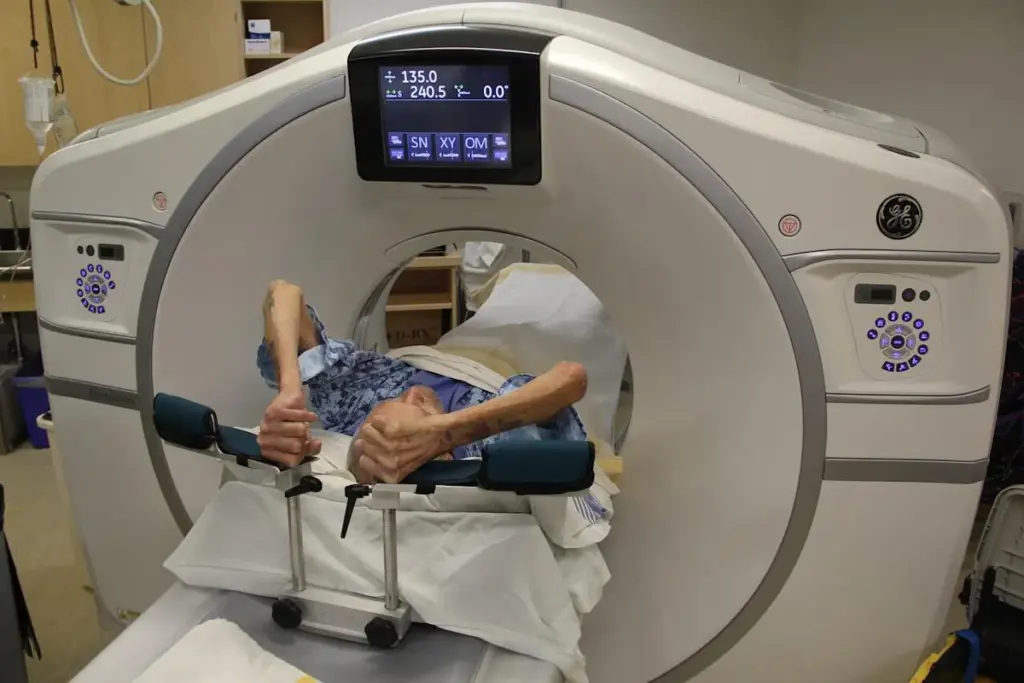
Cancer detection has become more advanced with new medical technology. Early detection of cancer is crucial for effective treatment strategies. Now, there are many ways to spot cancer before symptoms show up. Does a ct scan detect tumors effectively? Learn about amazing and vital tools that provide a perfect and fast diagnosis for you.
The best scan for cancer detection varies by cancer type and location. New breakthroughs include Multi-Cancer Early Detection (MCED) blood tests. These tests have shown great promise in finding different cancers early.
Cancer screening has evolved, giving us many options for early detection. It’s important to know the different cancer detection methods and cancer screening techniques. This knowledge helps us make better health choices.
Key Takeaways
- Early cancer detection improves treatment outcomes.
- MCED blood tests are a significant advancement in cancer detection.
- The best cancer screening method depends on the cancer type and location.
- Various cancer detection methods are now available.
- Cancer screening can identify cancer before symptoms appear.
The Critical Importance of Early Cancer Detection
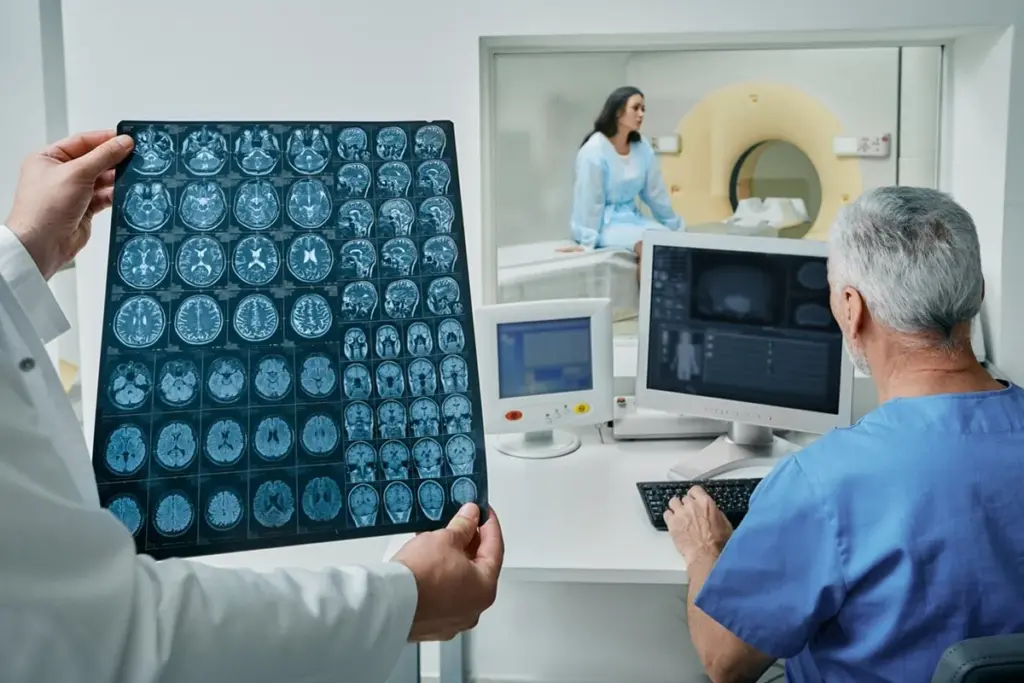
Early detection is key to effective cancer treatment. It greatly improves patient outcomes. Finding cancer early means more treatment options and a better chance of recovery.
How Early Detection Impacts Survival Rates
Research shows early detection boosts survival rates for many cancers. For example, women with early-stage breast cancer have a nearly 99% five-year survival rate. This is much higher than the 28% rate for those diagnosed later. This highlights the critical role of early detection in cancer treatment.
“The earlier cancer is detected, the more effective treatment is likely to be, leading to improved survival rates and quality of life for patients.”
Early detection also means less invasive treatments. At an early stage, treatments like surgery or localized radiation might be enough. This reduces the need for harsher treatments like chemotherapy.
The Evolution of Cancer Screening Technologies
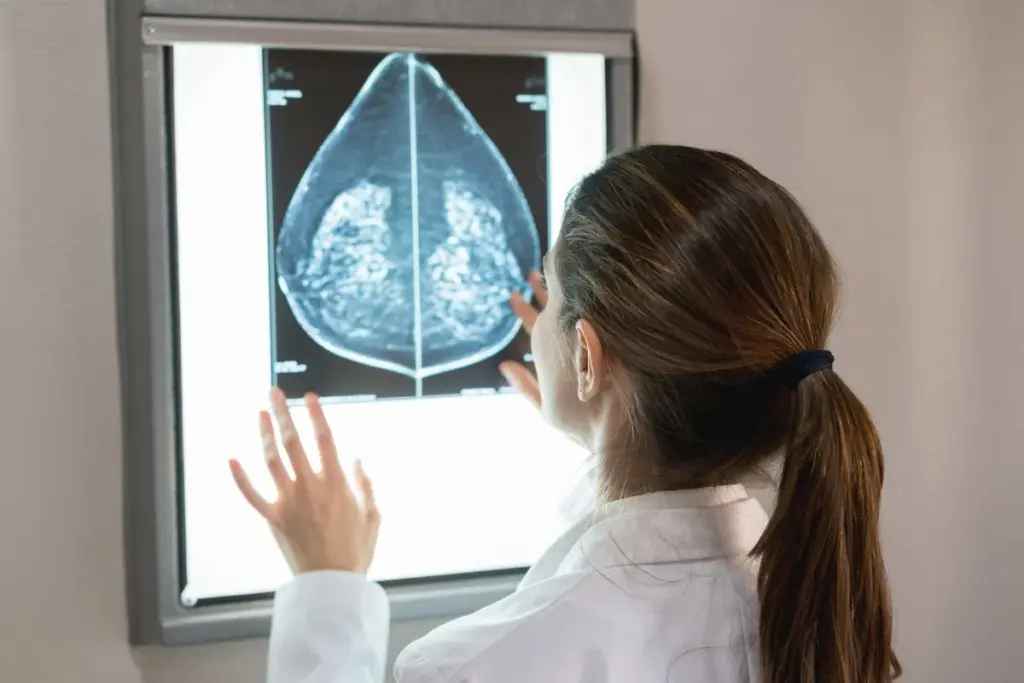
Cancer screening has made big strides, helping us catch cancer early. New imaging tech, like digital mammography and low-dose CT scans, boosts detection rates. They also cut down on radiation exposure.
|
Screening Technology |
Improvement |
Impact on Detection |
|---|---|---|
|
Digital Mammography |
Enhanced image quality |
Improved detection of breast cancer in dense tissue |
|
Low-Dose CT Scans |
Reduced radiation exposure |
Safer screening for high-risk populations |
|
Liquid Biopsy |
Non-invasive genetic analysis |
Potential for early detection of multiple cancer types |
New screening tech is on the horizon. Research into multi-cancer early detection tests is promising. These advancements could lead to even better early detection and outcomes for patients.
Does a CT Scan Detect Tumors? Capabilities and Limitations
CT scans are used to find tumors, but their strengths and weaknesses are not always clear. They use X-rays to show detailed images inside the body. Doctors can see tumors and other issues with these images.
How CT Scans Visualize Abnormal Tissue
CT scans are great at showing certain abnormal tissues, like tumors. They work by checking how much X-rays different tissues absorb. Tumors usually have different density than healthy tissue, making them stand out on scans.
Tumor visualization gets better with contrast agents. These substances absorb X-rays differently than normal tissue. This helps doctors tell apart different tumors and other issues.
Types of Tumors Most Effectively Detected by CT
CT scans are good at finding many tumor types. They work best on tumors that are big enough and have clear density differences. Some examples include:
- Lung tumors, because they are denser than lung tissue
- Liver tumors, which contrast agents help show
- Pancreatic tumors, which are hard to spot but can be seen with contrast
Finding these tumors early can greatly improve treatment and outcomes.
Situations Where CT Scans May Miss Tumors
Even though CT scans are useful, they’re not perfect. They might miss small tumors or those that blend in with the surrounding tissue. Tumors in hard-to-reach places, like the brain, can also be tricky to spot.
In some cases, other scans like MRI or PET might be needed. They can help find tumors that CT scans can’t see.
CT Scan Accuracy and Reliability for Cancer Detection
CT scans are key in finding cancer, but their accuracy depends on many things. How well CT scans spot tumors is vital for choosing the right treatment and knowing how a patient will do.
Sensitivity and Specificity Rates in Different Cancer Types
The success of CT scans in finding cancer is shown by their sensitivity and specificity. Sensitivity is when CT scans correctly find people with cancer. Specificity is when they correctly find people without cancer.
CT scans work differently for each cancer type. For example:
- Lung cancer: CT scans are very good at finding lung nodules and tumors, mainly in people at high risk.
- Colorectal cancer: CT scans can spot bigger tumors but might miss smaller ones or flat ones.
- Liver cancer: CT scans are good at finding liver tumors, better with contrast agents.
Research shows CT scans’ sensitivity for cancer detection can be between 70% and over 90%. But specificity can change based on things like benign lesions or inflammation.
Factors That Influence CT Scan Accuracy
Many things can change how accurate CT scans are in finding cancer:
- Technological advancements: Newer CT scanners with better algorithms and higher resolution help find more.
- Contrast agents: Contrast agents make tumors stand out, helping in some cancer types.
- Patient factors: Size, staying calm during the scan, and other patient factors can affect image quality.
- Radiologist expertise: The radiologist’s skill and experience greatly affect how well they spot tumors.
A study in a top radiology journal says, “The accuracy of CT scans in cancer detection is complex. It depends on technology and the doctor’s skill.”
“Using advanced imaging like CT scans in cancer screening has changed how we find and treat cancer early.”
Knowing these factors helps make CT scans better for finding cancer and understanding the results.
Comparing CT Scans to MRI for Cancer Detection
When it comes to finding cancer, doctors often use CT scans and MRI. Both are key tools, but they work in different ways.
Tissue Differentiation Capabilities
MRI is great at showing soft tissues clearly. This is key for spotting tumors and where they are.
CT scans, on the other hand, are better for bones and lungs. They can spot soft tissue issues, but not as well as MRI.
- MRI is top-notch for soft tissue, perfect for brain and spine tumors.
- CT scans are quicker and easier to get, great for emergencies and first checks.
Cancer Types Better Visualized by MRI
Some cancers are easier to see with MRI because of its soft tissue detail. These include:
- Brain tumors, where MRI shows tumor edges and swelling.
- Spinal tumors, where MRI is key for seeing how far the tumor goes and if it’s pressing on the spinal cord.
- Soft tissue sarcomas, where MRI helps see how the tumor relates to nearby tissues.
When Doctors Choose MRI Over CT
Doctors might choose MRI over CT for several reasons. This includes when they need to see soft tissues clearly or if the patient can’t have CT contrast.
MRI’s ability to show tissue without radiation is a big plus. It’s good for patients who need many scans or are worried about radiation.
The choice between CT and MRI depends on the situation, the cancer type, and the patient’s needs.
PET Scans and Nuclear Medicine in Cancer Diagnosis
PET scans have changed how we diagnose cancer. They detect metabolic activity in tumors. This method is key in nuclear medicine, helping doctors diagnose, stage, and plan treatments for cancer.
Detecting Metabolic Activity in Tumors
PET scans use a radioactive glucose analogue, like Fluorodeoxyglucose (FDG), which cancer cells take up. The PET scanner then shows where this FDG is in the body. This helps find tumors by their activity, not just size or location.
Key benefits of PET scans include:
- High sensitivity for detecting metabolically active tumors
- Ability to stage cancer and assess its spread
- Monitoring response to treatment
Benefits of Combined PET-CT Imaging
Using PET scans with CT imaging (PET-CT) gives a better view. It combines metabolic info from PET scans with detailed anatomy from CT scans. This combo makes cancer diagnosis, staging, and treatment planning more accurate.
|
Imaging Modality |
Primary Information |
Clinical Benefit |
|---|---|---|
|
PET Scan |
Metabolic Activity |
Detects active tumors, assesses treatment response |
|
CT Scan |
Anatomical Detail |
Provides structural information, aids in precise localization |
|
PET-CT |
Combined Metabolic and Anatomical Information |
Enhances diagnostic accuracy, improves treatment planning |
Experts say, “The integration of PET and CT imaging has significantly improved the diagnostic workup of cancer patients, providing a more complete understanding of the disease.” (
)
PET scans, when used with CT imaging, are a big step forward in cancer diagnosis and care. They give detailed metabolic info, helping doctors make better decisions for their patients.
Mammography: The Gold Standard for Breast Cancer Detection
Mammography is key in finding breast cancer early. It helps doctors spot tumors that are too small to feel. This is a big help in treating cancer before it spreads.
Studies show mammography works well in finding breast cancer. New tech, like 3D mammography, has made it even better.
2D vs 3D Mammography Effectiveness
2D mammography shows a flat image of the breast. It’s good but not perfect, mainly for women with dense breasts. 3D mammography takes pictures from different sides. This gives a 3D view that helps doctors see better.
Research shows 3D mammography finds more cancers in dense breasts. It’s more accurate, which means fewer false alarms and less need for more tests.
Supplemental Screening for Dense Breast Tissue
Women with dense breasts might need extra tests. These could be ultrasound or breast MRI. The right test depends on the woman’s risk and breast type.
It’s important for women to talk to their doctors about what’s best for them. Using mammography with other tests can catch cancer early. This makes treatment more likely to work.
Colonoscopy and Next-Generation Stool DNA Tests
Colonoscopy has been the top choice for finding colorectal cancer for a long time. But, new stool DNA tests are becoming a great option too. This part looks at how well both work to find colorectal cancer.
Detection Capabilities of Traditional Colonoscopy
Colonoscopy lets doctors see the colon and rectum directly. This helps find and take out polyps that could turn into cancer. It’s very good at catching cancer early, which helps people live longer.
Key benefits of colonoscopy include:
- Direct visualization of the colon
- Ability to remove precancerous polyps during the procedure
- High detection rate for colorectal cancer
The 95% Detection Rate of Next-Gen Stool DNA Tests
Next-generation stool DNA tests are a big step forward in finding cancer without invasive tests. They look for DNA from cancer cells or big polyps in the stool.
Studies have shown these tests can find colorectal cancer about 95% of the time. This makes them a good choice for people who don’t want to have a colonoscopy.
|
Screening Method |
Sensitivity |
Invasiveness |
|---|---|---|
|
Colonoscopy |
High |
Invasive |
|
Next-Gen Stool DNA Tests |
95% |
Non-Invasive |
Both colonoscopy and next-generation stool DNA tests are key in finding colorectal cancer early. Colonoscopy lets doctors see and remove polyps directly. Next-gen stool DNA tests are non-invasive but very sensitive.
Low-Dose CT Scanning for Lung Cancer Screening
Early detection of lung cancer through low-dose CT scanning has shown promising results in reducing mortality rates. Lung cancer is a leading cause of cancer-related deaths worldwide. Early diagnosis is critical for improving survival chances.
USPSTF Recommendations for High-Risk Individuals
The United States Preventive Services Task Force (USPSTF) recommends annual lung cancer screening with low-dose CT scans. This is for adults aged 50 to 80 years. They must have a 20 pack-year smoking history and currently smoke or have quit within the past 15 years. This guideline aims to identify lung cancer at an early stage when it is more treatable.
Key eligibility criteria for low-dose CT lung cancer screening include:
- Age between 50 and 80 years
- A 20 pack-year smoking history
- Current smoking status or having quit within the last 15 years
Detection Accuracy and Mortality Reduction
Studies have shown that low-dose CT screening can detect lung cancer at an early stage. This significantly improves the chances of successful treatment. The National Lung Screening Trial (NLST) found a 20% reduction in lung cancer mortality among high-risk individuals screened with low-dose CT compared to those receiving standard chest X-rays.
Balancing Benefits Against Radiation Exposure
While low-dose CT scans involve exposure to a small amount of radiation, the benefits of screening for high-risk individuals outweigh the risks. Modern CT scanners are designed to minimize radiation exposure while maintaining image quality. It’s essential for patients and healthcare providers to discuss the risks and benefits to make informed decisions about lung cancer screening.
Cervical Cancer Detection: Pap Smears and HPV Testing
Pap smears and HPV testing have changed how we find cervical cancer early. These tests have cut down on cervical cancer cases and deaths.
Combined Testing Approaches and Their Effectiveness
Using both Pap smears and HPV testing is very good at catching cervical cancer early. This way, doctors can check cervical health more thoroughly.
Benefits of Combined Testing:
- More precancerous lesions are found
- HPV types that are high-risk are spotted more accurately
- Early treatment leads to better patient results
A study in the Journal of the American Medical Association (JAMA) showed that Pap smears and HPV testing together find cervical cancer better than Pap smears alone.
“The addition of HPV testing to Pap smear screening substantially improves the detection of cervical precancer and cancer.”
Screening Interval Recommendations
How often you should get screened for cervical cancer depends on your age, risk factors, and past test results. Here are some guidelines:
|
Age Group |
Recommended Screening Interval |
|---|---|
|
21-29 years |
Pap smear every 3 years |
|
30-65 years |
Pap smear and HPV testing every 5 years or Pap smear alone every 3 years |
Future Directions in Cervical Cancer Screening
New technologies and research are leading to better and less painful ways to screen for cervical cancer. We’re looking at more sensitive HPV tests and maybe even self-testing.
As we keep moving forward, we expect to see even better ways to find and prevent cervical cancer.
Revolutionary Multi-Cancer Early Detection Blood Tests
MCED blood tests are a big step forward in finding cancer early. They can spot many types of cancer from just one blood sample. This changes how we find and treat cancer.
How MCED Tests Identify Cancer Signals
MCED tests look for special signs or biomarkers in the blood linked to cancer. These signs can be DNA, proteins, or other molecules. They might come from cancer cells or the body’s reaction to cancer.
The tests use cutting-edge genomic and proteomic tech to find these biomarkers. This lets us catch cancer early, often before symptoms show up.
The 79% Early-Stage Cancer Detection Rate
Research shows MCED tests can find early-stage cancers with about 79% accuracy. Finding cancer early is key for better treatment and survival chances.
Early detection also means less need for invasive tests. It can lead to milder treatments.
False Positive Minimization Strategies
Any cancer screening test faces the challenge of false positives. These can cause worry and extra tests.
MCED tests aim to cut down on false positives. They use smart algorithms to check biomarker data against many criteria.
- Advanced data analysis techniques
- Validation against multiple biomarkers
- Continuous updating of the test’s algorithm based on new data
By reducing false positives, MCED tests give more accurate results. This helps make sure those with cancer get the right treatment. It also spares those without cancer from unnecessary stress and tests.
Patient Awareness and Acceptance of New Cancer Tests
Patient awareness and acceptance are key to using new cancer screening technologies like MCED tests. As these new methods become more common, it’s important to understand what patients think. This helps in getting more people to use them.
The Willingness Rate for MCED Testing
Studies show many patients are open to MCED testing. In fact, a study found a 75% willingness rate among those tested. This shows a good attitude towards new cancer screening ways.
Why do patients want to try MCED tests? They see the benefits of catching cancer early and like that the tests are non-invasive. Patients are taking charge of their health, and MCED tests are a good way to do that.
Barriers to Adoption of New Screening Methods
Even with a high willingness rate, there are challenges to using new tests. These include:
- Lack of awareness about new screening technologies
- Concerns about the accuracy and reliability of new tests
- Costs for patients
- How easy it is to get these new tests
It’s important to tackle these challenges to get more people to use MCED tests and other new cancer screening methods.
Educational Initiatives for Increased Awareness
Educational efforts are vital to overcome these challenges. By teaching patients and doctors about new cancer screening methods, we help them make better choices.
|
Educational Initiative |
Description |
Impact |
|---|---|---|
|
Public Awareness Campaigns |
Using media and community events to teach about MCED tests |
More people know about and use MCED tests |
|
Healthcare Provider Training |
Teaching doctors the latest on new cancer screening technologies |
Doctors can better advise and support patients |
|
Patient Education Materials |
Creating easy-to-understand materials for patients |
Patients can make informed decisions |
With these educational efforts, we can connect patients with the latest cancer screening technologies. This leads to better detection and outcomes for patients.
Full Body Scanning for Cancer: Benefits and Limitations
Full body scanning is a new way to find cancer. It looks at the whole body for cancer or problems. This method has grown a lot, with good and bad sides to think about.
Available Technologies for Whole-Body Assessment
Many imaging tools are used for full body scanning. Each one has its own strengths:
- Computed Tomography (CT) scans: Give detailed pictures of the body. They help find tumors and other issues.
- Magnetic Resonance Imaging (MRI): Shows soft tissues clearly. It’s great for finding some cancers.
- Positron Emission Tomography (PET) scans: Spot cancer cells by their activity. They can find cancers that other scans miss.
Appropriate Candidates for Full Body Scans
Not everyone should get a full body scan. People at high risk of cancer, like those with a family history, might benefit from it.
|
Candidate Profile |
Benefit from Full Body Scanning |
|---|---|
|
High-risk individuals (family history, genetic predisposition) |
Yes |
|
Average-risk individuals |
No |
|
Individuals with previous cancer diagnosis |
Maybe |
Concerns About Incidental Findings and Overdiagnosis
Full body scanning can find things not related to the scan’s purpose. This can cause more tests, worry, and treatments that aren’t needed.
Overdiagnosis is when cancers are found that won’t cause symptoms or harm. This can lead to too much treatment and stress for patients.
In summary, full body scanning is a detailed way to find cancer. But, we must think about its good and bad sides and who should get it.
Radiation Exposure Considerations in Cancer Imaging
Cancer diagnosis often uses imaging that exposes patients to radiation. As imaging gets better, knowing about radiation is key. It helps balance the benefits of diagnosis with the risks.
Comparative Radiation Doses Across Imaging Modalities
Each imaging method has its own radiation level. For example:
- CT scans have higher doses than regular X-rays.
- PET scans use radioactive tracers, adding to exposure.
- MRI and ultrasound don’t use harmful radiation, making them safer.
Knowing these differences helps pick the best imaging for each patient.
Cumulative Exposure Concerns for Repeated Scans
Patients getting many scans over time face higher risks. This is a big worry for:
- Young patients, as their bodies are more sensitive to radiation.
- Patients needing many scans for long-term monitoring.
Doctors must think about the risks and benefits of repeated scans. They should look for safer options when possible.
Low-Dose Protocols and Technological Improvements
New tech has brought low-dose imaging, cutting down radiation. For example:
- Low-dose CT scans are now used for lung cancer screening in high-risk groups.
- Iterative reconstruction techniques make images better with less radiation.
These advances are key for lowering radiation while keeping diagnosis quality high.
Personalized Cancer Screening Approaches
Personalized cancer screening is changing how we find cancer early. It tailors methods to each person’s risk. This makes it easier to catch cancer early, which can lead to better treatment results.
Risk Assessment Models for Customized Screening
Risk models are key in making cancer screening personal. They look at genetics, family history, and environment to guess cancer risk. This helps doctors know who needs screening the most.
Studies show that focusing on high-risk groups can save lives. For example, a study in the Journal of Clinical Oncology found that targeted breast cancer screening cuts down on deaths in high-risk women.
Genetic and Family History Factors
Genetics and family history are big in personalized screening. People with a family history of cancer or certain genes (like BRCA1 and BRCA2) might need to start screening early.
|
Cancer Type |
Genetic Factor |
Recommended Screening Age |
|---|---|---|
|
Breast Cancer |
BRCA1/BRCA2 Mutation |
25-30 years |
|
Colon Cancer |
Lynch Syndrome |
20-25 years |
|
Ovarian Cancer |
BRCA1/BRCA2 Mutation |
30-35 years |
Age-Appropriate Screening Recommendations
Age is also important in cancer screening. Guidelines suggest starting screening at different ages based on risk. For example, the USPSTF says women should start mammograms at 40.
Age-Appropriate Screening: Screening that matches age and risk helps avoid too much testing. It also improves finding cancer early.
By using risk models, genetics, family history, and age guidelines, doctors can create better screening plans. This approach helps find cancer early and reduces unnecessary treatments.
Advanced Cancer Detection at Specialized Centers
Liv Hospital leads in cancer detection, using a team effort for early diagnosis. This team includes experts from many fields, working together for complete care.
Liv Hospital’s Multidisciplinary Approach
Liv Hospital’s cancer program is a team effort. It brings together oncologists, radiologists, surgeons, and more. This multidisciplinary team creates treatment plans that fit each patient’s needs.
This teamwork leads to better diagnoses and treatments. It gives a full view of each patient’s health.
Integration of Cutting-Edge Technologies
Liv Hospital uses the latest in cancer detection tech. It has top-notch imaging and diagnostic tools for early and accurate tumor detection.
Cutting-edge technologies like advanced MRI and PET-CT scans help in precise cancer staging and monitoring. This tech is key for effective treatments.
|
Technology |
Application |
Benefit |
|---|---|---|
|
Advanced MRI |
Detailed imaging of soft tissues |
Enhanced diagnostic accuracy |
|
PET-CT Scans |
Metabolic activity assessment in tumors |
Precise staging and monitoring |
|
3D Mammography |
Early detection of breast cancer |
Improved survival rates |
International Standards and Academic Protocols
Liv Hospital follows global standards and research in cancer care. This ensures patients get top-notch care.
By sticking to international guidelines and research, Liv Hospital’s cancer programs stay up-to-date. This focus on excellence shows in their high success rates.
Conclusion: The Evolving Landscape of Cancer Detection
The way we detect cancer is changing fast, thanks to new medical tech and a better understanding of cancer. Regular screenings can save lives and cut down on healthcare costs. They have helped prevent 4.75 million cancer deaths from 1975 to 2020.
The says early detection is key to better cancer outcomes. As we keep improving, we’ll see even better ways to find cancer early. For example, blood tests that can spot cancer signals at an early stage are showing great promise.
The future of cancer screening looks bright, with more research and development on the horizon. We aim to make detection more accurate, cut down on false alarms, and improve patient care. It’s vital to keep funding cancer research and education to make sure we get the most out of these advancements.
FAQ
Can a CT scan detect cancer?
Yes, CT scans can find cancer. But, how well they work depends on the cancer type, where it is, and its size. They’re best for spotting tumors in organs like the lungs, liver, and pancreas.
How accurate are CT scans in detecting tumors?
CT scans’ accuracy varies with cancer type and scan quality. They’re very good at finding some cancers but not all.
What is the difference between a CT scan and an MRI for cancer detection?
CT scans use X-rays to show body details. MRI uses magnetic fields and radio waves. MRI is better for soft tissue tumors. CT scans are better for denser tissues.
Can a PET scan detect cancer?
Yes, PET scans can find cancer by showing where cells are very active. They’re often used with CT scans for more detailed info.
What is the role of mammography in breast cancer detection?
Mammography is key for finding breast cancer early. New technologies like 3D mammography help find cancer in dense breasts better.
How effective are colonoscopies in detecting colorectal cancer?
Colonoscopies are very good at finding colorectal cancer. They can remove polyps and early cancers. New stool DNA tests are also being used as a non-invasive option.
What are the benefits and risks of low-dose CT scanning for lung cancer screening?
Low-dose CT scans are good for those at high risk of lung cancer. They can lower death rates. But, they also expose to radiation and can have false positives.
Can full body scanning detect cancer?
Full body scans can find cancer, but it depends on the technology and risk factors. There are concerns about finding things that aren’t cancer, overdiagnosis, and radiation.
How can radiation exposure be minimized in cancer imaging?
To lower radiation, use low-dose scans and optimize settings. Choose other imaging methods when you can. New scanners also use less radiation.
What is personalized cancer screening, and how is it developed?
Personalized screening matches screening to your risk, like family history. It uses models and guidelines to create plans just for you.
What are MCED blood tests, and how do they detect cancer?
MCED blood tests look for cancer signals in the blood. They’re promising for finding cancer early, with few false positives.
References
- Centers for Disease Control and Prevention (CDC). Advances in cancer screening and early detection. https://www.cdc.gov/pcd/issues/2025/25_0139.htm
- American Association for Cancer Research (AACR). Cancer screening for early detection. https://cancerprogressreport.aacr.org/progress/cpr25-contents/cpr25-cancer-screening-for-early-detection/
- Prevent Cancer Foundation. Innovation is key in cancer screenings. https://preventcancer.org/news/innovation-key-cancer-screenings/
- National Cancer Institute (NCI). Multi-cancer early detection research. https://www.cancer.gov/research/areas/diagnosis/mced
- Harvard Health Publishing. Multi-cancer blood test: the exciting future of early cancer detection. https://www.health.harvard.edu/blog/multi-cancer-blood-test-the-exciting-future-of-early-cancer-detection-202208312799























