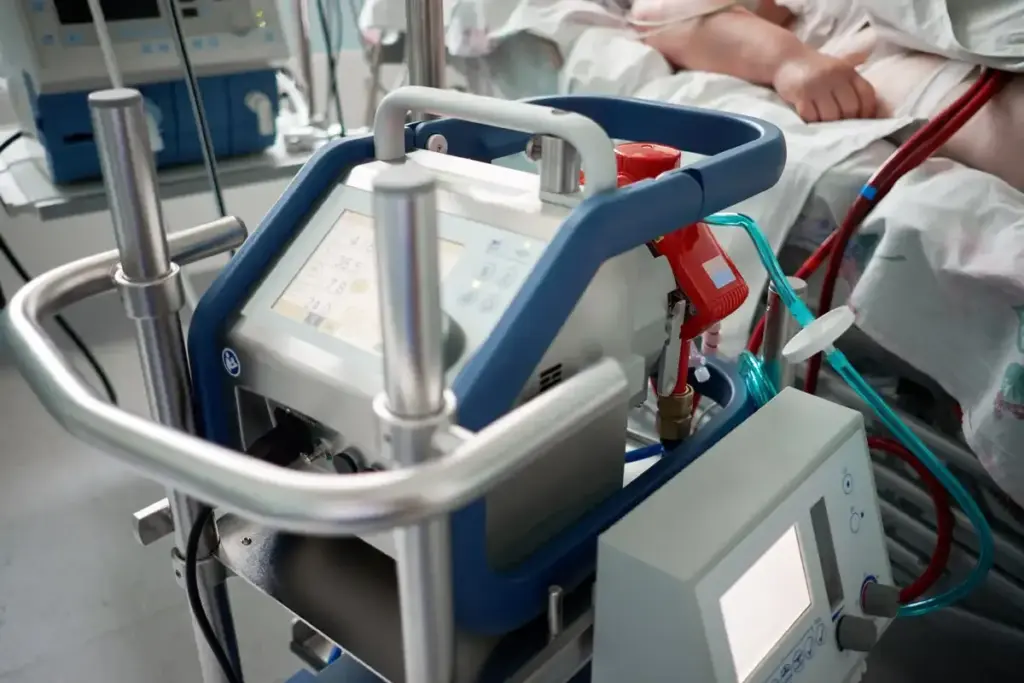
Many people confuse ECMO (Extracorporeal Membrane Oxygenation) with ventilators. But these technologies have different roles in critical care. Knowing their differences is key for those facing severe heart or lung failure.
ECMO is a high-tech tool used when regular ventilation isn’t enough. It’s not like ventilators, which help or take over breathing by pushing air into the lungs. ECMO does the job of oxygenating blood and removing carbon dioxide outside the body. This lets the lungs and/or heart rest and heal.
Studies have found that ECMO can greatly lower death rates in severe Acute Respiratory Distress Syndrome (ARDS) patients. At top hospitals like Liv Hospital, teams follow strict, evidence-based care plans. This ensures care keeps getting better and meets the highest standards.
Key Takeaways
- ECMO and ventilators are distinct life-support technologies used in critical care.
- ECMO is used when mechanical ventilation fails to provide adequate oxygenation.
- ECMO takes over the work of oxygenating the blood and removing carbon dioxide outside the body.
- Recent studies show ECMO can significantly reduce mortality in severe ARDS patients.
- Multidisciplinary care pathways at centers like Liv Hospital ensure high standards of ECMO care.
Understanding ECMO: Definition and Basic Principles

Extracorporeal Membrane Oxygenation, or ECMO, is a life-saving treatment. It’s used when a patient’s heart or lungs fail. This therapy takes over these functions, helping the organs recover.
What ECMO Stands For and Its Purpose
ECMO means Extracorporeal Membrane Oxygenation. “Extracorporeal” means doing a medical function outside the body. In ECMO, blood is taken from the body, oxygenated, and then returned.
The main goal of ECMO is to support life. It oxygenates the blood and removes carbon dioxide. This lets the lungs rest and recover from illness or injury.
Historical Development of Extracorporeal Support
ECMO’s history began in the 1950s and 1960s with early cardiopulmonary bypass technology. Over time, ECMO has become more advanced and widely used. Improvements in pumps, oxygenators, and cannula materials have made it safer and more effective.
Here are the key milestones in ECMO’s evolution:
|
Year |
Milestone |
Description |
|---|---|---|
|
1950s |
Early Cardiopulmonary Bypass |
Initial experiments with cardiopulmonary bypass technology laid the groundwork for ECMO. |
|
1970s |
First ECMO Trials |
The first human trials of ECMO were conducted, showing promising results in neonatal patients. |
|
1990s |
Advancements in Technology |
Significant improvements in ECMO technology, including better pumps and oxygenators, expanded its use. |
|
2000s |
Increased Adoption |
ECMO became more widely adopted in critical care settings, with growing evidence supporting its effectiveness. |
Today, ECMO is a vital therapy for severe heart or lung failure. It offers a bridge to recovery or transplantation.
How Mechanical Ventilators Work
Mechanical ventilators are advanced medical tools. They help patients who are very sick breathe. These devices are key in intensive care units where patients need help breathing.
Basic Function and Mechanism of Ventilators
A mechanical ventilator pushes air into the lungs through a tube. This helps or takes over breathing. The process involves setting the amount of air and how often it’s delivered.
Healthcare teams can adjust settings like pressure support and oxygen levels. This makes sure each patient gets the right help.
Types of Mechanical Ventilation
There are different ways to use mechanical ventilation. Invasive ventilation uses a tube in the throat for serious cases. Non-invasive ventilation uses a mask for less severe issues.
Each method is chosen based on the patient’s health. For example, non-invasive ventilation works well for COPD flare-ups. Invasive ventilation is needed for severe cases like ARDS.
Why ECMO Is Not a Ventilator: Fundamental Differences
While ventilators help with breathing, ECMO takes over to oxygenate the blood. This shows how these technologies have different roles in critical care.
Operational Mechanisms and Technology
ECMO and ventilators work in different ways. Ventilators push air into the lungs to help with breathing. On the other hand, ECMO technology diverts blood outside the body to oxygenate it, easing the lungs’ workload.
The ECMO circuit is complex. It includes pumps, oxygenators, and heat exchangers. These parts work together to oxygenate the blood and keep its temperature right, unlike mechanical ventilation.
Physiological Impact on the Body
The physiological impact of ECMO is big. It lets the lungs rest and recover, which is great for severe respiratory failure.
Compared to ventilators, ECMO supports the lungs and also eases the heart’s strain. This is key for patients with heart and lung problems.
It’s important for healthcare providers to know the differences between ECMO and ventilators. Both are critical in critical care, but their unique ways of working and effects on the body make them different.
The ECMO Circuit: Components and Function
The ECMO circuit has several key parts. It helps patients with severe heart or lung issues. This system is vital for those needing advanced life support.
Cannulas and Vascular Access
Cannulas are a key part of the ECMO circuit. They connect the patient’s blood to the ECMO machine. These cannulas are carefully designed and sized to ensure optimal blood flow while minimizing the risk of complications. The choice of cannula size and type depends on the patient’s specific needs and the configuration of the ECMO support.
Getting vascular access for ECMO involves careful planning and precise technique. Clinicians must assess the patient’s vascular anatomy to find the best spot for the cannula. They balance the need for effective ECMO support with the risk of vascular injury.
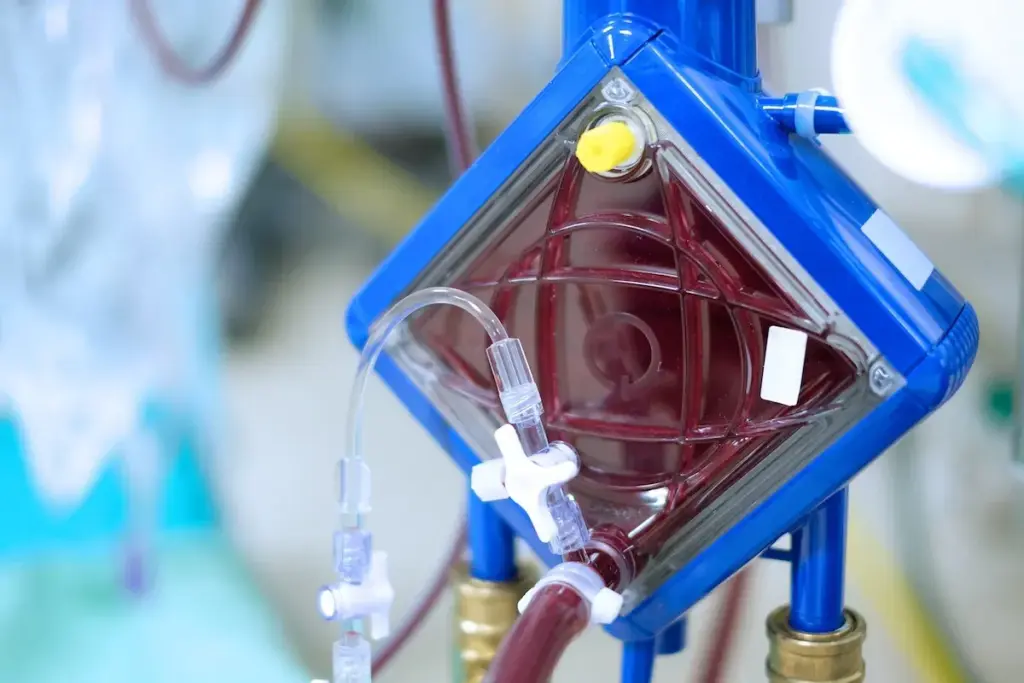
Pump Systems and Oxygenators
The pump system is vital in the ECMO circuit. It makes the blood flow needed for oxygenation and nutrient delivery. Modern ECMO pumps are highly sophisticated, capable of providing a range of flow rates to meet the individual needs of patients.
Oxygenators are where the blood gets oxygen and carbon dioxide is removed. This process is critical for supporting patients with respiratory failure, allowing for gas exchange outside the lungs. The design of oxygenators has evolved to improve efficiency and biocompatibility, reducing the risk of complications.
Heat Exchangers and Monitoring Equipment
Heat exchangers are key in keeping the patient’s blood temperature normal. This is essential for preventing hypothermia and ensuring optimal physiological function.
Monitoring equipment is also a key part of the ECMO circuit. It lets clinicians watch the patient’s status and the ECMO system’s performance. This includes sensors for pressure, flow, and gas exchange, among others, allowing for real-time adjustments to optimize ECMO support.
Types of ECMO Support and Their Applications
ECMO support is not a one-size-fits-all solution. It comes in various configurations tailored to specific patient needs. The type of ECMO used depends on the patient’s condition, the severity of their illness, and the specific support required.
Veno-Venous (VV) ECMO for Respiratory Failure
Veno-Venous (VV) ECMO is mainly used for patients with severe respiratory failure. This setup provides oxygenation support without directly supporting the heart. VV ECMO involves inserting cannulas into the venous system to exchange oxygen and carbon dioxide.
It is very helpful for patients with acute respiratory distress syndrome (ARDS) who haven’t responded to traditional ventilation. VV ECMO can be a lifesaving intervention by providing direct oxygenation support.
Veno-Arterial (VA) ECMO for Cardiac Support
Veno-Arterial (VA) ECMO is used when there is cardiac failure. It provides both oxygenation and cardiac support. This setup involves cannulation of both the venous and arterial systems.
VA ECMO is often used in severe cardiac dysfunction, like cardiogenic shock or cardiac arrest. It helps support the heart while it recovers from failure. It’s a critical tool for managing severe cardiac conditions.
Hybrid Configurations for Complex Cases
In complex cases, hybrid ECMO configurations may be used. These setups combine elements of VV and VA ECMO or use additional cannulas for specific needs. Hybrid configurations are useful for patients with both respiratory and cardiac failure.
By tailoring the ECMO configuration to the individual patient’s needs, we can optimize support and improve outcomes. Hybrid configurations offer a versatile approach to managing complex critical care cases.
When Is ECMO Used Instead of Conventional Ventilation?
When mechanical ventilation doesn’t work, ECMO steps in as a lifesaving option. ECMO, or Extracorporeal Membrane Oxygenation, is a complex therapy. It’s used when regular ventilation can’t support a patient’s breathing or heart.
Failure of Mechanical Ventilation
Mechanical ventilation is key in critical care for patients with breathing problems. But, it’s not always enough. Failure of mechanical ventilation can happen for many reasons, like severe lung damage.
When ventilation fails, doctors look for other ways to help. ECMO is one option. It provides an external way for gas exchange, giving the lungs a break to heal.
Specific Medical Conditions Requiring ECMO
Some medical conditions need ECMO because they’re very serious. These include:
- Severe ARDS (Acute Respiratory Distress Syndrome): This is a lung condition that makes breathing hard.
- Congenital Heart Defects: Some heart problems require ECMO before, after, or during surgery.
- Cardiac Failure: Severe heart failure can be helped by ECMO, which supports both heart and lungs.
Choosing ECMO depends on the patient’s condition, chance of recovery, and any reasons it might not work. Each case is different.
The ECMO Procedure: From Patient Selection to Decannulation
Starting ECMO support is a detailed process. It begins with choosing the right patient and preparing them well. The ECMO procedure is complex, needing precision and care for each patient.
Pre-ECMO Assessment and Preparation
Before starting ECMO, we do a full check to see if it’s right for the patient. We look at their medical history, current health, and how well they might recover. We consider many things, like why they need ECMO, how bad their condition is, and their overall health.
Cannulation Process and Initiation
The cannulation step is key in ECMO therapy. It involves putting cannulas in the patient’s blood vessels to move blood through the ECMO circuit. This step needs skilled hands and careful technique to avoid problems and ensure good ECMO support.
Management During ECMO Support
After starting ECMO, managing it well is vital for good results. This means adjusting ECMO settings, watching for any issues, and giving extra care as needed. We keep checking how the patient is doing on ECMO and make changes to help them the most.
Weaning and Removal Protocols
We start weaning from ECMO when the patient gets better and doesn’t need it anymore. This means slowly taking away ECMO support and seeing if the patient can breathe and circulate blood on their own. We have clear steps to follow for weaning, making sure it’s safe and works well.
From choosing patients to removing ECMO, a team of experts works together. By understanding ECMO well and following best practices, we can help patients recover better and live longer.
ECMO Indications and Contraindications
Choosing the right patients for ECMO therapy is key. It’s important to know when and when not to use it. ECMO helps those with severe heart or lung problems who haven’t gotten better with usual treatments.
Primary Indications for ECMO Therapy
ECMO is for patients with serious heart or lung issues. It’s used when these problems can be fixed. The main reasons include:
- Severe Acute Respiratory Distress Syndrome (ARDS)
- Cardiogenic shock
- Certain cases of cardiac arrest
- Bridge to lung transplantation or recovery
Doctors carefully check if a patient can get better or needs more help.
Absolute Contraindications
Some cases are too risky for ECMO. These are conditions where survival is unlikely or harm is possible. The absolute no-goes are:
- Irreversible brain damage
- Advanced or end-stage disease with no chance of recovery
- Severe coagulopathy or bleeding disorders
These are absolute no-goes because they either mean no chance of getting better or too much risk with ECMO.
Relative Contraindications and Risk Assessment
For some, the choice to use ECMO is not clear-cut. It’s about weighing the good against the bad. Things to think about include:
- Age and health problems
- How long on a ventilator before ECMO
- Other organ problems
We do a detailed risk check to see if ECMO is right for each patient. We look at their health and how likely they are to get better.
Clinical Outcomes: ECMO vs. Conventional Ventilation
Research on ECMO and conventional ventilation has grown a lot. It’s important to compare how well they work. This helps us improve care for critical patients.
Mortality Rates in Recent Studies
Studies show ECMO can lower death rates in severe ARDS patients. A key study found that ECMO patients had lower hospital death rates than those on traditional ventilation. ECMO is linked to better survival chances for the right patients.
A meta-analysis found ECMO is best for severe ARDS patients who can’t breathe on their own. It cuts down on death rates and reduces lung damage from the ventilator.
“ECMO is a lifesaver for those with severe respiratory failure. It offers a big survival advantage over just using a ventilator.”
Quality of Life After ECMO vs. Prolonged Ventilation
ECMO also improves life quality for many patients. They often get back to their normal life. Studies show ECMO leads to better long-term results and life quality than long-term ventilation.
ECMO patients face fewer long-term breathing problems. This is because they avoid the lung damage from high-pressure ventilation.
- ECMO reduces the risk of ventilator-induced lung injury.
- Patients receiving ECMO often have better long-term respiratory outcomes.
- The quality of life after ECMO is generally improved compared to prolonged ventilation.
As we keep improving ECMO and critical care, knowing these outcomes is key. It helps us give the best care and make smart choices about ECMO and ventilation.
Potential Complications of ECMO Therapy
ECMO therapy comes with risks. It’s important to know these to care for patients well. ECMO can save lives but also involves complex tech and invasive procedures. This can lead to different complications.
Mechanical and Technical Complications
ECMO therapy has mechanical and technical risks. These can come from the ECMO circuit, like the pump, oxygenator, and cannulas. Common issues include:
- Pump failure or malfunction
- Oxygenator dysfunction or failure
- Cannula-related problems, such as kinking or displacement
- Circuit thrombosis or clotting issues
Keeping the ECMO circuit in check is key. New tech has made systems better, but we must stay alert.
Patient-Related Complications
Complications from patients are a big worry with ECMO. These fall into several areas:
|
Complication Type |
Description |
Management Strategies |
|---|---|---|
|
Bleeding |
Risk of bleeding due to anticoagulation and cannulation sites |
Close monitoring of anticoagulation levels, management of bleeding sites |
|
Thrombosis |
Formation of clots within the circuit or patient |
Anticoagulation therapy, regular circuit checks |
|
Infection |
Risk of infection at cannulation sites or within the circuit |
Strict infection control measures, monitoring for signs of infection |
Managing these complications is vital. It helps prevent or lessen their effects on patients.
Long-Term Effects on Organ Systems
ECMO therapy can affect organs over time. The lungs, kidneys, and heart are at risk. For example, long ECMO use can harm the lungs or kidneys.
As ECMO tech improves, so does our knowledge of its risks. By tackling these complications, we can make ECMO therapy better. This helps improve patient results.
The Multidisciplinary ECMO Team
ECMO therapy’s success depends on a team of healthcare experts. This team works together to give patients full care. They help from the start to managing ECMO support and after.
Team Composition and Specialized Roles
The ECMO team includes intensivists, surgeons, perfusionists, nurses, and more. Each one brings their special skills to help the patient. Intensivists and surgeons help choose and manage patients. Perfusionists handle the technical ECMO work.
Nurses and others are key in constant care and watching the patient. Their teamwork makes sure all patient needs are met, leading to better results.
ECMO Specialists: Training and Certification
ECMO specialists get thorough training and certification. These programs teach them everything from ECMO basics to advanced care. Being certified means they know the latest in ECMO, giving patients top care.
Training mixes theory and practice, making sure specialists can handle ECMO’s challenges. They also keep learning as ECMO technology and methods change.
Continuous Education and Skill Maintenance
ECMO specialists must keep learning about new ECMO tech and care. They get training through sessions, workshops, and conferences. This keeps their skills sharp for the best patient care.
ECMO centers also have plans for keeping skills up, like simulation training. These help the team stay ready for any ECMO situation.
ECMO During the COVID-19 Pandemic
The COVID-19 pandemic brought huge challenges to healthcare systems around the world. ECMO became a key technology for saving lives. It was used in severe COVID-19 cases where regular ventilation wasn’t enough.
Utilization Patterns and Resource Allocation
How ECMO was used varied a lot between different places and hospitals. Some started using it early, while others waited for more serious cases. A study on theNational Center for Biotechnology Information website showed that how ECMO resources were used was very important.
Several things affected how ECMO was used:
- How much ECMO equipment and trained staff were available
- The severity of the patient’s condition when they arrived
- The hospital’s rules and guidelines for starting ECMO
Outcome Data and Survival Rates
Studies showed that ECMO helped a lot of critically ill COVID-19 patients survive. An in-depth look at ECMO results during the pandemic found that survival rates were similar to those before the pandemic.
A multicenter study found that:
“ECMO helped more COVID-19 patients survive than those who didn’t get it, mainly when regular ventilation wasn’t working.”
Protocol Developments and Lessons Learned
The pandemic pushed for faster development of ECMO protocols and guidelines. This was because of the need for consistent care in the face of new challenges. Important lessons included:
- Finding patients who could benefit from ECMO early
- Having clear rules for starting and managing ECMO
- Working together as a team for better patient care
These changes have made ECMO therapy better and safer for very sick patients.
Leading ECMO Centers and Their Approaches
ECMO care is getting better, thanks to top centers. They are known for their expertise and team work. This makes ECMO care more effective.
Liv Hospital’s Multidisciplinary Care Pathways
Liv Hospital is a leader in ECMO care. They have a team of experts like cardiologists and nurses. This team gives each patient the care they need.
Here’s what Liv Hospital focuses on:
- Pre-ECMO assessment and patient selection
- Standardized cannulation and ECMO initiation protocols
- Continuous monitoring and management during ECMO support
- Evidence-based weaning and decannulation protocols
Evidence-Based Protocols at Major Medical Centers
Centers like Liv Hospital use the latest research for ECMO care. This ensures patients get the best treatment.
These protocols cover important areas:
- Patient selection criteria
- ECMO configuration and settings
- Anticoagulation management
- Monitoring and troubleshooting during ECMO support
International Collaboration and Standards
Working together is key to better ECMO care. Centers share knowledge and help set global standards.
This teamwork has led to better care worldwide. It has improved patient outcomes and technology.
- Improved patient outcomes through standardized care
- Advancements in ECMO technology and techniques
- Enhanced training and education for ECMO specialists
Common Misconceptions About ECMO and Ventilators
Many people think ECMO is just a “super ventilator.” But this overlooks its unique abilities. ECMO and ventilators are both life-saving tools, but they do different things for patients.
ECMO as a “Super Ventilator”
One big mistake is thinking ECMO is just a better ventilator. While both help patients with breathing problems, they work in different ways. ECMO not only helps with breathing but also with the heart by oxygenating blood outside the body. Ventilators, on the other hand, help by adding oxygen to the lungs.
Key differences include:
- ECMO can oxygenate blood directly, skipping the lungs
- It supports both heart and lungs
- ECMO is more invasive, needing to be inserted into the body
Understanding the Complementary Relationship
ECMO and ventilators work together, not against each other. For example, a patient on ECMO might also need a ventilator for their lungs. Knowing how they work together is key to helping patients and their families.
“The use of ECMO in conjunction with mechanical ventilation requires a nuanced understanding of both technologies and their respective roles in supporting critically ill patients.” -Expert in Critical Care Medicine
Patient and Family Education Points
It’s important to teach patients and their families about ECMO. This includes why it’s not a replacement for ventilators but a different way to help patients with severe heart or lung issues.
Effective education points include:
- Explaining when ECMO is needed
- Talking about its benefits and risks
- Introducing the ECMO team that cares for patients
By clearing up misconceptions and sharing clear information, healthcare teams can support patients and families better. This helps them understand ECMO and ventilator therapy.
Future Directions in ECMO Technology
The future of ECMO looks bright, with many new advancements coming. We’re exploring new ways to improve life support technologies. This could change the field in big ways.
Advancements in Miniaturization and Portability
One exciting area is making ECMO systems smaller and more portable. Smaller, more compact systems could make ECMO therapy easier to use in different places. This could help more patients and lead to better results by starting treatment sooner.
As systems get smaller, patients might feel more comfortable and move around easier. This could lead to fewer problems and a better life during treatment.
The Role of Artificial Intelligence in ECMO Management
Using artificial intelligence (AI) in ECMO management is another big step forward. AI can look at lots of data from ECMO and patient health. This could make ECMO support more precise and effective.
AI could also help doctors make better choices about ECMO therapy. It could tailor treatment to each patient’s needs.
Emerging Hybrid Life Support Systems
Hybrid life support systems are another exciting area. These systems mix ECMO with other therapies. This could offer new ways to care for very sick patients.
For example, combining ECMO with kidney or heart support could help patients with many problems. This could lead to better results for patients.
Conclusion: ECMO as a Distinct Life-Saving Technology
ECMO plays a vital role in helping patients with severe respiratory or cardiac failure. It’s not a replacement for mechanical ventilation but a supportive therapy. It kicks in when regular ventilation isn’t enough.
This article has shown how important ECMO is in critical care. As ECMO technology gets better, it will save more lives and improve patient results. It’s a key part of advanced life support.
Seeing ECMO as a unique life-saving tool helps us value it more. This understanding improves care for critically ill patients, leading to better outcomes.
FAQ
What does ECMO stand for?
ECMO stands for Extracorporeal Membrane Oxygenation. It’s a therapy used when a patient’s lungs or heart fail.
How does ECMO differ from a ventilator?
ECMO is not a ventilator. It’s a more advanced technology that oxygenates blood outside the body. This lets the lungs rest. Ventilators, on the other hand, help breathe by pushing air into the lungs.
What is the primary function of a mechanical ventilator?
A mechanical ventilator’s main job is to help or replace breathing in patients who can’t breathe on their own. It does this by pushing air into the lungs through a tube.
What are the main components of an ECMO circuit?
An ECMO circuit has several key parts. These include cannulas for blood access, pumps for blood flow, and oxygenators to oxygenate the blood. There are also heat exchangers to keep blood temperature stable and monitoring equipment to manage the therapy.
What are the different types of ECMO support?
There are two main types of ECMO support. Veno-Venous (VV) ECMO is for severe respiratory failure. Veno-Arterial (VA) ECMO is for cardiac failure. Hybrid configurations are used in complex cases.
When is ECMO typically considered?
ECMO is considered when regular ventilation fails to provide enough oxygen. It’s also used for severe lung injury, like in severe ARDS.
What are the primary indications for ECMO therapy?
ECMO therapy is mainly for severe ARDS, cardiogenic shock, and some cardiac arrests.
What are the possible complications of ECMO therapy?
ECMO therapy can have complications. These include mechanical issues, patient problems like bleeding and thrombosis, and long-term effects on organs.
How is ECMO managed, and who is involved in the care team?
ECMO is managed by a team of experts. This team includes intensivists, surgeons, perfusionists, nurses, and more. ECMO specialists get special training and certification.
What advancements are being made in ECMO technology?
ECMO technology is getting better. There’s more miniaturization and portability. Artificial intelligence is being used in management, and new hybrid systems are emerging.
What is the role of ECMO during the COVID-19 pandemic?
ECMO was key in managing severe COVID-19 cases. It showed good results in improving survival rates for critically ill patients.
How does ECMO impact patient outcomes compared to conventional ventilation?
ECMO has been shown to reduce mortality in severe ARDS patients. A study found a significant drop in hospital mortality among ECMO-treated patients.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC9549020/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























