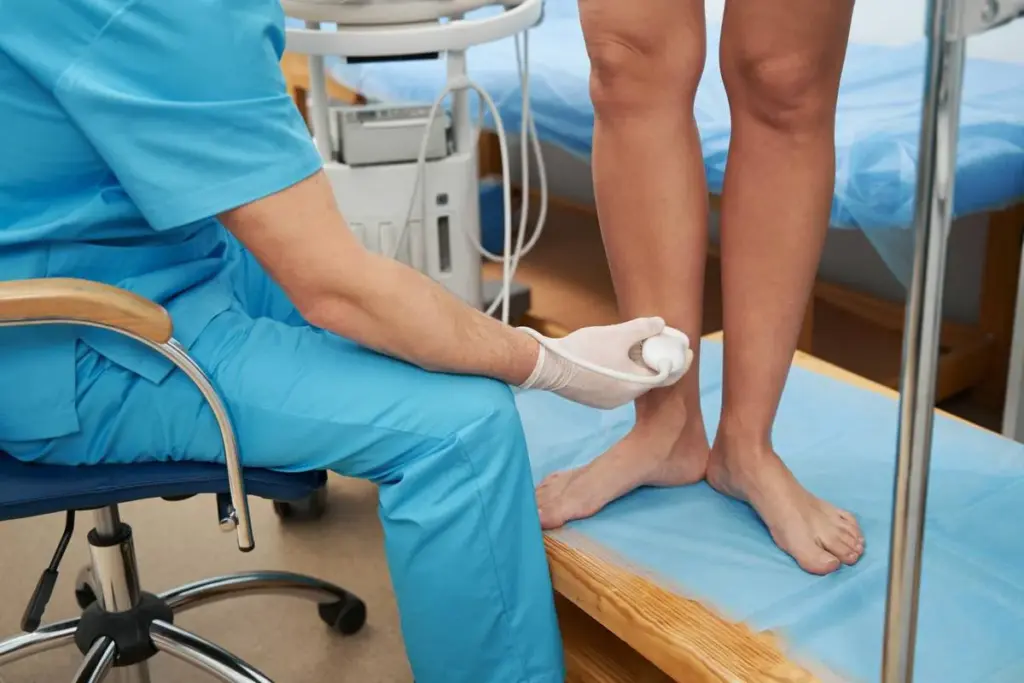
Nearly 202,000 people in the United States get angioplasty every year. A big part of these are for leg problems due to peripheral artery disease. This shows how key leg angioplasty is in today’s healthcare.Assessing how serious is leg angioplasty (generally low-risk) and discussing the typical leg angioplasty seriousness compared to open surgery.
Getting any medical treatment can be scary. Leg angioplasty is a way to open up blocked arteries. It’s a big help for many, but it’s normal to worry about its seriousness and risks.
We’ll dive into the details of leg angioplasty. We’ll look at its benefits and what patients can expect. This will give a full picture of this important treatment.
Key Takeaways
- Understanding the seriousness of leg angioplasty is key for patients.
- The procedure helps improve blood flow in the legs.
- Leg angioplasty has risks that patients should know about.
- Its importance comes from treating peripheral artery disease.
- Patients should know what to expect from the procedure.
Understanding Leg Angioplasty
Leg angioplasty is a procedure to open up narrowed or blocked arteries in the legs. It’s key for those with peripheral artery disease (PAD) and other vascular issues. These issues can limit blood flow to the lower legs.
Definition and Purpose
Leg angioplasty, or percutaneous transluminal angioplasty (PTA), aims to improve blood flow. It’s for patients with narrowed or blocked arteries. The goal is to ease pain when walking and prevent more serious problems.
The process uses a thin, flexible tube called a catheter. It carries a balloon to the blockage. When the balloon is inflated, it pushes the plaque against the artery walls. This widens the artery and boosts blood flow.
How Leg Angioplasty Works
The procedure starts with local anesthesia to numb the area. Then, a doctor uses imaging to guide the catheter to the blockage.
At the blockage, the balloon is inflated to open the artery. Sometimes, a stent is used to keep the artery open. Stents have greatly improved the success of angioplasty.
|
Procedure Step |
Description |
|---|---|
|
1. Catheter Insertion |
A thin catheter is inserted into the artery, guided by imaging technology. |
|
2. Balloon Inflation |
A balloon on the catheter is inflated to widen the narrowed artery. |
|
3. Stent Placement |
A stent may be placed to keep the artery open. |
Knowing how leg angioplasty works and its benefits helps patients choose the right treatment. It improves life quality and is vital for managing vascular diseases.
Conditions Requiring Leg Angioplasty

Some health problems need a treatment like leg angioplasty. Leg artery blockage dangers can cause serious health issues if not treated quickly. We will look at the main conditions that need this procedure, focusing on their effect on leg artery health and overall health.
Peripheral Artery Disease (PAD)
Peripheral Artery Disease (PAD) is when the arteries narrow, cutting off blood to the limbs. This is usually because of atherosclerosis, a buildup of plaque in the walls. PAD is a big reason for needing leg angioplasty because it directly harms the arteries in the legs.
Symptoms of PAD include pain when walking, cold legs, and weak pulses in the feet. If PAD is not treated, it can turn into a more serious condition. We will talk about this next.
Critical Limb Ischemia
Critical Limb Ischemia (CLI) is a severe form of PAD. It causes a big drop in blood flow to the limbs, leading to pain even when sitting and tissue loss. CLI is a serious condition that needs quick medical help to avoid losing a limb.
CLI symptoms are worse than PAD and include severe pain in the feet or toes even when sitting, wounds that won’t heal, and gangrene. Leg angioplasty is often a good treatment for CLI because it’s less invasive and works well to improve blood flow.
“Critical Limb Ischemia represents a major challenge in vascular medicine, requiring a complete treatment plan to save the limb and improve patient results.”— Vascular Specialist
Other Vascular Conditions
Other vascular problems might also need leg angioplasty. These include acute limb ischemia, a sudden blockage of an artery, and restenosis, when the arteries narrow again after angioplasty.
|
Condition |
Description |
Treatment Considerations |
|---|---|---|
|
PAD |
Narrowing of arteries due to plaque buildup |
Leg angioplasty to restore blood flow |
|
CLI |
Severe reduction in blood flow, pain at rest, tissue loss |
Urgent leg angioplasty, possible amputation if untreated |
|
Acute Limb Ischemia |
Sudden blockage of an artery |
Emergency leg angioplasty or thrombectomy |
Knowing about these conditions and their impact on leg artery health is key to finding the right treatment. Leg angioplasty is a helpful tool in managing these vascular issues, improving patient results and quality of life.
The Leg Angioplasty Procedure Explained
Leg angioplasty is a safe way to boost blood flow and ease leg pain. It involves several important steps. We will go over each one in detail.
Step-by-Step Process
The first step is making a small cut to reach the artery.
Next, a thin tube called a catheter is put in. It’s guided to the blockage using special images. Then, a balloon is used to make the artery wider.
- Preparation for the procedure, including administering local anesthesia.
- Insertion of a catheter into the femoral artery.
- Guiding the catheter to the site of the blockage.
- Inflating a balloon to widen the artery.
- Potential placement of a stent to keep the artery open.
Types of Stents Used
There are two main types of stents used: bare-metal and drug-eluting.
Bare-metal stents are made of metal. They help keep the artery open.
Drug-eluting stents release medicine. This helps prevent the artery from getting narrow again.
Duration and Anesthesia
The whole procedure usually takes 1 to 3 hours.
Local anesthesia is used to numb the area. Some might get conscious sedation too.
The type of anesthesia depends on the patient’s health and the procedure’s complexity.
Preparing for Leg Angioplasty
Getting ready for leg angioplasty means medical checks, adjusting meds, and knowing what to do on the big day. Knowing these steps helps lower risks and makes recovery easier.
Medical Evaluations
Before the procedure, you’ll get a full medical check-up. This might include:
- Blood tests to check for clotting disorders or other conditions that could affect the procedure.
- Imaging studies such as ultrasound, angiography, or magnetic resonance angiography (MRA) to visualize the arteries and plan the procedure.
- Electrocardiogram (ECG) to assess heart function.
These tests help us spot any risks and make the procedure fit your needs.
Medication Adjustments
Some meds might need to be changed or stopped before the procedure. This includes:
|
Medication Type |
Adjustment |
|---|---|
|
Blood Thinners |
May need to be stopped a few days before to reduce bleeding risk. |
|
Diabetes Medications |
Dosage may need adjustment based on fasting requirements. |
Day-of-Procedure Instructions
On the day of the procedure, you should:
- Arrive on time with someone to take you home.
- Wear comfy, loose clothes.
- Follow any fasting or diet rules given.
By following these steps, you can help make the procedure go smoothly.
Leg Angioplasty Seriousness: Risk Assessment
To understand how serious leg angioplasty is, we need to look at other vascular surgeries and individual risks. This procedure helps widen narrowed or blocked arteries in the legs. It’s a common treatment for many vascular conditions.
Comparing to Other Vascular Procedures
Leg angioplasty is often compared to bypass surgery. Research shows it has a lower death rate than more invasive surgeries like bypass grafting. For example, a study in the Journal of Vascular Surgery found leg angioplasty’s 30-day death rate was much lower than bypass surgery for patients with peripheral artery disease.
|
Procedure |
30-Day Mortality Rate |
Complication Rate |
|---|---|---|
|
Leg Angioplasty |
1.2% |
5.5% |
|
Bypass Surgery |
3.5% |
10.2% |
Patient Risk Factors
Patient risk factors are key in understanding leg angioplasty’s seriousness. Age, diabetes, kidney disease, and the severity of peripheral artery disease can affect outcomes. Patients with more health issues are at higher risk of complications.
For instance, a patient with diabetes and kidney disease might face higher risks after leg angioplasty. It’s important for patients to talk about their specific risks with their healthcare provider.
Mortality Statistics
Mortality rates for leg angioplasty are generally low, as shown in many studies. A meta-analysis in the European Journal of Vascular and Endovascular Surgery found the overall death rate was under 2%.
These numbers show leg angioplasty is relatively safe for the right patients. But, it’s key for patients to know the risks and benefits to make informed decisions about their care.
Potential Complications of Leg Angioplasty
It’s important to know the risks of leg angioplasty before deciding. This treatment helps with many vascular problems but comes with possible complications.
Immediate Complications
Right after or during the procedure, some issues can happen. These include:
- Bleeding or hematoma at the access site
- Vascular complications such as arterial dissection or rupture
- Allergic reactions to contrast dye
- Cardiovascular events like myocardial infarction or stroke
A study in the Journal of Vascular Surgery found that 5% to 10% of patients face immediate complications.
Short-Term Complications
Complications can also show up a few days to weeks later. These might be:
- Access site infections
- Restenosis or re-narrowing of the treated artery
- Stent thrombosis
According to the Journal of Endovascular Therapy, about 15% of patients deal with short-term issues.
Long-Term Complications
Months to years after the procedure, other problems can occur. These include:
- In-stent restenosis
- Stent fracture or deformation
- Progression of peripheral artery disease
|
Complication Type |
Timeframe |
Common Issues |
|---|---|---|
|
Immediate |
During/after procedure |
Bleeding, vascular complications |
|
Short-term |
Days to weeks |
Infection, restenosis |
|
Long-term |
Months to years |
In-stent restenosis, stent fracture |
Severe Leg Angioplasty Complications
Leg angioplasty is usually safe, but serious problems can happen. It’s key to know about these risks to make smart choices.
Arterial Rupture
Arterial rupture is a serious issue that can be life-threatening. It happens when the artery tears or is cut during the procedure. Quick action is needed to stop severe bleeding and other problems.
Things like complex blockages, severe hardening of the arteries, and big stents increase the risk. We’ll talk about how to handle arterial rupture later.
Acute Limb Ischemia
Acute limb ischemia is a severe problem that can happen after angioplasty. It’s when blood flow to the leg suddenly drops. This can cause a lot of pain, nerve damage, and even loss of the limb if not treated right away.
Things like dissection or clotting during the procedure can lead to this. It’s very important to act fast to get blood flow back and avoid lasting damage.
Contrast-Induced Nephropathy
Contrast-induced nephropathy (CIN) is a problem linked to the dye used in angioplasty. It can cause sudden kidney injury, mainly in people with kidney issues.
We check kidney health before the procedure and use hydration to reduce risk. It’s also key to watch kidney function after the procedure to catch and manage CIN early.
Rare but Serious Complications
There are other rare but serious risks with leg angioplasty. These include allergic reactions to the dye, infection, and stent clotting.
Knowing about these risks helps us prevent them and manage them if they happen.
|
Complication |
Description |
Risk Factors |
|---|---|---|
|
Arterial Rupture |
Tear or severing of the artery |
Complex lesions, severe calcification |
|
Acute Limb Ischemia |
Sudden reduction in limb blood flow |
Dissection, thrombosis |
|
Contrast-Induced Nephropathy |
Acute kidney injury due to contrast dye |
Pre-existing kidney disease |
Recovery Timeline After Leg Angioplasty
Knowing how long it takes to recover from leg angioplasty is key. This procedure helps open blocked arteries in the legs. Each person’s recovery is different, but there are common steps to follow.
Hospital Stay
After leg angioplasty, most people stay in the hospital for just a day or two. Doctors watch for any problems and help with pain during this time.
First Week Recovery
In the first week, rest and avoid hard work. You might see some bruising or feel sore where the catheter was. Always follow your doctor’s advice on caring for your wound, taking medicine, and when to come back for check-ups.
Complete Recovery Expectations
It can take weeks to months to fully recover from leg angioplasty. How long it takes depends on your health, the procedure’s complexity, and how well you follow your doctor’s advice. Most people can get back to normal in 1 to 3 months.
The benefits of leg angioplasty, like better blood flow and less PAD symptoms, make the recovery worth it. Knowing about the recovery helps patients get ready and get the best results from the procedure.
|
Recovery Stage |
Timeline |
Key Activities |
|---|---|---|
|
Hospital Stay |
24-48 hours |
Rest, monitoring for complications |
|
First Week |
1 week |
Avoid strenuous activities, wound care |
|
Complete Recovery |
1-3 months |
Gradual return to normal activities |
By knowing the recovery timeline and following your doctor’s advice, you can get the most out of leg angioplasty. This improves your life quality.
Benefits and Success Rates of Leg Angioplasty
Leg angioplasty is a key treatment for leg artery disease. It’s a minimally invasive procedure that has changed how we manage peripheral artery disease. It brings about significant improvements in patient outcomes.
Symptom Relief Statistics
Leg angioplasty greatly relieves symptoms of peripheral artery disease. A study in the Journal of Vascular Surgery found that over 80% of patients reported improved walking distances after the procedure.
It also reduces claudication, a pain in the legs during walking. By improving blood flow, leg angioplasty dramatically improves a patient’s quality of life. It makes daily activities easier.
Limb Salvage Rates
Leg angioplasty is also key in limb salvage. For those with critical limb ischemia, it’s a lifesaver. It prevents amputation by restoring blood flow. Studies show that leg angioplasty achieves limb salvage rates ranging from 70% to 90% at one year.
Quality of Life Improvements
Leg angioplasty also boosts quality of life. It enhances blood flow and reduces pain. This makes patients more active and able to enjoy activities they love.
A study in the Journal of Endovascular Therapy found that patients experienced significant improvements in their overall quality of life. This was measured by health surveys.
In conclusion, leg angioplasty offers many benefits. It relieves symptoms, saves limbs, and improves quality of life. As medical technology advances, these benefits will likely grow. Leg angioplasty is becoming a more viable option for patients with leg artery disease.
Factors Affecting Leg Angioplasty Outcomes
It’s important to know what affects leg angioplasty results. This procedure helps open blocked arteries in the legs. It can greatly improve life quality for those with PAD and other vascular issues.
Anatomical Considerations
The shape and health of leg arteries matter a lot for angioplasty success. Things like where and how bad the blockages are, and if there’s calcium buildup, can change results. Some spots are harder to fix than others.
|
Anatomical Factor |
Impact on Angioplasty |
|---|---|
|
Lesion Location |
Affects procedural complexity and success rate |
|
Arterial Calcification |
Increases risk of complications and restenosis |
|
Arterial Wall Condition |
Influences the likelihood of successful stent placement |
Physician Experience and Hospital Volume
The doctor’s experience and the hospital’s volume are very important. More experienced doctors and hospitals with high volumes usually get better results. This is because they have better techniques and care.
Knowing these factors helps doctors better plan treatments. This can lead to better results for patients having leg angioplasty.
Alternative Treatments to Consider
Patients have many treatment options beyond leg angioplasty. Each option has its own benefits and risks. It’s important to explore these alternatives in detail.
Medical Management Options
Medical management is often the first choice for patients with PAD or other vascular conditions. This approach includes lifestyle changes and medication to manage symptoms and slow disease progression.
- Exercise Therapy: Supervised exercise programs can improve walking distance and cardiovascular health.
- Medications: Antiplatelet agents, statins, and medications for hypertension and diabetes are commonly used.
- Lifestyle Changes: Quitting smoking, dietary changes, and managing weight are key for vascular health.
Bypass Surgery Comparison
Bypass surgery is a surgical option instead of leg angioplasty. It involves creating a detour around the blocked artery using a graft.
Key differences between bypass surgery and leg angioplasty:
- Invasiveness: Bypass surgery is more invasive, needing larger incisions and longer recovery times.
- Indications: Bypass surgery is recommended for more complex or extensive arterial disease.
- Outcomes: Both procedures have success rates, with bypass surgery sometimes giving more durable results for certain patients.
Emerging Therapies
Research into new treatments for PAD and other vascular diseases is ongoing. Several emerging therapies show promise.
Some of the emerging therapies include:
- Atherectomy Devices: These devices remove plaque from arteries, potentially reducing the need for stenting.
- Drug-Coated Balloons: These balloons deliver medication directly to the arterial wall, reducing restenosis rates.
- Stem Cell Therapy: Researchers are exploring the use of stem cells to promote angiogenesis and improve tissue perfusion.
As medical technology advances, patients and healthcare providers have more options than ever to manage vascular disease effectively.
When considering alternative treatments to leg angioplasty, it’s important to discuss these options with a healthcare provider. This helps determine the most appropriate treatment plan based on individual patient needs and medical history.
Cost and Insurance Considerations
It’s important for patients to understand the cost of leg angioplasty. The price can change based on where you are, who does the procedure, and what you need.
Insurance Coverage in the United States
Most insurance plans in the U.S. cover leg angioplasty. This is because it’s seen as a necessary treatment for Peripheral Artery Disease (PAD). But, the details of coverage can differ a lot between plans.
Key factors affecting insurance coverage include:
- Pre-approval requirements
- Deductibles and co-payments
- Network providers
- Specific procedure codes
It’s a good idea to talk to your insurance provider to know what’s covered.
Financial Assistance Programs
If you’re worried about the cost, there are help programs out there. Hospitals, non-profits, and device makers might offer financial aid.
Types of financial assistance:
- Sliding scale fees based on income
- Grants for patients with specific financial needs
- Patient advocacy services to help navigate insurance claims
Ask about these programs when you talk to your doctor about treatment.
Long-Term Management After Legioplasty
The journey doesn’t end with leg angioplasty. A good long-term plan is key for the best results. After the procedure, patients need a detailed care plan. This plan helps keep the blood vessels healthy and avoids future problems.
Follow-Up Protocol
Regular check-ups are important to watch the health of the treated arteries. We suggest a follow-up plan that includes:
- First check-up in 1-2 weeks after the procedure
- Follow-ups every 3-6 months for the first year
- Annual visits after that
These visits help us see if the artery is staying open. We can catch and fix any issues early. We also adjust the treatment plan as needed.
Medication Regimen
Following the prescribed medication is key to keeping leg angioplasty successful. Patients usually take:
|
Medication Type |
Purpose |
Duration |
|---|---|---|
|
Antiplatelet agents |
Prevent blood clots |
Lifelong or as directed |
|
Statins |
Lower cholesterol |
Lifelong |
|
Beta-blockers |
Manage blood pressure and heart rate |
Variable, based on individual health |
It’s important to stick to the medication plan. This helps avoid complications and keeps the artery open for longer.
Lifestyle Modifications for Vascular Health
Changing your lifestyle is important for keeping your blood vessels healthy after angioplasty. We recommend:
- Smoking cessation: Quitting smoking is key for better vascular health and overall health.
- Dietary changes: Eat a diet full of fruits, vegetables, whole grains, and lean proteins.
- Regular exercise: Do moderate activities like walking to improve blood flow and heart health.
- Weight management: Keep a healthy weight to reduce strain on your blood vessels.
- Stress management: Use stress-reducing activities like meditation or yoga.
By making these lifestyle changes, patients can greatly improve their vascular health. This reduces the risk of future heart problems.
Conclusion
Leg angioplasty is a major medical procedure that needs careful thought and understanding. We’ve looked into the details of leg angioplasty, including what it is, the conditions it treats, and how it’s done. We’ve also talked about possible complications, the recovery time, and managing health long-term after the procedure.
The importance of leg angioplasty is huge. It tackles serious vascular issues like Peripheral Artery Disease (PAD) and Critical Limb Ischemia. But, it offers big benefits like easing symptoms, saving limbs, and improving life quality. Knowing about leg angioplasty outcomes helps patients make smart choices about their health.
Understanding what affects leg angioplasty results is key. This includes the body’s structure, the patient’s health, and the doctor’s skill. We stress the need for full care, including follow-ups, medication, and healthy lifestyle choices for blood vessel health.
In the end, leg angioplasty is a key treatment for severe leg vascular problems. By knowing its importance, benefits, and results, patients can face their treatment with confidence and clear understanding.
FAQ
What is leg angioplasty, and how does it work?
Leg angioplasty is a procedure to improve blood flow in the legs. It widens narrowed or blocked arteries. A balloon is used to inflate the artery, and sometimes a stent is placed to keep it open.
What are the main conditions that require leg angioplasty?
Leg angioplasty is needed for Peripheral Artery Disease (PAD) and Critical Limb Ischemia. These conditions cause narrowed or blocked leg arteries, reducing blood flow.
What are the risks associated with leg angioplasty?
Risks include bleeding or artery rupture right away. Short-term risks are infection or artery narrowing again. Long-term risks are stent failure or needing more procedures.
How serious is leg angioplasty compared to other vascular procedures?
Leg angioplasty is generally safe but can vary based on patient risk and procedure complexity. It’s less risky than surgeries like bypass surgery.
What is the recovery time after leg angioplasty?
Recovery time varies, but most patients stay in the hospital for a day or two. The first week is for rest and slow activity return. Full recovery takes a few weeks to months.
What are the benefits and success rates of leg angioplasty?
It relieves symptoms, saves limbs, and improves life quality. Success rates are high, with many patients seeing better mobility and less pain.
Are there alternative treatments to leg angioplasty?
Yes, options include medication, lifestyle changes, bypass surgery, and new therapies like atherectomy or drug-coated balloons. Treatment choice depends on condition severity and patient health.
How much does leg angioplasty cost, and what are the insurance considerations?
Costs vary by location, hospital, and doctor fees. In the U.S., insurance often covers it, but coverage varies. Financial help may be available for those needing it.
What is involved in long-term management after leg angioplasty?
Long-term care includes artery monitoring, clot-preventing meds, and lifestyle changes like quitting smoking and exercising. These help keep the artery open.
Can leg angioplasty prevent the need for amputation in patients with Critical Limb Ischemia?
Yes, it can prevent amputation in Critical Limb Ischemia by improving blood flow. It’s a limb-saving procedure.
How do anatomical considerations and patient health factors affect leg angioplasty outcomes?
Outcomes depend on blockage location and severity, and patient health like diabetes or smoking. These factors greatly influence success and durability.
References
National Institutes of Health. Evidence-Based Medical Insight. Retrieved from https://www.nhlbi.nih.gov/health-topics/angioplasty


































