
Deciding to have a colonoscopy at a young age is complex. It depends on many risk factors. Even though guidelines suggest starting at 45, some people might need to start earlier.
Early detection of colorectal cancer screening is key. If you’re thinking about a colonoscopy at 35, talk to your doctor. Share your health history and risk factors.
Key Takeaways
- The recommended age for colorectal cancer screening is 45 for average-risk individuals.
- Individual risk factors may necessitate earlier screening.
- A colonoscopy is a vital tool for early detection and prevention.
- Discussing personal health history with a healthcare provider is essential.
- Screening guidelines may evolve with new evidence.
Understanding Colonoscopy and Its Importance
Colonoscopy is more than a test; it’s a way to stop colorectal cancer before it starts. With colon cancer on the rise in young people, knowing about colonoscopy is key.
What is a colonoscopy?
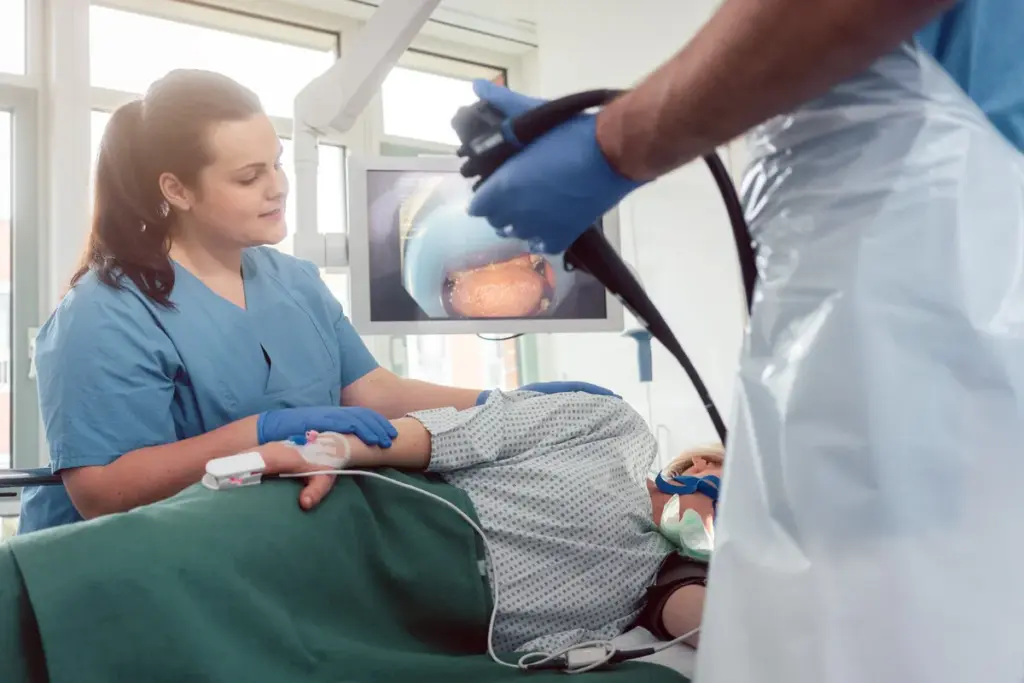
A colonoscopy lets doctors see inside the colon and rectum for polyps, cancer, and other issues. A flexible tube with a camera and light is used. The doctor can see images on a monitor.
“The American Cancer Society recommends starting regular screening at age 45 for most adults,” their guidelines say. But, those with a higher risk, like a family history of colorectal cancer, might need to start earlier.
Why colonoscopies are essential for cancer detection
Colonoscopy is the best way to find colorectal cancer early and remove precancerous polyps. This makes it a key tool for prevention. It can stop cancer from happening by removing polyps before they turn into cancer.
The role of colonoscopy in finding cancer is huge. Early detection leads to better survival rates. Catching cancer early makes a big difference in treatment success.
The preventive power of colonoscopies
Colonoscopy is great for preventing cancer. It finds and removes polyps that could turn into cancer. This is very important, as we see more colon cancer in young people. Starting colonoscopy at 35 might be needed for those at higher risk.
As we deal with more colon cancer in young people, colonoscopy’s role is more important than ever. It’s a powerful tool for early detection and prevention.
Standard Age Guidelines for Colonoscopy Screening
Health organizations have set guidelines for when to start colonoscopy screening. These guidelines help both patients and doctors make the right choices.
American Cancer Society Recommendations
The American Cancer Society (ACS) has clear guidelines for colorectal cancer screening. They say adults with average risk should start screening at age 45. This is because early detection can greatly improve outcomes.
“The American Cancer Society recommends that adults with an average risk of colorectal cancer start regular screening at age 45.”
American Cancer Society
USPSTF Guidelines
The U.S. Preventive Services Task Force (USPSTF) also has guidelines for colorectal cancer screening. They advise adults aged 45 to 75 to get screened. For those 76 to 85, the decision to screen depends on individual factors.
|
Age Group |
USPSTF Recommendation |
|---|---|
|
45-75 |
Screening recommended |
|
76-85 |
Screening decision based on individual factors |
|
>85 |
Screening not recommended |
Evolution of Screening Age Recommendations
Before, the age to start screening was 50. But, with more cases of early-onset colorectal cancer, guidelines have changed. Now, starting at 45 is recommended due to the disease’s rise in younger people.
As we watch trends in colorectal cancer, guidelines might change again. It’s important for both doctors and patients to stay updated.
The Rising Concern: Colorectal Cancer in Young Adults
Recent studies show a worrying trend: colon cancer is rising in young people. This change challenges the old idea that colorectal cancer mainly hits older adults. It’s a big shift in how we see this disease, with big implications for how we screen and prevent it.
Statistical Trends in Early-Onset Colorectal Cancer
The numbers for early-onset colorectal cancer are scary. Studies say the number of cases under 50 is going up. This isn’t just in the U.S.; it’s happening worldwide.
|
Year |
Incidence Rate Under 50 |
Incidence Rate 50 and Older |
|---|---|---|
|
2000 |
4.8 per 100,000 |
54.4 per 100,000 |
|
2010 |
5.2 per 100,000 |
53.9 per 100,000 |
|
2020 |
6.5 per 100,000 |
52.1 per 100,000 |
The 2% Annual Increase in Under-50 Diagnoses
There’s been a 2% annual increase in colorectal cancer in those under 50. This steady rise is alarming. It highlights the need for new screening guidelines and more awareness.
Many factors contribute to this rise, like lifestyle and diet changes, and environmental factors. Younger patients often have more advanced cancer because they get diagnosed later.
Why Younger Patients Often Present with Advanced Disease
Younger patients often have advanced cancer because their symptoms are not quickly linked to cancer. This delay in diagnosis can be due to several reasons:
- Lack of awareness about colorectal cancer among young adults
- Symptoms being attributed to other common conditions
- Absence of screening in younger populations
Understanding these factors is key to promoting early detection and better outcomes for younger patients.
Risk Factors That Warrant Early Screening at 35
Some people might need to get a colonoscopy early because of certain risks. Knowing these risks helps figure out if a colonoscopy at 35 is needed.
Family History Considerations
A big family history of colon cancer is a key risk factor. If a close relative, like a parent or sibling, got colon cancer young, your risk goes up. Research shows people with family history tend to get colon cancer sooner.
A study in the Journal of Clinical Oncology found a link. Those with family history of colon cancer face higher risk, more so if it happened before 50.
Hereditary Syndromes like Lynch Syndrome
Hereditary syndromes, like Lynch syndrome, raise colon cancer risk a lot. Lynch syndrome is a genetic disorder that increases cancer risk, including colon cancer. People with Lynch syndrome face a high risk of colon cancer, often at a young age.
“Lynch syndrome causes about 3% of all colon cancers. Those with Lynch syndrome have a 70-80% chance of getting colon cancer in their lifetime.”
Personal History of Inflammatory Bowel Disease
Having inflammatory bowel disease (IBD) like ulcerative colitis or Crohn’s disease ups colon cancer risk. IBD’s ongoing inflammation can cause colon cell mutations, leading to cancer.
Here’s a table on IBD and its risks:
|
Condition |
Risk Factor |
Screening Recommendation |
|---|---|---|
|
Ulcerative Colitis |
Increased risk after 8-10 years of disease |
Regular surveillance colonoscopies |
|
Crohn’s Disease |
Increased risk, more with colonic involvement |
Regular surveillance colonoscopies |
Lifestyle Factors Increasing Risk
Lifestyle choices also affect colon cancer risk. Eating too much processed meat and not enough fiber, not exercising, being overweight, and smoking all increase risk. Changing these habits can lower colon cancer risk.
- Eat more fiber and less processed meat
- Do at least 30 minutes of moderate exercise daily
- Stay at a healthy weight with balanced diet and exercise
- Quit smoking to lower cancer risk
Understanding and tackling these risk factors helps people decide on early screening, maybe at 35.
Genetic Predisposition and Lynch Syndrome
Lynch syndrome is a hereditary condition that raises the risk of colorectal cancer. Early screening is key. We’ll look at Lynch syndrome’s impact, genetic testing’s role, and screening for those who test positive.
Understanding Lynch Syndrome and Genetic Testing
Lynch syndrome is an inherited condition that ups the risk of cancers, like colorectal cancer. Genetic testing can spot mutations linked to Lynch syndrome. This leads to early action.
Those with a family history of colorectal cancer or other Lynch syndrome cancers should get tested. Testing can show if they have a mutation that raises their cancer risk.
Screening Recommendations for Mutation Carriers
Carriers of Lynch syndrome mutations should start colonoscopy between 30-35 years old. Regular checks are key for catching colorectal cancer early.
The table below shows screening advice for Lynch syndrome carriers:
|
Age to Start Screening |
Screening Method |
Frequency |
|---|---|---|
|
30-35 years |
Colonoscopy |
Every 1-2 years |
Research on Advanced Neoplasia Rates by Age 35
Research shows Lynch syndrome carriers face a higher risk of advanced neoplasia at a younger age. By 35, many carriers might already have advanced neoplasia.
This knowledge highlights the need for early and frequent screening. We suggest Lynch syndrome carriers work with their doctors to create a tailored screening plan.
Symptoms That Shouldn’t Be Ignored at Any Age
It’s important to know the signs of colorectal problems early. Regular screenings help prevent issues. But, some symptoms need immediate attention.
Rectal Bleeding and Its Significance
Seeing blood in your stool is a big warning sign. It can look like bright red blood or dark, tarry stools. Rectal bleeding is not normal and should never be ignored. It might be due to something simple like hemorrhoids, but it could also mean something serious like cancer.
“The presence of blood in the stool is always considered abnormal until proven.” This shows how serious it is to see blood and get it checked out.
Changes in Bowel Habits
Changes in how often you go or what your stool looks like can be a sign of trouble. If your bowel habits change a lot and don’t go back to normal, see a doctor.
- Diarrhea or constipation that lasts
- Stools that are very thin
- Feeling like you didn’t finish going
Persistent Abdominal Pain or Discomfort
Stomach pain that doesn’t go away needs to be checked out. This includes cramps, gas, or feeling too full. These symptoms can mean many things, but if they’re bad or last a long time, you should get it checked.
|
Symptom |
Possible Indication |
|---|---|
|
Rectal Bleeding |
Colorectal cancer, hemorrhoids, or other gastrointestinal issues |
|
Changes in Bowel Habits |
Irritable bowel syndrome, colorectal cancer, or other bowel disorders |
|
Abdominal Pain |
Inflammatory bowel disease, colorectal cancer, or other abdominal conditions |
Unexplained Weight Loss
Weight loss without trying to lose it is a warning sign. It can mean many things, including cancer. If you’re losing weight and don’t know why, see a doctor.
“Unexplained weight loss, with other symptoms, needs a full medical check-up.”
— Medical Expert
Knowing these symptoms and talking to your doctor can help find problems early. If you’re experiencing any of these, don’t wait to get help.
Colon Cancer Survival Rate: How Early Detection Impacts Outcomes
Colon cancer survival rates change a lot based on when it’s found. Finding it early makes it much easier to treat. This greatly improves how well patients do.
Stage-specific Survival Statistics
The survival rate for colon cancer depends a lot on when it’s found. For those caught early (Stage I), the five-year survival rate is about 90%. But for those found later (Stage IV), it’s only around 14%.
Here are the survival rates for each stage:
- Stage I: About 92% five-year survival rate
- Stage II: Approximately 63-87% five-year survival rate, depending on the substage
- Stage III: Around 40-53% five-year survival rate, varying by substage
- Stage IV: About 14% five-year survival rate
The Survival Advantage of Early Detection
Finding colon cancer early makes a big difference. Screening tests can spot polyps that might become cancer. This means treatments work better, leading to better results.
Early detection is very important. It not only helps patients live longer but also means they might not need as harsh treatments. This makes life better for them.
Age-related Differences in Prognosis
Age affects how well someone does with colon cancer. Younger people usually do better because they have fewer health problems. But, colon cancer is becoming more common in younger people too. So, it’s key to screen everyone, no matter their age.
Knowing how age affects prognosis helps doctors give better care. They can tailor screenings and treatments to fit each patient’s needs.
The Process of Requesting an Early Colonoscopy
Requesting an early colonoscopy involves several steps. These steps help make the process smoother. Taking charge of your health can feel empowering yet daunting, like when talking to your doctor.
Initiating the Conversation with Your Primary Care Physician
Talking to your primary care doctor is the first step. Be ready to share your health history and any symptoms. Write down your concerns and questions before your visit.
- Discuss your family’s health history, including any cancer.
- Share any symptoms you’re feeling, like changes in bowel habits.
- Ask for your doctor’s advice based on your risk factors.
Documenting Your Risk Factors
It’s important to document your risk factors. This includes your family’s health history and any past health issues. Keeping a detailed record helps your doctor understand your risk.
- Collect information about your family’s health, focusing on colorectal cancer.
- Document any personal health issues, like polyps or inflammatory bowel disease.
- Record any symptoms or health changes that might be important.
Navigating Insurance Challenges
Insurance can be a challenge when asking for an early colonoscopy. Many plans cover colonoscopies for those over 45, but younger people may face different rules. It’s key to know your insurance’s policy on early screenings. Call your insurance to find out about coverage and costs.
- Check your insurance plan for details on preventive and diagnostic services.
- Ask what you need to show to get an early colonoscopy.
- Know the difference between a diagnostic and preventive colonoscopy, as this can affect coverage.
Being informed and prepared helps you through the early colonoscopy request process. Taking proactive steps for your health is a positive move. Many doctors support patients who are proactive about their health.
Insurance Coverage for Early Screening
Getting insurance to cover early colonoscopy screenings is key to preventive care. Knowing how insurance handles these tests can make things easier for you.
How Insurance Typically Covers Colonoscopies
Most insurance plans do cover colonoscopies, but how much can change. Usually, they cover tests for people over 45. But, those under 45 might need to meet certain risk criteria.
Key factors influencing coverage include:
- Age and risk factors
- Family history of colorectal cancer
- Previous history of colon polyps or cancer
- Presence of symptoms
Diagnostic vs. Preventive Procedure Coding
How a colonoscopy is coded can affect your insurance. Preventive colonoscopies are often free for those at average risk, starting at 45, thanks to the Affordable Care Act.
But, if it’s coded as diagnostic because of symptoms or risk, you might face costs. Knowing the coding can help you prepare for expenses.
Appealing Insurance Denials
If your insurance denies a colonoscopy claim, you can appeal. The appeal process usually involves:
- Reviewing the denial reason
- Gathering supporting documentation from your healthcare provider
- Submitting a formal appeal to your insurance provider
Tips for a successful appeal:
- Clearly state the reason for your appeal
- Include any relevant medical records or letters from your doctor
- Follow up with your insurance provider to ensure your appeal is processed
Patient Assistance Programs
For those struggling to afford colonoscopy screenings, patient assistance programs can help. These programs offer financial aid, free or low-cost screenings, and help with insurance issues.
Examples of patient assistance programs include:
- Manufacturer-sponsored programs for diagnostic tests
- Non-profit organizations providing financial help for cancer screenings
- Hospital or healthcare system-based programs for low-income patients
Alternative Screening Options for Those Under 45
Colonoscopy is the top choice, but other tests are good for some under 45. These options are less invasive and fit based on risk and what the patient wants.
Stool-Based Tests
Stool tests like FIT, gFOBT, and stool DNA tests are non-invasive. They check for blood, hemoglobin, or cancer genes in the stool.
FIT is done yearly and is more accurate than gFOBT. Stool DNA tests, like Cologuard, add DNA analysis to FIT for a better look.
CT Colonography (Virtual Colonoscopy)
CT colonography uses CT scans to see the colon. It needs bowel prep like colonoscopy but is less invasive.
It spots polyps and cancers but misses small ones. If it finds something big, a colonoscopy is needed to confirm.
Flexible Sigmoidoscopy
Flexible sigmoidoscopy uses a camera tube in the rectum to check the sigmoid colon and rectum. It needs less prep than colonoscopy and can be done without sedation.
When Alternatives Are Appropriate vs. When a Full Colonoscopy Is Necessary
Choosing between tests depends on risk, medical history, and what the patient prefers. For average-risk people, stool tests or CT colonography might work. But for those at higher risk or showing symptoms, colonoscopy is best. It can see the whole colon and remove polyps.
Talking to a healthcare provider is key to finding the right screening method.
Preparing for Your Colonoscopy: What to Expect
To make your colonoscopy go well, it’s important to know the prep process. Getting ready right is key for good results and safety.
The Bowel Preparation Process
Bowel prep, or “bowel prep,” makes sure your colon is clean. This lets the doctor see everything clearly during the test. You’ll likely change your diet, take laxatives, or use enemas to clean out your colon.
Bowel Prep Options:
- Laxative solutions that you drink, which help flush out the colon.
- Prescription medications that induce bowel movements.
- Enemas, which are inserted into the rectum to clean out the lower part of the colon.
It’s key to follow your doctor’s prep instructions closely. The prep method can change based on your health, the procedure’s timing, and other factors.
Dietary Restrictions Before the Procedure
You’ll need to change your diet before your colonoscopy. You’ll likely eat a low-fiber diet or only clear liquids a day or two before.
|
Food Type |
Recommended |
Not Recommended |
|---|---|---|
|
Liquids |
Clear broths, water, clear juices |
Milk, cream, colored or cloudy liquids |
|
Foods |
Plain toast, plain crackers, gelatin |
Fruits, vegetables, nuts, seeds |
Sticking to these diet changes is important for a good prep and a successful colonoscopy.
Medication Considerations
Talk to your doctor about your medications before the colonoscopy. Some meds, like blood thinners, might need to be stopped or changed to avoid bleeding risks.
“It’s vital to tell your doctor about all meds you’re taking, including over-the-counter drugs and supplements, for your safety during the procedure.” – Gastroenterology Expert
The Day of the Procedure
On the day of your colonoscopy, arrive on time with someone to drive you home. You might be sleepy from sedation. Wear comfy clothes and leave jewelry and valuables at home.
Being well-prepared makes the process easier.
Recovery and Follow-up After a Colonoscopy
The time after a colonoscopy is just as important as the procedure itself. It needs careful attention to recovery and follow-up. We’ll guide you through this phase to ensure a smooth and comfortable experience.
Immediate Post-Procedure Care
After your colonoscopy, you’ll go to a recovery area. Medical staff will watch over you for a bit. You might feel groggy from the sedation.
It’s important to have someone drive you home. You won’t be able to drive yourself.
Key aspects of immediate post-procedure care include:
- Resting for the remainder of the day
- Avoiding heavy lifting or strenuous activities
- Following any specific instructions provided by your healthcare provider
Potential Side Effects and Complications
Colonoscopies are generally safe but can have side effects or complications. Common side effects are bloating, gas, or mild abdominal cramps. These usually go away in a few hours.
Serious complications, though rare, can happen. These include severe abdominal pain, rectal bleeding, or fever. If you have these symptoms, call your healthcare provider right away.
Understanding Your Results
Your healthcare provider will talk to you about your colonoscopy results. If polyps were removed, they’ll tell you about the type and number.
Understanding your results is key for your care. Your provider will plan your next steps based on the findings. This might include another colonoscopy.
Follow-up Recommendations Based on Findings
The timing of your next colonoscopy depends on your results. For example:
- No polyps or small, benign polyps might mean no colonoscopy for 10 years.
- Several or large polyps could mean a follow-up in 3 to 5 years.
Your healthcare provider will give you personalized advice. They’ll consider your health, family history, and colonoscopy findings.
The Psychological Impact of Early Screening
Early screening through colonoscopy is key for health but can affect our minds. When we think about getting this test younger, we must face the emotional side. This ensures a better experience.
Managing Anxiety About the Procedure
Many feel anxious about colonoscopies. This worry comes from the test itself, what it might find, or the prep needed. To ease this, people can:
- Learn about the test to clear up false beliefs.
- Talk to their doctor to know what to expect.
- Try relaxation methods like deep breathing or meditation.
By being proactive, we can lessen our anxiety. This makes the test less scary.
Coping with Possible Findings
Waiting for test results can be stressful. It doesn’t matter if the news is good, bad, or unclear. Having support is key. This includes:
- Family and friends for emotional support.
- Support groups to share experiences.
- Professional counseling for emotional help.
Knowing you’re not alone and help is out there helps a lot. It makes dealing with the results easier.
The Relief of Negative Results
Getting negative results is a big relief. It means you’re healthy and less worried about colon cancer. But it’s also a chance to:
- Talk to your doctor about future tests.
- Learn about lifestyle changes for better health.
- Remember to keep up with health checks.
A negative result is not just a relief. It also shows the value of keeping up with health checks.
|
Psychological Aspect |
Management Strategy |
Benefit |
|---|---|---|
|
Anxiety About Procedure |
Education and Relaxation Techniques |
Reduced Anxiety |
|
Coping with Findings |
Support Systems and Counseling |
Emotional Support |
|
Relief of Negative Results |
Future Screening and Lifestyle Changes |
Continued Health Vigilance |
Patient Stories: Young Adults Who Benefited from Early Screening
Young adults are now getting the benefits of early colonoscopy screenings. Their stories show how important it is to catch health issues early. They also highlight the need for more awareness about colorectal cancer among the young.
Case Studies of Early Detection Success
A 32-year-old with a family history of colorectal cancer got a colonoscopy. It found a tumor early on. Thanks to this, the patient got the right treatment and now spreads the word about colorectal cancer awareness.
A 28-year-old with ongoing stomach issues got a colonoscopy because of family history. It found a polyp that could have turned into cancer. This shows how early screening can prevent big problems.
These stories show how early screening is key in catching and stopping colorectal cancer in young adults.
Lessons Learned from Delayed Diagnoses
A 35-year-old who ignored symptoms for months was diagnosed with advanced cancer. This teaches us the risks of waiting too long. It’s vital to see a doctor right away if something feels off, even if you’re young.
These stories stress the need for more awareness about colorectal cancer. They also highlight the benefits of early screening, mainly for young people.
The emotional and physical effects of delayed diagnosis show why we need to take care of our health early on.
Advocacy Efforts by Young Survivors
Young survivors of colorectal cancer are making a big difference. They share their stories to stress the importance of early detection. They use social media, support groups, and events to spread the word.
They get support from groups focused on colorectal cancer research and support. These groups help them share their stories and experiences.
Together, they are making a big difference in promoting early detection and saving lives.
Talking to Your Doctor: Questions to Ask About Early Colonoscopy
To make an informed decision about early colonoscopy, patients should prepare a list of questions to ask their doctor. This conversation is key to understanding your personal risk factors and the benefits and risks of the procedure.
Assessing Your Personal Risk Level
Knowing your risk level is important to decide if an early colonoscopy is needed. Ask your doctor about your risk factors, such as family history, personal medical history, and lifestyle.
- Do I have a family history of colorectal cancer?
- Have I been diagnosed with any conditions that increase my risk, such as Lynch syndrome or inflammatory bowel disease?
- Are there any lifestyle changes I can make to reduce my risk?
Discussing Benefits vs. Risks
Every medical procedure has benefits and risks. When talking to your doctor about early colonoscopy, it’s important to understand both sides.
Benefits: Early detection of colorectal cancer, removal of precancerous polyps, and potentially improved survival rates.
Risks: Complications from the procedure, such as bleeding or perforation, and the possibility of unnecessary anxiety or procedures if abnormalities are found.
Exploring All Available Options
Colonoscopy is not the only screening method. Your doctor can explain other options, like stool-based tests or CT colonography.
- What are the alternative screening methods available to me?
- How do these alternatives compare to colonoscopy in terms of accuracy and convenience?
Creating a Long-term Screening Plan
Creating a long-term screening plan is vital, regardless of your decision on early colonoscopy. Your doctor can help you find the best schedule based on your risk factors and previous screening results.
Key questions to ask:
- What is the recommended screening schedule for my risk level?
- How will my screening plan change if I have a history of polyps or colorectal cancer?
- Are there any new screening technologies or methods that I should be aware of?
Conclusion: Making an Informed Decision About Early Colonoscopy Screening
Colorectal cancer is becoming more common in younger people. This makes it key to think about early colonoscopy screening. Knowing your risk factors, like family history and lifestyle, helps you talk to your doctor about screening.
FAQ
What is the recommended age for a colonoscopy?
Health groups say to start colonoscopy screening at 45. But, if you’re at high risk, you might need to go earlier.
Is colon cancer curable if detected early?
Yes, catching colon cancer early can make it very curable. The chances of survival greatly improve if caught early.
Why is colon cancer rising in young people?
Young adults are seeing more colon cancer, with a 2% yearly increase. Lifestyle and genetics are thought to play a role.
What are the symptoms of colon cancer in men?
Look out for rectal bleeding, changes in bowel habits, and persistent pain. Unexplained weight loss is also a sign. If you notice these, see your doctor.
What is the survival rate for stage 4 colon cancer?
Stage 4 colon cancer survival rates depend on age and health. Early detection is key because later stages have lower survival rates.
Can I request a colonoscopy at 35?
Yes, you can ask for a colonoscopy at 35 if you’re at risk or have symptoms. Talk to your doctor about your situation.
What are the alternative screening options for colon cancer?
Options include stool tests, CT colonography, and flexible sigmoidoscopy. But, a full colonoscopy is often needed for a thorough check.
How do I prepare for a colonoscopy?
Preparing involves a bowel prep, diet changes, and possibly adjusting meds. Your doctor will explain what to do.
What should I expect after a colonoscopy?
You’ll need to follow care instructions and watch for side effects. Your doctor will talk about the results and what comes next.
How does insurance cover colonoscopies?
Insurance rules for colonoscopies can vary. Knowing your plan and appealing denials can help get coverage for screenings.
What is Lynch syndrome, and how does it affect colon cancer risk?
Lynch syndrome increases the risk of colorectal cancer. People with it should start screening early, often at 20-25 or 2-5 years before family history suggests.
References
- U.S. Preventive Services Task Force. (n.d.). Colorectal cancer: Screening. Retrieved from https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/colorectal-cancer-screening USPSTF


































