disc disease surgery
Did you know that degenerative disc disease affects millions worldwide, causing significant pain and discomfort? This condition occurs when the spinal discs lose their cushioning ability, leading to a range of symptoms.
We understand that chronic back pain can be debilitating. When conservative treatments fail, spinal disc surgery becomes a viable option. In this article, we’ll explore the various surgical procedures available for treating degenerative disc disease.
Key Takeaways
- Degenerative disc disease is a common condition causing chronic pain.
- Surgical options are considered when conservative treatments fail.
- Various surgical procedures are available, each with its benefits.
- Understanding the surgical options can help patients make informed decisions.
- Recovery processes vary depending on the surgical procedure.
Understanding Degenerative Disc Disease
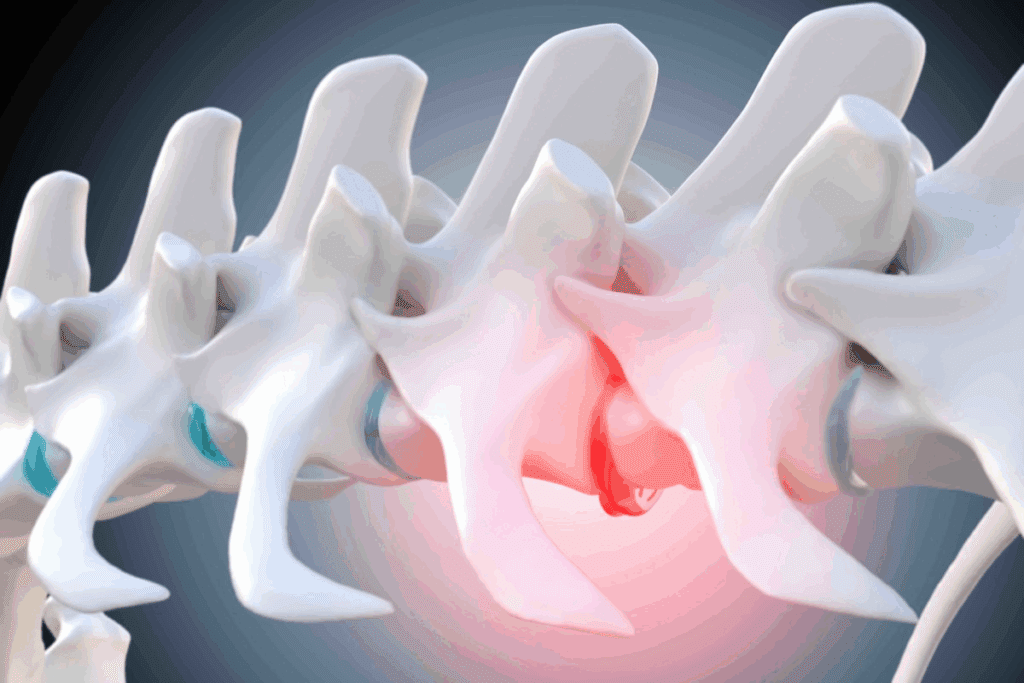
degenerative disc disease
Understanding degenerative disc disease is key for those with chronic back pain. This condition affects the spinal discs. These discs cushion the vertebrae and help with smooth spinal movement.
What Happens to Discs as They Degenerate
As we age, our spinal discs naturally degenerate. This means they lose water, becoming less flexible and more likely to get damaged. The outer layer can crack, letting the softer inside bulge out and irritate nerves.
Disc degeneration is a natural part of aging. But, injuries, lifestyle choices, or genetics can speed it up. As discs degenerate, they can cause pain, inflammation, and nerve compression. This can really affect our daily lives.
Common Symptoms and Progression
Symptoms of degenerative disc disease vary. People often experience chronic back pain, stiffness, and less mobility. Sometimes, it can lead to herniated discs, where the disc material bulges into the spinal canal. This can compress nerves and cause pain, numbness, or weakness in the limbs.
The disease can progress slowly, with periods of less pain. Knowing how it progresses and managing symptoms is crucial for a good quality of life.
When Surgery Becomes Necessary
disc disease surgery
When other treatments don’t work, surgery might be needed for degenerative disc disease. Doctors decide on surgery after checking the patient’s condition and how symptoms affect their life.
Failed Conservative Treatments
First, doctors try non-surgical treatments like physical therapy and medicine. But if these don’t help, surgery is considered. Failed back surgery syndrome shows why choosing the right patient for surgery is key.
Neurological Symptoms
Neurological symptoms like numbness or weakness mean nerves might be affected. Surgery is needed to ease this pressure and prevent more damage. Prompt surgical treatment can greatly help those with severe symptoms.
Quality of Life Considerations
How much degenerative disc disease affects a person’s life is important. If pain and limited mobility make daily tasks hard, surgery might be an option. Options like spinal fusion surgery or disc replacement can help restore function and ease pain.
| Factors Influencing Surgical Decision | Description | Impact on Treatment |
| Failed Conservative Treatments | Inability of non-surgical treatments to provide relief | Indicates need for surgical intervention |
| Neurological Symptoms | Presence of numbness, tingling, or weakness | May require prompt surgical relief |
| Quality of Life | Impact on daily activities and well-being | Influences decision for surgical options like spinal fusion |
Disc Disease Surgery: An Overview
disc disease surgery
Disc disease surgery includes many procedures to help with pain and improve spinal function. If other treatments don’t work, surgery might be needed. This is especially true for those with degenerative disc disease.
Goals of Surgical Intervention
The main goals of surgery for degenerative disc disease are to ease pain, stabilize the spine, and improve function. Surgery aims to fix the main problem, like a herniated disc or spinal stenosis.
We want to make the patient’s life better, so they can do things they love without pain. The type of surgery depends on how bad the disc is, the symptoms, and the patient’s health.
Evaluating Surgical Candidacy
To decide if surgery is right, we look at a patient’s medical history, symptoms, and imaging results. We consider how bad the symptoms are, how they affect daily life, and what treatments have been tried before. This helps us decide if surgery is the best choice.
People with serious nerve problems, a lot of pain, or trouble doing everyday things are often good candidates for surgery. A detailed check-up helps us find the best surgery for each person.
Preoperative Assessment Process
The preoperative assessment is key before surgery. It includes tests and checks to make sure the patient is ready. This includes looking at medical history, doing physical exams, and reviewing imaging like MRI or CT scans.
Patients might also have blood tests or heart checks if needed. This process helps us make a surgery plan that fits the patient’s needs, improving the chances of success.
Discectomy Procedure Explained
discectomy procedure
The discectomy procedure removes damaged disc material that presses on spinal nerves. It’s often chosen when other treatments don’t work for degenerative disc disease.
Traditional vs. Microdiscectomy
There are two main ways to do a discectomy: traditional and microdiscectomy. Traditional discectomy uses a big incision. Microdiscectomy, on the other hand, uses a small incision and a microscope to cause less damage.
Microdiscectomy is more popular because it’s less invasive. It leads to less pain after surgery and faster recovery. Research shows it can also mean shorter hospital stays and quicker return to daily activities.
Endoscopic Discectomy Advances
Endoscopic discectomy is a newer, less invasive spine surgery method. It uses a thin tube with a camera to see the disc and nerves through a small cut.
This method has many benefits. It causes less damage, less pain after surgery, and quicker recovery. Its popularity is growing because of its potential for better results and faster healing.
Recovery Expectations
Recovery from discectomy surgery depends on the method and the patient. Most people will feel some pain and discomfort after surgery. This can be managed with medicine.
| Surgical Technique | Recovery Time | Postoperative Pain Level |
| Traditional Discectomy | 6-8 weeks | Moderate to High |
| Microdiscectomy | 2-4 weeks | Low to Moderate |
| Endoscopic Discectomy | 1-3 weeks | Low |
Knowing the differences in these methods and their recovery times helps patients make better choices about their treatment.
Spinal Fusion Surgery Techniques
spinal fusion surgery
The goal of spinal fusion surgery is to join two or more vertebrae together. This makes the spine stable and reduces pain. It’s often chosen for those with degenerative disc disease who haven’t seen relief from other treatments.
How Fusion Stabilizes the Spine
Spinal fusion removes the damaged disc and replaces it with a bone graft. This graft fuses with the vertebrae over time. This process stops the spine from moving abnormally, which causes pain.
Using advanced imaging, we place the bone graft accurately. We watch how the fusion goes. Success depends on the patient’s health, how severe their condition is, and following post-op instructions.
Bone Graft Options and Substitutes
Bone grafts are key in spinal fusion. There are autografts (from the patient), allografts (donated), and synthetic grafts. Each has its benefits and is chosen based on the patient’s needs and the surgeon’s preference.
- Autografts: These are the best because they fuse faster and are less likely to be rejected.
- Allografts: Useful when a lot of graft is needed or if the patient can’t give their own.
- Synthetic grafts: Made to act like natural bone, often used with other grafts.
Fusion with Instrumentation
Fusion with instrumentation uses rods, screws, and plates for extra stability. These devices help keep the spine aligned and improve fusion success.
We pick the right instrumentation for each patient’s needs. Using these tools has made spinal fusion more successful.
Artificial Disc Replacement Alternatives
artificial disc replacement
Artificial disc replacement is now a good option for those who don’t want fusion surgery. This surgery replaces a damaged disc with a new one. It helps keep the spine moving naturally.
Disc Implant Technology Advancements
New technology has improved disc implants a lot. Now, there are many designs and materials. These include titanium and polyethylene, which are strong and safe for the body.
Candidacy Requirements
Not everyone with a bad disc can get this surgery. Doctors look at how bad the disc is, other spine problems, and the patient’s health.
Advantages Over Fusion
This surgery keeps the spine moving, unlike fusion. It also might prevent other parts of the spine from getting worse. This makes it a better choice for some people.
| Criteria | Artificial Disc Replacement | Spinal Fusion |
| Preservation of Spinal Motion | Preserves natural motion | Eliminates motion at the fused segment |
| Risk of Adjacent Segment Disease | Potentially lower risk | Higher risk due to increased stress on adjacent discs |
| Recovery Time | Generally shorter recovery | Longer recovery period due to bone graft healing |
| Surgical Complexity | More complex due to precise placement of prosthetic disc | Complex due to need for bone grafting and instrumentation |
Minimally Invasive Spine Surgery Options
minimally invasive spine surgery
Minimally invasive spine surgery is a new way to treat degenerative disc disease. It’s gentler than traditional surgery. This method uses new technology to cause less damage, reduce pain, and speed up healing.
Benefits of Smaller Incisions
Smaller incisions are a big plus in minimally invasive spine surgery. They cause less tissue trauma, which means less pain after surgery. Patients can get back to their daily lives faster.
These small cuts also mean less scarring. Plus, the chance of infection is lower. This is a big win for patients.
Computer-Assisted Navigation
Computer-assisted navigation is key to successful minimally invasive spine surgery. It gives surgeons real-time images and feedback. This helps them place instruments and implants more accurately.
This technology is a big step forward. It lets surgeons do complex surgeries with more confidence. This leads to better results for patients.
Reduced Tissue Trauma Advantages
Less tissue damage is a major benefit of minimally invasive spine surgery. It lowers the risk of complications and helps healing happen faster. Patients also feel less pain because of the smaller cuts.
Keeping tissues and muscles intact also helps maintain spinal stability. This is crucial for long-term health and recovery.
Laminectomy and Decompression Procedures
Decompression surgery, like laminectomy, aims to ease pressure on the spinal cord or nerves. It does this by making the spinal canal bigger. This surgery is key for those with severe spinal stenosis or degenerative disc disease.
Spinal Canal Enlargement Benefits
The main goal of laminectomy and decompression is to make the spinal canal bigger. This helps relieve pressure on the spinal cord or nerves. It can greatly improve a patient’s life by reducing pain, enhancing mobility, and improving overall quality of life.
By removing parts of the vertebrae or other structures, we can decompress the area. This not only eases symptoms but also stops further damage to the nerves.
Combined Decompression Approaches
In some cases, a mix of procedures is needed for the best results. This might include discectomy or foraminal decompression, based on the patient’s specific needs.
Our surgeons carefully look at each patient’s situation to find the best treatment. They make sure all factors causing compression are addressed.
Stability Considerations
When doing laminectomy and decompression, keeping the spine stable is key. Sometimes, extra steps are needed to prevent instability after surgery.
We use advanced tools and methods to check the spine’s stability. This helps us decide if fusion surgery or other methods are needed to keep the spine healthy long-term.
| Procedure | Benefits | Stability Considerations |
| Laminectomy | Relieves pressure on spinal cord or nerves | Potential for post-operative instability |
| Decompression Surgery | Enlarges spinal canal, reducing symptoms | May require additional stabilization measures |
| Combined Approach | Addresses multiple compressing factors | Careful evaluation necessary to prevent instability |
Region-Specific Surgical Approaches
Each part of the spine needs its own special surgery for degenerative disc disease. The spine is complex, with different areas needing different treatments. This is because each part of the spine works in its own way.
Cervical Disc Surgery Techniques
Cervical disc surgery is for the neck. It’s tricky because of the spinal cord and nerves nearby. The anterior cervical discectomy and fusion (ACDF) is a common method. It removes the bad disc from the front and fuses the vertebrae together.
The posterior cervical laminoforaminotomy is another option. It removes part of the lamina to ease nerve pressure. The choice depends on where the disc problem is and the patient’s spine.
- Key considerations for cervical disc surgery:
- Keeping the spine stable
- Protecting nerves
- Freeing up nerves
Lumbar Disc Surgery Considerations
Lumbar disc surgery is for the lower back. It’s a common surgery for degenerative disc disease. The surgery depends on how bad the symptoms are and how much the disc has degenerated.
Microdiscectomy is a small, less invasive surgery for the lower back. It uses a small cut and a microscope to remove the bad disc. This method tries to cause less damage and help the patient recover faster.
- Looking at how bad the symptoms are
- Checking the disc and spine for other problems
- Thinking about the patient’s health and if they can have surgery
Thoracic Disc Surgery Challenges
Thoracic disc surgery is hard because of the rib cage and the stable thoracic spine. Getting to the thoracic discs can be tough. Sometimes, a costotransversectomy or a thoracotomy is needed to reach the spine.
Thoracic disc surgery needs a very skilled team and careful planning before surgery. MRI and CT scans are key for understanding the spine and planning the surgery.
Preparing for Spine Surgery
To get the best results from your spine surgery, you need to prepare well. This means taking several important steps. We’ll guide you through what to do and how to get ready.
Medical Clearance Requirements
Getting medical clearance is a key step before spine surgery. It means checking your health to see if there are any risks. Your doctors will work together to make sure you’re ready for the surgery.
Clearance might include tests like blood work and imaging studies. These help us understand your health and make sure the surgery is safe for you.
| Test/Evaluation | Purpose |
| Blood Work | To check for infections, bleeding disorders, or other conditions that could affect surgery |
| Imaging Studies | To confirm the diagnosis and plan the surgical approach |
| Cardiovascular Evaluations | To assess heart health and identify any potential cardiovascular risks |
Medication Adjustments
We’ll look at your medications to see if any need to be changed. Some drugs, like blood thinners, might be stopped to avoid bleeding. It’s important to follow our advice on medications.
We’ll also talk about any supplements or over-the-counter drugs you’re taking. Our goal is to reduce risks and improve your surgery outcome.
Home Preparation Essentials
Getting your home ready is also key. You’ll need a comfy spot to rest without hurting your back. Make sure important things are easy to reach to avoid moving too much.
Having someone help with daily tasks and errands is also helpful. We can give you tips on what to expect and how to prepare for recovery.
- Set up a comfortable recovery area
- Have essential items within easy reach
- Arrange for assistance with daily tasks
By following these steps and working with your healthcare team, you can have a successful spine surgery experience.
The Day of Surgery Experience
The day of spine surgery can be scary, but knowing what to expect helps. We know that being informed can ease your worries. It’s important to know what’s going to happen.
Anesthesia Considerations
Anesthesia is a big part of the surgery day. Our team will talk to you about the best anesthesia for your surgery. This could be general anesthesia or something more local, to keep you comfortable.
The right anesthesia depends on:
- The type of spine surgery you’re having
- Your health and medical history
- What your surgical team thinks is best
Surgical Duration Expectations
The surgery time can vary a lot. It depends on how complex the surgery is and your specific case. Spine surgeries can take anywhere from a few hours to several hours.
Things that affect surgery time include:
- The surgical technique used
- How many levels are being treated
- If other procedures are being done at the same time
Immediate Post-Operative Care
After surgery, you’ll go to the recovery room. Our team will watch over you closely. We focus on your comfort and safety during this important time.
Post-operative care includes:
- Checking your vital signs and managing pain
- Checking your nerves to make sure everything is okay
- Teaching you about care after you go home and follow-up visits
By understanding these parts of the surgery day, we hope to lessen your anxiety. Our team is committed to giving you the best care during your spine surgery.
Recovery and Rehabilitation Timeline
The journey to full recovery after spine surgery is a planned process. Knowing what to expect can make recovery better and more successful.
Hospital Stay Duration
The time spent in the hospital after spine surgery varies. It depends on the surgery’s complexity and the patient’s health. Usually, patients stay for 1 to 3 days. During this time, doctors watch over the patient, manage pain, and start the first steps of recovery.
Physical Therapy Protocols
Physical therapy is key in spine surgery recovery. It helps regain strength, improve flexibility, and enhance spine function. Physical therapy starts a few weeks after surgery and goes on for weeks or months, based on progress.
Physical therapy includes:
- Gentle exercises to improve mobility
- Strengthening exercises for the back and core muscles
- Posture correction and body mechanics education
- Progressive aerobic activities
Return to Activities Milestones
Getting back to normal activities after spine surgery is a slow process. Patients are told to avoid heavy lifting, bending, or twisting for weeks. The time to get back to activities varies, but most reach big milestones in 6 to 12 weeks. Getting back to hard activities or sports can take several months.
Important milestones include:
- Starting light household tasks in 2-4 weeks
- Increasing activity levels over 6-12 weeks
- Going back to hard activities or work in 3-6 months
It’s crucial for patients to follow their surgeon’s advice and go to follow-up appointments. This ensures a smooth and effective recovery.
Potential Risks and Complications
Spine surgery, like any surgery, has its own risks and complications. We aim to give the best results, but it’s key for patients to know these risks. This helps them make informed choices about their care.
Common Surgical Risks
Common risks include infection, bleeding, and reactions to anesthesia. Infection is a risk in any surgery, and we take strict precautions. Bleeding can happen during or after surgery, and we watch patients closely to fix any problems quickly.
Nerve damage and dural tears are also risks. Nerve damage can cause numbness, weakness, or pain. Dural tears can lead to CSF leaks. These are rare but important to know about.
Procedure-Specific Complications
Each spine surgery has its own risks. For example, discectomy can lead to disc herniation or incomplete removal. Spinal fusion can result in nonunion or pseudarthrosis, where the bone doesn’t fuse right.
Artificial disc replacement risks include wear and tear, loosening, or migration of the implant. Knowing these risks helps manage patient expectations and outcomes.
Long-Term Adjacent Segment Issues
Spine surgery can lead to long-term issues like adjacent segment disease. This happens when the spinal segments near the surgery area degenerate, causing new symptoms. Not all patients will face this, but it’s a concern for long-term spinal health.
We closely monitor our patients’ spinal health after surgery. If new issues arise, we address them quickly. This might include more treatments or interventions to manage symptoms and keep the spine stable.
Choosing the Right Surgeon and Facility
Choosing a skilled surgeon and a reputable facility is key for surgery success. This choice greatly affects the surgery’s outcome and your experience.
Surgeon Qualifications to Consider
When looking at a surgeon’s qualifications, several factors are important. We seek surgeons with lots of experience in spinal surgery, especially for degenerative disc disease. It’s crucial they are board certified in orthopedic or neurosurgery, showing they meet high standards.
We also look at the surgeon’s past performance. This includes their complication rates and how happy patients are. A surgeon with a good track record and many successful surgeries is best.
- Board certification in orthopedic surgery or neurosurgery
- Experience with spinal surgery procedures
- Low complication rates
- High patient satisfaction scores
Hospital Quality Metrics
The quality of the hospital or surgical facility is as important as the surgeon’s skills. We check various metrics to judge a facility’s quality. These include infection rates, patient safety, and how happy patients are.
| Quality Metric | Description | Importance |
| Infection Rates | Percentage of patients who develop infections during their stay | High |
| Patient Safety Indicators | Measures of how well a hospital prevents medical errors and complications | High |
| Patient Satisfaction Scores | Feedback from patients on their care experience | Medium |
Questions to Ask Before Committing
Before deciding, ask surgeons and their teams several questions. These questions help understand their approach, experience, and care level.
- What experience do you have with this specific procedure?
- Can you share your complication rates and patient satisfaction scores?
- What is your approach to pain management and rehabilitation?
- How will you ensure continuity of care after the surgery?
By carefully evaluating these factors and asking the right questions, patients can make informed decisions. This leads to better outcomes.
Conclusion
Degenerative disc disease is a complex condition that needs a detailed treatment plan. When other treatments don’t work, surgery might be needed. We’ve looked at different surgeries for disc disease, like discectomy, spinal fusion, and artificial disc replacement.
It’s important to know the good and bad sides of these surgeries. This helps patients make smart choices. They should think about how bad their symptoms are, their health, and their lifestyle.
In the end, surgery can really help people with degenerative disc disease. It can make their lives better. We suggest talking to a doctor to figure out the best treatment.
FAQ
What is degenerative disc disease, and how is it treated surgically?
Degenerative disc disease happens when spinal discs lose their cushioning. This causes pain and discomfort. Treatments include discectomy, spinal fusion, and artificial disc replacement.
What are the benefits of minimally invasive spine surgery?
Minimally invasive spine surgery has many benefits. It uses smaller incisions and causes less tissue damage. This leads to less pain after surgery and a quicker recovery.
How is candidacy determined for artificial disc replacement surgery?
To qualify for artificial disc replacement, several factors are considered. These include the severity of disc degeneration and overall health. Certain medical conditions also play a role.
What is the role of physical therapy in spine surgery recovery?
Physical therapy is key in spine surgery recovery. It helps patients regain strength and flexibility. It also improves range of motion.
What are the potential risks and complications associated with spinal fusion surgery?
Spinal fusion surgery carries risks like infection and nerve damage. There’s also a chance of adjacent segment disease.
How long does it take to recover from a discectomy procedure?
Recovery from a discectomy varies. Most people can get back to normal in a few weeks.
What are the advantages of computer-assisted navigation in spine surgery?
Computer-assisted navigation makes spine surgery safer and more accurate. It allows for precise placement of instruments. This reduces the risk of complications.
Can degenerative disc disease be treated without surgery?
Yes, degenerative disc disease can be treated without surgery. This includes physical therapy, pain management, and lifestyle changes.
What are the differences between cervical, lumbar, and thoracic disc surgery?
Disc surgery varies by spine region. Cervical surgery is for the neck, lumbar for the lower back, and thoracic for the mid-back.
How is the success of spine surgery measured?
Success in spine surgery is measured by pain relief, improved function, and patient satisfaction.
What are the long-term implications of spinal fusion surgery?
Spinal fusion can lead to long-term issues like adjacent segment disease. This is when vertebrae near the fusion site degenerate over time.
Are there alternative treatments to spinal fusion surgery?
Yes, alternatives to spinal fusion include artificial disc replacement. This aims to preserve spinal motion and reduce the risk of adjacent segment disease.
References
- Zigler, J., Sachs, B. L., Rashbaum, R. F., et al. (2017). Comparison of lumbar total disc replacement with lumbar fusion: a systematic review and meta-analysis. https://pmc.ncbi.nlm.nih.gov/articles/PMC6022955/




































