more, depending on the situation.
References
https://my.clevelandclinic.org/health/treatments/14618-dialysis


































