Calcium Pyrophosphate Deposition Disease (CPPD) is a type of arthritis that affects millions, mostly those over 60. It happens when calcium pyrophosphate dihydrate crystals build up in joint cartilage. This causes painful inflammation, making it hard to tell it apart from osteoarthritis or rheumatoid arthritis what causes calcium pyrophosphate deposition disease.
We are getting to know more about CPPD, a condition often not well understood. Studies show that an imbalance in pyrophosphate and pyrophosphatase levels in cartilage leads to it. Understanding the underlying factors is key to managing it well.
Key Takeaways
- CPPD is a type of crystal arthropathy affecting synovial and periarticular tissues.
- It is characterized by the accumulation of calcium pyrophosphate dihydrate crystals in joint cartilage.
- CPPD can cause painful inflammation and joint pain.
- The exact cause remains unknown, but research points to an imbalance in pyrophosphate production and pyrophosphatase levels.
- Understanding CPPD is essential for effective management and treatment.
Understanding Calcium Pyrophosphate Deposition Disease (CPPD)
CPPD is a unique condition in medicine. It has different forms, from sudden to long-lasting. It causes calcium pyrophosphate dihydrate crystals to build up in joints, leading to various symptoms.
Definition and Basic Pathology
Calcium Pyrophosphate Deposition Disease (CPPD) is a form of arthritis. It happens when calcium pyrophosphate dihydrate crystals build up in joints. This can cause pain, stiffness, and damage to the joints.
Key aspects of CPPD pathology include:
- Crystal deposition in joints
- Inflammatory response to crystal deposition
- Joint damage and degeneration
Pseudogout vs. CPPD: Clarifying the Terminology
CPPD is also known as pseudogout because it looks like gout. But CPPD covers more, including both sudden and long-term forms. Pseudogout is just the sudden, painful form of CPPD.
“The term CPPD is preferred over pseudogout because it encompasses the full spectrum of the disease, including chronic forms and asymptomatic crystal deposition.”
It’s important to know the difference between CPPD and pseudogout. This helps doctors give the right treatment. Recognizing CPPD as a broader condition helps manage it better.
The Pathophysiology of CPPD
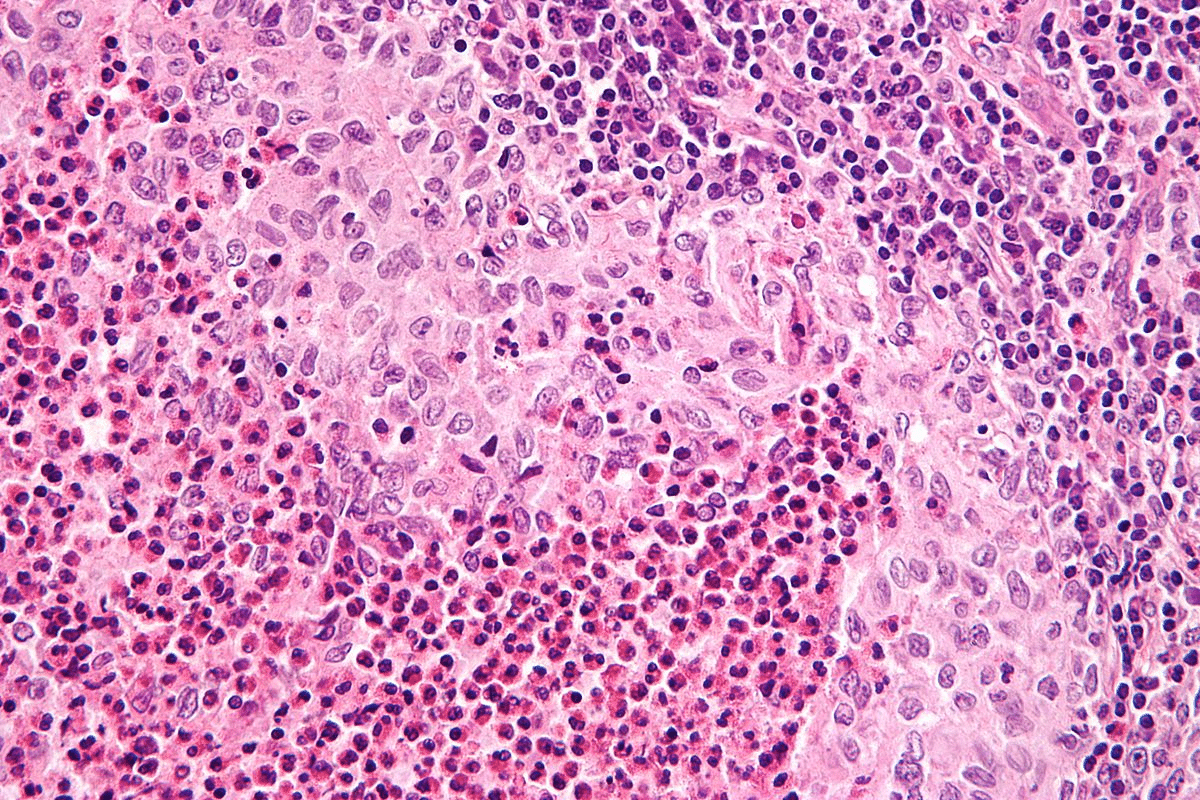
CPPD, or Calcium Pyrophosphate Deposition Disease, involves a complex process. This process leads to crystals forming in the cartilage. Knowing how this happens is key to finding good treatments.
Crystal Formation Process
The formation of calcium pyrophosphate crystals is a major part of CPPD. Calcium crystals form in the cartilage when there’s an imbalance. This imbalance causes calcium pyrophosphate dihydrate crystals to build up, which are typical of CPPD.
We’ll look at what causes this imbalance. We’ll see how it leads to CPPD crystals in the cartilage.
Pyrophosphate Metabolism Imbalance
An imbalance in pyrophosphate metabolism is key to CPPD. Pyrophosphate is a byproduct of cell processes. In normal cartilage, its levels are well-controlled. But in CPPD, this control is lost, causing pyrophosphate levels to rise. This rise leads to the formation of calcium pyrophosphate crystals.
|
Condition |
Effect on Pyrophosphate Metabolism |
Outcome |
|---|---|---|
|
Normal Cartilage |
Regulated pyrophosphate levels |
No crystal formation |
|
CPPD |
Elevated pyrophosphate levels |
Calcium pyrophosphate crystal formation |
Inflammatory Response to Crystal Deposition
The presence of calcium pyrophosphate crystals in the cartilage triggers an inflammatory response. This is a key feature of CPPD. The response includes the activation of immune cells and the release of pro-inflammatory mediators. This leads to joint inflammation and pain.
We’ll explore how understanding this inflammatory response can help in treating CPPD.
What Causes Calcium Pyrophosphate Deposition Disease?
CPPD is a complex condition affecting joints. It can be caused by different factors. We will look at the main causes and risk factors, including metabolic and genetic conditions.
Primary (Idiopathic) CPPD
Primary CPPD happens without a known cause. It often affects older people and can occur in those who seem healthy.
Secondary CPPD
Secondary CPPD is linked to metabolic and endocrine disorders. Conditions like hyperparathyroidism, hemochromatosis, and hypophosphatasia raise the risk of CPPD.
- Hyperparathyroidism disrupts calcium and phosphate balance.
- Hemochromatosis, with too much iron, can lead to CPPD.
- Hypophosphatasia, a rare genetic disorder, also increases risk.
Genetic Factors
Genetics also play a big role in CPPD. Certain genetic mutations can affect pyrophosphate metabolism. This increases the risk of crystal deposition.
In summary, CPPD can be caused by a mix of primary and secondary factors. These include metabolic disorders and genetic predispositions. Knowing the causes is key to managing and treating the disease effectively.
Metabolic Conditions Associated with CPPD
Calcium Pyrophosphate Deposition Disease (CPPD) is a complex condition. It is often linked to various metabolic abnormalities. These include those affecting mineral and bone metabolism. These conditions can significantly influence the development and progression of CPPD.
Hyperparathyroidism
Hyperparathyroidism is a condition where the body makes too much parathyroid hormone (PTH). PTH helps regulate calcium levels in the blood. High levels of PTH can cause hypercalcemia. This can lead to the deposition of calcium pyrophosphate crystals in joints, increasing the risk of CPPD.
Hemochromatosis
Hemochromatosis is a genetic disorder that causes the body to absorb too much iron from food. This leads to iron overload. The condition can affect various organs and is associated with an increased risk of CPPD. The excess iron can influence the metabolism of pyrophosphate, contributing to crystal formation.
Hypophosphatasia
Hypophosphatasia is a rare genetic disorder. It is characterized by defective bone mineralization due to low alkaline phosphatase activity. This condition can lead to the accumulation of inorganic pyrophosphate. Inorganic pyrophosphate is a key component of CPPD crystals. This links hypophosphatasia to an increased risk of developing CPPD.
Understanding these metabolic conditions is key to managing CPPD effectively. By identifying and addressing the underlying metabolic abnormalities, healthcare providers can develop more targeted treatment strategies.
|
Metabolic Condition |
Effect on CPPD Risk |
Key Mechanism |
|---|---|---|
|
Hyperparathyroidism |
Increased risk due to hypercalcemia |
Elevated PTH levels |
|
Hemochromatosis |
Increased risk due to iron overload |
Influence on pyrophosphate metabolism |
|
Hypophosphatasia |
Increased risk due to defective bone mineralization |
Accumulation of inorganic pyrophosphate |
By recognizing the metabolic conditions associated with CPPD, we can better understand the disease’s pathophysiology. This improves patient outcomes through more effective management strategies.
Electrolyte Abnormalities Contributing to CPPD
Electrolyte imbalances are key in the growth of Calcium Pyrophosphate Deposition Disease (CPPD). These issues can change how CPPD crystals form and how severe the disease is.
Hypomagnesemia
Hypomagnesemia, or low magnesium, is linked to CPPD. Magnesium helps control calcium levels, and not enough of it can lead to more CPPD crystals. Magnesium supplements are often used to treat CPPD and lessen attack risks.
“Magnesium deficiency can make CPPD worse by increasing crystal formation,” say rheumatology experts.
Gitelman Syndrome
Gitelman syndrome is a rare genetic disorder that causes low magnesium and other electrolyte problems. It raises the risk of CPPD because of these imbalances. Patients with Gitelman syndrome need to manage their electrolytes carefully to avoid CPPD.
Gitelman syndrome shows how important electrolyte balance is for preventing CPPD. Keeping electrolyte levels in check is key to stopping CPPD crystals from forming.
Familial Hypocalciuric Hypercalcemia
Familial hypocalciuric hypercalcemia (FHH) is a genetic issue that affects calcium levels, causing high calcium. This can lead to CPPD by changing the body’s calcium balance. Knowing the genetic causes of FHH is important for managing CPPD risk in those affected.
FHH leads to lifelong high calcium levels, which can affect CPPD crystal formation. It’s important to recognize this condition to give the right care and lower CPPD risk.
In summary, electrolyte problems like hypomagnesemia, Gitelman syndrome, and FHH are big factors in CPPD. Understanding and fixing these imbalances is key to treating CPPD and avoiding complications.
Age as a Primary Risk Factor
As people get older, their chance of getting Calcium Pyrophosphate Deposition Disease (CPPD) goes up. This makes age a key factor in understanding CPPD. We’ll look at how age affects the risk of CPPD and why older adults are more likely to get it.
Prevalence Across Age Groups
CPPD becomes more common with age. Research shows it’s more common in older people. The risk starts to rise in the sixth decade of life.
|
Age Group |
Prevalence of CPPD |
|---|---|
|
40-49 years |
Low |
|
50-59 years |
Moderate |
|
60-69 years |
High |
|
70+ years |
Very High |
This table shows how CPPD becomes more common with age. It points out the strong link between CPPD and older age groups.
Why Elderly Populations Are More Susceptible
Several reasons make older people more likely to get CPPD. These include changes in pyrophosphate metabolism with age. Also, older people are more likely to have metabolic conditions. And, they tend to have more calcium pyrophosphate crystals in their joints over time.
It’s important to understand these factors for diagnosing and treating CPPD in older adults. We’ll keep exploring the clinical aspects of CPPD in the next sections.
Clinical Presentation and Diagnosis
CPPD can show different symptoms, making it hard to diagnose without the right tools. This condition, also known as calcium pyrophosphate deposition disease, causes calcium crystals to build up in joints. This leads to various symptoms.
Common Symptoms
People with CPPD often feel pain and swelling in their joints. These can be short-term or long-lasting. The knees, wrists, and hips are usually affected.
Some may get pseudogout, which is sudden, severe pain and swelling. This is often seen with redness and warmth around the joint.
Diagnostic Methods
To diagnose CPPD, doctors use a few methods. They look at the patient’s symptoms, use imaging like X-rays and MRI, and check the joint fluid. Finding calcium pyrophosphate dihydrate crystals in the fluid confirms CPPD.
|
Diagnostic Method |
Description |
Key Findings in CPPD |
|---|---|---|
|
X-ray |
Imaging technique to assess joint damage and calcification |
Chondrocalcinosis, joint space narrowing |
|
Synovial Fluid Analysis |
Analysis of fluid aspirated from the joint |
Presence of calcium pyrophosphate dihydrate crystals |
|
Ultrasound |
Imaging technique to evaluate joint inflammation and crystal deposition |
Hyperechoic deposits within the cartilage |
In conclusion, diagnosing CPPD needs a detailed approach. This includes looking at symptoms, using imaging, and analyzing joint fluid. Knowing the symptoms and using the right tests are key to diagnosing and treating CPPD.
Treatment Approaches for CPPD
Understanding the different treatment options for CPPD is key. The main goal is to manage acute attacks, prevent future crystal formation, and treat any underlying conditions.
Managing Acute Attacks
To tackle acute CPPD attacks, doctors often prescribe anti-inflammatory drugs. Nonsteroidal anti-inflammatory drugs (NSAIDs) are usually the first choice. Sometimes, colchicine is used when NSAIDs can’t be given.
Long-term Management Strategies
For long-term management, the focus is on reducing attack frequency and severity. Medications that lower urate levels are being explored. Making lifestyle changes, like diet and weight management, is also important.
Addressing Underlying Conditions
It’s vital to identify and treat conditions that make CPPD worse. This includes hyperparathyroidism, hemochromatosis, and hypophosphatasia. Treating these can help lessen CPPD symptoms.
Conclusion
Calcium pyrophosphate deposition disease (CPPD) is a complex condition. It is influenced by many factors, including metabolic and genetic conditions, electrolyte abnormalities, and age. Knowing what causes CPPD is key to effective patient care.
We have looked into CPPD’s different aspects. This includes its pathophysiology, clinical presentation, and diagnosis. The condition is marked by calcium pyrophosphate crystals in joints, causing inflammation and damage. Metabolic conditions like hyperparathyroidism and hemochromatosis can lead to CPPD.
Understanding CPPD’s causes helps healthcare providers create better treatment plans. Managing acute attacks and treating underlying conditions are vital for better patient outcomes. By grasping the complexities of CPPD, we can offer more effective care and support to those affected.
FAQ
What is Calcium Pyrophosphate Deposition Disease (CPPD)?
CPPD is a type of arthritis. It happens when calcium pyrophosphate crystals build up in joints. This is also known as pseudogout or calcium pyrophosphate arthropathy.
What is the difference between CPPD and pseudogout?
CPPD is a term for the condition where calcium pyrophosphate crystals form in joints. Pseudogout is when these crystals cause sudden inflammation in the joints.
What causes the formation of calcium pyrophosphate crystals in CPPD?
The buildup of these crystals is due to an imbalance in pyrophosphate metabolism. This imbalance can be caused by genetics, metabolic conditions, and age.
What are the metabolic conditions associated with an increased risk of developing CPPD?
Certain conditions like hyperparathyroidism, hemochromatosis, and hypophosphatasia increase the risk of CPPD. These conditions affect calcium and pyrophosphate metabolism.
How does age affect the risk of developing CPPD?
Age is a big risk factor for CPPD. As people get older, the risk goes up. This is because more crystals build up over time and joints change with age.
What are the common symptoms of CPPD?
Symptoms of CPPD include joint pain, swelling, and stiffness. These can affect the knee, wrist, or other joints. Symptoms can be mild or severe and can last a short time or be ongoing.
How is CPPD diagnosed?
Doctors diagnose CPPD by looking at symptoms, doing X-rays, and analyzing joint fluid. They look for calcium pyrophosphate crystals.
What are the treatment approaches for managing CPPD?
Treatment for CPPD includes using anti-inflammatory drugs for acute attacks. Long-term, doctors try to reduce crystal buildup. They also treat any metabolic conditions that contribute to the disease.
Can CPPD be prevented?
While you can’t prevent CPPD completely, managing metabolic conditions and staying healthy can help. Watching for early signs can also reduce its impact.
What is the role of electrolyte abnormalities in CPPD?
Electrolyte issues like hypomagnesemia can lead to CPPD. This is because they affect pyrophosphate metabolism and crystal formation.
References
Government Health Resource. Evidence-Based Medical Guidance. Retrieved from https://www.njmonline.nl/getpdf.php


































