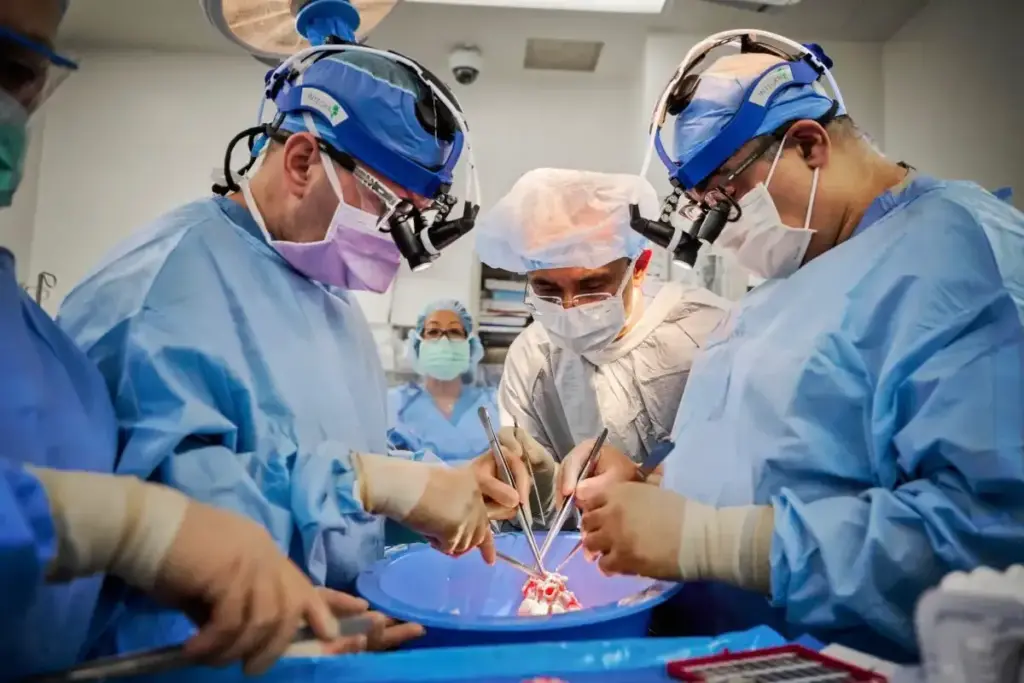
Cardiovascular surgeons are medical experts who work on the heart and big blood vessels. They deal with many issues, like heart disease and birth defects.
Our cardiac and heart surgeons offer top-notch care. They use the latest methods to help patients get better. These surgeons do many tough surgeries, like fixing heart valves and transplanting hearts.
Key Takeaways
- Cardiovascular surgeons perform surgical operations on the heart and great vessels.
- They handle a wide range of conditions, from coronary artery disease to complex congenital heart defects.
- Our cardiac and heart surgeons provide world-class care using cutting-edge techniques.
- Complex procedures include CABG, heart valve repair and replacement, and heart transplantation.
- Cardiovascular surgeons ensure the best possible outcomes for patients.
The Vital Role of a Cardiothoracic Surgeon in Modern Medicine
Cardiothoracic surgeons are key in saving lives through surgery. They specialize in heart, lung, and chest organ surgeries. Their work is vital in modern medicine.
Many people get confused about heart specialists. Let’s clear up the difference between cardiologists and cardiovascular surgeons. Cardiologists treat heart issues with medicine and lifestyle changes. Cardiovascular surgeons, on the other hand, perform surgeries on the heart and chest.
Difference Between Cardiologists and Cardiovascular Surgeons
It’s important to know the difference between cardiologists and cardiovascular surgeons. Cardiologists focus on heart health through medicine and lifestyle. Cardiovascular surgeons do surgeries on the heart and chest.
For example, a cardiologist might use medicine for heart failure. A cardiovascular surgeon might do a heart transplant if needed.
Educational Path and Training Requirements
Becoming a cardiovascular surgeon is a big journey. It starts with a bachelor’s degree and four years of medical school for an MD or DO. Then, they do a general surgery residency for five to seven years.
After that, they get specialized training in cardiothoracic surgery. This can take two to three years or more. A study on the National Center for Biotechnology Information shows that this training is key for high-quality surgery.
|
Stage |
Duration |
Description |
|---|---|---|
|
Bachelor’s Degree |
4 years |
Pre-medical education |
|
Medical School |
4 years |
Earn MD or DO degree |
|
General Surgery Residency |
5-7 years |
Hands-on surgical training |
|
Cardiothoracic Surgery Fellowship |
2-3 years |
Specialized training in cardiothoracic surgery |
Specializations Within Cardiovascular Surgery
Cardiovascular surgery has many specializations. These include pediatric cardiac surgery, heart transplantation, and adult cardiac surgery. Pediatric cardiac surgeons fix heart defects in children. Heart transplant surgeons transplant hearts from donors to recipients.
Adult cardiac surgeons do a variety of surgeries, like coronary artery bypass grafting and valve repairs. Each specialization needs a deep understanding of the heart and the latest techniques.
As cardiovascular surgeons improve their skills, they can offer better and less invasive treatments. This helps their patients more.
The Evolution of Cardiovascular Surgery Through the Decades
Cardiovascular surgery has seen huge changes over the years. It started simple and has grown into today’s advanced field. This shows how much humans have learned and improved in medicine.
Historical Milestones in Heart Surgery
Heart surgery has a long and exciting history. The first successful heart surgery was done early in the 20th century. This was just the start of many important steps forward.
One big step was the creation of coronary artery bypass grafting (CABG). It’s now a key way to treat heart disease. Another major moment was the first heart transplant in 1967 by .This surgery was a big leap for treating severe heart failure.
Technological Advancements Shaping Modern Practices
New technologies have greatly changed heart surgery today. Robot-assisted surgery is one example. It makes surgeries less invasive, leading to faster recovery and better results.
Also, new imaging and diagnostic tools help heart surgeons do complex surgeries more accurately. These technologies keep improving, making care better and opening up more treatment options.
Pioneers Who Revolutionized Cardiac Surgery
Many pioneers have greatly helped heart surgery are two examples. They’ve pushed the field forward and improved care for patients.
Their work inspires today’s cardiac care specialists. We keep adding to their achievements, aiming to give the best care to our patients. As thoracic surgery experts, we honor their legacy and strive for excellence.
Coronary Artery Bypass Grafting (CABG): The Gold Standard Procedure

Coronary Artery Bypass Grafting (CABG) is a key treatment for severe heart disease. It’s a surgery that fixes blocked arteries by using grafts. This improves blood flow to the heart.
When CABG Is Necessary: Indications and Patient Selection
CABG is for those with serious heart blockages who haven’t gotten better with other treatments. Doctors decide if CABG is right based on symptoms, disease extent, and overall health.
Those with many blockages, complex heart structures, or past failed angioplasty might need CABG. People with diabetes or at high risk of heart problems also might get CABG.
The Surgical Process Explained Step by Step
The CABG surgery starts with general anesthesia to keep the patient comfortable. The surgeon then opens the chest to reach the heart. Usually, this is done by splitting the breastbone.
Next, the surgeon takes grafts from the leg or chest. These are used to bypass the blocked arteries. The grafts are carefully attached to the arteries to ensure blood flow.
After the grafts are in place, the surgeon checks the heart’s function. The chest is closed, and the patient goes to the ICU for recovery.
Recovery and Outcomes After CABG
Recovery from CABG includes hospital stay and a rehab program. Patients are watched for any issues and given meds for pain and infection prevention.
Most patients see big improvements in symptoms after CABG. They feel less pain and live better lives. CABG’s long-term results are good, with many patients living longer and needing fewer treatments.
Knowing about CABG can be scary. But, with better surgery and care, it’s a powerful treatment for heart disease. It gives patients a second chance at life.
Heart Valve Repair and Replacement: Restoring Proper Blood Flow
Fixing heart valves is key to keeping blood flowing right. Heart valves make sure blood moves in one direction through the heart. If they get sick, it can cause big problems.
Mitral Valve Procedures and Success Rates
The mitral valve is between the heart’s chambers. It can get sick, causing problems like mitral regurgitation or stenosis. Mitral valve repair is better than replacing it if you can, because it keeps your own valve tissue.
Most people who get mitral valve repair feel a lot better afterward. How well it works depends on the valve’s problem, who you are, and the surgeon’s skill.
Aortic Valve Procedures: Traditional and Innovative Approaches
The aortic valve is also important and can get sick. Aortic valve replacement used to be the only choice, but now transcatheter aortic valve replacement (TAVR) is an option for some.
- TAVR is less invasive and helps patients who can’t have open-heart surgery.
- Traditional surgery is best for many, giving great long-term results.
Tricuspid and Pulmonary Valve Surgeries
Tricuspid and pulmonary valve diseases are not as common but need careful treatment. Tricuspid valve repair is common, mainly for regurgitation.
Pulmonary valve disease might need surgery, more so in people born with heart problems. The choice between repair or replacement depends on the problem and the patient.
Mechanical vs. Biological Valve Options: Making the Right Choice
Choosing between a mechanical valve and a biological valve is important when replacing a valve. Mechanical valves last long but need lifelong blood thinners. Biological valves don’t need blood thinners but don’t last as long.
- Mechanical valves are best for younger people who can handle blood thinners.
- Biological valves are for older people or those who can’t take blood thinners.
The right choice between mechanical and biological valves depends on the patient’s age, lifestyle, and health. Our cardiac care team helps pick the best option for each patient.
Aortic Surgery: Addressing the Body’s Main Arterial Highway
Aortic surgery treats many conditions, like aneurysms and dissections. The aorta is the biggest artery, carrying blood from the heart. Diseases here can be deadly and need surgery.
Aortic Aneurysm Repair Techniques
Fixing an aortic aneurysm is a big part of aortic surgery. An aneurysm is when the aorta bulges and might burst. There are two main ways to fix it: open surgery and endovascular repair.
Open surgery means cutting the chest or belly to reach the aorta. Surgeons replace the weak part with a synthetic graft. But, it takes longer to get better.
Endovascular repair is less invasive. A stent-graft is put in through the groin and goes to the aneurysm. It stops the aorta from getting worse. This method is good for those at high risk or with complex anatomy.
Emergency Aortic Dissection Treatment
Aortic dissection is a tear in the aorta’s inner layer. It can cause severe pain and organ failure. Quick surgery is needed to fix the tear and stop the dissection.
The treatment depends on the tear’s location and size. For the top part of the aorta, surgery is usually needed right away. For the bottom part, treatment starts with medicine, with surgery if needed.
Endovascular vs. Open Surgical Approaches: Pros and Cons
Endovascular and open surgery have their benefits and drawbacks. Endovascular is less invasive, leading to shorter stays and faster recovery. But, it’s not for everyone, like those with complex anatomy.
Open surgery is more invasive but treats some conditions better. It’s needed in emergencies for direct repair. But, it takes longer to recover and might be riskier for some.
Choosing between endovascular and open surgery depends on many factors. The patient’s health, the condition, and the surgeon’s skills are all important. Each case is different, and the best choice varies.
Congenital Heart Defect Corrections: From Infancy to Adulthood
Fixing congenital heart defects is key in heart surgery, from babies to grown-ups. These defects are heart problems that babies are born with. They can be simple or very complex, needing surgery.
Common Congenital Heart Conditions Requiring Surgical Intervention
Many congenital heart defects need surgery. Here are some examples:
- Septal defects, which involve holes in the walls between the heart’s chambers.
- Tetralogy of Fallot, a combination of four heart defects that can lead to cyanosis.
- Coarctation of the aorta, a narrowing of the major artery that carries blood from the heart.
- Transposition of the great arteries, where the two main arteries that carry blood out of the heart are reversed.
|
Condition |
Description |
Surgical Approach |
|---|---|---|
|
Septal Defects |
Holes in the heart’s chambers |
Closure with a patch or device |
|
Tetralogy of Fallot |
Combination of four heart defects |
Corrective surgery to repair defects |
|
Coarctation of the Aorta |
Narrowing of the aorta |
Resection and grafting or balloon angioplasty |
Pediatric Cardiovascular Surgical Approaches and Considerations
Pediatric heart surgery is very specialized. It must consider the unique heart anatomy and function of children. Surgeons look at the child’s age, size, and health when planning surgery.
Key considerations include:
- The need for precise preoperative planning and imaging.
- The use of cardiopulmonary bypass techniques adapted for pediatric patients.
- Minimizing the impact of surgery on the child’s development and quality of life.
Adult Congenital Heart Disease: Delayed and Revisional Surgery
More children with heart defects are living into adulthood. This means they need ongoing heart care. Some may need surgery again because of new or old defects.
Challenges in adult congenital heart disease include:
- Managing complex anatomy that has been altered by previous surgeries.
- Addressing issues related to long-term cardiac function and possible other health problems.
- Coordinating care between pediatric and adult cardiology teams.
Heart Transplantation: The Ultimate Life-Saving Cardiac Surgery
For those with severe heart issues, a heart transplant can be a second chance. This complex surgery replaces a sick heart with a healthy one from a donor. As a cardiothoracic surgeon, we know the details of this life-saving surgery.
Patient Selection Criteria and Waiting List Process
The journey to a heart transplant starts with choosing the right patient. People with end-stage heart failure, with no other options, are considered. We look at how sick they are, their overall health, and if they can recover well after the transplant.
The waiting list is strict. We check the patient’s medical history, current health, and if they match with donors. Patients are ranked by how urgent they need a transplant and if they match well with donors.
|
Criteria |
Description |
Importance Level |
|---|---|---|
|
Medical Urgency |
Severity of heart failure and need for immediate transplant |
High |
|
Compatibility |
Matching donor and recipient based on blood type, tissue type, and other factors |
High |
|
Overall Health |
Evaluation of other health issues that could affect transplant success |
Medium |
The Transplantation Procedure: Donor to Recipient
The transplant process is a team effort. When a donor heart is found, the team acts fast. They remove the sick heart and put in the new one, connecting it to the recipient’s blood vessels.
The surgical steps include:
- Preparation of the recipient, including anesthesia and connection to a heart-lung machine
- Removal of the diseased heart, preserving key blood vessels
- Implantation of the donor heart, connecting it to the recipient’s vessels
- Monitoring and support during the initial recovery phase
Post-Transplant Care, Rejection Prevention, and Survival Rates
After the transplant, care is key. Patients need lifelong medicine to avoid rejecting the new heart. Regular check-ups and monitoring help catch any problems early.
Studies show heart transplant survival rates have gone up.
“The one-year survival rate after heart transplantation is now over 85%, with many patients enjoying a good quality of life post-transplant.”
We take a team approach to care after the transplant. This includes cardiologists, surgeons, and more to support our patients fully.
Minimally Invasive Cardiovascular Surgical Techniques
New medical tech has brought about big changes in heart surgery. These changes offer patients new, less invasive options instead of old open-heart surgery.
Robotic-Assisted Heart Surgery: Precision and Control
Robotic heart surgery is a big step forward. It lets surgeons do complex surgeries with better precision and control. This way, they can do detailed work through small cuts, which means less damage and quicker healing.
Key benefits of robotic-assisted heart surgery include:
- Improved dexterity and visualization for surgeons
- Smaller incisions, resulting in less scarring and trauma
- Reduced risk of complications and infection
- Faster recovery times for patients
Small Incision Approaches for Reduced Recovery Time
Small incision surgery is gaining popularity. It’s known for helping patients recover faster. With smaller cuts, there’s less damage, less pain, and quicker return to daily life.
The advantages of small incision approaches include:
- Less post-operative pain
- Shorter hospital stays
- Faster return to normal activities
- Improved cosmetic outcomes
Benefits and Limitations of Minimally Invasive Techniques
Minimally invasive heart surgery has many benefits but also some downsides. It’s important for patients to know both sides to make the best choice for their care.
The good news is faster recovery, less pain, and better looks. But, there are challenges too. These include the need for skilled surgeons, the cost of new tech, and limits on the types of surgeries it can handle.
|
Technique |
Benefits |
Limitations |
|---|---|---|
|
Robotic-Assisted Surgery |
Enhanced precision, less trauma |
High cost, specialized training |
|
Small Incision Approaches |
Faster recovery, less pain |
Limited complexity, possible complications |
Transcatheter Procedures: The Cutting Edge of Cardiovascular Surgery
Transcatheter procedures are a new way to treat heart problems. They use small catheters to reach the heart through tiny cuts. This method is less invasive than traditional surgery and helps patients recover faster.
Transcatheter Aortic Valve Replacement (TAVR): Revolution in Valve Treatment
TAVR has changed how we treat aortic valve stenosis. It replaces the old valve with a new one through a catheter. TAVR has greatly improved survival and quality of life for high-risk patients.
Transcatheter Mitral Valve Repair: MitraClip and Beyond
Transcatheter mitral valve repair, like the MitraClip, is a new treatment for mitral regurgitation. It clips the mitral valve leaflets together. This method has been effective in reducing mitral regurgitation and improving patient outcomes.
Emerging Catheter-Based Interventions Changing Patient Outcomes
New catheter-based treatments are also making a big difference. These include devices and techniques for treating various heart conditions. We are dedicated to keeping up with these advancements. This ensures our patients get the best treatments available.
Global Trends and Future Projections in Cardiovascular Surgery
Cardiovascular surgery trends show a mix of aging populations, new tech, and healthcare access. As more people get older and heart disease grows, the need for heart surgeries will jump a lot.
New, less invasive surgeries are becoming common. This change is thanks to tech progress and the goal for better patient results. But, this change isn’t the same everywhere. Different places face challenges in access and practice.
Projected Growth to 1.8 Million Surgeries by 2040
By 2040, we expect 1.8 million heart surgeries. This rise comes from more older people and more heart disease. Healthcare systems worldwide will need to handle this increased demand.
A study in a top medical journal said we’ll need more heart surgery capacity. This means more surgeons, facilities, and better tech and methods.
“The future of cardiovascular surgery is heavily dependent on our ability to adapt to the changing healthcare landscape, leveraging technology and innovation to meet the growing demand for surgical services.”
A Cardiothoracic Surgeon
Demographic Factors Driving Increased Surgical Demand
Older populations and more heart disease are key reasons for more surgeries. As people live longer, they face more heart problems, leading to more surgeries.
- Aging population
- Increasing prevalence of heart disease
- Rising rates of obesity and diabetes
These trends mean more heart disease, which means more surgeries. It’s important for health planners and policymakers to understand these trends. They need to make sure there are enough resources for heart surgeries in the future.
Regional Variations in Cardiovascular Surgical Practices and Access
Cardiovascular surgery varies a lot around the world. This is due to things like healthcare setup, money, and the number of skilled surgeons.
|
Region |
Number of Cardiothoracic Surgeons per Million Population |
Access to Cardiovascular Surgical Care |
|---|---|---|
|
North America |
15.6 |
High |
|
Europe |
12.3 |
Moderate to High |
|
Asia-Pacific |
6.8 |
Variable |
|
Africa |
2.1 |
Low |
The table shows big differences in getting heart surgery around the world. Fixing these gaps is key to making sure everyone can get the heart surgery they need.
Mortality Rates and Outcome Improvements: A Success Story
The world of heart surgery has changed a lot. Mortality rates have dropped a lot. This is thanks to better surgery methods, care before and after surgery, and new technology.
Historical vs. Current Mortality Statistics
Oldly, heart surgeries had high death rates. But now, the numbers have gone down a lot. For example, the death rate for coronary artery bypass grafting (CABG) has dropped a lot in recent years.
This drop is due to better patient choices, surgery techniques, and care after surgery. The job of a cardiothoracic surgeon has changed too. Now, they focus more on being precise and caring for each patient personally.
Factors Contributing to Improved Outcomes
Many things have helped make heart surgery better. These include:
- Improvements in surgery methods and technology
- Better care before and after surgery
- More use of less invasive procedures
- Cardiac care specialists getting better training
These changes have made heart surgery safer and more successful. Now, more people can get the help they need without as much risk.
Procedure-Specific Success Rates
Top hospitals are seeing great results from heart surgeries. For example, CABG success rates are over 95% in many places. Some hospitals even have higher success rates.
We keep working to be the best in heart care. Our cardiac care specialists and modern facilities are key to our success. We’re dedicated to giving our patients the best care possible.
.
Key aspects of our protocol adherence include:
- Regular training and education for our cardiothoracic surgeons
- Implementation of the latest surgical techniques and technologies
- Continuous monitoring of patient outcomes to improve care
International Standards and Benchmark Outcomes
We compare our results with the best worldwide. This ensures our patients get top-notch care.
Commitment to international standards in cardiac care is a testament to its dedication to patient well-being and medical excellence.” –
Medical Expert Review
We strive for the best outcomes through a team effort. This ensures every patient gets full and coordinated care.
Multidisciplinary Team Approach to Complex Cardiac Cases
Handling complex heart cases needs a team of specialists. Our team creates personalized treatment plans for each patient.
The benefits of our team approach include:
- Comprehensive care that addresses all aspects of a patient’s condition
- Improved patient outcomes through coordinated treatment plans
- Enhanced patient experience through supportive and empathetic care
By combining the skills of heart surgeons, cardiologists, and other experts, we give our patients the best care for complex heart issues.
Conclusion: The Bright Future of Cardiovascular Surgical Interventions
The future of heart surgery looks bright. New techniques and technologies are coming along. As a heart surgeon, we aim to give top-notch care.
More people will need heart surgery worldwide. This means we need more skilled doctors. We’re working hard to use new ideas to help our patients.
We follow international standards. This ensures our patients get the best care. We’re committed to helping patients from around the world get the care they need.
FAQ
What is the difference between a cardiologist and a cardiovascular surgeon?
A cardiologist treats heart conditions with medicine. A cardiovascular surgeon fixes or replaces damaged heart parts with surgery.
What kind of training is required to become a cardiovascular surgeon?
To be a cardiovascular surgeon, you need a medical degree and lots of surgical training. This includes a residency in cardiothoracic surgery and maybe more training in areas like pediatric cardiac surgery.
What are some common procedures performed by cardiovascular surgeons?
Cardiovascular surgeons do many things. They do coronary artery bypass grafting, heart valve repairs, and aortic surgery. They also transplant hearts and fix congenital heart defects.
What is coronary artery bypass grafting (CABG), and when is it necessary?
CABG is a surgery to bypass blocked arteries. It’s needed when heart disease is severe and medicine doesn’t work.
What are the benefits of minimally invasive cardiovascular surgical techniques?
Minimally invasive surgeries, like robotic heart surgery, have big benefits. They use smaller cuts, cause less damage, and help you recover faster. They might also lead to fewer complications.
What is transcatheter aortic valve replacement (TAVR), and how does it differ from traditional aortic valve replacement?
TAVR is a less invasive way to replace the aortic valve. It uses a catheter instead of open-heart surgery. This can mean less recovery time.
How has the field of cardiovascular surgery evolved over the decades?
Cardiovascular surgery has grown a lot. Advances in tech, surgery, and understanding heart disease have been key. Milestones include CABG, heart transplants, and new, less invasive methods.
What are the success rates for cardiovascular surgical procedures?
Success rates vary by procedure and patient. But, thanks to better tech and understanding, many surgeries have high success rates and low death rates.
What is the role of a cardiovascular surgeon in treating congenital heart defects?
Cardiovascular surgeons are key in fixing heart defects at birth. They work with pediatric cardiologists and others to care for patients from birth to adulthood.
How do cardiovascular surgeons contribute to the management of complex cardiac cases?
Cardiovascular surgeons are part of a team for complex heart cases. They use their surgical skills, working with others to get the best results for patients.
What are some of the emerging trends and future projections in cardiovascular surgery?
The field of cardiovascular surgery is growing. It’s driven by more heart disease and an aging population. New trends include better minimally invasive methods and new tech.
How has the mortality rate for cardiac surgeries changed over time?
The death rate for heart surgeries has dropped a lot. This is thanks to better surgery, care, and tech. Today, many heart surgeries have very low death rates.
What is the significance of a multidisciplinary team approach in cardiovascular surgery?
A team approach is vital in heart surgery. It brings together experts for complex cases. This ensures patients get the best care and outcomes.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC8406810/[1























