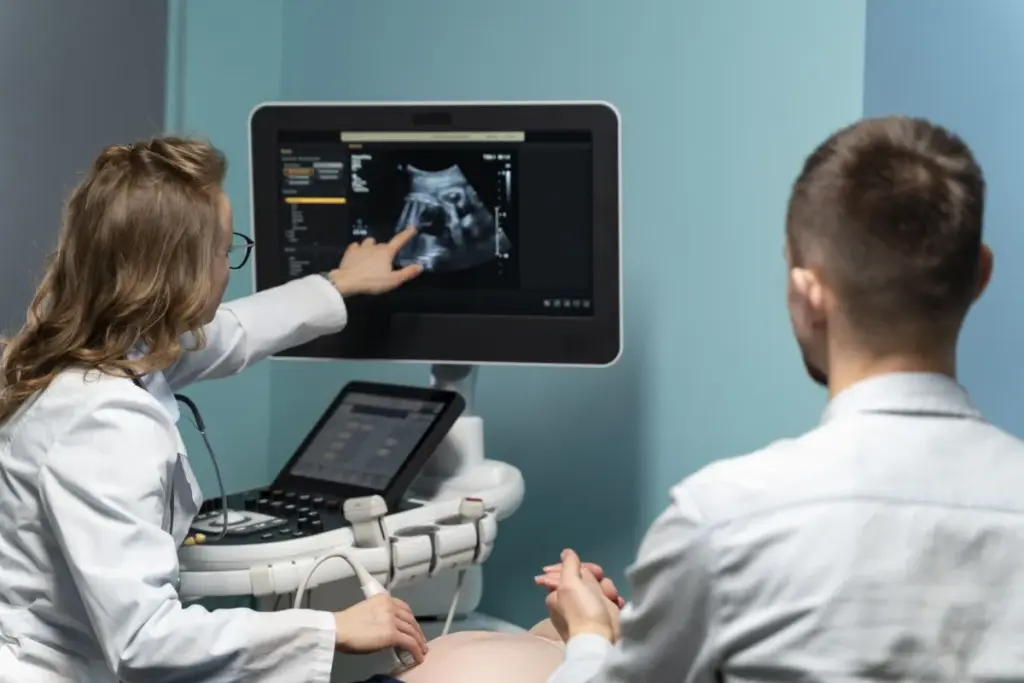
Medical interventions have become more precise with new imaging technologies. We use these technologies to guide complex procedures in the body. Two main methods are fluoroscopic guidance and ultrasound guidance.
Fluoroscopic guidance uses continuous X-ray imaging to show body structures in real-time. On the other hand, ultrasound guidance uses sound waves for real-time images without radiation. A study on found both methods give similar pain relief and outcomes for many procedures.
It’s important to know the differences between these imaging techniques. We’ll look at their uses, benefits, and downsides. This will help us see which one is safer and more effective for patients.
Key Takeaways
- Fluoroscopic guidance uses continuous X-ray imaging for real-time visualization.
- Ultrasound guidance relies on sound waves, eliminating radiation exposure.
- Both methods provide comparable pain relief and functional outcomes.
- Ultrasound guidance results in less radiation exposure and fewer needle adjustments.
- Procedures guided by ultrasound are considered more efficient and cost-effective.
The Fundamentals of Medical Imaging Guidance
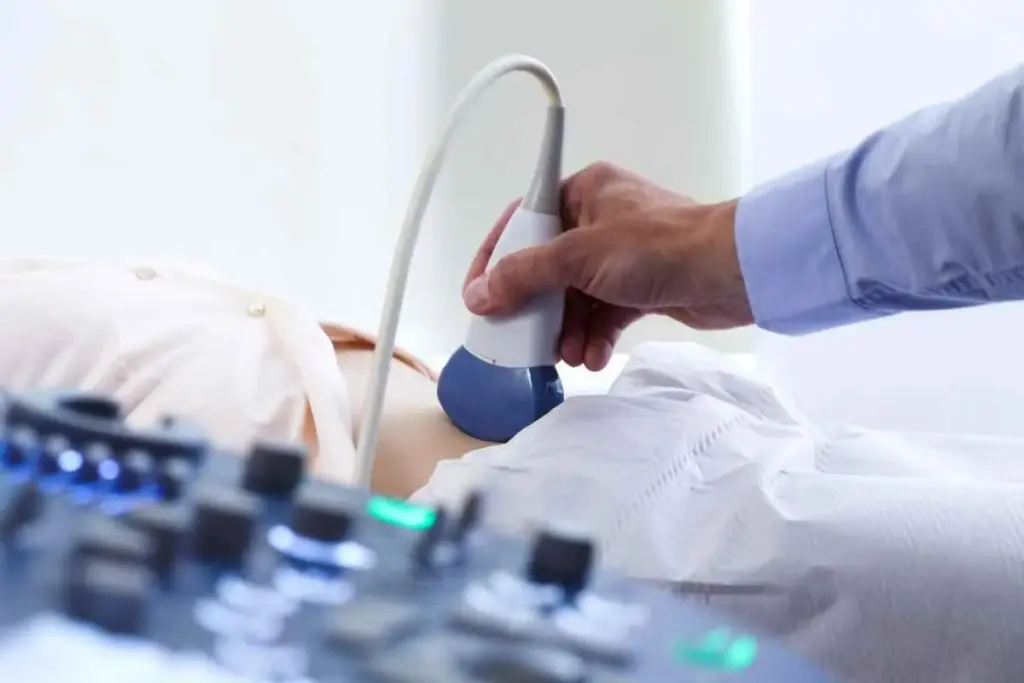
Medical imaging guidance has changed interventional medicine a lot. It makes procedures precise and less invasive. This change comes from better procedural guidance and the need for real-time images.
Evolution of Procedural Guidance in Interventional Medicine
Interventional medicine has grown a lot. Guidance during procedures is key to this growth. At first, doctors had to rely on landmarks and their own skills because of limited vision.
But, new imaging technologies have made things better. show that ultrasound and fluoroscopy can give similar results. A 2024 study found that both methods gave 75-77% pain relief after 30 minutes.
The Growing Importance of Real-Time Visualization
Real-time images are now vital in interventional medicine. They help doctors do procedures more accurately and safely. Seeing what’s happening as it happens lets doctors make quick changes.
This has many benefits. It makes needle placement better, reduces the chance of damage, and boosts doctor confidence.
Both fluoroscopy guidance and ultrasound modalities offer real-time images. But, they work differently and are used in different ways. Knowing the differences helps choose the best method for each procedure.
Fluoroscopy Guidance Technology Explained

Fluoroscopy guidance plays a crucial role in medical imaging. It lets doctors see what’s happening inside the body in real time. This helps make sure procedures are done right and safely.
The Science Behind Fluoroscopic Imaging
Fluoroscopy uses X-rays to show what’s inside the body. An X-ray tube sends out X-rays, which go through the body. Then, a detector catches these X-rays and shows them on a screen.
Equipment Components and Setup Requirements
To use fluoroscopy, you need an X-ray generator, tube, detector, and a screen. The setup involves placing the X-ray tube and detector around the patient. This lets doctors see the area they’re working on from different angles.
The setup is designed to keep radiation low while keeping images clear. This is done by adjusting the X-ray settings and using tools to focus the beam.
Image Acquisition and Processing in Fluoro Guidance
Fluoroscopy captures X-ray images continuously. These images are then improved to make them clearer and reduce noise. Techniques like digital subtraction angiography help make certain parts, like blood vessels, stand out.
|
Feature |
Basic Fluoroscopy |
Advanced Fluoroscopy |
|---|---|---|
|
Image Quality |
Standard resolution |
High resolution with enhanced contrast |
|
Radiation Exposure |
Higher dose |
Lower dose with advanced shielding |
|
Pulse Rate |
Fixed rate |
Adjustable pulse rate for reduced dose |
Fluoroscopy guidance is a crucial tool in medicine. It offers real-time images that help doctors perform procedures more accurately and safely. Knowing how it works helps healthcare professionals use it better in different medical situations.
Ultrasound Guidance Technology Explained
Ultrasound guidance technology has changed the game in interventional medicine. It gives doctors real-time images without using harmful radiation. This method is key in many medical procedures, making them safer and more effective.
The Science Behind Ultrasound Imaging
Ultrasound imaging uses sound waves to see inside the body. It works like echolocation, sending sound waves and catching echoes to make images. This non-invasive method lets doctors see in real-time, making it crucial for many procedures.
A probe, or transducer, is placed on the skin. It turns electrical energy into sound waves and catches the echoes. These echoes are turned back into electrical signals, creating the images we see.
Equipment Components and Probe Selection
The tools for ultrasound guidance include the machine, transducer probes, and sometimes extra items like gel or needle guides. Choosing the right transducer probe is key, as different ones work for different tasks, like looking at the surface or deeper tissues.
Choosing a probe depends on the procedure and where it’s done. For example, a high-frequency probe is best for the surface, while a lower frequency one is better for deeper areas.
Image Acquisition and Interpretation in USG Procedures
In ultrasound-guided procedures, getting the best images is important. This means adjusting the machine settings for the best view. Understanding these images well is vital for the procedure’s success, needing knowledge of ultrasound and anatomy.
Doctors must know how to see the right structures and spot problems. They also need to adjust the settings to place needles correctly and succeed in the procedure.
Ultrasound is especially useful for procedures on the surface or in small joints and soft tissue injections. Its ability to show images in real-time is a big plus.
Radiation Exposure: A Critical Distinction
Radiation exposure is key when comparing fluoroscopy to ultrasound in medical procedures. It’s important for both patient and provider safety to understand this difference.
Quantifying Radiation in Fluoroscopy Procedures
Fluoroscopy uses X-rays for real-time images of the body’s inside. This means patients and staff get exposed to radiation. The amount of radiation depends on the procedure’s length, X-ray strength, and the patient’s BMI.
Research shows that ultrasound can cut down radiation exposure. On average, ultrasound reduces the need for X-rays by 80%. This makes ultrasound a safer choice for many patients.
Is There Radiation in Ultrasound Procedures?
Ultrasound doesn’t use ionizing radiation like fluoroscopy does. It uses sound waves to create images. This makes ultrasound safer for those worried about radiation.
Patient and Provider Safety Considerations
Reducing radiation in medical procedures is very important. It’s crucial for patients, especially those needing repeated scans. It also keeps healthcare workers safe, improving patient care.
Choosing the right imaging method is vital. Knowing the radiation differences between fluoroscopy and ultrasound helps make safer choices. This balances the need for clear images with the goal of reducing radiation risks.
The Difference Between USG and Ultrasound Terminology
It’s important to know the terms used in medical imaging. Terms like USG (Ultrasonography) and ultrasound are often mixed up. But they have different meanings and uses.
Defining USG (Ultrasonography) vs. Ultrasound
USG, or Ultrasonography, is about using ultrasound for medical tests. Ultrasound is a wider term that includes both tests and treatments. The main difference is that USG is for testing, while ultrasound is the technology used for many medical needs.
USG Scan Meaning in Clinical Context
A USG scan is a test using ultrasonography. It’s used to check on things like how a baby is growing, liver health, or other organs. It’s a way to say the test uses ultrasonography for diagnosis.
USG vs. Sonography: Clarifying Common Misconceptions
Many people mix up USG with sonography. Sonography is another word for ultrasonography, showing how sound waves make images of inside the body. So, USG and sonography mean the same thing, both about using ultrasound for tests. The mix-up comes from different words used in different places and by different doctors.
Knowing these details helps doctors and patients talk better. It makes medical tests and treatments more accurate and effective.
Image Quality and Visualization Capabilities
Image quality is key for both fluoro-guided and ultrasound-guided procedures. It’s all about seeing the target anatomy clearly and accurately.
Tissue Differentiation and Resolution Comparison
Being able to tell different tissues apart is crucial. Fluoroscopy shines when it comes to seeing bones and contrast agents. On the other hand, ultrasound is better at showing soft tissues.
Let’s look at how both modalities compare in terms of resolution. This helps us understand their uses in medical settings.
|
Modality |
Tissue Differentiation |
Resolution |
|---|---|---|
|
Fluoroscopy |
Excellent for dense structures |
High resolution for contrast agents |
|
Ultrasound |
Excellent for soft tissues |
Variable resolution depending on probe frequency |
Depth Penetration and Anatomical Limitations
How deep a modality can see is also important. Fluoroscopy can look deep into tissues, which is great for certain procedures. But, ultrasound can only go so deep, depending on the probe’s frequency.
Here’s a quick look at how both modalities compare in depth penetration and their limitations:
|
Modality |
Depth Penetration |
Anatomical Limitations |
|---|---|---|
|
Fluoroscopy |
Deep penetration |
Limited soft tissue contrast |
|
Ultrasound |
Limited by probe frequency |
Limited by acoustic window availability |
Ultrasound Modalities and Their Specific Applications
Ultrasound has many types, each for different uses. B-mode ultrasound is great for looking at anatomy. Doppler ultrasound helps check blood flow.
Here’s a quick rundown of ultrasound modalities and their uses:
|
Ultrasound Modality |
Application |
|---|---|
|
B-mode |
Anatomical imaging |
|
Doppler |
Blood flow assessment |
|
Elastography |
Tissue stiffness assessment |
Clinical Applications of Fluoroscopy-Guided Procedures
Fluoroscopy has changed how we do medicine. It gives doctors real-time images. This helps them do complex tasks safely and accurately.
Spinal Interventions and Epidural Injections
Fluoroscopy is key in spinal work, like epidural shots. It helps place needles exactly right. This makes treatments work better and cuts down on risks.
Things like facet joint shots and spinal cord stimulators get a big boost from fluoroscopy. It makes these procedures safer and more effective.
Joint Injections and Aspirations
Fluoroscopy is also great for joint shots and taps. It helps put needles in the right spot in joints like the shoulder and knee.
It’s super for treating arthritis. For example, it lets doctors put pain relief right where it’s needed.
Vascular and Cardiac Interventional Procedures
In heart and blood vessel work, fluoroscopy is a big help. It’s used for things like angiograms and stenting. It lets doctors guide tools through blood vessels with precision.
It’s also key for heart rhythm treatments. Fluoroscopy helps place tools exactly where they need to be. This makes these tricky procedures safer and more successful.
Fluoroscopy is a game-changer in medicine. It gives doctors the tools they need to do their jobs better. This leads to better care for patients.
Clinical Applications of Ultrasound-Guided Procedures
Ultrasound-guided procedures have become more precise with technology advancements. They are used for many clinical applications. This offers real-time visualization and better accuracy.
Peripheral Nerve Blocks and Regional Anesthesia
Ultrasound intervention has changed regional anesthesia. It allows for direct nerve and tissue visualization. Ultrasound-guided peripheral nerve blocks are now a top choice for pain management.
Studies show ultrasound guidance boosts nerve block success rates. It also lowers complication risks .
The benefits of ultrasound-guided regional anesthesia include:
- Improved accuracy in needle placement
- Reduced risk of nerve damage
- Enhanced patient comfort
- Faster onset of anesthesia
Musculoskeletal Interventions and Joint Injections
Ultrasound guidance is also key for musculoskeletal interventions. This includes joint injections and aspirations. Ultrasound’s real-time imaging allows for precise targeting.
|
Procedure |
Benefits of Ultrasound Guidance |
|---|---|
|
Joint Injections |
Improved accuracy, reduced risk of infection |
|
Aspirations |
Real-time visualization, reduced risk of complications |
Vascular Access and Soft Tissue Procedures
Ultrasound guidance is crucial for vascular access procedures. This includes central line placement and peripheral intravenous access. It reduces complication risks and boosts success rates.
In soft tissue procedures, ultrasound guidance helps target lesions accurately. This makes diagnosis and treatment more precise.
Procedural Accuracy and Precision Comparison
It’s key for doctors to know how fluoro-guided and ultrasound-guided procedures differ. The right choice can make a big difference in treatment success.
We’ll look at what each method does best. This includes how well they show targets, place needles, and how fast they are. We’ll see what each method is good at and where they might fall short.
Target Visualization Success Rates
Seeing the target clearly is crucial for procedure success. Fluoroscopic guidance uses X-rays to show dense structures like bones. Ultrasound guidance shows soft tissues and blood vessels without radiation.
Both methods work well, but the choice depends on the procedure and the patient. Fluoroscopy is often used for spinal procedures. Ultrasound is better for vascular and soft tissue work.
Needle Placement Accuracy Studies
Getting the needle in the right spot is key. Studies show both methods can be very accurate. But, ultrasound guidance is better for some tasks, like nerve blocks, because it shows the needle and area in real-time.
How accurate needle placement is can depend on the doctor, the patient, and the technology used.
Procedural Time Efficiency Analysis
How fast a procedure is done matters for patient care and costs. Ultrasound-guided procedures are often quicker because they’re easier to do and can be done at the bedside.
Fluoro-guided procedures might take longer because of setup needs. But, the time it takes can also depend on the procedure’s complexity and the doctor’s experience.
Pain Management Outcomes: Research Evidence
Research on pain management shows how effective fluoro-guided and ultrasound-guided procedures are. Both methods have been studied for their pain relief outcomes. This research helps doctors make better choices for their patients.
Short-term Pain Relief Comparisons
Studies have looked at how well these procedures work for short-term pain relief. A meta-analysis found no big difference in pain relief between the two methods . This means both can help with short-term pain.
But, other things like the patient, the procedure, and the doctor’s preference might also play a role. We’ll look at these factors more closely below.
Long-term Functional Outcomes at 6 Months
Improving function over time is key in pain management. Research shows both methods can lead to better function at 6 months. Yet, more research is needed to know which is better.
Patient-reported Experience and Satisfaction Differences
How patients feel and their satisfaction are important in pain management. Studies show ultrasound-guided procedures make patients happier because of the clear view and less radiation. Fluoro-guided procedures might make patients more anxious because of radiation worries.
|
Outcome Measure |
Fluoro-guided |
Ultrasound-guided |
|---|---|---|
|
Short-term Pain Relief |
Effective |
Effective |
|
Long-term Functional Outcomes |
Improved |
Improved |
|
Patient Satisfaction |
Variable |
Higher |
In conclusion, both fluoro-guided and ultrasound-guided procedures can help with pain. The right choice depends on the patient, the procedure, and the doctor’s skills.
Cost and Resource Considerations
Healthcare facilities must think about the costs of using fluoroscopy guidance versus ultrasound modalities. The price difference between these two can affect a facility’s budget and how well it runs.
Equipment Investment and Maintenance Expenses
Fluoroscopy guidance equipment costs more to buy than ultrasound modalities. Fluoroscopy needs expensive parts like the X-ray generator and image intensifier. Ultrasound machines are cheaper and can do more things.
Maintenance costs also differ. Fluoroscopy needs more frequent and expensive upkeep because it’s more complex.
A study showed that fluoroscopy systems cost between $200,000 and over $500,000. High-end ultrasound machines usually cost between $50,000 and $200,000.
Procedure Room Requirements and Modifications
Fluoroscopy guidance needs more because it requires radiation shielding and special setup. This can make setting up procedure rooms very expensive. On the other hand, ultrasound modalities can often be used in rooms that already exist with little change.
The differences in room needs affect both the upfront costs and ongoing expenses. Facilities must think about radiation safety and keeping equipment in good shape.
Staff Training and Expertise Development Costs
Teaching staff to use fluoroscopy guidance and ultrasound modalities costs a lot. Both need special training, but fluoroscopy also includes learning about radiation safety.
Healthcare facilities need to plan for training that covers how to use the equipment and its clinical uses. They also need to learn about safety rules for each method.
Learning Curve and Training Requirements
Medical technology keeps getting better. Knowing how to train for different guidance systems is key. The skill level of practitioners affects how well procedures work. This skill comes from good training.
Developing Proficiency in Fluoroscopy Guidance
Fluoroscopy needs a deep understanding of radiation safety and image interpretation. Training must cover both theory and practice to help practitioners. The learning curve for fluoroscopy is high, needing long training and practice to stay good.
Learning fluoroscopy means knowing how to use the equipment and read images. It’s about understanding anatomy and matching images with body parts. Also, training must teach how to keep everyone safe from radiation.
Mastering Ultrasound Intervention Techniques
Ultrasound needs different skills, like real-time imaging and moving under ultrasound. Training focuses on fine motor skills and reading ultrasound images. It’s about learning to do things with precision and accuracy.
Learning ultrasound involves classroom lessons, simulation, and practice. It’s considered easier than fluoroscopy but still needs focused training and regular practice to stay good.
Cross-training Considerations for Medical Practitioners
Practitioners already skilled in one method can learn another. Cross-training broadens their skills, helping them choose the best method for each case. But, it must be done carefully to grasp the new method’s challenges.
Good cross-training programs match the individual’s skills and experience. They focus on the differences and any missing skills. This way, practitioners can use their current skills and learn new ones, improving care for patients.
Patient Selection and Procedural Decision-Making
Choosing between fluoroscopy or ultrasound for guidance depends on many things. These include the patient’s body and the problem they have. We also think about the procedure’s needs, the patient’s health, and the risks of each method.
Anatomical and Pathological Considerations
The shape and health of a patient’s body are key in picking a guidance method. Fluoroscopy is best for complex bone work or deep problems because it shows the needle path well.
Ultrasound is better for surface work or when seeing things live is important. It lets us place needles accurately and safely.
Procedure-specific Selection Criteria
Each procedure has its own needs for guidance. For example, joint injections and aspirations need ultrasound for seeing soft tissues and fluids. But, vascular and heart work often use fluoroscopy for detailed images of blood vessels.
|
Procedure |
Preferred Guidance Modality |
Rationale |
|---|---|---|
|
Joint Injections |
Ultrasound |
Real-time visualization of soft tissue and fluid dynamics |
|
Vascular Interventions |
Fluoroscopy |
High-resolution imaging of complex vascular structures |
Contraindications and Limitations for Each Modality
Fluoroscopy and ultrasound each have things they can’t do. Fluoroscopy uses X-rays, so it’s not good for pregnant women or those sensitive to radiation. Ultrasound might not work well for some body types or if there’s gas in the body.
By looking at these points and what each patient needs, we can choose the best guidance for their procedure.
USG vs Ultrasound: Comparative Advantages and Limitations
USG and ultrasound are related but have different uses in healthcare. Knowing their strengths and weaknesses helps doctors choose the best tests and treatments.
Procedural Efficiency and Workflow Integration
How well USG and ultrasound work can affect how smoothly things run in a clinic. USG, or ultrasonography, is great for live images during procedures like biopsies. It also has Doppler and elastography, making it versatile for many tests.
USG is better for simple tests, but ultrasound is better for complex ones. The choice depends on the situation and the doctor’s skills.
Visualization Capabilities for Different Tissue Types
Seeing what’s inside the body is key for both USG and ultrasound. USG is good for looking at things close to the surface and guiding treatments. But, it’s not as good for deeper tissues or if the doctor isn’t skilled enough.
Ultrasound, with its many types, can see more. Doppler checks blood flow, and elastography looks at tissue stiffness. This makes ultrasound great for many diseases, from blood vessel problems to liver issues.
Safety Profile and Risk Assessment
Both USG and ultrasound are safe because they don’t use harmful radiation. But, knowing the risks of each is important. For example, some ultrasound tests use contrast agents that can be risky.
When thinking about safety, we must look at how dependent the test is on the doctor, the chance of wrong diagnoses, and what it can’t see. By understanding these, doctors can make safer choices for patients.
|
Modality |
Procedural Efficiency |
Visualization Capabilities |
Safety Profile |
|---|---|---|---|
|
USG |
High for simple diagnostic tasks |
Excellent for superficial structures and real-time guidance |
Safe, non-ionizing radiation |
|
Ultrasound |
Variable, depending on modality |
Broad range of capabilities, including Doppler and elastography |
Safe, with considerations for contrast agent use |
Future Trends in Image-Guided Procedures
Image-guided procedures are on the verge of a big change thanks to new tech. These advancements will make medical procedures more precise and safe. They will change how we do things in medicine.
Advancements on the Horizon
New tech like artificial intelligence (AI) and machine learning (ML) will change image-guided procedures. They will help doctors understand images better and guide procedures more accurately. This could lead to fewer mistakes.
Hybrid imaging technologies are also coming. They mix different imaging types to give clearer images. For example, mixing fluoroscopy guidance with ultrasound imaging could make procedures better.
Artificial Intelligence Integration in Imaging Guidance
AI will make a big difference in imaging guidance. It can analyze images and suggest the best paths for needles. This will make procedures more precise. AI can also do routine tasks, letting doctors focus on the hard parts.
Research shows AI can spot tiny details and make image interpretation more consistent. As AI gets better, we’ll see even more ways it can help in medical procedures. This could lead to better results for patients.
Emerging Hybrid Technologies and Fusion Imaging
New hybrid technologies and fusion imaging are big steps forward. They combine different imaging types, like ultrasound and fluoroscopy. This gives doctors a clearer view of what’s going on inside the body.
Fusion imaging overlays different images in real-time. This gives a complete view of the area being treated. It can make needle placement more accurate and reduce risks. As these techs get better, they’ll be used more often, making procedures safer and more efficient.
In conclusion, the future of image-guided procedures looks bright. New tech will make procedures more precise, safe, and effective. We’re excited to see how these advancements will improve medical care and help patients.
Conclusion: Selecting the Optimal Guidance Method
Choosing the best guidance method depends on many factors. These include the clinical situation, what the patient needs, and the specifics of the procedure. We’ve looked at the differences between using fluoroscopy and ultrasound for guidance.
It’s important to know the difference between USG and ultrasound when deciding. Fluoroscopy gives real-time images for complex procedures. On the other hand, ultrasound is safer and doesn’t use radiation for many procedures.
When picking between these methods, we must think about the situation, the patient’s body, and what the procedure needs. Knowing the good and bad of each helps doctors make better choices. This improves care and the success of procedures.
In the end, the best method is one that works well, is safe, and meets the patient’s needs. This shows how modern medicine is all about personal and detailed care.
FAQ
What is the main difference between fluoroscopic guidance and ultrasound guidance?
Fluoroscopy uses X-rays to show real-time images. Ultrasound uses sound waves to create images. This makes ultrasound safer because it doesn’t use radiation.
Is there radiation in ultrasound procedures?
No, ultrasound doesn’t use ionizing radiation. This makes it safer for patients and doctors.
What is fluoroscopic guidance used for?
It’s used for spinal injections, joint injections, and vascular procedures. It helps place needles accurately.
What is the difference between USG and ultrasound?
USG stands for Ultrasonography, often used for diagnosis. Ultrasound can mean both diagnostic and therapeutic uses.
How does image quality compare between fluoroscopy and ultrasound?
Fluoroscopy is great for bones and some soft tissues. Ultrasound is better for soft tissues, tendons, and nerves. It also offers real-time images.
Are ultrasound-guided procedures more accurate than fluoroscopy-guided procedures?
Both have their own strengths. Ultrasound is very accurate for soft tissue work. Fluoroscopy is better for bones and some vascular work.
What are the safety considerations for patients undergoing fluoroscopy-guided procedures?
Patients get exposed to radiation. It’s important to keep doses low for their safety.
Can ultrasound be used for vascular access procedures?
Yes, ultrasound is used for vascular access. It’s safe and offers real-time images.
How do the costs of fluoroscopy and ultrasound equipment compare?
Ultrasound equipment is cheaper than fluoroscopy. Ultrasound also has lower maintenance costs.
What are the future trends in image-guided procedures?
Future trends include artificial intelligence and hybrid technologies. These will make procedures safer and more accurate.
What is the role of ultrasound modalities in interventional procedures?
Ultrasound modalities like Doppler and elastography are key. They help see tissues and blood flow in real-time.
How do procedural times compare between fluoroscopy-guided and ultrasound-guided procedures?
Times vary by procedure and patient. But ultrasound is often faster because of its real-time images.
What are the training requirements for healthcare providers using fluoroscopy and ultrasound guidance?
Providers need special training in both. They must learn to interpret images and place needles accurately.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK546144/























