Explaining the cause and mechanism behind brittle bones (Osteogenesis Imperfecta) and its impact on the body. Osteogenesis imperfecta, also known as brittle bone disease, is a genetic disorder. It affects about 1 in 15,000 to 20,000 people globally. This condition makes bones very fragile, causing them to break easily.
The genetic cause of osteogenesis imperfecta is quite complex. It involves mutations in genes that code for type I collagen. This disorder can lead to many problems, like a curved spine, muscle weakness, and breathing issues. These issues can greatly affect the quality of life for those who have it.
Key Takeaways
- Osteogenesis imperfecta is a genetic disorder affecting 1 in 15,000 to 20,000 people worldwide.
- The condition is caused by defects in type I collagen synthesis or processing.
- It leads to fragile bones that fracture easily, even with minimal trauma.
- Complications can include a curved spine, muscle weakness, and breathing difficulties.
- Understanding the genetic basis is key to managing the condition effectively.
What is Osteogenesis Imperfecta?
Brittle bone disease, or Osteogenesis Imperfecta, has been studied for centuries. It’s a genetic disorder that affects collagen production. This makes bones extremely fragile.
Historical Context: Vrolik and Lobstein Syndromes
Osteogenesis Imperfecta has been known for ages. But, the term “osteogenesis imperfecta” was first used in the 19th century. It was linked to Vrolik and Lobstein syndromes, named after the researchers who studied it.
These early studies helped us understand the genetic basis of the disease.
Alternative Names: Glass Bone Disease and OI
Osteogenesis Imperfecta is also called “glass bone disease” because of the bones’ extreme fragility. The term “OI” is used in medical texts. These names highlight the condition’s effect on bone strength and its genetic roots.
Prevalence and Global Distribution
Osteogenesis Imperfecta is found worldwide, affecting people everywhere. Its prevalence varies in different populations. It’s considered rare but is a major health concern needing ongoing research and support.
The Science Behind Brittle Bones
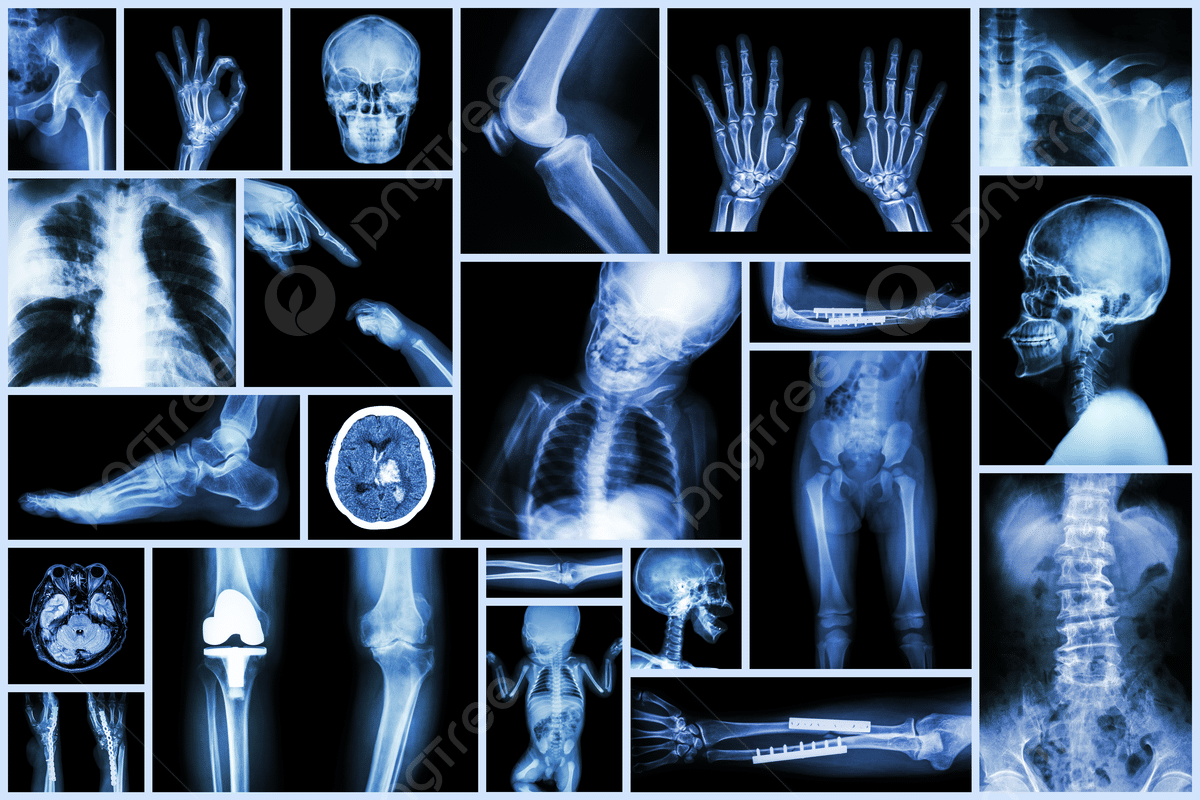
Type I collagen is key to bone health, but it’s affected in Osteogenesis Imperfecta. This leads to bones that break easily. This protein is essential for bone structure, and without it, bones become brittle.
Type I Collagen: Structure and Function
Type I collagen is everywhere in our bodies, important for bones, skin, and teeth. It’s made of three strands twisted together, giving bones strength and flexibility. In bones, it helps minerals like calcium and phosphate to harden the bone.
Type I collagen’s role in bone health is huge. It’s vital for bone formation and mineralization. When its genes are mutated, bones can become weak.
Genetic Mutations in Osteogenesis Imperfecta
Genetic changes in OI affect the COL1A1 and COL1A2 genes. These genes code for type I collagen. These changes can lead to less or abnormal collagen, weakening bones.
These mutations greatly affect collagen production and function. This is why OI bones are so fragile. Knowing this helps us find new treatments.
Bone Formation and Remodeling Abnormalities
In OI, type I collagen problems disrupt bone formation and remodeling. Bone remodeling, which involves breaking down and rebuilding bones, is off track. This makes bones weak and deformed.
|
Process |
Normal Function |
OI Impact |
|---|---|---|
|
Bone Formation |
Normal collagen matrix supports mineralization |
Defective collagen leads to poor mineralization |
|
Bone Remodeling |
Balanced resorption and formation |
Disrupted balance due to collagen defects |
The problems with bone formation and remodeling cause OI symptoms. This includes many fractures and skeletal issues.
Types and Classification of Osteogenesis Imperfecta
Osteogenesis Imperfecta (OI) has been classified into several types. These types are based on clinical features and genetic analysis. The condition shows a range of bone fragility, skeletal deformities, and extraskeletal features.
Type I: Mild Form with Blue Sclerae
Type I OI is the mildest form. It is often seen with blue sclerae. This is because the sclera is transparent, showing the veins underneath.
People with Type I OI may have few fractures. Some are not diagnosed until they are adults. Genetic counseling is important for families to understand the risk of passing it on.
Type II: Severe and Often Fatal Form
Type II OI is the most severe form. It often leads to perinatal death or early infant mortality. This type has extreme bone fragility, with many fractures in utero or shortly after birth.
Prenatal diagnosis is key for families to make informed choices.
Type III: Progressive Deforming Type
Type III OI is a progressive and deforming form. It has significant bone fragility and skeletal deformities. People with Type III may have a lot of fractures and need a lot of orthopedic care.
Type IV and Beyond: Expanding Classification System
The classification of OI has grown beyond the original four types. Type IV OI is moderately severe, with variable bone fragility and deformities. The new classification shows the genetic diversity of OI.
“new types of OI continue to be identified, underscoring the complexity of collagen-related disorders”
, as researchers in the field have noted.
Clinical Manifestations of Brittle Bone Disease
Brittle Bone Disease, or Osteogenesis Imperfecta, shows many symptoms beyond just weak bones. People with OI often get many symptoms that affect their health and happiness.
Skeletal Fragility and Fracture Patterns
Weak bones are a key sign of OI, causing many fractures. These fractures can happen with little effort. Fractures often happen in long bones, vertebrae, and ribs. In severe cases, they can cause big deformities and disability.
Dentinogenesis Imperfecta and Oral Health
Dentinogenesis imperfecta is a common dental issue in OI. It makes teeth look blue-gray or yellow-brown because of the dentin’s transparency. Good dental care is key to avoid tooth decay and wear.
Blue/Purple Sclerae and Ocular Findings
Blue or purple sclerae are a key sign of OI. They happen because the scleral collagen is clear. While it’s not harmful, it’s a big clue for doctors. Rarely, eye problems like retinal detachment can occur.
Hearing Loss and Auditory Complications
Hearing loss is a big problem for many with OI, getting worse with age. It can be conductive, sensorineural, or mixed. Often, hearing aids or surgery are needed to help.
A study points out, “The symptoms of Osteogenesis Imperfecta are varied. They need a full management plan that covers bones, teeth, eyes, and ears.”
Diagnosis and Assessment
Diagnosing Osteogenesis Imperfecta involves several steps. These include clinical assessment, radiological findings, and genetic analysis. Getting the diagnosis right is key to managing the condition well.
Clinical Evaluation and Physical Examination
First, doctors do a thorough clinical evaluation. They look at the patient’s medical history and physical traits. They also check for symptoms like frequent fractures or skeletal deformities.
Clinical features like blue sclerae and dentinogenesis imperfecta are important clues too.
Radiological Findings and Imaging Studies
Radiological imaging is a big help in diagnosing OI. X-rays show bone deformities, fractures, and other skeletal issues typical of the condition. DEXA scans are used to check bone density too.
|
Imaging Technique |
Use in OI Diagnosis |
|---|---|
|
X-ray |
Reveals fractures, bone deformities |
|
DEXA Scan |
Assesses bone density |
Genetic Testing Approaches
Genetic testing is a big part of diagnosing OI. It helps find the specific genetic mutations that cause the condition. This involves looking at the genes that code for type I collagen.
Differential Diagnosis and Misdiagnosis Risks
Differential diagnosis is key to rule out other conditions that might look like OI. This includes osteoporosis or child abuse. Getting it wrong can lead to the wrong treatment. So, a detailed diagnostic process is vital.
Treatment Strategies for Brittle Bones
Osteogenesis Imperfecta (OI) treatment has grown a lot. It now aims to lower fractures and boost life quality. Treatment plans mix medical care, orthopedic management, and rehab.
Bisphosphonate Therapy: Mechanisms and Benefits
Bisphosphonates are key for OI treatment, mainly for kids. They stop bone breakdown, making bones denser and lowering fracture risk. Clinical trials show a big drop in fractures for those on bisphosphonates.
|
Treatment |
Mechanism |
Benefits |
|---|---|---|
|
Bisphosphonates |
Inhibit bone resorption |
Increased bone density, reduced fracture risk |
|
Orthopedic Management |
Surgical interventions for fracture repair and deformity correction |
Improved mobility, reduced deformity |
|
Physical Therapy |
Exercise programs tailored to patient needs |
Enhanced strength, improved mobility |
Orthopedic Management and Surgical Interventions
Orthopedic care is key for OI. It helps manage fractures and deformities. Surgeries like rodding stabilize bones and fix deformities. Planning and doing these surgeries right is vital to avoid problems.
Physical and Occupational Therapy
Physical and occupational therapy are vital for OI. They boost muscle strength, improve movement, and help patients be more independent. Custom-made exercise plans help patients safely and effectively.
Emerging Treatments: Gene Therapy and Stem Cells
Gene and stem cell therapy look promising for OI. They aim to fix the disease’s genetic causes. Studies are checking if these new treatments are safe and work well.
In summary, treating Osteogenesis Imperfecta needs a wide approach. It combines known treatments with new ones. This way, healthcare teams can give personalized care, making life better for those with OI.
Living with Osteogenesis Imperfecta
Osteogenesis Imperfecta is more than a medical condition. It’s a life filled with challenges that require adaptability and resilience. People with OI need a strong support network to manage their condition well.
Adaptive Equipment and Home Modifications
Using adaptive equipment is key for those with OI. It helps with mobility and safety. This includes wheelchairs, walkers, and other devices for daily life.
Home modifications are also important. Installing ramps, widening doorways, and making a safe living space can prevent fractures.
Pain Management Strategies
Pain management is critical for OI patients. They often deal with chronic pain from fractures and bone deformities. Treatment may include medication, physical therapy, and alternative methods like acupuncture or massage.
Psychological Impact and Mental Health Support
OI can have a big psychological impact on mental health. It’s important to offer mental health support. Counseling, therapy, and support groups help individuals cope with emotional challenges.
Community Resources and Support Organizations
Community resources and support groups are vital. They help individuals with OI and their families. These organizations provide educational resources, advocacy, and peer support, improving life quality.
By using these resources, people with Osteogenesis Imperfecta can live fulfilling lives. They can manage their condition well and stay independent and well.
Special Considerations Across the Lifespan
People with Osteogenesis Imperfecta (OI) face unique challenges at every stage of life. They need special care and understanding of their changing needs. This is why managing OI well requires a deep grasp of these evolving requirements.
Pregnancy and Family Planning with OI
Pregnancy can be tough for women with OI, with higher risks of fractures and delivery issues. It’s vital to get advice before getting pregnant and to keep a close eye on things during the pregnancy. A study in the Orphanet Journal of Rare Diseases says, “Women with OI should be counseled about the risks and complications of pregnancy and childbirth.”
“Women with OI should be counseled about the risks and complications associated with pregnancy and childbirth.”
Orphanet Journal of Rare Diseases
Educational Accommodations for Children
Children with OI need special help in school to stay safe and learn well. This might include special physical education and changes to the classroom.
Transitioning to Adult Care
Moving from child to adult care is a big step for those with OI. It’s important to work with adult doctors who know how to manage OI.
Aging with Brittle Bone Disease
As people with OI get older, they may face new challenges like osteoporosis and less mobility. It’s key to manage these issues proactively to help them stay healthy.
|
Life Stage |
Key Considerations |
Management Strategies |
|---|---|---|
|
Pregnancy |
Increased fracture risk, delivery complications |
Pre-pregnancy counseling, close monitoring |
|
Childhood Education |
Safety, accessibility, adaptive education |
Adaptive PE programs, classroom modifications |
|
Transition to Adult Care |
Coordination with adult healthcare providers |
Careful planning, communication with providers |
|
Aging |
Osteoporosis, decreased mobility |
Proactive management, lifestyle adjustments |
Conclusion
Osteogenesis imperfecta, or brittle bone disease, is a complex genetic disorder. It affects people in many ways. It causes fragile bones, skeletal deformities, and sometimes other issues.
Knowing the different types of osteogenesis imperfecta is key. It helps in providing the right care. This is important for managing the condition effectively.
Managing osteogenesis imperfecta needs a team effort. This includes bisphosphonate therapy, orthopedic care, physical therapy, and new treatments like gene therapy. A detailed care plan helps those with the disease live better lives.
The disease’s complexity means ongoing support is needed. This support is essential throughout a person’s life. It helps them stay active and happy.
In summary, osteogenesis imperfecta needs a deep understanding and a detailed management plan. This approach improves the lives of those affected by the disease.
FAQ
What is Osteogenesis Imperfecta?
Osteogenesis Imperfecta, or brittle bone disease, is a genetic disorder. It makes bones fragile and can cause skeletal deformities. It also affects other parts of the body.
What causes Osteogenesis Imperfecta?
It’s caused by mutations in genes that code for type I collagen. This protein is key for strong bones.
What are the different types of Osteogenesis Imperfecta?
There are several types, ranging from mild to severe. The severity varies, affecting bone strength and shape differently.
How is Osteogenesis Imperfecta diagnosed?
Doctors use a mix of clinical checks, X-rays, and genetic tests. These help find the condition’s cause.
What are the treatment options for Osteogenesis Imperfecta?
Treatments include bisphosphonates to strengthen bones and orthopedic care for fractures. Physical therapy helps with movement. Gene therapy is also being explored.
How does Osteogenesis Imperfecta affect daily life?
People with Osteogenesis Imperfecta might need special tools and pain relief. They also need emotional support to deal with the condition’s challenges.
Can Osteogenesis Imperfecta be cured?
There’s no cure yet, but treatments can help manage symptoms. This improves life quality.
Is Osteogenesis Imperfecta hereditary?
Yes, it’s a genetic disorder passed down in an autosomal dominant pattern. This means one mutated gene can cause the condition.
What is the prevalence of Osteogenesis Imperfecta?
It affects about 1 in 15,000 to 1 in 20,000 births globally. The real number might be higher due to missed diagnoses.
What are the alternative names for Osteogenesis Imperfecta?
It’s also known as brittle bone disease, glass bone disease, and Vrolik syndrome. These names highlight its effects on bones and other areas.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK536957/


































