
Every year, thousands of people face leg blood clots that can be very serious. A potentially life-threatening condition, blood clots often show subtle signs. We aim to help you spot the silent symptoms of a blood clot in a leg.
It’s vital to catch these signs early. Leg blood clots symptoms might include swelling, pain, or color changes in the leg. Knowing these signs helps you get medical help fast.
Key Takeaways
- Leg blood clots can lead to serious health issues if not treated early.
- Silent symptoms include swelling, pain, or discoloration.
- Awareness of these signs can save lives.
- Prompt medical attention is key when symptoms appear.
- Early detection is essential for effective treatment.
Understanding Blood Clots: Formation and Types
It’s important to know how blood clots form and the types that exist. Blood clots are made through a complex process. This process occurs when a blood vessel is injured.
The body tries to stop the bleeding by forming a clot. This is a natural response.
The Blood Clotting Process
The blood clotting process, or coagulation, has several steps. These steps lead to the formation of a fibrin clot. This clot is essential for stopping excessive bleeding when a blood vessel is damaged.
But, if this process happens too much or in the wrong way, it can cause harmful clots.
Beneficial vs. Harmful Blood Clots
Not all blood clots are bad. Some clots help stop bleeding and let healing happen. But, other clots can block blood flow or travel to other parts of the body.
This can cause serious conditions like pulmonary embolism or stroke.
Common Locations for Blood Clots
Blood clots can form anywhere in the body. But, they are more likely to happen in certain areas. Deep vein thrombosis (DVT) is when a clot forms in the deep veins, usually in the legs.
Other common places include the arms, lungs (pulmonary embolism), and brain (stroke).
|
Location |
Type of Clot |
Potential Complication |
|---|---|---|
|
Legs |
Deep Vein Thrombosis (DVT) |
Pulmonary Embolism |
|
Lungs |
Pulmonary Embolism |
Respiratory Failure |
|
Brain |
Stroke |
Brain Damage |
In conclusion, knowing about blood clots is key to understanding their risks. By understanding how they form and where they can occur, we can spot health threats early. This helps us get medical help quickly.
Deep Vein Thrombosis (DVT): The Most Common Dangerous Clot
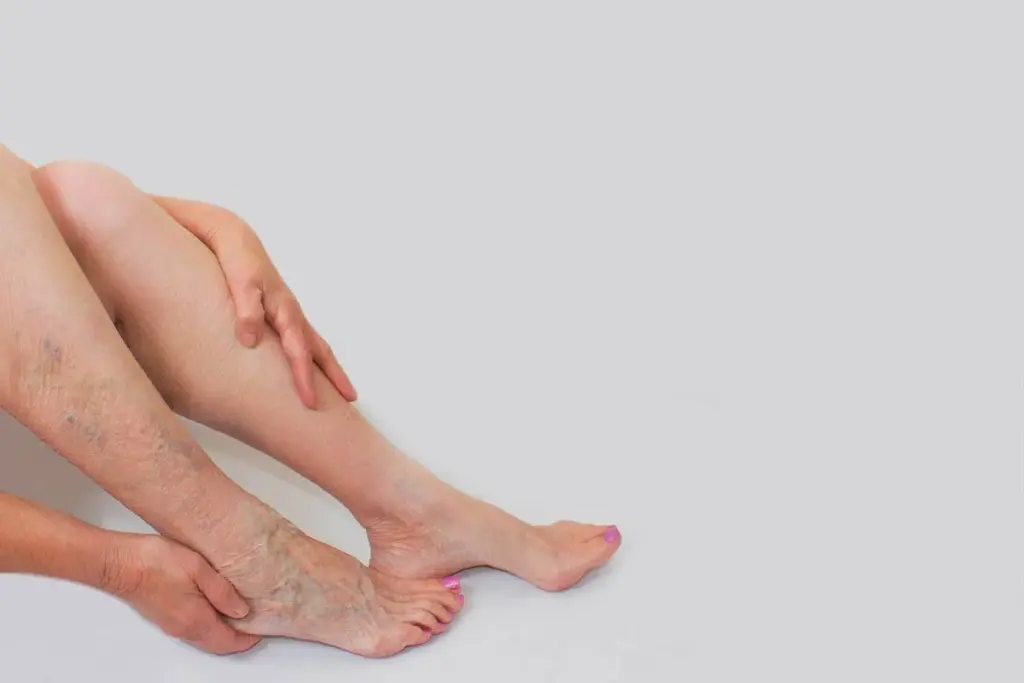
Deep Vein Thrombosis (DVT) is a common and dangerous blood clot. It forms in deep veins, usually in the legs. We will look at what DVT is, where it happens, and its serious link to pulmonary embolism.
What Makes DVT Different
DVT is different because it forms in deep veins. Unlike surface clots, DVTs are more dangerous. They can break loose and travel to the lungs, causing a pulmonary embolism. This can be deadly if not treated right away.
Common Locations for DVT
DVT often happens in the legs, mainly in the calf and thigh. It can also occur in other deep veins, but leg DVT is most common. Prolonged sitting, genetics, and certain health issues can raise your risk.
The Relationship Between DVT and Pulmonary Embolism
DVT and pulmonary embolism are closely linked. When a DVT clot breaks loose, it can travel to the lungs. This can block blood flow to the lungs, leading to serious health problems, including death. Knowing the risks of DVT is key to preventing such outcomes.
Blood Clot in a Leg Symptoms: The Classic Warning Signs
Leg blood clot symptoms include swelling, pain, and skin discoloration. These signs are important to spot early. A blood clot in the leg, or deep vein thrombosis (DVT), is serious and can be deadly if not treated fast. We’ll cover the key signs to help you catch clots early.
Swelling in the Affected Leg
Swelling is a common sign of a blood clot in the leg. This happens because the clot blocks blood flow, leading to fluid buildup in the limb. Swelling can be in one spot or spread across the leg.
Pain and Tenderness
Pain or tenderness in the leg is another big symptom. The pain can feel like a dull ache or a sharp, severe pain. It often gets worse when you stand or walk. It’s important to tell this pain apart from muscle strains.
Skin Discoloration and Warmth
The skin around the clot may turn red or blue and feel warm. This happens because of the inflammation caused by the clot.
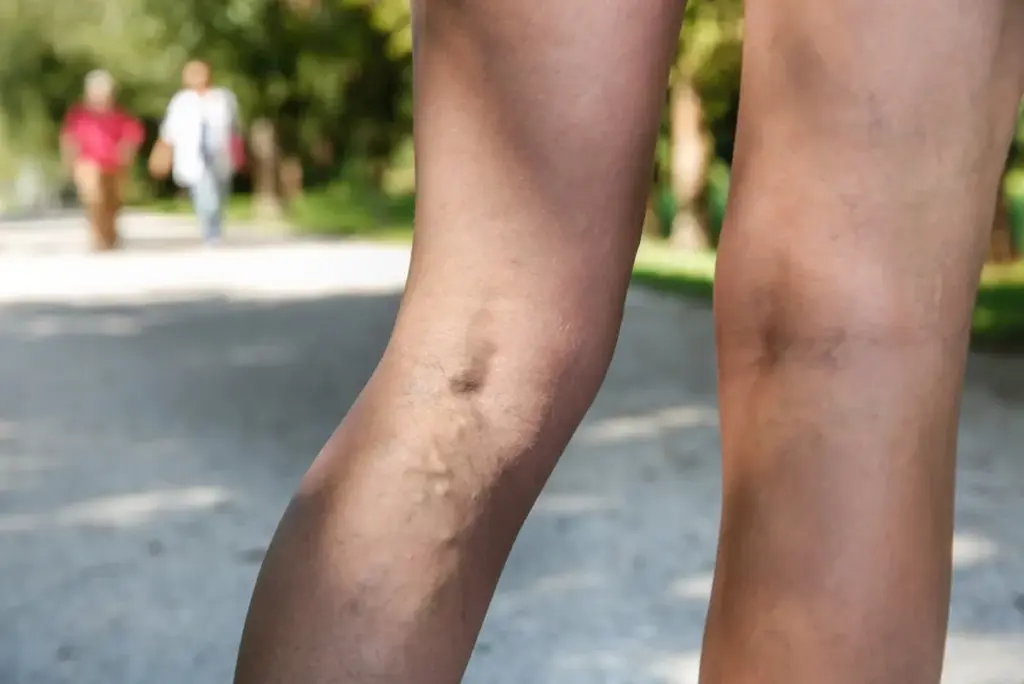
Visible Surface Veins
In some cases, you might see the surface veins more clearly. This is a sign that the clot is big enough to block normal blood flow.
|
Symptom |
Description |
|---|---|
|
Swelling |
Localized or widespread swelling due to obstructed blood flow |
|
Pain/Tenderness |
Dull ache or sharp pain, often worsened by standing or walking |
|
Skin Discoloration |
Red or blue discoloration due to inflammation |
|
Visible Surface Veins |
Increased visibility of veins due to altered circulation |
Spotting these classic warning signs early can greatly improve treatment outcomes for leg blood clots. If you or someone you know shows these symptoms, getting medical help right away is key.
Silent and Subtle Symptoms That Are Often Missed
Not all blood clot symptoms are dramatic. Sometimes, it’s the quiet signs that need our attention. Knowing these subtle indicators is key to getting medical help on time.
Mild Calf Discomfort Mistaken for Muscle Soreness
Mild calf discomfort can be a sign of a blood clot. It might feel like muscle soreness, but it’s important to notice it. Paying attention to any unusual sensations in your calf can help catch it early.
Slight Swelling That Goes Unnoticed
Even slight swelling in one leg can be a sign of a blood clot. This swelling might be so small you don’t notice it until it gets worse. Checking your legs for swelling regularly can help spot a clot early.
Unexplained Fatigue and Malaise
Feeling tired or unwell without a clear reason can be a sign of a blood clot. Fatigue is common, but if you’re feeling it a lot, it could mean something serious. Talking to your doctor about persistent fatigue is important.
Skin Changes Without Pain
Skin changes like discoloration or redness without pain can also be a sign. These changes might be small and easy to miss. Keeping an eye on your skin for any unusual changes is a good habit.
|
Subtle Symptom |
Description |
Action |
|---|---|---|
|
Mild Calf Discomfort |
Discomfort that feels like muscle soreness |
Monitor for unusual sensations |
|
Slight Swelling |
Minor swelling in one leg |
Regularly check leg swelling |
|
Unexplained Fatigue |
Feeling tired without a clear reason |
Discuss persistent fatigue with a healthcare provider |
|
Skin Changes |
Discoloration or redness without pain |
Monitor skin for unusual changes |
Knowing about these silent symptoms can help catch blood clots early. If you notice any of these signs, seeing a doctor is very important.
Differentiating Blood Clots From Other Conditions
It’s not always easy to tell if symptoms are from a blood clot or something else. Blood clots can look like muscle strains, cellulitis, or peripheral artery disease. We must look closely at the symptoms and the patient’s health history to figure it out.
Blood Clots vs. Muscle Strains
Muscle strains and blood clots can both cause pain and swelling in the legs. But muscle strains usually happen after you’ve been active. Blood clots can happen anytime and aren’t always linked to activity.
If the pain gets worse or you see skin color changes, it might be a blood clot. This is different from a muscle strain.
Blood Clots vs. Cellulitis
Cellulitis is a skin infection that causes redness, swelling, and warmth. These signs can also show up with blood clots. But cellulitis often comes with a fever and more intense redness.
It’s important to look closely and might need tests to tell them apart.
Blood Clots vs. Peripheral Artery Disease
Peripheral artery disease (PAD) is when arteries narrow, cutting off blood flow. It can cause pain in the legs when walking, which might seem like a blood clot. But PAD pain usually goes away when you rest.
Blood clot symptoms can happen even when you’re not moving.
When to Suspect a Clot
If someone suddenly has leg pain or swelling, with warmth, redness, or color changes, think of a blood clot. A detailed medical history and physical check are key. Tests like ultrasound can confirm if there’s a clot.
Recognizing Dangerous Progression of Symptoms
It’s important to know when a blood clot is getting worse. Blood clots can cause serious problems if not treated quickly. Knowing the signs of a worsening condition is key.
When Leg Symptoms Worsen Rapidly
If your leg symptoms get worse fast, like more pain or swelling, it might mean the clot is growing. Seeking medical help right away is vital to avoid more serious issues.
- Increased pain or tenderness in the affected leg
- Swelling that worsens over time
- Redness or discoloration of the skin
Signs the Clot May Be Moving
A moving blood clot is very dangerous. It can go to the lungs and cause a pulmonary embolism. Look out for these signs:
- Sudden chest pain or discomfort
- Shortness of breath or difficulty breathing
- Rapid heartbeat or palpitations
Warning Signs of Pulmonary Embolism
Pulmonary embolism is a serious issue that needs quick medical help. Watch for these signs:
- Chest pain that worsens with deep breathing
- Coughing up blood
- Lightheadedness or fainting
Symptoms Requiring Immediate Emergency Care
If you have these symptoms, get emergency care right away:
- Severe difficulty breathing
- Chest pain or pressure
- Severe pain or swelling in the legs
Knowing these symptoms and getting medical help quickly can greatly improve your chances of recovery from blood clots.
Risk Factors That Increase Your Chances of Developing Blood Clots
Many factors can raise your risk of getting blood clots. Knowing these can help you prevent them. We’ll look at genetic predispositions, lifestyle choices, medical conditions, and medications that might cause clots.
Genetic Predispositions
Some people are more likely to get blood clots because of their genes. Conditions like Factor V Leiden and Antithrombin III deficiency make clotting more common.
Lifestyle Factors
Our lifestyle choices can also affect our risk of blood clots. For example, long periods of sitting, like on flights or in bed, can lead to clots.
Medical Conditions That Increase Risk
Some health issues can also raise your risk of blood clots. These include cancer, heart disease, and obesity. Knowing these risks can help you manage them better.
Medications That May Contribute to Clotting
Some medicines, like hormonal contraceptives and hormone replacement therapy, can increase clot risk. It’s important to talk to your doctor about these risks.
|
Risk Factor |
Description |
Preventive Measures |
|---|---|---|
|
Genetic Predispositions |
Conditions like Factor V Leiden |
Genetic testing and counseling |
|
Lifestyle Factors |
Prolonged immobility |
Regular movement and exercise |
|
Medical Conditions |
Cancer, heart disease, obesity |
Managing underlying conditions |
|
Medications |
Hormonal contraceptives |
Discussing risks with healthcare provider |
Understanding these risk factors can help you lower your chance of blood clots. It’s key to know your personal risks and talk to your doctor about them.
How Blood Clots Are Diagnosed: From Symptoms to Confirmation
Diagnosing blood clots involves many steps. Doctors use different methods to find out if a clot is present. When someone shows signs of a blood clot, doctors start a detailed check-up.
Physical Examination Techniques
A physical exam is the first step in finding a blood clot. Doctors look for swelling, redness, and warmth in the affected area. They also check for pain when they press on it.
Imaging Tests for Blood Clots
Imaging tests are key to confirm a blood clot. They help find where the clot is. Here are some common tests:
- Ultrasound: This test uses sound waves to see blood vessels and find clots.
- Venography: It’s an X-ray test that uses dye to show veins and clots.
- CT Scan: CT scans can spot clots in different parts of the body, like the lungs.
Blood Tests That Help Diagnose Clots
Blood tests are important in finding blood clots. The D-dimer test checks for a protein that shows when a clot breaks down.
The Diagnostic Process Timeline
How long it takes to diagnose a blood clot varies. It depends on the symptoms and tests used. Usually, doctors can make a diagnosis in a few hours.
Treatment Options for Blood Clots in the Leg
It’s important for patients and doctors to know about blood clot treatments. The right treatment can lower the chance of serious problems and help patients get better.
Anticoagulant Medications
Anticoagulant drugs are key in treating leg blood clots. They stop the clot from growing and prevent new ones. Heparin and warfarin are common, along with rivaroxaban and apixaban. The right drug depends on the patient’s health and the clot’s details.
Thrombolytic Therapy
Thrombolytic therapy is for serious clots. It uses drugs to break down the clot. But, it can cause bleeding and is used only when needed.
Surgical Interventions
Surgery might be needed for some blood clots. Thrombectomy removes the clot, and a vena cava filter stops clots from reaching the lungs. These are options when drugs don’t work or can’t be used.
Recovery and Follow-up Care
Recovery and check-ups are vital after treating blood clots. Patients should wear compression stockings to help circulation. They also need to see their doctor often and make healthy lifestyle choices to avoid future clots.
Preventing Blood Clots: Strategies for Everyone
We can lower blood clot risks by making lifestyle changes. Knowing what causes blood clots helps us take action. This improves our health.
Movement and Exercise Recommendations
Exercise is key to preventing blood clots. It boosts blood flow, lowering clot chances. Aim for 30 minutes of moderate exercise daily, like walking or swimming.
For those who can’t move much, simple leg exercises help. Ankle rotations and toe lifts are good. Avoid sitting for long periods, even on flights or trips.
Dietary Considerations
Eating right is vital for clot prevention. Omega-3s in foods like salmon help blood vessels. Eating fruits, veggies, and whole grains also boosts heart health.
Drinking water is linked to diet. It keeps blood flowing and prevents dehydration, which can lead to clots.
Hydration and Its Importance
Drinking enough water is key to preventing blood clots. Dehydration makes blood thicker and more likely to clot. Drink at least eight glasses a day, more if you’re active or in a hot place.
Compression Garments: Who Should Use Them
Compression stockings help prevent blood clots, mainly for those at high risk. They apply pressure to improve blood flow and lower clot risk.
See a doctor to see if you need compression garments. They’ll help choose the right fit and level of compression.
By following these tips, we can lower blood clot risks. This improves our health and well-being.
Special Risk Populations: Who Needs Extra Vigilance
Knowing who is at risk for blood clots can save lives. Some people are more likely to get blood clots because of their health or lifestyle. We must watch out for these groups to help prevent blood clots.
Pregnant Women and Postpartum Period
Pregnant women face a higher risk of blood clots. This is because of changes in blood and increased pressure from the growing uterus. The risk doesn’t stop after giving birth, so it’s important to stay alert during this time. A medical expert notes,
“Pregnancy is a hypercoagulable state, and understanding this can help us manage the risks associated with blood clots.”
Pregnant women should watch for signs of blood clots and tell their doctor if they notice anything unusual.
Cancer Patients
Cancer patients are more likely to get blood clots. This is because tumors can trigger the clotting system. Some cancers, like pancreatic cancer, are more linked to clotting problems. We need to keep a close eye on these patients and manage their risks well.
Post-Surgical Patients
Patients after surgery, like those who had hip or knee replacements, are at higher risk of blood clots. The risk is highest in the first few weeks but can last for months. Moving early and using blood-thinning medicines are key to lowering this risk.
Medical guidelines stress the importance of early mobilization and anticoagulant medications in preventing blood clots in post-surgical patients.
Long-Distance Travelers
People traveling long distances, like on flights or car rides over four hours, are at risk of blood clots. Staying hydrated, moving often, and wearing compression socks can help. It’s good for long-distance travelers to take breaks to stretch and move around.
By knowing who is at risk, we can take steps to prevent blood clots and save lives. It’s vital to be alert and take preventive actions seriously.
Living with Clotting Disorders: Long-term Management
For those with clotting disorders, managing the condition long-term is key. It helps avoid serious issues and boosts life quality. This management includes medical care, lifestyle changes, and constant monitoring.
Ongoing Medication Management
Medicine is a big part of managing clotting disorders. Doctors often give anticoagulant drugs to stop new clots and stop old ones from getting bigger. Sticking to the medication plan is very important to avoid problems.
It’s also important to have regular blood tests. These tests check if the medicine is working right. They help doctors adjust the dosage if needed. Patients should talk to their doctors about any side effects or drug interactions.
Lifestyle Adjustments
Making lifestyle changes can really help manage clotting disorders. Keeping a healthy weight, exercising regularly, and not sitting for too long can lower clot risk.
- Eating a balanced diet with lots of fruits, veggies, and whole grains
- Not smoking and drinking alcohol in moderation
- Drinking plenty of water to stay hydrated
Monitoring for Recurrence
It’s important to watch for any signs of clots coming back. Knowing the signs of deep vein thrombosis (DVT) and pulmonary embolism (PE) is key. If you notice any unusual symptoms, get medical help right away.
Psychological Impact of Chronic Clotting Risk
Clotting disorders can also affect your mind. Anxiety, fear, and depression are common. Getting help from doctors, support groups, or counselors can help deal with these feelings.
“Managing a clotting disorder needs a full approach. It’s about both physical and mental health. Working with doctors and making smart lifestyle choices can help manage the condition and improve life quality.”
Conclusion: Taking Action Against Silent Blood Clots
It’s important to know the signs of blood clots early. We’ve looked at how blood clots form and the dangers of Deep Vein Thrombosis (DVT). We’ve also talked about the quiet symptoms that are easy to miss.
Being aware of blood clots can save lives. Knowing the signs and risk factors helps us stay healthy. If you think you have a blood clot, get help right away.
Stopping silent blood clots needs knowledge and quick action. By staying informed and watching for symptoms, we can fight blood clot problems. This helps us stay healthy and avoid serious issues.
FAQ
What are the common symptoms of a blood clot in the leg?
A blood clot in the leg often causes swelling, pain or cramping (usually in one leg), warmth, redness or discoloration, and visible, enlarged surface veins, though some people have no clear symptoms.
Can a blood clot in the leg be painless?
Yes, a clot can be painless (a “silent” DVT), which makes it harder to detect, so swelling, skin color change, or warmth in one leg should still be evaluated even without pain.
How is a blood clot in the leg diagnosed?
Doctors start with a physical exam and symptom history, then usually order an ultrasound of the leg veins and sometimes a D‑dimer blood test or other imaging to confirm the clot.
What are the risk factors for developing a blood clot in the leg?
Risk factors include genetics, prolonged sitting or bed rest, cancer, surgery, heart disease, pregnancy, obesity, smoking, some medications (like estrogen‑based hormones), and major trauma.
Can blood clots move to other parts of the body?
Yes, part of a leg clot can break loose and travel through the bloodstream, most dangerously to the lungs, causing a pulmonary embolism.
What are the warning signs that a blood clot is moving?
Warning signs that a clot may have moved to the lungs include sudden shortness of breath, chest pain that worsens with breathing, rapid heart rate, dizziness or fainting, and sometimes coughing up blood; these need emergency care.
How are blood clots in the leg treated?
Treatment usually includes anticoagulant (“blood‑thinner”) medicines to stop the clot from growing, sometimes clot‑dissolving (thrombolytic) therapy, and in severe cases catheter‑guided or surgical clot removal.
Can blood clots be prevented?
Yes, you can lower the risk by staying active, avoiding long‑term sitting, managing weight and medical conditions, using compression stockings when advised, and, in high‑risk situations, taking preventive anticoagulants.
Are there any specific populations that are at higher risk for blood clots?
Higher‑risk groups include pregnant women, cancer patients, people after surgery or trauma, older adults, and long‑distance travelers, especially if they also have other risk factors.
What is the psychological impact of living with a clotting disorder?
Living with a clotting disorder can cause anxiety, fear of recurrence, and stress about long‑term medication, so psychological support, education, and regular follow‑up with a healthcare team are important.
References
https://www.ncbi.nlm.nih.gov/books/NBK507708


































