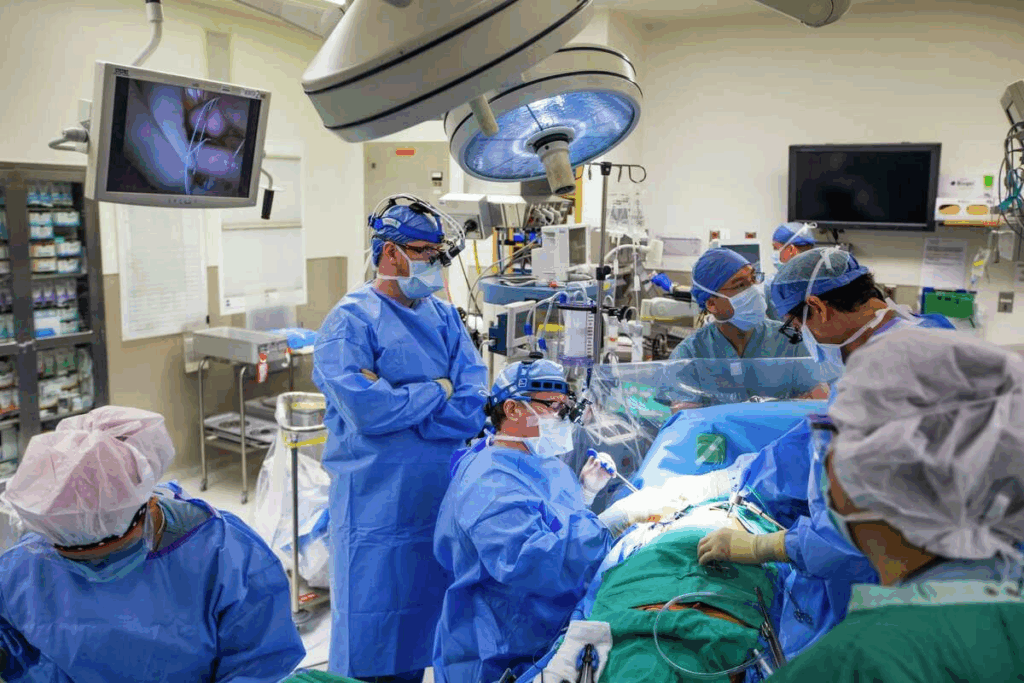
Recovering from a heart attack or surgery can feel overwhelming. But, starting cardiac therapy exercises in Phase 1 while in the hospital greatly improves your future health and life quality.
A dedicated healthcare team will help you with gentle heart rehabilitation exercises. These therapeutic exercises are key to a cardiac exercise program. They help improve your heart health and fitness. Guide to starting cardiac therapy exercises during Phase 1 (inpatient hospital recovery) safely.
Key Takeaways
- Starting cardiac therapy exercises in Phase 1 rehabilitation improves long-term outcomes.
- Gentle exercises reduce the risk of future cardiac events.
- A dedicated healthcare team guides patients through the rehabilitation process.
- Cardiac exercise programs are designed to improve heart health and overall fitness.
- Phase 1 rehabilitation is a critical step in the recovery process.
What Happens During Phase 1 Cardiac Rehabilitation
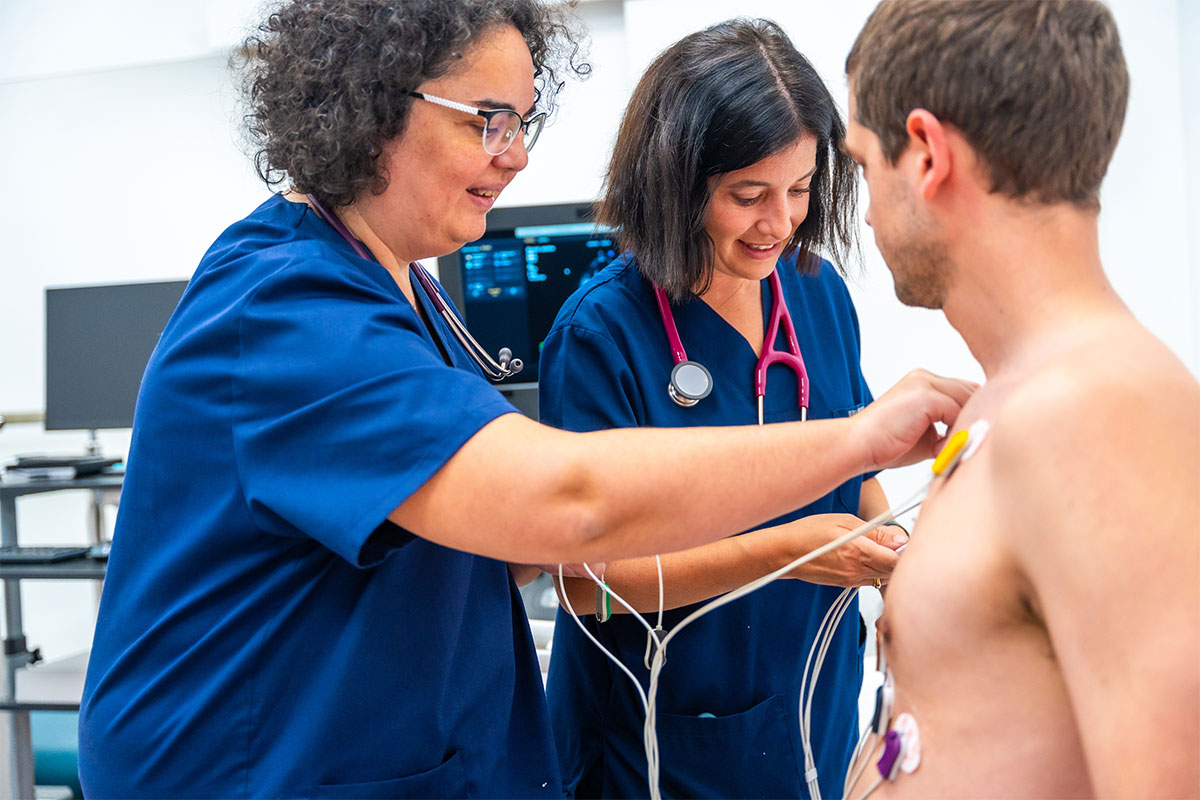
The journey to recovery begins with Phase 1 cardiac rehabilitation. It starts while the patient is in the hospital. This phase is key for setting the stage for recovery.
The Acute Inpatient Recovery Period
During this time, patients are watched closely by doctors and nurses. It’s a critical period to avoid complications and make sure the patient is ready to go home.
Early mobilization is important here. It helps prevent muscle loss and keeps blood flowing. Patients do gentle exercises and move around as they can.
Medical Supervision and Monitoring
Medical care is top priority in Phase 1. Doctors keep an eye on heart rate and blood pressure. This makes sure the patient is safe while being active.
They also watch how the patient reacts to exercise. This helps adjust the plan to keep it safe and effective.
Monitoring Aspect | Description | Importance |
Heart Rate | Monitoring heart rate response to exercise | Ensures safe exercise intensity |
Blood Pressure | Tracking blood pressure changes during activity | Prevents hypertensive responses |
Symptoms | Observing for signs of distress or discomfort | Early detection of possible problems |
Setting Realistic Recovery Goals
Setting realistic goals is vital in Phase 1. Doctors and patients work together to set goals that are reachable. This helps keep the patient motivated and moving forward.
These goals are made just for the patient. They take into account the patient’s health, abilities, and overall situation. This makes the rehabilitation more personal.
Benefits of Early Cardiac Therapy Exercises

Starting cardiac therapy exercises early in recovery greatly improves patient outcomes. These exercises help patients recover faster and feel better overall. They are a key part of a good rehabilitation plan.
Preventing Complications from Prolonged Bed Rest
Early cardiac therapy exercises prevent problems from too much bed rest. Patients at risk of deep vein thrombosis, muscle loss, and heart function decline. Early movement helps avoid these issues, keeping muscles strong and heart healthy.
Studies show that exercise training can make walking much better. It’s even better than just medical treatment alone. This shows how important starting exercise early is.
Improving Circulation and Oxygen Delivery
These exercises also boost blood flow and oxygen to body tissues. They make the heart work better and improve blood circulation. This leads to better heart function, helping patients recover faster.
Building Confidence for Recovery
Starting exercises early also boosts patient confidence. Seeing physical improvements makes patients believe in their recovery. This mental support is key to their recovery journey.
Benefits | Description | Impact on Recovery |
Preventing Complications | Reduces risks associated with prolonged bed rest | Decreases risk of DVT, muscle atrophy |
Improving Circulation | Enhances blood flow and oxygen delivery | Improves cardiovascular function |
Building Confidence | Empowers patients through visible progress | Enhances psychological well-being and active participation in recovery |
Cardiac rehab aims to reduce stress from heart disease, lower death risk, and improve heart function. Early cardiac therapy exercises help achieve these goals. This leads to better patient outcomes and a better quality of life.
Medical Clearance and Safety Protocols
Starting cardiac therapy exercises needs a full medical check first. This step is key to make sure patients are fit for physical activity. It also helps spot any risks or problems.
Pre-Exercise Assessment Requirements
Before starting cardiac rehab, a detailed check is needed. This check looks at the heart’s health, how well the patient can exercise, and makes a plan just for them. It includes looking at the patient’s health history and any heart issues they’ve had.
We also do tests like ECGs and stress tests. These help figure out if the patient is ready for exercise. They help make the rehab program fit the patient’s needs.
Vital Sign Parameters for Safe Activity
Keeping an eye on vital signs is key in cardiac rehab. We watch heart rate, blood pressure, and oxygen levels closely. This makes sure they stay safe during exercise.
We check the heart rate to make sure it doesn’t get too high or low. We also watch blood pressure to avoid it getting too high or low.
When to Stop Exercising Immediately
It’s important for patients to know when to stop exercising right away. Signs like chest pain, severe shortness of breath, dizziness, or palpitations mean it’s time to stop.
If these symptoms happen, we tell patients to stop and rest. Sometimes, they need to see a doctor right away. Spotting these signs early helps keep the rehab safe and effective.
Essential Cardiac Therapy Exercises for Phase 1
Starting Phase 1 of cardiac rehabilitation means learning about safe and effective exercises. These exercises help your heart recover and get stronger. They also improve your overall health without putting too much strain on you.
Gentle Range of Motion Activities
Gentle exercises are key in Phase 1. They keep your muscles flexible, prevent stiffness, and boost blood flow. Here are some examples:
- Seated marching: This is marching in place while sitting. It’s great for your legs and blood circulation.
- Ankle pumps and rotations: These simple moves help prevent blood clots and improve ankle flexibility.
- Arm raises: These help keep your shoulders moving smoothly.
Healthcare professionals watch over you to make sure you do these exercises right and safely.
Progressive Mobility Techniques
Progressive mobility means slowly increasing the intensity and time of your exercises. This is based on how well you’re doing and how you feel. You might start with:
- Short walks in hallways: You’ll walk a little bit at first and then more as you get better.
- Transferring from bed to chair: This helps build strength and balance.
- Gradually increasing sitting time: Sitting for longer helps you get more endurance.
Progressive mobility is tailored to your specific needs. This ensures the exercises are safe and effective for you.
Customizing Exercises to Your Condition
It’s important to tailor exercises to your heart condition, health, and any limitations. Healthcare providers look at:
- Current health status
- Recovery progress
- Any comorbidities or physical limitations
This helps create a plan that’s right for you. It balances rehabilitation with avoiding too much strain.
Bed-Based Exercise Techniques
We offer bed-based exercises as part of our cardiac rehab program. These exercises help keep blood flowing and prevent muscle loss. They are key for patients in Phase 1, helping them start their recovery safely.
Ankle Pumps and Rotations
Ankle pumps are a simple start. Patients move their ankles up and down to boost blood flow. This helps avoid blood clots and leg swelling.
Ankle rotations also play a role. Patients rotate their ankles in circles, first one way and then the other. This keeps ankles flexible and mobile.
To perform ankle pumps:
- Lift your toes up towards your head, then down towards the bed.
- Repeat this motion for 10-15 repetitions.
- Rest, then repeat the exercise.
Leg Slides and Gentle Knee Bends
Leg slides are another effective exercise. Patients slide one heel along the bed towards their buttocks, then back. This keeps knees flexible and strengthens leg muscles.
To perform leg slides:
- Slowly slide one heel towards your buttocks, keeping your heel on the bed.
- Return your leg to the starting position.
- Repeat with the other leg.
Upper Body Circulation Exercises
Exercises for the upper body improve blood flow and prevent stiffness. Arm raises help keep shoulders mobile. Squeezing and releasing hands also boosts circulation and reduces swelling.
To perform arm raises:
- Lift one arm straight out to the side, then above your head.
- Lower your arm back to your side.
- Repeat with the other arm.
These exercises are vital for Phase 1 cardiac rehab patients. They help patients recover better. Our team ensures these exercises are done safely and right.
Seated Cardiac Rehabilitation Activities
As patients move forward in their cardiac rehab, they start doing seated activities. These are key for recovery. They help build strength, improve blood flow, and boost heart health.
Proper Seated Posture for Heart Health
Keeping the right seated posture is vital for cardiac rehab patients. Good posture lessens heart strain and aids breathing. Sit with your back straight, shoulders down, and feet flat or on a footrest.
Chair Marching Techniques
Chair marching is a simple yet powerful exercise. It involves lifting legs off the floor, one at a time, like marching. This boosts blood flow and strengthens legs.
To do chair marching, sit straight and hold armrests for support. Lift one leg straight up, then march in place a few times. Switch to the other leg.
Torso and Arm Strengthening
Torso and arm strengthening exercises can also be done seated. They enhance muscle strength and endurance. Try arm raises, shoulder rolls, and gentle torso twists.
Do these exercises at a pace you’re comfortable with. Avoid any pain or discomfort. Breathe smoothly to keep oxygen flowing.
Adding these seated activities to your rehab plan can greatly improve heart health. Always follow your healthcare team’s advice to do these exercises safely and right.
Standing and Walking in Phase 1 Recovery
Standing and walking are key steps in Phase 1 recovery. They help patients get stronger and move better. These activities are important for a full recovery and getting ready for more challenging rehab phases.
Safe Transition from Sitting to Standing
Going from sitting to standing is a big step in rehab. To do it safely:
- Start by sitting on the edge of a bed or chair with feet on the floor.
- Lean forward a bit and push up using armrests or the bed.
- Stand up slowly to avoid getting dizzy and keep your balance.
Having someone nearby to help is very important. They can offer support and help you sit back down if needed.
Hallway Walking Progression
Hallway walking is a big part of Phase 1 recovery. It helps blood flow and makes legs stronger. The goal is to increase the distance gradually:
- Begin with short walks, like 10-15 feet, and then walk further as you get better.
- Watch the patient’s heart rate, blood pressure, and comfort while and after walking.
- Encourage them to walk at a pace they’re comfortable with and rest when needed.
Using Assistive Devices When Needed
Some people need help with walking and standing. Assistive devices like:
- Walkers offer extra stability and support.
- Canes help with balance and ease leg strain.
These tools make walking and standing safer and more effective. Choosing the right device is key for the patient’s needs and abilities.
Monitoring Your Body During Cardiac Therapy Exercises
Starting cardiac therapy exercises means watching how your body reacts. This is key for a safe and effective recovery. Keeping an eye on your vital signs and physical condition helps spot any problems early.
Heart Rate and Blood Pressure Guidelines
It’s important to track your heart rate and blood pressure during these exercises. Your doctor will tell you what levels are safe for you. Your heart rate should not go too high, based on your age and health.
Also, watch your blood pressure to make sure it stays safe while you exercise. Your healthcare team will tell you what’s okay for your situation.
Using the Rate of Perceived Exertion Scale
The Rate of Perceived Exertion (RPE) Scale helps you know how hard you’re working. It goes from 6 (no effort) to 20 (max effort). For most exercises, aiming for an RPE of 11-14 is best.
The RPE Scale lets you feel how hard you’re working without always checking your heart rate or blood pressure. It’s based on how you feel physically.
Recognizing Normal vs. Concerning Symptoms
It’s important to know the difference between normal and concerning symptoms. Normal signs might include a slightly faster heart rate and breathing. These should go back to normal when you rest.
Signs that are not normal include chest pain, severe shortness of breath, dizziness, or palpitations. If you feel any of these, stop right away and tell your doctor.
By watching how your body reacts and knowing what’s normal versus concerning, you can safely do cardiac therapy exercises. This way, you can get the best results.
Breathing Techniques for Cardiac Patients
Effective breathing techniques are key for managing stress and improving heart health in cardiac patients. By adding these techniques to their daily routine, people can greatly improve their recovery and well-being.
Diaphragmatic Breathing Practice
Diaphragmatic breathing, or belly breathing, uses the diaphragm muscle. It’s more efficient than shallow chest breathing and can lower stress and blood pressure. Here’s how to do it:
- Lie on your back with your knees bent and head supported.
- Place one hand on your belly and the other on your chest.
- Inhale slowly through your nose, letting your belly rise while your chest stays steady.
- Exhale slowly through your mouth, letting your belly fall.
Regular practice of diaphragmatic breathing can improve lung capacity and reduce stress and anxiety symptoms.
Breath-Movement Coordination
Linking breathing with movement can make cardiac rehabilitation exercises more effective. This involves breathing in sync with your movements, making exercises more harmonious and efficient. For example, inhale for a few steps and exhale for the same number of steps while walking.
“Breathing is the bridge between the body and the mind,” and linking it with movement can boost the benefits of cardiac rehabilitation exercises.
Reducing Cardiac Stress Through Breathing
Breathing techniques are vital for reducing cardiac stress. By practicing controlled breathing, cardiac patients can lower their heart rate and blood pressure. This reduces the heart’s workload. Techniques like paced breathing, where you breathe at a controlled rate, are very effective.
“Teaching cardiac patients breathing techniques is a vital part of their rehabilitation program, helping them manage stress and improve their heart health.”
By mastering these breathing techniques, cardiac patients can actively participate in their recovery. This improves their heart health and lowers the risk of future cardiac events.
Psychological Aspects of Beginning Heart Rehabilitation
Starting cardiac rehabilitation means facing the mental side of recovery. It’s not just about getting better physically. It’s also about building mental strength and feeling emotionally well.
Managing Fear and Anxiety About Exercise
One big challenge in cardiac rehab is feeling scared or anxious about exercising. People worry it’s not safe after a heart issue. We tell our patients that exercise is key to getting better, and it’s safe with the right help.
We suggest starting with easy exercises and slowly getting more active. This way, patients feel more confident and less worried about moving their bodies.
Setting Positive Mental Frameworks
Having a positive mindset is key for a good rehab journey. We help patients set achievable goals and celebrate their small wins. This keeps them motivated and hopeful about getting better.
By focusing on their progress and steps towards healing, patients can stay optimistic. This boosts their physical recovery and overall happiness.
Building a Support System for Recovery
A strong support network is essential for cardiac rehab. We encourage patients to have family, friends, and support groups around them. These people offer emotional support and encouragement.
Having a support system greatly helps with mental and emotional healing. It provides a safety net and keeps patients positive about their rehab.
In summary, the mental side of cardiac rehabilitation is just as important as the physical. By tackling fear and anxiety, setting positive goals, and having a support system, patients can do well in their rehab journey.
Transitioning to Phase 2 Cardiac Rehabilitation
When patients get better, they move to Phase 2 cardiac rehab. This is a big step in their healing. It’s a more detailed and intense program, usually done outside of the hospital.
Discharge Criteria and Home Preparation
Before starting Phase 2, patients must meet certain discharge criteria. They need to have stable vital signs, manageable pain, and be able to do daily tasks without too much effort. Doctors also check if patients understand their health and can follow a home workout plan.
Getting ready for home is also important. Patients learn to make their home safe, like removing tripping hazards and making sure they can easily get to what they need. They also get tips on continuing exercise safely and effectively at home.
Outpatient Rehabilitation Planning
Outpatient rehabilitation planning is key in Phase 2. It involves making a detailed exercise plan that’s tougher than Phase 1. The goal is to boost heart health, strength, and flexibility. Patients work with their healthcare team to plan regular visits and track their progress.
The program is made just for the patient. It might include group workouts, personal training, and classes on heart health, eating right, and managing stress.
Continuing Exercise Between Phases
Continuing exercise between phases is very important. It helps keep progress going and makes the move to the next phase smoother. Patients are told to stick to their workout plan, slowly adding more intensity and time as their doctors suggest.
It’s key to remember that continuing exercise is not just for physical healing. It’s about making a lasting change to support heart health. Regular exercise can help manage risks, improve health, and make life better overall.
Conclusion
Cardiac therapy exercises are key in cardiac rehabilitation, mainly in Phase 1. They help patients recovering from heart issues. These exercises prevent complications, improve blood flow, and boost confidence.
A good cardiac rehab program includes exercise, lifestyle changes, and support for the mind. Gentle exercises, progressive mobility, and breathing help patients move through rehab safely.
In conclusion, cardiac rehab is more than just physical recovery. It also helps with mental health. By focusing on therapy exercises and following a rehab plan, patients can get better and live better lives.
FAQ
What is the primary goal of cardiac therapy exercises during Phase 1 rehabilitation?
The main goal is to help patients recover after heart events. They do this by improving heart health and fitness through gentle exercises and medical supervision.
What happens during the acute inpatient recovery period in Phase 1 cardiac rehabilitation?
In this period, patients are watched closely by healthcare teams. They start with gentle exercises to avoid problems from too much bed rest and to improve blood flow.
Why is medical clearance important before starting cardiac therapy exercises?
Medical clearance makes sure patients are okay to start exercising. It lets healthcare teams check their health and give them personalized advice.
What are some essential cardiac therapy exercises for Phase 1?
Important exercises include gentle movements, progressive mobility, ankle pumps, leg slides, and upper body exercises. These help prevent getting weaker and improve blood flow.
How can patients monitor their body during cardiac therapy exercises?
Patients can watch their heart rate and blood pressure. They can also use the Rate of Perceived Exertion Scale and know when to stop to stay safe.
What breathing techniques are beneficial for cardiac patients?
Diaphragmatic breathing and coordinating breath with movement can lower heart stress. It helps keep the heart healthy.
How can patients manage fear and anxiety about exercise during cardiac rehabilitation?
Patients can handle fear and anxiety by setting positive thoughts, building a support network, and getting help from healthcare teams.
What is the purpose of transitioning to Phase 2 cardiac rehabilitation?
The goal is to keep improving in an outpatient setting. It focuses on more challenging exercises and making lasting lifestyle changes.
How can patients prepare for Phase 2 cardiac rehabilitation?
Patients can get ready by meeting the necessary criteria, making their home safe, and planning for outpatient care.
What is the importance of continuing exercise between phases of cardiac rehabilitation?
Keeping up with exercise between phases helps the transition smoothly. It keeps the progress made in the previous phase, helping with recovery and heart health.
What are some cardiovascular exercise programs that can be done at home?
At-home exercises include walking, chair exercises, and low-impact activities. These promote heart health and are tailored to each patient’s needs.
How can patients increase their cardio recovery?
Patients can boost their cardio recovery by slowly increasing their exercises, listening to their body, and getting advice from healthcare teams.
References
National Health Service (NHS). Evidence-Based Medical Guidance. Retrieved fromhttps://www.nhs.uk/conditions/cardiac-rehabilitation/



































