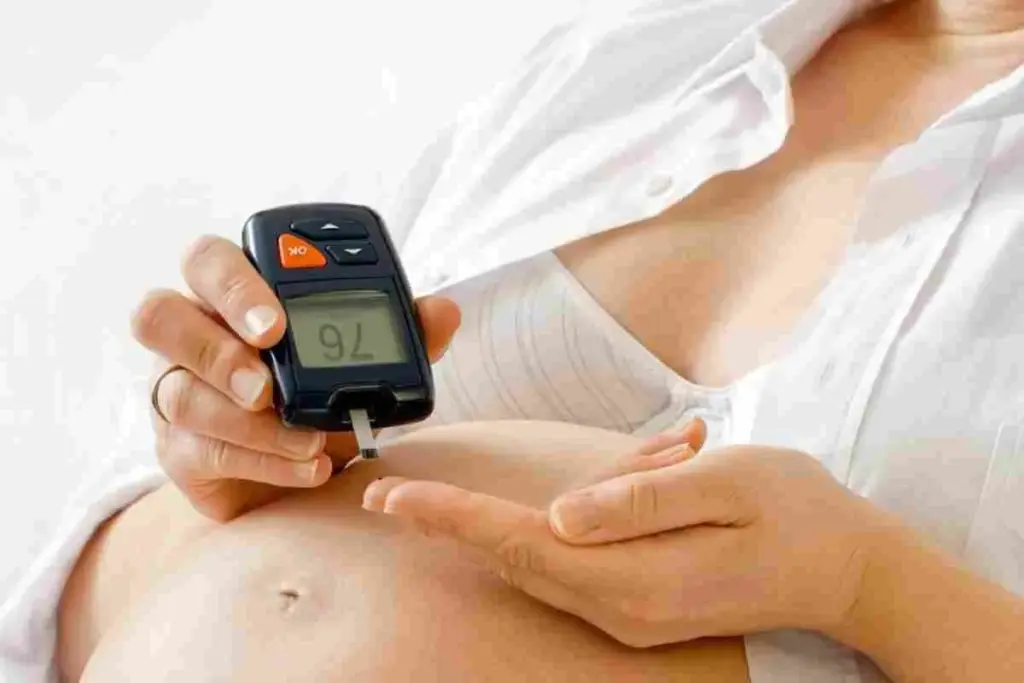
Gestational diabetes mellitus (GDM) is a condition where blood sugar levels are too high during pregnancy. It affects about 2-10% of pregnancies in the U.S. each year. This condition is risky for both the mother and the baby.
It’s important to know what happens if you don’t take insulin therapy. Insulin is key in treating GDM. It helps keep blood sugar stable during pregnancy.
Key Takeaways
- Gestational diabetes mellitus (GDM) is a form of glucose intolerance first recognized during pregnancy.
- GDM poses significant short and long-term risks to both mother and fetus.
- Insulin therapy is a primary treatment for managing GDM.
- Refusing insulin treatment can have implications for maternal and fetal health.
- Understanding patient rights and alternative treatment options is essential.
Understanding Gestational Diabetes and Why Insulin Is Recommended

Gestational diabetes mellitus (GDM) is a condition where blood sugar levels are high during pregnancy. It’s found in women who didn’t have diabetes before. This condition is important because it can harm both the mother and the baby.
What Is Gestational Diabetes Mellitus?
GDM is when blood sugar levels are too high during pregnancy. The American College of Obstetricians and Gynecologists (ACOG) suggests checking for type 2 diabetes early in pregnancy. This is for women with certain risk factors.
Some risk factors for GDM include:
- Increased body weight
- Decreased physical activity
- A family history of diabetes
- Previous history of delivering a macrosomic infant or having GDM in a previous pregnancy
Insulin as First-Line Pharmacologic Treatment
Insulin is a key treatment for GDM. Taking insulin while pregnant is safe and helps control blood sugar. It reduces risks for both the mother and the baby.
Insulin is recommended by many healthcare professionals. It’s safe and effective for managing blood sugar during pregnancy. Insulin for GDM is used when diet and exercise alone aren’t enough.
Prevalence and Diagnosis in the United States
About 2-10% of pregnancies in the United States are affected by gestational diabetes annually. GDM is usually diagnosed between 24 and 28 weeks of pregnancy. Women at high risk should be screened early.
The high number of GDM cases shows how important prenatal care is. It includes screening and diagnosis. Knowing about GDM risks and how to manage them is key for pregnant women and healthcare providers.
Your Legal Right to Decline Medical Treatment
Women with gestational diabetes often ask if they can skip insulin treatment. This is a big decision that needs careful thought about legal rights and health risks.
Patients can say no to any medical treatment, like insulin for gestational diabetes. This right is key in healthcare, showing the importance of patient choice and knowing what’s best.
It’s important to know what happens if you don’t take insulin. Insulin helps control blood sugar, which is good for both mom and baby.
The Importance of Informed Decision-Making

Deciding on insulin therapy needs careful thought. You must think about the good it does, like keeping blood sugar right, and any worries or risks.
Not taking insulin can be risky for mom and baby. It might cause big babies, birth problems, and health issues later for mom. Talking to a doctor can help understand these risks and benefits.
| Considerations | Insulin Therapy | Refusing Insulin |
| Blood Sugar Control | Effective in managing blood glucose levels | May lead to high blood sugar levels |
| Fetal Health Risks | Reduces risk of fetal macrosomia and birth injuries | Increases risk of fetal macrosomia and birth injuries |
| Maternal Health Risks | Low risk of complications when used correctly | May increase risk of long-term health complications |
Choosing to take or not take insulin should be talked over with a doctor. This ensures you understand all the possible outcomes.
Insulin Safety, Administration, and Consequences of Refusal
Insulin therapy is often recommended for managing gestational diabetes. It’s important to know about its safety and proper use. Expectant mothers need to understand the implications of insulin treatment for their health and their baby’s.
Is Taking Insulin While Pregnant Safe?
Pregnant women with gestational diabetes often worry about insulin therapy’s safety. Insulin is generally safe during pregnancy because it doesn’t pass through the placenta. But, wrong use can cause low blood sugar.
Proper insulin administration is key to keeping blood sugar levels healthy. It involves knowing the different types of insulin, their effects, and how to adjust doses based on blood tests.
Insulin Injections for Gestational Diabetes
Insulin injections are common for managing gestational diabetes. The injections go into the fat under the skin, usually in the abdomen, thighs, or arms. Rotating injection sites helps avoid lipodystrophy, a condition where fat under the skin gets uneven.
| Type of Insulin | Onset of Action | Duration of Action |
| Rapid-acting | 15-30 minutes | 3-5 hours |
| Short-acting | 30-60 minutes | 5-8 hours |
| Intermediate-acting | 1-2 hours | 12-18 hours |
| Long-acting | 2-4 hours | 20-24 hours |
Risks of Refusing Insulin Treatment
Refusing insulin when advised can harm both mother and baby. Uncontrolled diabetes can cause maternal complications like preeclampsia and the need for cesarean delivery. It can also lead to fetal macrosomia, birth injuries, and a higher risk of NICU admission for the baby.
Knowing the risks and benefits of insulin therapy helps expectant mothers make informed choices. It’s vital to talk to a healthcare provider to ensure the best outcomes.
Conclusion
Understanding gestational diabetes and its treatment is key for a healthy pregnancy. Insulin therapy is often used to manage gestational diabetes. It’s important to weigh the risks and benefits of refusing insulin.
Insulin is a common and effective way to keep blood sugar levels healthy. It helps lower the risk of complications for both mom and baby. Women should talk to their healthcare provider about their treatment options.
Managing gestational diabetes is important for long-term health. Effective insulin treatment can improve health outcomes. It supports a healthy pregnancy and a positive birth experience.
FAQ
Can I refuse insulin for gestational diabetes?
Yes, patients can refuse insulin, but doing so may increase health risks for both mother and baby.
Healthcare providers strongly recommend insulin if lifestyle measures do not adequately control blood sugar.
Is taking insulin while pregnant safe?
Yes, insulin is considered safe during pregnancy.
It does not significantly cross the placenta and protects the baby from complications of high maternal blood sugar.
What are the risks of refusing insulin treatment for gestational diabetes?
Refusing insulin can lead to high blood sugar, macrosomia (large baby), birth complications, and neonatal hypoglycemia.
It may also increase the risk of preterm birth and long-term metabolic issues for the child.
How is insulin administered for gestational diabetes?
Insulin is given subcutaneously via injection in the abdomen, thigh, or upper arm.
Dosing schedules are individualized, often using rapid-acting insulin at meals and long-acting insulin at bedtime.
Can insulin therapy be used in conjunction with other gestational diabetes treatments?
Yes, insulin is often combined with diet modification, exercise, and frequent glucose monitoring.
Oral medications are less commonly used but may be considered in some cases under medical supervision.
What are the possible side effects of insulin therapy during pregnancy?
Common side effects include hypoglycemia, injection site reactions, and mild weight gain.
Severe allergic reactions are rare, and careful monitoring minimizes risks.
How does gestational diabetes affect pregnancy?
Gestational diabetes can cause high birth weight, preterm delivery, cesarean delivery, and neonatal hypoglycemia.
It also increases the risk of preeclampsia and long-term type 2 diabetes for the mother.
Is insulin the only treatment option for gestational diabetes?
No, many cases are managed with diet and lifestyle changes alone.
Insulin is recommended only if blood sugar targets are not achieved with non-medication measures.
References
This article aimed to conduct a study that reviews the current published data available about patients with DKA and COVID-19.https://pmc.ncbi.nlm.nih.gov/articles/PMC4085289/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























