
Thumb arthritis affects millions globally, causing pain and limiting hand use. It’s a common form of osteoarthritis, making everyday tasks hard like gripping and twisting. Caring for your cmc joint is essential for hand function. Discover amazing and powerful ways to keep your cmc joint healthy and pain-free.
At our institution, we know how thumb arthritis affects daily life. Our skilled doctors offer tailored thumb joint replacement to ease pain and improve hand movement. We’ll look at CMC joint surgery options, their benefits, and what to expect.
Knowing about surgical choices helps patients make better decisions. We aim to provide top-notch healthcare and support for patients from around the world.
Key Takeaways
- Thumb arthritis is a common condition that can significantly impact daily life.
- Customized thumb joint replacement solutions are available to alleviate pain and restore mobility.
- Experienced physicians work with patients to determine the best course of treatment.
- CMC joint surgery options are designed to improve hand function and quality of life.
- Our institution is dedicated to providing extensive support for international patients.
Understanding Thumb Anatomy and the CMC Joint
To understand thumb joint replacement, knowing the thumb’s anatomy is key. The thumb has bones, joints, and soft tissues. These work together for motion and function.
The Structure of Thumb Bones and Joints
The thumb has three bones: the proximal phalanx, distal phalanx, and metacarpal bone. These bones are linked by three joints. The CMC joint, at the thumb’s base, is a saddle-shaped joint for opposition.
The thumb’s unique shape lets it grasp, pinch, and manipulate objects. Knowing its bones and joints is vital for diagnosing and treating thumb issues.
The Importance of the Carpometacarpal (CMC) Joint
The CMC joint is key for thumb function, enabling opposition and circumduction. It’s prone to osteoarthritis from high stresses. Its saddle shape allows for wide motion while keeping things stable.
The CMC joint’s role is huge. Problems here can greatly affect hand function and life quality.
How the Trapezium Bone Functions
The trapezium bone is small and irregular, part of the CMC joint. It’s vital for thumb function, providing a stable base for the metacarpal bone. It articulates with the metacarpal to enable smooth movement and opposition.
The trapezium’s unique shape and position support the thumb’s complex movements. It’s a key part of thumb anatomy.
Common Causes of Thumb Joint Pain
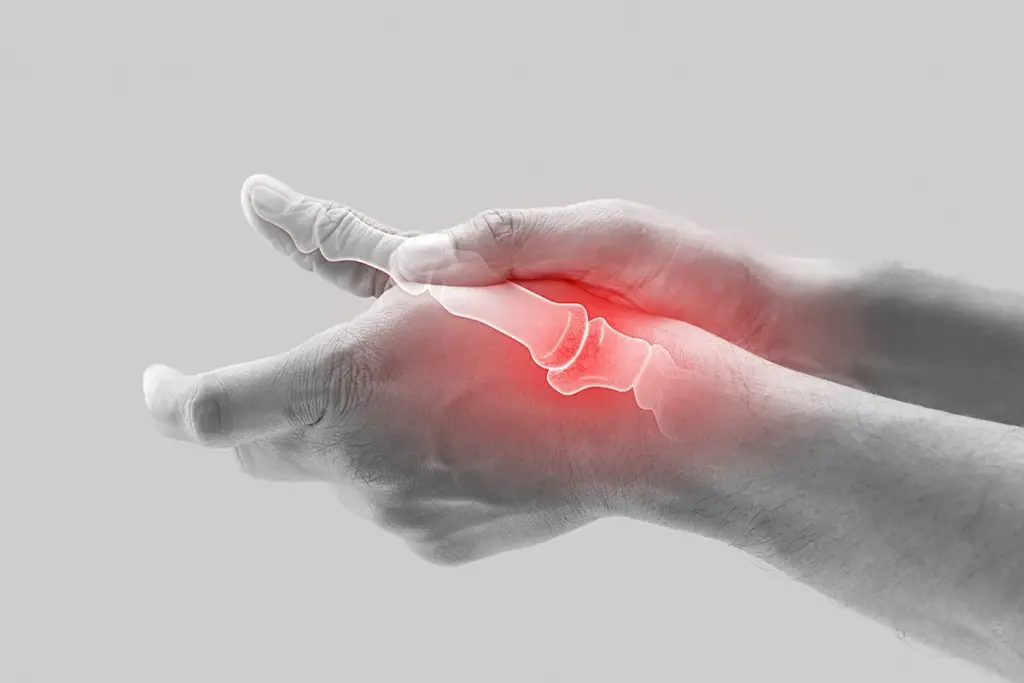
Pain in the thumb joint can really affect your daily life. Knowing why it happens is key. The carpometacarpal (CMC) joint at the thumb’s base is often hit by different issues that cause pain.
Osteoarthritis at the Base of the Thumb
Osteoarthritis is a disease that wears down the CMC joint. It happens when the cartilage that protects the joints wears out. This leads to bone rubbing against bone, causing pain. Symptoms include pain, swelling, and weaker grip. As it gets worse, it can make it hard to use your hand.
Rheumatoid Arthritis Effects on the Thumb
Rheumatoid arthritis (RA) is an autoimmune disease that can hit any joint, like the CMC joint of the thumb. In RA, the immune system attacks the joint lining, causing inflammation and pain. Symptoms include pain, stiffness, and swelling, and can affect both hands.
Traumatic Injuries to the Thumb Joint
Traumatic injuries, like fractures or sprains, can also cause thumb pain. These injuries might happen from falls, sports accidents, or other incidents. They can cause severe pain, swelling, and bruising. If not treated right, they can lead to long-term pain and arthritis.
|
Condition |
Common Symptoms |
Potential Long-term Effects |
|---|---|---|
|
Osteoarthritis |
Pain, swelling, reduced grip strength |
Impaired hand function, chronic pain |
|
Rheumatoid Arthritis |
Pain, stiffness, swelling |
Joint damage, deformity |
|
Traumatic Injuries |
Severe pain, swelling, bruising |
Chronic pain, arthritis |
Knowing why your thumb joint hurts is the first step to feeling better. Whether it’s osteoarthritis, rheumatoid arthritis, or an injury, each needs a special plan to ease symptoms and improve function.
Diagnosing Problems in the CMC Joint
Diagnosing CMC joint problems involves several steps. We use physical exams, imaging studies, and tests for thumb arthritis. Accurate diagnosis is key for effective treatment. Our process aims to clearly understand your thumb joint health.
Physical Examination Techniques
A thorough physical exam is the first step. We check the thumb’s range of motion, strength, and stability. We also look for swelling, tenderness, or deformity.
Specific tests, like the grind test, are used. This test checks for pain and crepitus, signs of joint degeneration. It helps us understand the joint’s condition and guides further steps.
Imaging Studies for Thumb Joint Assessment
Imaging studies are key for confirming the diagnosis and assessing the severity of CMC joint arthritis. X-rays are used to check the joint space, bone spurs, and any deformity. Sometimes, we recommend MRI for soft tissue assessment.
These studies give us valuable information about the joint’s condition. They help us determine the best treatment plan for you. By knowing the extent of joint degeneration, we can tailor our recommendations.
Thumb Arthritis Tests and Evaluations
We conduct specific tests for thumb arthritis, in addition to physical exams and imaging studies. These tests include assessing opposition and pinch strength, and evaluating hand function. We also use questionnaires to understand how thumb pain affects your daily life.
By combining the results of these tests, we gain a full understanding of your CMC joint health. This allows us to create a personalized treatment plan that meets your unique needs and goals.
Non-Surgical Treatment Options for Thumb Arthritis
Before surgery, people with thumb arthritis can try non-surgical treatments. These methods aim to lessen pain, improve function, and boost life quality.
Activity Modification and Rest
Managing thumb arthritis starts with changing how you do things. This means doing tasks differently or resting your hands often.
Making small changes, like using ergonomic tools or holding things differently, can help a lot. Avoiding repetitive actions and heavy lifting can also ease symptoms.
Splinting and Bracing Options
Splints are a common non-surgical treatment for thumb arthritis. They can be custom-made or bought off the shelf. Wearing a splint can support the thumb and lessen pain.
There are many types of splints, some letting you move your thumb a bit. The right splint depends on how bad the arthritis is and what you need.
Medications for Pain and Inflammation
Several medicines can help with thumb arthritis symptoms. Over-the-counter pain relievers like acetaminophen or ibuprofen can help with pain and swelling.
Doctors might prescribe stronger medicines or suggest corticosteroid shots for severe swelling.
|
Treatment Option |
Description |
Benefits |
|---|---|---|
|
Activity Modification |
Changing daily activities to reduce strain on the thumb |
Reduces pain, improves function |
|
Splinting |
Using splints to immobilize and support the thumb |
Provides support, reduces pain |
|
Medications |
Using pain relievers and anti-inflammatory drugs |
Reduces pain and inflammation |
Non-surgical treatments offer many ways to manage thumb arthritis. By using these methods together, people can often find a lot of relief.
“The key to managing thumb arthritis is a multi-faceted approach that includes lifestyle changes, supportive devices, and medication.”
CMC Joint Injections: Procedure and Effectiveness
CMC joint injections are a key treatment for thumb arthritis. They aim to lessen pain and swelling, and help move the joint better. We’ll look at the types of injections, how they’re done, and how well they work.
Corticosteroid Injections
Corticosteroid injections are a common choice for thumb arthritis. They help by cutting down inflammation and swelling in the CMC joint. These shots mix a corticosteroid with a local anesthetic.
Benefits: They offer quick pain relief, reduce swelling, and improve joint movement.
Potential Risks: You might feel temporary pain at the injection site. Skin thinning and weakening of tendons and ligaments can happen with repeated use.
Hyaluronic Acid Treatments
Hyaluronic acid injections add to the joint’s natural lubricant. This can help reduce pain and swelling.
Procedure: You’ll get a series of shots over several weeks.
Effectiveness: They can greatly reduce pain and improve joint function. But, results can vary.
Platelet-Rich Plasma (PRP) Therapy
PRP therapy uses platelet-rich plasma from your own blood. It’s injected into the CMC joint to help heal and reduce inflammation.
Benefits: It uses your body’s healing powers, which might offer longer-lasting relief.
Procedure: It starts with a blood draw, then processing to concentrate platelets. The platelet-rich plasma is then injected into the joint.
|
Treatment |
Procedure |
Effectiveness |
|---|---|---|
|
Corticosteroid Injections |
Single injection, potentially repeated |
Quick pain relief, reduced inflammation |
|
Hyaluronic AcidTreatments |
Series of injections over several weeks |
Significant pain relief, improved joint function |
|
PRP Therapy |
Blood draw, processing, and injection |
Longer-term relief through natural healing processes |
In conclusion, CMC joint injections provide several options for treating thumb arthritis. Each has its own benefits and risks. Knowing about these treatments helps patients make better choices for their care.
Thumb Joint Exercises for Pain Relief and Mobility
Experiencing thumb joint pain? A good exercise plan can change your life. These exercises strengthen the muscles around the CMC joint. They also improve flexibility and thumb function.
Strengthening Exercises for Thumb Stability
Strengthening your thumb is key to better stability and less pain. Here are some exercises we suggest:
- Thumb Opposition: Touch the tip of your thumb to the tip of each finger on the same hand. Do this 10-15 times.
- Thumb Flexion: Hold a light weight (less than 1 pound) in your hand with your palm facing upwards. Bend your thumb towards your palm and then straighten it. Repeat 10-15 times.
Range of Motion Exercises
These exercises keep your thumb joint flexible. Try these:
- Thumb Circles: Move your thumb in a circular motion, first clockwise and then counterclockwise. Do 5-10 times in each direction.
- Thumb Extension: Gently pull your thumb away from your other fingers to stretch it. Hold for a few seconds and release. Repeat 10-15 times.
Hand Therapy Techniques
Hand therapy can help with recovery and pain management. Here are some effective methods:
|
Therapy Technique |
Description |
Frequency |
|---|---|---|
|
Thumb Splinting |
Using a splint to immobilize the thumb and reduce strain |
As recommended by a healthcare professional |
|
Heat or Cold Therapy |
Applying heat or cold packs to reduce pain and inflammation |
2-3 times a day |
|
Massage Therapy |
Gentle massage to improve blood flow and reduce stiffness |
Daily, as tolerated |
Adding these exercises and hand therapy to your daily routine can help. You might see less pain, better mobility, and improved thumb function.
When to Consider Surgical Intervention
If thumb joint pain doesn’t get better with non-surgical treatments, surgery might be needed. This choice is made after checking the patient’s condition and how well previous treatments worked.
Failed Conservative Treatment Indicators
Some signs show that non-surgical treatments aren’t working anymore. These include ongoing pain, less thumb movement, and weaker thumb strength. If these problems keep happening even with non-surgical methods, surgery might be the next step.
|
Indicator |
Description |
|---|---|
|
Persistent Pain |
Continuous pain despite medication and therapy |
|
Limited Mobility |
Reduced range of motion in the thumb |
|
Decreased Strength |
Weakness in the thumb, affecting grip and pinch |
Quality of Life Considerations
Thumb joint pain’s effect on daily life is a big reason for choosing surgery. Simple tasks like getting dressed or cooking can become hard. Surgery aims to fix these problems and make life better.
“The goal of thumb joint surgery is not just to alleviate pain but to restore function and improve the patient’s overall quality of life.” –
Orthopedic Specialist
Choosing surgery can help patients do things they couldn’t before. It brings back independence and lets them enjoy activities again.
Types of Thumb Joint Replacement Procedures
Understanding the different thumb joint replacement surgeries is key. This surgery is for those with severe thumb arthritis who haven’t found relief with other treatments.
Total Joint Replacement Options
Total joint replacement means replacing the whole carpometacarpal (CMC) joint with artificial parts. It’s often chosen for those with advanced osteoarthritis or rheumatoid arthritis in the thumb joint.
Benefits of Total Joint Replacement:
- Significant pain reduction
- Improved thumb mobility
- Enhanced grip strength
Partial Joint Replacement Techniques
Partial joint replacement only fixes the damaged part of the CMC joint. This method keeps more of the patient’s natural bone. It might feel more natural after surgery.
|
Procedure |
Description |
Benefits |
|---|---|---|
|
Total Joint Replacement |
Replaces the entire CMC joint |
Significant pain relief, improved mobility |
|
Partial Joint Replacement |
Replaces only the damaged portion |
Preserves natural bone, potentially more natural feel |
Synthetic vs. Biological Implants
Choosing between synthetic and biological implants is important in thumb joint replacement. Synthetic implants are made from materials like metal or plastic. Biological implants come from natural tissues.
Synthetic implants are durable and can last long but may wear out faster. Biological implants, like tendon or ligament tissue, offer a natural option but success varies.
The right choice depends on the patient’s joint damage, health, and personal preferences. It’s a decision based on individual needs.
Trapeziectomy: An Alternative to Joint Replacement
The trapeziectomy procedure is getting more attention as a joint replacement alternative. It involves removing the trapezium bone at the thumb’s base. This is mainly for those with thumb CMC joint arthritis.
Surgical Procedure Explained
In a trapeziectomy, the surgeon takes out the trapezium bone. This bone is part of the wrist’s CMC joint with the thumb’s first metacarpal bone. The surgery is done under regional anesthesia, keeping the patient comfortable.
The surgeon makes an incision at the thumb’s base to reach the CMC joint. After removing the trapezium, they might use a tendon piece to keep the thumb in place. This helps prevent it from shortening.
Recovery and Outcomes
After trapeziectomy, the thumb is immobilized for a while. Then, physical therapy helps regain strength and mobility. Patients often see less pain and better thumb function, but recovery times vary.
Research shows trapeziectomy can greatly reduce pain and improve thumb function for CMC joint arthritis patients. But, results can vary based on the patient’s health and other hand conditions.
Comparing Trapeziectomy to Joint Replacement
Patients with CMC joint arthritis often compare trapeziectomy and joint replacement. Joint replacement substitutes the damaged joint with an artificial one. Trapeziectomy, on the other hand, removes the problematic trapezium bone.
|
Procedure |
Trapeziectomy |
Joint Replacement |
|---|---|---|
|
Bone Removal |
Trapezium bone removed |
Damaged joint surfaces replaced |
|
Implant Use |
No implant or tendon interposition |
Artificial joint implant used |
|
Recovery Time |
Variable, often longer rehabilitation |
Generally shorter recovery, but depends on implant |
|
Pain Relief |
Significant pain reduction reported |
Effective pain relief, but risk of implant failure |
The choice between trapeziectomy and joint replacement depends on the patient’s condition and lifestyle. It’s important to talk to a hand surgeon to decide the best option.
Modern Approaches to CMC Arthroplasty
Modern surgery for CMC arthroplasty is changing how we treat thumb pain. The carpometacarpal (CMC) joint of the thumb often gets arthritis. This leads to a lot of pain and makes it hard to move. New surgical methods are now giving patients better results.
Ligament Reconstruction and Tendon Interposition (LRTI)
LRTI is a common surgery for CMC arthritis. It removes the arthritic trapezium bone and rebuilds the ligament. This makes the thumb stable. The tendon helps cushion the joint, easing pain and improving movement.
Research shows LRTI greatly reduces pain and boosts thumb function in those with CMC arthritis. It’s very helpful for those with severe arthritis who haven’t found relief with other treatments.
Suspension Arthroplasty Methods
Suspension arthroplasty is another way to treat CMC arthritis. It suspends the thumb metacarpal from the surrounding bones. This keeps the space open after the trapezium bone is removed. The method can use tendons or synthetic grafts.
|
Surgical Technique |
Benefits |
Complications |
|---|---|---|
|
LRTI |
Significant pain relief, improved thumb function |
Potential for tendon irritation |
|
Suspension Arthroplasty |
Maintains thumb metacarpal space, reduces pain |
Risk of graft failure or loosening |
Innovative Techniques in CMC Joint Reconstruction
New methods in CMC joint reconstruction are emerging. They include advanced biomaterials, less invasive surgeries, and custom implants made with 3D printing.
As technology and research grow, so will the improvements in CMC arthroplasty. Our team is dedicated to keeping up with these advancements. We aim to give our patients the best care possible.
Preparing for Thumb Joint Surgery
Thumb joint surgery needs careful preparation for a smooth recovery. We’ll guide you through the key steps before your surgery.
Pre-operative Assessments
A thorough pre-operative assessment is key before surgery. It helps us spot any risks and make sure you’re ready. The assessment includes:
- A detailed medical history to check for any conditions that might affect your surgery or recovery.
- A physical examination to look at your thumb and overall health.
- Imaging studies, like X-rays or an MRI, to see your thumb joint clearly.
It’s important to follow your healthcare provider’s instructions on pre-operative testing and preparation.
Medication Management
Managing your medications before surgery is vital. Some drugs can increase bleeding risk or interact with anesthesia. We suggest:
- Telling your healthcare provider about all medications you’re taking, including over-the-counter drugs and supplements.
- Following specific instructions on which medications to stop or continue before surgery.
- Talking about alternative pain management options if your current medications might interfere with surgery.
Always talk to your healthcare provider before changing your medication regimen.
Setting Realistic Expectations
Setting realistic expectations is key for a good outcome. Knowing what to expect can help you prepare mentally and physically. We recommend:
- Talking to your healthcare provider about your expectations to make sure they match what’s possible.
- Understanding the recovery timeline and what to expect during rehabilitation.
- Planning for post-operative care, including arranging for someone to help you during the initial recovery period.
“The key to a successful surgery is not just the procedure itself, but the preparation and care that surrounds it.” –
A renowned orthopedic surgeon
By preparing well for thumb joint surgery, you can greatly improve your chances of a successful outcome and a smooth recovery. Always follow your healthcare provider’s advice and ask any questions you have.
The Thumb Joint Replacement Surgery Process
Understanding thumb joint replacement surgery is key for those considering it. This complex process includes anesthesia, the surgical technique, and post-operative care.
Anesthesia Options
Anesthesia is vital for comfort during thumb joint replacement surgery. We offer two main options: local anesthesia with sedation or general anesthesia. The choice depends on the patient’s health, the procedure’s complexity, and personal preference.
Local anesthesia with sedation numbs the area and keeps the patient relaxed. It’s often chosen for its quicker recovery and lower risks compared to general anesthesia.
General anesthesia makes the patient unconscious during surgery. It’s used for more complex cases or those with significant anxiety.
Step-by-Step Surgical Procedure
The surgery involves several precise steps:
- Making an incision at the base of the thumb to access the CMC joint.
- Removing the damaged or arthritic joint surfaces.
- Preparing the joint for the implant by reshaping the bone.
- Inserting the chosen implant, which can be made of metal, plastic, or other biocompatible materials.
- Closing the incision with sutures or staples.
|
Surgical Step |
Description |
Importance |
|---|---|---|
|
Incision |
Making an incision to access the CMC joint |
Allows for direct access to the damaged joint |
|
Joint Preparation |
Removing damaged joint surfaces and preparing for the implant |
Ensures a smooth surface for the implant |
|
Implant Insertion |
Placing the chosen implant |
Restores joint function and alleviates pain |
Immediate Post-Operative Care
After surgery, we focus on immediate post-operative care. This includes:
- Monitoring the patient’s pain levels and administering appropriate pain management.
- Applying a bandage or splint to protect the thumb and support the healing process.
- Providing instructions on wound care and follow-up appointments.
By managing the post-operative period carefully, we can reduce complications and help patients recover faster.
Recovery Timeline After Thumb Joint Surgery
Knowing the recovery timeline after thumb joint surgery is key. It helps manage expectations and get the best results. The journey includes immediate care, several stages of healing, and long-term rehab.
The First Few Weeks
The first weeks are critical. Patients are told to keep their hand up to lessen swelling and pain. They also need to follow their doctor’s pain and infection prevention advice.
Key activities during the first few weeks include:
- Gentle exercises to keep fingers moving
- Wearing a splint or cast to protect the thumb
- Watching for signs of infection or complications
Rehabilitation and Physical Therapy
As healing moves forward, rehab and physical therapy take center stage. This phase is vital for regaining strength and improving thumb movement. We tailor therapy plans to meet each patient’s needs and goals.
The rehabilitation process typically includes:
- Exercises to boost thumb flexibility
- Strengthening exercises for better grip and pinch
- Activities to enhance daily living skills
|
Rehabilitation Phase |
Typical Duration |
Key Activities |
|---|---|---|
|
Initial Healing |
2-4 weeks |
Pain management, swelling reduction, gentle exercises |
|
Rehabilitation |
6-12 weeks |
Range of motion exercises, strengthening, functional activities |
|
Advanced Strengthening |
3-6 months |
Progressive strengthening, high-level functional activities |
Long-term Recovery Expectations
Recovery from thumb joint surgery can take months. Patients will see thumb function improve and pain lessen over time. It’s important to stick to the rehab plan and keep up with follow-up appointments.
Long-term expectations include:
- Improved thumb function and strength
- Reduced pain and discomfort
- Enhanced ability to perform daily activities
By understanding the recovery timeline and actively participating in rehab, patients can get the best results from thumb joint surgery.
Advancements in Thumb Joint Replacement Technology
The field of thumb joint replacement is seeing big changes, thanks to new technologies. These advancements make the surgery more precise, safe, and effective.
3D-Printed Implants
3D-printed implants are a big deal in thumb joint replacement. They are made to fit each patient perfectly, which could lead to better results and fewer problems. 3D printing lets us create complex shapes that old methods can’t.
Minimally Invasive Techniques
Minimally invasive surgical techniques are also getting better. These methods use smaller cuts, cause less damage, and might let patients recover faster. Doctors are working hard to make these techniques even better, aiming to reduce pain and improve the patient’s experience.
Future Directions in CMC Joint Treatment
Researchers are looking into new materials and technologies for thumb joint replacement. They’re exploring stronger implant materials, using stem cells to help healing, and adding tech to track recovery. These advancements will likely lead to even better results for patients.
As we keep exploring new ways to improve thumb joint replacement, the future looks bright. With ongoing research and tech advancements, we’re moving towards treatments that are more tailored, effective, and less invasive.
Cost and Insurance Considerations for Thumb Joint Procedures
When looking into thumb joint procedures, it’s key to understand the costs and insurance. The money side of these surgeries can be tricky. Many factors affect how much you’ll pay.
Average Costs in the United States
The price of thumb joint replacement surgery in the U.S. changes a lot. This depends on the surgery type, the doctor’s fees, and where it’s done.
|
Procedure Type |
Average Cost |
Range |
|---|---|---|
|
Total Joint Replacement |
$15,000 |
$10,000 – $20,000 |
|
Partial Joint Replacement |
$12,000 |
$8,000 – $18,000 |
|
Trapeziectomy |
$10,000 |
$6,000 – $15,000 |
These prices are just estimates. They can change based on your situation. Always talk to your doctor and insurance to get a better idea of what you’ll pay.
Insurance Coverage for Joint Replacement
Insurance for thumb joint replacement surgery differs by provider and policy. Most plans help pay for necessary surgeries.
- Check your insurance before surgery
- Know your out-of-pocket costs, like deductibles and copays
- See if there are any special rules for coverage
It’s important to work with your insurance to know what they cover. This way, you can understand any costs you might have to pay yourself.
Financial Assistance Options
If money is tight, there are ways to get help. You might find financing plans, patient aid programs, or non-profit groups that help with medical costs.
Financial Assistance Resources:
- Patient advocacy groups
- Non-profit groups that offer financial help
- Healthcare financing companies
Looking into these options can help with the cost of thumb joint replacement surgery.
Conclusion: Making an Informed Decision About Thumb Joint Treatment
Understanding the carpometacarpal (CMC) joint is key when choosing thumb joint treatment. We’ve looked at the thumb’s anatomy, common pain causes, and treatment methods. These include non-surgical options and surgeries like joint replacement and trapeziectomy.
It’s important to think about the pros and cons of each treatment. Consider your needs and health. Talking to a healthcare professional can help find the best treatment for you.
Knowing your options well is the first step to treating your thumb joint. We hope this guide helps you move forward in addressing your concerns.
FAQ
What is thumb joint replacement surgery?
Thumb joint replacement surgery is a procedure to fix the damaged or arthritic joint at the base of the thumb. It uses an artificial joint or implant to replace the old one.
What are the symptoms of thumb arthritis?
Thumb arthritis symptoms include pain, stiffness, and swelling at the base of the thumb. You might also find it hard to grip or grasp things.
How is thumb arthritis diagnosed?
Doctors diagnose thumb arthritis by examining you, reviewing your medical history, and using X-rays or MRI. These tests help see how the joint and tissues are doing.
What are the non-surgical treatments for thumb arthritis?
Non-surgical treatments include changing your activities, using splints, and taking pain and inflammation medicines. You might also get injections like corticosteroids or hyaluronic acid.
What is trapeziectomy, and how does it differ from joint replacement?
Trapeziectomy is a surgery that removes the trapezium bone in the CMC joint. It’s different from joint replacement because it doesn’t use an artificial joint. Instead, it lets the body heal naturally.
What is the recovery time for thumb joint surgery?
Recovery time for thumb joint surgery varies. Generally, it takes several weeks to a few months of physical therapy and rehabilitation.
Are there any exercises that can help alleviate thumb joint pain?
Yes, exercises like strengthening and range of motion can help with thumb joint pain. Hand therapy techniques also improve mobility.
How much does thumb joint replacement surgery cost?
Thumb joint replacement surgery costs vary. Factors like location, surgeon’s fees, and insurance coverage affect the price. In the U.S., costs can be quite different.
Is thumb joint replacement surgery covered by insurance?
Many insurance plans cover thumb joint replacement surgery. But, coverage can vary. It’s important to check with your insurance before surgery.
What are the advancements in thumb joint replacement technology?
New advancements include 3D-printed implants and minimally invasive techniques. These aim to improve results and reduce recovery time.
Can I undergo thumb joint surgery if I have other health conditions?
Deciding on thumb joint surgery with other health conditions depends on your specific situation. A healthcare provider will need to evaluate you thoroughly.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC11634552/



































