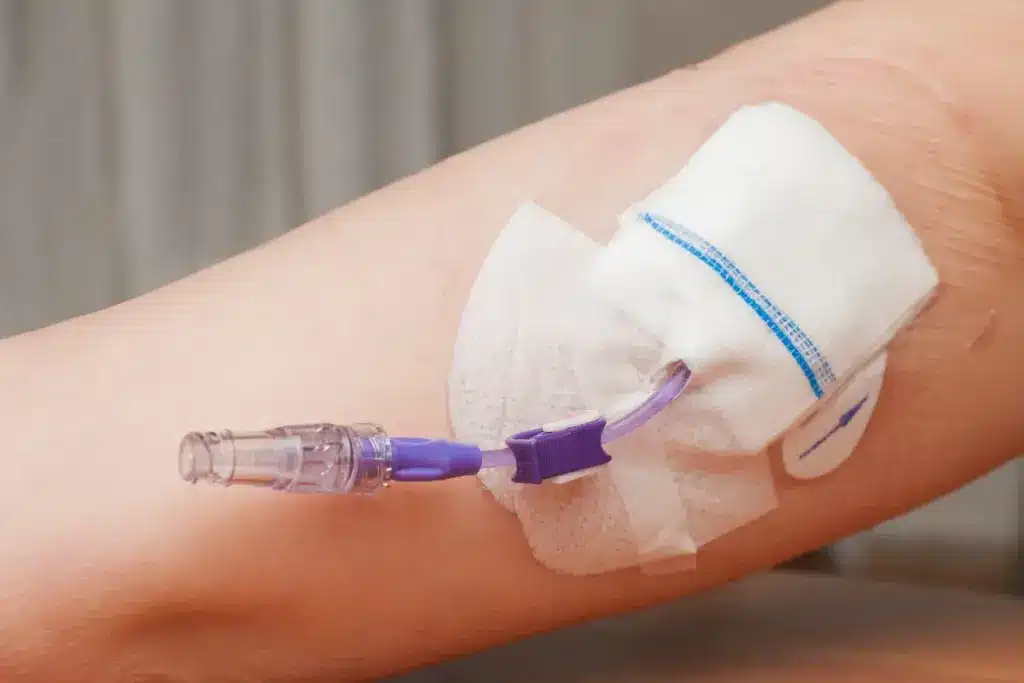
Complete Do You Need A Catheter After A PAE (Catheter After PAE)? Prostate Artery Embolization (PAE) is a treatment that has shown promise in easing urinary issues by shrinking the prostate. A key part of this treatment is whether or not a catheter is needed during or after it.
Men looking into PAE for prostate problems need to know about catheters. Using a catheter is a common part of PAE. It’s important to understand why and when a catheter might be used during this procedure.
Key Takeaways
- PAE is a procedure aimed at reducing prostate size to alleviate urinary tract symptoms.
- The use of a catheter may be required during or following PAE.
- Understanding the need for catheterization is vital for patients considering PAE.
Understanding Prostate Artery Embolization (PAE)
Prostate Artery Embolization (PAE) is a new treatment for Benign Prostatic Hyperplasia (BPH). It has become popular in recent years. This method is less invasive than traditional surgeries for BPH symptoms.
What is PAE and how does it work?

PAE blocks the blood flow to the prostate gland. This makes the gland shrink, easing BPH symptoms. An interventional radiologist uses a catheter to inject embolic agents into the prostate arteries. They do this under imaging to be precise and safe.
Common indications for PAE
PAE helps men with moderate to severe BPH symptoms. Symptoms include frequent urination, urgency, weak flow, and waking up to urinate. It’s for those who haven’t improved with medicine or want to avoid surgery risks.
A healthcare provider will decide if PAE is right for you. They look at symptom severity, prostate size, and your health.
The Role of Catheters in Urological Procedures
Urinary catheters are key in urology, helping with many urinary issues. They are vital for those who can’t urinate by themselves because of health problems.
Types of Urinary Catheters
There are many types of urinary catheters. Each is made for different needs and urinary problems.
Foley Catheters
Foley catheters stay in the bladder for a while. They are used for ongoing urine drainage, common in hospitals and care homes.
Intermittent Catheters
Intermittent catheters are for short-term bladder drainage. They are put in when needed and taken out after use. This lowers risks from long-term catheters.
External Catheters
External catheters, or condom catheters, are worn outside the penis. They are good for men who can urinate but have incontinence issues.
General Purposes of Catheter Use
Catheters serve many purposes in urology. They help with urinary retention, incontinence, and tracking urine in sick patients. The right catheter depends on the patient’s needs and health.
Key purposes of catheter use include:
- Managing urinary retention by providing a means to drain urine from the bladder.
- Addressing incontinence issues, especially in patients who are unable to control their urination.
- Monitoring urine output in patients who are critically ill or undergoing surgery.
Understanding different catheters and their uses helps healthcare providers choose the best one for each patient.
Do You Need a Catheter After PAE?
Figuring out if you need a catheter after PAE depends on a few things. It looks at the usual steps and what’s special about you.
Standard Protocol for Catheter Use Post-PAE
Doctors follow different rules for using catheters after PAE. But, most people don’t need one. Yet, some might because of trouble with their urine.
Factors Determining Catheter Necessity
There are a few things that decide if you’ll need a catheter after PAE. These include:
Prostate Size and Urinary Symptoms
If your prostate is big or you have bad urine problems, you might need a catheter.
Pre-existing Urinary Retention
If you had trouble peeing before the procedure, you might need a catheter to help.
Procedural Considerations
The way the PAE was done and what materials were used can also play a part.
|
Factor |
Influence on Catheter Need |
|---|---|
|
Prostate Size |
Larger prostate may increase the need |
|
Pre-existing Urinary Retention |
Higher likelihood of needing a catheter |
|
Procedural Technique |
Variations in technique can affect catheter necessity |
In short, needing a catheter after PAE depends on your situation and the procedure details.
Pre-Procedure Catheter Considerations
Placing a catheter before PAE is key for post-procedure care and outcomes. Some patients might already have a catheter due to urinary issues.
Catheter Placement Before PAE
Deciding on a catheter before PAE depends on several things. This includes how bad the urinary symptoms are and the patient’s health. Some patients need a catheter because of urinary retention, while others might not until after the procedure.
|
Factors Influencing Pre-PAE Catheter Placement |
Description |
|---|---|
|
Severity of Urinary Symptoms |
Patients with severe urinary retention or other urinary issues may require a catheter before PAE. |
|
Overall Health |
Patients with certain health conditions may be more likely to require a catheter before PAE. |
How Pre-Procedure Catheterization Affects Post-Procedure Needs
A catheter before PAE can change what’s needed after the procedure. Research suggests that patients with a catheter before PAE might have different outcomes than those without.
“The presence of a pre-procedure catheter can influence the duration of catheter use after PAE.”
Knowing these factors helps healthcare providers create better treatment plans for each patient.
Post-PAE Catheter Duration
After PAE, how long you need a catheter can vary. It depends on your health, BPH symptoms, and how well you recover. Each person’s situation is different.
Typical Timeframes for Catheter Removal
Most people use a catheter for a few days to a couple of weeks after PAE. The catheter comes out when you can pee easily again. Early removal helps avoid problems.
Factors Affecting Catheter Duration
Several things can change how long you need a catheter. These include:
Severity of BPH Symptoms
If your BPH symptoms are worse, you might need the catheter longer. The severity of symptoms affects how quickly you can pee normally again.
Urinary Flow Improvements
How fast your pee flow gets better also matters. If it improves quickly, you might get to remove the catheter sooner.
Individual Recovery Rates
Everyone recovers at their own pace. Your health and age can affect how long you need the catheter.
Knowing these factors helps both patients and doctors decide about catheters after PAE. It leads to a recovery plan that fits you best.
Managing Urinary Retention After PAE
Managing urinary retention is key for patients after PAE. It’s important for a smooth recovery. Several factors can cause urinary retention after PAE. Knowing these causes helps in managing it effectively.
Causes of post-PAE urinary retention
Urinary retention after PAE can stem from different reasons. These include:
Prostate swelling
Swelling of the prostate gland is a common reason. This swelling can block urine flow, making it hard to urinate.
Bladder dysfunction
Bladder dysfunction is another factor. PAE can sometimes affect bladder function, leading to emptying issues.
Medication effects
Certain medications used during or after PAE can also cause urinary retention. These medications can affect bladder muscles, making it harder to urinate.
Treatment options for urinary retention
Fortunately, there are several treatment options for managing urinary retention after PAE. These include:
- Catheterization: Temporary use of a urinary catheter can help manage urinary retention by allowing the bladder to drain.
- Medications: Certain medications can help alleviate urinary retention by reducing prostate swelling or improving bladder function.
- Pelvic floor physical therapy: This therapy can help strengthen the muscles around the bladder and improve urinary function.
The choice of treatment depends on the underlying cause of urinary retention and the individual patient’s condition. A healthcare provider can determine the most appropriate treatment plan.
|
Cause |
Symptoms |
Treatment |
|---|---|---|
|
Prostate swelling |
Difficulty urinating, weak urine flow |
Medications to reduce swelling |
|
Bladder dysfunction |
Inability to empty bladder, frequent urination |
Pelvic floor physical therapy, catheterization |
|
Medication effects |
Urinary retention, difficulty starting urination |
Adjusting or changing medications |
Potential Complications of Catheter Use After PAE
Catheterization is common after PAE, but it comes with risks. Knowing these risks is key. Catheter use can lead to several complications that affect recovery and comfort.
Common Catheter-Related Complications
Catheter-related complications can range from mild to severe. Here are some common ones:
Urinary Tract Infections
Urinary tract infections (UTIs) are a big risk with catheters. Proper catheter care is vital to lower this risk.
Bladder Spasms
Bladder spasms can happen due to catheter irritation. Medications can help ease these spasms.
Discomfort and Pain
It’s common to feel discomfort or pain with a catheter. Pain management can help reduce this discomfort.
Preventing and Managing Complications
To prevent and manage catheter complications, focus on proper care and watch for infection signs. Also, address any discomfort quickly. Here’s a summary of key strategies:
|
Complication |
Prevention Strategy |
Management |
|---|---|---|
|
Urinary Tract Infections |
Proper catheter hygiene |
Antibiotics |
|
Bladder Spasms |
Catheter securement |
Antispasmodic medications |
|
Discomfort/Pain |
Catheter comfort measures |
Pain relief medications |
By understanding catheter complications after PAE and using prevention and management strategies, patients can have a better recovery.
Catheter Alternatives After PAE
Exploring alternatives to catheters after PAE can help. These options are tailored to each patient’s needs. They can make recovery better and improve urinary health.
Non-invasive management options
Non-invasive options include timed voiding and pelvic floor exercises. These can improve how well you urinate. Medications may also be used to manage urinary issues.
These alternatives are great for those at risk of catheter problems. Or for those who don’t want to use catheters.
When alternatives are appropriate
Choosing alternatives depends on the patient’s situation. This includes how bad their urinary symptoms are and their overall health. Doctors look at these factors to pick the best plan.
This helps balance the good and bad of different treatments. It aims to improve the patient’s life and health.
Patient Experiences with Catheters After PAE
After PAE, patients face challenges with catheter use. These challenges vary based on health, procedure specifics, and post-op care. Each person’s experience is unique.
Common Patient Concerns and Questions
Patients often worry about catheter use after PAE. They ask:
- How long will I need to use a catheter?
- Will I experience discomfort or pain?
- How do I manage daily activities with a catheter?
- What are the signs of possible complications?
Answering these questions early can make a big difference. It helps reduce anxiety and improves the patient’s experience.
Tips for Coping with Temporary Catheterization
Here are some tips to make living with a catheter easier:
Hygiene Practices
Good hygiene is key to avoiding infections. Clean the catheter site regularly. Watch for signs of infection like unusual smells or discharge.
Mobility Considerations
Be careful with your movements to avoid problems. Make sure the catheter is secure to prevent it from coming out.
Psychological Adjustment
Living with a catheter can affect your mind. Stay informed about your situation. Knowing it’s temporary can help manage stress and anxiety.
Understanding catheter use after PAE helps patients recover better. Being prepared makes a big difference.
Discussing Catheter Options with Your Doctor
Talking about catheters with your doctor before PAE is key. It affects your procedure and how you recover. It’s important for you to know and help decide about your catheter needs.
Important Questions to Ask Before Your Procedure
Make sure to ask your doctor these questions:
- Will I need a catheter after PAE?
- How long will I need to use a catheter?
- What are the possible risks or problems with catheters?
- Are there other options instead of catheterization?
These questions help you know what to expect. They also help you make smart choices about your care.
Shared Decision-Making About Catheter Management
Shared decision-making means working together with your doctor. You talk about what you want, your values, and worries. This way, you find the best way to manage your catheter.
By being part of this process, you make sure your needs are met. You also feel okay with the treatment plan chosen for you.
Conclusion
Knowing how catheters work after Prostate Artery Embolization (PAE) is key to good urinary health. Whether or not to use a catheter depends on the patient and the doctor’s advice.
We’ve looked at many parts of using catheters after PAE. This includes what the procedure is, the types of catheters, and possible problems. This information helps patients understand their choices and make smart decisions about their health.
Managing urinary health after PAE needs a plan that fits each person. Working with doctors helps patients deal with the challenges of catheters. This way, they can get the best results.
The main aim of PAE is to improve how well you can urinate and your overall life quality. By knowing how catheters fit into this, patients can better follow their treatment. This leads to the best outcomes.
FAQ
Do I need a catheter after Prostate Artery Embolization (PAE)?
Whether you need a catheter after PAE depends on several things. These include your health, the details of the procedure, and if you have trouble urinating. Talking to your doctor about catheter options before the procedure can help figure out what’s best for you.
What type of catheter is typically used after PAE?
After PAE, different types of catheters might be used. These include Foley catheters, intermittent catheters, and external catheters. The choice depends on your specific needs and what your doctor recommends.
How long do I need to use a catheter after PAE?
How long you’ll need a catheter after PAE varies. It depends on if you have trouble urinating, how well the procedure worked, and how quickly you heal. Usually, catheters are only used temporarily until you can urinate on your own again.
What are the possible complications of catheter use after PAE?
Using a catheter after PAE can lead to a few complications. These include urinary tract infections (UTIs), damage to the urinary tract, and blockages. Taking good care of your catheter and watching for any problems can help avoid or manage these issues.
Are there alternatives to catheter use after PAE?
Yes, there are other ways to manage things after PAE instead of using a catheter. These can include taking medicine or doing pelvic floor exercises. What’s best for you will depend on your situation and what your doctor says.
How can I manage urinary retention after PAE?
Managing urinary retention after PAE might involve using a catheter, taking medicine, or other methods. It’s important to follow your doctor’s advice on how to handle this to avoid discomfort and complications.
What should I discuss with my healthcare provider regarding catheter use before PAE?
Before PAE, it’s important to talk to your doctor about catheters. Discuss the options, possible problems, and what to expect after the procedure. Asking about how long you’ll need a catheter, how to care for it, and what signs of trouble to watch for can help you prepare for recovery.
Can I prevent complications associated with catheter use after PAE?
While you can’t prevent all complications, taking good care of your catheter and watching for signs of trouble can help. Following your doctor’s instructions can also reduce the risk of problems with your catheter after PAE.
How does pre-procedure catheter placement affect post-PAE catheter needs?
Whether you need a catheter before PAE can affect what you need after it. Talking to your doctor about needing a catheter before the procedure can help figure out the best way to manage your urinary function after PAE.
What are the benefits of discussing catheter management with my healthcare provider before PAE?
Talking to your doctor about catheters before PAE helps make decisions together. It sets realistic expectations and prepares you for recovery, including any catheter use or other management strategies.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9394104/



































