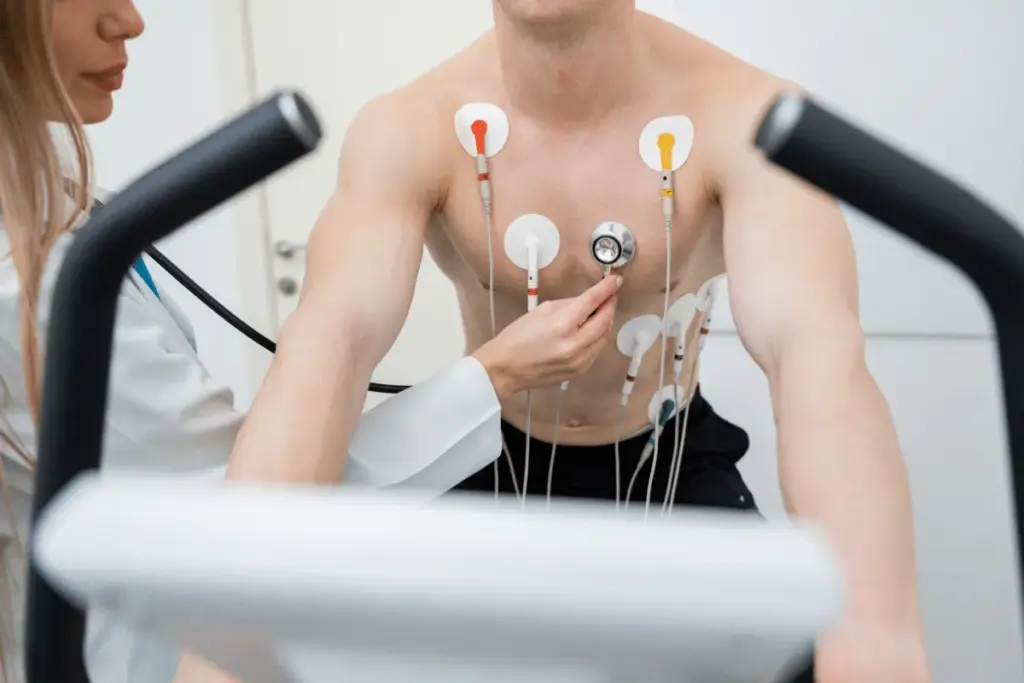
An estimated 40 million people worldwide live with arrhythmia. This condition causes irregular heartbeats, ranging from harmless to dangerous. An electrocardiogram (ECG) is a simple test that checks the heart’s electrical activity. It shows how fast or slow the heart is beating.
ECG is key in finding heart rhythm problems. It helps doctors diagnose irregular heartbeats. This is why ECG is so important in cardiology.
Key Takeaways
- ECG is a vital tool for diagnosing heart rhythm disorders.
- Arrhythmias can be harmless or life-threatening, needing accurate diagnosis.
- ECG measures the heart’s electrical activity, showing its rate.
- Getting the diagnosis right with ECG is key for good treatment.
- ECG is a quick and painless test.
The Science Behind Electrocardiography
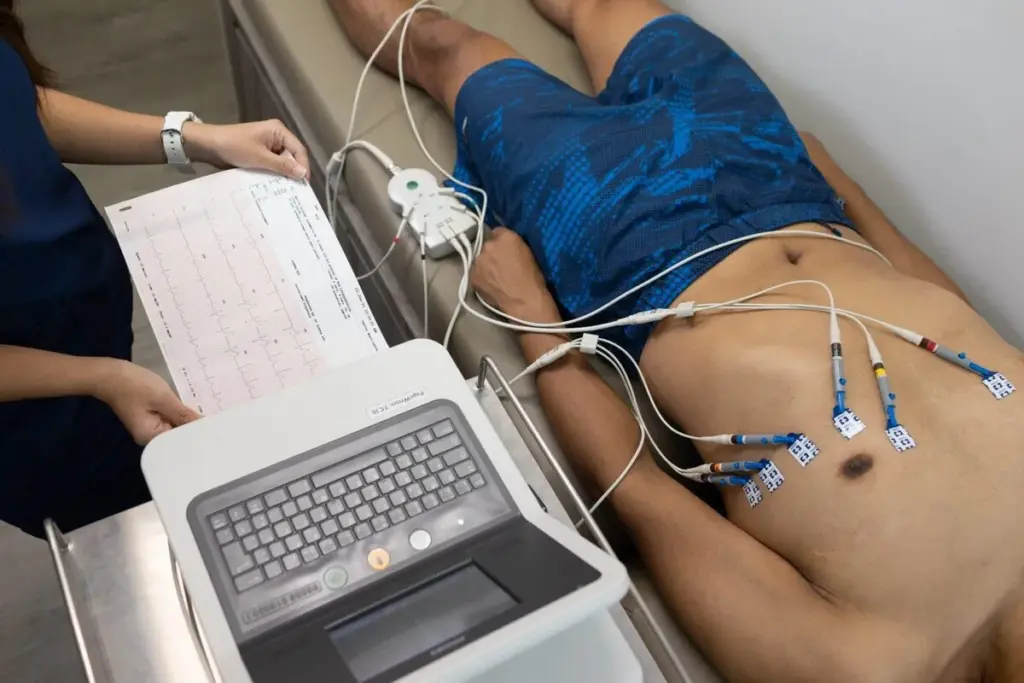
Electrocardiography lets us see how the heart works. It’s a safe and useful way to check the heart’s health. This method helps find problems early.
What is an ECG and How Does it Work?
An electrocardiogram (ECG) tracks the heart’s electrical signals. It uses electrodes on the skin to do this. These electrodes pick up the heart’s electrical changes during each beat.
The ECG machine turns these signals into a graph. This graph shows how the heart beats and works. It’s key for spotting heart issues.
Getting an ECG is easy. Patients lie down and electrodes are put on their chest, arms, and legs. These electrodes send signals to the ECG machine. It records the heart’s electrical activity, helping diagnose heart problems.
The Components of an ECG Reading
An ECG reading has several parts. These parts show the heart’s electrical activity. The main parts are the P wave, QRS complex, and T wave.
|
Component |
Description |
|---|---|
|
P Wave |
Represents atrial depolarization, indicating the electrical activation of the atria. |
|
QRS Complex |
Signifies ventricular depolarization, marking the electrical activation of the ventricles. |
|
T Wave |
Denotes ventricular repolarization, representing the recovery period of the ventricles. |
Doctors look at these parts to find heart rhythm problems. They can spot arrhythmias and decide how to treat them. Knowing how ECG works helps us understand its importance in heart health.
What is Arrhythmia? Types and Classifications
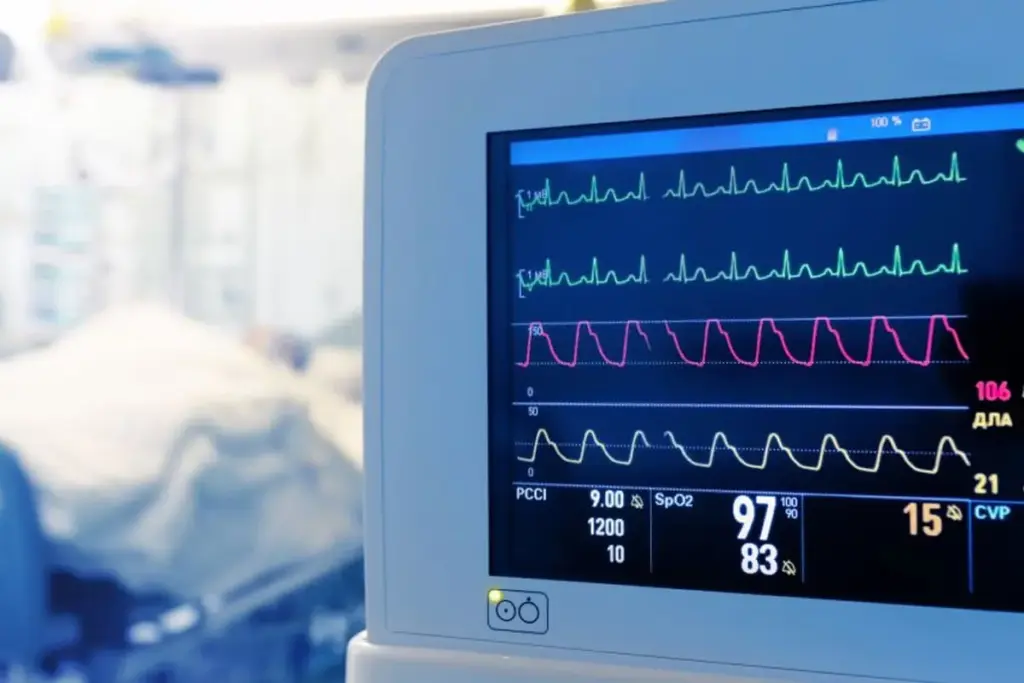
Arrhythmias, or irregular heartbeats, affect millions globally. They are disturbances in the heart’s rhythm. This can take many forms.
Definition and General Understanding of Arrhythmias
An arrhythmia happens when the heart’s electrical signals get disrupted. This can make the heart beat too fast, too slow, or irregularly. Heart palpitations are common symptoms, where people feel their heart skipping beats or fluttering.
Arrhythmias can start in the atria or ventricles. Knowing where they start helps doctors choose the right arrhythmia treatment.
Common Causes of Heart Rhythm Disorders
Many things can cause arrhythmias, like heart disease or certain medications. Ventricular tachycardia is a serious arrhythmia that starts in the ventricles. It’s dangerous if not treated quickly.
|
Cause |
Description |
Potential Arrhythmia |
|---|---|---|
|
Heart Disease |
Conditions like coronary artery disease or heart failure |
Atrial Fibrillation, Ventricular Tachycardia |
|
Electrolyte Imbalance |
Abnormal levels of potassium, sodium, or calcium |
Various Arrhythmias |
|
Certain Medications |
Drugs that affect heart rhythm |
Arrhythmias due to drug side effects |
Healthcare providers can treat arrhythmias by understanding their causes and types. They might use medications, procedures, or lifestyle changes. These aim to manage symptoms and prevent complications.
The Mechanism of Arrhythmia Detection Through ECG
ECG can detect arrhythmias by capturing the heart’s electrical patterns. It shows the heart’s electrical activity on a screen. This helps doctors spot irregular heartbeats.
Electrical Patterns in Normal vs. Irregular Heartbeats
A normal heartbeat has a consistent pattern on the ECG. This pattern shows the heart’s electrical activity. It includes a P wave, a QRS complex, and a T wave.
But, irregular heartbeats or arrhythmias mess up this pattern. They cause abnormal ECG tracings. For example, atrial fibrillation shows an irregular rhythm without P waves. Ventricular tachycardia has rapid, wide QRS complexes.
Key ECG Markers for Arrhythmia Detection
Several ECG markers are key for spotting arrhythmias. These include:
- Abnormal P wave morphology or absence: Shows atrial fibrillation or other atrial arrhythmias.
- Wide or irregular QRS complexes: Points to ventricular arrhythmias or conduction problems.
- Prolonged PR intervals: May mean first-degree atrioventricular (AV) block.
- ST segment changes: Can show ischemia or other heart issues.
|
ECG Marker |
Possible Arrhythmia or Condition |
|---|---|
|
Absent P waves, irregularly irregular rhythm |
Atrial Fibrillation |
|
Wide QRS complexes, rapid rate |
Ventricular Tachycardia |
|
Prolonged PR interval |
First-degree AV Block |
|
ST segment elevation or depression |
Myocardial Ischemia or Infarction |
Doctors use these ECG markers to diagnose arrhythmias. They then plan the right treatment. Accurate ECG interpretation is key for managing heart rhythms.
Types of Arrhythmias Detectable by ECG
Healthcare professionals use ECG to find several arrhythmias that need medical help. An electrocardiogram shows the heart’s electrical activity. This helps spot irregular heart rhythms.
Atrial Fibrillation and Flutter
Atrial fibrillation (AFib) is a common arrhythmia with fast and irregular heartbeats. It happens when the upper heart chambers (atria) beat chaotically. This makes it hard for blood to move into the ventricles. ECG shows AFib as an irregular rhythm without clear P waves.
Atrial flutter is a rapid but regular rhythm in the atria. It looks like a “sawtooth” pattern on the ECG.
Key characteristics of AFib and atrial flutter on ECG:
- Irregularly irregular rhythm for AFib
- “Sawtooth” pattern for atrial flutter
- Absence of distinct P waves in AFib
Ventricular Tachycardia and Fibrillation
Ventricular tachycardia (V-tach) is a serious arrhythmia starting in the ventricles. It has a fast heart rate over 100 beats per minute. Ventricular fibrillation (V-fib) is even worse, where the ventricles fibrillate instead of contract. This stops blood circulation. ECG is key in diagnosing these, showing fast wide QRS complexes for V-tach and chaotic patterns for V-fib.
ECG markers for V-tach and V-fib:
- Wide QRS complexes in V-tach
- Rapid heart rate in V-tach
- Chaotic pattern in V-fib
Bradyarrhythmias and Heart Blocks
Bradyarrhythmias are heart rhythms that are too slow. They can be caused by problems with the heart’s electrical system. Heart blocks are a type of bradyarrhythmia where there’s a delay or block in the electrical pathway. ECG can spot these by showing slow heart rates and specific patterns.
Premature Contractions and Other Minor Arrhythmias
Premature contractions, like premature atrial contractions (PACs) and premature ventricular contractions (PVCs), are common. They can be found by ECG. PACs start in the atria, and PVCs start in the ventricles. ECG shows these by their early occurrence and unique shape.
Characteristics of premature contractions on ECG:
- Premature occurrence
- Distinct morphology compared to normal beats
- PACs have abnormal P wave morphology
- PVCs have wide and bizarre QRS complexes
The Accuracy of ECG in Arrhythmia Detection
How well ECG detects arrhythmias is key in heart care. We use electrocardiography to spot heart rhythm problems. Knowing how accurate it is is very important.
ECG’s accuracy is measured by its sensitivity and specificity. Sensitivity is how well it finds people with arrhythmia. Specificity is how well it finds people without it.
Sensitivity and Specificity Rates
Research shows ECG’s sensitivity and specificity vary with arrhythmia types. For example, it’s very good at spotting atrial fibrillation. But, it might miss arrhythmias that only happen sometimes.
“The ECG is a key tool for diagnosing arrhythmias,” say heart experts. But, many things can affect its accuracy. This includes the quality of the recording, the interpreter’s skill, and any noise or artifacts.
Factors Affecting ECG Accuracy
- Quality of the ECG recording: Bad electrode placement or patient movement can mess up readings.
- Skill of the interpreter: Knowing how to read ECGs well is very important.
- Type of arrhythmia: Some arrhythmias are easier to spot than others.
- Presence of other heart conditions: Some conditions can make ECG readings harder to understand.
Understanding these factors helps doctors improve heart rhythm diagnosis and treatment. As we keep improving in heart care, ECG’s role in finding arrhythmias is more important than ever.
Different Types of ECG Tests for Arrhythmia
Healthcare professionals use many ECG tests to find arrhythmias. These tests show how the heart works in different situations. They give a full picture of the heart’s rhythm.
Standard 12-Lead ECG
The standard 12-lead ECG is the most used test for arrhythmias. It uses electrodes on the chest and limbs to record the heart’s electrical activity from 12 angles. This test is fast, painless, and gives quick results.
Advantages: Quick and easy to perform, provides a snapshot of the heart’s activity.
Holter Monitoring
Holter monitoring uses a portable device that records the heart’s activity for 24 to 48 hours. It’s great for finding arrhythmias that happen at random times.
Advantages: Provides a longer recording period, capturing more heart activity.
Limitations: Can be cumbersome to wear, and data analysis can be time-consuming.
Event Recorders and Loop Recorders
Event recorders capture arrhythmias that don’t happen often. Patients press a button when they feel symptoms, and it records the heart’s activity. Loop recorders do the same but are implanted under the skin for longer monitoring.
Advantages: Captures arrhythmias that occur infrequently, providing valuable diagnostic information.
Limitations: Requires patient activation, which can be a limitation if the patient is asymptomatic or unable to activate it.
|
ECG Test Type |
Description |
Advantages |
Limitations |
|---|---|---|---|
|
Standard 12-Lead ECG |
Records heart activity from 12 angles |
Quick, easy, immediate results |
May miss intermittent arrhythmias |
|
Holter Monitoring |
Continuous recording over 24-48 hours |
Captures more heart activity |
Cumbersome, time-consuming analysis |
|
Event Recorders |
Records heart activity during symptoms |
Captures infrequent arrhythmias |
Requires patient activation |
“The choice of ECG test depends on the frequency and nature of the arrhythmia, as well as the patient’s specific needs.”
A Cardiologist
In conclusion, there are many ECG tests for diagnosing arrhythmias. Each has its own benefits and drawbacks. Knowing these differences helps doctors pick the best test for each patient. This ensures accurate diagnosis and effective treatment.
Limitations of ECG in Detecting Certain Arrhythmias
ECG is very useful, but it has its limits. It can’t always find certain arrhythmias, like the ones that don’t happen all the time. A standard ECG only shows heart activity for a short time. So, it might miss arrhythmias that only show up sometimes or not during the test.
Intermittent Arrhythmias and Detection Challenges
Intermittent arrhythmias are hard to diagnose because they don’t always show up on an ECG. They can be caused by stress, exercise, or some medicines. This makes it tough to catch them during a regular ECG test.
To get around this problem, doctors use longer monitoring methods. But, even with these, there’s a chance of missing the arrhythmia if it happens very rarely.
When ECG May Miss Arrhythmias
There are a few times when ECG might not find arrhythmias:
- When the arrhythmia is intermittent and not captured during the recording.
- If the arrhythmia is of short duration, it might not be recorded.
- In cases where the patient is asymptomatic during the ECG recording.
The table below shows the challenges and possible ways to find intermittent arrhythmias:
|
Challenge |
Potential Solution |
|---|---|
|
Intermittent arrhythmias not captured during standard ECG |
Holter monitoring or event recorders for longer-term monitoring |
|
Short-duration arrhythmias |
Continuous monitoring or implantable cardiac monitors |
|
Asymptomatic periods during ECG |
Patient-activated event recorders or mobile ECG technology |
It’s important for both doctors and patients to know about these ECG limits. This highlights the need for a more detailed approach to diagnosis. Sometimes, this means doing more tests than just a standard ECG.
Beyond Standard ECG: Advanced Techniques for Arrhythmia Detection
There are advanced methods beyond the standard ECG that greatly improve arrhythmia detection. These techniques are key in our ongoing fight against heart rhythm disorders. They help us diagnose better than ever before.
Signal-Averaged ECG (SAECG)
Signal-Averaged ECG (SAECG) averages many ECG signals to cut down on noise. It makes it easier to spot low-amplitude signals. This is super helpful in finding patients at risk for ventricular tachycardia.
Key Benefits of SAECG:
- Improved detection of late potentials
- Enhanced risk stratification for ventricular arrhythmias
- Better noise reduction compared to standard ECG
Implantable Cardiac Monitors
Implantable cardiac monitors (ICMs) are tiny devices that track the heart’s rhythm all the time. They’re great for catching arrhythmias that don’t show up on a standard ECG or Holter monitor.
|
Feature |
Standard ECG |
Implantable Cardiac Monitors |
|---|---|---|
|
Monitoring Duration |
Short-term (minutes to hours) |
Long-term (months to years) |
|
Detection Capability |
Limited to the recording period |
Continuous monitoring |
|
Patient Comfort |
Non-invasive |
Minimally invasive |
Mobile ECG Technology and Wearables
Mobile ECG technology and wearables have changed how we track heart rhythms outside of hospitals. Smartwatches and fitness trackers with ECG features let us monitor our heart in real-time. They can even alert us to irregular rhythms.
Advantages of Mobile ECG Technology:
- Convenience and accessibility
- Real-time monitoring and alerts
- Integration with other health and fitness data
Alternative Diagnostic Methods for Arrhythmia
There are more ways to diagnose arrhythmias than just the ECG. These methods give a deeper look into heart rhythm problems. They help doctors understand and treat arrhythmias better.
Electrophysiology Studies
Electrophysiology studies (EPS) are detailed tests that go inside the heart. They use thin catheters to record the heart’s electrical signals. EPS is great for finding the cause of arrhythmias and planning treatments.
Key aspects of EPS include:
- Direct measurement of the heart’s electrical signals
- Identification of arrhythmia mechanisms
- Guidance for therapeutic interventions
Echocardiogram and Other Imaging Techniques
Echocardiography, or echo, is a non-invasive test that uses sound waves to see the heart. It doesn’t measure electrical activity but can spot structural heart issues. Other tests like MRI or CT scans also help check the heart’s shape and how it works.
|
Imaging Technique |
Primary Use |
Benefits |
|---|---|---|
|
Echocardiogram |
Assess heart structure and function |
Non-invasive, real-time imaging |
|
Cardiac MRI |
Detailed heart structure and tissue characterization |
High-resolution images, no radiation |
|
Cardiac CT |
Coronary artery assessment, calcium scoring |
Quick, detailed coronary artery imaging |
Tilt Table Testing
Tilt table testing is mainly for finding out why people faint. It checks blood pressure, heart rate, and ECG when the table tilts. This test helps see if fainting is due to heart rate or blood pressure issues.
Using these tests, doctors can understand arrhythmias better. They can then create treatment plans that fit each patient’s needs.
Interpreting ECG Results: What Your Doctor Sees
Reading ECGs is both an art and a science. It needs skill to tell normal heart activity from signs of arrhythmia. We look at the heart’s electrical signals to find patterns that show if the heart is working right or not.
Normal vs. Abnormal ECG Patterns
A normal ECG shows a steady heart rate and rhythm. It has specific intervals and segments that are within normal ranges. Abnormal ECG patterns can mean many things, from small issues to serious heart problems.
We check several important parts when we analyze an ECG. The P wave shows when the heart’s upper chambers depolarize. The QRS complex shows when the lower chambers depolarize. The T wave shows when they repolarize. Any oddness in these parts can mean an arrhythmia or other heart problems.
Common Misinterpretations and False Positives
Even with the best intentions, ECGs can sometimes be misread. False positives can cause extra tests or worry for patients. Mistakes can happen when noise is seen as arrhythmia or when a normal variation is thought to be a problem.
To avoid these mistakes, we use experience, follow guidelines, and sometimes, more tests to check our findings. It’s a detailed process that needs knowledge of ECG patterns and understanding the patient’s health situation.
When to Seek Medical Attention for Suspected Arrhythmia
Knowing when to get medical help for arrhythmia can save lives. Arrhythmias, or irregular heartbeats, can show up in many ways. Some need quick medical help. We’ll show you the signs and symptoms that mean you should see a doctor.
Warning Signs and Symptoms
Arrhythmia symptoms can differ from person to person. Common ones include palpitations, shortness of breath, dizziness, and chest pain. If you notice any of these, it’s important to figure out how serious they are and how long they last. For example, occasional skipped beats might not be as bad as long periods of fast heartbeat.
Important symptoms to watch for include:
- Palpitations or irregular heartbeats
- Shortness of breath or trouble breathing
- Dizziness or feeling lightheaded
- Chest pain or discomfort
- Fainting or feeling like you’re going to faint
Emergency vs. Non-Emergency Situations
Not all arrhythmia symptoms need emergency care, but some do. If you or someone else has severe symptoms like chest pain, really hard breathing, or losing consciousness, call emergency services right away.
For milder symptoms, it’s wise to talk to your doctor. They can check you out and decide what to do next. It’s always safer to be careful with your heart health.
In short, knowing the signs and symptoms of arrhythmia and when to get medical help is key to your health. We urge you to keep an eye on your heart health and talk to doctors if you have any worries.
Treatment Options for Arrhythmias Detected by ECG
ECG-detected arrhythmias can be treated in many ways. This includes medicines and lifestyle changes. The right treatment depends on the arrhythmia type, its severity, and the patient’s health.
Medications for Arrhythmia Management
Medicines are key in managing arrhythmias. They help control heart rate and rhythm. They also prevent serious problems like stroke.
Medicines like beta-blockers, anti-arrhythmic drugs, and anticoagulants are used. Beta-blockers slow the heart rate and reduce workload. Anti-arrhythmic drugs fix the heart rhythm. Anticoagulants stop blood clots that could cause stroke.
|
Medication Type |
Primary Use |
Examples |
|---|---|---|
|
Beta-blockers |
Control heart rate |
Metoprolol, Propranolol |
|
Anti-arrhythmic drugs |
Restore normal heart rhythm |
Amiodarone, Flecainide |
|
Anticoagulants |
Prevent stroke |
Warfarin, Apixaban |
Interventional Procedures and Surgery
For some, interventional procedures or surgery are needed to treat arrhythmias.
Catheter ablation destroys the heart tissue causing arrhythmia. It’s used for SVT and some ventricular tachycardia.
The Maze procedure is another surgical option. It creates scar tissue in the heart’s upper chambers. This directs electrical impulses along a controlled path.
Lifestyle Modifications
Lifestyle changes are vital in managing arrhythmias. They help reduce symptoms and improve life quality.
Avoiding triggers like caffeine, alcohol, and stress is advised. Regular exercise, a balanced diet, and a healthy weight are also key.
Managing conditions like high blood pressure, diabetes, and sleep apnea also helps control arrhythmias.
Recent Advances in ECG Technology for Arrhythmia Detection
ECG technology has seen big changes thanks to AI, ML, and remote monitoring. These new tools help us spot and handle arrhythmias better.
AI and Machine Learning Applications
AI and ML have changed how we look at ECGs. AI algorithms can sift through lots of data to find patterns humans might miss. This makes spotting arrhythmias more accurate and lets us act sooner.
- Enhanced pattern recognition
- Predictive analytics for arrhythmia risk
- Automated analysis reducing clinician workload
A study in a top cardiology journal showed AI-enhanced ECGs are better at finding atrial fibrillation than old methods.
“The use of AI in ECG analysis represents a major breakthrough in cardiology, giving us new insights into heart function and arrhythmia detection.”
A Cardiologist
Remote Monitoring Innovations
Remote monitoring is a big step forward in ECG tech. It lets us keep an eye on patients with arrhythmias all the time, sending updates to doctors.
The good things about remote monitoring are:
- Spotting arrhythmias early
- Less need for hospital trips
- Better care for patients with quick actions
As we keep using these techs in healthcare, we’ll see even better care for arrhythmia patients.
Living with Arrhythmia: Management and Long-Term Monitoring
Managing arrhythmia means more than just treatment. It’s about improving your life quality through long-term monitoring and management. Understanding how to manage this condition is key to a better life.
Long-term ECG Monitoring Strategies
ECG monitoring is vital for managing arrhythmia. It lets doctors track your heart’s rhythm over time. This gives them important insights into your condition.
There are several ways to monitor your heart long-term:
- Holter monitoring, which records your heart’s activity for 24 to 48 hours
- Event recorders, which can be worn for longer periods to catch arrhythmias when they happen
- Implantable cardiac monitors, which monitor your heart continuously for years
Quality of Life Considerations
Arrhythmia management goes beyond medical treatment. It’s about improving your overall well-being. People with arrhythmia often feel anxious, stressed, and limited in their daily activities.
To enhance your quality of life, consider:
- Making lifestyle changes, like exercising regularly and eating a balanced diet
- Trying stress management techniques, such as meditation and yoga
- Regularly checking in with your healthcare provider to adjust your treatment plan
Here’s a comparison of different long-term ECG monitoring strategies:
|
Monitoring Strategy |
Duration |
Benefits |
|---|---|---|
|
Holter Monitoring |
24-48 hours |
Provides detailed information on heart activity during daily routines |
|
Event Recorders |
Several days to weeks |
Captures intermittent arrhythmias, useful for diagnosing less frequent events |
|
Implantable Cardiac Monitors |
Several years |
Offers continuous monitoring, ideal for long-term management and detecting rare arrhythmias |
By using effective long-term ECG monitoring and improving your quality of life, you can live more actively and happily with arrhythmia.
Conclusion: The Role of ECG in Arrhythmia Management
ECG is key in arrhythmia diagnosis and management. It helps spot irregular heart rhythms, making it vital in cardiology. We’ve learned how various ECG tests help diagnose heart rhythm disorder.
ECG findings guide treatment for arrhythmia patients. Doctors use this info to pick the best treatment. This could be medicine, procedures, or changes in lifestyle.
In ECG in arrhythmia management, long-term monitoring is critical. Tools like implantable monitors and mobile ECGs help keep an eye on the heart. This leads to better care and results. With new ECG tech, like AI, we’ll see even better diagnosis and care.
ECG’s role in managing arrhythmias shows its importance in heart care. It helps us give better care and improve outcomes for those with heart rhythm issues.
FAQ
What is an ECG and how does it detect arrhythmias?
An electrocardiogram (ECG) is a test that checks the heart’s electrical activity. It spots arrhythmias by looking at the heart’s electrical patterns. It finds irregular heartbeats and tells us about the heart’s rhythm.
What are the different types of arrhythmias that can be detected by ECG?
ECG can find many arrhythmias, like atrial fibrillation and ventricular tachycardia. It also finds bradyarrhythmias and premature contractions.
How accurate is ECG in detecting arrhythmias?
ECG’s accuracy in finding arrhythmias varies. It depends on the arrhythmia type, ECG quality, and the interpreter’s skill. Usually, ECG is good at spotting many arrhythmias.
What are the limitations of ECG in detecting arrhythmias?
ECG might miss arrhythmias that happen rarely. It doesn’t show the heart’s full electrical activity. Other tests might be needed to confirm a diagnosis.
What are the different types of ECG tests used to diagnose arrhythmias?
There are several ECG tests, like the standard 12-lead ECG and Holter monitoring. Each has its own benefits and drawbacks.
How do I interpret ECG results?
Understanding ECG results needs knowledge and skill. A healthcare expert will look at the ECG tracing. They’ll identify normal or abnormal patterns and make a diagnosis.
What are the warning signs and symptoms of arrhythmias?
Signs of arrhythmias include palpitations and dizziness. Shortness of breath and chest pain are also common. If you notice these, see a doctor.
What are the treatment options for arrhythmias detected by ECG?
Treatments for arrhythmias include medicines and procedures. Lifestyle changes are also important, depending on the arrhythmia type and severity.
How can I manage arrhythmias and improve my quality of life?
Managing arrhythmias involves long-term ECG monitoring and lifestyle changes. Sticking to treatment plans can also help improve your life.
What are the recent advances in ECG technology for arrhythmia detection?
New ECG tech includes AI and remote monitoring. Mobile ECGs also help in detecting and tracking arrhythmias better.
Can arrhythmias be cured?
Some arrhythmias can be treated and cured. Others need ongoing care. The cure chance depends on the arrhythmia type, severity, and treatment success.
How often should I have an ECG to monitor my heart rhythm?
How often you need an ECG depends on your health and treatment. Talk to your doctor to find the best schedule for you.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC12096014/


































