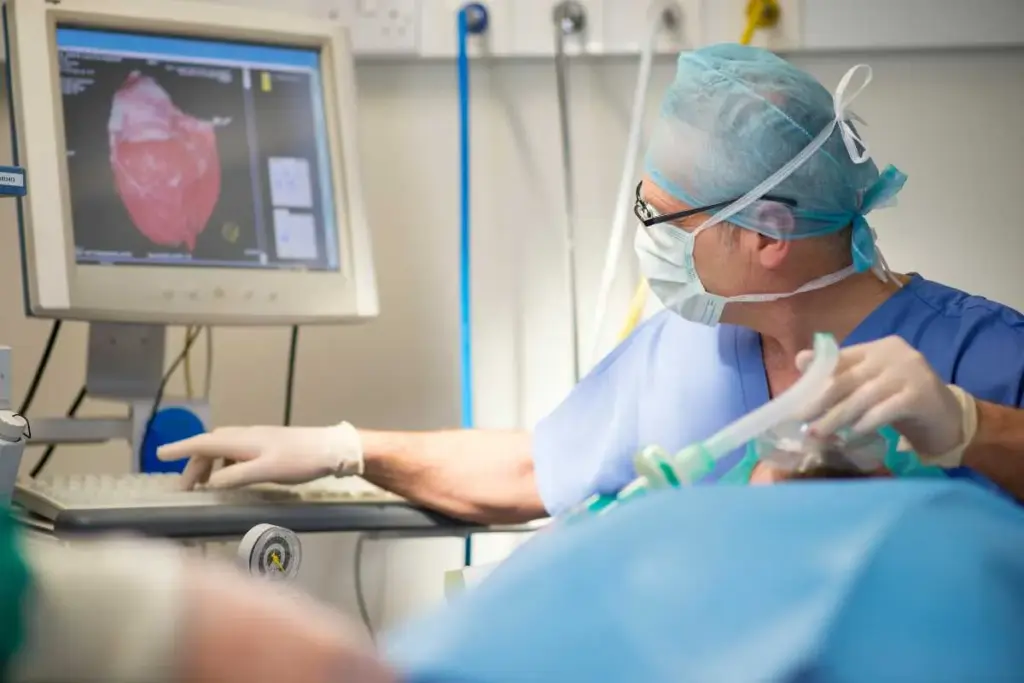
Cardiac rehabilitation is key for heart disease recovery. It has multiple phases to boost heart health. says many patients benefit from this program. Understanding the stages, such as Phase 1 and Phase 2, is essential for comprehensive care.
Phase1 starts in the hospital, focusing on the first steps of recovery. Phase2 comes after, with more exercise and lifestyle changes. This plan helps patients get stronger and lower heart risks. Knowing these phases helps patients on their recovery path.
Key Takeaways
- Cardiac rehabilitation involves multiple phases to improve cardiovascular health.
- Phase1 focuses on initial recovery during hospitalization.
- Phase2 emphasizes more intense exercise and lifestyle changes after discharge.
- Understanding the differences between Phase1 and Phase2 is key for full care.
- A medically supervised program helps patients regain strength and lower heart risks.
Understanding Cardiac Rehab Programs
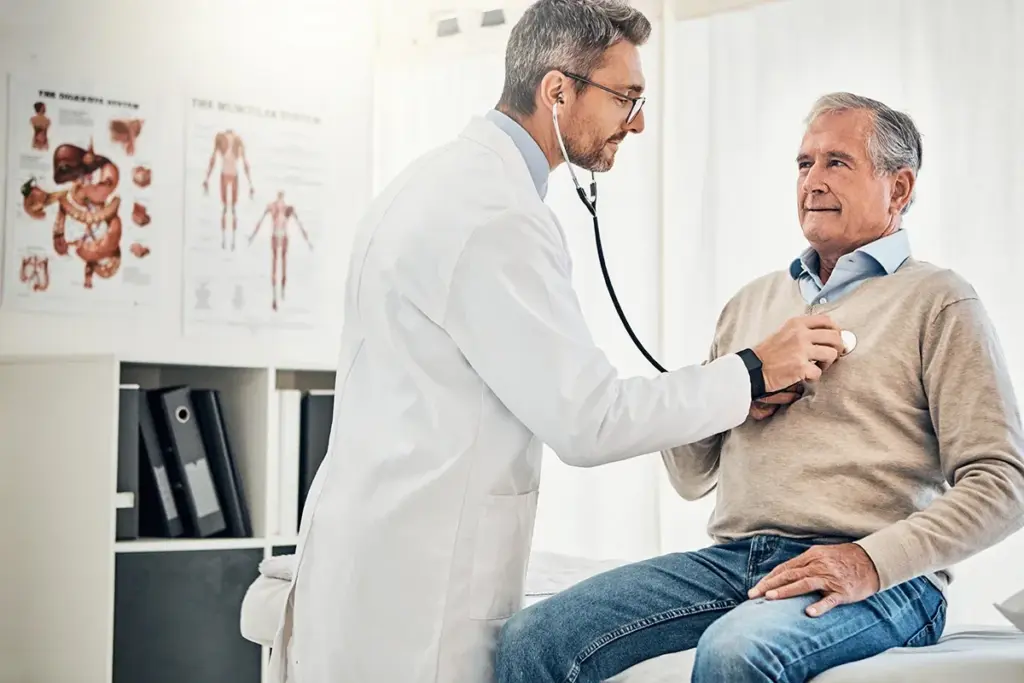
It’s important to know about cardiac rehab programs for those looking to get better and improve their heart health. These programs mix exercise, education, and lifestyle changes. They help patients with heart issues get back on track.
Definition and Purpose of Cardiac Rehabilitation
Cardiac rehab is a program supervised by doctors. It’s for people who have had heart problems or surgery. Its main goal is to help patients fully recover, lower the risk of future heart issues, and improve their life quality.
We understand that everyone’s recovery path is different. Our cardiac rehab programs are customized to fit each patient’s needs. We focus on exercise, teaching heart-healthy habits, and making lifestyle changes. This helps patients take charge of their recovery.
The Four-Phase Approach to Heart Recovery
The cardiac rehab process has four phases, each with its own goals. These phases offer a care plan that supports patients from the start of their recovery to maintaining their heart health long-term.
- Phase 1: Inpatient care during hospitalization
- Phase 2: Outpatient program after discharge
- Phase 3: Supervised maintenance program
- Phase 4: Long-term independent lifestyle maintenance
Medical Conditions That Require Cardiac Rehab
Cardiac rehab is suggested for those with heart issues or who have had heart surgery. Some conditions that might need it include:
|
Condition |
Description |
|---|---|
|
Myocardial Infarction |
Heart attack caused by a blockage in the coronary arteries |
|
Coronary Artery Bypass Grafting (CABG) |
Surgical procedure to bypass blocked coronary arteries |
|
Heart Transplant |
Surgical replacement of a diseased heart with a healthy donor heart |
|
Heart Failure |
Condition where the heart is unable to pump enough blood to meet the body’s needs |
Knowing about the different phases of cardiac rehab and the conditions it treats helps patients. It guides them through their recovery and towards better heart health.
The Critical Role of Cardiac Rehab in Heart Disease Recovery
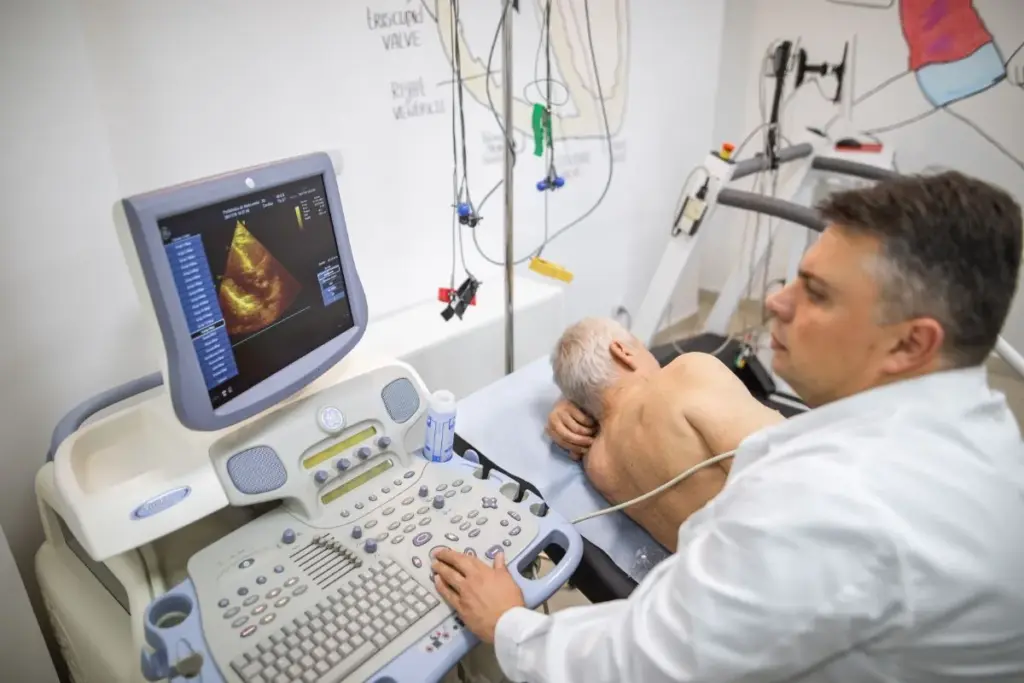
Heart disease recovery gets a big boost from cardiac rehab programs. These programs cover physical, emotional, and educational needs of heart disease patients.
Cardiac rehab is key for many reasons. It helps prevent more heart problems, boosts heart function, and improves life quality for patients.
Preventing Secondary Cardiac Events
Preventing more heart issues is a main goal of cardiac rehab. Research shows it cuts down the risk of future heart problems. It does this by managing risks, changing lifestyles, and improving medication.
A good cardiac rehab program might include:
- Risk factor assessment and management
- Lifestyle counseling on diet and exercise
- Stress management techniques
- Medication adherence education
Improving Cardiovascular Function
Cardiac rehab also aims to boost heart function. It does this through supervised exercise that fits each patient’s needs. This exercise strengthens the heart, improves blood flow, and boosts fitness.
Improved heart function means patients can do more without getting tired. It also means fewer heart disease symptoms and a lower risk of future heart problems.
|
Benefits |
Description |
|---|---|
|
Enhanced Physical Capacity |
Patients can perform daily activities with more ease and less fatigue. |
|
Reduced Symptoms |
Symptoms such as chest pain and shortness of breath are minimized. |
|
Lower Risk of Future Cardiac Events |
The risk of heart attacks and other cardiac events is significantly reduced. |
Enhancing Overall Quality of Life
Cardiac rehab also boosts patients’ quality of life. It tackles both physical and emotional heart disease aspects. This helps patients regain independence, return to normal activities, and enjoy a better life.
We make sure each cardiac rehab program is customized for each patient. This ensures they get the right support and care for the best recovery.
Phase1 Cardiac Rehab: The Inpatient Experience
For those recovering from heart issues, Phase1 cardiac rehab is key. It offers vital care and advice during their hospital stay. This first phase is vital for a good recovery.
Timing and Initiation
Starting Phase1 cardiac rehabearly is important for a good recovery, as says. It usually starts soon after the patient is stable, often in 24 to 48 hours. The exact start time depends on the patient’s health and the heart event they had.
Primary Goals and Expected Outcomes
The main goals of Phase1 cardiac rehab are to stabilize the patient and lower the risk of future problems. It also prepares them for the next steps in their recovery. Patients can expect better heart function, improved health, and a lower chance of more heart issues.
Typical Duration
Phase1 cardiac rehab usually lasts as long as the patient is in the hospital. This can vary based on how serious their condition is. On average, it can last from a few days to over a week.
|
Aspect |
Description |
Benefits |
|---|---|---|
|
Timing |
Initiated within 24-48 hours after cardiac event |
Early stabilization, reduced risk of complications |
|
Primary Goals |
Stabilize condition, reduce complication risk, prepare for next phase |
Improved cardiovascular function, enhanced well-being |
|
Duration |
Lasts for the duration of hospital stay |
Personalized care, monitored recovery |
Knowing about Phase1 cardiac rehab helps patients and doctors work together. This ensures a smooth and effective recovery.
Key Components and Activities in Phase1 Cardiac Rehabilitation
Phase 1 cardiac rehabilitation is key for patients starting their recovery. It’s vital for those who have had heart events or surgery. This phase helps set the stage for long-term heart health.
Initial Clinical Assessment Procedures
The first step is a detailed clinical assessment. We conduct thorough evaluations to understand the patient’s health. This includes their medical history, symptoms, and physical abilities. It helps create a personalized rehabilitation plan.
Bedside Exercises and Early Mobilization
Early mobilization is a big part of Phase 1. Bedside exercises start to prevent bed rest problems. These exercises are chosen based on the patient’s health and are gradually increased to boost fitness.
Breathing Techniques and Respiratory Care
Breathing techniques and care are key for cardiac surgery patients or those with breathing issues. We teach patients various breathing exercises to improve lung function. This is vital for recovery and reducing respiratory risks.
Patient and Family Education Sessions
Education is a big part of Phase 1. We provide patients and their families with detailed heart health information. This includes diet, exercise, medication, and lifestyle tips. These sessions help patients and their families make informed health choices.
- Initial clinical assessment procedures
- Bedside exercises and early mobilization
- Breathing techniques and respiratory care
- Patient and family education sessions
By focusing on these areas, Phase 1 cardiac rehabilitation lays a strong foundation for recovery.
Medical Supervision During Phase1 Cardiac Rehab
Effective medical supervision is key in Phase1 cardiac rehab. It ensures patient safety and the best recovery. A strong supervision framework is at the heart of cardiac care.
The Multidisciplinary Inpatient Care Team
The inpatient care team is vital in Phase1 cardiac rehab. It includes cardiologists, nurses, physiotherapists, and other healthcare professionals. They work together to watch patients’ progress, solve problems, and make rehab plans fit each person’s needs.
This team makes sure all parts of a patient’s health are looked after. This includes the heart, physical health, and emotional well-being.
Continuous Cardiac Monitoring Protocols
Continuous cardiac monitoring is a key part of Phase1 cardiac rehab. It lets healthcare providers keep a close eye on heart activity. They can quickly respond to any heart issues.
This monitoring is vital for catching complications early and adjusting treatment plans. It helps ensure patients get the right care and lowers risks.
Risk Stratification and Safety Measures
Risk stratification is a big part of Phase1 cardiac rehab. It helps healthcare providers spot patients at higher risk of problems. This way, they can focus on safety measures for each patient.
Safety in Phase1 includes heart monitoring and emergency management. We also prevent falls and accidents. Our aim is to make a safe space for recovery and lower the chance of bad events.
Phase2 Cardiac Rehab: Structured Outpatient Programming
After leaving the hospital, Phase2 cardiac rehab offers a structured program for outpatient care. It’s key for patients to regain strength, improve heart health, and lower the risk of future heart problems.
Transition Process from Hospital to Outpatient Care
The move from hospital to outpatient care in Phase2 is well-planned. It starts with a detailed check of the patient’s health and readiness for outpatient care. Healthcare providers create a personalized plan that meets the patient’s needs and goals.
Research shows that a structured outpatient program in Phase2 boosts patient outcomes and rehab adherence. Outpatient programs provide a detailed and intense rehab, including exercise, heart-healthy education, and lifestyle changes.
Comprehensive Goals of Phase2 Rehabilitation
The main goals of Phase2 cardiac rehab are to improve heart function, enhance quality of life, and lower the risk of future heart issues. Patients learn to manage their condition through exercise, education, and support.
|
Goals |
Description |
Benefits |
|---|---|---|
|
Improve Cardiovascular Function |
Through aerobic exercise and other physical activities |
Enhanced heart health, increased stamina |
|
Enhance Quality of Life |
By incorporating lifestyle changes and stress management |
Better overall well-being, reduced stress |
|
Reduce Risk of Secondary Cardiac Events |
Through education on risk factors and management strategies |
Lower risk of future heart problems |
Typical Duration and Session Frequency
Phase2 cardiac rehab usually lasts several months. Sessions are held 1-3 times a week. The exact schedule depends on the patient’s needs and progress.
Understanding Phase2 cardiac rehab helps patients navigate their recovery better. It leads to improved heart health.
Exercise Training Protocols in Phase2 Cardiac Rehab
In Phase 2 cardiac rehab, we create exercise plans that fit each patient’s needs. This ensures a safe and effective recovery. It’s a key phase that builds on the progress made in Phase 1, improving heart health and physical function.
Individualized Exercise Prescription
The heart of Phase 2 cardiac rehab is the individualized exercise prescription. We tailor each plan to the patient’s health, medical history, and goals. This way, we make sure the exercises are safe and effective, helping each patient get the most benefits.
Aerobic Exercise Components
Aerobic exercises are key in Phase 2 cardiac rehab. Activities like walking, cycling, or swimming boost heart function and endurance. We adjust the intensity and duration based on the patient’s starting point and progress.
Resistance Training Guidelines
Resistance training is also important in Phase 2. It helps strengthen muscles and improve physical function. We start with moderate intensity and gradually increase as the patient gets stronger.
Flexibility and Balance Activities
Flexibility and balance exercises are also part of the program. They improve flexibility, reduce fall risks, and enhance mobility. These are great for older adults or those with balance or flexibility issues.
By combining these exercises, Phase 2 cardiac rehab offers a complete approach to heart recovery. It addresses the varied needs of patients, supporting their path to better health.
Educational and Lifestyle Components of Phase2 Cardiac Rehab
The outpatient Phase 2 cardiac rehab program helps patients achieve long-term heart health. It focuses on education and lifestyle changes. Moving from the hospital to home, a structured recovery plan is key.
Nutritional Counseling for Heart Health
Nutritional counseling is a key part of Phase 2 cardiac rehab. It teaches patients about heart-healthy diets. We stress the need for fruits, vegetables, whole grains, and lean proteins.
By choosing the right foods, patients can lower their heart disease risk.
Medication Management Education
Medication management is also vital in Phase 2 cardiac rehab. We teach patients how to use their meds correctly. We cover side effects and why sticking to their treatment plan is important.
This education helps patients take charge of their recovery and health.
Stress Management and Relaxation Techniques
Stress management and relaxation are key in Phase 2. We teach deep breathing, meditation, and yoga. These methods help manage stress and boost overall health.
Smoking Cessation Support
Smoking cessation support is essential for smokers in Phase 2. We offer counseling and resources to help quit. Quitting smoking greatly lowers heart disease risk and improves health.
Phase 2 cardiac rehab offers a complete approach to heart recovery. It empowers patients to make lasting changes for better heart health and life quality.
Key Differences Between Phase1 and Phase2 of Cardiac Rehab
It’s important to know the differences between Phase 1 and Phase 2 of cardiac rehab. Patients move from the hospital care of Phase 1 to the outpatient programs of Phase 2. This change helps them progress in their recovery.
Clinical Setting and Environment Comparison
Phase 1 happens in a hospital, where patients get care right after a heart event. Phase 2 takes place in a cardiac rehab center or clinic. This setting is more like home, helping patients recover better.
Exercise Intensity and Complexity Differences
In Phase 1, exercises are easy and help prevent problems. When patients move to Phase 2, the exercises get harder. They include aerobic, strength, and flexibility workouts, all based on the patient’s progress.
Levels of Medical Supervision and Monitoring
Phase 1 has constant medical watch because patients are just after a heart event. In Phase 2, the medical watch is less strict. This shows the patient is getting better and can handle their health more on their own.
Patient Autonomy and Self-Management Expectations
When moving to Phase 2, patients are expected to take more control of their health. Phase 2 teaches patients how to manage their health, make lifestyle changes, and follow medication. This prepares them for long-term health and recovery.
|
Characteristics |
Phase 1 |
Phase 2 |
|---|---|---|
|
Clinical Setting |
Inpatient (Hospital) |
Outpatient (Rehab Center/Clinic) |
|
Exercise Intensity |
Low-intensity, early mobilization |
Increased intensity, varied exercises |
|
Medical Supervision |
Continuous monitoring |
Less intensive supervision |
|
Patient Autonomy |
Limited autonomy |
Increased autonomy and self-management |
The Cardiac Rehab Team: Professional Roles Across Phases
A team of experts is key in cardiac rehabilitation. They work together to give patients the best care. This team helps patients get better during their recovery.
Cardiologists and Medical Specialists
Cardiologists and other medical experts are vital in cardiac rehab. They oversee the program and guide patients. They create treatment plans and check on patient progress.
“The cardiologist’s role is not just about treating the heart condition, but also about improving the patient’s overall quality of life,” saysa leading cardiologist.
Cardiac Nurses and Case Managers
Cardiac nurses and case managers are key team members. They coordinate care and educate patients and their families. They also help with the transition between program phases.
They offer emotional support and help patients understand the healthcare system.
Exercise Physiologists and Physical Therapists
Exercise physiologists and physical therapists create exercise plans for patients. They focus on improving fitness, strength, and flexibility. They also ensure safety during exercise.
Dietitians, Psychologists, and Support Staff
Dietitians teach patients about heart-healthy eating. Psychologists help with emotional support and stress management. Other staff, like administrators and educators, also play a big role.
This team addresses physical, emotional, and educational needs of patients. By working together, they help patients recover well and live better lives.
Measuring Progress: Assessment Methods in Each Phase
To make rehabilitation programs better, regular checks are key. These checks help doctors change treatment plans to fit each patient’s needs. This ensures the best recovery and results.
Baseline Testing and Evaluation Procedures
Starting with baseline testing is vital in cardiac rehab. It sets a base for tracking progress. This includes looking at the patient’s medical history, current health, and how well they can function. Key components of baseline testing include:
- Medical history review
- Physical examination
- Electrocardiogram (ECG) testing
- Exercise stress testing
Functional Capacity and Exercise Testing
Assessing how well a patient can function is critical. Tests like exercise stress tests show physical limits and how well they can exercise. Exercise testing protocols may include:
- Treadmill or stationary bike tests
- Monitoring of heart rate and blood pressure
- Assessment of symptoms and ECG changes
Cardiovascular Metrics and Vital Signs
Keeping an eye on heart health and vital signs is important in cardiac rehab. This means watching heart rate, blood pressure, and more. Key cardiovascular metrics include:
- Heart rate variability
- Blood pressure response to exercise
- ECG monitoring for ischemia or arrhythmias
Quality of Life and Psychological Assessments
Checking how well a patient feels and their mental health is key in cardiac rehab. These checks help doctors see how recovery is going and where more help is needed. Quality of life assessments may involve:
- Questionnaires on physical and emotional well-being
- Evaluations of stress and anxiety levels
- Assessment of social support systems
By using these methods, cardiac rehab programs can offer full care. They address physical, emotional, and social needs. This improves recovery and long-term health.
Insurance Coverage and Financial Considerations for Cardiac Rehab
It’s important for patients to understand the costs of cardiac rehab. This care is key for many heart conditions. Insurance coverage greatly affects how much patients pay.
Medicare Coverage Guidelines for Cardiac Rehab
Medicare helps with cardiac rehab costs, but there are rules. It covers rehab for those with heart attacks or bypass surgeries.
To get Medicare help, patients need a doctor’s order. The rehab program must be approved by Medicare. It should be in a doctor’s office or hospital outpatient area.
|
Condition/Surgery |
Medicare Coverage |
|---|---|
|
Heart Attack |
Yes |
|
Coronary Artery Bypass Grafting |
Yes |
|
Heart Valve Repair/Replacement |
Yes |
Private Insurance Policies and Requirements
Private insurance plans differ in what they cover for cardiac rehab. Some may pay for a set number of sessions. Others might ask for copays or coinsurance.
Patients should review their insurance to know what’s covered. Many plans require a doctor’s referral. Some have specific rules for the rehab program or provider.
Documentation Needed for Coverage Approval
To get insurance to cover cardiac rehab, patients need to provide some documents. These include a doctor’s referral, medical records, and details about the rehab program.
Working with the rehab team and insurance is key. This ensures all needed documents are submitted and coverage is approved.
Patient Financial Assistance Programs
For those struggling to pay for rehab, financial help is available. This aid comes from rehab centers, non-profits, or government agencies.
Patients should ask about these programs when talking to their healthcare provider. This help makes rehab more affordable and accessible.
Overcoming Challenges in Transitioning Between Cardiac Rehab Phases
The journey through cardiac rehabilitation comes with its own set of challenges. These challenges are more pronounced when moving from one phase to another. Patients face transitioning challenges as they move from inpatient Phase 1 to outpatient Phase 2 and then to managing their health on their own.
Common Barriers to Program Participation
Several cardiac rehab barriers can make it hard for patients to fully engage in cardiac rehab programs. These include a lack of motivation, not understanding the program’s benefits, and scheduling conflicts. We tackle these issues with personalized education and support.
Transportation and Accessibility Issues
Transportation issues are a big problem for many, mainly in rural or underserved areas. Without a way to get to outpatient sessions, patients miss out on vital care. We advise patients to talk to their healthcare providers about their transport needs.
Psychological Adjustments and Motivation
Cardiac rehabilitation also means big psychological adjustments. Patients must accept their condition and the lifestyle changes needed for recovery. Keeping motivated is key, and we help with counseling and setting goals.
Support Systems and Community Resources
A strong support system is essential for cardiac rehab challenges. Family, friends, and support groups offer emotional and practical help. Using community resources can also help patients get the care they need. We help connect patients with these resources.
Understanding and tackling the challenges of moving through cardiac rehab phases helps our patients recover better. Our team is dedicated to guiding, supporting, and providing resources to help overcome these obstacles.
Patient Experiences: Navigating the Cardiac Rehab Journey
The journey through cardiac rehab is unique for everyone. It’s a personal and transformative experience. Understanding what patients go through is key.
What to Expect in Your First Days of Phase1
In the early days of Phase 1, patients are in a hospital. They get close medical care. The goal is to stabilize their condition and start gentle exercises.
Key activities during this phase include:
- Initial clinical assessments to determine the patient’s baseline health status.
- Bedside exercises and early mobilization to improve circulation and prevent muscle atrophy.
- Breathing techniques and respiratory care to enhance lung function.
- Patient and family education sessions to understand the condition, treatment, and necessary lifestyle changes.
The Initial Phase2 Experience
Phase 2 marks a big step towards outpatient care. It’s more structured. Patients get a tailored exercise program.
Patients can expect:
- A thorough assessment to determine their current health status and functional capacity.
- An individualized exercise prescription that includes aerobic exercise, resistance training, and flexibility activities.
- Educational sessions on nutrition, medication management, stress reduction, and smoking cessation if applicable.
Milestones and Progress Markers
Patients reach many milestones in cardiac rehab. These show their progress. They can include better exercise tolerance and reduced symptoms.
Notable progress markers are:
- Increased ability to perform daily activities without fatigue.
- Improved cardiovascular metrics such as blood pressure and heart rate.
- Better management of cardiac risk factors through lifestyle changes.
Patient Testimonials and Success Stories
Listening to patients’ stories can be very motivating. Their experiences show the challenges and successes of cardiac rehab. It highlights the program’s positive impact on their lives.
“Cardiac rehab was a game-changer for me. It not only helped me recover from my heart surgery but also taught me how to live a healthier life. I’m grateful for the support and guidance I received throughout the program.”
We share these stories to inspire and support others. We want to show that there’s a supportive community in cardiac rehab.
Beyond Phase2: Continuing Your Cardiac Recovery
It’s important to keep working on your heart health after Phase2. Knowing about the next phases helps a lot. They are key to keeping your heart strong.
Introduction to Phase3 Supervised Maintenance
Phase3 is all about keeping up with your heart health. It’s the next step after Phase2. Here, you get help and support to keep improving your heart health. Supervised maintenance means you’ll see doctors often to check on your progress and adjust your plans as needed.
Phase4 Independent Lifestyle Maintenance
Phase4 is the last step in cardiac rehab. It’s when you learn to take care of your heart on your own. You’ll keep up the good habits you learned in rehab. But, you’re also encouraged to keep practicing those heart-healthy habits.
Long-term Adherence Strategies
Staying on track with heart-healthy habits is vital. Here are some ways to keep going:
- Regular check-ups with your doctor
- Learning more about heart health and nutrition
- Keeping up with exercise and staying active
- Using stress-relief techniques
Integrating Heart-Healthy Habits for Life
Making heart-healthy habits a part of your daily life is essential. This means eating well, staying active, and managing stress. We help you create a plan that fits your life. This way, you can keep up these habits for a long time.
|
Phase |
Description |
Key Activities |
|---|---|---|
|
Phase3 |
Supervised Maintenance |
Regular check-ins, monitored exercise, lifestyle adjustments |
|
Phase4 |
Independent Lifestyle Maintenance |
Self-managed heart health, continued education, sustained lifestyle changes |
Conclusion: Maximizing Benefits from Your Cardiac Rehabilitation Program
Following a detailed cardiac rehab program helps patients recover better and stay healthy longer. We’ve looked at the various stages of cardiac rehab. This includes the inpatient care in Phase1 and the outpatient programs in Phase2 and beyond.
A good cardiac rehab program offers many benefits. These include better heart function, a higher quality of life, and fewer heart problems later on. To get the most out of it, patients should fully participate. This means sticking to the exercise plans, learning from the educational parts, and making lifestyle changes as advised by the rehab team.
We urge patients to be active in their rehab program. Working closely with their doctors can lead to the best results. This way, people can recover fully, keep their hearts healthy, and live better lives.
FAQ
What is cardiac rehabilitation, and why is it necessary?
Cardiac rehabilitation is a program for people who have had heart problems or surgery. It helps prevent more heart issues and improves health. It also makes life better overall.
What are the different phases of cardiac rehabilitation?
There are four phases. Phase1 is in the hospital, Phase2 is outpatient, Phase3 is supervised, and Phase4 is independent.
What happens during Phase1 cardiac rehab?
Phase1 starts in the hospital. It focuses on recovery and getting ready for more rehab. You’ll do exercises, learn breathing techniques, and get educated.
How does Phase2 cardiac rehab differ from Phase1?
Phase2 is for those who have left the hospital. It’s more intense with exercises and education. It aims to improve health and quality of life.
Will aspirin lower my blood pressure?
Aspirin might slightly lower blood pressure. But it’s not mainly for lowering blood pressure. It’s used for heart health, and its effect on blood pressure is small.
What is the role of exercise in cardiac rehabilitation?
Exercise is key in cardiac rehab. It boosts heart health and reduces symptoms. You’ll do different exercises based on your needs.
How is progress measured during cardiac rehabilitation?
Progress is checked through tests and evaluations. These include initial tests, functional assessments, and quality of life checks. They help make the program fit your needs.
Is cardiac rehabilitation covered by insurance?
Yes, many insurances, including Medicare, cover it. But, what’s covered and what you need to show can vary. Always check with your insurance.
What are the benefits of cardiac rehabilitation?
It improves heart health, reduces symptoms, and boosts quality of life. It also lowers the risk of future heart problems.
Can I continue cardiac rehabilitation at home?
Yes, after Phase2, you can keep up with heart-healthy habits at home. Phases 3 and 4 focus on maintaining a healthy lifestyle.
What is the best time to take low-dose aspirin?
Taking low-dose aspirin in the evening might help prevent heart issues at night. But, always talk to your doctor about what’s best for you.
How long does cardiac rehabilitation last?
It varies based on your needs and the phase. Phase1 is during hospital stay, Phase2 is several months. Phases 3 and 4 are for long-term maintenance.
Can cardiac rehabilitation help with stress management?
Yes, it includes stress management and relaxation techniques. This can help you deal with stress and anxiety.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3839175/[5



































