
Blood transfusions play a key role in cancer treatment. They help keep patients’ quality of life up during therapy. This allows for more aggressive treatments.
Cancer patients often get blood transfusions to fight anemia and other issues caused by treatment. About 18% of cancer surgery patients get blood transfusions before or after surgery.
The number of blood transfusions a patient gets depends on their cancer type and stage. It also depends on their treatment plan. Knowing how transfusions help in cancer care is key to better patient results.
Key Takeaways
- Cancer patients often need blood transfusions to handle treatment side effects.
- About 18% of cancer surgery patients get blood transfusions before or after surgery.
- The number of blood transfusions varies based on cancer type and stage.
- Blood transfusions are vital in supporting cancer treatment.
- They help keep patients’ quality of life good during therapy.
The Role of Blood Transfusions in Cancer Treatment
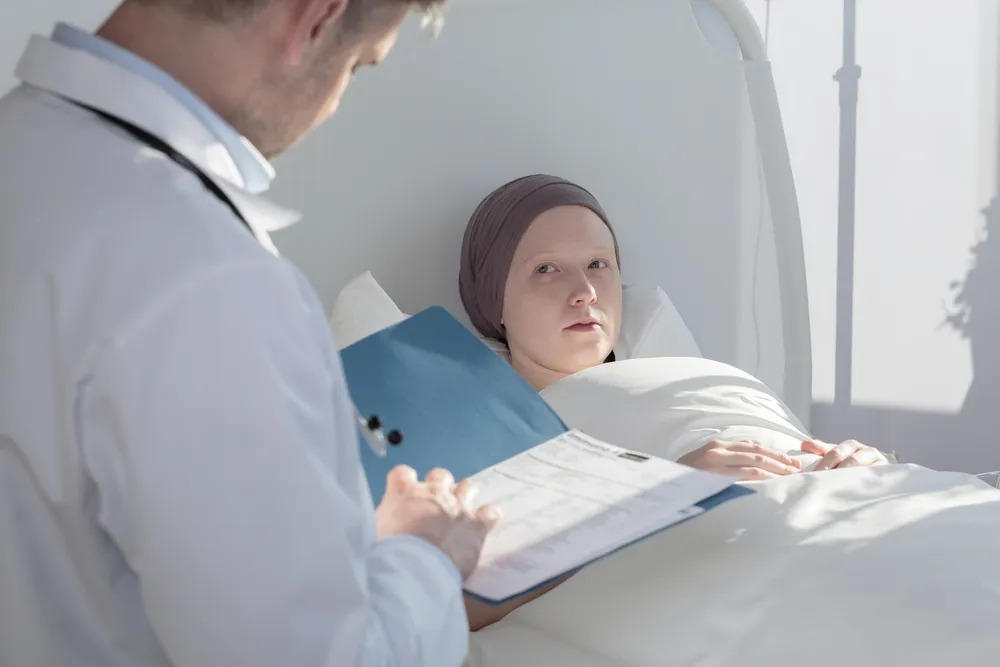
In oncology, blood transfusions are key in handling treatment side effects. They are vital for cancer patients going through chemotherapy, radiation, and surgery.
Common Blood Components Used in Oncology
Blood transfusions include different blood parts, such as:
- Red blood cells help fight anemia from cancer treatment.
- Platelets are needed to prevent and treat low platelet counts.
- Plasma has clotting factors and proteins for managing bleeding.
These parts are essential for supporting cancer patients during treatment.
Primary Reasons Cancer Patients Require Transfusions
Cancer patients need blood transfusions for several main reasons:
- Anemia Management: Chemotherapy and radiation can lower red blood cell production, causing anemia.
- Thrombocytopenia Treatment: Low platelet counts from treatment increase bleeding risks.
- Bleeding Complications: Surgery and some cancers can cause major blood loss, needing transfusions.
Medical experts say, “Blood transfusions are a key part of cancer patient care, helping reduce treatment side effects.”
Understanding blood transfusions in cancer treatment helps healthcare teams support patients better. This improves outcomes and quality of life.
Statistical Overview: Frequency of Transfusions in Cancer Care

The need for blood transfusions in cancer care changes a lot depending on the type and stage of cancer. This shows how different cancer patients have different needs during treatment.
General Prevalence Across Cancer Types
Blood transfusions are very important in cancer care. Research shows that how often transfusions are needed varies by cancer type. For example, people with blood cancers often need more transfusions than those with solid tumors.
Key statistics highlighting the prevalence include:
- About 18% of cancer surgery patients get red blood cell (RBC) transfusions before or after surgery.
- Patients getting chemotherapy or radiation might need transfusions because of anemia or low platelets caused by treatment.
The 18% Benchmark in Cancer Surgery Patients
The 18% rate for RBC transfusions in cancer surgery patients is a key number. This rate can change based on the surgery type, the patient’s health before surgery, and the hospital’s transfusion rules.
Variation by Cancer Type and Stage
The need for blood transfusions also changes with cancer type and stage. In later stages of cancer, patients often need more transfusions because of severe anemia or low platelets from the disease or treatment.
Factors influencing transfusion frequency include:
- The specific type of cancer and its stage.
- The treatment methods, like surgery, chemotherapy, or radiation.
- Things specific to the patient, like their starting hemoglobin levels and overall health.
Blood Therapy for Cancer: Supporting Treatment Protocols
Blood transfusions are key in cancer care. They help patients handle tough treatments. By adding blood components, transfusions lessen treatment side effects, supporting the treatment plan.
How Transfusions Complement Primary Cancer Treatments
Blood transfusions are vital for cancer treatments like chemotherapy and radiation. These treatments can cause anemia, low platelets, or low white blood cells. Targeted transfusions can manage these issues.
Transfusions keep blood cell counts up. This lets patients keep up with their treatments. It’s key for those getting intense chemotherapy or radiation.
Maintaining Quality of Life During Therapy
Keeping quality of life high is key in cancer care. Blood transfusions help a lot. They ease symptoms like tiredness, short breath, and dizziness from anemia.
|
Symptom |
Impact on Quality of Life |
Benefit of Blood Transfusion |
|---|---|---|
|
Fatigue |
Reduces ability to perform daily activities |
Improves energy levels |
|
Shortness of Breath |
Limitations in physical activity |
Enhances oxygen delivery |
|
Dizziness |
Increases risk of falls |
Stabilizes blood pressure |
Enabling Aggressive Treatment Approaches
Blood transfusions help reduce side effects of cancer therapy. This lets doctors use stronger treatments. This can lead to better results for patients with tough cancers.
Being able to use strong treatments is very important. It’s linked to better chances of beating cancer.
Declining Trends in Cancer-Related Transfusions
Recent studies have shown a big drop in cancer-related transfusions over the past few years. This change is thanks to better protocols and patient blood management strategies.
Statistical Evidence: From 20.1% to 12.7% (2012-2015)
A study found a drop in transfusion rates among cancer patients from 20.1% in 2012 to 12.7% in 2015. This shows a clear trend of less blood transfusions in cancer care.
Key statistics:
- 20.1% transfusion rate in 2012
- 12.7% transfusion rate in 2015
- 7.4% absolute reduction in transfusion rates over 3 years
Factors Driving the Reduction in Transfusion Rates
Several factors have led to the drop in transfusion rates among cancer patients. These include:
- Improved patient blood management: Strategies aimed at optimizing patients’ blood components before, during, and after surgery or other treatments have reduced the need for transfusions.
- Enhanced surgical techniques: Advances in surgical procedures have minimized blood loss, reducing the need for transfusions.
- Better management of anemia: Early detection and treatment of anemia have decreased the reliance on blood transfusions.
“The reduction in transfusion rates is a positive outcome for cancer patients, as it indicates improved care and potentially fewer complications.”
The drop in cancer-related transfusions is a good sign, showing progress in cancer care and patient management. As medical practices keep improving, transfusion rates are likely to keep going down. This will help lead to better patient outcomes.
Transfusion Frequency During Different Cancer Treatments
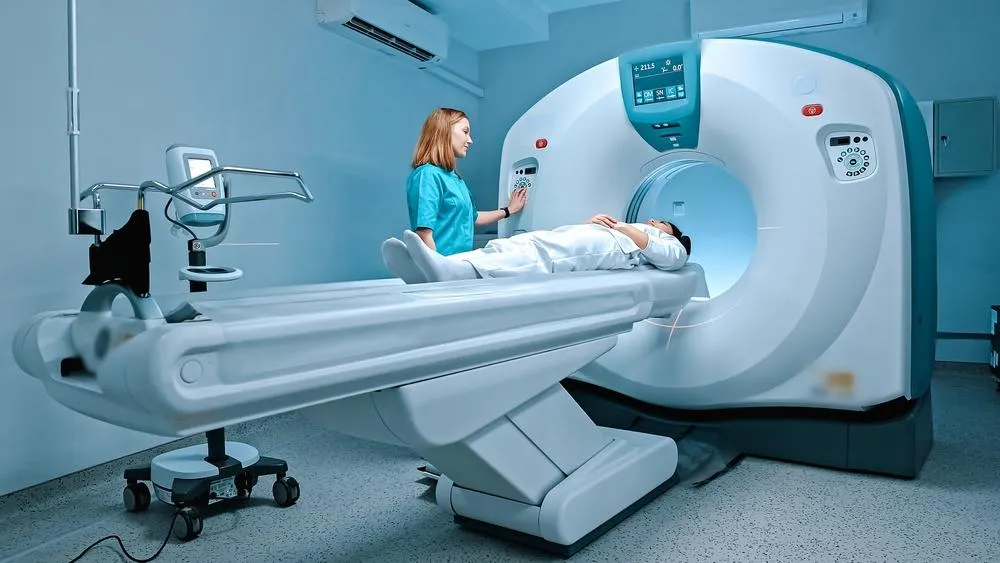
The need for blood transfusions in cancer patients changes with each treatment type. Treatments like chemotherapy, radiation, and surgery each have their own impact. This means the frequency of transfusions can vary a lot.
Chemotherapy-induced Anemia and Thrombocytopenia
Chemotherapy is a common cancer treatment. It can cause anemia and thrombocytopenia by weakening the bone marrow. Anemia means fewer red blood cells, while thrombocytopenia means fewer platelets. Both can lead to the need for blood transfusions to prevent tissue damage and bleeding.
How often a patient needs a transfusion during chemotherapy depends on several things. These include the type of chemotherapy, how strong the doses are, and how the patient reacts. Some patients might need transfusions often, while others might not need them as much.
Radiation Therapy Effects on Bone Marrow
Radiation therapy is another key cancer treatment. It can harm the bone marrow’s ability to make blood cells. The damage depends on the radiation dose and where it’s applied. If the bone marrow is hit hard, it can lead to anemia and thrombocytopenia, which might require transfusions.
Surgical Interventions and Blood Loss
Surgery is often needed for cancer diagnosis, staging, or treatment. These surgeries can cause a lot of blood loss. This blood loss might need blood transfusions before, during, or after surgery.
Knowing what affects transfusion frequency in cancer treatments helps in better patient care. Tailoring transfusion plans to each patient’s needs can improve their quality of life and treatment outcomes.
Clinical Indicators: When Cancer Patients Need Blood Transfusions
Blood transfusions in cancer care are based on a patient’s condition. They help guide when to give blood transfusions. This ensures patients get the support they need during treatment.
Hemoglobin Thresholds and Guidelines
Hemoglobin levels are key in deciding if a cancer patient needs a blood transfusion. Guidelines suggest transfusions when hemoglobin is below 7-8 g/dL. But, this can change based on the patient’s health and treatment type.
|
Hemoglobin Level (g/dL) |
Transfusion Recommendation |
|---|---|
|
< 7 |
Strongly Recommended |
|
7-8 |
Recommended |
|
> 8 |
Generally Not Recommended |
Platelet Count Considerations
Platelet count is also important for blood transfusions, mainly for those getting chemotherapy or radiation. The decision to give platelets depends on the count and the risk of bleeding.
Platelet transfusion thresholds vary: For severe thrombocytopenia, transfusions are often considered at a count below 10,000/µL.
Symptom-Based Decision Making
Symptoms like fatigue, shortness of breath, or dizziness also guide transfusion decisions. Even if hemoglobin is just above the usual threshold, symptoms can indicate the need for a transfusion.
Healthcare providers use these indicators to decide when cancer patients need blood transfusions. This helps support their care and treatment outcomes.
Perioperative Transfusions in Cancer Surgery
<SEP-1869_image_3>
Effective perioperative transfusion strategies are key for cancer surgery patients. They help manage blood loss and keep patients stable during and after surgery.
Preoperative Assessment and Preparation
Preoperative assessment is vital to find out who might need blood transfusions. It checks the patient’s hemoglobin, platelet count, and health to predict blood loss risk.
Key factors assessed preoperatively include:
- Patient’s current hemoglobin and hematocrit levels
- Platelet count and coagulation profile
- History of bleeding disorders or previous transfusion reactions
Intraoperative Transfusion Practices
Intraoperative transfusion practices change based on surgery type, patient condition, and surgical team. Restrictive transfusion strategies are used to avoid unnecessary transfusions.
Red blood cell transfusions are usually given when hemoglobin levels drop below 7-8 g/dL. This can change based on the patient’s specific needs.
Postoperative Transfusion Requirements
Postoperative transfusion needs depend on the patient’s condition. Monitoring hemoglobin levels and watching for symptoms like tachycardia or shortness of breath is important.
About 18% of cancer surgery patients get perioperative red blood cell transfusions. This shows the importance of careful perioperative management.
Platelet Transfusion Practices in Oncology
In cancer treatment, platelet transfusions are key to stop bleeding in patients with low platelet counts. Low platelet counts, or thrombocytopenia, often happen due to cancer treatments like chemotherapy and radiation.
Low-dose versus Standard-dose Approaches
The debate is ongoing between low-dose and standard-dose platelet transfusions. Low-dose transfusions give fewer platelets, which might be enough for some patients. This approach helps save blood components. On the other hand, standard-dose transfusions give more platelets and are used for patients at higher risk of bleeding.
Studies show that low-dose platelet transfusions can work as well as standard-dose for some patients. This could reduce the need for blood and lower the risk of complications from transfusions.
Frequency Considerations for Thrombocytopenic Patients
The need for platelet transfusions varies based on several factors. These include the cause of low platelet counts, the patient’s current platelet count, and their overall health. Patients getting intense chemotherapy or undergoing stem cell transplants might need transfusions often to keep platelet counts safe.
Guidelines suggest giving platelets when counts drop below 10 × 10/L. But, this can change based on the patient’s risk and the hospital’s rules.
Impact on Bleeding Risk Management
Platelet transfusions are vital for managing bleeding risk in patients with low platelet counts. They help prevent bleeding and reduce the risk of bleeding during procedures.
By managing bleeding risk with platelet transfusions, patients can handle more intense cancer treatments. This reduces the need for extra steps to stop bleeding.
Blood Transfusions in Advanced Cancer and Palliative Care
Blood transfusions are key in managing symptoms for advanced cancer patients in palliative care. They aim to enhance the patient’s quality of life. This is done by easing symptoms like fatigue, shortness of breath, and dizziness due to anemia or low blood cell counts.
Symptom-Driven Transfusion Decisions
In advanced cancer and palliative care, blood transfusions are often based on symptoms. Symptom-driven transfusion decisions consider the patient’s overall condition. This includes their fatigue, pain, and other symptoms that affect their quality of life.
For example, a patient with advanced cancer who is very tired and short of breath might benefit from a blood transfusion. This is even if their hemoglobin level is not below the usual threshold for transfusion.
Effectiveness Rates: The 80% Non-Improvement Statistic
Research shows that many advanced cancer patients don’t see a big improvement from blood transfusions. Up to 80% of patients may not see a significant change in their symptoms after a transfusion.
This finding stresses the need to carefully weigh the benefits and risks of blood transfusions for each patient. Effectiveness rates can differ based on individual patient factors. These include the cause of their anemia and their overall health.
Quality of Life Considerations
For advanced cancer patients in palliative care, quality of life considerations are critical. Blood transfusions can help improve quality of life by reducing symptoms and boosting overall well-being.
Yet, it’s important to consider the risks and burdens of blood transfusions. This includes the need for repeated hospital visits and the risk of complications from transfusions.
The Transfusion Process for Cancer Outpatients
<SEP-1869_image_4>
Many cancer outpatients get blood transfusions as part of their treatment. The transfusion process aims to support these patients. It makes sure they have a safe and comfortable experience.
Day Transfusion Centers
Day transfusion centers are key for cancer outpatients. They offer a safe and convenient place for transfusions. This setup helps patients get the care they need without interrupting their daily lives.
Efficient management of these centers is vital. This includes scheduling, monitoring patient flow, and making sure staff and equipment are ready.
Duration and Monitoring Protocols
The length of a transfusion varies based on several factors. It can last from a few hours to several hours. Patients are watched closely for any bad reactions during this time.
There are strict monitoring protocols to keep patients safe. These include checking vital signs, watching for signs of reaction, and adjusting the transfusion rate if needed.
Patient Experience During Transfusion Sessions
The experience of patients during transfusions is very important. Making them comfortable and informed can greatly improve their experience. Many centers offer amenities like comfy seating, entertainment, and refreshments to enhance the experience.
Effective communication between healthcare providers and patients is essential. Patients should feel free to ask questions and share any concerns they have during the transfusion.
Potential Risks and Long-term Considerations
Blood transfusions are key in cancer treatment but come with risks and long-term effects. Patients with cancer face complications from blood transfusions. It’s important to understand and manage these risks to get the best results.
Acute Transfusion Reactions
Acute transfusion reactions happen quickly, within minutes to hours after a transfusion. These can be mild or severe, including allergic reactions and hemolytic reactions. It’s vital to quickly spot and treat these reactions to avoid serious problems.
Iron Overload with Multiple Transfusions
Getting many blood transfusions can lead to iron overload. This is when too much iron builds up in the body. It can harm organs like the heart and liver. It’s important to keep an eye on iron levels and find ways to manage iron overload for those needing frequent transfusions.
Do Blood Transfusions Affect Survival Outcomes?
Research is ongoing about how blood transfusions affect survival in cancer patients. Some studies link transfusions to lower survival rates in some cancers. This might be because transfused blood can affect the immune system. But, the research is not clear, and more studies are needed.
It’s key to understand the risks and long-term effects of blood transfusions in cancer care. By managing these risks well, healthcare teams can help patients live better and longer.
Evidence-Based Transfusion Triggers in Oncology
Evidence-based transfusion triggers are key in oncology. They help decide when a cancer patient needs a blood transfusion. This ensures patients get the right support while keeping risks low.
Restrictive versus Liberal Transfusion Strategies
The debate on restrictive versus liberal transfusion strategies is ongoing. Restrictive means giving blood at lower hemoglobin levels. Liberal means giving at higher levels. Research shows that being more restrictive can cut down on transfusions without harming patients.
A study in the Journal of Clinical Oncology found that being more conservative works just as well. It compared a restrictive strategy (transfusion at 7-9 g/dL) to a liberal one (10-12 g/dL) in chemotherapy patients [1]. This shows that being cautious with blood transfusions can lower risks like reactions and iron overload.
Patient-Specific Factors Affecting Decisions
Each patient’s situation affects their need for blood transfusions. Factors include their health, cancer type and stage, and any other health issues. For example, patients with heart disease might need more blood to ensure enough oxygen.
|
Patient Factor |
Impact on Transfusion Decision |
|---|---|
|
Age |
Older patients may require more cautious transfusion strategies due to decreased physiological reserve. |
|
Comorbidities |
Presence of heart disease may necessitate a more liberal transfusion threshold. |
|
Cancer Type and Stage |
Advanced cancer or certain types like leukemia may require frequent transfusions. |
Balancing Benefits Against Risks
It’s important to weigh the good and bad of blood transfusions for cancer patients. Transfusions can help with anemia and low platelets but also come with risks like reactions and infections. Using evidence-based triggers helps doctors make the best choices for their patients.
Key considerations include:
- Monitoring patient’s hemoglobin and platelet levels closely.
- Assessing the patient’s symptoms and overall clinical condition.
- Considering alternative treatments to blood transfusions when possible.
By using evidence-based transfusion triggers, healthcare providers can give cancer patients the best care. This improves their outcomes and quality of life.
Patient Blood Management in Cancer Care
Effective patient blood management is key in cancer care. It affects treatment results and patient quality of life. It involves strategies to use the patient’s own blood, reducing the need for transfusions.
Minimizing Transfusion Requirements
One main goal is to cut down on transfusions. This is done by watching the patient’s blood counts closely. It helps prevent anemia and low platelet counts.
By doing this, doctors can lower the risk of transfusion reactions and iron overload.
Alternative Approaches to Manage Anemia
Managing anemia is a big part of patient blood management. Erythropoiesis-stimulating agents and iron supplements are used. They help make more red blood cells and improve hemoglobin levels.
This reduces the need for blood transfusions.
- Erythropoiesis-stimulating agents to stimulate red blood cell production
- Iron supplements to improve hemoglobin levels
- Careful monitoring of blood counts to prevent anemia and thrombocytopenia
Blood Conservation Strategies
Blood conservation strategies are also vital. Autologous blood transfusion is one, where the patient’s blood is collected and given back during surgery. Surgical techniques that reduce blood loss also help.
These strategies improve patient outcomes. They reduce the need for blood transfusions and enhance cancer care quality.
Special Considerations for Pediatric Cancer Patients
Pediatric cancer patients have unique needs for blood transfusions. Their bodies are growing, and they react differently to treatments. This includes how they handle blood transfusions.
Transfusion Frequency Differences from Adults
Children with cancer need blood transfusions more often than adults. Their smaller blood volumes and how they handle anemia and low platelets are different. For example, a study found kids might need more transfusions because of their size and how chemotherapy affects their bone marrow.
Key differences in transfusion frequency include:
- More frequent monitoring of blood counts due to smaller blood volumes
- Different thresholds for transfusion based on age and weight
- Consideration of developmental stages in transfusion decisions
Long-term Implications for Developing Bodies
Blood transfusions can have lasting effects on kids’ bodies. They can affect the child’s blood-making system, leading to iron overload or changes in the immune system. A medical expert noted,
“The impact of repeated transfusions on a child’s developing body must be carefully weighed against the benefits of transfusion.”
Long-term effects may include:
- Iron overload from frequent red blood cell transfusions
- Potential impacts on the developing immune system
- Effects on growth and development due to chronic anemia or thrombocytopenia
Family-Centered Decision Making
Family-centered decision making is key for kids with cancer needing blood transfusions. This approach involves the medical team and the family in discussions about risks, benefits, and alternatives. It makes sure care matches the family’s values and preferences.
Effective family-centered decision making includes:
- Clear communication about the need for and risks of transfusions
- Involvement of family members in the decision-making process
- Consideration of the family’s cultural and personal values
International Best Practices and Institutional Approaches
International best practices and institutional approaches are key in guiding blood transfusions in cancer care. These guidelines ensure patients get top-notch support during treatment.
Liv Hospital’s Evidence-Based Protocols
Liv Hospital follows evidence-based protocols for blood transfusions, meeting international standards. These protocols aim to improve patient outcomes by ensuring safe and effective transfusions.
The hospital assesses patient needs carefully, plans well, and monitors closely during and after transfusions.
Academic Care Pathways in Leading Cancer Centers
Top cancer centers have created academic care pathways based on the latest research and guidelines. These pathways are key for standardizing care and better patient outcomes.
Following established protocols helps healthcare providers reduce risks and enhance benefits of blood transfusions.
Ethical Standards in Transfusion Medicine
Ethical standards are essential in transfusion medicine, ensuring patients get the right care while respecting their rights and dignity.
Healthcare institutions must weigh the need for blood transfusions against the risks. They make decisions that put patient well-being first.
By adopting international best practices and sticking to ethical standards, cancer care providers offer top support to patients getting blood transfusions.
Conclusion
Blood transfusions are key in cancer treatment. They help patients live better and recover faster. How often a patient gets a transfusion depends on their cancer type and stage.
Studies show that transfusions help with anemia and low platelet counts in cancer patients. A study found that most transfusions were for low hemoglobin levels. This shows how vital blood therapy is for cancer patients.
Managing blood transfusions well is critical for patient care. Knowing when and how often to give transfusions helps doctors improve treatment plans. This leads to better care and outcomes for patients.
FAQ
Why do cancer patients need blood transfusions?
Cancer patients might need blood transfusions to fight anemia and other issues. These transfusions help keep their quality of life good while they’re getting treatment.
How often do cancer patients receive blood transfusions?
How often patients get blood transfusions depends on their cancer type and stage. Some might need them more often than others, based on their treatment plans.
What are the common blood components used in oncology?
In oncology, common blood components include red blood cells, platelets, and plasma. These help manage anemia and other complications from treatment.
What are the clinical indicators that guide the decision to administer blood transfusions?
Doctors use hemoglobin levels, platelet counts, and symptoms to decide on blood transfusions. These indicators help ensure patients get the right support during treatment.
How do blood transfusions support cancer treatment protocols?
Blood transfusions support cancer treatments by keeping patients’ quality of life high. They also allow for more aggressive treatments. This is key to improving patient outcomes.
What are the possible risks and long-term effects of blood transfusions?
Blood transfusions can lead to acute reactions, iron overload, and affect survival rates. Careful management and monitoring are needed to minimize these risks.
How do patient-specific factors affect transfusion decisions?
Factors like age, health, and treatment plans influence transfusion decisions. Evidence-based triggers help balance risks and benefits for each patient.
What is patient blood management in cancer care?
Patient blood management aims to reduce transfusion needs. It uses alternative methods for anemia and blood conservation strategies. This approach improves outcomes and cuts down on transfusions.
Are there special considerations for pediatric cancer patients?
Yes, pediatric cancer patients need special care with blood transfusions. Considerations include transfusion frequency, long-term effects, and family involvement in decisions.
What are the international best practices for blood transfusions in cancer care?
International best practices include evidence-based protocols and ethical standards. These ensure patients receive top-notch support during treatment.
Do blood transfusions shorten a patient’s life?
Research is ongoing on blood transfusions and survival. While there are risks, they are generally safe when managed well.
Why does a person need a blood transfusion during cancer treatment?
Patients might need transfusions to manage complications like anemia or bleeding. Transfusions support their health and let them keep up with treatment.
What are the signs that you need a blood transfusion?
Signs include low hemoglobin, low platelet count, fatigue, and bleeding. Healthcare providers check these to see if a transfusion is needed.
What is a day transfusion?
A day transfusion is when patients get transfusions on an outpatient basis. This way, they can keep up with their daily life while getting treatment.
References
- Annals of Hepato-Biliary-Pancreatic Surgery (AHBPS). Blood transfusion needs among cancer patients. Available at: https://www.ahbps.org/journal/view.html?doi=10.14701%2Fahbps.25-072
- PubMed Central (PMC). Patterns of blood transfusion in oncology care. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC12362034/
- Karger – Transfusion Medicine and Hemotherapy. Platelet transfusion for patients with cancer: An update. Available at: https://karger.com/tmh/article/doi/10.1159/000546566/928731/Platelet-Transfusion-for-Patients-with-Cancer-An
- Journal of the National Cancer Institute (JNCI). Blood transfusion practices in oncology. Available at: https://academic.oup.com/jnci/article/99/24/1864/2522248
- CA: A Cancer Journal for Clinicians. Cancer care and transfusion support. Available at: https://acsjournals.onlinelibrary.wiley.com/doi/full/10.3322/caac.70011
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK557754/



































