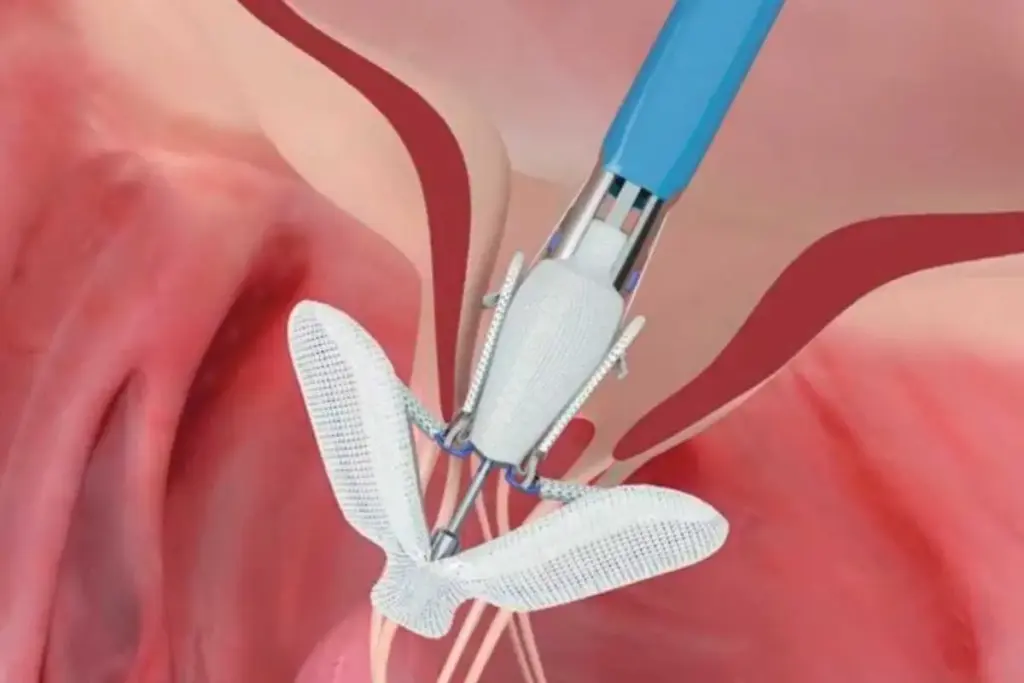
Transcatheter aortic valve replacement (TAVR) has changed how we treat aortic stenosis. It’s a less invasive option compared to open-heart surgery. But, like any medical procedure, TAVR comes with risks. Significant complications can affect how long a patient lives and their quality of life. It’s important for doctors and patients to know about these risks.
The “big five” complications of TAVR are very important. These include severe or moderate paravalvular leak, major vascular and bleeding issues, disabling stroke, acute kidney injury, and severe conduction disorders. It’s key to recognize and reduce these risks to improve patient outcomes. Big Five Complications After Transcatheter Aortic Valve Replacement: Crucial Risks
Key Takeaways
- TAVR is a less invasive alternative to traditional aortic valve replacement surgery.
- The “big five” TAVR complications significantly impact patient survival and quality of life.
- Understanding TAVR complications is important for doctors and patients.
- Severe or moderate paravalvular leak is a big complication of TAVR.
- Major vascular and bleeding complications are significant adverse events associated with TAVR.
Understanding Transcatheter Aortic Valve Replacement (TAVR)
TAVR has changed how we treat aortic valve disease. It’s a less invasive method that has made treating aortic stenosis easier. Aortic stenosis is when the aortic valve opening gets too narrow.
The TAVR Procedure Explained
The TAVR procedure puts a new valve in place through a catheter. This catheter goes in through an artery in the leg or chest. This method is less invasive than open-heart surgery. It means less recovery time and fewer risks.
Evolution and Current State of TAVR
Over time, TAVR has gotten better. It’s now used for more people, even those at lower risk. Thanks to new technology, the results are better and there are fewer problems.
Comparing TAVR to Surgical Valve Replacement
TAVR has many benefits over traditional surgery. It has fewer risks, shorter hospital stays, and quicker recovery. But, whether to choose TAVR or surgery depends on the patient. It’s based on their health and the shape of their heart.
The Big Five Complications After Transcatheter Aortic Valve Replacement
It’s key to know about TAVR complications to better care for patients. The big five complications after TAVR greatly affect patients’ lives and health.
Significance of Post-TAVR Complications
Complications after TAVR can make patients sicker, increase death rates, and raise healthcare costs. It’s vital to spot and handle these issues to improve care.
Incidence Rates and Trends
Research shows different rates for TAVR complications. The table below lists the big five complications’ rates after TAVR.
|
Complication |
Incidence Rate (%) |
|---|---|
|
Stroke |
2-5 |
|
Vascular Access Complications |
5-10 |
|
Conduction Abnormalities |
10-20 |
|
Bleeding Complications |
5-15 |
|
Paravalvular Leak |
5-15 |
Impact on Patient Outcomes and Quality of Life
The big five complications after TAVR can really harm patients’ health and happiness. Good management plans are needed to lessen these issues and help patients more.
By grasping the importance, rates, and effects of TAVR complications, doctors can create better plans to help patients.
Stroke and Neurovascular Events
Neurovascular events, like stroke, are serious issues after TAVR. They need careful management and prevention. Stroke is a major concern because it affects patient outcomes and quality of life.
Mechanisms of Stroke During and After TAVR
Stroke during and after TAVR happens for many reasons. Embolic events and hypoperfusion are key factors. Embolic events often come from the procedure itself.
Risk Factors for Neurovascular Complications
Several factors increase the risk of neurovascular complications after TAVR. These include advanced age, history of stroke or transient ischemic attack, and presence of atrial fibrillation.
Prevention Strategies and Cerebral Protection Devices
To lower stroke risk, cerebral protection devices have been created. These devices aim to catch embolic debris before it hits the brain, reducing stroke risk.
“The use of cerebral protection devices during TAVR has shown promise in reducing the risk of stroke, though their routine use is being studied.”
Management of Post-TAVR Stroke
Managing stroke after TAVR is urgent. It involves immediate neurological assessment and appropriate antithrombotic therapy. The aim is to lessen brain damage and improve outcomes.
Effective prevention and management are key to lowering stroke risk after TAVR. Understanding the causes and risk factors helps healthcare providers tailor care better.
Vascular Access Complications
The success of TAVR depends on avoiding vascular access problems. These issues can affect how well a patient does. It’s important to know about the types of injuries, risk factors, and how to prevent and treat them.
Types of Vascular Injuries
Vascular injuries from TAVR can be small or serious. Major complications include big bleeds, artery tears, and fake aneurysms. Minor complications might be small blood clots or temporary issues at the access site.
Risk Factors for Vascular Complications
Some things make vascular problems more likely during TAVR. These include advanced age, female gender, and peripheral artery disease. The size and type of delivery system also play a role.
Preventative Approaches and Access Site Selection
Picking the right access site is key to avoiding vascular problems. Pre-procedural imaging helps check the blood vessels and spot risks. Using smaller sheaths and a minimally invasive approach can also help.
Treatment Options for Vascular Complications
When vascular problems happen, quick and effective treatment is needed. Endovascular repair is often the first choice for big injuries, being less invasive than surgery. Sometimes, surgical intervention is needed for severe damage.
Experts say, “The key to managing vascular access complications lies in prevention and preparedness.” Good management can greatly improve patient outcomes and lower the risk of TAVR complications.
“Careful planning and execution are key to avoiding vascular access complications during TAVR procedures.”
Conduction Abnormalities and Pacemaker Implantation
After TAVR, many people face conduction disturbances. This often means they need a pacemaker. It’s important to understand why this happens to help manage their care.
Mechanisms of Conduction Disturbances
There are several reasons for conduction disturbances after TAVR. The main ones are the valve’s close location to the heart’s electrical system. Also, how the valve is placed can affect nearby tissues. And, some people might already have heart conduction issues.
Key factors contributing to conduction disturbances:
- Anatomical proximity to the conduction system
- Effects of valve implantation
- Pre-existing conduction abnormalities
Predictors of Conduction Abnormalities
Knowing who might face conduction issues is key. This helps doctors plan better care. Factors include:
|
Predictor |
Description |
|---|---|
|
Pre-existing RBBB |
Right bundle branch block, a condition that affects the electrical conduction system of the heart. |
|
Depth of Implantation |
The depth at which the valve is implanted can affect the surrounding conduction system. |
|
Calcium Burden |
The amount of calcium on the valve can influence the risk of conduction disturbances. |
Management Strategies and Monitoring Protocols
Managing conduction issues requires careful watching and quick action. Doctors should keep a close eye on patients after TAVR. They should also be ready to implant a pacemaker if needed.
Long-term Implications of Pacemaker Dependency
Living with a pacemaker after TAVR has its challenges. Patients need ongoing care, might face battery issues, and could deal with emotional stress. It’s vital to understand these challenges to provide the best care.
Long-term care considerations:
- Ongoing pacemaker monitoring
- Patient education on pacemaker dependency
- Psychological support
Bleeding Complications
After TAVR, patients face the risk of bleeding complications. These can greatly affect their quality of life. It’s important to know how to manage and prevent these issues for better care.
Classification of Bleeding Events
Bleeding events after TAVR vary in severity and location. The Valve Academic Research Consortium (VARC) criteria help standardize these definitions. VARC divides bleeding into major, minor, and life-threatening categories.
|
Bleeding Classification |
Description |
|---|---|
|
Major Bleeding |
Overt bleeding with a drop in hemoglobin of ≥3 g/dL or requiring transfusion of ≥2 units of blood |
|
Minor Bleeding |
Overt bleeding not meeting criteria for major bleeding |
|
Life-Threatening Bleeding |
Bleeding with fatal outcome, or bleeding in a critical organ, or bleeding requiring surgical intervention |
Risk Factors for Bleeding
Several factors increase the risk of bleeding after TAVR. These include patient-related factors, procedural factors, and post-procedural antithrombotic therapy. Patient-related factors like advanced age, renal impairment, and female gender are linked to higher bleeding risk.
Antithrombotic Therapy Considerations
Antithrombotic therapy is key to prevent valve thrombosis and thromboembolic events after TAVR. Yet, it also raises the risk of bleeding. Finding the right balance is essential.
- Aspirin and P2Y12 inhibitors are commonly used in antithrombotic regimens.
- The duration and intensity of antithrombotic therapy should be tailored to the individual patient’s risk profile.
Management of Bleeding Complications
Managing bleeding complications after TAVR requires quick action and the right approach. This might include adjusting antithrombotic therapy, applying local compression, or using hemostatic agents. In severe cases, blood transfusions or surgery may be needed.
Understanding the risk factors and implementing strategies to minimize bleeding complications can improve patient outcomes after TAVR.
Paravalvular Leak
Paravalvular leak (PVL) is a big problem after TAVR. It happens when blood leaks around the new valve, not through it. This can be due to how the valve is placed or the patient’s body.
Mechanisms and Classification
PVL can happen for a few reasons. These include incomplete valve expansion, valve malpositioning, and calcification of the native valve. It’s classified from mild to severe, with severe being more serious.
Clinical Impact of Paravalvular Leak
PVL can have big effects on patients. It might cause heart failure, hemolysis, and the need for more surgery. How bad the PVL is determines how serious it is.
Predictors and Prevention Strategies
Things that might lead to PVL include patient-specific factors and procedural factors. To prevent it, doctors plan carefully, place the valve right, and use imaging modalities to guide them.
Treatment Options for Significant Paravalvular Leak
For serious PVL, treatments vary. Mild cases might just need watching, while severe cases might need reintervention. This could be balloon post-dilation, valve-in-valve TAVR, or surgical correction. The right treatment depends on the patient and the PVL.
In summary, PVL is a serious issue after TAVR. Knowing how it happens, who’s at risk, and how to treat it is key to helping patients.
Risk Assessment and Patient Management Strategies
TAVR is growing, and so is the need for detailed risk checks and patient care plans. Managing patients well before and after TAVR is key. It’s a team effort that starts early and goes on after the procedure.
Pre-procedural Evaluation and Risk Scoring
Checking patients thoroughly before TAVR is vital. It helps spot risks and predict how well the procedure will go. This way, doctors can sort patients by how risky they are.
Individualized Approach to Patient Selection
Choosing the right patient for TAVR is all about personal touch. Doctors look at the patient’s health history, current state, and what they want. This makes treatment fit the patient better, leading to better results and fewer problems.
Post-TAVR Monitoring and Follow-up Protocols
Keeping an eye on patients after TAVR is essential. Regular check-ups help catch and fix problems early. This makes patients’ lives better and their health outcomes better too.
Multidisciplinary Heart Team Approach
A team of experts is key to good TAVR care. Cardiologists, surgeons, and imaging experts work together. They give patients the best care possible, covering all their needs.
In short, careful risk checks and patient plans are vital for TAVR success. A team effort and care tailored to each patient lead to better lives and outcomes.
Conclusion: Advancing TAVR Safety and Outcomes
Transcatheter aortic valve replacement (TAVR) is becoming more common. It’s important to know about the big five complications after it. This knowledge helps improve patient care.
Improving TAVR safety involves new technology and techniques. It also means following the latest guidelines. Learning from past experiences is also key.
Looking at long-term trends helps doctors predict and manage risks. This leads to better results for patients. Keeping up with new guidelines is also vital for safety.
Refining TAVR technology and understanding its safety better are important. These efforts will shape the future of TAVR. It’s critical to keep working on making TAVR safer and better for patients.
FAQ
What are the big five complications after a transcatheter aortic valve replacement?
The big five complications after TAVR include stroke and neurovascular events. Vascular access complications and conduction abnormalities are also common. Bleeding and paravalvular leak are the last two.
How does TAVR compare to traditional surgical valve replacement in terms of complications?
TAVR has a different set of complications compared to surgery. It has less bleeding and infection risk. But, it has more vascular access and paravalvular leak risks.
What are the risk factors for stroke during and after TAVR?
Advanced age and stroke history are stroke risk factors for TAVR. Atrial fibrillation and aortic disease also increase the risk.
How can vascular access complications be minimized during TAVR?
To reduce vascular access complications, plan and execute carefully. Use imaging and choose the right access site. Vascular closure devices help too.
What are the predictors of conduction abnormalities after TAVR?
Conduction problems after TAVR are linked to pre-existing disease and left ventricular hypertrophy. The depth of valve implantation also matters.
How is bleeding risk assessed and managed after TAVR?
Bleeding risk is assessed with risk scores after TAVR. Manage it with antithrombotic therapy and careful monitoring. Use bleeding avoidance strategies too.
What are the treatment options for significant paravalvular leak after TAVR?
For significant leaks after TAVR, consider post-dilation or valve-in-valve implantation. Closure devices are also an option. The choice depends on the leak’s severity and location.
What is the role of a multidisciplinary heart team in TAVR patient management?
A multidisciplinary team is key in TAVR management. They evaluate, select patients, and monitor post-TAVR. Their role is vital.
How can long-term outcomes be improved after TAVR?
Improve long-term outcomes by selecting patients carefully and using the best techniques. Close follow-up and monitoring are also essential. Ongoing safety and outcome advancements help too.
What are the current guideline updates for TAVR safety and outcomes?
Current guidelines stress the importance of a multidisciplinary team. They emphasize careful patient selection and ongoing monitoring. Evidence-based practices are key to minimizing complications and improving outcomes.
What are the preventative strategies for TAVR complications?
Prevent TAVR complications by selecting patients carefully and using the best techniques. Evidence-based practices and ongoing safety efforts are also important.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7443820/



































