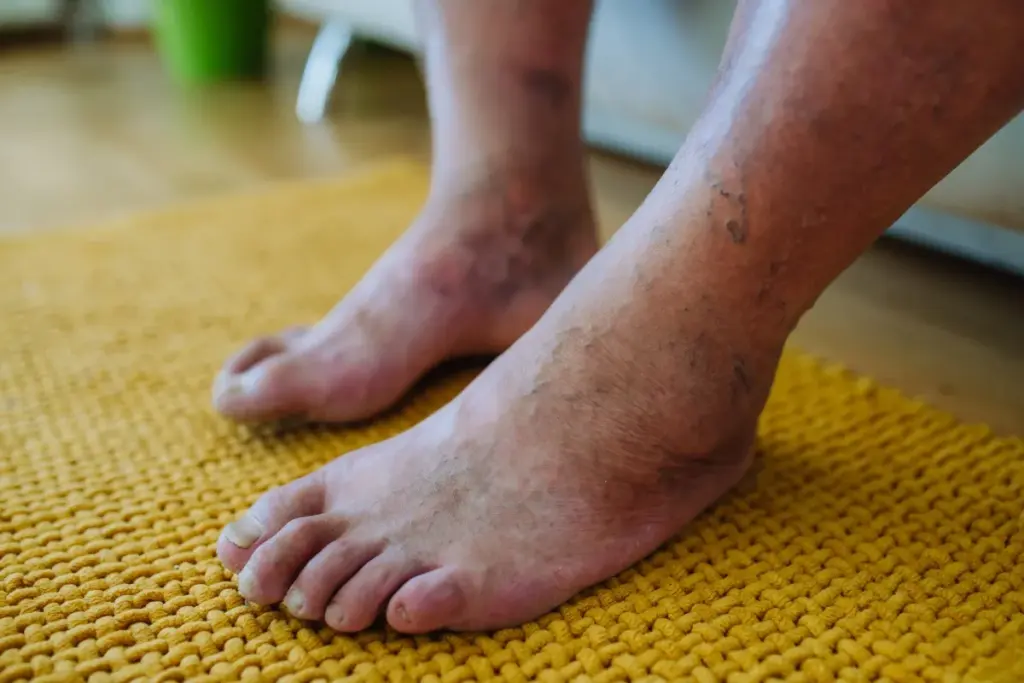
Did you know dehydration can raise your risk of Deep Vein Thrombosis (DVT)? Blood clots form in deep veins. Recent studies have shown a link between fluid levels and clot formation does dehydration cause blood clots.
Dehydration happens when we lose more fluids than we take in. It disrupts our body’s water and electrolyte balance. This can make our blood thicker, increasing clotting risk.
It’s important to understand how dehydration and DVT are connected. We’ll look at how staying hydrated can help prevent DVT and other health issues.
Key Takeaways
- Dehydration can increase the risk of developing DVT by thickening the blood.
- Maintaining proper fluid levels is essential for preventing blood clots.
- DVT is a serious condition that can lead to life-threatening complications if not addressed.
- Staying hydrated is a simple yet effective way to reduce the risk of DVT.
- Understanding the link between dehydration and DVT can help in taking preventive measures.
Understanding Dehydration: Definition, Causes, and Effects

Dehydration is a condition where the body loses more fluids than it takes in. This leads to an imbalance in water and electrolyte levels. It affects the body’s fluid balance, causing health issues.
What Constitutes Dehydration in the Body
Dehydration happens when the body doesn’t have enough fluids. This can disrupt normal body functions. Even mild dehydration can cause headaches, fatigue, and dry mouth.
It’s not just about losing water. Losing essential electrolytes like sodium, potassium, and chloride is also important. These electrolytes help with nerve and muscle function.
Common Causes of Dehydration
Dehydration can be caused by many factors. Inadequate fluid intake is a common reason. This can happen if you don’t drink enough water or if you drink fluids that don’t have electrolytes.
- Excessive sweating due to physical activity or hot weather
- Medical conditions such as diabetes, kidney disease, or gastrointestinal disorders
- Certain medications like diuretics
Understanding these causes aids in preventing dehydration and its related complications.
Physiological Effects of Dehydration
Dehydration can have severe effects on the body. It can lower blood volume and blood pressure. This makes it hard for the body to transport nutrients and oxygen to cells.
“Dehydration can lead to serious complications if not addressed promptly. It’s essential to recognize the signs and symptoms early to prevent long-term damage.”
Some effects include:
- Reduced blood volume and blood pressure
- Electrolyte imbalance
- Impaired kidney function
Understanding these effects shows why keeping hydration levels right is so important.
Deep Vein Thrombosis (DVT) Explained
Deep vein thrombosis, or DVT, is a serious condition. It happens when a blood clot forms in the deep veins. This can lead to severe problems if not treated right away.
What is DVT and How Does It Form?
DVT is when a blood clot forms in the deep veins, usually in the legs. It can happen because of being immobile, having a genetic condition, or certain health issues. When a clot forms, it blocks blood flow, causing swelling, pain, and other symptoms.
The clot forms when the blood’s clotting mechanism is triggered. This can happen due to injury, surgery, or being immobile for a long time. Knowing how DVT forms helps us find who’s at risk and how to prevent it.
Common Risk Factors for DVT Development
Several things can make you more likely to get DVT. These include:
- Prolonged immobility, such as during long-distance travel or bed rest
- Genetic predisposition, including conditions like factor V Leiden
- Certain medical conditions, such as cancer or heart disease
- Surgery or trauma, specially orthopedic surgery
- Age, with the risk increasing significantly after the age of 40
|
Risk Factor |
Description |
Prevention Strategies |
|---|---|---|
|
Immobility |
Prolonged periods of inactivity |
Regular movement, stretching exercises |
|
Genetics |
Family history of clotting disorders |
Genetic testing, anticoagulant therapy |
|
Medical Conditions |
Presence of conditions like cancer or heart disease |
Managing underlying conditions, preventive medication |
Complications of Untreated DVT
If DVT is not treated, it can cause serious problems. The biggest risk is a pulmonary embolism. This happens when a clot breaks loose and goes to the lungs, blocking blood flow.
Other problems can include post-thrombotic syndrome. This is chronic pain, swelling, and skin discoloration in the affected limb. Knowing the risks of DVT shows why quick diagnosis and treatment are so important.
The Physiology of Blood Clotting
The body’s ability to form blood clots is a delicate balance. It prevents too much bleeding and avoids unwanted clots. We will look at how blood clots normally and how dehydration can increase the risk of Deep Vein Thrombosis (DVT).
Normal Blood Clotting Mechanisms
Blood clotting is a complex process. It involves many clotting factors, which are proteins in the blood. When a blood vessel is injured, the body first constricts it to reduce blood flow.
Then, platelets stick to the injury site, forming a plug. The coagulation cascade starts, leading to fibrin formation. This stabilizes the clot.
Factors That Influence Blood Viscosity
Blood viscosity is how thick and sticky blood is. Several things can change blood viscosity, like hydration, temperature, and medical conditions. Dehydration makes blood more concentrated and thicker.
|
Clotting Factor |
Function |
|---|---|
|
Fibrinogen |
Converted to fibrin to stabilize the clot |
|
Prothrombin |
Converted to thrombin, which facilitates clot formation |
|
Platelets |
Adhere to injury sites to form a platelet plug |
Understanding blood clotting is key to knowing DVT risk, even with dehydration. Keeping hydrated and knowing what affects clotting can lower blood clot risk.
Does Dehydration Cause Blood Clots? Examining the Evidence
Medical research has looked closely at how dehydration affects blood clots. Studies have shown that dehydration might increase the risk of blood clots. It’s important to understand this link to prevent Deep Vein Thrombosis (DVT) and other health problems.
Scientific Research on Dehydration and Clotting Risk
Recent studies have found a link between dehydration and blood clots. Dehydration can make blood more likely to clot because it reduces blood volume. This concentration of blood cells and clotting factors raises the risk of clotting.
Even mild dehydration can make blood more likely to clot. A study found that dehydration increases DVT risk in hospitalized patients. This shows how important staying hydrated is, even more so for those who are more vulnerable.
Expert Medical Opinions on the Connection
Medical experts agree that dehydration can lead to blood clots. They stress the importance of staying hydrated to prevent DVT and other blood clotting issues. Leading medical experts say dehydration affects blood clotting, making it a key factor in patient care.
Experts also suggest that people at high risk of DVT, like those undergoing surgery or long-distance travelers, should drink plenty of water. By understanding how dehydration affects blood clotting, we can help patients manage their risk better through proper hydration.
How Dehydration Affects Blood Composition and Flow
Dehydration changes our blood, making it thicker and more concentrated. This can harm our heart and blood vessels.
Changes in Blood Viscosity During Dehydration
When we lose fluids, our blood gets thicker. This makes it harder for blood to move through our body. Increased blood viscosity is a significant risk factor for the development of blood clots, as it promotes the formation of thrombosis.
A study in the Journal of Clinical Rheology and Microcirculation found changes in blood viscosity. It showed that even mild dehydration can affect blood flow and increase vascular resistance.
Impact on Circulation and Vascular Function
Dehydration affects blood flow and vascular function. Our blood vessels constrict, reducing blood flow to vital organs. This can cause dizziness, fatigue, and decreased athletic performance.
Proper hydration is essential for maintaining healthy blood flow and vascular function. Drinking enough fluids helps our blood vessels dilate, improving circulation and reducing blood pressure.
|
Condition |
Blood Viscosity |
Circulation |
|---|---|---|
|
Normal Hydration |
Normal |
Optimal |
|
Dehydration |
Increased |
Reduced |
Hemoconcentration and Its Effects on Clotting
Hemoconcentration happens when we lose fluids and our red blood cells increase. This makes blood more likely to clot.
“Dehydration can lead to hemoconcentration, which increases the risk of thrombosis. It’s vital to stay hydrated, mainly in high-risk individuals, to avoid dehydration-related complications.”
To avoid clotting issues, staying hydrated is key. Drink plenty of water, and avoid caffeine and alcohol. This helps keep our hydration levels right.
High-Risk Scenarios: When Dehydration Becomes Dangerous for Clotting
Dehydration in high-risk situations can cause serious health problems, like deep vein thrombosis (DVT). Certain conditions and activities raise the risk of dehydration and clotting issues.
Long-Distance Travel and Dehydration
Traveling long distances by air, land, or sea can lead to dehydration. Prolonged sitting causes blood to pool in the legs, raising clotting risks. We suggest travelers stretch and move often and drink lots of water.
Hospitalization and Illness-Related Dehydration
Hospital patients or those with certain illnesses face higher dehydration risks. It’s vital for doctors to watch fluid levels closely to avoid dehydration and clotting issues.
Athletic Performance and Dehydration Risks
Athletes, mainly those in endurance sports, risk dehydration from sweating. Adequate hydration is key before, during, and after sports. Athletes should create a hydration plan for their needs and the environment.
Dehydration in Hot Climates and Extreme Environments
People in hot climates or extreme environments face dehydration risks. High temperatures and humidity cause more fluid loss through sweat. It’s important to drink lots of fluids and take breaks in cooler places.
Knowing these high-risk situations helps us prevent dehydration and clotting risks. Staying informed and taking steps to prevent dehydration are essential for health and safety in tough situations.
Recognizing the Warning Signs: Symptoms of Dehydration and DVT
It’s important to know the signs of dehydration and Deep Vein Thrombosis (DVT) early. This helps us get medical help fast. Knowing these symptoms can prevent serious problems and improve our health.
Early Dehydration Symptoms to Monitor
Dehydration shows itself in different ways, some of which are easy to miss. Early signs include headaches, feeling very tired, a dry mouth, and feeling dizzy. We should watch for these, more so in hot weather or when we’re very active.
If you notice these signs, it’s key to rebalance your fluid levels by drinking water or drinks with electrolytes. Not paying attention to these signs can make dehydration worse.
Severe Dehydration Warning Signs
Severe dehydration can cause serious problems, like kidney damage or even death. Warning signs include feeling very thirsty, dark urine, not making much urine, and in bad cases, seizures or losing consciousness.
If you or someone you know has these symptoms, seek medical attention right away. Quick treatment can stop long-term damage and help a lot.
DVT Symptoms That Require Medical Attention
DVT symptoms can be hard to spot but need quick medical help if they’re bad. Common symptoms are pain or swelling in the leg, redness or color change, and warmth or tenderness in the leg.
If you’re feeling these symptoms, or if you’re at risk for DVT, talk to a healthcare professional fast. Not treating DVT can lead to serious problems, like a pulmonary embolism.
Vulnerable Populations: Who’s at Greatest Risk?
Dehydration and DVT risks aren’t spread out evenly. Some groups face higher risks. Knowing who these groups are is key to preventing these issues.
Age-Related Risk Factors
Older adults are at high risk for dehydration and DVT. As we get older, our bodies change. These changes can affect how we handle fluids and blood clots.
Older people might not feel thirsty as much, move less, and have different body compositions. This makes them more likely to get dehydrated. Also, conditions like diabetes and heart disease raise their risk even more.
Medical Conditions That Increase Vulnerability
Some medical conditions make dehydration and DVT more likely. Heart failure, kidney disease, and cancer can mess with fluid balance and blood flow.
People with mobility issues, like stroke or spinal cord injury, are also at higher risk. They stay immobile for long periods. We need to act fast to prevent dehydration and DVT in these groups.
Medication Effects on Dehydration and Clotting
Some medicines can up the risk of dehydration and DVT. Diuretics, for example, can cause dehydration if not watched closely. Hormonal and chemotherapy drugs can also affect blood clotting.
People taking these meds need to know the risks. They should talk to their doctors to manage these risks. Understanding medication side effects helps reduce dehydration and DVT risks.
Dehydration and Blood Clot Risk During Travel
Traveling long distances can lead to dehydration and blood clot risks. This is true for both air and road travel. Various factors increase these risks, including Deep Vein Thrombosis (DVT).
Travel, whether by plane or car, can cause dehydration. This is because you move less and face different environments. Air travel, in particular, has dry air that speeds up dehydration.
Air Travel Considerations and Prevention
Air travel has its own dehydration and DVT risks. The dry air in cabins can cause dehydration if you don’t drink enough water. Also, tight seats and less movement can make blood pool in your legs, raising clot risk.
To lower these risks in the air:
- Drink lots of water to stay hydrated.
- Drink less alcohol and caffeine, as they dry you out.
- Walk up and down the aisle often to keep blood flowing.
- Wear compression socks to reduce swelling and improve blood flow.
Road Trip and Long-Distance Travel Precautions
Road trips also increase dehydration and DVT risks. This is because not taking breaks to stretch can cause blood to pool in your legs, like in air travel.
To stay safe on long drives:
- Make regular stops to stretch and move around.
- Drink water often to stay hydrated.
- Avoid big meals that make you uncomfortable and limit movement.
- Adjust your seat to improve blood flow.
Knowing the risks and taking steps to prevent them can lower dehydration and DVT risks while traveling. By being informed and ready, you can enjoy your trips while keeping your health in check.
|
Travel Type |
Dehydration Risk Factors |
DVT Prevention Strategies |
|---|---|---|
|
Air Travel |
Dry cabin air, limited mobility |
Stay hydrated, wear compression socks, move regularly |
|
Road Trip |
Prolonged sitting, limited fluid intake |
Take regular breaks, stay hydrated, adjust seating for circulation |
Optimal Hydration: How Much Fluid Do You Really Need?
Daily hydration needs change based on age, how active you are, and where you live. Knowing these factors helps keep you hydrated and avoids dehydration problems.
Daily Hydration Requirements by Age and Activity Level
Hydration needs differ by age and how active you are. Older adults might need more water because they don’t feel thirsty as much. People who are very active also need more water to replace lost fluids.
General Guidelines for Daily Fluid Intake:
- Adults should drink 8-10 cups (64-80 ounces) of water each day.
- Those who are very active might need 16 cups (128 ounces) or more.
- Older adults should drink more, even in hot weather or when sick.
Adjusting Intake Based on Activity and Environment
It’s important to adjust how much water you drink based on your activity and where you are. For example, in hot weather or when you’re very active, you lose more water through sweat. So, you need to drink more.
“The key to optimal hydration is balancing fluid intake with individual needs, considering factors like climate, physical activity, and overall health.”
Watching your urine can help you know if you’re drinking enough water. If it’s dark yellow or you’re not making much urine, you might not be drinking enough.
Best Fluids for Hydration and Clot Prevention
Not all drinks are good for staying hydrated and preventing blood clots. Water is the best because it helps you stay hydrated without adding calories or sugar.
Other beneficial fluids include:
- Herbal teas, which can help you stay hydrated without caffeine.
- Electrolyte-rich drinks, which help replace lost salts during hard exercise.
- Low-sugar sports drinks, good for long workouts.
Keeping yourself well-hydrated is key to your health. It helps prevent dehydration problems, like blood clots. By knowing how much water you need and adjusting it for your lifestyle, you can stay healthy.
Preventive Strategies: Reducing Dehydration-Related Clot Risk
To prevent dehydration-related clots, several strategies are key. Understanding and using these methods can lower the risk of blood clots caused by dehydration.
Hydration Schedules and Reminders
Keeping hydrated is essential to avoid dehydration-related clots. A hydration schedule helps keep fluid intake steady. Use reminders or apps to track water intake.
Drink water at set times, like when you wake up, eat, and before bed. Adjust how much you drink based on how active you are and the weather.
Movement and Exercise Recommendations
Regular movement and exercise are important for health and preventing blood clots. Physical activity improves blood flow, which helps prevent clots. Try simple exercises like leg stretches or short walks, even when you’re not active for long periods.
If you have trouble moving, try ankle rotations or toe wiggles. Always talk to a doctor to create an exercise plan that fits your needs.
Dietary Considerations for Hydration and Vascular Health
Dietary considerations are key for staying hydrated and keeping your blood vessels healthy. Eating foods with lots of water, like fruits and veggies, helps meet your hydration needs. Also, eat foods rich in omega-3s, antioxidants, and fiber for better blood vessel health.
Avoid foods high in sodium to prevent dehydration. Eating a balanced diet with whole foods can help keep your blood vessels healthy and lower clot risk.
Compression Garments and Other Preventive Tools
Compression garments are great for preventing blood clots, mainly for those at high risk or when they can’t move much. These garments apply pressure to help blood flow better and prevent clots.
Other tools like compression stockings and pneumatic compression devices can also help. Always talk to a doctor to find the best tools for your risk level and health.
By using these strategies every day, you can greatly lower your risk of dehydration-related blood clots. It’s a proactive way to stay healthy by focusing on hydration, exercise, diet, and using preventive tools.
Medical Interventions: When to Seek Help
When dehydration and DVT symptoms get worse, knowing what to do can save lives. It’s important to know when to get medical help to avoid serious problems.
Emergency Warning Signs That Require Immediate Attention
Certain symptoms mean you need to go to the emergency room fast. For dehydration, look out for:
- Severe thirst and dry mouth
- Dark urine or very little urine
- Dizziness or fainting
- Rapid heartbeat and breathing
For DVT, watch for:
- Swelling, pain, or tenderness in one leg
- Redness or discoloration of the affected leg
- Warmth or tenderness to the touch
If you or someone you’re caring for has these symptoms, act fast. Waiting too long can lead to serious problems, like pulmonary embolism, which can be deadly.
Diagnostic Tests for Dehydration and DVT
When you get medical help, doctors will do tests to see how bad dehydration and DVT are. They might do:
Blood tests to check for dehydration and clotting factors
- Imaging tests like ultrasound to see the clot
- Venography, an imaging test that uses X-rays to see the veins
Getting the right diagnosis is important for treatment. These tests help doctors know how bad dehydration is and where and how big the clots are. This guides the treatment.
Treatment Options for Dehydration and Suspected DVT
Treatment for dehydration and DVT often involves several steps. For dehydration, this usually means:
- Fluid replacement therapy to rehydrate the body
- Electrolyte supplements to restore balance
For DVT, treatment might include:
- Anticoagulant medications to prevent the clot from growing
- Thrombolytic therapy in severe cases to dissolve the clot
- Use of compression stockings to reduce swelling
As doctors say,
“Quick treatment of dehydration and DVT can greatly lower the risk of complications and improve patient outcomes.”
Dealing with a medical emergency can be scary. But knowing what to do can make a big difference in getting the best care.
Recovery and Rehabilitation After Dehydration-Related Clotting Issues
Recovering from dehydration-related clotting issues takes careful medical care and big lifestyle changes. It’s a journey that needs a full plan to fix immediate health problems and keep you well in the long run.
Medical Follow-up Protocols
After dehydration-related clotting issues, regular medical follow-ups are key. They help keep an eye on your health and change treatment plans if needed. These steps usually include:
- Regular check-ups with healthcare providers to assess recovery progress
- Monitoring of blood clotting factors and overall vascular health
- Adjustments to anticoagulant medication, if prescribed
Good medical follow-up helps spot problems early and act fast.
Lifestyle Adjustments After a Clotting Event
Making lifestyle adjustments is critical to stop future clotting and keep you healthy. Important changes are:
- Increasing fluid intake to maintain optimal hydration levels
- Incorporating regular physical activity, tailored to the individual’s health status
- Adopting a balanced diet rich in nutrients that support vascular health
These steps help you recover and stay healthy for a long time.
Long-term Prevention Strategies
It’s vital to use long-term prevention strategies after clotting issues. These strategies might include:
- Continued monitoring of hydration levels, specially in high-risk situations
- Avoiding known risk factors for dehydration and clotting
- Staying informed about the latest research and recommendations on clot prevention
Real-Life Cases: Dehydration and Blood Clot Incidents
Dehydration and blood clots are linked, as shown by real-life examples. These cases teach us about the dangers of not drinking enough water. They also show how to prevent blood clots caused by dehydration.
Patient Stories and Outcomes
Many cases show how dehydration can lead to blood clots. For example, a traveler who didn’t drink water on a long flight got a DVT. Prompt medical attention helped avoid worse problems. An athlete who didn’t drink water during a marathon got a blood clot and was hospitalized. These stories stress the need to stay hydrated, even in tough situations.
Results from these cases vary. Some patients fully recovered, while others faced long-term health issues. Quick and right medical care is often key to recovery. Learning from these stories helps doctors and patients prevent risks.
Lessons Learned from Clinical Cases
Doctors have learned a lot from these cases. First, it’s important to spot patients at high risk. This includes those with clotting problems, surgery patients, and those who can’t move much. Second, teaching patients about dehydration risks and the need to stay hydrated is essential. Lastly, having effective prevention strategies like drinking schedules and exercise can lower blood clot risks.
By studying these cases, we can make better guidelines for preventing and treating dehydration and blood clots. This helps improve patient care and supports public health efforts to reduce these problems.
Conclusion: Understanding the Dehydration-DVT Connection
It’s key to know how dehydration and Deep Vein Thrombosis (DVT) are connected. Dehydration can raise the risk of blood clots. So, it’s vital to understand the risks and take steps to prevent them.
Staying hydrated can lower the risk of blood clots caused by dehydration. We’ve looked at how dehydration and DVT are linked. This includes the effects of dehydration on the body and the risk factors for DVT.
There are ways to prevent and treat the link between dehydration and DVT. Drinking enough water is one. Knowing the signs of dehydration and DVT is also important. And, taking steps to prevent blood clots during long trips is helpful.
We stress the need to understand dehydration and DVT to prevent and manage them well. By using preventive measures and getting medical help when needed, people can lower their risk of blood clotting problems.
FAQ
Can dehydration cause blood clots?
Yes, dehydration can make blood more likely to clot. This includes Deep Vein Thrombosis (DVT). Dehydration makes blood thicker, which increases clotting risk.
How does dehydration affect blood composition and flow?
Dehydration changes blood composition. It leads to hemoconcentration, making blood cells and clotting factors more concentrated. This increases the risk of blood clots.
What are the symptoms of dehydration that I should monitor?
Watch for early signs like headaches, fatigue, dry mouth, and dark urine. Severe dehydration can cause kidney damage. Seek medical help if symptoms get worse.
What are the risk factors for developing DVT?
DVT risk factors include immobility, genetics, certain medical conditions, and dehydration. Knowing these can help prevent DVT.
How can I stay hydrated to prevent DVT and other related health issues?
Drink enough fluids, adjusting for age, activity, and environment. Water, electrolyte-rich drinks, and hydrating beverages are best. Avoid caffeine and alcohol.
What are the preventive strategies for reducing dehydration-related clot risk?
Preventive strategies include staying hydrated, exercising regularly, and making healthy diet choices. Use compression garments and other tools too.
When should I seek medical help for dehydration or DVT symptoms?
Seek immediate medical help for severe dehydration or DVT symptoms. Diagnostic tests and treatments like fluid replacement and anticoagulation therapy are available.
Can certain medical conditions increase the risk of dehydration and DVT?
Yes, conditions like kidney disease, heart failure, and diabetes raise dehydration and DVT risk. Preventive measures can help reduce these risks.
How does travel affect dehydration and DVT risk?
Travel, long-distance travel in particular, can increase dehydration and DVT risk. Stay hydrated, move regularly, and use compression garments to reduce risk.
What are the long-term prevention strategies for dehydration-related clotting issues?
Long-term prevention includes a healthy lifestyle, staying hydrated, and regular exercise. Dietary choices and medical follow-up are also key to preventing complications.
References
Does Dehydration Cause Blood Clots? Scary Truth
https://pubmed.ncbi.nlm.nih.gov/27206642/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News






























