Providing the complete arthropathy definition (joint disease) and examples of conditions that fall under this term.
Arthropathy is a wide term for many joint disorders. It’s key to know about arthropathy to spot and treat joint diseases. These diseases affect millions of people around the world.
The word arthropathy comes from Greek. “Arthro” means joint, and “pathos” means disease or suffering. It covers a broad range of joint problems, affecting how joints work and look.
Knowing the definition of arthropathy helps both patients and doctors. It makes it easier to spot symptoms, get treatment early, and avoid worse problems.
Key Takeaways
- Arthropathy is a term for many joint diseases.
- It includes various disorders that affect joints’ function and structure.
- Understanding arthropathy is key for diagnosis and treatment.
- The term comes from Greek words “arthro” and “pathos”.
- Arthropathy has many causes and types.
Understanding the Arthropathy Definition
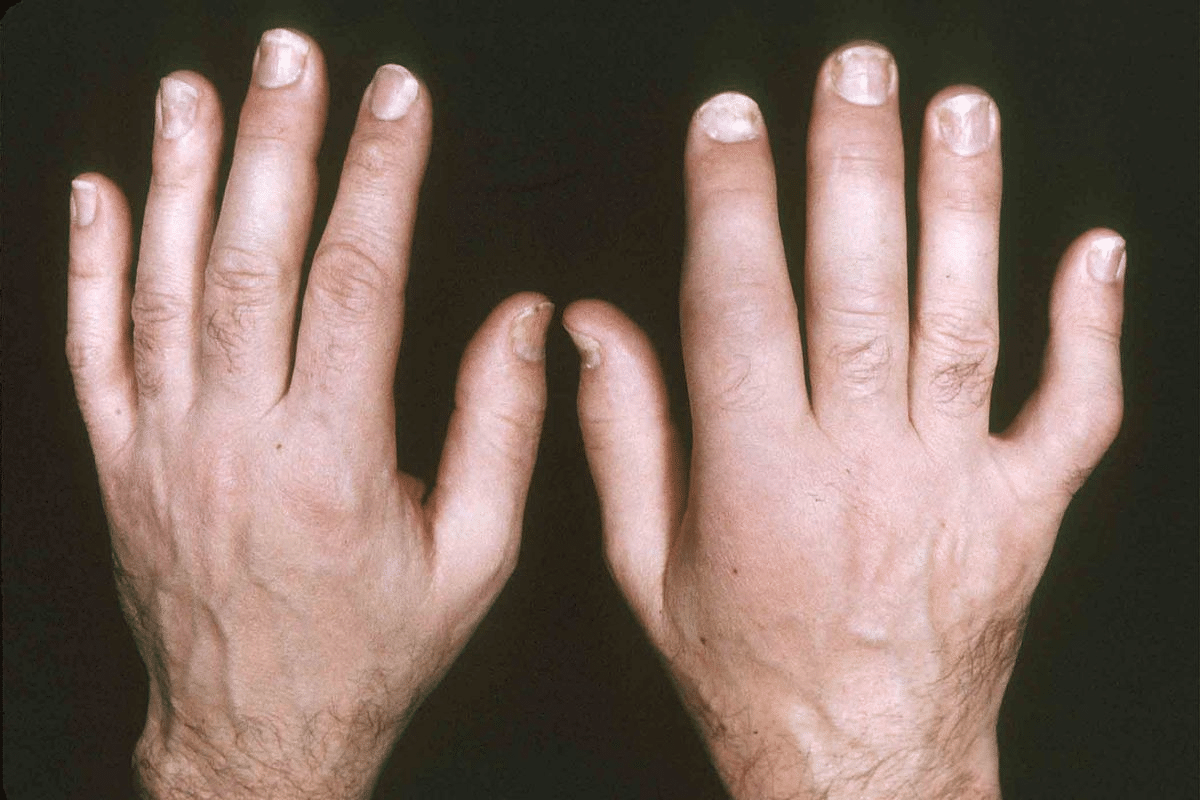
To grasp arthropathy, we must explore its roots and medical aspects. The word arthropathy comes from Greek. “Arthron” means joint, and “pathos” means disease or suffering. This background helps us understand its use in medicine.
Etymology and Origin of the Term
The word arthropathy comes from Greek. “Arthron” is for a joint, and “pathos” means disease or suffering. So, arthropathy means joint disease or suffering.
Medical Expert, a rheumatologist, says, “Arthropathy covers many joint disorders. It shows how complex joint diseases are.” This complexity is seen in the many forms and causes of arthropathies.
Medical Context and Usage
In medicine, arthropathy describes diseases or disorders of the joints. It’s often confused with arthritis, but they’re not the same. Arthropathy is a wider term that includes different joint conditions, like inflammatory and degenerative ones.
The medical field uses arthropathy to talk about joint conditions. It shows how important it is to diagnose and treat them right. The American College of Rheumatology says, “Knowing the type of arthropathy is key for good management and treatment of joint diseases.”
Arthropathy vs. Arthritis: Key Differences
Arthropathy and arthritis both deal with joint diseases, but they’re different. Arthritis usually means inflammation in the joints. Arthropathy is a broader term that includes many joint disorders, not just inflammatory ones.
- Arthritis is often linked to inflammation.
- Arthropathy covers a wider range of joint conditions.
- Knowing the difference is important for correct diagnosis and treatment.
As
“The difference between arthropathy and arthritis is not just about words. It affects how we treat and the outcomes for patients.”
The Prevalence and Impact of Joint Diseases
Arthropathies, or joint diseases, are a big health issue worldwide. They not only affect people’s quality of life but also put a heavy load on healthcare systems.
Statistical Overview in the United States
In the United States, arthropathies are quite common. The CDC says 18.9% of adults aged 18 and up had arthritis in 2022. This means millions of Americans live with some form of joint disease.
Arthritis hits different groups in different ways. For example, it’s more common in women than men. It also gets worse with age. Knowing this helps us focus our health efforts better.
|
Demographic Group |
Prevalence of Arthritis |
|---|---|
|
Women |
21.1% |
|
Men |
16.5% |
|
Adults aged 18-44 years |
8.4% |
|
Adults aged 45-64 years |
24.6% |
|
Adults aged 65 years and older |
43.2% |
Economic and Social Burden
Arthropathies cost a lot. The expenses include medical bills and lost work time. The total annual cost of arthritis in the US is over $300 billion. It’s one of the most expensive chronic diseases.
Arthropathies also affect society in big ways. They can cause disability and lower quality of life. It’s important to find good treatments to lessen these effects.
It’s key to understand how arthropathies affect us. By looking at demographics, costs, and social impacts, we can improve life for those with these conditions.
Pathophysiology of Arthropathies
It’s important to know how arthropathies work to treat joint diseases. Arthropathies are conditions that harm joints, causing pain and swelling. They involve complex interactions in the joint.
Joint Structure and Function
A normal joint has articular cartilage, synovium, ligaments, and muscles. The synovium makes synovial fluid, which helps the joint move smoothly. Articular cartilage absorbs shock and helps with movement.
The joint stays healthy when cartilage is made and broken down in balance. If this balance is off, the joint can get damaged.
Disease Mechanisms
Arthropathies come from inflammation, degeneration, and metabolic issues. Inflammatory arthropathies, like rheumatoid arthritis, harm joints through immune attacks.
Degenerative arthropathies, like osteoarthritis, wear down cartilage and bone over time. Metabolic problems, like in gout, cause crystals in the joint, leading to pain and swelling.
“The pathophysiology of arthropathies involves a complex interplay of genetic, environmental, and hormonal factors that ultimately lead to joint damage and dysfunction.”
Progression of Joint Damage
Joint damage in arthropathies can progress differently. Inflammatory diseases cause bone and cartilage loss. Degenerative diseases lead to cartilage loss and bone spurs, causing pain and stiffness.
|
Disease Mechanism |
Characteristics |
Joint Impact |
|---|---|---|
|
Inflammatory |
Immune-mediated inflammation |
Erosion of bone and cartilage |
|
Degenerative |
Gradual wear and tear |
Loss of cartilage, bone spurs |
|
Metabolic |
Crystal deposition |
Inflammation, pain |
Knowing how arthropathies work helps us find better treatments. We can target the root causes of these diseases.
Common Symptoms and Clinical Presentation
Knowing the symptoms of arthropathy is key for early diagnosis and treatment. Arthropathy is a term for many joint disorders. It shows in different ways, affecting patients’ lives greatly.
Physical Manifestations
Arthropathy shows in many ways, affecting one or more joints. Common signs include:
- Joint swelling and redness
- Warmth or tenderness to the touch
- Deformity or misalignment of the joint
- Crepitus or grinding sensation with movement
These signs come from inflammation, degeneration, or other joint problems. How and how much they show can differ a lot.
Pain Patterns and Characteristics
Pain is a big symptom of arthropathy. Its patterns and characteristics help doctors diagnose. The pain can be:
- Acute: Sudden, often very severe
- Chronic: Lasts a long time or keeps coming back
- Inflammatory: Gets worse after rest, better with activity
- Mechanical: Gets worse with activity, better with rest
Knowing the pain’s nature helps find the cause and plan treatment.
Functional Limitations
Arthropathy can make daily tasks hard, affecting work and life quality. Common issues include:
|
Activity |
Common Challenges |
|---|---|
|
Walking or standing |
Pain, stiffness, or instability |
|
Dressing or grooming |
Limited range of motion, pain with movement |
|
Lifting or carrying |
Weakness, pain, or reduced grip strength |
Checking these limitations helps create a detailed treatment plan. It meets the patient’s specific needs and goals.
Major Types of Arthropathies
It’s important to know about the different types of arthropathies. They are various joint disorders with unique causes, symptoms, and treatments.
Inflammatory Arthropathies
Inflammatory arthropathies are marked by joint inflammation. This usually comes from an autoimmune response. Rheumatoid arthritis (RA) is a common example, where the immune system attacks the joints’ lining. This leads to pain, swelling, and serious damage.
Other types include psoriatic arthritis and ankylosing spondylitis. Treatment often includes anti-inflammatory drugs and DMARDs.
Degenerative Arthropathies
Degenerative arthropathies, like osteoarthritis (OA), are due to joint wear and tear. OA is the most common arthritis and affects weight-bearing joints like knees and hips. Symptoms include pain, stiffness, and reduced mobility.
Management strategies include lifestyle changes, physical therapy, and pain relief medications.
Crystal-Induced Arthropathies
Crystal-induced arthropathies happen when crystals form in joints, causing inflammation and pain. Gout is a well-known example, caused by monosodium urate crystals. Another is calcium pyrophosphate deposition disease (CPPD), where calcium pyrophosphate dihydrate crystals build up in joints.
Treatment usually involves medications to reduce inflammation and manage crystal formation.
Infectious Arthropathies
Infectious arthropathies are caused by joint infections, often from bacteria, viruses, or fungi. Septic arthritis is a serious condition that needs quick treatment to avoid joint damage. Symptoms include sudden joint pain, swelling, and fever.
Diagnosis involves joint aspiration and culture. Treatment usually includes antibiotics or antifungal medications, based on the cause.
In conclusion, the main types of arthropathies differ in causes and symptoms. Accurate diagnosis and proper treatment are key to managing these conditions well and improving patient outcomes.
Specialized Forms of Arthropathy
Arthropathy comes in many forms, each with its own challenges. Understanding their causes, symptoms, and treatments is key.
Reactive Arthropathy: Causes and Characteristics
Reactive arthropathy is a condition linked to bacterial infections. It often affects the joints, causing pain and swelling. Treatment aims to fight the infection and ease symptoms.
Diabetic Arthropathy: Mechanisms and Management
Diabetic arthropathy is a diabetes complication caused by nerve damage. It harms joints, usually in the foot or ankle. Managing it involves controlling blood sugar and protecting the joints. Sometimes, surgery is needed to fix the joint.
Neuropathic Arthropathy: The Charcot Joint
Neuropathic arthropathy, or Charcot joint, damages joints due to nerve loss. It causes joints to degenerate, leading to deformity. Early treatment and rest are vital to prevent further damage.
Spondylarthropathy: Spinal Joint Involvement
Spondylarthropathy affects the spine and sacroiliac joints. It causes pain, stiffness, and can fuse vertebrae. Treatment includes medicine, physical therapy, and sometimes surgery to improve life quality.
Diagnosis and Assessment Methods
Diagnosing arthropathies requires a detailed approach. It involves clinical checks, lab tests, and imaging to accurately diagnose and manage joint diseases.
Clinical Evaluation and History Taking
A thorough clinical evaluation is key in diagnosing arthropathies. It starts with a detailed patient history. This helps identify symptoms like pain, stiffness, and limited mobility.
Healthcare providers look at when symptoms started, how long they last, and what they feel like. This helps narrow down possible causes.
Key components of clinical evaluation include:
- Patient history to identify risk factors and symptoms
- Physical examination to assess joint swelling, tenderness, and range of motion
- Assessment of functional limitations and impact on daily activities
Laboratory Tests and Biomarkers
Laboratory tests are vital in diagnosing and differentiating arthropathies. They help find inflammatory markers, autoimmune factors, and biochemical changes linked to joint diseases.
Common laboratory tests include:
- Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) to assess inflammation
- Rheumatoid factor (RF) and anti-citrullinated protein antibody (anti-CCP) for rheumatoid arthritis
- Uric acid levels to diagnose gout
Imaging Techniques and Their Applications
Imaging studies are essential for seeing joint damage and tracking disease progression. They help guide treatment decisions. Different imaging modalities offer unique benefits in diagnosing arthropathies.
Common imaging techniques include:
- X-rays to assess joint damage and bone erosion
- Ultrasound to evaluate soft tissue inflammation and synovitis
- Magnetic Resonance Imaging (MRI) for detailed assessment of joint structures and soft tissues
By combining clinical evaluation, lab tests, and imaging, healthcare providers can accurately diagnose and manage arthropathies. This improves patient outcomes.
Treatment Approaches for Arthropathies
Managing arthropathies requires a mix of treatments. These aim to ease symptoms, slow disease growth, and boost life quality.
Pharmacological Interventions
Medicines are key in treating arthropathies. They include:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Good for cutting pain and swelling.
- Disease-Modifying Antirheumatic Drugs (DMARDs): Help slow disease in inflammatory types.
- Biologic Agents: Target specific inflammation molecules, for a more precise treatment.
- Corticosteroids: Strong anti-inflammatory drugs for quick relief or during flare-ups.
Physical and Occupational Therapy
Physical and occupational therapy are vital in managing arthropathies. They help by:
- Boosting joint mobility and strength.
- Improving daily function.
- Lessening pain with methods like heat, cold, and electrical stimulation.
A good physical therapy plan can greatly enhance life quality for those with arthropathies.
Surgical Options and Considerations
Surgery is an option when other treatments don’t work or when joints are badly damaged. Common surgeries include:
|
Procedure |
Description |
Benefits |
|---|---|---|
|
Joint Replacement |
Replacing damaged joint with prosthetic |
Pain relief, improved function |
|
Synovectomy |
Removing inflamed synovial tissue |
Less inflammation, pain relief |
|
Arthrodesis |
Fusing joint to stop pain |
Permanent pain relief, stability |
Decisions on surgery depend on many factors. These include disease severity, patient health, and expected benefits.
Prevention and Management Strategies
To prevent and manage arthropathies, it’s key to understand the importance of changing risk factors and protecting joints. Good management strategies can greatly improve life quality for those with these conditions.
Risk Factor Modification
Changing risk factors is a big step in preventing arthropathies. Keeping a healthy weight reduces joint stress, regular exercise improves mobility and strength, and avoiding repetitive strain injuries is important.
- Maintaining a Healthy Weight: Excess weight can make joint stress worse, mainly in weight-bearing joints like the knees and hips.
- Regular Exercise: Swimming, cycling, and walking can improve joint function without causing too much strain.
- Avoiding Repetitive Strain: Taking regular breaks and changing tasks can prevent repetitive strain injuries.
Joint Protection Techniques
Protecting joints is key to preventing more damage in those with arthropathies. Using proper body mechanics, avoiding heavy lifting, and using assistive devices when needed are important.
|
Technique |
Description |
Benefit |
|---|---|---|
|
Proper Body Mechanics |
Using correct posture and movement techniques |
Reduces strain on joints |
|
Avoiding Heavy Lifting |
Limiting or avoiding heavy lifting tasks |
Prevents excessive joint stress |
|
Assistive Devices |
Using devices like canes or walkers |
Reduces joint stress and improves mobility |
When to Seek Medical Attention
Knowing when to seek medical attention for arthropathy symptoms is important. Persistent pain, swelling, or trouble moving a joint means it’s time to see a doctor.
Early intervention can greatly impact managing arthropathies. It can slow disease progression and improve outcomes.
Complementary and Alternative Approaches
Along with traditional treatments, approaches like acupuncture, physical therapy, and certain dietary supplements may help some people.
By using these strategies every day, people can better manage their arthropathies and improve their quality of life.
Conclusion: The Future of Arthropathy Research and Care
Understanding arthropathy is key for doctors and patients. Arthropathy covers many joint diseases. This article has explored its roots and types, showing how complex these conditions are.
Research on arthropathy keeps growing, giving us new ways to fight these diseases. As we learn more, we can better treat them. New medicines, physical therapy, and surgery have made a big difference for patients.
The future looks bright for arthropathy research. We might see even better treatments and maybe even cures. It’s vital to keep funding medical research. This is how we’ll make life better for those with these conditions.
FAQ
What does arthropathy mean?
Arthropathy is a term for diseases or disorders that affect the joints. It includes many conditions that harm joint health and function.
What is the difference between arthropathy and arthritis?
Arthropathy is a wider term for any joint disease. Arthritis, on the other hand, usually means inflammation of the joints.
What are the major types of arthropathies?
The main types are inflammatory, degenerative, crystal-induced, and infectious arthropathies. Each has its own causes and characteristics.
What is the pathophysiology of arthropathies?
The pathophysiology involves complex interactions. It includes the joint structure, disease mechanisms, and how joint damage progresses. This varies across different arthropathies.
How are arthropathies diagnosed?
Diagnosis uses clinical evaluation, lab tests, and imaging. These help figure out the specific type and extent of joint disease.
What are the treatment approaches for arthropathies?
Treatments include medicines, physical and occupational therapy, and surgery. They are chosen based on the type and severity of the arthropathy.
Can arthropathies be prevented?
Some risk factors can’t be changed, but prevention and management strategies exist. They include modifying risk factors, protecting joints, and using complementary approaches.
What is reactive arthropathy?
Reactive arthropathy is a type of arthropathy caused by an infection elsewhere in the body. It often affects the joints.
What is diabetic arthropathy?
Diabetic arthropathy refers to joint disorders linked to diabetes. It involves mechanisms related to neuropathy and other diabetes-related complications.
What is neuropathic arthropathy?
Neuropathic arthropathy, also known as Charcot joint, is a condition where joint degeneration occurs due to nerve damage. It’s often associated with diabetes or other neuropathic conditions.
What is spondylarthropathy?
Spondylarthropathy is a group of inflammatory rheumatic diseases. They mainly affect the spine and other joints.
When should I seek medical attention for arthropathy?
Seek medical attention if you have persistent joint pain, swelling, or limited mobility. Early diagnosis and treatment can greatly improve outcomes.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5372453/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























