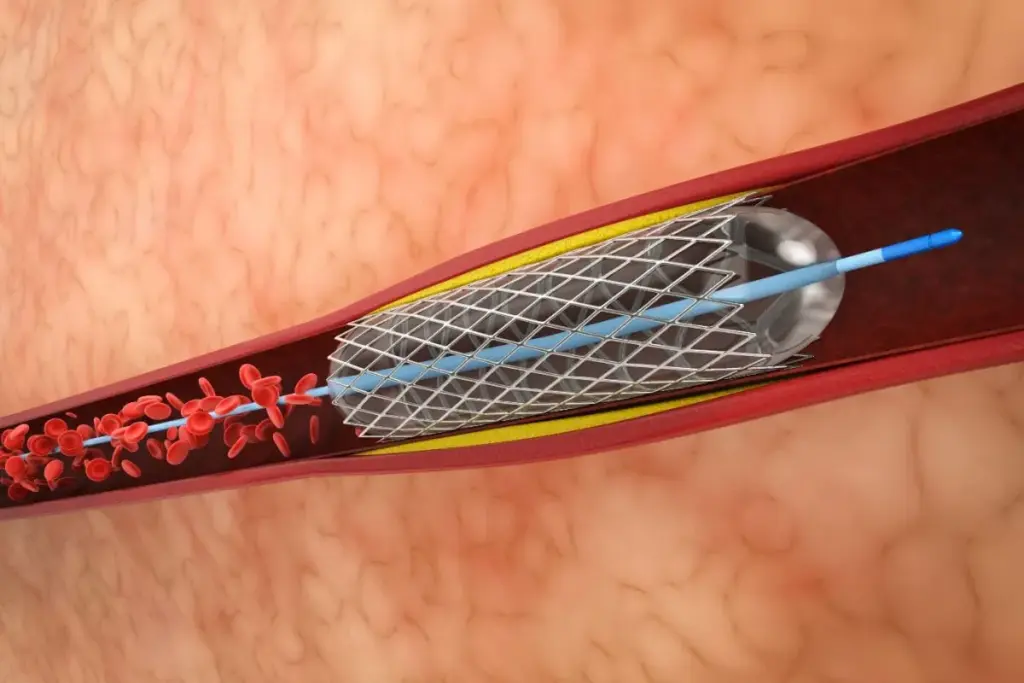
Nearly 500,000 people worldwide are diagnosed with aortic valve stenosis each year. This condition makes the heart’s aortic valve narrow, blocking blood flow. While surgery used to be the only option, new medical technologies offer alternatives.
Right now, aortic stenosis medicine helps manage symptoms but can’t cure it. But, procedures like Transcatheter Aortic Valve Replacement (TAVR) are showing great promise. They treat the condition without needing open-heart surgery.
Key Takeaways
- TAVR is a minimally invasive alternative to open-heart surgery for treating aortic stenosis.
- Current aortic stenosis medicine can manage symptoms but not cure the condition.
- Treating aortic valve stenosis without surgery can lower complication risks and ease recovery.
- Minimally invasive procedures are becoming increasingly popular for heart valve replacement.
- Patients with heart disease may benefit from non-surgical treatment options.
Understanding Aortic Stenosis: Causes and Progression
It’s important to know about aortic stenosis to manage it well. This condition affects about 20% of older adults in the U.S. It’s a serious valve problem.
What Happens in Aortic Valve Stenosis
Aortic valve stenosis happens when the aortic valve gets narrower. This blocks blood flow from the heart. It makes the heart work harder, which can lead to heart failure if not treated.
Common Causes of Aortic Valve Narrowing
Age, congenital heart defects, and calcium buildup are common causes. These factors make the valve stiff and narrow over time.
How Aortic Stenosis Progresses Over Time
Aortic stenosis gets worse over time if not treated. Symptoms like chest pain, shortness of breath, and fainting can appear. These symptoms can really affect your life.
Managing aortic stenosis means knowing its causes and how it progresses. Recognizing symptoms early helps. This way, you can get the right aorta stenosis treatment and improve your chances.
Diagnosing Aortic Stenosis: From Mild to Severe
Healthcare providers use physical exams and advanced tests to diagnose aortic stenosis. This method ensures an accurate diagnosis. It’s key for finding the best aortic stenosis and treatment plan.
Diagnostic Tests and Procedures
Doctors often suspect aortic stenosis through physical exams. They confirm it with transthoracic echocardiography. This test lets them check the heart’s size and function and measure stenosis.
- Echocardiography to evaluate heart valve function
- Cardiac catheterization to assess coronary artery disease
- Electrocardiogram (ECG) to check for heart rhythm abnormalities
These tests give a full view of the heart’s condition. They help doctors figure out the aortic valve stenosis treatment needed.
Grading Severity: Mild, Moderate, and Severe Stenosis
The severity of aortic stenosis is graded by the valve area and blood flow velocity. The grades are:
- Mild Stenosis: Valve area > 1.5 cm²
- Moderate Stenosis: Valve area between 1.0-1.5 cm²
- Severe Stenosis: Valve area
Knowing the severity is vital for choosing the right aortic stenosis and treatment plan.
Traditional Surgical Approaches to Aortic Stenosis
Treating aortic stenosis often means replacing the valve surgically. This method is key for severe cases, helping those with tight valves.
Open Heart Surgery for Valve Replacement
Open-heart surgery, or surgical aortic valve replacement (SAVR), is a common treatment. It swaps the old valve for a new one, mechanical or bioprosthetic. In 2020, the American College of Cardiology reported 57,626 SAVR surgeries in the U.S.
Risks and Recovery Associated with Surgical Intervention
SAVR is effective but comes with big risks like bleeding, infection, and stroke. Recovery takes weeks, with hospital and rehab time needed. Yet, many find the surgery’s benefits worth the risks, improving their life and survival chances.
|
Aspect |
Open Heart Surgery (SAVR) |
|---|---|
|
Procedure Frequency (2020) |
57,626 (US) |
|
Risks |
Bleeding, Infection, Stroke |
|
Recovery Time |
Several Weeks |
With new tech, treatments like TAVR are gaining ground. But SAVR is vital for many, like those with complex valve disease or other heart issues needing surgery.
Minimally Invasive Alternatives to Open Heart Surgery
Minimally invasive procedures are changing how we treat aortic stenosis. They offer safer and more effective ways to treat this condition. These new methods help patients recover faster and face fewer risks than traditional surgery.
Transcatheter Aortic Valve Replacement (TAVR)
Transcatheter Aortic Valve Replacement (TAVR) is a new way to fix aortic valve stenosis without major surgery. TAVR uses a thin, flexible tube called a catheter to replace the damaged valve. It’s great for patients at high risk for complications from open heart surgery.
This method avoids opening the chest, lowering risks of infection and bleeding. The TAVR procedure is done under local anesthesia. Patients usually stay in the hospital less time than with traditional surgery.
Recovery times vary, but many patients see big improvements in symptoms and quality of life.
Balloon Valvuloplasty Procedures
Balloon valvuloplasty is a minimally invasive procedure for moderate aortic stenosis. It uses a balloon catheter to widen the narrowed valve. Though less common for adults, it’s an option for some patients.
Recovery and Outcomes Compared to Open Surgery
TAVR and balloon valvuloplasty have shorter recovery times than open heart surgery. Patients feel less pain and can get back to normal activities sooner. TAVR has shown to improve outcomes for severe aortic stenosis patients, including lower mortality rates and better quality of life.
In summary, TAVR and balloon valvuloplasty are transforming aortic stenosis treatment. They offer effective, less invasive options. These procedures are improving patient outcomes and reducing risks from traditional surgery.
Aortic Stenosis Medicine: Pharmaceutical Treatment Options
Managing aortic stenosis often involves a multi-faceted approach. This includes using various medications to alleviate symptoms and improve quality of life. These medications cannot cure the condition but play a key role in controlling symptoms and supporting heart health.
Statins and Lipid-Lowering Medications
Statins are commonly prescribed to patients with aortic stenosis. They help manage cholesterol levels and slow the progression of atherosclerosis. This can contribute to the narrowing of the aortic valve. By reducing LDL cholesterol, statins help decrease the risk of heart disease. It’s important to note that statins do not directly affect the stenosis itself but are used to manage associated cardiovascular risk factors.
Blood Pressure Management Medications
Managing blood pressure is critical for patients with aortic stenosis. Medications like ACE inhibitors, beta-blockers, and diuretics may be prescribed. These medications help relax blood vessels, reduce heart rate, or eliminate excess fluid. This alleviates some of the strain on the heart.
Heart Failure Medications for Symptom Control
In cases where aortic stenosis leads to heart failure, specific medications can help manage symptoms. These may include diuretics to reduce fluid buildup and medications that improve the heart’s pumping efficiency. By controlling heart failure symptoms, these medications can significantly improve a patient’s quality of life.
Anticoagulants and Antiplatelets
Anticoagulants and antiplatelet drugs may be prescribed to patients with aortic stenosis. This is often the case if they have a mechanical valve or atrial fibrillation. These medications help prevent blood clots from forming on the valve or elsewhere in the heart. This reduces the risk of stroke and other thromboembolic events.
Limitations of Medication-Only Approaches
While medication is vital for managing aortic stenosis, it is not a substitute for surgery in severe cases. For many patients, surgery or transcatheter aortic valve replacement (TAVR) may be necessary. This is to restore normal valve function and improve survival.
Lifestyle Modifications for Aortic Stenosis Management
Lifestyle changes are key in managing aortic stenosis. They improve quality of life and overall health. By making smart choices, people can manage their condition better and slow its growth.
Dietary Recommendations and Restrictions
Eating a heart-healthy diet is vital for those with aortic stenosis. It means avoiding foods high in saturated fats, cholesterol, and sodium. Increasing fruits, vegetables, and whole grains helps manage weight and blood pressure. It’s also good to limit alcohol.
- Focus on whole, unprocessed foods like vegetables, fruits, and whole grains.
- Choose lean protein sources and low-fat dairy products.
- Limit foods high in salt, sugar, and unhealthy fats.
Safe Exercise Guidelines for Valve Disease Patients
Regular exercise is good, but it must be safe and right for your condition. Low-impact activities like walking, cycling, or swimming are often suggested. Always talk to a healthcare provider before starting or changing your exercise routine.
Stress Management and Mental Health Support
Chronic stress can harm heart health. So, managing stress is key in aortic stenosis care. Meditation, yoga, or deep breathing exercises can help lower stress. Also, getting help from mental health experts or support groups can offer emotional support and coping strategies.
When Non-Surgical Approaches Are Not Enough: Indicators for Intervention
At first, treatment for aortic stenosis might not need surgery. But, there are signs that show when surgery is needed. Knowing these signs is key to managing the condition well.
Warning Signs That Surgery May Be Necessary
Certain symptoms and test results can mean non-surgical methods won’t work anymore. Look out for worsening symptoms like chest pain, shortness of breath, or fainting. Also, a very narrow aortic valve and signs of heart failure are red flags. In these cases, transcatheter aortic valve replacement (TAVR) or balloon valvuloplasty might be the next step.
Risk Assessment for Delaying Surgical Intervention
Waiting too long for surgery can harm patient outcomes. A detailed risk assessment is vital to decide when to operate. This assessment looks at the aortic stenosis’s severity, other heart issues, and the patient’s health.
Aortic Stenosis Life Expectancy Without Surgery
The outlook for those with aortic stenosis not getting surgery varies. It depends on how severe their condition is. Aortic stenosis gets worse over time if not treated.
People with mild aortic stenosis might live for years without big problems. But, once symptoms show up or it gets worse, the outlook is not as good.
Prognosis for Different Severity Levels
The severity of aortic stenosis greatly affects life expectancy without surgery. Studies have found:
- Those with mild aortic stenosis might live a normal life, but need regular check-ups.
- People with moderate aortic stenosis are at higher risk of symptoms and need closer watch.
- Severe aortic stenosis has a worse outlook, with a high risk of death within a few years without surgery.
|
Severity Level |
Typical Life Expectancy Without Surgery |
Symptoms and Complications |
|---|---|---|
|
Mild |
Generally normal, with close monitoring |
Few or no symptoms |
|
Moderate |
Variable, often requiring close surveillance |
Possible development of symptoms such as chest pain or shortness of breath |
|
Severe |
Significantly reduced, often a few years |
High risk of heart failure, arrhythmias, and sudden death |
Quality of Life Considerations with Non-Surgical Management
For those with aortic stenosis not getting surgery, managing symptoms is key. This includes taking medicine, making lifestyle changes, and seeing a doctor regularly.
Transcatheter Aortic Valve Replacement (TAVR) is a good option for many. It offers better results and quicker recovery. But, its long-term effects are being studied, showing promising results for 3- and 5-year outcomes.
Dealing with aortic stenosis without surgery needs a full plan. It includes managing symptoms, making lifestyle changes, and watching how the condition changes.
Conclusion: Making Informed Decisions About Aortic Stenosis Treatment
Treating aortic valve stenosis without surgery is becoming more common. Procedures like Transcatheter Aortic Valve Replacement (TAVR) are less invasive than open-heart surgery. This makes recovery shorter and easier for many patients.
There are many ways to treat aortic stenosis, from medication to minimally invasive procedures. It’s important to understand these options to make informed choices about managing the condition.
Patients can work with their healthcare providers to find the best treatment. This involves considering the severity of the stenosis, overall health, and personal preferences. By doing so, individuals can actively manage their condition and improve their quality of life.
FAQ
Can a heart valve be replaced without open heart surgery?
Yes, a procedure called Transcatheter Aortic Valve Replacement (TAVR) is a less invasive option. It’s an alternative to traditional open heart surgery.
What are the common treatments for aortic stenosis?
Treatments for aortic stenosis include medication and lifestyle changes. For severe cases, surgical options like TAVR or open heart surgery are considered.
How is aortic stenosis diagnosed?
Doctors use tests like echocardiograms and electrocardiograms to diagnose aortic stenosis. Cardiac catheterization also helps determine the condition’s severity.
What are the risks associated with surgical intervention for aortic stenosis?
Surgical risks include bleeding, infection, stroke, and reactions to anesthesia. These are serious complications to consider.
Can lifestyle modifications help manage aortic stenosis?
Yes, making dietary changes, exercising safely, and managing stress can help manage aortic stenosis. These changes can improve your quality of life.
What are the limitations of relying solely on medication to manage aortic stenosis?
Medication can manage symptoms but can’t cure aortic stenosis. For severe cases, surgery is often necessary.
How does the severity of aortic stenosis impact life expectancy without surgery?
Severe aortic stenosis can significantly reduce life expectancy without surgery. The prognosis is poorer for severe cases.
What are the warning signs that surgery may be necessary for aortic stenosis?
Symptoms like chest pain, shortness of breath, and fainting may indicate the need for surgery. Diagnostic tests also play a role in determining this.
Can aortic stenosis be managed in elderly patients?
Yes, elderly patients can manage aortic stenosis with medication, lifestyle changes, and procedures like TAVR. Their overall health and risk factors are considered.
What is the role of statins in managing aortic stenosis?
Statins help manage cholesterol levels and slow atherosclerosis progression. They don’t directly treat the valve narrowing, though.
How does aortic sclerosis differ from aortic stenosis?
Aortic sclerosis is when the valve thickens or calcifies but doesn’t narrow much. Aortic stenosis involves significant narrowing of the valve opening.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC6519423/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News






























