
Extracorporeal membrane oxygenation, or ECMO, is a life-saving therapy. It’s used for patients with severe heart or lung failure. The time a person stays on ECMO can vary a lot.
We look into how long this support usually lasts. Studies show different times for ECMO support depending on the condition and how well the patient responds. Most people stay on ECMO for 3 to 10 days.
Key Takeaways
- The length of ECMO support varies based on the patient’s condition and response to treatment.
- Most patients receive ECMO support for between 3 and 10 days.
- Underlying conditions and complications can influence the duration of ECMO.
- Understanding the average duration helps patients and families prepare for treatment.
- ECMO is a life-support therapy for severe cardiac or respiratory failure.
What is ECMO and How Does It Work?

Extracorporeal Membrane Oxygenation, or ECMO, is a complex medical treatment. It takes over the heart and lungs’ functions. This therapy is used when these organs fail severely.
The Basics of Extracorporeal Membrane Oxygenation
ECMO works by taking some blood from the body to a bypass machine. There, it’s oxygenated and cleaned of carbon dioxide. Then, it’s returned to the patient, helping the heart and lungs rest and recover.
To start the ECMO procedure, large tubes called cannulae are inserted into major blood vessels. The size and type of cannulae depend on the patient’s size and condition.
Types of ECMO Support Systems
There are two main types of ECMO: Veno-Arterial ECMO (VA-ECMO) and Veno-Venous ECMO (VV-ECMO). VA-ECMO supports both the heart and lungs by returning oxygenated blood to the arteries. VV-ECMO mainly supports the lungs by returning oxygenated blood to the veins.
|
Type of ECMO |
Primary Use |
Blood Return |
|---|---|---|
|
VA-ECMO |
Cardiac Support |
Arterial System |
|
VV-ECMO |
Respiratory Support |
Venous System |
Studies show that patients on VA-ECMO usually stay for about 2.6 days. The choice between VA-ECMO and VV-ECMO depends on the patient’s condition and the cause of their failure.
“The use of ECMO has become increasingly important in the management of critically ill patients, offering a lifeline when conventional therapies are insufficient.”
ECMO is a flexible therapy that can provide cardiac, respiratory, or both types of support. Knowing how ECMO works and its types is key to understanding its role in critical care.
Average Duration of ECMO Support
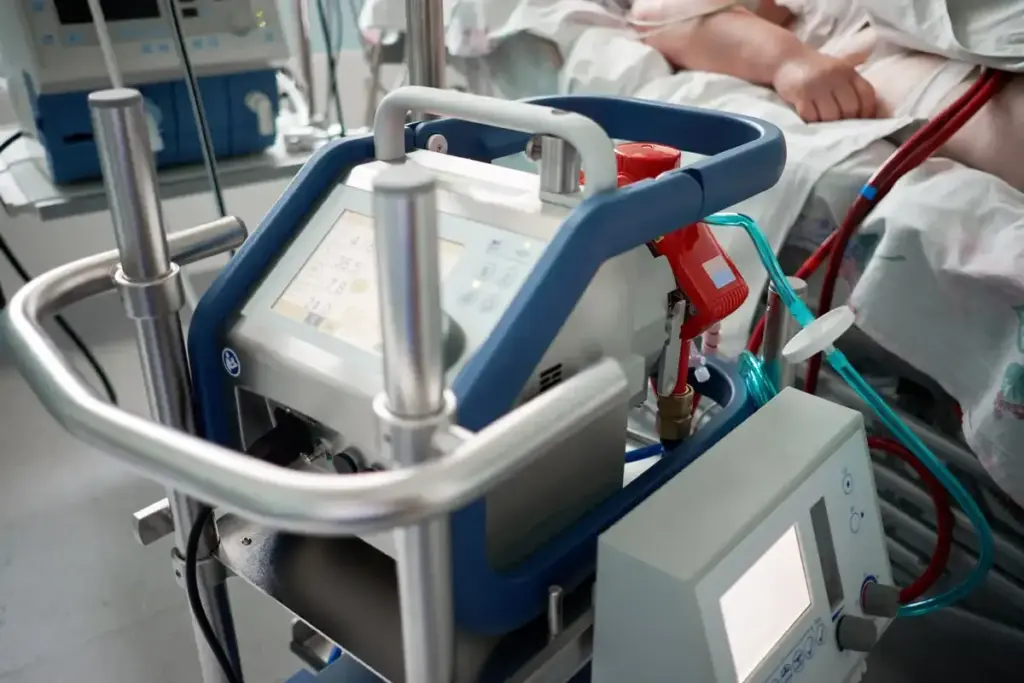
Knowing how long ECMO therapy lasts is key for patient care. The time on ECMO varies with the condition and how well the patient responds.
Typical Length of Stay on ECMO Therapy
Most patients on ECMO stay for 3 to 10 days. This time lets doctors check how well the therapy is working. Managing this period well is important for better results.
While on ECMO, patients are watched closely for any changes. This helps doctors decide if to keep or stop the therapy.
Variations by Patient Population
ECMO time can differ a lot among patients. For example, heart patients might need more time than lung patients. Knowing these differences helps in giving better care.
Things like the patient’s condition, how they react, and any complications affect ECMO time. Doctors use these to guess how long therapy will last for each patient.
We know every patient’s ECMO journey is different. So, we tailor our care to fit each person’s needs. This way, we aim to make ECMO support as effective as possible for everyone.
VA-ECMO Duration for Cardiac Conditions
VA-ECMO therapy is key for patients with severe heart issues. It helps those who have had heart surgery or are facing heart failure.
Studies show that the average time on VA-ECMO for heart cases is about 2.6 days. This time can change based on the heart problem and how well the patient responds to treatment.
Median Support Time
The average time of 2.6 days means half of patients were on ECMO for less than this. The other half needed it longer. This shows how important it is to tailor care for each patient.
Post-Cardiac Surgery Support
VA-ECMO is crucial for patients after heart surgery. It helps manage heart failure after surgery, giving the heart time to heal. The time on VA-ECMO is closely watched to match the patient’s recovery.
We know that needing VA-ECMO can worry patients and their families. By sharing how long VA-ECMO therapy usually lasts, we hope to make the treatment process clearer and more reassuring.
VV-ECMO Duration for Respiratory Failure
VV-ECMO therapy is a lifeline for patients with severe respiratory failure. It offers a critical bridge to recovery. This advanced life-support technology is key in managing complex respiratory conditions, including those from COVID-19.
Average Support Time
The average time on VV-ECMO is longer than VA-ECMO, about 8.4 days. This longer support is vital for patients with severe respiratory distress. It lets their lungs rest and recover.
“The use of VV-ECMO in patients with severe respiratory failure has shown promising results, with many patients experiencing significant improvement in their condition.”
COVID-19 Patients on ECMO
The COVID-19 pandemic has shown VV-ECMO’s importance in managing severe respiratory failure. Studies indicate VV-ECMO is effective for COVID-19 patients with acute respiratory distress syndrome (ARDS).
|
Condition |
Average ECMO Duration |
Survival Rate |
|---|---|---|
|
COVID-19 ARDS |
8-14 days |
40-50% |
|
Non-COVID-19 ARDS |
7-12 days |
50-60% |
Understanding VV-ECMO’s duration and use is crucial for healthcare providers. It helps them make informed decisions about patient care. By using this advanced technology, we can improve outcomes for patients with severe respiratory failure.
Factors Influencing ECMO Duration
ECMO duration is influenced by many factors. These include the patient’s health, the condition being treated, and the hospital’s ECMO program. Each patient’s situation is unique, leading to varying ECMO therapy lengths.
Patient-Specific Factors
Factors like the patient’s age and health are key in determining ECMO duration. Younger patients with fewer health problems tend to have shorter ECMO stays. Health conditions can greatly affect recovery, impacting how long ECMO support is needed.
A leading ECMO specialist notes, “The patient’s ability to recover is crucial for ECMO duration.” This shows the need for tailored care in ECMO therapy.
Condition-Specific Factors
The condition being treated also affects ECMO duration. Conditions vary in how long they take to recover, and their severity matters too. For instance, those with severe respiratory failure may need longer ECMO support.
- The type and severity of the underlying condition
- The presence of complications or organ dysfunction
- The response to ECMO therapy
These factors are key in deciding how long ECMO support is needed.
Institutional Factors
ECMO duration is also influenced by the hospital’s ECMO program. Centers with more experience may have better outcomes. The availability of resources, like staff and equipment, also plays a role.
“The quality of care and the multidisciplinary approach to ECMO management significantly affect patient outcomes and ECMO duration.”
Understanding these factors helps healthcare providers improve ECMO therapy. The mix of patient, condition, and hospital factors shows the complexity of ECMO care.
The ECMO Procedure Timeline
The ECMO treatment process has several key stages, from starting the cannulation to weaning. It’s vital for both patients and healthcare providers to understand this timeline. This helps them manage ECMO therapy effectively.
Cannulation Process
The ECMO support starts with cannulation. Large cannulae are put into the patient’s blood vessels for extracorporeal circulation. This is done under ultrasound or fluoroscopic guidance for accurate placement. Starting ECMO early is linked to better organ recovery and survival rates.
A leading ECMO specialist notes, “The cannulation process is a critical step that requires precision and expertise to ensure successful ECMO support.”
“The key to successful ECMO is not just the technology itself, but how it is applied with careful patient selection and meticulous management.”
Daily Management and Monitoring
After starting ECMO, daily management and monitoring are key. This includes adjusting the ECMO circuit settings and watching the patient’s blood flow. A team of experts is needed to care for ECMO patients fully.
- Regular checks of the ECMO circuit for any issues.
- Monitoring the patient’s vital signs and lab results to adjust ECMO support.
- Managing anticoagulation to prevent circuit blockages without increasing bleeding risk.
The Weaning Process
Weaning from ECMO is a gradual and careful process. It involves slowly reducing ECMO flow to see if the patient can oxygenate and circulate on their own. Successful weaning needs teamwork, considering the patient’s health and the reason for ECMO.
Deciding to wean a patient from ECMO depends on their health improvement and ability to handle less support. As we wean, it’s important to balance support needs with the goal of freeing the patient from ECMO.
Complications That Extend ECMO Support Time
ECMO therapy is lifesaving but comes with complications that can make it last longer. It’s important to know about these issues to manage patient care well and make ECMO support better.
Mechanical Complications
Mechanical problems during ECMO can affect how long it lasts. Issues like oxygenator failure, pump malfunction, and cannula-related problems can happen. For example, if the oxygenator fails, it needs to be replaced, which can add to the ECMO time.
These mechanical issues can also raise the risk of infection, bleeding, and thromboembolic events. A team effort from ECMO specialists, surgeons, and other healthcare professionals is needed to manage these risks and keep support going.
Patient Complications
Complications in patients also play a big role in how long ECMO lasts. These can include renal failure, hepatic dysfunction, neurological issues, and severe infections. These issues often mean ECMO support needs to go on longer until the patient gets better or until other treatments can be tried.
Also, pre-existing conditions can make it harder to take patients off ECMO. Careful monitoring and management of these patients are key to avoiding further problems and helping them recover.
In summary, both mechanical and patient-related complications are key in deciding how long ECMO support lasts. Understanding and tackling these issues can help healthcare providers improve patient results and make the ECMO therapy process smoother.
Survival Rates Related to ECMO Duration
ECMO survival rates change a lot based on the condition and how long support lasts. It’s key for doctors, patients, and families to know these rates. This helps them make smart choices about ECMO therapy.
Short-Term Survival Outcomes
Studies show that ECMO patients’ short-term survival rates vary. For heart issues, survival rates range from 28% to 34% at 30- or 90-day marks. These numbers show how complex ECMO therapy is and how important personalized care is.
We know that short-term ECMO survival depends on many things. These include the patient’s starting health, the ECMO type, and any other health problems.
Long-Term Survival Considerations
While short-term survival rates are useful, long-term ECMO survival matters too. Long-term survival depends on the patient’s health, how well ECMO works, and post-ECMO care quality.
Our research shows that ECMO for heart issues might have different long-term survival rates than for lung problems. This highlights the need for custom treatment plans and ongoing care.
Knowing both short-term and long-term survival rates helps doctors manage patient hopes better. It also helps them create more effective treatment plans.
Decision-Making for ECMO Initiation and Termination
Deciding when to start or stop ECMO is very complex. It needs careful thought about many clinical factors. These decisions are crucial and involve a detailed look at the patient’s health, medical history, and chances of getting better.
Clinical Criteria for Starting ECMO
We look at several important factors when starting ECMO. These include how severe the patient’s condition is, if their heart or lungs can recover, and if there are any reasons ECMO might not work. Starting ECMO early, when these criteria are met, can lead to better results.
ECMO is considered for patients with severe heart or lung failure who haven’t gotten better with usual treatments. We make the decision to start ECMO based on the patient’s overall health and their chances of recovery.
Determining When to Stop ECMO
Deciding when to stop ECMO is also complex. It involves checking the patient’s progress, any complications, and if they can still get better. We keep a close eye on patients on ECMO and adjust our care as needed to improve their chances.
We stop ECMO when it’s clear it won’t help the patient much more or when their health has improved enough. This decision is made with input from a team of healthcare experts.
Life After ECMO Treatment
Life after ECMO treatment is complex and varies greatly. It depends on the initial condition and overall health. At Liv Hospital, we aim to improve patient outcomes and follow international ECMO management standards.
Recovery Trajectories Post-ECMO
The recovery process after ECMO differs for each patient. Recovery is influenced by the condition needing ECMO, how long ECMO was used, and the patient’s health before and after treatment. We’ve seen that patients needing ECMO for heart issues might recover differently than those needing it for breathing problems.
It’s important to understand these differences for personalized care. Our team works with patients and families to create rehabilitation plans. These plans are tailored to meet each patient’s needs and help them recover as best as possible.
Long-Term Quality of Life
Long-term quality of life after ECMO is a big concern for patients and doctors. Studies show that some patients do well after ECMO, but others face ongoing challenges. Age, health before ECMO, and other health issues can greatly affect long-term outcomes.
At Liv Hospital, we focus on improving long-term quality of life for ECMO patients. We offer comprehensive follow-up care and support. Our commitment to international standards and best practices ensures our patients get the best care during their recovery.
Recent Advances in ECMO Technology
The field of ECMO is changing fast, thanks to new technologies. These changes are making care better and easier for doctors. At Liv Hospital, we use the newest tools and methods to give top-notch care.
Innovations Affecting Support Duration
New ECMO tech is changing how long patients need support. Improved cannula designs and better oxygenators mean fewer problems and more comfort. For example, biocompatible surfaces cut down on blood clots and swelling, letting patients stay on ECMO longer if needed.
Some big changes include:
- New membrane materials that help oxygen get to the blood better
- Smaller ECMO parts that are less invasive
- Better monitoring systems for quick patient data checks
Emerging Management Protocols
New care plans are also changing how we use ECMO. Multidisciplinary teams are working better together, thanks to new ways of managing ECMO. These plans focus on choosing the right patients, better ways to put in and take out ECMO, and how to wean patients off it.
“The integration of ECMO into critical care has been a game-changer. Emerging protocols are helping us tailor treatment to individual patient needs, significantly improving outcomes.” -ECMO Specialist
Some new care plans include:
- Standardized ways to put in and take out ECMO
- Better ways to manage pain and sedation
- Early programs to get patients moving and rehabbing
By using these new tools and plans, Liv Hospital is dedicated to giving the best care for ECMO patients. We aim for the best results and quality of life for our patients.
Liv Hospital’s Approach to ECMO Management
Liv Hospital leads in ECMO care, using new methods and team-based care. We aim to give top-notch healthcare, following the latest research and teamwork.
Academic ECMO Protocols
We follow strict ECMO rules at Liv Hospital to help patients get better. Our rules change often to keep up with new ECMO tech and care methods. This means our patients get the best care based on the latest science.
Key parts of our ECMO rules include:
- Watching patients closely and checking their health
- Creating treatment plans that fit each patient’s needs
- Working with ECMO experts worldwide to learn new ways
|
Protocol Component |
Description |
Benefit |
|---|---|---|
|
Continuous Monitoring |
Always checking patient health and ECMO system |
Finding problems early |
|
Personalized Treatment Plans |
Plans made just for each patient |
Therapy that works best for them |
|
International Collaboration |
Sharing knowledge with ECMO experts worldwide |
Getting the newest ways to manage ECMO |
Multidisciplinary Care Pathways
We have team-based care for ECMO patients at Liv Hospital. This team includes experts in heart, lung, critical care, and rehab medicine.
Our team care offers:
- Support for all parts of a patient’s health
- Plans that work smoothly from start to finish
- Help for patients and families through education and support
By mixing ECMO rules with team care, Liv Hospital aims to give the best ECMO management. We want to improve patient results and set a high standard in healthcare worldwide.
International Standards and Variations in ECMO
The world of ECMO care shows big differences in how it’s done, who gets it, and how it’s managed. It’s key to know these differences and how global registries track results to offer top-notch ECMO care.
Regional Differences in Practice
ECMO practices change a lot from one place to another. This is because of local health policies, what resources are available, and clinical guidelines. For example, some places might be stricter about who gets ECMO, while others are more open.
At Liv Hospital, we adjust to these regional differences. We do this while staying true to our goal of excellence in global healthcare. Our ECMO care plans are flexible and meet the needs of patients from all over.
Global Registries and Outcome Data
Global registries are crucial for tracking ECMO results. They give us insights into what works best and what needs work. By looking at this data, healthcare teams can find the best ways to care for patients.
The table below shows how ECMO results vary across different registries:
|
Registry |
Number of Patients |
Survival Rate |
|---|---|---|
|
ELSO Registry |
10,000+ |
60% |
|
EuroECMO Registry |
5,000+ |
55% |
|
Australia and New Zealand ECMO Registry |
2,000+ |
65% |
Looking at data from global registries helps us understand what affects ECMO results. This knowledge helps us improve care for our patients.
Conclusion: The Future of ECMO Support
ECMO technology and management are getting better. This means better care for patients. We expect to see more ECMO use in hospitals.
New tech and care methods are changing ECMO support. This change will help patients get better faster. Healthcare teams will be able to give top-notch care to those needing ECMO.
Liv Hospital is all about top-notch healthcare for international patients. We have special care plans and ECMO protocols. We’re excited to keep improving ECMO support and helping patients.
FAQ
What is ECMO and how does it work?
ECMO, or extracorporeal membrane oxygenation, is a therapy for severe heart or lung failure. It takes over the heart and lungs’ work. This lets them rest and recover.
What are the main types of ECMO?
ECMO has two main types. VA-ECMO supports the heart, and VV-ECMO supports the lungs.
How long do patients typically stay on ECMO?
Patients usually stay on ECMO for 3 to 10 days. The exact time depends on their condition and how well they respond.
What is the median duration of VA-ECMO support for cardiac cases?
For heart issues, VA-ECMO support lasts about 2.6 days on average. But, it can vary based on the condition and treatment response.
How long do patients with respiratory failure typically stay on VV-ECMO?
Patients with lung issues usually stay on VV-ECMO for about 8.4 days.
What factors influence the duration of ECMO support?
Several things affect how long a patient stays on ECMO. These include their health, the condition being treated, and hospital practices.
What are the potential complications of ECMO therapy?
ECMO can lead to mechanical and patient-related issues. These can make a patient stay on ECMO longer.
What are the survival rates for patients on ECMO?
Survival rates for ECMO patients vary. They depend on the condition and how long they’re on ECMO. Short-term survival rates are between 28-34%.
How is the decision made to initiate or terminate ECMO?
Deciding to start or stop ECMO is based on several factors. These include the patient’s condition, treatment response, and complications.
What can patients expect during the recovery process after ECMO treatment?
Recovery after ECMO varies for each patient. It depends on their recovery path and long-term quality of life.
What are the recent advances in ECMO technology?
ECMO technology and management are constantly improving. These advancements help patients and expand ECMO’s use in healthcare.
How does Liv Hospital approach ECMO management?
Liv Hospital focuses on top-notch healthcare with ECMO. They use the latest academic protocols and team care.
Are there regional differences in ECMO practice?
Yes, ECMO practices differ worldwide. Regional variations exist, and global registries track outcomes.
What is the future of ECMO support?
ECMO’s future looks bright. Ongoing advancements will likely improve patient outcomes and increase ECMO’s use in healthcare.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC10455442/

































