Endometriosis is a condition where uterine-like tissue grows outside the uterus. It affects about 10% of women of reproductive age. This disease is a major cause of pelvic pain during menstruation and during sex. For many, vaginal pain is a big problem that hurts their life and relationships.endometriosis and vaginal pain10 Common Causes of Stomach Ache and Chest Pain: Symptoms and When to Get Help
Dealing with vaginal pain from endometriosis can be tough. But, there are ways to feel better. In this article, we’ll look at five methods doctors suggest to ease endometriosis-related vaginal pain.
Key Takeaways
- Understanding the causes and symptoms of endometriosis-related vaginal pain
- Exploring relief strategies recommended by healthcare providers
- Learning about innovative treatments for managing vulvar endometriosis
- Discovering lifestyle changes that can help alleviate symptoms
- Finding support for managing the emotional impact of endometriosis
Understanding Endometriosis and Its Prevalence
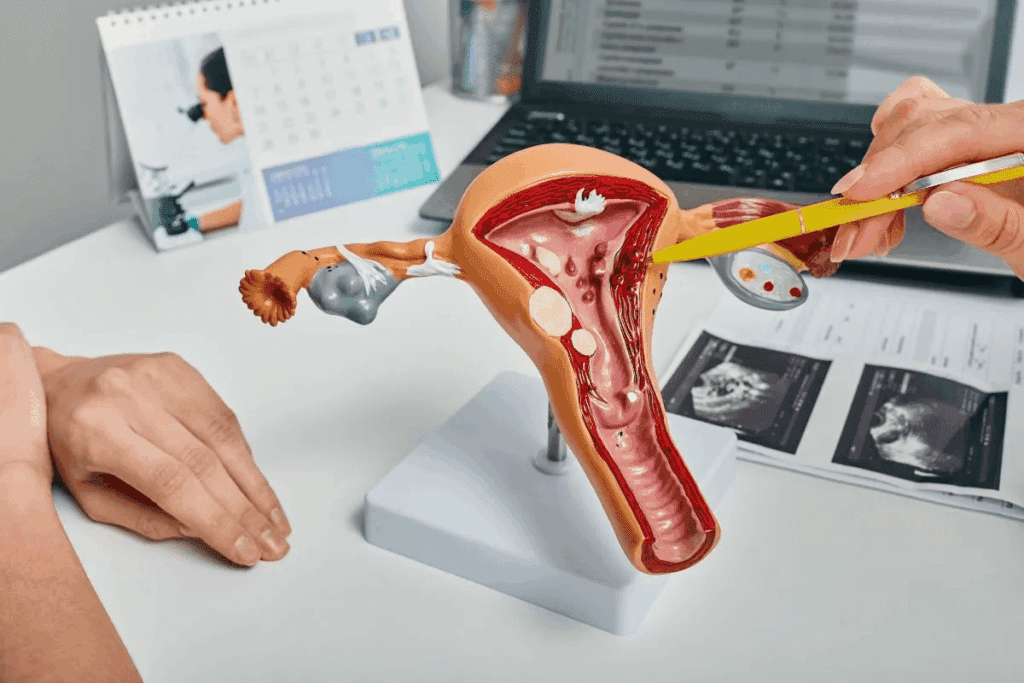
Endometriosis is a major cause of pelvic pain and infertility. It’s a health issue that needs a lot of attention. We’ll look at what it is, its symptoms, and how common it is, focusing on pelvic pain and infertility.
What Is Endometriosis?
Endometriosis is a chronic condition where endometrial tissue grows outside the uterus. This leads to inflammation, scarring, and adhesions. The misplaced tissue can cause painful periods, painful ovulation, chronic pelvic pain, and infertility. The exact cause is not known, but it’s thought to involve genetics, hormones, and environment.
The symptoms of endometriosis vary among women. Some common ones include:
- Painful periods (dysmenorrhea)
- Painful ovulation
- Chronic pelvic pain
- Painful bowel movements or urination during periods
- Painful penetrative sex
- Fatigue
- Digestive issues
- Infertility
Statistics and Demographics
Endometriosis affects about 1 in 10 women of reproductive age worldwide. In the United States, around 6.5 million women are affected. Research shows that in women with pelvic pain and infertility, endometriosis lesions are found 33 percent and 40 percent of the time, respectively.
Condition | Prevalence of Endometriosis |
Pelvic Pain | 33% |
Infertility | 40% |
Knowing how common endometriosis is helps healthcare providers treat it better. By understanding symptoms and risk factors, we can offer better care and support to those affected.
The Connection Between Endometriosis and Vaginal Pain

It’s important to understand how endometriosis and vaginal pain are connected. This knowledge helps in managing the condition effectively. Endometriosis can cause a lot of discomfort, and its effects on the vaginal area are key.
How Endometriosis Affects the Vaginal Area
Endometriosis can lead to painful lesions or endometriomas in the vaginal area. These can hurt during sex and before or during periods. Studies show that many women with endometriosis face challenges in their sex lives.
A 2023 study found that 80% of participants reported that endometriosis had a negative impact on their sex lives.
Types of Pain Experienced
Women with endometriosis may feel sharp vulvar pain, burning pain, and other vulvodynia symptoms. The pain can be different for everyone. Some feel sharp, stabbing pain, while others feel a burning sensation.
These symptoms can get worse during certain activities, like sex.
Type of Pain | Characteristics | Triggers |
Sharp Vulvar Pain | Stabbing or shooting pain | Sexual activity, menstruation |
Burning Pain | Continuous burning sensation | Hormonal changes, certain activities |
Cyclical Pain | Pain associated with menstrual cycle | Menstruation, ovulation |
Recent data shows that vulvar endometriomas are very painful. They often hurt during sex and before or during periods.
Vulvar Endometriomas and Related Conditions
Vulvar endometriomas are a rare but significant condition linked to endometriosis. They cause a lot of discomfort. These are painful, blood-filled cysts that form when endometrial tissue grows in the vulva, an area not usually affected by endometriosis.
Vulvar Endometriomas Explained
Vulvar endometriomas happen when endometrial tissue grows in the vulvar region. This can cause cysts or nodules that hurt, often during menstruation or sex. The exact reason for vulvar endometriomas is not fully known, but it’s thought to be due to abnormal endometrial cell growth in the vulvar area.
Symptoms include a painful vaginal opening, discomfort during sex, and visible swelling or lumps in the vulvar area. Doctors usually diagnose these cysts through a clinical exam and sometimes with imaging studies.
Comorbidity with Vulvodynia
There’s a strong link between endometriosis and vulvodynia, with about 11 percent of those with endometriosis also having vulvodynia. Vulvodynia is chronic pain in the vulvar area without a clear cause. Its symptoms can be similar to or worse with vulvar endometriomas.
Vulvodynia symptoms include burning, stinging, or rawness in the vulvar area. These can be constant or triggered by touch or pressure. Treating vulvodynia often involves pain meds, pelvic floor therapy, and changes in lifestyle.
It’s important to understand the connection between vulvar endometriomas and vulvodynia for better care. By tackling both physical and emotional symptoms, healthcare providers can greatly improve patients’ lives.
Impact of Endometriosis and Vaginal Pain on Quality of Life
Women with endometriosis face more than just physical pain. It affects their overall well-being. It impacts their sexual health, intimacy, and emotional stability.
Effects on Sexual Health and Intimacy
Endometriosis can cause big problems with sex and intimacy. The pain, including at the vaginal opening, makes sex hard or impossible. A 2023 study showed 80 percent of women said endometriosis hurt their sex lives.
This can hurt relationships and emotional health. It’s key to talk about sexual health when dealing with endometriosis. Doctors can help manage pain and improve intimacy.
“The pain and discomfort associated with endometriosis can significantly impact a woman’s sexual health and intimacy, affecting her relationship with her partner and her overall quality of life.”
Psychological and Emotional Impacts
Endometriosis’ chronic pain affects the mind and emotions too. Women might feel anxious, depressed, and isolated. The ongoing pain can cause emotional distress, affecting daily life.
It’s important to recognize the mental toll of endometriosis. Seeking help from mental health experts is vital. They can offer ways to deal with the emotional side of the condition.
Aspect of Life | Impact of Endometriosis |
Sexual Health | Painful vaginal opening, discomfort during sex |
Intimacy | Strained relationships due to pain |
Psychological Well-being | Anxiety, depression, emotional distress |
It’s key to understand how endometriosis affects life. By tackling both physical and emotional sides, women can manage their condition better.
Diagnosing the Source of Vaginal Pain
Finding the cause of vaginal pain is key to treating endometriosis. It takes both medical checks and what the patient says. This mix helps pinpoint the pain’s source.
Medical Evaluations and Tests
First, doctors look at your medical history and do a physical check. They might do a pelvic exam to find any issues or pain. Ultrasound or MRI scans can show the organs and find endometriosis spots or cysts.
At times, a laparoscopy is needed. This surgery lets doctors see the implants up close. They make a small cut in the belly to look at the pelvic area.
Communicating Effectively with Healthcare Providers
Talking well with doctors is important for a right diagnosis. Patients should tell their doctors about their pain. This includes if it’s burning or throbbing, how often, and what makes it better or worse.
“The key to diagnosing vulvodynia and related conditions lies in understanding the patient’s pain narrative,” says Medical Expert, a leading specialist in endometriosis. “By listening carefully to their symptoms and medical history, we can tailor our diagnostic approach to their specific needs.”
Keeping a pain diary helps track symptoms. This can be very useful when talking to doctors.
With detailed medical checks and good communication, we can find the cause of vaginal pain. Then, we can make a plan to treat it.
Strategy 1: Medical Treatments for Endometriosis Vaginal Pain
Medical treatments are a key way to fight endometriosis vaginal pain. They aim to lessen symptoms, boost quality of life, and ease pain caused by endometriosis.
Hormonal Therapy Options
Hormonal therapies are a common treatment for endometriosis. They work by cutting down on endometrial tissue growth, which reduces pain. These treatments change the body’s hormonal balance, often by lowering estrogen levels. This helps slow down endometrial tissue growth.
Some hormonal therapy options include:
- Birth Control Pills: These can lessen menstrual cramps and make periods lighter, which helps reduce pain.
- Gonadotropin-Releasing Hormone (GnRH) Agonists: These meds cut down estrogen production, slowing endometrial tissue growth.
- Progestins: Synthetic progestins help slow down endometrial tissue growth and are used to treat endometriosis.
Hormonal Therapy | Mechanism of Action | Benefits |
Birth Control Pills | Regulate hormones to reduce menstrual cramps | Reduces pain, lightens periods |
GnRH Agonists | Reduce estrogen production | Decreases growth of endometrial tissue, reduces pain |
Progestins | Reduce growth of endometrial tissue | Effective in treating endometriosis, reduces pain |
Pain Management Medications
Pain management meds are also key in treating endometriosis pain. They range from over-the-counter options to stronger prescription drugs.
Some common pain management options include:
- Over-the-Counter Pain Relievers: Such as ibuprofen or naproxen, which can lessen pain and swelling.
- Prescription Pain Medications: For severe pain, stronger prescription meds may be needed.
It’s vital for patients to work closely with their healthcare providers. This helps find the best treatment plan, as everyone reacts differently to treatments.
Strategy 2: Surgical Approaches for Pain Relief
Surgical methods, like laparoscopic excision, can help with endometriosis pain. They are a good option for those with severe symptoms. We’ll look at how laparoscopic excision works and what recovery is like.
Laparoscopic Excision of Endometriosis
Laparoscopic excision is a small surgery to remove endometrial lesions. It’s seen as the best treatment for severe symptoms. The surgery uses small cuts in the belly to insert tools to find and remove growths.
Medical Expert, “Laparoscopic excision is a highly effective method for treating endometriosis, giving patients a chance at significant pain relief.” This shows how important this surgery is.
Recovery and Post-Surgical Care
Recovery time from laparoscopic excision varies, but most women can get back to normal in a few weeks. It’s key to follow the care instructions to avoid problems and help healing. This includes not lifting heavy, eating right, and going to check-ups.
During recovery, patients learn about managing pain and watching for complications. Talking well with doctors is very important.
In summary, surgeries like laparoscopic excision can greatly help women with endometriosis pain. Knowing about the surgery and recovery helps patients make better choices for their care.
Strategy 3: Physical Therapy and Rehabilitation
Physical therapy is now seen as a key way to fight endometriosis pain. It uses rehabilitation methods to help manage vaginal pain from endometriosis.
Pelvic Floor Therapy Techniques
Pelvic floor therapy focuses on the muscles around the pelvic area. It uses special techniques to ease pain and improve life for those with endometriosis. These include manual therapy, biofeedback, and exercises made just for you.
Manual therapy uses hands-on methods to relax muscles, boost blood flow, and cut down pain. Biofeedback helps you feel and control your pelvic muscles, which is great for pain management. Therapeutic exercises strengthen the pelvic floor, boost flexibility, and lessen discomfort.
At-Home Exercises for Pain Management
At-home exercises also help manage pain. Simple yet powerful exercises can be added to your daily routine to ease endometriosis pain. These might include pelvic tilts, bridges, and Kegel exercises to strengthen the pelvic floor and enhance pelvic health.
It’s vital to talk to a healthcare provider or physical therapist to create a plan that fits your needs. With professional advice and regular practice at home, you can manage your pain better and live a fuller life.
Strategy 4: Lifestyle Modifications and Self-Care
Self-care and lifestyle changes can help reduce endometriosis vaginal pain. Managing endometriosis needs a mix of medical treatments, lifestyle changes, and self-care. By making smart choices, people can lessen the pain from endometriosis.
Dietary Changes That May Reduce Inflammation
Changing your diet can help manage endometriosis symptoms. Increasing omega-3 intake and cutting down on saturated fats can reduce inflammation. Omega-3s, found in salmon and flaxseeds, are anti-inflammatory. Also, eating more fruits, vegetables, and whole grains can boost health and lessen pain.
Some foods can increase inflammation. A diet low in processed foods and high in antioxidants may help. Keeping a food diary helps find out which foods worsen symptoms, leading to better choices.
Stress Management and Pain Reduction
Managing stress is key to handling endometriosis vaginal pain. High stress can make symptoms worse. Techniques like mindfulness meditation, yoga, and deep breathing can help reduce stress and promote calm.
Regular exercise is also good. It can lower stress, improve mood, and possibly reduce pain. It’s important to pick activities that are fun and fit your energy level.
By adding these lifestyle changes and self-care practices, people with endometriosis may see a big improvement in their pain and overall well-being.
Strategy 5: Complementary and Alternative Approaches
Complementary and alternative methods can help with endometriosis vaginal pain. They can be used with traditional treatments to better manage pain and improve life quality.
Evidence-Based Complementary Therapies
Acupuncture has shown promise in managing endometriosis symptoms. It may help reduce pain and improve well-being. Studies suggest it can balance hormones and reduce inflammation, helping with pain management.
Herbal medicine is also of interest for its anti-inflammatory properties. But, it’s important to talk to a healthcare provider before trying herbal remedies. They can interact with other treatments or have side effects.
Therapy | Description | Potential Benefits |
Acupuncture | Ancient practice involving the insertion of thin needles into specific body points | Reduced pain, improved hormonal balance |
Herbal Medicine | Use of plants or plant extracts for medicinal purposes | Anti-inflammatory effects, symptom relief |
Mindfulness Meditation | Practice of focusing on the present moment to reduce stress | Reduced stress, improved pain management |
Home Remedies and Comfort Measures
Home remedies and comfort measures can also offer relief. Applying heat therapy or using warm baths can relax muscles and reduce pain. Some find relief through dietary changes, like avoiding inflammatory foods.
It’s key to work with a healthcare provider to find the right mix of treatments for your needs.
Conclusion: Creating a Personalized Pain Management Plan
Creating a personalized pain management plan is key for managing endometriosis-related vaginal pain. Women with endometriosis can find relief by using different strategies. This approach improves their quality of life.
We’ve looked at many ways to handle endometriosis vaginal pain. These include medical treatments, surgery, physical therapy, lifestyle changes, and natural therapies. A good plan involves working with healthcare providers to find the best mix of these options for each person.
By tailoring their approach to managing endometriosis, women can control their symptoms better. This reduces pain and boosts their overall health. Personalized pain management helps people take charge of their lives and make smart choices about their care.
FAQ
What is endometriosis and how does it cause vaginal pain?
Endometriosis is when tissue like the uterus lining grows outside the uterus. This causes inflammation and pain. When this tissue grows near the vagina, it leads to pain and discomfort during sex.
What are vulvar endometriomas and how are they related to endometriosis?
Vulvar endometriomas are rare growths of endometrial tissue on the vulva. They are linked to endometriosis and can cause pain and discomfort in the vulvar area.
Can endometriosis cause vulvodynia symptoms?
Yes, endometriosis can cause vulvodynia symptoms. Women with endometriosis may feel burning, sharp, or throbbing pain in the vulva.
How is endometriosis-related vaginal pain diagnosed?
Diagnosing this pain involves a detailed medical check-up. This includes a physical exam, medical history, and sometimes imaging tests or laparoscopy to confirm endometriosis.
What are the treatment options for endometriosis-related vaginal pain?
Treatments include hormonal therapy, pain meds, and surgery like laparoscopic excision. Physical therapy and lifestyle changes are also options.
Can dietary changes help reduce endometriosis-related pain?
Yes, eating more omega-3 fatty acids and avoiding inflammatory foods can help. Staying hydrated also reduces inflammation and pain.
How can stress management techniques help with endometriosis-related pain?
Stress management like meditation, yoga, or deep breathing can reduce stress. This helps relax and may ease endometriosis pain.
Are there any complementary therapies that can help with endometriosis-related pain?
Yes, therapies like acupuncture, physical therapy, and cognitive-behavioral therapy can manage pain. They also improve overall well-being.
What is the role of pelvic floor therapy in managing endometriosis-related pain?
Pelvic floor therapy relaxes pelvic muscles, improves circulation. It reduces pain and discomfort from endometriosis.
How can I create a personalized pain management plan for endometriosis-related vaginal pain?
To create a plan, work with your healthcare provider. Combine medical treatments, lifestyle changes, and complementary therapies that fit your needs and preferences.
National Center for Biotechnology Information. Enlarged Ovary: Causes, Diagnosis, and Treatment Options. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC10047373/.

































