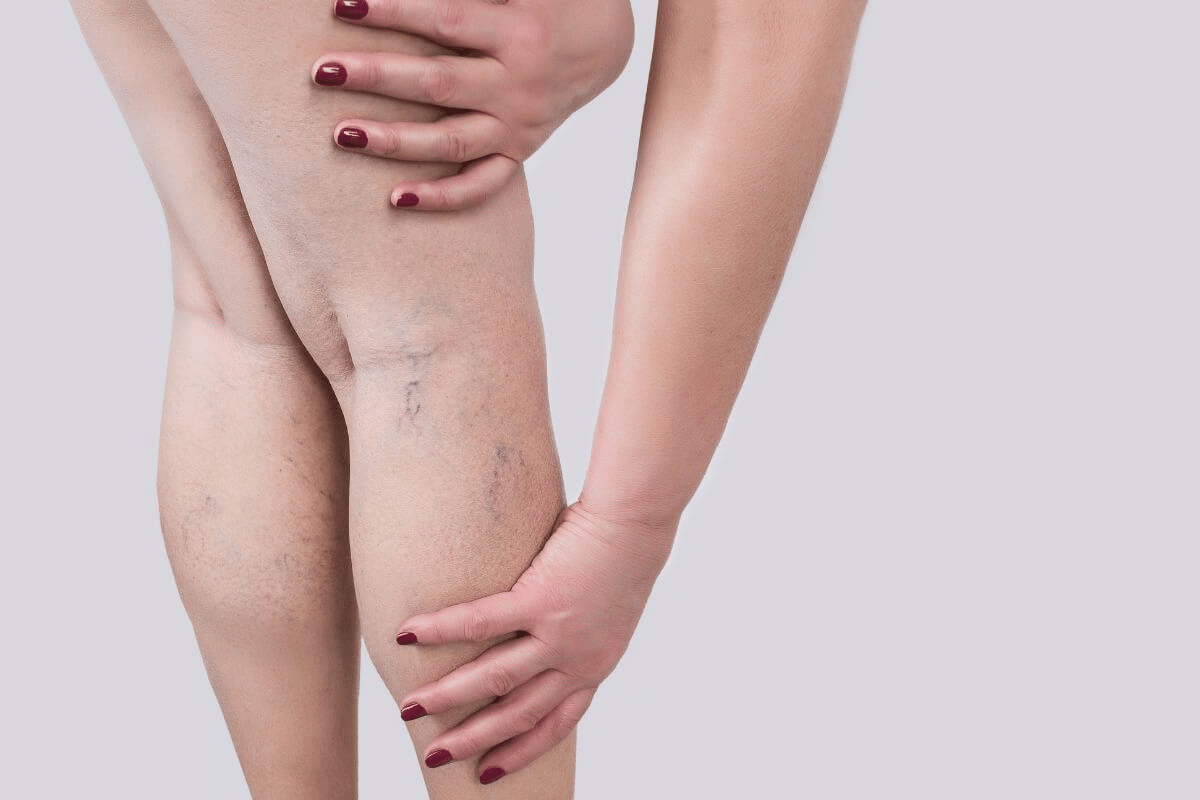
Answering are varicose veins dangerous (usually not, but can lead to complications) and detailing the associated risks. Varicose veins are common and affect many people. They are often seen as just a cosmetic issue. But, they can also pose health risks.
Understanding these risks is key to keeping you healthy. At Liv Hospital, we aim to give you the right medical info and top-notch care.
Experts say varicose veins are usually not dangerous. But, ignoring them can cause problems. It’s important to know the risks and get the right medical help.
Key Takeaways
- Varicose veins can lead to complications if not treated properly.
- Understanding the risks associated with varicose veins is key for long-term health.
- Seeking medical care is essential for managing varicose veins effectively.
- Liv Hospital provides world-class care for patients with varicose veins.
- Being informed about varicose veins helps in making better health decisions.
Understanding Varicose Veins

Varicose veins are a sign of problems in the venous system. They can cause discomfort and even more serious issues.
What Are Varicose Veins?
Varicose veins are big, twisted veins under the skin, often in the legs. They happen when vein valves get weak or damaged. This makes blood pool and veins get big and twisted.
The valves in the veins stop blood from flowing backward. If these valves fail, blood builds up. This makes veins stretch and become varicose.
How and Why They Develop
Varicose veins come from genetics, environment, and lifestyle. Genetics are a big factor, with family history playing a role.
Other things that help varicose veins develop include:
- Aging
- Prolonged standing or sitting
- Obesity
- Pregnancy
|
Risk Factor |
Description |
Impact on Varicose Veins Development |
|---|---|---|
|
Aging |
Wear and tear on vein valves |
Increased likelihood of valve failure |
|
Prolonged Standing/Sitting |
Increased pressure on veins |
Higher risk of blood pooling |
|
Obesity |
Additional pressure on veins |
Increased risk of varicose veins |
Knowing these factors helps prevent and treat varicose veins. By tackling the root causes, people can lower their risk and manage symptoms.
The Prevalence of Varicose Veins
It’s important to know how common varicose veins are. They are a common problem that affects many people around the world. These veins are enlarged and twisted, usually found in the legs.
Statistics and Demographics
About 30% of people have varicose veins. Women and those with a family history are more likely to have them. In the U.S., over 23 million adults have varicose veins.
Some groups are more likely to get varicose veins. Women are more at risk because of hormonal changes. People who stand or sit a lot for work are also at higher risk.
Common Risk Factors
Several things can increase your chance of getting varicose veins. Genetics are a big factor, as is age. As you get older, your veins wear out more.
- Family history of varicose veins
- Age
- Gender (female)
- Obesity
- Prolonged standing or sitting
- Pregnancy
Knowing these risk factors helps prevent and treat varicose veins. Doctors can suggest changes to lower your risk. This way, you can avoid getting varicose veins.
Common Symptoms and Warning Signs
It’s important to know the signs of varicose veins early. These symptoms can range from mild to severe pain and swelling.
Physical Manifestations
The signs of varicose veins are often easy to spot. Look out for:
- Visible, twisted, or bulging veins
- Swelling in the legs, ankles, or feet
- Skin discoloration around the affected veins
- Ulcerations or sores in severe cases
Visible veins are a clear warning sign. If you see these signs, think about varicose veins.
Pain and Discomfort Levels
The pain from varicose veins varies by person. You might feel:
- Aching or heaviness in the legs
- Pain that gets worse during the day, after standing
- Sharp pains or cramping
Pain from varicose veins means it’s getting worse. Watch how often and how bad the pain is.
Progression of Symptoms
Ignoring varicose vein symptoms can lead to bigger problems. Look out for signs that things are getting worse, like:
- Increased pain or swelling
- Changes in skin color or texture
- The development of ulcers or sores
Knowing the warning signs of varicose veins helps you get help early. This can stop more serious issues.
Being aware of symptoms lets you manage varicose veins better. This improves your life quality.
Are Varicose Veins Dangerous? The Truth About Risks
It’s important to know the risks of varicose veins. They are not just about looks. Varicose veins can cause serious health problems.
General Risk Assessment
Varicose veins are not usually life-threatening. But, they can be very uncomfortable. They might also lead to other health issues.
Risks Associated with Varicose Veins
- Development of blood clots
- Deep vein thrombosis (DVT)
- Pulmonary embolism
- Skin ulcers
Managing and treating varicose veins can lower these risks.
Misconceptions About Varicose Vein Dangers
Many people have wrong ideas about varicose veins. Some think they’re always a sign of something serious. Others see them as just a cosmetic issue. The truth is in between.
Common Misconceptions:
- Varicose veins are always dangerous.
- They are only a cosmetic issue.
- They will always lead to severe complications.
It’s key to clear up these myths to understand the real risks of varicose veins.
When to Be Concerned
Knowing when to get medical help is important. If you notice any of these signs, see a doctor.
|
Symptom |
Description |
|---|---|
|
Pain |
Persistent pain in the legs |
|
Swelling |
Swelling that doesn’t improve with elevation |
|
Skin Changes |
Discoloration or ulcers around the varicose veins |
If you have these symptoms, talk to a doctor. They can check your risk and suggest the best treatment.
Potential Complications of Untreated Varicose Veins
Varicose veins can cause many problems if not treated. These issues can be mild or severe and affect your health and wellbeing. They can also impact your overall health, not just your legs.
Bleeding and Ulceration
Untreated varicose veins can lead to serious issues like bleeding and ulcers. The veins can become weak and bleed easily, even with minor injuries. The skin over the veins can also thin and form ulcers, known as venous ulcers.
- Bleeding: Bleeding from varicose veins is a big concern, more so for older adults or those with a history of injury.
- Ulceration: Venous ulcers are painful and hard to heal, greatly affecting your quality of life.
Skin Changes and Discoloration
Varicose veins can also cause skin changes and discoloration. The increased pressure and fluid leakage can make the skin discolored, leading to stasis dermatitis.
Skin Changes: The skin may become thick, hard, or discolored, often showing as a brownish color around the ankles.
Impact on Mobility and Quality of Life
Untreated varicose veins can greatly affect your mobility and quality of life. Pain, discomfort, and ulcers or skin changes can limit your movement and make daily tasks hard.
- Pain and discomfort can limit your movement and activities.
- Ulcers or severe skin changes may require big lifestyle changes.
- Reduced mobility can worsen venous insufficiency, creating a cycle of problems.
In conclusion, untreated varicose veins can lead to many serious issues. These problems can deeply affect your health and wellbeing. It’s important to get medical help to prevent or manage these issues effectively.
Serious Complications: When Varicose Veins Become Harmful
Varicose veins are often seen as just a cosmetic issue. But, they can lead to serious problems. It’s important to know these risks to get medical help quickly.
Deep Vein Thrombosis (DVT)
Deep Vein Thrombosis is a serious issue where a blood clot forms in deep veins, usually in the legs. DVT can be deadly if the clot moves to the lungs, causing a pulmonary embolism. Signs of DVT include pain, swelling, and redness in the leg. Risk factors include being immobile for a long time, having a family history, and certain health conditions.
Seeing a doctor right away is key if symptoms don’t get better or get worse. Doctors use ultrasound to diagnose DVT. Treatment often includes medicines to stop the clot from getting bigger.
Pulmonary Embolism: Can Varicose Veins Be Life-Threatening?
A pulmonary embolism happens when a blood clot, often from DVT, goes to the lungs. This is a life-threatening situation that needs immediate medical help. Symptoms include sudden breathlessness, chest pain, and coughing up blood. The link between varicose veins and pulmonary embolism shows why managing varicose veins is so important.
Superficial Thrombophlebitis
Superficial thrombophlebitis is when veins get inflamed because of a blood clot. It usually affects the surface veins. It can cause pain, redness, and swelling along the vein. While not as serious as DVT, it can be quite uncomfortable and may need a doctor’s check-up.
Treatment for superficial thrombophlebitis often includes pain relief and, sometimes, medicines to prevent clotting. Knowing the risks and recognizing symptoms can help people get medical help early. This can prevent serious problems.
Chronic Venous Insufficiency and Progressive Vein Disease
Chronic venous insufficiency is linked to varicose veins. It happens when veins have valve problems, causing poor blood flow. Veins can’t efficiently return blood to the heart because of damaged valves or reflux.
The Connection Between Varicose Veins and CVI
Varicose veins and chronic venous insufficiency (CVI) are closely related. Varicose veins can cause CVI by not letting blood flow well. This increases pressure on the vein walls.
CVI can also make varicose veins worse. This creates a cycle where both conditions worsen each other.
CVI often starts with varicose veins. Damaged valves in veins stop blood from flowing back to the heart. This causes blood to build up in the legs, leading to symptoms.
Long-term Consequences of Venous Insufficiency
If not treated, chronic venous insufficiency can cause serious problems. These include:
- Persistent swelling and pain in the legs
- Skin changes, such as discoloration and thickening
- Development of venous ulcers, which can be challenging to heal
- Increased risk of deep vein thrombosis (DVT) and other complications
Seeking medical help is key if symptoms don’t go away or get worse. Early treatment can greatly improve outcomes and lower the risk of serious issues.
Do Varicose Veins Go Away on Their Own?
Many wonder if varicose veins can fix themselves or if they need treatment. Varicose veins are enlarged, twisted veins in the legs. They might go away on their own, but it’s not always the case, which is why some people seek treatment.
This is more common in people who get varicose veins during pregnancy. Pregnancy can make veins swell due to more blood and pressure.
Pregnancy-Related Varicose Veins
Pregnancy can lead to varicose veins. The blood volume and vein pressure increase. Research shows that these veins often get better after the baby is born. But, not everyone sees improvement, and some veins might come back in future pregnancies.
Natural Regression Possibilities
Varicose veins can get better on their own, but it’s not a sure thing. They might look less noticeable or even go away. How likely this is depends on why the veins are varicose and the person’s health.
For example, veins that get worse during pregnancy might get better by themselves. But veins that are always a problem might not improve without help.
Factors Affecting Spontaneous Improvement
Several things can affect if varicose veins will get better on their own. These include:
- The reason for the varicose veins
- How bad the veins are
- If there are other vein problems
- How active and heavy a person is
Living a healthy lifestyle, like exercising and not standing too long, can help. Wearing compression stockings also supports the veins and eases symptoms.
“Managing varicose veins involves lifestyle changes and sometimes medical help. Knowing what affects them can help manage them better.”
In summary, some varicose veins might get better by themselves, like those from pregnancy. But others might stay the same or get worse. Knowing what can help them improve can guide people in taking care of themselves.
When to Seek Medical Attention for Varicose Veins
Varicose veins are common, but some situations need immediate medical care. They can be more than just a cosmetic issue. They might show signs of venous insufficiency or other circulatory problems.
Warning Signs That Require Immediate Care
Knowing when to seek immediate medical attention for varicose veins is key. Studies by Petrova, Vento, & Vasquez (2023) and Smith, Johnson, & Lee (2022) show that severe pain, swelling, or deep vein thrombosis (DVT) symptoms need quick action.
- Severe pain or aching in the legs
- Swelling that doesn’t improve with elevation
- Signs of DVT, such as warmth, redness, or tenderness
- Bleeding or ulceration around varicose veins
Immediate care is vital to avoid serious issues like pulmonary embolism. This is a life-threatening condition linked to DVT.
Differentiating Between Routine and Emergency Situations
Telling routine varicose vein symptoms from emergency ones can be hard. A study by Smith, Johnson, & Lee (2022) stresses the need to know these differences. This ensures you get the right medical help on time.
|
Symptom |
Routine Care |
Emergency Care |
|---|---|---|
|
Pain |
Mild, manageable pain |
Severe, unbearable pain |
|
Swelling |
Swelling that improves with elevation |
Swelling that doesn’t improve with elevation |
|
Skin Changes |
Mild discoloration |
Ulceration or bleeding |
Finding the Right Vascular Specialist
Finding a vascular specialist is critical for varicose vein care. Petrova, Vento, & Vasquez (2023) say a specialist can guide you on the best treatments. This includes both conservative management and minimally invasive procedures.
“The key to managing varicose veins effectively lies in seeking timely medical attention and working with a qualified vascular specialist.” –
Varicose Vein Expert
When looking for a vascular specialist, check their qualifications, experience, and patient reviews. This ensures you get the best care possible.
Preventive Measures and Lifestyle Modifications
Preventive care and lifestyle changes are key to easing varicose vein symptoms. Simple daily habits can greatly lower the risk of these veins getting worse.
Exercise and Weight Management
Staying active and at a healthy weight are essential for managing varicose veins. Activities like walking or cycling boost blood flow and ease vein pressure.
Recommended Exercises:
- Walking
- Cycling
- Swimming
- Leg lifts
Compression Therapy
Wearing compression stockings is a top preventive step for varicose veins. They apply pressure to help blood flow back to the heart, reducing swelling and pain.
Benefits of Compression Therapy:
|
Benefit |
Description |
|---|---|
|
Improved Circulation |
Enhances blood flow back to the heart |
|
Reduced Swelling |
Minimizes leg swelling associated with varicose veins |
|
Discomfort Relief |
Alleviates pain and heaviness in the legs |
Dietary Considerations
Eating foods rich in fiber, vitamins, and minerals is good for your veins. Foods like berries and leafy greens are packed with antioxidants and flavonoids, which can help your veins.
By adopting these preventive steps and lifestyle changes, you can actively manage varicose veins. This can greatly improve your overall well-being.
Treatment Options for Varicose Veins
Managing varicose veins involves different methods, based on how severe they are. Treatment aims to ease symptoms, prevent problems, and enhance life quality.
Conservative Management Approaches
For many, the first step is making lifestyle changes. This includes regular exercise, staying at a healthy weight, and not sitting or standing for too long. Compression therapy is also used, with compression stockings to help blood flow and reduce swelling.
- Regular exercise to improve circulation
- Weight management to reduce pressure on veins
- Avoiding prolonged standing or sitting
- Use of compression stockings
Minimally Invasive Procedures
When lifestyle changes don’t work, minimally invasive procedures are considered. Sclerotherapy involves injecting a solution to close the vein. Endovenous laser therapy uses heat to seal it off. These are done on an outpatient basis and have quicker recovery times than surgery.
Other options include radiofrequency ablation and venaseal closure. These methods aim to close the vein, reducing symptoms.
Surgical Interventions
In severe cases or when other treatments fail, surgical interventions are needed. Vein stripping and ligation are traditional surgeries to remove or tie off varicose veins. Though effective, they require longer recovery times and carry more risks than minimally invasive treatments.
It’s vital for patients to talk to a vascular specialist. They can help choose the best treatment based on the patient’s condition and health.
Conclusion: Living With and Managing Varicose Veins
Managing varicose veins is key to keeping your blood vessels healthy. It helps avoid serious problems. By knowing the risks and taking action early, you can live better.
Dealing with varicose veins means changing your lifestyle and getting medical help. This mix helps control the condition. It lowers the chance of serious issues like blood clots and vein problems.
Choosing the right treatment for varicose veins is important. This includes simple steps, small procedures, and surgery. Talking to a vascular expert helps find the best treatment for you.
Being aware and managing varicose veins well is the main goal. With the right steps and medical care, you can reduce risks. This keeps your blood vessels in top shape.
FAQ
Can varicose veins kill you?
While rare, varicose veins can cause serious problems like pulmonary embolism if not treated.
Can varicose veins go away on their own?
Sometimes, varicose veins may get better or even go away, like during pregnancy. But, this doesn’t always happen, and you might need to see a doctor.
Are varicose veins dangerous?
Varicose veins can be a sign of a bigger problem with your veins. They might not be dangerous all the time. But, they can make you uncomfortable and affect your life.
Is varicose veins harmful?
Varicose veins can cause serious issues like bleeding, ulcers, or deep vein thrombosis. Getting medical help quickly is key to avoiding these problems.
Do varicose veins go away?
Varicose veins might not go away without treatment. But, you can manage symptoms and prevent complications with the right care.
Are varicose veins in feet dangerous?
Varicose veins in your feet can be a sign of a bigger issue. They need to be checked by a doctor to figure out the best treatment.
What are the dangers of varicose veins?
Varicose veins can lead to bleeding, ulcers, skin changes, and a higher risk of deep vein thrombosis and pulmonary embolism. If left untreated, they can really affect your life.
Can varicose veins be dangerous?
Yes, varicose veins can be dangerous if they cause serious problems. If your symptoms get worse or you notice warning signs, you should see a doctor right away.
When are varicose veins dangerous?
Varicose veins are dangerous when they cause serious issues like deep vein thrombosis, pulmonary embolism, or a lot of bleeding. You need to get medical help fast if this happens.
How can I manage varicose veins?
To manage varicose veins, you can try lifestyle changes like exercising, losing weight, and using compression stockings. You can also get medical treatments, from simple options to surgery, depending on your case.
What are the treatment options for varicose veins?
Treatment for varicose veins includes lifestyle changes, minimally invasive procedures, and surgery. The best option depends on how bad your veins are and what you need.
References
National Center for Biotechnology Information. Varicose Veins: Risks and What You Need to Know. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK470194/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























