Who performs AVM treatment? Meet the successful surgical experts and learn amazing facts about the specialists who save lives every day.
Arteriovenous malformation (AVM) is a complex condition. It needs a team of experts for the best treatment. Did you know AVMs affect about 1 in 100,000 people every year?
AVM treatment is complex. It requires a team of specialists. This team includes neurosurgeons, radiologists, and other medical experts. Knowing who performs AVM surgery is key for effective care.
Key Takeaways
- AVM is a rare condition requiring specialized treatment.
- A multidisciplinary team is essential for effective AVM care.
- Neurosurgeons and radiologists play key roles in AVM surgery.
- Understanding AVM treatment options is vital for patient care.
- Specialists involved in AVM care include various medical professionals.
Understanding Arteriovenous Malformations (AVMs)
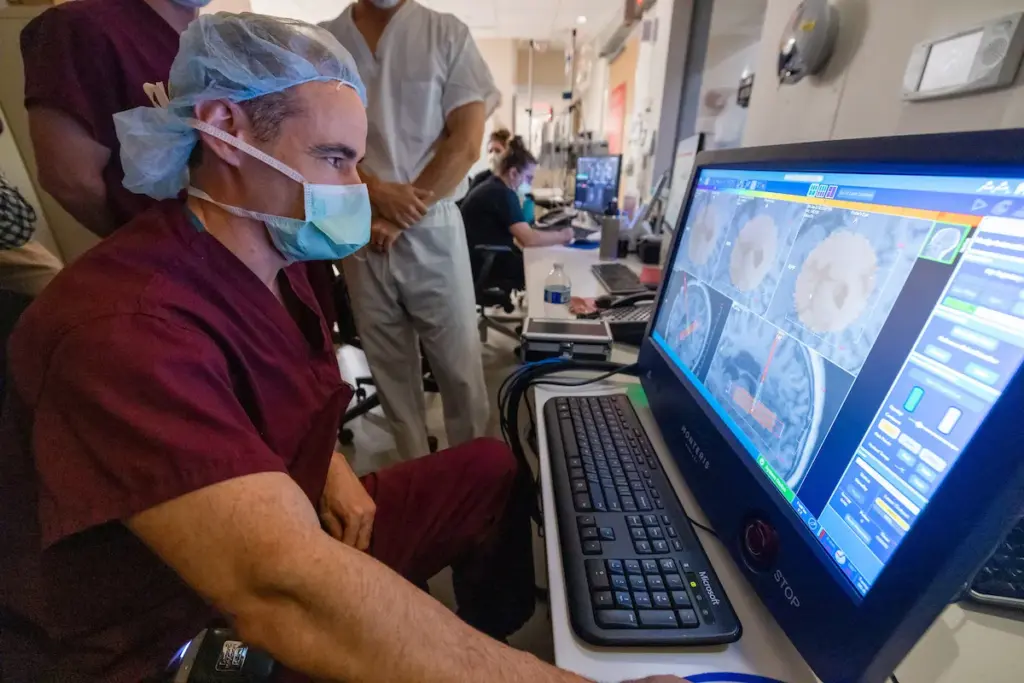
AVM brain
Learning about arteriovenous malformations (AVMs) is key for those who have them. AVMs mix up arteries and veins in the brain. They are a complex problem that can affect health a lot.
What is an AVM?
An arteriovenous malformation (AVM) is when arteries and veins connect in a bad way. This can cause high-pressure blood flow into veins, leading to damage or rupture. AVMs often happen in the brain, making “AVM brain” a big concern.
Common Locations of AVMs
AVMs can pop up in different brain spots, with some spots more common than others. They might be found in:
- Cerebral cortex
- Basal ganglia
- Cerebellum
- Brainstem
Cerebral AVMs are very worrying because they can lead to bleeding or other brain issues.
Risk Factors and Prevalence
The exact reason for AVMs is not known, but some things might make you more likely to get one. These include:
- Genetic predisposition
- Family history of AVMs or other vascular malformations
- Certain genetic disorders, such as Osler-Weber-Rendu syndrome
AVMs are not very common, affecting about 1 in 100,000 people each year. Knowing about risk factors and how common they are helps in dealing with AVM disease brain.
The Multidisciplinary Team Approach to AVM Management
Effective AVM treatment needs a team effort. Experts from different fields come together. This is because AVMs are complex and require a detailed care plan.
Importance of Specialized Care
Managing AVMs requires a team of specialists. Neurosurgeons, interventional neuroradiologists, and radiation oncologists are all part of it.
Specialized care means better diagnoses and treatment plans. It leads to better patient outcomes. Specialists work together to understand the patient’s condition fully, creating effective treatment plans.
Coordinated Treatment Planning
Coordinated treatment planning is key to managing AVMs well. The team works together to create a treatment plan that fits the patient’s needs. They consider the AVM’s size, location, the patient’s health, and the risk of rupture.
Effective communication among team members is vital. Regular meetings help them share their knowledge. This leads to a more effective treatment plan.
Using a multidisciplinary team approach helps provide complete AVM care. This teamwork is essential for the best treatment outcomes.
Neurosurgeons: Primary AVM Surgery Specialists
Neurosurgeons specializing in AVM surgery have a lot of training and know-how. They are key in treating cerebral arteriovenous malformations.
Training and Qualifications
Neurosurgeons go through tough training to master AVM surgery. This includes:
- Completing medical school and a neurosurgical residency program
- Acquiring specialized training in cerebrovascular surgery
- Staying updated with the latest techniques and advancements in AVM treatment
Many also get extra fellowship training in complex cerebrovascular cases, like AVMs. This training helps them handle complex AVM surgeries.
Surgical Expertise for AVMs
Neurosurgeons use their skills to treat AVMs with microsurgery. They aim to remove the malformation while keeping the brain safe. Their knowledge is key in:
- Assessing the complexity and risk of the AVM
- Planning the most appropriate surgical approach
- Executing the surgery with precision and care
Their surgical expertise is essential for the best results in AVM surgery.
When a Neurosurgeon Takes the Lead
A neurosurgeon leads in AVM treatment when surgery is the best option. This choice is made after a team of experts, including neurologists and radiologists, evaluate the case.
When an AVM is ruptured or at high risk of rupture, neurosurgeons may do emergency surgery. They are also key in managing any surgery complications.
With their extensive training, surgical expertise, and experience, neurosurgeons are vital in treating AVMs. They give patients a good chance of recovery and a better life.
Interventional Neuroradiologists: Endovascular Specialists
Interventional neuroradiologists are key in treating arteriovenous malformations (AVMs) with endovascular techniques. They are experts in navigating complex blood vessels. This skill is vital in managing AVMs.
Role in AVM Diagnosis and Treatment
Interventional neuroradiologists are key players in AVM diagnosis and treatment. They use advanced imaging to understand the malformation’s anatomy. This is essential for treatment planning.
These specialists perform endovascular procedures, like embolization. This is a minimally invasive method to reduce blood flow to the AVM.
Embolization Procedures
Embolization involves interventional neuroradiologists placing materials in the AVM’s blood vessels. The goal is to reduce or eliminate the malformation’s blood supply. Various materials, such as coils, glue, or particles, are used.
|
Embolization Material |
Characteristics |
Use in AVM Treatment |
|---|---|---|
|
Coils |
Mechanical occlusion, promotes clotting |
Often used for pedicle occlusion or to reduce flow |
|
N-butyl cyanoacrylate (NBCA) |
Permanent embolic agent, polymerizes upon contact with blood |
Used for nidus occlusion and to achieve more permanent results |
|
Onyx |
Liquid embolic agent, precipitates upon contact with ionic solutions |
Preferred for its ability to penetrate the nidus and achieve a more complete occlusion |
Collaboration with Neurosurgeons
The teamwork between interventional neuroradiologists and neurosurgeons is crucial for AVM management. Embolization can be a standalone treatment or a pre-surgical step. This reduces the AVM’s size, making surgery safer and more possible.
Together, these specialists create personalized treatment plans. This approach optimizes outcomes and minimizes risks for each patient.
Radiation Oncologists: Specialists in Radiosurgery
Radiation oncologists are key in managing AVMs. They use radiosurgery, a precise radiation therapy. This method targets the AVM without harming nearby healthy tissue.
Stereotactic Radiosurgery for AVMs
Stereotactic radiosurgery is a main treatment for AVMs. An expert, has shown its success. This method uses advanced imaging and radiation to close the AVM over time.
Gamma Knife and CyberKnife Expertise
Radiation oncologists are skilled in Gamma Knife and CyberKnife. These tools deliver radiation precisely to the AVM. This helps keep the brain safe. Gamma Knife radiosurgery is great for deep AVMs. CyberKnife can treat AVMs anywhere in the body.
Patient Selection for Radiation Treatment
Choosing radiosurgery depends on the AVM’s size, location, and the patient’s health. Radiation oncologists team up with neurosurgeons and neuroradiologists. They decide the best treatment for each patient. Radiosurgery might be the main treatment or used with others.
Radiation oncologists are essential in AVM care. They offer a range of treatments tailored to each patient’s needs.
Comprehensive AVM Treatment Options and Approaches
AVM treatment varies because each case is unique. The right treatment depends on the AVM’s size, location, and the patient’s health. It also considers the risk of bleeding.
Surgical Resection
Surgical resection is a common and effective way to treat AVMs. It removes the malformation to prevent bleeding. Neurosurgeons use their skills to safely remove the AVM.
Choosing surgery depends on the AVM’s location and the patient’s health. Microsurgical techniques have improved. Now, they allow for precise removal with less damage to nearby tissue.
Endovascular Embolization
Endovascular embolization is a less invasive method. It uses a catheter to block the AVM. This method is often used with surgery or radiosurgery to improve results.
“Endovascular embolization has become an indispensable tool in the management of AVMs, providing a less invasive option compared to traditional surgery.” – An Interventional Neuroradiologist
Stereotactic Radiosurgery
Stereotactic radiosurgery (SRS) is a precise radiation therapy for hard-to-reach AVMs. It delivers focused radiation to the AVM, aiming to close it over time.
|
Treatment Option |
Advantages |
Limitations |
|---|---|---|
|
Surgical Resection |
Immediate removal of AVM |
Invasive, risk of surgical complications |
|
Endovascular Embolization |
Minimally invasive, can be used with other treatments |
May not completely eliminate AVM, risk of recanalization |
|
Stereotactic Radiosurgery |
Non-invasive, effective for deep or complex AVMs |
Delayed effect, risk of radiation-induced complications |
Combined Approaches
Many patients benefit from combining treatments. For example, embolization might shrink an AVM before surgery or radiosurgery. This approach aims for the best results.
Using multiple treatments shows the value of a team effort. Specialists from neurosurgery, interventional neuroradiology, and radiation oncology work together. They create a treatment plan that meets the patient’s needs.
Factors Determining Which Specialist Performs Your AVM Treatment
AVM size and location
Choosing the right specialist for AVM treatment is complex. It depends on many factors. These include the patient’s condition and the AVM’s characteristics.
AVM Size and Location
The size and location of an AVM are key. Larger or harder-to-reach AVMs might need a different doctor than smaller ones.
For example, a neurosurgeon might treat a small AVM. But a bigger or deeper AVM might need an interventional neuroradiologist for embolization.
Patient Age and Overall Health
The patient’s age and health matter a lot. Older patients or those with health issues might not be good candidates for surgery. This makes radiation oncology a better option.
Younger patients with fewer health problems might do better with surgery or endovascular treatment.
Risk of Rupture
The risk of rupture is very important. AVMs at high risk might need quick and aggressive treatment. This could involve a neurosurgeon or interventional neuroradiologist.
Previous Treatments
What treatments the patient has had before also matters. For example, a patient who has had embolization might need a different approach. This could involve radiation oncology for any remaining AVM.
|
Factor |
Influence on Specialist Choice |
Potential Specialist |
|---|---|---|
|
AVM Size and Location |
Larger or deeper AVMs may require more complex treatment |
Neurosurgeon, Interventional Neuroradiologist |
|
Patient Age and Health |
Older or less healthy patients may require less invasive treatment |
Radiation Oncologist |
|
Risk of Rupture |
Higher risk may necessitate more aggressive treatment |
Neurosurgeon, Interventional Neuroradiologist |
|
Previous Treatments |
Previous treatments can influence the choice of subsequent treatments |
Various specialists based on previous treatment |
In conclusion, picking the right specialist for AVM treatment is complex. It depends on many factors like AVM size, patient age, risk of rupture, and previous treatments. A team of specialists is best to find the right treatment plan.
The Diagnostic Process: Who Identifies AVMs?
Diagnosing arteriovenous malformations (AVMs) is a complex task. It needs the skills of many medical experts. The process involves different tools and methods to find the right diagnosis.
Neurologists and Initial Diagnosis
Neurologists are often the first to spot AVMs. They check patients with symptoms like seizures or brain problems. They might start with tests like CT scans or MRI to look for issues.
Neuroradiologists and Advanced Imaging
Neuroradiologists are key when something looks off. They use special imaging like digital subtraction angiography (DSA). This method gives clear pictures of the AVM’s size and where it is.
Referral to Treatment Specialists
After finding an AVM, doctors send patients to a team for treatment. This team might include neurosurgeons, interventional neuroradiologists, and radiation oncologists. They decide the best treatment based on the AVM and the patient’s health.
|
Specialist |
Role in AVM Diagnosis |
|---|---|
|
Neurologist |
Initial evaluation and ordering preliminary imaging tests |
|
Neuroradiologist |
Advanced imaging techniques for detailed AVM assessment |
|
Treatment Specialists |
Determining the best treatment plan based on AVM characteristics and patient health |
The process of finding and treating AVMs is a team effort. Knowing who does what helps patients understand their journey better.
Risks and Complications: How Different Specialists Manage Them
Dealing with AVMs needs a deep understanding of the condition and managing risks. Specialists play key roles in reducing these risks. This ensures the best results for patients.
Surgical Complications and Management
Surgery to remove AVMs is complex and comes with risks like bleeding, infection, and neurological damage. Neurosurgeons plan and perform the surgery carefully. They use advanced imaging and monitoring to manage these risks.
Intraoperative angiography helps surgeons check if the AVM is fully removed. This reduces the chance of leftover malformation. Specialized care in a neurosurgical ICU is also key for managing complications after surgery.
Embolization Risks
Endovascular embolization for AVMs also has risks, like ischemic complications and unintended embolization of normal vessels. Interventional neuroradiologists need to understand the AVM’s structure well to lower these risks.
Using advanced embolic materials and techniques has made embolization safer and more effective. But, careful patient selection and planning are necessary to avoid complications.
Radiosurgery Side Effects
Stereotactic radiosurgery is a non-invasive option for AVMs, but it has risks. Radiation-induced complications, such as edema and radiation necrosis, can happen. Radiation oncologists must plan the treatment carefully to avoid harming surrounding brain tissue.
Follow-up care is important for managing radiosurgery risks. It helps in early detection and treatment of any side effects.
Emergency Response to AVM Rupture
AVM rupture can happen despite preventive measures. Emergency response protocols are key for managing acute hemorrhage. This includes quick imaging, neurosurgical consultation, and sometimes emergency embolization or surgery.
A team of neurosurgeons, interventional neuroradiologists, and critical care specialists is vital. They work together to stabilize the patient and prevent further issues.
AVM Centers of Excellence in the United States
In the U.S., many top centers offer the best AVM treatment. These places have expert teams, the latest tech, and a focus on quality care.
Finding Specialized AVM Teams
Finding the right AVM treatment team is key. Start by asking your doctor for referrals. Professional groups like the American Association of Neurological Surgeons also help find specialists.
Look into the team’s credentials and success stories. Check their technology and what patients say about them.
Choosing a top AVM treatment center is important. Look at the team’s experience and the tech they use. This helps patients make good choices.
In conclusion, the U.S. has many AVM treatment centers. Understanding the need for specialized care and experienced teams helps patients choose wisely.
Patient Experiences and Outcomes with Different AVM Treatment Specialists
Patient outcomes and experiences with AVM treatment specialists vary a lot. This is due to several key factors. These include the type of treatment and the specialist’s expertise.
Recovery Timelines by Treatment Type
The recovery process for AVM patients changes a lot based on the treatment. For example, patients who get surgical resection might take longer to recover. This is compared to those who get stereotactic radiosurgery.
Recovery times can range from a few weeks for less invasive procedures to several months for more invasive ones.
Quality of Life Considerations
Quality of life is a big part of AVM treatment outcomes. Patients who get treated by specialists who use a team approach often have a better quality of life.
Things that affect quality of life include any neurological problems after treatment, the need for ongoing medication, and the emotional impact of the diagnosis and treatment.
Long-term Follow-up Requirements
Long-term follow-up is key for AVM patients, no matter the treatment. They need regular imaging studies to watch for any problems or if the AVM comes back.
The number of follow-up visits can change. Patients who get radiosurgery might need to be checked more often than those who have surgery.
In conclusion, it’s important to understand the differences in patient experiences and outcomes with different AVM treatment specialists. This helps make better treatment choices.
Emerging Techniques and Future of AVM Treatment
The world of Arteriovenous Malformation (AVM) treatment is changing fast. New medical technologies and methods are coming out. These advancements aim to make treatments better for patients.
Advances in Microsurgery
Microsurgery has long been key in treating AVMs. Recent improvements have made it even better. Improved microsurgical techniques now help remove AVMs more precisely, cutting down on risks.
High-resolution imaging and intraoperative monitoring are now common. They help surgeons work in complex areas with more accuracy.
New Endovascular Approaches
Endovascular methods have also made big strides. They offer less invasive ways to treat AVMs. New embolic materials and improved catheter designs make these procedures safer and more effective.
Techniques like liquid embolization and stent-assisted coiling are getting better. They give more choices for patients with hard-to-treat AVMs.
|
Treatment Approach |
Advantages |
Limitations |
|---|---|---|
|
Microsurgery |
High precision, immediate results |
Invasive, risk of surgical complications |
|
Endovascular Embolization |
Minimally invasive, reduced recovery time |
Limited by AVM size and location, risk of incomplete occlusion |
|
Stereotactic Radiosurgery |
Non-invasive, effective for small AVMs |
Delayed effect, risk of radiation-induced complications |
Hybrid Operating Rooms and Combined Specialties
Hybrid operating rooms are changing AVM treatment. They let teams do combined endovascular and surgical procedures together. This teamwork improves results.
Advanced imaging in these rooms helps teams work better. It makes both endovascular and surgical steps more precise.
The future of AVM treatment looks bright. With new tech and teamwork, care will keep getting better for patients.
Conclusion
Knowing who does AVM surgery is key for patients looking for the best treatment. A team of experts, including neurosurgeons and interventional neuroradiologists, is vital. They work together to give the best care for AVMs.
This team approach means patients get treatment plans made just for them. They use surgery, endovascular embolization, and radiosurgery to help patients. This way, they can get the best results possible.
The teamwork in AVM treatment is very important. It helps patients get the best care with fewer risks. As AVM treatment gets better, the team’s role will stay critical in giving top-notch care.
FAQ
What is an Arteriovenous Malformation (AVM)?
An AVM is a tangled mess of blood vessels in the brain or spine. It can mess up normal blood flow. This might cause bleeding or other problems.
Who treats Arteriovenous Malformations?
A team of experts usually treats AVMs. This team includes neurosurgeons, interventional neuroradiologists, and radiation oncologists.
What is the role of a neurosurgeon in AVM treatment?
Neurosurgeons are skilled in removing or repairing AVMs. They often lead in planning and coordinating treatment.
What is embolization, and who performs it?
Embolization is a procedure that blocks blood flow to an AVM. It’s done by interventional neuroradiologists.
What is stereotactic radiosurgery, and who performs it?
Stereotactic radiosurgery uses radiation to destroy an AVM. It’s performed by radiation oncologists.
What are the risks and complications of AVM treatment?
Treatment can have risks like surgical complications, embolization risks, and radiosurgery side effects. Specialists manage these risks differently.
How is an AVM diagnosed?
AVMs are diagnosed with advanced imaging like MRI or angiography. Neuroradiologists often do this.
What factors determine which specialist will perform AVM treatment?
Several things decide who treats an AVM. These include the AVM’s size and location, the patient’s age and health, and the risk of rupture.
What are the different treatment options for AVMs?
Treatment options include surgery, embolization, radiosurgery, or a mix of these.
What is the importance of a multidisciplinary team approach in AVM management?
A team approach ensures patients get the best care. Different specialists bring their expertise to the planning process.
How do I find a specialist for AVM treatment?
To find a specialist, talk to your primary care doctor or get referrals. You can also look for AVM Centers of Excellence.
What are AVM Centers of Excellence?
AVM Centers of Excellence have programs for AVM treatment. They have experienced teams and modern facilities.
What are the emerging techniques in AVM treatment?
New techniques include better microsurgery, new endovascular methods, and hybrid operating rooms.
What is the role of cerebral arteriovenous malformation (AVM) specialists in treatment?
Specialists like neurosurgeons, interventional neuroradiologists, and radiation oncologists work together. They provide complete care for AVM patients.
Reference
Surgical management of auricular arteriovenous malformations: A literature review. https://pmc.ncbi.nlm.nih.gov/articles/PMC9008162/























