Many people wonder if they can handle diverticulitis by themselves. New research shows that self-care can work for mild cases.
Studies show that up to 90-95% of mild diverticulitis can be treated at home. This supports the idea that some cases don’t need hospital care.
We’ll look into how to manage diverticulitis symptoms at home. This includes making lifestyle changes and using antibiotics when needed.
Key Takeaways
- Outpatient management is effective for up to 90-95% of uncomplicated diverticulitis cases.
- Lifestyle adjustments play a critical role in managing symptoms.
- Oral antibiotics or no antibiotics can be safe for select patients.
- Self-care is a viable option for mild cases.
- Knowing when to seek medical help is key.
What Is Diverticulitis and How Does It Develop?
Diverticulitis is a complication of diverticular disease. It happens when diverticula, small pouches in the colon, get inflamed. This condition ranges from mild diverticulosis to severe diverticulitis.
The Anatomy of Diverticular Disease
Diverticula are small pouches in the colon’s wall. They mostly appear in the sigmoid colon, the lower part. A low fiber diet can cause constipation and increase pressure in the colon.
The colon’s muscles can weaken over time. This allows diverticula to form. While they’re not usually a problem, they show changes in the colon.
The Progression from Diverticulosis to Diverticulitis
Diverticulosis means having diverticula without symptoms or inflammation. But, when they get inflamed, it’s called diverticulitis. Several factors can lead to this change, including:
- Increased pressure within the colon
- Low fiber diet
- Obesity
- Physical inactivity
- Smoking
Diverticulitis causes symptoms like abdominal pain, changes in bowel habits, and fever. Knowing these factors helps manage diverticulitis better.
|
Condition |
Description |
Symptoms |
|---|---|---|
|
Diverticulosis |
Presence of diverticula without inflammation |
Often asymptomatic |
|
Diverticulitis |
Inflammation of diverticula |
Abdominal pain, changes in bowel habits, fever |
Recognizing Diverticulitis Symptoms
It’s important to know the signs of diverticulitis to tell it apart from other stomach problems. Symptoms of diverticulitis can really affect a person’s life. Spotting them early is key to managing the condition well.
Common Signs of a Diverticulitis Flare-Up
When diverticulitis flares up, people often notice several symptoms. The main signs include:
- Abdominal pain, usually on the lower left side
- Fever, which means there’s an infection
- Nausea and changes in bowel habits, like constipation or diarrhea
- Bloating and discomfort in the belly
These symptoms can be different in how bad they are. They might start suddenly or slowly over time.
How Diverticulitis Pain Differs from Other Digestive Issues
Diverticulitis pain is usually constant and in the lower left abdomen. It’s more severe than pain from other stomach problems, like IBS. It often comes with fever and other infection signs.
|
Symptom |
Diverticulitis |
IBS |
|---|---|---|
|
Pain Location |
Typically lower left abdomen |
Variable, often lower abdomen |
|
Fever |
Common during flare-ups |
Rare |
|
Nausea and Vomiting |
Frequent |
Less common |
|
Bowel Habits |
Changes in bowel habits |
Alternating constipation and diarrhea |
Knowing these differences helps patients get the right diagnosis and treatment. If you think you might have diverticulitis, see a doctor right away.
Uncomplicated vs. Complicated Diverticulitis
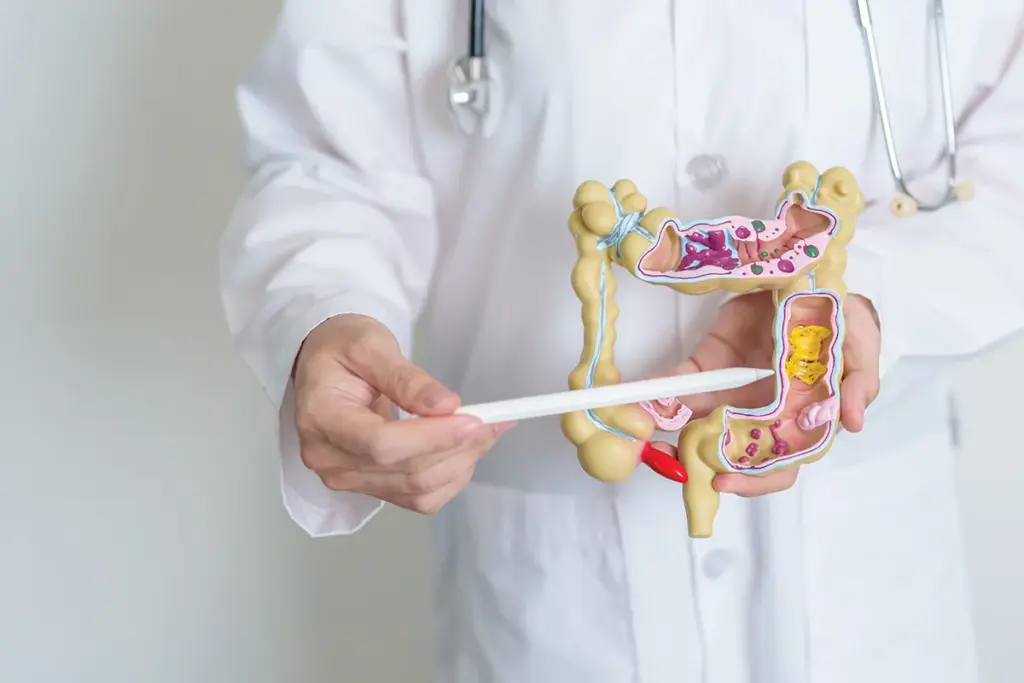
It’s important to know the difference between uncomplicated and complicated diverticulitis. This helps decide the right treatment. Diverticulitis is when the diverticula in the gut get inflamed. It can be mild or severe.
Defining Uncomplicated Diverticulitis Cases
Uncomplicated diverticulitis means the inflammation is not too bad, and there are no big problems. People with this usually have belly pain, changes in bowel movements, and maybe a fever. Getting it treated early can stop it from getting worse.
Treating uncomplicated diverticulitis often means making diet changes, drinking lots of water, and sometimes antibiotics. This depends on how bad it is and the patient’s health.
Complications That Require Medical Intervention
Complicated diverticulitis is when the inflammation is worse. It can cause abscesses, holes in the gut, serious infections, or a lot of bleeding. These cases need quick medical help, often in the hospital. They might need surgery.
It’s key to spot the signs of complicated diverticulitis. Look out for severe belly pain, high fever, signs of sepsis, or a lot of bleeding. These mean it’s not just a simple case and needs urgent care.
The Evidence Supporting Self-Management
Research shows that self-management is effective in treating diverticulitis. Studies prove that most uncomplicated cases can be treated outside the hospital.
Outpatient Success Rates
90-95% of uncomplicated diverticulitis cases can be managed at home. This means most patients don’t need to stay in the hospital. A study on shows how well outpatient treatment works for diverticulitis.
Antibiotic vs. Non-Antibiotic Approaches
New studies look at using antibiotics for diverticulitis. They found that non-antibiotic treatments can work as well for some patients. This change is important because it lowers the risk of antibiotic resistance and side effects.
The main points from recent studies are:
- Outpatient treatment works for 90-95% of uncomplicated cases.
- Non-antibiotic treatments are promising, reducing antibiotic use.
- Picking the right patients is key for successful self-management.
These findings support self-management as a good treatment option for diverticulitis. As research grows, we’ll see better ways to treat patients safely and effectively.
Who Should Not Attempt Self-Treatment
Not everyone with diverticulitis can safely treat themselves at home. Some need immediate medical care. While many can manage their condition at home, some face risks that require professional help.
Immunocompromised Patients and Special Considerations
People with weakened immune systems are at higher risk. This includes those on chemotherapy, organ transplant recipients, and those with HIV/AIDS. Their bodies struggle to fight off infections, which can lead to serious problems if not treated properly.
Immunocompromised patients should always consult their healthcare provider before attempting self-treatment for diverticulitis. They might need stronger treatments, like hospital care, to manage their condition well.
Signs of Sepsis or Severe Infection
Some patients with diverticulitis may show signs of sepsis or severe infection. These are serious conditions that need immediate medical help. Symptoms that mean you need urgent care include:
- High fever above 101.5°F (38.6°C)
- Severe abdominal pain
- Vomiting or inability to keep fluids down
- Blood in the stool or black, tarry stools
- Confusion or altered mental state
- Rapid heart rate
If you or someone you know has these symptoms, get emergency medical care right away. Prompt treatment can greatly improve outcomes in these critical situations.
It’s important to know the risks of treating diverticulitis on your own. By knowing who should not try self-treatment, we can make sure those at higher risk get the medical care they need. This helps prevent serious complications.
Diverticulitis Treatment Options for Home Care
Diverticulitis treatment is changing, with more focus on home care for some patients. This change comes from new knowledge about the condition and better treatment methods.
Evolving Approach to Antibiotics
How we use antibiotics for diverticulitis is being rethought. Studies show not all patients need antibiotics, mainly those with mild cases. are being explored, aiming to use fewer antibiotics and their risks.
We’re moving towards treatments tailored to each patient. Decisions on antibiotics depend on symptom severity, health, and more. Research backs the idea that many can heal without antibiotics.
|
Criteria |
Antibiotic Treatment |
Non-Antibiotic Management |
|---|---|---|
|
Severity of Symptoms |
Severe symptoms may require antibiotics |
Mild symptoms can often be managed without antibiotics |
|
Patient Health Status |
Immunocompromised patients may require antibiotics |
Healthy individuals might not need antibiotics |
Non-Antibiotic Management Strategies
There are key non-antibiotic ways to manage diverticulitis at home. These include changing your diet, staying hydrated, and resting.
Dietary Adjustments: Start with a clear liquid diet to ease bowel rest. Then, move to a low-fiber diet before going back to normal or high-fiber to avoid future issues.
Hydration: Drinking enough water helps prevent constipation and aids in healing.
Using these non-antibiotic strategies can help manage symptoms and aid in recovery at home.
The Diverticulitis Diet Plan During Acute Flare-Ups
Choosing the right foods is key when you have diverticulitis. Eating the right way can help ease symptoms and aid in recovery. We’ll cover the diet plan, starting with clear liquids and then moving to low-fiber foods as you get better.
What to Eat With Diverticulitis: The Clear Liquid Phase
At first, a clear liquid diet is often suggested to calm your digestive system. This step is vital for managing symptoms and preventing complications. Clear liquids include:
- Water
- Clear broths (chicken or vegetable)
- Electrolyte-rich beverages (sports drinks)
- Clear juices (apple or grape)
- Gelatin
Transitioning to Low-Fiber Foods
When symptoms start to fade, you can start adding low-fiber foods to your diet. This step is important for managing symptoms and getting the nutrients you need. Low-fiber foods include:
- Cooked pasta and rice
- White bread
- Lean proteins (chicken, fish)
- Canned fruits and vegetables
- Low-fiber cereals
Start with small amounts of these foods to see how your body reacts. This helps avoid any irritation.
A key principle is to listen to your body. If a new food makes symptoms worse, go back to clear liquids for a bit.
“The dietary management of diverticulitis involves a careful balance between giving the digestive system rest and providing necessary nutrients for recovery.”
By sticking to this diet, people with diverticulitis can better handle their symptoms during flare-ups. It also helps with overall recovery.
How to Relieve Diverticulitis Pain Fast
Managing diverticulitis pain is key for comfort and recovery. This pain can really affect someone’s life, making it important to find good ways to ease it.
Safe Over-the-Counter Pain Management
OTC pain meds can help a lot with diverticulitis pain. Acetaminophen is often the first choice because it works well and is safe. But, it’s important to only take the amount suggested to avoid side effects. Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can also help, but they might upset your stomach.
Always talk to a doctor before taking OTC pain meds, if you have stomach issues or take other meds. It’s best to get advice from your doctor to make sure you’re treating your pain safely and effectively.
Heat Therapy and Comfort Measures
Heat therapy is also helpful for diverticulitis pain. Using a heating pad on the painful area can relax muscles and lessen pain. Also, lying down with your knees bent can help ease tension in your stomach.
Drinking lots of clear liquids helps keep you hydrated and prevents constipation, which can put pressure on the diverticula. Resting and not doing too much can also help you recover and feel better. By using these methods together, you can manage your pain and feel more comfortable during a flare-up.
Natural Remedies for Diverticulitis Relief
Along with traditional treatments, natural remedies can help with diverticulitis. Many people use these methods to manage their symptoms and improve their gut health. We will look at herbal remedies and probiotics that support digestive health.
Evidence-Based Herbal Approaches
Some herbal remedies may help with diverticulitis symptoms. For example, peppermint oil can reduce abdominal pain and discomfort. It has anti-inflammatory properties. Another herb, turmeric, contains curcumin, which also has anti-inflammatory effects.
A study in the Journal of Ethnopharmacology showed that curcumin can reduce symptoms of irritable bowel syndrome (IBS). IBS and diverticulitis share some symptoms. This suggests that herbal remedies might be helpful.
Probiotics and Gut Health Support
Probiotics are live bacteria and yeasts that are good for gut health. They help keep the gut microbiome healthy, which is important for digestion. Research shows that probiotics can reduce diverticulitis symptoms by improving gut motility and reducing inflammation.
|
Probiotic Strain |
Potential Benefits |
|---|---|
|
Lactobacillus acidophilus |
Improves gut motility, reduces symptoms of IBS |
|
Bifidobacterium lactis |
Enhances immune function, reduces inflammation |
|
Streptococcus thermophilus |
Supports gut barrier function, improves digestion |
When picking a probiotic supplement, look for one with multiple strains and a high CFU count. Always talk to a healthcare provider before starting any new supplements.
Using natural remedies like herbal approaches and probiotics can help with diverticulitis symptoms. But, it’s important to work with your healthcare provider to make sure these treatments fit with your overall plan.
Rest and Lifestyle Adjustments During Recovery
Rest and making lifestyle changes are key to getting better from diverticulitis. Getting enough rest and changing your lifestyle can really help your body heal and feel better.
Physical Activity Guidelines During a Flare-Up
When you’re having a diverticulitis flare-up, finding the right balance is important. You should avoid too much exercise, but gentle activities like walking can help keep your bowels moving and your health up.
Gentle exercises to consider:
- Short walks
- Light stretching
- Breathing exercises
Always listen to your body and stop any activity that hurts or feels wrong.
Stress Management Techniques for Gut Health
Stress can really hurt your gut health and make diverticulitis symptoms worse. Using stress management techniques can help you recover and feel better overall.
Effective stress management techniques include:
- Meditation and mindfulness practices
- Yoga
- Deep breathing exercises
- Progressive muscle relaxation
These methods not only reduce stress but also help keep your gut healthy.
By adding rest, the right amount of physical activity, and stress management to your recovery plan, you can help your body heal faster. This will also improve your overall quality of life.
Monitoring Your Condition at Home
Managing diverticulitis at home is as important as following your treatment plan. By monitoring your condition, you can spot changes in symptoms early. This can help prevent complications and improve your health.
Daily Symptom Assessment Tools
To track your diverticulitis, use tools to monitor your symptoms every day. You can:
- Keep a symptom journal to record pain, bowel movements, and other symptoms
- Use mobile apps for tracking digestive health
- Note any changes in your condition or how you’re responding to treatment
These tools help you give your healthcare provider detailed information. This information can help them tailor your treatment to your needs.
Warning Signs That Treatment Is Failing
It’s important to know the signs that your treatment might not be working. Look out for:
- Increasing or severe abdominal pain
- Fever above 101°F (38.3°C)
- Vomiting or trouble keeping fluids down
- Blood in the stool or black, tarry stools
- Signs of dehydration, like excessive thirst, dark urine, or dizziness
If you notice any of these symptoms, get medical help right away. Quick action can prevent serious problems.
|
Symptom |
Action |
|---|---|
|
Mild abdominal pain |
Continue with prescribed treatment, monitor closely |
|
Severe abdominal pain |
Seek immediate medical attention |
|
Fever below 101°F |
Continue treatment, monitor temperature |
|
Fever above 101°F |
Contact healthcare provider |
a gastroenterologist, says, “Being vigilant is key in managing diverticulitis. By knowing your symptoms and warning signs, you can help your recovery.”
Preventing Future Diverticulitis Flare-Ups
To avoid future diverticulitis flare-ups, it’s important to focus on diet and lifestyle. Making smart choices can lower the chance of getting sick again. This can also make life better overall.
Long-Term Dietary Modifications
Eating a high-fiber diet is key to preventing diverticulitis. Foods high in fiber help keep your bowels regular and stop diverticula from forming. Good fiber sources include:
- Fruits such as berries, apples, and bananas
- Vegetables like broccoli, carrots, and leafy greens
- Whole grains, including brown rice, quinoa, and whole-wheat bread
- Legumes, such as beans, lentils, and peas
It’s also wise to limit or avoid certain foods that might make symptoms worse. These include processed meats, spicy foods, and high-fat dairy products.
Lifestyle Changes for Diverticulitis Management
Besides diet, making lifestyle changes can help manage diverticulitis. Regular physical activity is vital for regular bowel movements and better gut health. Drinking plenty of water is also important.
Other lifestyle changes that help include:
- Managing stress through techniques like meditation or deep breathing
- Avoiding smoking and limiting alcohol consumption
- Maintaining a healthy weight to reduce pressure on the digestive system
By making these dietary and lifestyle changes, you can greatly lower your risk of future diverticulitis episodes.
Creating Your Diverticulitis Self-Care Action Plan
Creating a detailed self-care plan is key to managing diverticulitis well. It helps you act fast and right when your condition changes. This can lower the chance of serious problems.
Preparing for Possible Episodes
To get ready for diverticulitis episodes, follow some important steps. Know the early signs of a flare-up, like changes in bowel habits, stomach pain, or fever. Having a clear liquid diet ready can help manage symptoms during an episode. Here’s what we recommend:
- Keep clear liquids like broth, electrolyte-rich drinks, and water on hand.
- Have over-the-counter pain relief options ready, as your doctor suggests.
- Keep a symptom journal to track when and how symptoms start and grow.
Communication Strategies with Healthcare Team
Talking well with your healthcare team is key to managing diverticulitis. We suggest:
- Regular check-ins with your healthcare provider to talk about your condition and any changes.
- Inform your healthcare team about your symptoms, treatment, and any worries.
- Ask questions and get clear on any part of your care you don’t get.
By using these strategies and keeping communication open, you can work well with your healthcare team to manage diverticulitis.
When Surgery Becomes Necessary for Diverticulitis
Most diverticulitis cases don’t need surgery. But, some complications might require it. Knowing when surgery is needed is key for patients.
Indications for Surgical Intervention
About 2-5% of diverticulitis cases need surgery. This is usually because of complications like abscesses or perforations. These issues can be serious if not treated quickly.
Here are when surgery might be needed:
- When other treatments don’t work.
- If abscesses or perforations happen.
- For those with many episodes of diverticulitis.
Types of Surgical Procedures for Diverticulitis
There are different surgeries for diverticulitis, each with its own use. The right surgery depends on the case’s complexity and the patient’s health.
|
Surgical Procedure |
Description |
Indications |
|---|---|---|
|
Bowel Resection |
Removing the bad part of the colon. |
Recurring diverticulitis, abscesses, or perforations. |
|
Laparoscopic Surgery |
Using small cuts for surgery. |
Simple diverticulitis needing surgery. |
|
Emergency Surgery |
Quick surgery for serious problems. |
Severe abscess, perforation, or sepsis. |
Knowing about these surgeries helps both patients and doctors make better choices.
Conclusion: Balancing Self-Care with Professional Medical Support
Managing diverticulitis well means finding a balance between taking care of yourself and getting help from doctors. We’ve looked at many parts of caring for diverticulitis. This includes understanding the condition, its signs, and how to care for yourself and when to see a doctor.
Combining these steps helps patients get the best results and live better lives. Taking care of yourself is key in managing diverticulitis. It lets people play a big part in their healing and stopping future problems.
But, getting help from doctors is also very important. It gives the guidance and help needed at times. We stress the need to work with doctors to make a plan that fits you.
By using both self-care and doctor’s help, people can handle diverticulitis better. They can use the strengths of both to get the best health results.
FAQ
What is diverticulitis, and how does it develop?
Diverticulitis is when the diverticula in the colon get inflamed or infected. It starts with diverticulosis, where diverticula form in the colon wall. A low fiber diet, age, and lifestyle play a role in its development.
Can I treat diverticulitis myself?
For mild cases, self-management is possible through dietary changes, adequate hydration, rest, and, when necessary, the use of antibiotics. But, if you’re immunocompromised, you should see a doctor.
What are the symptoms of a diverticulitis flare-up?
Symptoms include pain in the lower abdomen, usually on the left side, fever, nausea, and changes in bowel habits. You might also see blood in your stool. The pain can get worse over time.
How do I manage diverticulitis pain at home?
To manage pain, try over-the-counter pain relievers, heat therapy, and rest. Always follow your doctor’s advice on managing pain.
What dietary changes should I make during a diverticulitis flare-up?
Start with a clear liquid diet, then move to low-fiber foods. Avoid high-fiber, spicy, and nutty foods during a flare-up to ease symptoms.
Are there any natural remedies that can help with diverticulitis symptoms?
Some herbal remedies and probiotics might help by supporting gut health. But, talk to your doctor before adding new supplements or remedies.
How can I prevent future diverticulitis flare-ups?
To prevent flare-ups, eat a high-fiber diet, stay hydrated, exercise regularly, and manage stress. These habits can reduce your risk.
When should I seek medical help for diverticulitis?
Get medical help right away for severe pain, high fever, signs of sepsis, or if your symptoms get worse or don’t get better with self-care.
Can lifestyle changes help manage diverticulitis?
Yes, making lifestyle changes like exercising, managing stress, and eating a balanced diet can help your gut health. This might reduce how often you get diverticulitis.
What are the indications for surgery in diverticulitis?
Surgery might be needed for complicated cases, if you keep getting episodes, or if there’s a high risk of complications. The decision depends on how severe and frequent your episodes are.
How do I create a self-care action plan for diverticulitis?
Create a self-care plan by understanding your symptoms, knowing when to seek help, making dietary changes, managing stress, and preparing for episodes. Having a clear plan is key.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from
References
https://pmc.ncbi.nlm.nih.gov/articles/PMC10065882



































