Endometrial cancer is a common uterine cancer in the U.S. It’s expected to affect about 69,120 people each year. It starts when cells in the endometrium grow too much. Finding it early is key to better treatment outcomes.This is your ultimate guide to endometrial ca treatment. Discover the most effective, powerful options available for every stage.
At Liv Hospital, we offer top-notch care with international standards. Our goal is to give patients the best endometrial cancer treatment. We often start with surgery. Sometimes, we add chemotherapy, hormone therapy, or radiation to get the best results.
Key Takeaways
- Endometrial cancer is a common gynecological malignancy in the U.S.
- Early detection significantly improves treatment outcomes.
- Surgery is the primary treatment for endometrial cancer.
- Combination therapies may be used to achieve optimal results.
- Liv Hospital provides high-quality, innovative care for international patients.
Understanding Endometrial Cancer
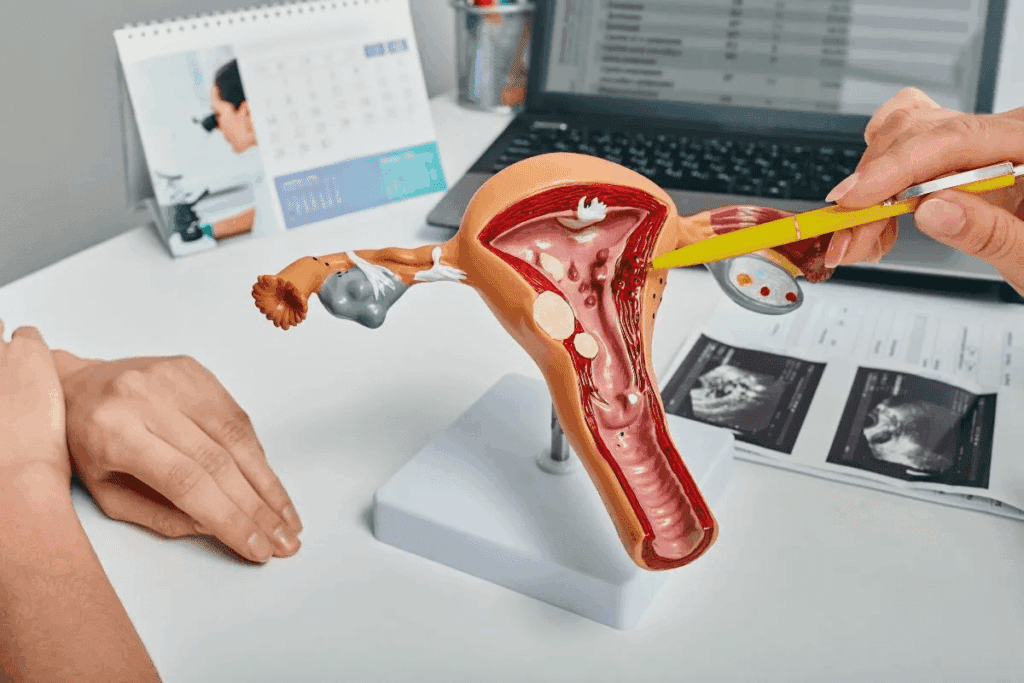
Endometrial cancer is the most common gynecological cancer in the United States. It’s important to know its causes, symptoms, and treatments. We’ll explore this condition to help patients understand their diagnosis and treatment options.
What is Endometrial Cancer?
Endometrial cancer starts in the endometrium, the uterus lining. It’s when cells grow abnormally in this layer. This can spread to other parts of the body. Knowing about this cancer is key for making treatment choices.
Prevalence and Statistics in the United States
In the United States, endometrial cancer is a big health concern. Many new cases are diagnosed each year. The 5-year survival rate for localized endometrial cancer is about 95 percent. This shows how vital early detection and treatment are.
Risk Factors and Warning Signs
Several factors can raise the risk of getting endometrial cancer, including:
- Obesity: Being very overweight can increase the risk.
- Hormone Replacement Therapy: Some hormone therapies can raise the risk.
- Genetic Syndromes: Conditions like Lynch syndrome can make you more likely to get endometrial cancer.
Common symptoms include abnormal vaginal bleeding. This needs quick medical check-up. Knowing these signs and risk factors can help catch the cancer early and treat it better.
To diagnose endometrial cancer, doctors use tests like pelvic exam, ultrasound, hysteroscopy, and biopsy. It’s important for patients to understand these tests. This helps them grasp their diagnosis and cancer stage.
Diagnosis and Staging of Endometrial Cancer
Getting a correct diagnosis and staging is key to finding the right treatment for endometrial cancer. The cancer’s stage is the most important factor in picking uterus cancer treatment. We use tests like a chest X-ray, CT scan, blood tests, and PET scan to figure out the stage.
Common Diagnostic Procedures
Diagnosing endometrial cancer involves several steps. First, a pelvic exam checks the uterus’s size and shape. Then, imaging tests like transvaginal ultrasound look at the endometrium’s thickness and for any issues.
An endometrial biopsy is a key test. It takes a tissue sample from the uterus lining for lab tests. This confirms cancer and its type.
The FIGO Staging System Explained
The International Federation of Gynecology and Obstetrics (FIGO) staging system is used for endometrial cancer. It divides the cancer into stages based on how far it has spread. The stages go from I (cancer in the uterus) to IV (cancer in distant parts of the body).
Knowing the FIGO stage is vital for planning uterine cancer treatments. It helps doctors choose the best treatment, like surgery, radiation, chemotherapy, or a mix.
How Staging Influences Treatment Decisions
The cancer’s stage greatly affects treatment choices. For early-stage cancer (Stage I and II), surgery is often the first step. Then, radiation or chemotherapy might be added to lower the chance of cancer coming back.
For more advanced stages (Stage III and IV), treatment might include surgery, radiation, and chemotherapy. The right treatment for uterus cancer depends on the stage, tumor grade, and the patient’s health.
New treatments like immunotherapy and targeted therapies are showing promise. They help in treating endometrial cancer when usual treatments don’t work. These new options give hope to patients with advanced or recurring cancer.
Surgical Treatment Options
For most patients with endometrial cancer, surgery is the main treatment. It involves removing the uterus, fallopian tubes, and ovaries. This is key to managing the disease.
Total Hysterectomy with Bilateral Salpingo-Oophorectomy
A total hysterectomy with bilateral salpingo-oophorectomy is the standard surgery for endometrial cancer. It removes the uterus, both fallopian tubes, and ovaries. This helps get rid of the cancer and stop it from spreading.
For patients with early-stage disease and low recurrence risk, doctors might skip adjuvant systemic therapy. They focus on surgery alone.
Lymph Node Dissection and Sampling
Lymph node dissection and sampling are key in surgical staging for endometrial cancer. They check if the cancer has spread to lymph nodes. This is important for planning further treatment.
- Lymph node dissection removes lymph nodes in the pelvic area.
- Sampling takes a few lymph nodes for examination.
Minimally Invasive Surgical Approaches
Minimally invasive surgical approaches, like laparoscopic or robotic surgery, have many benefits. They cause less pain, shorter hospital stays, and faster recovery. These methods are becoming more common for treating endometrial cancer.
Radiation Therapy for Endometrial Cancer
Radiation therapy is a key treatment for endometrial cancer. It uses high-energy rays to kill cancer cells. It might be used before surgery to shrink tumors or after to kill any left-over cells, lowering the chance of cancer coming back.
External Beam Radiation Therapy
External Beam Radiation Therapy (EBRT) sends high-energy beams from outside the body to kill cancer cells. It’s precise, aiming to harm healthy tissues less. EBRT treats larger areas, like the pelvis, to catch any cancer that might have spread.
Vaginal Brachytherapy
Vaginal Brachytherapy puts a small radioactive source close to the tumor in the vagina. It delivers a high dose of radiation right to the tumor while protecting other tissues. It’s often used after hysterectomy or for tumors in the vagina.
When Radiation Therapy is Recommended
Radiation therapy depends on the cancer’s stage and the patient’s health. For early-stage cancer, it’s used after surgery to kill any remaining cells. In more advanced cases, it might be combined with chemotherapy. New radiation techniques have made treatment better and less harmful for many patients.
As we learn more about endometrial cancer, new treatments like immunotherapy are showing promise. While radiation therapy is a mainstay, research and new therapies are opening up more options for care.
Endometrial CA Treatment: Chemotherapy Approaches
Chemotherapy plays a key role in treating endometrial cancer. It uses medicines to kill cancer cells. These medicines can be given before surgery to shrink the tumor or after surgery to lower the risk of cancer coming back.
Common Chemotherapy Drugs and Combinations
Chemotherapy for endometrial cancer often uses a mix of drugs. Common drugs include carboplatin, cisplatin, doxorubicin, and paclitaxel. These drugs can be used alone or together, based on the cancer’s stage and type.
Chemotherapy Drug | Common Usage | Side Effects |
Carboplatin | Often used in combination with paclitaxel | Nausea, hair loss, fatigue |
Cisplatin | Used for advanced or recurrent endometrial cancer | Nausea, kidney damage, hearing loss |
Doxorubicin | Used for various types of cancer, including endometrial cancer | Hair loss, heart damage, nausea |
Paclitaxel | Often used in combination with carboplatin | Hair loss, numbness in hands and feet, nausea |
Treatment Protocols and Regimens
Treatment plans for endometrial cancer vary based on several factors. Chemotherapy regimens are tailored to each patient’s needs. This includes their overall health and any previous treatments.
“The choice of chemotherapy regimen depends on several factors, including the extent of disease, patient comorbidities, and patient preferences.” NCCN Guidelines for Patients
Managing Side Effects and Complications
Managing side effects is key when undergoing chemotherapy. Common side effects include nausea, hair loss, and fatigue. Supportive care measures, such as anti-nausea medications and nutritional counseling, can help lessen these side effects.
For those concerned about fertility, fertility-sparing endocrine therapies are available. Options like medroxyprogesterone acetate, megestrol acetate, and levonorgestrel-releasing intrauterine devices offer alternatives. These options help manage endometrial cancer while considering reproductive health.
Hormone Therapy Options
For those with advanced or recurring endometrial cancer, hormone therapy is a good choice. It involves medicines that lower hormone levels or block their action. This can kill cancer cells that need hormones to grow. It’s best for patients with tumors that have hormone receptors.
Progestin Therapy Mechanisms
Progestin therapy uses synthetic progestins to treat endometrial cancer. It changes the hormonal environment, making it hard for cancer cells to grow. Medroxyprogesterone acetate and megestrol acetate are common progestins used in treatment.
The success of progestin therapy depends on several factors. These include the cancer’s stage and if it has hormone receptors. Patients with well-differentiated tumors and hormone receptor-positive cancers tend to respond well.
Tamoxifen and Aromatase Inhibitors
Other hormone therapies like Tamoxifen and aromatase inhibitors are also used. Tamoxifen can act like estrogen in some tissues but block it in others. It’s often used with progestins.
Aromatase inhibitors block the enzyme aromatase, which makes estrogen. By lowering estrogen levels, they slow the growth of hormone receptor-positive cancer cells.
Patient Selection for Hormone Therapy
Choosing the right patients for hormone therapy is key. It involves looking at the cancer’s stage, grade, hormone receptor status, and the patient’s health. Hormone receptor-positive status is a major factor.
We consider hormone therapy for patients with advanced or recurring endometrial cancer. This is for those who have tried other treatments or have hormone receptor-positive tumors. The choice is made based on each patient’s needs and medical history.
Fertility-Sparing Treatment Options
Fertility-sparing treatments give hope to women with endometrial cancer who want to have kids later. For young patients with early-stage endometrial cancer, keeping fertility is key. We look into treatments that manage cancer and keep the dream of having children alive.
Medroxyprogesterone Acetate and Megestrol Acetate
Progestin therapy is a common choice for fertility-sparing treatment in endometrial cancer. Medroxyprogesterone acetate and megestrol acetate are two progestins used to treat endometrial cancer. They work by balancing estrogen’s effects on the endometrium, helping the cancer to shrink or even disappear for a while.
Research shows progestin therapy can be effective in treating early-stage endometrial cancer. It’s important to watch patients closely during and after treatment to prevent cancer from getting worse.
Levonorgestrel-Releasing Intrauterine Devices
LNG-IUDs are another option for fertility-sparing treatment. These devices release a progestin hormone directly into the uterus. This local release of progestin helps treat early-stage endometrial cancer while preserving fertility.
LNG-IUDs are effective in treating early-stage endometrial cancer. They are a good choice for patients who want to avoid systemic hormone therapy. The local delivery of progestin helps in shrinking the cancer while keeping fertility options open.
Patient Selection Criteria
Not all patients with endometrial cancer are good candidates for fertility-sparing treatments. Choosing the right patients is key to successful outcomes.
When selecting patients for fertility-sparing treatments, several criteria are considered:
Criteria | Description |
Early-stage disease | Patients with stage IA, grade 1 or 2 endometrial cancer are typically considered. |
Desire for fertility preservation | Patients who wish to conceive in the future. |
No deep myometrial invasion | Cancer that has not deeply invaded the uterine muscle. |
No evidence of metastasis | No spread of cancer to other parts of the body. |
By carefully evaluating these factors, healthcare providers can find patients most likely to benefit from fertility-sparing treatments. This gives them a chance to preserve their fertility while managing their cancer.
Emerging Treatments: Immunotherapy and Targeted Therapies
Immunotherapy and targeted therapies are new and promising for endometrial cancer. They could lead to better treatment results and fewer side effects.
Immune Checkpoint Inhibitors
Immune checkpoint inhibitors boost the immune system to fight cancer cells better. They work well in endometrial cancer, mainly in tumors with high microsatellite instability.
Key Benefits: They help the immune system attack cancer cells more effectively. This could lead to better survival rates.
Targeted Molecular Therapies
Targeted molecular therapies aim at specific genetic changes or proteins in cancer cells. In endometrial cancer, therapies targeting the PI3K/AKT/mTOR pathway show promise.
Clinical Trials and Research Developments
Clinical trials are testing immunotherapies and targeted therapies in endometrial cancer. These studies help find the best treatments and identify who might benefit most.
Treatment Type | Mechanism of Action | Potential Benefits |
Immune Checkpoint Inhibitors | Release brakes on the immune system to attack cancer cells | Improved survival rates, enhanced immune response |
Targeted Molecular Therapies | Target specific genetic mutations or proteins in cancer cells | Reduced side effects, improved treatment outcomes |
As research grows, we’ll see more tailored treatments for endometrial cancer. Using immunotherapy and targeted therapies could greatly improve patient results.
Multidisciplinary Approach to Treatment Planning
Creating personalized treatment plans for endometrial cancer patients is key. A team of experts, like gynecologic oncologists and radiation oncologists, work together. They ensure patients get the best care.
The Tumor Board Process
The tumor board is a vital part of this team effort. It’s a meeting where specialists share patient information and decide on treatment. This teamwork leads to better care plans.
At the tumor board, the team looks at patient data and talks about the cancer’s stage. They consider the patient’s health and other important factors. This helps decide on treatments like surgery or chemotherapy.
Personalized Treatment Plans
Each patient gets a treatment plan that fits their needs. The team considers the cancer’s details and the patient’s health. This way, they can offer the best chance of success.
Things like the cancer’s stage and the patient’s health goals matter. For example, a young woman might get treatments that help her keep her fertility.
Post-Treatment Surveillance and Follow-up
After treatment, patients need regular checks to watch for cancer return. They also get help with any lasting side effects. The follow-up plan is made to fit each patient’s needs.
Regular checks are key to catching problems early. They also help patients get support during the recovery. We work with patients to make sure they get the care they need.
Conclusion: Prognosis and Future Directions
Effective treatment for endometrial cancer can greatly improve a patient’s chances of recovery. The cancer’s stage and grade, along with the patient’s health, are key factors. These elements help determine the outcome.
We’ve looked at different treatment methods. These include surgery, radiation, chemotherapy, and hormone therapy. A team approach to treatment planning is vital. It helps doctors create personalized plans for each patient.
Research is moving forward, leading to better treatments. New therapies like immunotherapy and targeted molecular therapies are showing promise. The goal of finding a cure for uterine cancer is driving this progress.
FAQ
What is endometrial cancer and how is it treated?
Endometrial cancer starts in the uterus. Treatment depends on the cancer’s stage and type. It may include surgery, radiation, chemotherapy, or hormone therapy.
What are the common treatments for endometrial cancer?
Treatments include total hysterectomy and lymph node dissection. Radiation, chemotherapy, and hormone therapy are also used. The choice depends on the cancer’s stage and the patient’s health.
How is endometrial cancer staged?
The FIGO system is used to stage endometrial cancer. It looks at the tumor’s size, lymph nodes, and if it has spread. Accurate staging helps choose the best treatment.
What is the role of surgery in treating endometrial cancer?
Surgery is often the first step in treating endometrial cancer. It may involve removing the uterus and affected tissues. The goal is to remove the tumor.
What is radiation therapy and when is it used to treat endometrial cancer?
Radiation therapy kills cancer cells with high-energy rays. It’s used when cancer has spread or to lower the risk of it coming back after surgery.
How is chemotherapy used to treat endometrial cancer?
Chemotherapy kills cancer cells with medications. It’s used for cancer that has spread or to lower the risk of it coming back after surgery.
What is hormone therapy and how is it used to treat endometrial cancer?
Hormone therapy uses medications to affect hormone production. It’s used for hormone-receptor-positive cancer to slow or stop cancer cell growth.
Are there any fertility-sparing treatment options available for endometrial cancer?
Yes, options like medroxyprogesterone acetate and levonorgestrel-releasing intrauterine devices are available. They help treat cancer while preserving fertility.
What are the emerging treatments for endometrial cancer?
New treatments include immunotherapy and targeted therapies. They’re being tested in clinical trials to improve outcomes and reduce side effects.
Why is a multidisciplinary approach important in treating endometrial cancer?
A team approach ensures patients get the best care. It involves a variety of healthcare professionals working together.
What can I expect during post-treatment surveillance and follow-up?
After treatment, regular check-ups are needed. These include physical exams and imaging tests to watch for any signs of cancer coming back.
How can I find out more about clinical trials and research developments for endometrial cancer?
Look online for clinical trials or ask your healthcare team. They can provide information on studies and if you can participate.
Reference
Government Health Resource. Endometrial Cancer: Treatment Options and Early Detection. Retrieved from https://guidelines.esgo.org/media/2025/09/ESGO-ESTRO-ESP-Guidelines-for-EC_-LO-July-2025.pdf



































