
The best treatment for heart muscle disease depends on the type and how severe it is. Find amazing treatments for cardiomyopathy. Learn vital steps to strengthen your heart and ensure a brilliant, long-term recovery. Find amazing treatments for cardiomyopathy. Learn vital steps to strengthen your heart and ensure a brilliant, long-term recovery.
Recent studies have shown that targeted therapies, such as tafamidis for cardiac amyloidosis, have significantly improved patient outcomes. They reduced all-cause mortality to 29.5% compared to 42.9% for placebo.
Different types of cardiomyopathy, such as dilated, hypertrophic, and restrictive cardiomyopathy, need different treatments. We will look at the latest in cardiomyopathy treatment. This includes advanced therapies and team care to help patients live better lives.
Key Takeaways
- Individualized treatment plans are key for managing cardiomyopathy effectively.
- Targeted therapies have shown great promise in improving patient outcomes.
- Different types of cardiomyopathy need different treatments.
- Advanced therapies and team care are essential for better survival and quality of life.
Understanding Cardiomyopathy: A Complete Overview
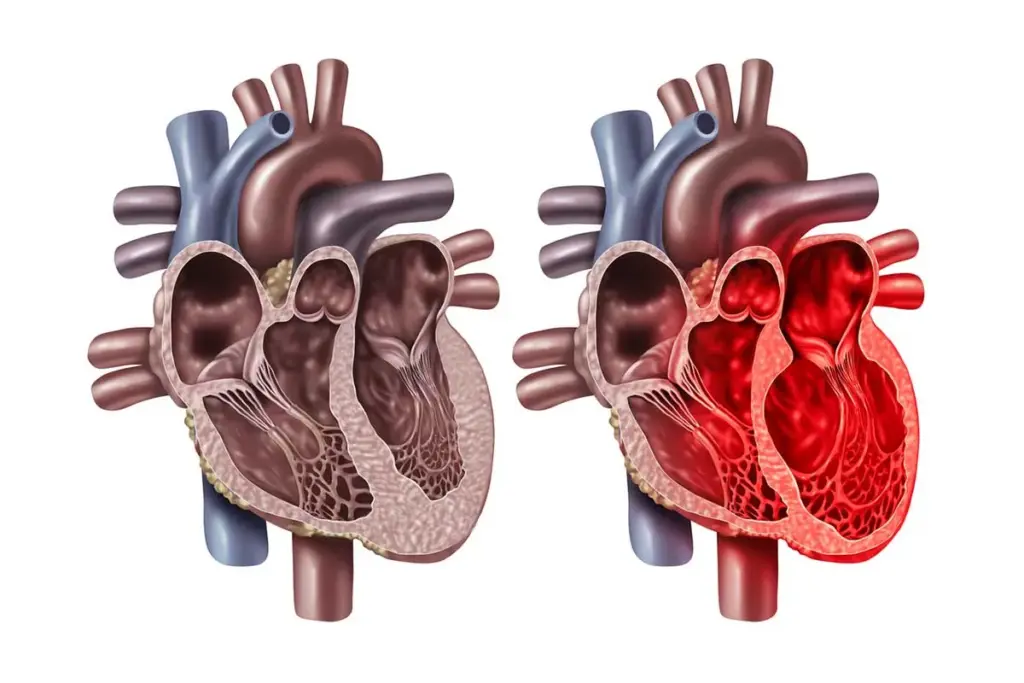
Cardiomyopathy refers to different heart muscle diseases. These diseases affect the heart’s structure and function. They can make the heart muscle enlarge, thicken, or become rigid, making it hard for the heart to pump blood well.
Definition and Impact on Heart Function
Cardiomyopathy is a group of heart muscle disorders. It makes the heart muscle structurally and functionally abnormal. This can lead to heart failure because the heart can’t meet the body’s blood and oxygen needs.
The heart’s function can be affected in different ways. Some types cause the heart chambers to dilate. Others make the heart muscle abnormally thick.
This condition can also cause arrhythmias or abnormal heart rhythms. These rhythms can increase the risk of sudden cardiac death. Knowing the specific type of cardiomyopathy is key to finding the right treatment.
Global Prevalence and Statistics
Cardiomyopathy is a big global health problem with increasing numbers. The global prevalence of cardiovascular diseases, including cardiomyopathy, is expected to rise by 90% from 2025 to 2050. This shows the need for better treatments and management strategies.
Some important statistics about cardiomyopathy include:
- Cardiomyopathy affects millions worldwide, with varying prevalence depending on the type and population.
- It is a leading cause of heart failure and sudden cardiac death in younger populations.
- The economic burden of cardiomyopathy is substantial, with significant costs associated with healthcare utilization and lost productivity.
These statistics highlight the need for ongoing research and new treatments for cardiomyopathy.
Types of Cardiomyopathy and Their Distinctive Features
It’s important to know the different types of cardiomyopathy for better treatment and care. Cardiomyopathy is a group of heart muscle problems, each with its own signs and effects.
Dilated Cardiomyopathy
Dilated cardiomyopathy makes the heart’s chambers bigger. This makes it hard for the heart to pump blood well. It can cause heart failure and irregular heartbeats.
Key Features: Enlarged heart chambers, reduced ejection fraction, and risk of heart failure.
Hypertrophic Cardiomyopathy
Hypertrophic cardiomyopathy makes the heart muscle thick. This can block blood flow. It’s a big reason for sudden heart deaths in young athletes.
Key Features: Thickened heart muscle, possible blockage, and risk of sudden death.
Restrictive Cardiomyopathy
Restrictive cardiomyopathy makes the heart muscle stiff. This makes it hard for the heart to fill with blood. It can lead to heart failure and needs careful management.
Key Features: Stiffened heart muscle, hard to fill with blood, and risk of heart failure.
Arrhythmogenic Right Ventricular Cardiomyopathy
Arrhythmogenic right ventricular cardiomyopathy replaces the right ventricle’s muscle with fat. This can cause dangerous heart rhythms.
Key Features: Replaced muscle with fat, risk of dangerous heart rhythms, and risk of sudden death.
|
Type of Cardiomyopathy |
Key Features |
Clinical Implications |
|---|---|---|
|
Dilated Cardiomyopathy |
Enlarged heart chambers, reduced ejection fraction |
Heart failure, arrhythmias |
|
Hypertrophic Cardiomyopathy |
Thickened heart muscle, outflow tract obstruction |
Sudden cardiac death, heart failure |
|
Restrictive Cardiomyopathy |
Stiffened heart muscle, impaired diastolic function |
Heart failure, restrictive physiology |
|
Arrhythmogenic Right Ventricular Cardiomyopathy |
Replacement of right ventricular muscle with fatty tissue |
Ventricular arrhythmias, sudden cardiac death |
New treatments, like Hemostemix’s stem cell therapy, are helping with heart problems, including cardiomyopathy.
“The classification of cardiomyopathy into distinct types helps clinicians tailor their approach to individual patient needs, improving outcomes and quality of life.”
Common Causes and Risk Factors
Understanding cardiomyopathy’s causes and risk factors is key to managing it well. This condition is complex, influenced by genetics, lifestyle, and other health issues.
Genetic Predisposition
Genetics play a big role in some cardiomyopathies. Studies show that certain types, like dilated and hypertrophic cardiomyopathy, often have a genetic link. Specific mutations can harm the heart’s structure and function.
Genetic testing can spot those at risk early. It helps families with a cardiomyopathy history understand their risk. They can then take steps to monitor and manage it.
|
Genetic Condition |
Type of Cardiomyopathy |
Key Features |
|---|---|---|
|
Familial Dilated Cardiomyopathy |
Dilated Cardiomyopathy |
Enlarged heart chambers, reduced heart function |
|
Hypertrophic Cardiomyopathy |
Hypertrophic Cardiomyopathy |
Thickened heart muscle, possible blood flow blockage |
|
Arrhythmogenic Right Ventricular Cardiomyopathy |
Arrhythmogenic Right Ventricular Cardiomyopathy |
Fatty tissue replaces heart muscle, arrhythmia risk |
Lifestyle and Environmental Factors
Lifestyle and environment also play a part in cardiomyopathy risk. Exposure to toxins and certain chemicals can harm the heart. Nutritional deficiencies, like thiamine (vitamin B1) lack, can also cause it.
We advise those at risk or with cardiomyopathy to avoid too much alcohol. Eating a healthy diet rich in nutrients is also important for heart health.
Secondary Causes and Comorbidities
Cardiomyopathy can also stem from secondary causes and comorbidities. Conditions like coronary artery disease and hypertension can lead to it. Myocarditis, a heart muscle inflammation, often caused by viruses, is another risk factor.
Managing these secondary causes and comorbidities is key to preventing cardiomyopathy’s worsening. Treating underlying conditions is essential to protect heart health.
|
Secondary Cause/Comorbidity |
Description |
Impact on Heart |
|---|---|---|
|
Coronary Artery Disease |
Narrowing or blockage of coronary arteries |
Reduced blood flow to the heart muscle |
|
Myocarditis |
Inflammation of the heart muscle |
Damage to heart muscle cells |
|
Hypertension |
High blood pressure |
Increased workload on the heart, possible hypertrophy |
Recognizing Symptoms: When to Seek Medical Attention
It’s key to spot cardiomyopathy symptoms early to stop the disease from getting worse. The signs can vary from person to person. Knowing the common symptoms helps get medical help fast.
Early Warning Signs
The first signs of cardiomyopathy are often shortness of breath when you’re active, fatigue, and swelling in your legs, ankles, and feet. These happen because your heart can’t pump blood well. You might also feel palpitations or irregular heartbeats, which can be scary.
Other early signs include dizziness or lightheadedness. These happen when your brain doesn’t get enough blood. If you notice these, see a doctor right away.
Advanced Symptoms and Complications
As cardiomyopathy gets worse, symptoms get more serious. You might cough a lot and have frothy sputum, showing fluid in your lungs. You could also gain weight quickly because of fluid in your body.
In the worst cases, cardiomyopathy can cause heart failure. This means your heart can’t supply enough blood and oxygen. Signs of heart failure include severe shortness of breath, chest pain, and confusion. Seeing a doctor right away is very important.
We stress the need to watch for these symptoms and get medical help quickly. This can prevent serious problems and help treatment work better.
Diagnostic Approaches for Cardiomyopathy
Getting a correct diagnosis is key to managing cardiomyopathy well. We use a mix of clinical checks, lab tests, and imaging to look at the heart’s function fully.
Physical Examination and Medical History
First, we do a detailed physical check and look at your medical history. We look for signs of heart failure like swelling and unusual heart sounds. Your medical history helps us find possible causes and risk factors.
Laboratory Tests and Biomarkers
Labs are very important in diagnosing and managing cardiomyopathy. We check for:
- B-type natriuretic peptide (BNP) or N-terminal pro b-type natriuretic peptide (NT-proBNP) to see how bad heart failure is
- Troponin levels to find heart muscle damage
- Complete blood count (CBC) and metabolic panels to find other health issues
These heart failure labs help us see how bad heart failure is and if treatment is working.
Imaging Techniques (ECG, Echocardiogram, MRI)
Imaging is key for diagnosing and understanding cardiomyopathy. We use:
- Electrocardiogram (ECG) to find heart rhythm problems
- Echocardiogram to look at heart structure and function
- Cardiac MRI to see heart details and find scarring or infiltration
Cardiac MRI gives us detailed images of the heart. It helps us see cardiac function and any scarring or infiltration.
Genetic Testing and Family Screening
Genetic testing is very helpful for some cardiomyopathies, like hypertrophic cardiomyopathy. It helps us find genetic mutations early. We recommend family screening for first-degree relatives of those with genetic cardiomyopathy.
A leading cardiologist says, “Genetic testing has changed how we diagnose cardiomyopathy. It lets us find at-risk people before symptoms start.”
“The use of genetic info in practice has greatly improved our ability to diagnose and manage cardiomyopathy.”
By using all these methods, we can accurately diagnose cardiomyopathy. Then, we can create a treatment plan that meets each patient’s needs.
The Individualized Nature of Cardiomyopathy Treatment
Effective cardiomyopathy treatment plans are made just for each patient. We know that every person is different. We consider things like the type and severity of cardiomyopathy, other health issues, and what the patient prefers.
Factors Affecting Treatment Selection
Several key factors influence the selection of cardiomyopathy treatment. These include:
- The specific type of cardiomyopathy diagnosed
- The severity of symptoms and the stage of the disease
- Presence of comorbidities or secondary conditions
- Patient’s overall health, lifestyle, and preferences
- Genetic predisposition and family history
We carefully consider these factors to create a treatment plan that works best for each patient.
The Importance of Multidisciplinary Care
A team of specialists is key in treating cardiomyopathy. Our team includes cardiologists, cardiac surgeons, imaging specialists, and more. They work together to meet the complex needs of patients with cardiomyopathy.
The benefits of this approach include:
- Comprehensive assessment and diagnosis
- Coordinated treatment planning and implementation
- Access to a wide range of treatment options, including advanced therapies and surgical interventions
- Ongoing support and monitoring to adjust treatment as needed
By working together, we can give our patients the best care. This improves their outcomes and quality of life.
Medication Therapies: First-Line Treatments
First-line treatments for cardiomyopathy include various medications. These help ease symptoms and improve patient outcomes. They are key in managing the condition and boosting patients’ quality of life.
ACE Inhibitors and ARBs
ACE inhibitors and Angiotensin II Receptor Blockers (ARBs) are vital for heart failure treatment. They relax blood vessels, lower blood pressure, and ease the heart’s workload. This improves heart function and reduces symptoms.
Benefits: They improve survival rates, cut down hospital stays, and enhance life quality.
Potential Side Effects: Side effects include cough, dizziness, and high potassium levels.
Beta-Blockers and Calcium Channel Blockers
Beta-blockers slow the heart rate and reduce contraction force. This lowers blood pressure and the heart’s oxygen need. Calcium channel blockers also lower blood pressure and reduce heart workload by widening blood vessels.
|
Medication Class |
Primary Effect |
Common Examples |
|---|---|---|
|
Beta-Blockers |
Reduce heart rate and contraction force |
Metoprolol, Carvedilol |
|
Calcium Channel Blockers |
Dilate blood vessels, reduce heart workload |
Amlodipine, Verapamil |
Diuretics and Aldosterone Antagonists
Diuretics remove excess fluid, reducing swelling and shortness of breath. Aldosterone antagonists block aldosterone’s effects, a hormone that can lead to heart failure.
“Diuretics are essential in managing fluid overload in heart failure patients.” – A clinical expert.
Anticoagulants and Antiarrhythmics
Anticoagulants prevent blood clots that can cause stroke. Antiarrhythmics manage irregular heart rhythms.
For example, warfarin is a common anticoagulant that needs regular INR level checks.
Medications play a vital role in managing cardiomyopathy. They offer symptom relief and better outcomes. Understanding different medications helps healthcare providers create personalized treatment plans.
Advanced Pharmacological Interventions
New treatments are making a big difference for people with cardiomyopathy. Scientists are learning more about this condition every day. This knowledge helps them create new medicines that meet the needs of patients.
Newly Approved Medications
Recently, several new medicines have been approved for treating cardiomyopathy. One of these is Tafamidis. It has been shown to help patients with cardiac amyloidosis live longer.
Tafamidis works by stopping the formation of amyloid fibrils in the heart. These fibrils can cause cardiomyopathy. Studies have shown that Tafamidis can also reduce the number of times patients need to go to the hospital.
Targeted Therapies for Specific Types
Researchers are working on medicines that target specific types of cardiomyopathy. For example, in hypertrophic cardiomyopathy, a new drug called mavacamten is being tested. It aims to reduce the heart’s overactive contraction.
Mavacamten works by blocking the interaction between myosin and actin in the heart. This can help patients with hypertrophic cardiomyopathy feel better and do more. Early results from clinical trials are promising.
These targeted treatments are a big step forward in managing cardiomyopathy. They offer hope for better care and outcomes for patients.
|
Medication |
Type of Cardiomyopathy |
Mechanism of Action |
Clinical Benefit |
|---|---|---|---|
|
Tafamidis |
Cardiac Amyloidosis/Restrictive Cardiomyopathy |
Stabilizes transthyretin protein, preventing amyloid fibril formation |
Reduced all-cause mortality, fewer hospitalizations |
|
Mavacamten |
Hypertrophic Cardiomyopathy |
Inhibits myosin-actin interaction, reducing hypercontractility |
Improved symptoms, enhanced functional capacity |
Treating Dilated Cardiomyopathy: Specific Approaches
Dilated cardiomyopathy makes the heart bigger. It needs special treatments to help patients. These treatments include medicines, devices, and surgery.
Medical Management Strategies
Medical care is key for treating dilated cardiomyopathy. It aims to lessen symptoms and slow the disease. We use medicines like ACE inhibitors, beta-blockers, and diuretics to help the heart.
“The use of evidence-based medications has significantly improved outcomes in patients with dilated cardiomyopathy,” as noted by recent clinical guidelines.
ACE inhibitors and ARBs help the heart work better. Beta-blockers lower the risk of death and illness. Diuretics help with too much fluid in the body.
Device Therapies and Surgical Options
Device therapies have changed how we treat dilated cardiomyopathy. Cardiac Resynchronization Therapy (CRT) makes the heart beat better. This improves its function and reduces symptoms.
Other devices, like Implantable Cardioverter-Defibrillators (ICDs), prevent sudden death in high-risk patients. Surgery, like heart transplant, is for severe cases when other treatments don’t work.
“The advancement in device therapies has provided new avenues for improving the quality of life and survival in patients with dilated cardiomyopathy,” as highlighted in recent medical literature.
Hypertrophic Cardiomyopathy Treatment Options
Managing hypertrophic cardiomyopathy requires a variety of treatments to help patients. Each case is different, so we tailor our approach to fit each patient’s needs.
Medication Regimens
Medicines are key in treating hypertrophic cardiomyopathy. Beta-blockers are often the first choice. They help by slowing the heart rate and reducing contraction force. We also use calcium channel blockers and disopyramide to ease symptoms and boost exercise ability.
Septal Reduction Therapies
For those with severe symptoms, we consider septal reduction therapies. Alcohol septal ablation is a procedure that thins the septal wall. This improves blood flow. We also look into surgical septal myectomy, which removes part of the thickened wall.
Managing Outflow Tract Obstruction
Reducing left ventricular outflow tract obstruction (LVOTO) is vital. We use medicines and septal therapies to do this. Sometimes, pacemaker implantation is needed to better coordinate the heartbeat and lessen obstruction.
Our goal is to improve patients’ lives with a detailed and personalized treatment plan. We follow the latest guidelines and focus on patient-centered care.
Restrictive Cardiomyopathy: Treatment Challenges and Solutions
Restrictive cardiomyopathy is a condition where the heart muscle gets stiff. This makes it hard for the heart to fill with blood. Finding the right treatment is a big challenge.
Symptom Management
Managing symptoms of restrictive cardiomyopathy is key to better patient care. Diuretics help reduce fluid buildup. This relieves symptoms like shortness of breath and swelling. We also use other medicines to handle related issues, like irregular heartbeats.
It’s important to keep an eye on how patients respond to treatment. This helps us adjust plans as needed. Each patient’s case is different, so we tailor our approach.
Treating Underlying Causes
Sometimes, restrictive cardiomyopathy is caused by other conditions like amyloidosis or hemochromatosis. Treating these causes is vital. For example, treatments that reduce amyloid deposits can slow the disease’s progress.
Genetic factors also play a role in some cases. We consider genetic screening when it’s relevant. This helps us catch and manage the condition early.
Market Growth in Treatment Options
The market for treatments for restrictive cardiomyopathy is expected to grow a lot. It’s forecasted to jump from USD 112.3 million in 2025 to USD 195.5 million by 2035, according to Future Market Insights. This growth is due to new treatments and more awareness among doctors.
As research improves, we hope to see more treatments that target the heart’s specific issues. This could bring new hope to those dealing with this tough condition.
Surgical Interventions and Device Therapies
Surgical and device therapies have changed how we treat heart disease. They offer hope to those with severe heart conditions. These treatments aim to boost heart function, lessen symptoms, and improve life quality for those who haven’t seen results from medicine.
Implantable Cardioverter-Defibrillators (ICDs)
ICDs are small devices implanted under the skin. They watch the heart’s rhythm and shock it when needed to stop dangerous arrhythmias. ICDs have been shown to significantly reduce mortality in patients with cardiomyopathy at high risk of sudden cardiac death. Doctors decide to implant an ICD based on heart failure severity, left ventricular ejection fraction, and arrhythmia presence.
Cardiac Resynchronization Therapy (CRT)
CRT is a treatment for heart failure that uses a pacemaker to sync the left and right ventricles. This therapy is beneficial for patients with certain cardiomyopathy types who have electrical conduction delays. It improves heart function, reduces heart failure symptoms, and enhances life quality.
Ventricular Assist Devices (VADs)
VADs are mechanical devices implanted in patients with advanced heart failure. They support the heart’s pumping function. VADs have been shown to improve survival and quality of life in patients with end-stage heart failure.
Heart Transplantation
Heart transplantation is the ultimate treatment for some patients with end-stage cardiomyopathy. The decision to transplant involves a thorough evaluation of the patient’s health, heart failure severity, and other medical conditions. Advances in immunosuppressive therapy have significantly improved the long-term outcomes of heart transplant recipients.
|
Therapy |
Indications |
Benefits |
|---|---|---|
|
ICDs |
High risk of sudden cardiac death |
Prevention of life-threatening arrhythmias |
|
CRT |
Heart failure with ventricular dyssynchrony |
Improved heart function, reduced symptoms |
|
VADs |
Advanced heart failure |
Support for heart function, bridge to transplantation |
|
Heart Transplantation |
End-stage cardiomyopathy |
Definitive treatment, improved long-term survival |
Emerging Treatments and Future Directions
New treatments bring hope to those with cardiomyopathy. Research is moving towards more tailored and creative ways to help.
Gene Therapy Approaches
Gene therapy is a promising new way to treat cardiomyopathy. It targets the genetic causes of the disease. Recent studies have shown encouraging results in early trials, hinting at future human use.
Gene editing, like CRISPR/Cas9, is also being explored. It could fix genetic mutations that cause cardiomyopathy. This could be a game-changer for inherited forms of the disease.
Stem Cell Therapies
Stem cell therapies are getting a lot of attention for their ability to heal the heart. Hemostemix’s stem cell therapy, for example, has shown promise. It helps create new blood vessels and improves heart function.
Clinical trials are ongoing to see if stem cell therapies work for cardiomyopathy. Early signs are positive, with patients showing better heart function and fewer symptoms.
|
Therapy Type |
Mechanism |
Potential Benefits |
|---|---|---|
|
Gene Therapy |
Targets genetic causes |
Corrects underlying mutations |
|
Stem Cell Therapy |
Promotes regeneration |
Improves heart function |
|
Remote Monitoring |
Continuous patient monitoring |
Early detection of complications |
Remote Monitoring Technologies
Remote monitoring is changing how we manage cardiomyopathy. It lets us keep an eye on patients’ health 24/7. This means we can catch problems early.
Advanced biosensors and wearable devices are part of this. They help us collect and analyze data in real-time. This improves care and makes life better for patients by cutting down on hospital visits.
As we dive deeper into these new treatments, it’s clear the future is bright. A mix of new therapies and tech will lead to better care. By keeping up with these advances, we can give our patients the best care possible.
Lifestyle Modifications and Supportive Care
Managing cardiomyopathy goes beyond just medicine. It includes important lifestyle changes and supportive care. These changes can greatly improve life for those with cardiomyopathy.
Dietary Recommendations
Eating well is key for managing cardiomyopathy. We suggest a diet full of fruits, veggies, whole grains, and lean proteins. It’s also good to cut down on sodium, as too much can worsen heart failure symptoms.
Try to keep sodium intake under 2,000 mg a day. This can help control fluid and blood pressure.
- Choose low-sodium options when available.
- Use herbs and spices to flavor food instead of salt.
- Limit processed and packaged foods, which are often high in sodium.
It’s also important to drink enough water but not too much. Too much water can put extra strain on the heart. Talk to your doctor about how much water is right for you.
Exercise Guidelines
Regular exercise is good for the heart and overall health in people with cardiomyopathy. But, the right exercise depends on the person’s health and ability. Always talk to a doctor before starting any new exercise.
- Start with gentle activities like walking or yoga.
- Slowly increase the intensity and time as you get stronger and with doctor’s advice.
- Watch for signs like shortness of breath, chest pain, or feeling dizzy during exercise.
Exercise not only boosts physical health but also helps with mental well-being. It can lower stress and anxiety.
Stress Management and Mental Health Support
Managing stress is a big part of caring for cardiomyopathy. Stress can harm the heart, so finding ways to manage it is important. Mindfulness, meditation, and deep breathing can help reduce stress.
“The mind and heart are closely linked; taking care of one helps the other.”
— Cardiologist’s Insight
Also, getting help from mental health professionals is key. They can teach ways to deal with the emotional side of cardiomyopathy. Support groups, online or in-person, can also offer a sense of community and understanding.
By making these lifestyle changes and getting supportive care, people with cardiomyopathy can see better symptoms and quality of life. We encourage patients to work with their healthcare team to create a plan that fits their needs.
Specialized Cardiac Care Programs
. These programs include:
- Advanced tests to accurately diagnose and monitor cardiomyopathy
- Personalized treatment plans from a team of experts
- Latest therapies like medication, devices, and surgery
- Support services like diet advice, exercise plans, and mental health help
Our team always looks for the latest in treating cardiomyopathy. This helps us have significant success rates in managing the condition and improving patient results.
Patient Outcomes and Success Rates
We are proud of our success with cardiomyopathy patients. Our special care programs have led to:
- Better symptom control and quality of life for patients
- Fewer hospital stays thanks to effective treatment and monitoring
- Happier patients with care and support tailored to them
We aim to provide the best healthcare for international patients. Our cardiomyopathy treatment is designed to meet each patient’s unique needs, ensuring the best results.
Conclusion: The Future of Cardiomyopathy Treatment
Cardiomyopathy treatment is a complex field that needs a full approach. With ongoing research and new treatments, the future looks bright.
Recent studies and market forecasts show a positive outlook for treating cardiomyopathy. We can expect more investment in new therapies and technologies. This means we’ll see more progress in cardiomyopathy treatment, like targeted therapies and new device technologies.
The future directions in managing cardiomyopathy will be influenced by emerging treatments like gene therapy and stem cell therapies. These new methods will likely lead to better patient outcomes and a higher quality of life.
We’re dedicated to top-notch healthcare for international patients. By keeping up with the latest in cardiomyopathy treatment, we aim to give our patients the best care and support.
FAQ
What is cardiomyopathy and how does it affect the heart?
Cardiomyopathy is a disease that affects the heart muscle. It makes it hard for the heart to pump blood. This can lead to heart failure and other problems. It can be caused by genetics, lifestyle, and the environment.
What are the different types of cardiomyopathy?
There are several types of cardiomyopathy. These include dilated cardiomyopathy, hypertrophic cardiomyopathy, restrictive cardiomyopathy, and arrhythmogenic right ventricular cardiomyopathy. Each type needs a specific treatment plan.
What are the common symptoms of cardiomyopathy?
Symptoms of cardiomyopathy include shortness of breath, fatigue, swelling, and palpitations. It’s important to notice these symptoms early. This way, you can get medical help quickly.
How is cardiomyopathy diagnosed?
Doctors use a few ways to diagnose cardiomyopathy. They do a physical exam, run lab tests, and use imaging like ECG, echocardiogram, and MRI. They also do genetic testing. These tools help them understand the heart’s function and decide on treatment.
What are the treatment options for cardiomyopathy?
Treatment for cardiomyopathy varies based on the type and how severe it is. It might include medicines, devices, surgery, or changes in lifestyle. We focus on treating each patient as an individual and work together as a team for the best results.
What is the role of medication in treating cardiomyopathy?
Medicines like ACE inhibitors, beta-blockers, diuretics, and anticoagulants are key in treating cardiomyopathy. They help manage symptoms and improve outcomes. We talk about the benefits and possible side effects of these medicines.
What are the latest advancements in cardiomyopathy treatment?
New treatments for cardiomyopathy include gene therapy, stem cell therapies, and remote monitoring. We look at the good and bad sides of these new methods.
How can lifestyle modifications help manage cardiomyopathy?
Making lifestyle changes can greatly help patients with cardiomyopathy. This includes following a special diet, exercising, and managing stress. We offer advice on these helpful changes.
What is the significance of multidisciplinary care in cardiomyopathy treatment?
A team of specialists is important for treating cardiomyopathy. This team approach ensures patients get the best care. We explain why working together is key.
What is non-ischemic cardiomyopathy?
Non-ischemic cardiomyopathy is a type of cardiomyopathy not caused by heart attacks or blocked arteries. We discuss its unique features and how it’s treated.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/23321515/


































