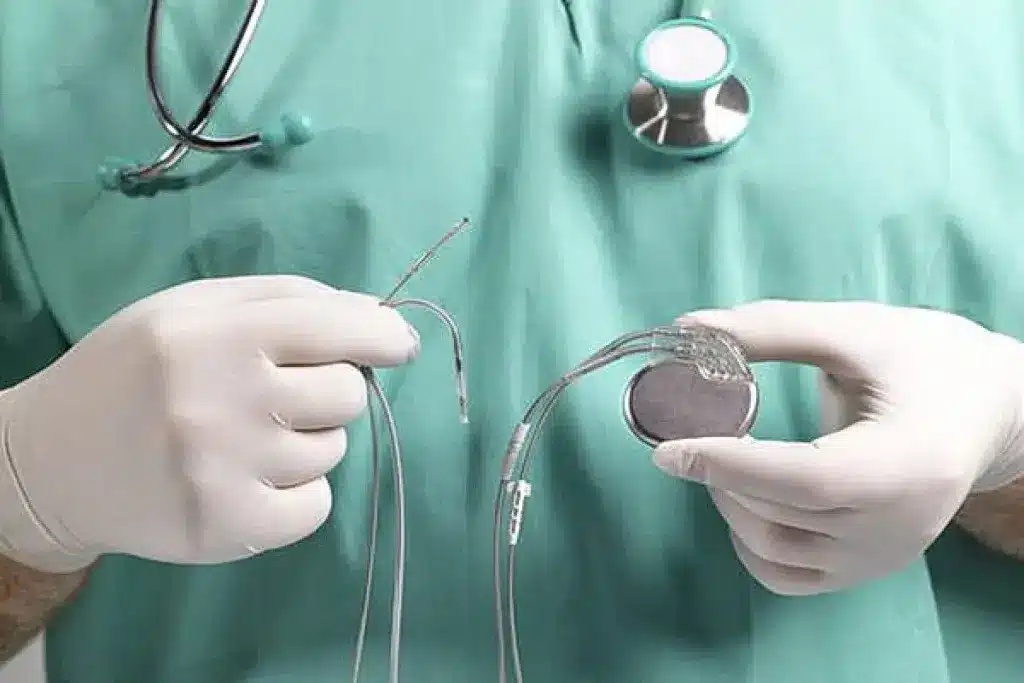
Atrial fibrillation (AFib) affects millions globally, causing irregular heartbeats. This can lead to serious health issues and even death. A common cardiac arrhythmia, AFib can make life less enjoyable and increase stroke risk pacemaker atrial fibrillation treatment.
A pacemaker helps manage AFib, mainly for those with slow heart rates or heart block. It keeps the heart beating right, improving its function.
This treatment is key for those with AFib symptoms. It can greatly improve their quality of life.
Key Takeaways
- AFib is a common cardiac arrhythmia that can lead to significant morbidity and mortality.
- Pacemakers are used to manage AFib, specially for those with slow heart rates or heart block.
- Pacemaker therapy can help restore a normal heart rhythm, improving cardiac function.
- Regulating heart rhythm with a pacemaker can enhance the quality of life for AFib patients.
- Pacemaker atrial fibrillation treatment is a vital therapy for managing AFib symptoms.
Understanding Atrial Fibrillation (AFib)
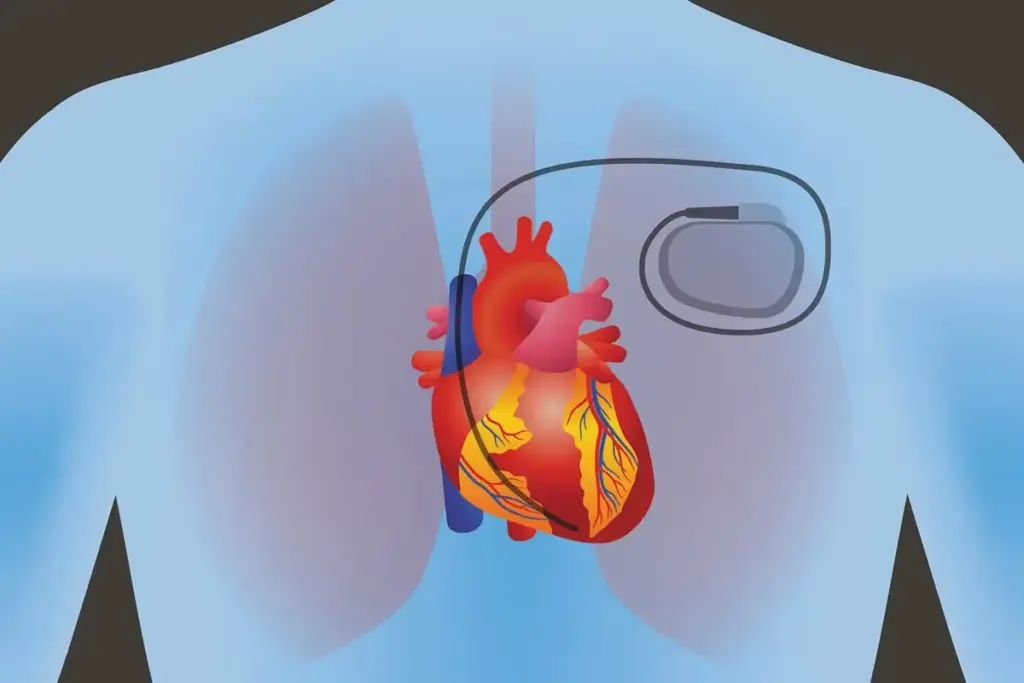
Knowing about atrial fibrillation (AFib) is key to managing its effects on patients. It’s a heart rhythm problem that can cause serious health issues. AFib is when the heart’s upper chambers beat chaotically, not moving blood well.
The Normal Heart Rhythm vs. AFib
A normal heart has coordinated electrical signals for a regular beat. But, AFib makes these signals chaotic, causing irregular heartbeats. This can make the heart beat too fast, too slow, or irregularly, leading to symptoms like palpitations and shortness of breath.
A normal heart rhythm is steady and coordinated. AFib, on the other hand, is irregular and often fast. This irregularity can cause serious problems, like stroke and heart failure.
Symptoms and Complications of AFib
AFib symptoms vary from person to person. Some may have mild symptoms, while others face severe ones that affect their daily life. Common symptoms include palpitations, shortness of breath, and fatigue.
If not treated, AFib can lead to serious issues like stroke and heart failure. It can also increase the risk of other heart diseases. The risk of stroke is higher because blood clots can form in the heart and travel to the brain.
Impact on Quality of Life
AFib can greatly affect a patient’s quality of life. Symptoms like palpitations and shortness of breath can limit physical activity and daily routines. The emotional toll of living with an irregular heart rhythm should not be ignored, as it can cause anxiety and depression.
Effective management of AFib is essential to improve quality of life. This includes medical treatments and lifestyle changes. Understanding AFib and its effects helps patients manage their condition better and reduce its impact on their daily lives.
The Basics of Cardiac Pacemakers
Cardiac pacemakers are small, implantable devices that keep the heart rhythm normal. They manage heart rhythm disorders like Atrial Fibrillation (AFib). This ensures the heart beats at the right rate.
How Pacemakers Function
Pacemakers send electrical impulses to make the heart beat. They have a pulse generator and leads (thin wires) in the heart. The pulse generator has the electronics and battery.
When the heart’s rhythm is slow or irregular, the pacemaker corrects it. Modern pacemakers adjust the heart rate based on activity. They speed up during exercise and slow down at rest.
Components of a Modern Pacemaker
A modern pacemaker has several key parts:
- Generator: This is the main part with the battery and electronics.
- Leads: These wires connect the generator to the heart, sending impulses.
- Electrodes: At the lead tips, electrodes touch the heart, sending signals.
- Battery: The battery powers the pacemaker. Modern ones last many years.
Evolution of Pacemaker Technology
Pacemaker technology has grown a lot. Early pacemakers were simple. Now, they’re advanced with features like:
- Remote Monitoring: Doctors can check the device and heart rhythm from afar.
- Adaptive Rate Response: The heart rate changes with activity level.
- Multi-Point Pacing: Pacing pulses go to different heart sites for better pumping.
These updates have made pacemakers more effective. They’ve greatly improved life for patients with heart rhythm issues.
Pacemaker Atrial Fibrillation Treatment: How It Works
Pacemakers are key in managing atrial fibrillation (AFib). They help control heart rhythm and ease symptoms. AFib causes irregular heartbeats, leading to less efficient heart function and higher risks of complications.
Regulating Heart Rhythm in AFib Patients
Pacemakers regulate heart rhythm in AFib patients. They send electrical impulses to make the heart beat regularly. This improves heart function and reduces symptoms like palpitations and shortness of breath.
They use advanced pacing algorithms to detect and adjust irregular heartbeats. These algorithms are customized for each patient, making treatment more effective.
Rate Control vs. Rhythm Control
There are two main strategies for managing AFib: rate control and rhythm control. Rate control slows the heart rate, while rhythm control tries to restore a normal rhythm.
Pacemakers can help with both. For rate control, they limit the heart rate. For rhythm control, they use algorithms to keep the rhythm normal.
- Rate Control: Slows the heart rate to prevent it from racing.
- Rhythm Control: Works to keep the heart rhythm normal.
Pacing Algorithms for AFib Management
Pacing algorithms are vital in managing AFib with pacemakers. They detect irregular heartbeats and adjust pacing to regulate rhythm.
Some common algorithms include:
- Atrial Pacing: Stimulates the atria to contract and maintain a normal rhythm.
- Ventricular Pacing: Ensures ventricles contract at a controlled rate, managing heart rate.
- Multisite Pacing: Paces multiple heart sites to improve contraction efficiency.
These advanced algorithms make pacemakers a powerful tool in managing AFib. They improve patient outcomes and quality of life.
Types of Pacemakers Used for AFib
AFib patients can benefit from different pacemaker technologies. These include single-chamber, dual-chamber, and biventricular devices. Each type is designed to meet the unique needs of AFib patients, with various functionalities and benefits.
Single-Chamber Pacemakers
Single-chamber pacemakers have one lead, usually in the right atrium or ventricle. They help control the heart rate in patients with AFib, mainly those with slow heart rates. They are a less invasive option, but not for everyone, mainly those needing more complex treatments.
Dual-Chamber Pacemakers
Dual-chamber pacemakers have two leads, one in each chamber. This allows for better coordination of heart contractions. They are great for patients with heart block or those needing more natural pacing. Dual-chamber pacemakers can improve symptoms and quality of life for some AFib patients.
Biventricular Pacemakers (CRT)
Biventricular pacemakers, or CRT devices, are for patients with heart failure and arrhythmias like AFib. They have three leads: one in each chamber and one over the left ventricle. They help the heart’s left and right ventricles work better together, improving efficiency and reducing heart failure symptoms. They’re used in more advanced cases or for specific indications.
In conclusion, choosing the right pacemaker for AFib depends on several factors. These include the patient’s heart condition, symptoms, and overall health. Knowing about the different pacemaker types helps patients and doctors make the best treatment choice.
When Is a Pacemaker Recommended for AFib?
A pacemaker is often suggested for AFib patients with slow heart rates or heart block. The choice to get a pacemaker depends on how bad the symptoms are and if other heart issues exist.
AFib with Bradycardia
AFib can lead to a slow heart rate, known as bradycardia. In these cases, a pacemaker helps control the heart’s rhythm and ensures blood flows well. Symptomatic bradycardia is a main reason for getting a pacemaker.
People with AFib and bradycardia might feel dizzy, tired, or have trouble breathing. A pacemaker can help by keeping the heart rate steady.
AFib with Heart Block
Heart block is another reason for a pacemaker in AFib patients. It happens when the heart’s electrical signals get disrupted.
A pacemaker can fix the heart rhythm in AFib patients with heart block. The pacemaker type depends on how severe the heart block is and other factors.
|
Condition |
Pacemaker Type |
Benefits |
|---|---|---|
|
AFib with Bradycardia |
Single-Chamber or Dual-Chamber |
Regulates heart rate, alleviates symptoms |
|
AFib with Heart Block |
Dual-Chamber or Biventricular |
Restores normal heart rhythm, improves cardiac function |
After AV Node Ablation
AV node ablation stops the bad electrical signals that cause AFib. After this, a pacemaker is usually needed to keep the heart’s rhythm steady.
The pacemaker helps the heart beat at a stable rate, lowering the risk of AFib problems. AV node ablation with pacemaker implantation is a common treatment for AFib symptoms.
In summary, a pacemaker is advised for AFib patients with bradycardia, heart block, or after AV node ablation. Pacemaker therapy offers better heart rhythm, symptom relief, and a better life quality.
The Pacemaker Implantation Procedure
For those with AFib, getting a pacemaker is a big step. It’s a small surgery to help control the heart’s rhythm. This is for those who need a pacemaker to keep their heart beating right.
Pre-Procedure Preparation
Before the surgery, tests are done to check if you’re ready. These might include blood tests, ECGs, and chest X-rays. Telling your doctor about any medicines you take is very important.
There are also things you should do before the surgery:
- Make sure someone can drive you home.
- Follow any diet advice from your doctor.
- Tell your doctor about any allergies or worries.
Step-by-Step Implantation Process
The surgery to put in a pacemaker has several steps:
- You’ll get local anesthesia to numb the area.
- A small cut is made in your chest. The pacemaker leads are then put into your heart using X-rays.
- The pacemaker generator is connected to the leads and put under your skin.
- The cut is closed with stitches or staples, and you’ll have a bandage.
Hospital Stay and Immediate Recovery
After the surgery, you’ll stay in the hospital for a day. This is to make sure the pacemaker is working right.
Right after, you’ll need to:
|
Activity |
Guideline |
|---|---|
|
Rest |
Avoid hard activities for a few days after |
|
Driving |
Usually okay in a few days, but check with your doctor |
|
Wound Care |
Keep the cut clean and dry; follow your doctor’s advice for dressing changes |
You can usually get back to normal in a week. It’s key to follow your doctor’s recovery advice for a safe and easy recovery.
Benefits of Pacemakers for AFib Patients
Pacemakers greatly improve the lives of those with AFib. They help control heart rhythm and treat related issues. This brings many benefits to AFib patients.
Symptom Relief and Quality of Life Improvements
Pacemakers help AFib patients feel better by managing their heart rate. This reduces symptoms like palpitations and shortness of breath. Patients can then enjoy daily activities more easily.
These improvements make life better in many ways:
- Patients sleep better, thanks to fewer symptoms at night.
- They have more energy, making it easier to stay active.
- Less symptoms mean less worry and stress about AFib episodes.
Reduced Risk of Complications
Pacemakers also lower the risk of serious problems linked to AFib. They keep the heart rhythm steady, which helps avoid stroke and heart failure. This is key for those at high risk.
Pacemakers help in several ways:
- They prevent slow heart rates that can cause dizziness or fainting.
- They reduce fast heart rates that can be uncomfortable or worse.
- They help the heart work better, lowering the chance of heart failure.
Enhanced Exercise Tolerance
Pacemakers also make it easier for AFib patients to exercise. They ensure the heart rate is right for physical activity. This boosts fitness and health.
Patients with pacemakers can:
- Do physical tasks without getting as tired.
- Do better in exercises like walking or swimming.
- Feel safer while exercising, thanks to the pacemaker’s control.
In summary, pacemakers are a big help for AFib patients. They ease symptoms, lower the risk of serious problems, and make exercising easier. Pacemakers are key in managing AFib.
Potential Risks and Complications
Pacemakers are generally safe, but there are risks to know about. Knowing these risks helps patients make better choices about their treatment.
Procedure-Related Complications
The procedure to implant a pacemaker is usually safe but can have risks. These include infection, bleeding, or a hematoma at the implant site. Rarely, there’s a chance of a collapsed lung or blood in the chest. Proper post-procedure care can help avoid these issues.
Infection is a serious problem that might need the pacemaker to be removed. To lower this risk, patients often get antibiotics before and after the procedure. Monitoring for signs of infection, like redness or fever, is key after the implant.
Device-Related Complications
Complications with the pacemaker itself can happen. These include lead displacement or malfunction, pacemaker failure, or allergic reactions. Regular follow-up with a doctor is vital to catch and fix these problems early.
Lead displacement can cause the pacemaker to not work right. Newer lead technology has made this risk lower, but it’s not gone.
Long-Term Risks
Over time, pacemakers may need a battery replacement, every 5 to 15 years. There’s also a risk of pacemaker syndrome, where the heart doesn’t contract right. But this is more common with certain types of pacing.
Battery depletion is a known event, and regular monitoring helps plan for replacement. This usually involves a small surgery to swap out the pacemaker generator.
It’s important to know about these risks and complications. Patients with pacemakers should watch for signs of trouble and keep up with doctor visits.
Recovery and Aftercare Following Pacemaker Implantation
Pacemaker implantation is just the start. Proper aftercare is key for AFib patients to get the most from their device. The recovery process includes important steps to ensure the device works right and the patient heals fully.
Immediate Post-Procedure Care
Right after the procedure, patients stay in the hospital for a bit. Doctors will check the device’s function and make sure it’s working right. Monitoring heart rate and rhythm is key to catch any problems early.
Patients might feel some soreness at the implant site. This can be managed with over-the-counter pain medications. It’s important to follow the doctor’s advice on medication and care.
Activity Restrictions
Patients need to follow certain activity rules to heal right and avoid complications. Avoiding heavy lifting, bending, or strenuous activities is advised for a few weeks. They should also be careful with the arm on the implant side, avoiding raising it too high or doing things that stress the implant site.
Wound Care and Follow-Up
Keeping the implant site clean and dry is critical to prevent infection and ensure healing. Patients should follow their healthcare provider’s specific instructions. Follow-up appointments are set to check on healing and the pacemaker’s function.
At these visits, the healthcare team might adjust the pacemaker settings to improve its performance. It’s a chance for patients to talk about any concerns or questions they have about their device or recovery.
By following aftercare instructions and going to scheduled follow-ups, patients can greatly improve their recovery. This way, they can fully enjoy the benefits of their pacemaker therapy.
Living with a Pacemaker for AFib
Living with a pacemaker for AFib means making some changes. But with the right info, patients can adjust well. A pacemaker can greatly improve life for those with atrial fibrillation by controlling their heart rhythm.
Daily Life Adjustments
After getting a pacemaker, patients must make some lifestyle changes. They should avoid heavy lifting or bending to prevent the pacemaker from moving. They also need to be careful around electronic devices that could mess with the pacemaker’s work.
It’s important to know the signs of pacemaker trouble, like dizziness or swelling. Regular check-ups with the doctor are key to keeping the device working right.
Environmental Considerations
Some things in the environment can affect a pacemaker. For example, strong magnetic fields, like those in MRI machines, can mess with it. Patients should tell their doctors about any upcoming tests that might use such equipment.
Most pacemakers today are safe from common devices like microwaves and cell phones. But it’s best to stay away from them when they’re in use.
Travel and Security Screenings
Traveling with a pacemaker needs some planning. Tell security people about your pacemaker before they scan you. Carry a pacemaker ID card to help with this.
At security checkpoints, ask for a manual search instead of going through metal detectors. This helps avoid any problems with your pacemaker.
Medical ID and Emergency Information
Patients with a pacemaker should always wear a medical alert ID. This could be a bracelet or necklace that shows they have a pacemaker. It’s very important in emergencies when doctors need to know about the pacemaker.
Keep your emergency contact info up to date. Make sure your doctors have the latest on how to reach you.
|
Aspect |
Precaution |
Benefit |
|---|---|---|
|
Daily Activities |
Avoid heavy lifting or bending |
Ensures pacemaker stability |
|
Environmental Factors |
Maintain distance from strong magnetic fields |
Prevents device interference |
|
Travel |
Inform security personnel; carry pacemaker ID |
Facilitates safe travel |
|
Emergency Preparedness |
Wear medical ID; update emergency contacts |
Ensures timely and appropriate medical response |
Pacemaker Monitoring and Maintenance
To keep a pacemaker working well, regular checks and care are key.
Pacemakers are complex devices that need regular checks to work right. Remote monitoring systems have changed how we manage them. They let doctors see how the pacemaker is doing in real time.
Remote Monitoring Systems
Remote monitoring lets doctors keep an eye on pacemakers. They can spot problems early and fix them. This tech helps patients and cuts down on doctor visits.
The good things about remote monitoring are:
- Spotting device problems early
- Less need for doctor visits
- Better health outcomes
- More convenience for patients
Regular Check-Ups
Regular doctor visits are also important for pacemaker care. These visits happen every 3 to 6 months. It depends on the device and the patient’s needs.
|
Check-Up Frequency |
Typical Interval |
|---|---|
|
Initial Check-Up |
1-3 months post-implantation |
|
Follow-Up Visits |
Every 3-6 months |
|
Battery Life Check |
Annually or as recommended |
Battery Life and Replacement
Pacemaker batteries don’t last forever. They can last from 5 to 15 years. It depends on the device and how much it’s used.
Replacement procedures are usually less invasive than the first implant. They can often be done with local anesthesia.
By using remote monitoring, regular visits, and replacing batteries on time, AFib pacemaker patients can stay healthy. They get the best from their device.
Combining Pacemaker Therapy with Other AFib Treatments
Pacemaker therapy for AFib works best when paired with other treatments. Atrial fibrillation (AFib) is a complex condition needing a multi-faceted approach. Pacemakers help manage symptoms and regulate heart rhythm, but they’re often used alongside other treatments for the best results.
Medication Management
Medication is key in managing AFib symptoms and preventing complications. Anti-arrhythmic drugs help control heart rhythm, and anticoagulants lower stroke risk. Combining pacemaker therapy with medication can greatly improve patient outcomes.
Ablation Procedures
Ablation procedures, like catheter ablation, destroy abnormal heart pathways causing AFib. Paired with pacemaker therapy, ablation can restore normal heart rhythm and lessen symptoms. This approach can greatly enhance AFib patients’ quality of life.
Lifestyle Modifications
Lifestyle changes are vital in managing AFib. Patients are encouraged to stay healthy, exercise, and avoid alcohol and caffeine. Combining these lifestyle changes with pacemaker therapy and other treatments helps manage the condition and lowers complication risk.
In summary, combining pacemaker therapy with other AFib treatments like medication, ablation, and lifestyle changes offers a complete management strategy. This approach can lead to better symptom control, reduced complications, and improved quality of life for patients.
Alternative Treatments for AFib
There are many treatments for AFib beyond pacemakers. These options meet different needs and the severity of AFib. They help manage the condition well.
Medication-Only Approaches
For many, medication is the first treatment for AFib. It can control heart rate, change AFib to normal rhythm, or prevent stroke. The right medication depends on the patient’s health and AFib type.
Common Medications Used:
- Beta-blockers
- Calcium channel blockers
- Anti-arrhythmic drugs
- Anticoagulants
Catheter Ablation
Catheter ablation is a less invasive procedure. It uses energy to destroy the heart’s abnormal electrical pathways. It’s for those who don’t respond to medication or want a more lasting solution.
Success Rates: Studies show it can work well for many, keeping the heart rhythm normal.
Surgical Options
Surgery for AFib is for severe cases or during other heart surgeries. The Maze procedure creates scar tissue to guide heart impulses.
|
Surgical Option |
Description |
Indications |
|---|---|---|
|
Maze Procedure |
Creates scar tissue to redirect electrical impulses |
Severe AFib, undergoing other heart surgery |
|
Minimally Invasive Surgical Ablation |
Less invasive than traditional Maze, uses ablation to treat AFib |
Symptomatic AFib, failed other treatments |
Emerging Therapies
New treatments for AFib are being researched. These include new anticoagulants, advanced ablation methods, and better pacemakers and ICDs.
The treatment options for AFib are growing. This means more choices for patients and doctors. Knowing these options helps make better care decisions.
Advancements in Pacemaker Technology for AFib
Pacemaker technology is changing fast, bringing hope to those with atrial fibrillation (AFib). These changes are making life better for AFib patients and making pacemakers work better.
Miniaturization and Leadless Options
One big change is making pacemakers smaller. Today’s pacemakers are tiny, making them easier to use and more comfortable for patients. Leadless pacemakers are a big step forward. They go right into the heart, avoiding the need for wires that can cause problems.
A study in the Journal of the American College of Cardiology found leadless pacemakers have fewer complications than old ones. This is great for AFib patients, as it cuts down on problems with the leads.
Enhancing Compatibility: MRI-Compatible Devices
Another big step is MRI-compatible pacemakers. These let patients get MRI scans safely, without worrying about the device or leads getting damaged. This is key for AFib patients, who might need MRI scans for other health checks.
“The development of MRI-compatible pacemakers has been a game-changer for patients with AFib, providing them with the freedom to undergo necessary diagnostic tests without restrictions.”
Smart Features and Connectivity
Today’s pacemakers are getting smarter, with new features and ways to connect. They can watch heart rhythms, spot arrhythmias, and send data to doctors remotely. This helps doctors make quick changes to help patients better.
|
Feature |
Benefit |
|---|---|
|
Remote Monitoring |
Allows for timely interventions and adjustments |
|
Arrhythmia Detection |
Enhances early detection of possible issues |
|
Data Transmission |
Helps with ongoing patient care |
Patient Experiences: Living with an AFib Pacemaker
People with AFib pacemakers share their real-life stories. Living with a pacemaker can change your life, bringing both good and bad sides.
Success Stories
Many patients say their AFib symptoms got better after getting a pacemaker. They report fewer irregular heartbeats. This lets them do more things without worrying about AFib.
One patient said, “Getting my pacemaker let me go hiking and spend time with family again. It’s been a big change for the better.”
Key benefits reported by patients include:
- Less AFib episodes
- More freedom to move
- Better overall life quality
Challenges and Adaptations
While pacemakers help a lot, there are also tough parts. Some feel sore or uncomfortable where the pacemaker is. This usually goes away by itself.
Getting used to a pacemaker means:
- Getting used to the device’s presence
- Learning about and managing the device settings
- Dealing with the emotional side of having a device inside you
Advice from Pacemaker Recipients
Those who got pacemakers have advice for others. They say to:
“Listen to your doctor’s advice before and after the surgery. Knowing how to live with your pacemaker helps a lot.”
Also, joining support groups can help. You get emotional support and practical tips from others who’ve been through it.
Some key advice includes:
- Be patient during recovery
- Stay informed about your device
- Don’t be afraid to ask health professionals questions
Conclusion
Atrial fibrillation (AFib) is a complex condition that needs a multi-faceted treatment. Pacemaker therapy has become a valuable tool for managing AFib, mainly for those with irregular heart rhythms.
Pacemaker treatment for AFib involves using a pacemaker to control the heart’s rhythm. This helps reduce symptoms and improves quality of life. It can be used alongside other treatments like medication and lifestyle changes for better results.
It’s important for both patients and healthcare providers to understand pacemaker therapy’s role in AFib treatment. Recognizing its benefits and limitations helps individuals make informed decisions about their care. This leads to better outcomes.
As medical technology advances, pacemaker therapy’s role in managing AFib will grow. Staying updated on new pacemaker technologies and treatment methods helps patients actively participate in their care. This improves their overall well-being.
FAQ
What is atrial fibrillation (AFib), and how does it affect the heart?
Atrial fibrillation (AFib) is a heart rhythm problem. It makes the heart beat too fast and irregularly. This happens when the upper heart chambers beat chaotically, not effectively moving blood to the lower chambers.
How does a pacemaker help manage AFib?
A pacemaker is a small device implanted under the skin. It helps control the heartbeat. For AFib patients, it can regulate the heart rate, improve symptoms, and lower the risk of complications.
What are the different types of pacemakers used to treat AFib?
There are several pacemakers for AFib, like single-chamber, dual-chamber, and biventricular ones. The choice depends on the patient’s needs and heart condition.
What is the difference between rate control and rhythm control in AFib management?
Rate control aims to prevent symptoms by controlling the heart rate. Rhythm control tries to restore a normal rhythm. Pacemakers can help with both.
What are the benefits of pacemaker therapy for AFib patients?
Pacemaker therapy can improve symptoms and quality of life. It also helps with exercise and reduces complications. It manages AFib symptoms and improves health outcomes.
What are the possible risks and complications of pacemaker implantation?
Risks include procedure and device complications, and long-term risks. Choosing an experienced provider and following aftercare can minimize these risks.
How is a pacemaker implanted, and what is the recovery process like?
Implantation is a minor surgery done under local anesthesia. Recovery involves a short hospital stay, activity restrictions, and wound care.
How often do pacemakers need to be checked and maintained?
Pacemakers need regular check-ups, every 3-6 months. Remote monitoring systems track function and detect issues.
Can I travel with a pacemaker, and are there any special precautions I need to take?
Yes, you can travel with a pacemaker. Carry a medical ID, inform your airline, and know about security screening procedures.
What are the alternatives to pacemaker therapy for AFib, and when are they considered?
Alternatives include medication, catheter ablation, surgery, and new therapies. They’re considered for those not suited for pacemakers or who haven’t responded well.
How do advancements in pacemaker technology impact AFib treatment?
Advances in pacemaker tech, like miniaturization and MRI-compatibility, have made treatment safer and more effective for AFib patients.
What can I expect after receiving a pacemaker for AFib, and how will it impact my daily life?
After a pacemaker, you’ll likely see improved symptoms and quality of life. You might need to adjust your lifestyle, avoiding certain factors and taking precautions during screenings.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1501106/


































