
Childhood leukemia is a treatable cancer, with ALL survival rates up to 96 percent. At Liv Hospital, we aim to provide top-notch healthcare. We support international patients with the latest treatments, both traditional and natural. Explore childhood leukemia therapy options and natural approaches to improve outcomes.
Parents and caregivers look for reliable therapies for childhood leukemia. Our hospital is dedicated to global standards and patient care. We offer hope to families seeking the safest and most effective ways to treating leukemia.
Key Takeaways
- Childhood leukemia is highly treatable with survival rates up to 96% for ALL.
- Liv Hospital offers support for international patients.
- Conventional therapies include chemotherapy, targeted drugs, and immunotherapies.
- Emerging research explores natural and integrative approaches.
- Patient-centered innovation is at the heart of our treatment options.
Childhood Leukemia: A Highly Treatable Form of Cancer
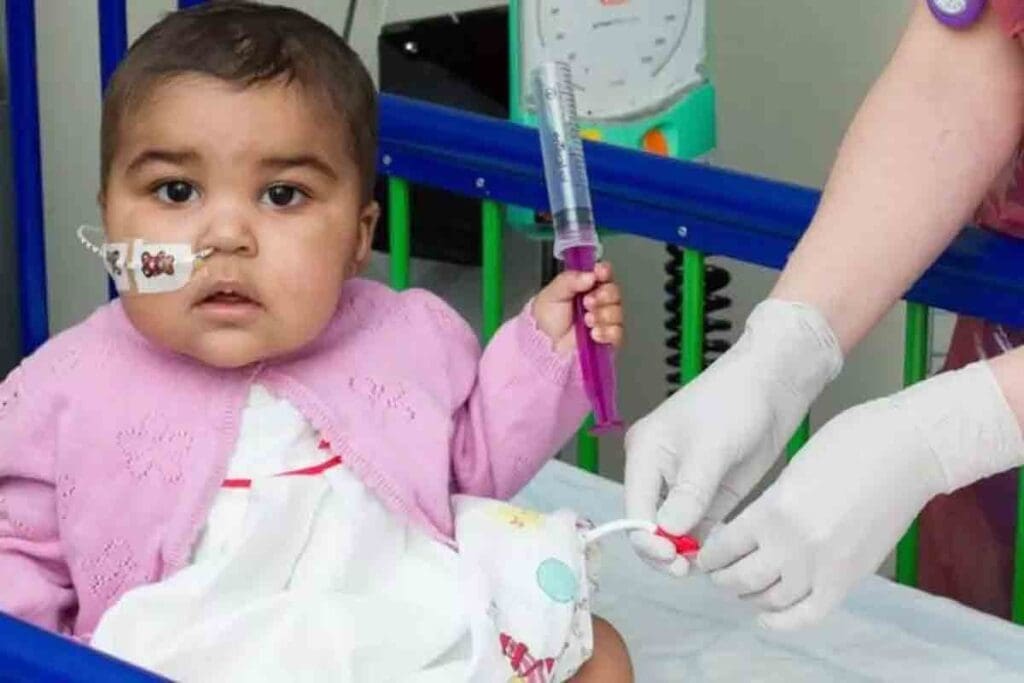
Medical science has made big strides in treating childhood leukemia. This has led to better survival rates for kids. The progress is thanks to a deeper understanding of the disease and new treatments.
Types of Childhood Leukemia and Their Characteristics
Childhood leukemia comes in several types, each with its own traits. Acute Lymphoblastic Leukemia (ALL) is the most common, making up about 80% of cases. It’s marked by the fast growth of immature lymphocytes, a type of white blood cell.
Other types, like Acute Myeloid Leukemia (AML), Chronic Lymphocytic Leukemia (CLL), and Chronic Myeloid Leukemia (CML), are less common in kids. Each type has its own unique features that help doctors choose the best treatment.
Key characteristics of common childhood leukemia types:
- ALL: Starts quickly, has immature lymphocytes, and is very treatable with chemotherapy.
- AML: More aggressive, needs strong chemotherapy and sometimes bone marrow transplant.
Current Survival Rates Reaching 96% for ALL
Survival rates for childhood leukemia, mainly ALL, have seen a big jump. Studies show that the five-year survival rate for ALL in kids is now up to 96%. This improvement is thanks to better chemotherapy, targeted therapies, and care support.
Several factors have contributed to this high survival rate:
- Early diagnosis and starting treatment right away.
- Customized treatment plans based on the leukemia’s genetic makeup.
- Advances in chemotherapy and targeted therapy.
Factors Affecting Treatment Success
While the outlook for childhood leukemia is good, several factors can impact treatment success. These include the leukemia type, the child’s age, genetic factors, and how well the leukemia responds to treatment.
Knowing these factors helps doctors create treatment plans that fit each child’s needs. This approach can lead to better results.
Factors influencing treatment success:
- Genetic factors: Certain genetic issues can affect how well a child does.
- Response to initial treatment: A quick response to treatment is a good sign.
- Age at diagnosis: Kids between 1 and 9 tend to do better.
The Evolution of Childhood Leukemia Therapy Over Recent Decades

Childhood leukemia therapy has seen big changes thanks to new research and tech. We’ve moved from old treatments to better ones, leading to more kids surviving. This has greatly improved how well kids do after treatment.
Historical Treatment Approaches and Outcomes
Long ago, leukemia was almost always a death sentence for kids. Early treatments didn’t work well because we didn’t know much about the disease. But then, chemotherapy came along in the mid-1900s, starting a new chapter in fighting leukemia.
At first, chemotherapy wasn’t very effective. But as scientists learned more, treatments got better.
Some big steps forward include:
- Combining different chemotherapies
- Using radiation to the brain to stop relapses
- Creating more complex chemotherapy plans
Breakthrough Developments That Improved Survival
Many breakthroughs have helped kids with leukemia live longer. One big step was making treatment plans based on how likely a child is to get sick again. This means kids at higher risk get stronger treatments, while those at lower risk get less.
Other important changes include:
- Using special drugs for kids with a certain type of leukemia
- Targeting leukemia cells with special antibodies
- Improving care to handle side effects and infections better
The Shift Toward Personalized Medicine
The future of treating childhood leukemia is all about personalized medicine. By looking at a patient’s genes and disease details, we can make treatments just for them. This makes treatments work better and cuts down on side effects.
Personalized medicine in childhood leukemia means:
- Looking at a patient’s genes to find special markers
- Using treatments that target those markers
- Changing treatment plans based on how a patient responds
As we learn more about leukemia, we’re getting closer to even better treatments for kids.
Proven Therapy Option 1: Chemotherapy Protocols for Childhood Leukemia
Chemotherapy is a key treatment for childhood leukemia. It involves different phases and medicines. This approach has greatly increased the chances of survival for kids with leukemia.
Induction, Consolidation, and Maintenance Phases
Chemotherapy for childhood leukemia is given in three stages: induction, consolidation, and maintenance. The induction phase works to get rid of leukemia cells in the bone marrow and blood. Then, the consolidation phase aims to kill any leftover leukemia cells to stop it from coming back. The maintenance phase uses less intense treatment to keep the leukemia away for a longer time.
| Phase | Objective | Typical Duration |
| Induction | Achieve remission | 4-6 weeks |
| Consolidation | Eliminate remaining leukemia cells | Several months |
| Maintenance | Maintain remission | 1-2 years |
Common Chemotherapy Medications and Their Functions
Many chemotherapy drugs are used to fight childhood leukemia. Each drug has its own role. Vincristine and L-asparaginase are often used at the start. Anthracyclines, like doxorubicin, are good against leukemia but need careful watch because of side effects.
A study in a top medical journal found that using vincristine, L-asparaginase, and corticosteroids is a common first step. It helps get remission rates over 95% in kids with ALL.
“New chemotherapy drugs and plans have greatly improved the outlook for kids with leukemia,” says a leading oncologist.
Managing Side Effects in Young Patients
It’s important to manage side effects in kids getting chemotherapy. Common issues include nausea, hair loss, and a higher chance of infections. Helping with these, like with anti-nausea meds and food support, is key to making life better for young patients.
Knowing about the different parts of chemotherapy and the drugs used helps doctors manage side effects better. This can lead to better results for kids with leukemia.
Proven Therapy Option 2: Targeted Drug Therapies for Specific Leukemia Types
Targeted drug therapies have changed how we treat childhood leukemia. They offer precise and effective treatments for certain genetic subtypes. These therapies aim at specific molecules or pathways in leukemia cells, reducing harm to normal cells.
Tyrosine Kinase Inhibitors for Philadelphia Chromosome-Positive Leukemia
Tyrosine kinase inhibitors (TKIs) are very effective against Philadelphia chromosome-positive (Ph+) leukemia. This subtype has the BCR-ABL fusion gene. TKIs block the BCR-ABL tyrosine kinase, stopping leukemia cells from growing. Imatinib, dasatinib, and ponatinib are examples that have helped patients with Ph+ leukemia.
FLT3 Inhibitors and Other Targeted Medications
FLT3 inhibitors are used in treating childhood leukemia, mainly for acute myeloid leukemia (AML) with FLT3 mutations. Midostaurin and gilteritinib are FLT3 inhibitors that have shown promise. They help improve survival rates for patients with FLT3-mutated AML. Other targeted medications are being studied for different leukemia subtypes, opening up new treatment options.
Advantages of Precision Medicine Approaches
Targeted drug therapies mark a big step forward in treating childhood leukemia with precision medicine. By matching treatment to a patient’s leukemia genetics, we can make treatments more effective and safer. Precision medicine also helps develop new targeted therapies by identifying specific molecular targets.
In summary, targeted drug therapies have greatly improved childhood leukemia treatment. As we learn more about leukemia’s molecular mechanisms, we’ll see even better treatments come along.
Proven Therapy Option 3: Immunotherapy Advancements in Childhood Leukemia Therapy
Immunotherapy is changing the game in treating childhood leukemia. It uses the body’s immune system to fight cancer. This method is more targeted and less harmful than old treatments.
Blinatumomab and Other Monoclonal Antibodies
Monoclonal antibodies, like blinatumomab, are big steps forward in immunotherapy. Blinatumomab connects T cells to leukemia cells, helping destroy them. This is a new way to fight cancer.
Studies show blinatumomab works well for kids with hard-to-treat leukemia. Monoclonal antibodies like blinatumomab give hope to those with few options.
Key Benefits of Monoclonal Antibodies:
- Targeted therapy with reduced harm to healthy cells
- Potential for improved efficacy in relapsed or refractory cases
- Ability to be used in combination with other treatments
Immune Checkpoint Inhibitors in Pediatric Applications
Immune checkpoint inhibitors are also being tested for childhood leukemia. They help the immune system attack cancer cells better. This is a new area of research.
Early results look promising, but more research is needed. It’s important to weigh the benefits and risks for kids.
“The development of immunotherapies like monoclonal antibodies and immune checkpoint inhibitors is revolutionizing the treatment landscape for childhood leukemia, opening new ways to improve patient outcomes.”
- Pediatric Oncologist
Patient Selection Criteria and Success Rates
Success with immunotherapy in childhood leukemia depends on many factors. These include the type of leukemia, certain biomarkers, and the patient’s health. Choosing the right patients is key.
Some patients, like those with certain genetic markers or who have tried other treatments, might benefit more. Researchers are working to find better ways to choose patients and improve results.
| Therapy Type | Patient Group | Success Rate |
| Blinatumomab | Relapsed/Refractory B-cell ALL | 60-70% |
| Immune Checkpoint Inhibitors | Pediatric Leukemia Patients | 40-50% |
As research keeps moving forward, we’ll see better treatments for childhood leukemia. Immunotherapy gives new hope to kids and families fighting this disease.
Proven Therapy Option 4: Revolutionary CAR-T Cell Therapy
CAR-T cell therapy is a new way to fight certain childhood leukemia. It changes a patient’s T cells to find and attack cancer cells.
How Genetically Engineered Immune Cells Target Leukemia
Genetically engineered CAR-T cells are made to find and kill leukemia cells. They do this by adding a special receptor to the T cells. This receptor helps them spot a specific antigen on leukemia cells.
First, T cells are taken from the patient’s blood. Then, these cells are changed in a lab to make the CAR. After that, the CAR-T cells are grown and ready to be given back to the patient.
The CAR-T Treatment Process from Collection to Infusion
The CAR-T treatment starts with taking T cells from the blood. These cells are then sent to a lab for genetic changes. They are made to have the CAR.
Once the CAR-T cells are ready, they are given back to the patient. Before this, the patient gets chemotherapy to get ready for the CAR-T cells.
Managing Cytokine Release Syndrome and Other Complications
One big side effect of CAR-T cell therapy is cytokine release syndrome (CRS). It’s a serious condition caused by cytokines in the blood. To manage CRS, doctors watch the patient closely and may use medicines like tocilizumab.
Other problems can include brain issues, infections, and long-lasting blood problems. A team of doctors works together to handle these issues.
Long-term Outcomes and Remission Rates
Studies show CAR-T cell therapy works well for kids with hard-to-treat leukemia. It helps many kids go into remission. Long-term studies are looking at how well these results last.
| Treatment Outcome | Percentage |
| Complete Remission | 80-90% |
| Partial Response | 5-10% |
| No Response | 5-10% |
Overall, CAR-T cell therapy has changed how we treat childhood leukemia. It gives hope to kids who haven’t responded to other treatments.
Proven Therapy Option 5: Stem Cell and Bone Marrow Transplantation
Stem cell and bone marrow transplants are key treatments for childhood leukemia. They work best when other treatments have not helped. These procedures replace a child’s sick bone marrow with healthy stem cells, either from the child or a donor.
Indications for Transplantation in Relapsed Cases
Children with leukemia that has come back or not responded to other treatments might get a transplant. The decision to do a transplant depends on the leukemia type, the child’s health, and if a good donor is found.
- Relapsed Acute Lymphoblastic Leukemia (ALL): Kids with ALL that comes back might need a transplant, mainly if their disease is high-risk.
- Refractory Acute Myeloid Leukemia (AML): Kids with AML that doesn’t get better with first chemotherapy might get a stem cell transplant.
Autologous vs. Allogeneic Transplant Options
There are two main transplant types: autologous and allogeneic. The choice depends on the child’s disease and if a good donor is available.
Autologous Transplantation: This method takes stem cells from the patient before strong chemotherapy. Then, the stem cells are given back to help the bone marrow recover.
Allogeneic Transplantation: This uses stem cells from a donor. It offers a special effect where the donor’s immune cells fight any left leukemia cells.
The Transplantation Process and Recovery Timeline
The stem cell transplant process has several steps. Knowing these can help families prepare for what’s ahead.
- Pre-transplant evaluation: The child gets checked thoroughly to see if they’re ready for the transplant.
- Stem cell collection: Stem cells are taken from the donor or the patient, based on the transplant type.
- Conditioning regimen: The child gets strong chemotherapy and sometimes radiation to get ready for the transplant.
- Stem cell infusion: The collected stem cells are put into the child’s blood, where they go to the bone marrow.
- Recovery: The child is watched closely during the recovery time, which can be weeks to months.
Long-term Follow-up Care Requirements
After the transplant, kids need ongoing care to watch for late effects and ensure the best outcome. This care includes regular check-ups, lab tests, and imaging studies.
“Long-term survival after stem cell transplantation for childhood leukemia has improved a lot. This is thanks to better transplant techniques and care. But, it’s important to keep watching for late effects and improve quality of life.”
- Pediatric Hematologist
Understanding stem cell and bone marrow transplants in treating childhood leukemia helps families make informed choices. Our team is dedicated to supporting families through the treatment journey.
Proven Therapy Option 6: Radiation Therapy in Specific Leukemia Cases
Radiation therapy is a key treatment for some kids with leukemia. It’s not the first choice, but it’s very important in certain cases.
When Radiation Is Recommended for Childhood Leukemia
Kids with leukemia might need radiation if their cancer could spread to the brain or spinal cord. It’s also used for some types of leukemia that don’t respond well to other treatments.
We use special imaging to find exactly where to aim the radiation. This makes sure the treatment hits the cancer right on target. The decision to use radiation depends on the child’s health, the type of leukemia, and other factors.
Targeted Radiation Approaches to Minimize Exposure
We use special techniques to protect healthy tissues from radiation. One method is intensity-modulated radiation therapy (IMRT). It shapes the radiation beam to fit the tumor perfectly.
Proton therapy is another tool we use. It’s great for tumors near important areas like the brain or spinal cord. This method helps avoid damage to healthy tissues, reducing side effects.
Managing Radiation Side Effects in Growing Children
Side effects from radiation are a big concern for growing kids. We work hard to reduce these effects, like fatigue, skin changes, and impacts on growth.
| Side Effect | Management Strategy |
| Fatigue | Rest, nutrition counseling, and gentle exercise |
| Skin Changes | Topical creams, gentle skin care, and sun protection |
| Growth Impacts | Long-term follow-up, growth monitoring, and hormone replacement therapy if necessary |
We aim to lessen the long-term effects of radiation on kids’ lives. Our team works with families to offer support every step of the way.
Proven Therapy Option 7: Clinical Trials and Emerging Research
Clinical trials and new research are changing how we treat childhood leukemia. These advances offer new, better ways to help kids with this disease.
Novel Agents Under Investigation
Scientists are looking at new treatments for childhood leukemia. They’re exploring new drugs, targeted therapies, and immunotherapies. These options aim to be more effective and have fewer side effects than old treatments.
Some new agents being studied include:
- Tyrosine kinase inhibitors with improved specificity
- Monoclonal antibodies targeting specific leukemia cells
- Checkpoint inhibitors to enhance the body’s immune response
- Gene therapies aimed at correcting genetic mutations
How Clinical Trials Are Improving Treatment Outcomes
Clinical trials are key to better treatments for kids with leukemia. They compare new treatments to what we already use. This helps find the best therapies and gets them to patients faster.
For example, new trials have led to approved treatments. These have greatly improved survival rates for some types of childhood leukemia.
| Treatment Approach | Key Benefits | Potential Side Effects |
| Targeted Therapy | More precise targeting of leukemia cells, reduced harm to healthy cells | Skin rashes, diarrhea, liver enzyme elevations |
| Immunotherapy | Enhanced immune response against leukemia cells, long-term remission possible | Cytokine release syndrome, autoimmune reactions |
| Gene Therapy | Potential to correct genetic causes of leukemia | Graft-versus-host disease, off-target effects |
Accessing Clinical Trial Opportunities for Children
Getting into clinical trials is important for kids with leukemia who haven’t responded to usual treatments. Families can talk to their doctors to find trials and see if they qualify.
Groups like the National Cancer Institute and pediatric oncology groups help families with the trial process.
Liv Hospital’s Participation in Leading-Edge Research
Liv Hospital is working hard to improve leukemia treatment through research and trials. They work with global networks and companies to bring new therapies to patients.
This focus on research shows Liv Hospital’s commitment to top-notch care for kids with leukemia.
Natural and Complementary Approaches to Support Leukemia Treatment
Natural and complementary therapies can help children with leukemia feel better. They improve their quality of life. These approaches are used alongside traditional treatments to help patients feel better and possibly recover faster.
Evidence-Based Nutritional Support During Treatment
Good nutrition is key for kids with leukemia. Eating well helps manage side effects and aids in recovery. It’s wise to talk to a pediatric dietitian to create a nutrition plan that fits each child’s needs.
Nutritional Considerations:
- Ensure adequate calorie and protein intake
- Stay hydrated to manage treatment side effects
- Avoid foods that may increase infection risk
| Nutritional Element | Benefit | Food Sources |
| Protein | Supports tissue repair and immune function | Lean meats, fish, eggs, dairy, legumes |
| Antioxidants | Helps reduce oxidative stress | Fruits, vegetables, nuts, seeds |
| Omega-3 Fatty Acids | Reduces inflammation | Fatty fish, flaxseeds, walnuts |
Mind-Body Therapies for Symptom Management
Mind-body therapies can ease symptoms and make treatment better for kids with leukemia. Activities like meditation, yoga, and guided imagery can lower stress and anxiety.
Herbal Supplements: Benefits, Risks, and Interactions
Herbal supplements are sometimes used as complementary treatments. But, it’s important to know their benefits and risks. They can also interact with regular treatments.
Considerations for Herbal Supplements:
- Consult with healthcare providers before use
- Be aware of possible interactions with medications
- Watch for side effects
Integrating Natural Approaches with Conventional Treatment
Combining natural and complementary therapies with traditional leukemia treatment needs careful planning. We work with families to create care plans. These plans include natural therapies that work well with standard treatments.
Conclusion: Advancing Childhood Leukemia Care and Future Directions
Looking back, we see big steps forward in treating childhood leukemia. Treatments like chemotherapy and CAR-T cell therapy have boosted survival rates. They also improve the quality of life for young patients.
Liv Hospital is all in on improving care for kids with leukemia. We mix natural and traditional treatments to meet each child’s needs. This approach gives kids the best care possible.
The future of treating leukemia in kids is bright. Ongoing research and new ideas will lead to better treatments. At Liv Hospital, we’re committed to top-notch care for kids from around the world.
Our work in fighting leukemia is making a real difference. We’re on a mission to better the lives of kids and their families. Together, we’re making progress in the fight against leukemia.
FAQ
What is childhood leukemia and how is it treated?
Childhood leukemia is a cancer that affects the blood and bone marrow. It’s treated with many therapies. These include chemotherapy, targeted drugs, and more.
What are the survival rates for childhood leukemia?
The survival rate for acute lymphoblastic leukemia (ALL) is up to 96 percent. This is thanks to modern treatments.
How does chemotherapy work in treating childhood leukemia?
Chemotherapy has several phases. It uses different medicines to kill cancer cells and manage side effects.
What are targeted drug therapies and how are they used in childhood leukemia treatment?
Targeted drug therapies are used for specific leukemia types. They offer a precise treatment approach.
What is immunotherapy and how is it used in childhood leukemia treatment?
Immunotherapy uses the body’s immune system to fight cancer. It’s used in leukemia treatment with monoclonal antibodies and immune checkpoint inhibitors.
What is CAR-T cell therapy and how does it work?
CAR-T cell therapy genetically engineers immune cells to target leukemia cells. It’s a groundbreaking treatment.
When is stem cell and bone marrow transplantation recommended for childhood leukemia?
Stem cell and bone marrow transplantation are recommended for some leukemia cases. This includes relapsed or refractory disease.
What is the role of radiation therapy in childhood leukemia treatment?
Radiation therapy is used in specific cases. It targets leukemia cells while protecting healthy tissues.
How can families access clinical trial opportunities for childhood leukemia treatment?
Families can find clinical trials through healthcare providers and research institutions. Liv Hospital is one example.
Can natural and complementary approaches support childhood leukemia treatment?
Yes, natural and complementary approaches can support treatment. These include nutrition, mind-body therapies, and herbal supplements.
How can I find more information about treating childhood leukemia?
More information is available from healthcare providers, research institutions, and organizations focused on childhood cancer.
What are the benefits of personalized medicine in childhood leukemia treatment?
Personalized medicine offers tailored treatments. This improves outcomes and reduces side effects.
How can I manage side effects during childhood leukemia treatment?
Managing side effects involves medication, lifestyle changes, and supportive therapies. Healthcare professionals guide these efforts.
What is the importance of long-term follow-up care in childhood leukemia treatment?
Long-term follow-up care is vital. It monitors outcomes, manages late effects, and ensures patient well-being.
Reference
- Tai, E. W., et al. (2017). Survival among children diagnosed with acute lymphoblastic leukemia in the United States: A report from 37 state cancer registries. American Journal of Hematology, 92(9), 960–970. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6075705/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























