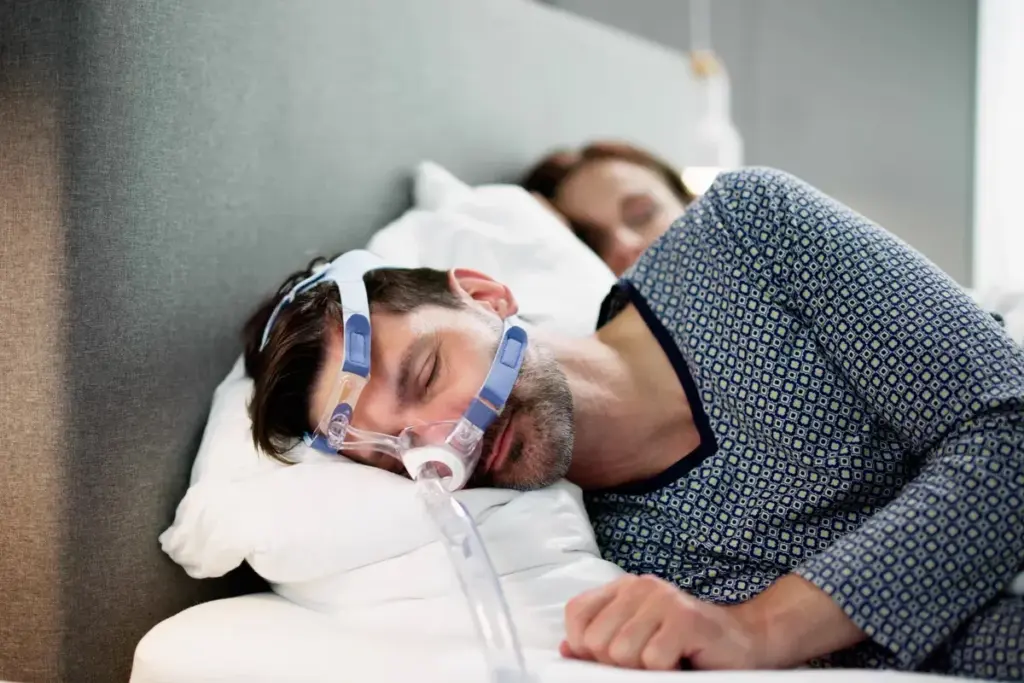
Diagnosing sleep apnea needs a detailed approach. ENT specialists lead this effort. They begin by examining symptoms such as daytime sleepiness and loud snoring. These signs can point to sleep apnea.
A detailed check-up and physical exam are key. They help decide if more tests are needed.
ENT doctors use the latest tools for diagnosis. They include and biometric analysis. These help find sleep apnea and guide treatment.
Polysomnography is the top choice. It tracks apneas and hypopneas per hour. This gives a key number called the Apnea-Hypopnea Index (AHI).
Key Takeaways
- ENT specialists diagnose sleep apnea through a combination of clinical evaluation, physical examination, and sleep study data.
- Symptoms such as daytime sleepiness and loud snoring are assessed to determine the need for further testing.
- Polysomnography is used to track apneas and hypopneas per hour, providing a critical metric for diagnosis.
- Finding the right doctor for sleep apnea treatment is essential for effective care.
- Advanced diagnostic technologies play a critical role in guiding treatment for better patient outcomes.
Understanding Sleep Apnea: Types, Symptoms, and Health Impacts
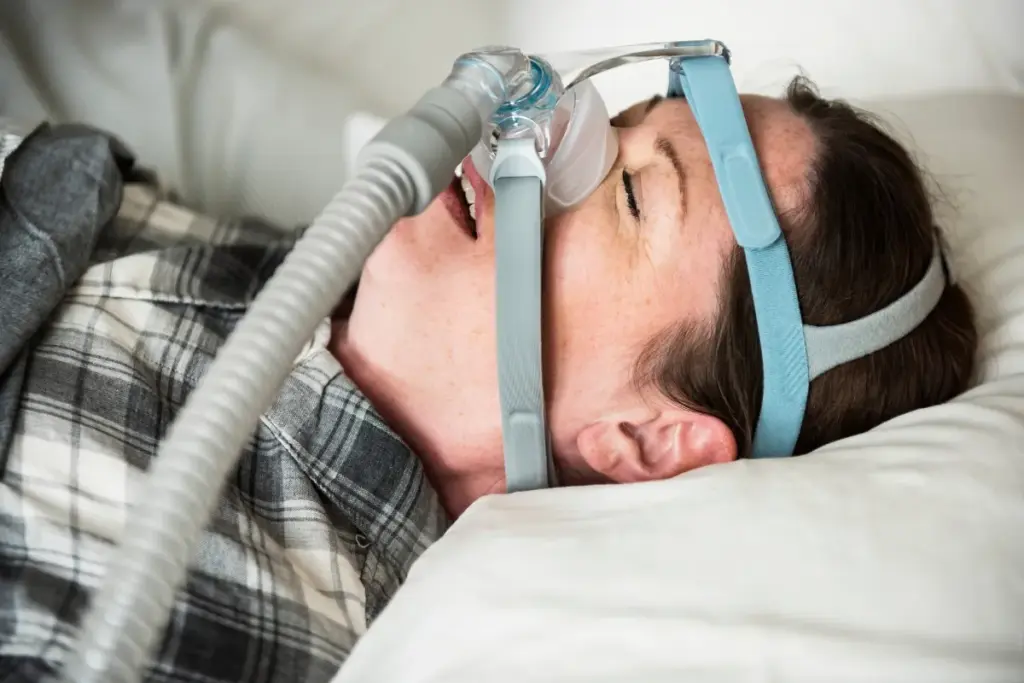
Sleep apnea is a sleep disorder that affects millions. It’s important to know its types, symptoms, and health effects. This condition causes breathing pauses or shallow breathing during sleep. If not treated, it can harm your health a lot.
Obstructive, Central, and Complex Sleep Apnea Defined
Sleep apnea has three main types: obstructive, central, and complex. Obstructive Sleep Apnea (OSA) happens when the throat muscles relax, blocking the airway. Central Sleep Apnea (CSA) is when the brain can’t send signals to breathe. Complex Sleep Apnea is a mix of OSA and CSA, making it harder to diagnose and treat.
|
Type of Sleep Apnea |
Description |
Key Characteristics |
|---|---|---|
|
Obstructive Sleep Apnea (OSA) |
Airway blockage due to relaxed throat muscles |
Common in individuals with obesity, loud snoring |
|
Central Sleep Apnea (CSA) |
Brain fails to send breathing signals |
Often associated with neurological conditions |
|
Complex Sleep Apnea |
Combination of OSA and CSA |
More challenging to diagnose and treat |
Common Symptoms and Warning Signs
It’s key to know the symptoms of sleep apnea for early treatment. Symptoms include loud snoring, stopped breathing during sleep, and waking up with a dry mouth or sore throat. Morning headaches, daytime fatigue, and feeling irritable are also signs. A sleep apnea specialist can check these symptoms to see if you have sleep apnea.
“Sleep apnea is a major risk factor for cardiovascular disease, and its diagnosis requires a thorough evaluation including sleep studies and physical examination.”
Long-term Health Consequences of Untreated Sleep Apnea
Untreated sleep apnea can lead to serious health problems. These include heart disease, diabetes, and brain problems. The breathing pauses during sleep can harm the heart and oxygen levels. A sleep apnea treatment center can help manage sleep apnea to avoid these risks.
Studies show that physical signs like a big neck, large tongue, and big tonsils can mean you’re at risk for sleep apnea. Seeing a sleep doctor for a detailed check-up is important if you have these signs.
The Role of ENT Specialists in Sleep Apnea Diagnosis

ENT specialists are key in diagnosing sleep apnea. They know a lot about the upper airway. This includes the nasal passages, throat, and ears. They are perfect for checking sleep-related breathing problems.
Why ENTs Are Uniquely Qualified for Sleep Apnea Assessment
ENT specialists, or otolaryngologists, are doctors who deal with ear, nose, and throat issues. Their specialized traininghelps them spot problems like nasal blockages or narrow airways. These can cause sleep apnea.
They are great at looking at the upper airway. This is key for diagnosing sleep apnea. They can do nasal endoscopy to see inside the nose and throat. This gives them important clues about blockages.
ENT vs. Other Sleep Specialists: Understanding the Differences
Many healthcare professionals help with sleep apnea, but ENT specialists have a special view. They look at the physical parts of sleep apnea. This often means finding and fixing structural problems.
For example, an ENT might suggest surgery to clear blockages or improve nasal airflow. On the other hand, a sleep medicine doctor might suggest non-surgical treatments like CPAP therapy. This teamwork ensures patients get the best care.
When to See an ENT for Sleep-Related Breathing Disorders
If you snore loudly, feel tired all day, or stop breathing during sleep, see an ENT. They can check your airway and suggest treatments.
Go to an ENT if other treatments haven’t worked or if you think your body’s shape is the problem. Their expertise is very helpful in these situations.
Initial Consultation: What to Expect When Visiting an ENT
When you first see an ENT specialist, they will look at your medical history and sleep habits. This first step is key to figuring out if you have sleep apnea and what treatment you might need.
Medical History Review and Sleep Questionnaires
We start by checking your medical history to see if it’s linked to your sleep apnea. You might fill out sleep questionnaires to share your sleep patterns and how bad your symptoms are.
It helps if you bring info about your medical history and sleep habits to your visit. This includes your sleep schedule, any sleep problems, and your current medications.
Discussing Your Sleep Habits and Symptoms
Talking about your sleep and symptoms with your ENT is very important. Be ready to share your sleep experiences, like paused breathing, loud snoring, or morning headaches.
Your honesty and openness are key for your ENT to understand your condition. It’s also a chance to ask questions and share any worries you have about sleep apnea.
Bringing a Sleep Partner: The Importance of Observed Symptoms
Having a sleep partner with you can give us important insights. They can tell us about your sleep, like apnea episodes or restless sleep, which helps us diagnose sleep apnea.
A sleep partner can give us a different view of your sleep habits. This helps us make a more accurate diagnosis.
Knowing what to expect at your first visit with an ENT specialist helps you talk about your sleep apnea symptoms. If you’re worried about sleep apnea, seeing a specialist is a good first step to better sleep and health.
Clinical Evaluation: How ENTs Assess Sleep Apnea Risk Factors
ENTs use a clinical evaluation to figure out if someone might have sleep apnea. They look at different factors that could lead to sleep apnea.
Evaluating Daytime Sleepiness and Fatigue Levels
Daytime sleepiness is a key sign of sleep apnea. We use the Epworth Sleepiness Scale to measure how sleepy someone is. Assessing fatigue levels is also important because it affects how well someone lives their life.
Assessing Comorbid Conditions
Sleep apnea often goes hand in hand with other health issues like high blood pressure and diabetes. We look at a patient’s medical history to find any related conditions. This helps us plan the best treatment.
Risk Factor Analysis: Age, Gender, Weight, and Family History
Some things make it more likely for someone to have sleep apnea. We look at:
- Age: Older people are more likely to have it.
- Gender: Men are more at risk than women.
- Weight: Being overweight can block the airway.
- Family History: If your family has sleep apnea, you might too.
Knowing these risk factors helps us find and help people who might have sleep apnea.
Our detailed check-ups help us spot who’s at risk for sleep apnea and find the right treatment. If you’re worried about sleep apnea, seeing a top sleep apnea doctor or a best doctor for sleep disorders is key for getting the right help.
Finding the Right Doctor for Sleep Apnea: Physical Examination Components
When you first see an ENT specialist, they do a detailed physical check-up. This check-up is key to figuring out if you might have sleep apnea. They look for any physical traits that could lead to sleep apnea.
Upper Airway Assessment Techniques
Checking the upper airway is a big part of the exam. ENT doctors use different methods to see how well your airway works. They look at your nose, mouth, and throat to find any blockages that might cause sleep apnea.
Upper airway assessment techniques include:
- Visual inspection of the nasal passages and sinuses
- Examination of the oral cavity and tongue
- Evaluation of the tonsils and adenoids
Neck Circumference Measurement and Its Significance
Measuring your neck is also important. Research shows that a bigger neck can mean a higher risk of sleep apnea. that extra fat in the neck can block the airway while you sleep.
|
Neck Circumference |
Sleep Apnea Risk |
|---|---|
|
Less than 16 inches |
Low |
|
16-17 inches |
Moderate |
|
Greater than 17 inches |
High |
Evaluation of Macroglossia and Tonsil Hypertrophy
The exam also looks at your tongue and tonsils. If they’re too big, they can block your airway. The doctor checks if these issues might be causing your sleep apnea symptoms.
Nasal Passage and Sinus Examination
Lastly, the doctor checks your nose and sinuses. Problems here can make you breathe through your mouth, raising your risk of sleep apnea.
By looking at all these things, ENT specialists can understand your sleep apnea risk. If you think you might have sleep apnea, see a board-certified sleep doctor or sleep apnea specialist. They can do a full check-up and suggest the best treatment.
Advanced Diagnostic Procedures in the ENT Office
ENT specialists use advanced tests to find sleep apnea. These tests help see if the airway is blocked. They also find the best treatment for you.
Nasal Endoscopy: Visualizing Upper Airway Obstructions
Nasal endoscopy is a key tool for ENTs. It lets them see inside the nasal cavity. They check the nasal passages, adenoids, and tonsils.
This helps them see if these areas are causing sleep apnea. It’s important for finding the right treatment.
Fiberoptic Examination of the Throat and Larynx
A fiberoptic exam gives a close look at the throat and larynx. ENTs can see how the larynx and tissues work. This helps find any problems that might cause sleep apnea.
Drug-Induced Sleep Endoscopy (DISE): When and Why It’s Used
Drug-Induced Sleep Endoscopy (DISE) is a special test. It looks at the upper airway when it’s like sleep. ENTs use a sedative to make it look like sleep.
DISE is great for complex sleep apnea cases. It helps find problems that other tests miss. It’s used when other treatments don’t work.
These tests help ENTs understand sleep apnea better. They can then create good treatment plans. If you think you have sleep apnea, see an ENT specialist. They can help you get the right treatment.
Sleep Studies: The Gold Standard for Sleep Apnea Diagnosis
Sleep studies are the top choice for diagnosing sleep apnea. They give a full view of how a person sleeps. This is key for figuring out how bad the sleep apnea is and what treatment is best.
In-Lab Polysomnography: What Happens During an Overnight Study
In-lab polysomnography (PSG) is a detailed sleep study done in a lab. It tracks brain waves, muscle activity, heart rate, and breathing while you sleep. This info helps doctors spot sleep apnea and other sleep issues.
“Polysomnography is the most accurate test for diagnosing sleep apnea,” it gives a clear look at sleep patterns. The data from PSG is very helpful for figuring out how severe sleep apnea is and what treatment to use.
Home Sleep Apnea Testing: Convenience and Limitations
Home sleep apnea testing (HSAT) lets you test for sleep apnea at home. It’s easier than PSG but not as detailed. It’s good for spotting moderate to severe sleep apnea in people who are likely to have it.
But HSAT has its downsides. It might miss other sleep problems. So, it’s best for people with clear sleep apnea symptoms and no other health issues.
Understanding the Apnea-Hypopnea Index (AHI) and Oxygen Desaturation
The Apnea-Hypopnea Index (AHI) shows how bad sleep apnea is. It counts the number of breathing pauses and shallow breaths per hour of sleep. Oxygen drops during these pauses are also important for measuring sleep apnea severity.
Knowing AHI and oxygen levels is key for diagnosing sleep apnea. A higher AHI means more severe sleep apnea, which needs stronger treatment.
Getting sleep apnea right can really improve a person’s life. Sleep studies like PSG and HSAT help doctors tailor care to each patient’s needs.
Interpreting Sleep Study Results: How ENTs Make a Diagnosis
Diagnosing sleep apnea requires a detailed look at sleep study results. ENT specialists use this data to figure out how severe the apnea is. They also decide the best treatment plan. Sleep studies show important details like breathing pauses, oxygen levels, and sleep quality.
When we look at sleep study results, we focus on a few key things. These help us understand how serious the apnea is. We use the Apnea-Hypopnea Index (AHI) to measure this. It counts the number of breathing pauses and shallow breaths per hour of sleep.
Classification of Sleep Apnea Severity Based on AHI
The AHI score helps us sort sleep apnea into different levels. Scores are usually categorized as follows: normal, mild, moderate, or severe. Accurate classification is key to finding the right treatment.
For example, someone with severe sleep apnea might need CPAP therapy. But, someone with mild apnea might just need to change their lifestyle or use oral appliances.
Distinguishing Between Different Types of Sleep Apnea
ENT specialists also need to tell apart different types of sleep apnea. There’s obstructive sleep apnea (OSA), central sleep apnea (CSA), and complex sleep apnea syndrome. OSA happens when the airway gets blocked. CSA is when the brain doesn’t tell the body to breathe.
Additional Metrics Beyond AHI That Influence Treatment Decisions
Other metrics from sleep studies also play a role in treatment choices. These include oxygen levels, how fragmented sleep is, and if there are other sleep disorders. For instance, someone with low oxygen levels might need stronger treatment to avoid heart problems.
By looking at all these factors, ENT specialists can create a treatment plan that fits each patient’s needs. This approach improves outcomes and quality of life.
Advanced Diagnostic Technologies in Sleep Apnea Assessment
Advanced diagnostic technologies are changing how we check for sleep apnea. New tools and methods help us find and treat this condition better.
Machine Learning and EEG Analysis
Machine learning, using EEG, is very good at spotting sleep apnea. Studies show it can be 95% accurate in finding sleep apnea episodes. shows how machine learning can make diagnosis more precise.
EEG looks at brain activity during sleep. Machine learning on EEG data helps doctors spot sleep apnea signs, like sleep pattern changes.
Multivariable Prediction Scores
Multivariable prediction scores are a big step forward in diagnosing sleep apnea. They mix different factors like age, gender, and BMI to guess who might have sleep apnea. This helps doctors find who’s most at risk.
These scores aren’t always 100% right, but they’re useful. They help decide who needs more tests and who should be checked first.
Imaging Studies: CT Scans and MRIs
Imaging like CT scans and MRIs is key for looking at the airway in sleep apnea patients. They show the airway’s shape, helping find where it might block.
|
Imaging Modality |
Key Features |
Clinical Utility |
|---|---|---|
|
CT Scan |
High-resolution images of bony structures |
Assesses nasal passages and sinus anatomy |
|
MRI |
Detailed soft tissue visualization |
Evaluates tongue base and upper airway morphology |
Using these advanced tools, we can better diagnose and treat sleep apnea. This leads to better health outcomes for patients.
Predictive Physical Findings for Sleep Apnea Diagnosis
When we diagnose sleep apnea, certain physical signs can help us guess if someone has it. A detailed physical check-up is key to spotting those at risk of sleep apnea.
Significance of Increased Neck Circumference
A bigger neck is a known risk for sleep apnea. A larger neck means a narrower airway, making sleep breathing harder. Research shows that every inch of neck size increase raises sleep apnea risk a lot.
Macroglossia as a Predictor
Macroglossia, or a big tongue, is another sign of sleep apnea risk. A big tongue can block the airway, causing breathing trouble at night. We check the tongue size against the mouth to see if it’s causing sleep apnea symptoms.
Tonsil Hypertrophy Assessment
Tonsil hypertrophy, or big tonsils, can also narrow the airway and lead to sleep apnea. We look at tonsil size and how it affects breathing at night. Removing tonsils might be an option if they’re too big.
Spotting these signs helps us diagnose and treat sleep apnea better. A full physical check-up, along with other tests, lets us create a treatment plan that fits each patient’s needs.
Multidisciplinary Approach: When Your ENT Works with Other Specialists
Dealing with sleep apnea needs a team effort. ENT specialists team up with other doctors to tackle this complex issue. This way, they offer complete care to their patients.
Collaboration with Sleep Medicine Physicians
Sleep medicine doctors are key in diagnosing and treating sleep disorders. They work hand in hand with ENT specialists. Together, they create treatment plans that cover all angles of sleep apnea.
Referrals to Pulmonologists, Cardiologists, and Neurologists
Patients with sleep apnea often face other health issues too. Pulmonologists help with breathing problems, while cardiologists focus on heart health. Neurologists step in when sleep apnea is linked to brain conditions.
|
Specialist |
Role in Sleep Apnea Management |
|---|---|
|
Pulmonologists |
Manage respiratory complications and provide expertise on lung function |
|
Cardiologists |
Address cardiovascular issues related to sleep apnea |
|
Neurologists |
Diagnose and treat neurological conditions associated with sleep apnea |
The Role of Dental Specialists in Sleep Apnea Management
Dental specialists, trained in sleep medicine, offer oral appliance therapy. This is a common treatment for mild to moderate sleep apnea. ENT specialists often send patients to these dental experts, showing the value of teamwork in treating sleep apnea.
When ENT specialists and other doctors work together, they can offer better care for sleep apnea patients. This teamwork leads to better health outcomes for everyone.
Treatment Planning: From Diagnosis to Management Strategy
After a thorough diagnosis, we focus on creating an effective treatment plan for sleep apnea. This plan is tailored to the individual’s specific needs. It considers the severity of their condition, lifestyle, and personal preferences.
Surgical vs. Non-Surgical Approaches
There are various options for treating sleep apnea, from surgical interventions to non-surgical therapies. The choice depends on several factors. These include the severity of sleep apnea, the patient’s overall health, and their comfort with the treatment.
Surgical options may be recommended for severe sleep apnea or when other treatments fail. These can include removing excess tissue in the throat or repositioning the jaw.
CPAP Therapy: When and How It’s Prescribed
Continuous Positive Airway Pressure (CPAP) therapy is a common treatment for sleep apnea. It involves wearing a mask over the nose and/or mouth during sleep. This delivers a steady stream of pressurized air to keep the airway open.
CPAP is often prescribed for patients with moderate to severe sleep apnea. The pressure settings are determined through a sleep study. This ensures the most effective treatment.
|
CPAP Benefits |
CPAP Limitations |
|---|---|
|
Effective in reducing apnea episodes |
Can be uncomfortable to wear |
|
Improves sleep quality |
Requires regular maintenance |
|
Reduces daytime fatigue |
Can be noisy |
Oral Appliances and Positional Therapy Options
For patients with mild to moderate sleep apnea, oral appliances can be an effective treatment. These custom-made devices advance the position of the lower jaw. This keeps the airway open during sleep.
Positional therapy is another option. It involves using a device to encourage sleeping on the side. This reduces the likelihood of airway obstruction.
Lifestyle Modifications and Weight Management
Lifestyle changes play a key role in managing sleep apnea. Weight loss is often recommended for overweight patients. Excess weight can contribute to sleep apnea.
Other lifestyle modifications include avoiding alcohol and sedatives before bedtime. Adopting a regular sleep schedule and engaging in regular physical activity are also important.
By combining these approaches, we can develop a treatment plan that addresses each patient’s unique needs. This improves their quality of life and reduces the risks associated with sleep apnea.
Conclusion: The Importance of Proper Sleep Apnea Diagnosis and Treatment
Getting sleep apnea diagnosed and treated right is key to better health. If left untreated, sleep apnea can lead to serious health issues. This shows how vital it is to diagnose and treat it well.
Diagnosing sleep apnea means looking at a patient’s medical history, doing a physical check-up, and using advanced tests. Treatments like CPAP therapy, oral appliances, and changing lifestyle habits can greatly help patients. These steps can make a big difference in their quality of life.
Knowing how important it is to diagnose and treat sleep apnea helps us manage it better. This approach can lower the risk of other health problems. Accurate diagnosis and effective treatment are key to better patient outcomes and overall well-being.
FAQ
What kind of doctor treats sleep apnea?
Doctors like ENT specialists, sleep medicine physicians, and pulmonologists can help. Even primary care physicians can treat it. We work together to give you the best care.
When should I see an ENT for sleep-related breathing disorders?
See an ENT if you snore loudly, stop breathing during sleep, or feel very tired during the day. Our specialists are experts in treating these issues.
What happens during an initial consultation with an ENT specialist for sleep apnea?
We’ll talk about your health history and sleep habits. You might fill out sleep questionnaires. Bringing a sleep partner is also helpful.
How do ENT specialists diagnose sleep apnea?
We use a few methods to find out if you have sleep apnea. This includes checking you physically and using sleep studies. Our goal is to find the right treatment for you.
What is the role of sleep studies in diagnosing sleep apnea?
Sleep studies are key in diagnosing sleep apnea. They can be done in a lab or at home. These tests help us understand how severe your sleep apnea is.
How do you interpret sleep study results?
We look at things like the Apnea-Hypopnea Index (AHI) and oxygen levels. This helps us know how serious your sleep apnea is. Then, we plan the best treatment for you.
What treatment options are available for sleep apnea?
There are many ways to treat sleep apnea. Options include CPAP therapy, oral appliances, and lifestyle changes. We choose the best treatment for you based on your needs.
Can I find a sleep apnea doctor near me?
Yes, we can help you find a sleep apnea specialist near you. Our network is dedicated to helping patients with sleep apnea.
What is the importance of a multidisciplinary approach in sleep apnea management?
Working together with different doctors is important. It ensures you get the best care. This team effort helps us find the best treatment for you.
How can I prepare for a sleep study?
To get ready for a sleep study, stick to your usual sleep schedule. Avoid caffeine and heavy meals beforehand. Follow any instructions from our team for accurate results.
Are there any new technologies being used in sleep apnea diagnosis?
Yes, we use new technologies like machine learning and imaging studies. These tools help us diagnose and treat sleep apnea better.
References:
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/19960649/



































