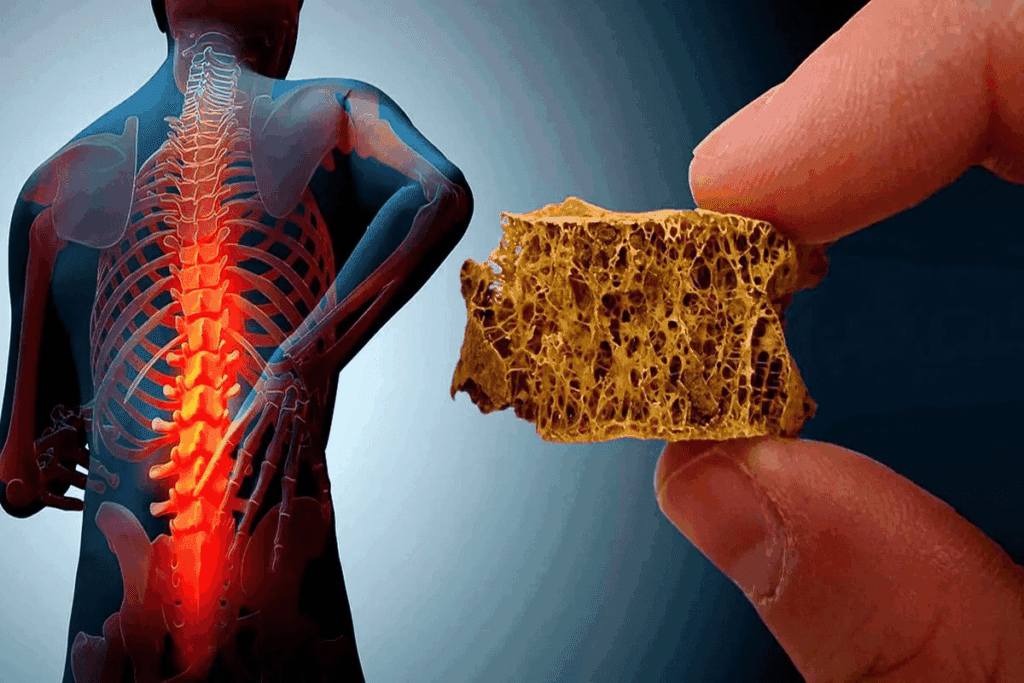
Estrogen is key in keeping our bones healthy. It controls the cells that build and break down bones.Estrogen bone density has a surprising, critical link. This vital guide explains how low estrogen leads to bone loss and how to protect yourself.
As we get older, estrogen levels drop, which is a big problem during menopause. This drop raises the risk of weak bones and fractures. It’s important to know how estrogen and bone density are connected to keep our bones strong.
At Liv Hospital, we offer deep insights into this important topic. We combine expert knowledge with care focused on you. This helps you make smart choices about your bone health.
Key Takeaways
- Estrogen regulates bone metabolism and density.
- Declining estrogen levels increase the risk of osteoporosis.
- Understanding estrogen’s role is critical for bone health.
- Estrogen affects bone formation and resorption.
- Menopause is a key time for bone health because estrogen levels drop.
The Critical Relationship Between Estrogen and Skeletal Health
Estrogen has a big impact on our bones. It helps with bone growth and breaking down. We’ll see how estrogen keeps our bones strong.
Defining Estrogen’s Role in the Body
Estrogen helps our bones by boosting osteoblasts. These cells build new bone. It’s key for keeping bones healthy.
When estrogen goes down, bones start to lose more. This is a big problem for women after menopause. They are more likely to get osteoporosis.
Overview of Bone Metabolism
Bones are always being remade. Osteoblasts build bones, while osteoclasts break them down. This is called bone remodeling.
Using estrogen can help prevent osteoporosis. It stops bones from losing calcium by slowing down osteoclasts. This shows how important estrogen is for our bones.
Understanding Estrogen Bone Density Connections
The link between estrogen and bone density is quite complex. It involves many cellular processes that affect bone health. Estrogen is key in keeping bones strong, and without it, the risk of osteoporosis and fractures goes up. We’ll look into how estrogen affects bone cells and what it means for our bones.
How Estrogen Maintains Bone Mass
Estrogen helps keep bones healthy by controlling bone cells. Osteoblasts build bones, and osteoclasts break them down. Estrogen boosts osteoblasts, helping bones grow, and slows down osteoclasts, reducing bone loss.
The Cellular Mechanisms of Estrogen in Bone Tissue
Estrogen works on bone cells in several ways. It lowers RANKL expression in bone cells, which helps prevent bone loss. It also helps the body absorb more calcium, which is good for bones.
The table below shows how estrogen affects bone cells and calcium:
Mechanism | Effect on Bone Health |
Suppression of RANKL expression | Reduced bone resorption |
Promotion of osteoblast activity | Enhanced bone formation |
Enhanced duodenal calcium absorption | Increased calcium availability for bone health |
It’s important to understand how estrogen and bones interact. This knowledge helps in finding better treatments for osteoporosis.
The Global Impact of Osteoporosis
Osteoporosis affects over 200 million people worldwide, making it a major health issue. It weakens bones, leading to a higher risk of fractures. This condition has big effects on individuals, healthcare, and the economy.
Prevalence Statistics Worldwide
Osteoporosis is common, with more cases as people get older. Studies show over 200 million people have it, with many being postmenopausal women. The drop in estrogen during menopause increases their risk.
Region | Prevalence of Osteoporosis | Affected Population |
North America | 15% | Approximately 44 million |
Europe | 12% | Around 61 million |
Asia | 10% | Nearly 100 million |
Higher Risk Factors for Women
Women, and those who have gone through menopause, face a higher risk of osteoporosis. This is because estrogen helps keep bones strong, and its decrease leads to bone loss. Other factors include family history, low BMI, smoking, and not being active.
Biological Mechanisms: How Estrogen Regulates Bone Metabolism
Estrogen is key in keeping bones healthy through several ways. We’ll see how it affects bone cells to keep our skeletons strong.
Osteoblast Activity Promotion
Estrogen boosts osteoblast activity, helping bones grow. Osteoblasts are cells that build bone. Estrogen makes these cells work better, making bones denser.
Studies show estrogen receptors in osteoblasts. This lets estrogen directly help these cells. So, estrogen keeps bones healthy by making osteoblasts more active.
Inhibition of Osteoclast Function
Estrogen also slows down osteoclasts, which break down bone. Estrogen’s effect on osteoclasts helps balance bone growth and breakdown.
Research finds estrogen can make osteoclasts die. This reduces bone breakdown. Estrogen’s effect on both bone-building and breaking cells is vital for bone health.
RANKL Suppression Pathway
Estrogen lowers RANKL in bone cells, which controls osteoclasts. The RANKL/RANK/OPG pathway is important for bone breakdown. By lowering RANKL, estrogen reduces bone breakdown.
This pathway is a big way estrogen keeps bones healthy. Knowing about it helps us find new treatments for bone problems.
Mechanism | Effect on Bone | Cell Type Involved |
Osteoblast Activity Promotion | Increased Bone Formation | Osteoblasts |
Inhibition of Osteoclast Function | Reduced Bone Resorption | Osteoclasts |
RANKL Suppression Pathway | Reduced Osteoclast Activation | Bone Lining Cells, Osteoclasts |
Estrogen’s Role in Calcium Regulation
Estrogen plays a key role in how our bodies absorb and use calcium. This is important for keeping our bones strong. We’ll look into how estrogen affects calcium, which is vital for bone health.
Calcium Absorption and Utilization
Estrogen helps our bodies absorb more calcium by affecting PMCA1b, a calcium pump. This helps in fighting osteoporosis. Research shows estrogen’s role in calcium absorption and use is key for bone health.
Estrogen also controls genes that help transport calcium. This is important for bone health and other bodily functions that need calcium.
Parathyroid Hormone Interaction
Estrogen and parathyroid hormone (PTH) work together to regulate calcium. PTH helps keep calcium levels in the blood right. Estrogen affects how PTH is made and works, which is important for calcium balance.
This balance is key for bone health and other body functions.
Vitamin D Metabolism and Estrogen
Vitamin D and estrogen are closely linked in calcium regulation. Estrogen affects enzymes in vitamin D metabolism, which impacts calcium absorption. Vitamin D is vital for gut calcium absorption, showing estrogen’s role in bone health.
Understanding estrogen, calcium, and vitamin D’s relationship helps us grasp bone health better. This knowledge is essential for fighting bone diseases.
Menopause and Accelerated Bone Loss
When women reach menopause, their bones start losing density faster. This is because estrogen levels drop, which is bad for bones. This period is key for keeping bones strong, as estrogen helps maintain bone health.
Timeline of Bone Density Changes
Menopause brings big changes to bone density. Estrogen levels drop, causing bones to lose density quickly. Some women lose up to 2-3% of bone density each year in the first few years after menopause.
The rate of bone loss varies by person. But, the biggest loss happens in the early years after menopause. This is because estrogen levels drop sharply.
Quantifying Bone Mineral Density Loss
Studies show that bone loss can be 9.1 percent at the femoral neck and 10.6 percent at the lumbar spine over 10 years after menopause. This highlights the need to watch bone health closely during this time.
Measuring bone loss is key to understanding osteoporosis risk. Doctors use tests to track bone density changes. This helps them decide on treatments.
Transition Phases and Bone Health Implications
The start of menopause brings big changes in hormones. These changes affect bones, making them more prone to loss. Estrogen’s protective role in bones weakens, leading to more bone breakdown and less formation.
It’s important to understand how these changes affect bones. This knowledge helps in finding ways to prevent bone loss. Changes in lifestyle, diet, and sometimes medicine can help support bone health during and after menopause.
Clinical Consequences of Estrogen Deficiency
Estrogen deficiency has big effects on bone health. It shows how important estrogen is for keeping bones strong and healthy.
Increased Fracture Risk Assessment
One big problem with estrogen deficiency is a higher risk of fractures. Women with low estrogen are more likely to break bones. This can really hurt their quality of life.
We use tests and assessments to check fracture risk. These tools help us understand how estrogen affects bones.
Studies show that very low estrogen levels raise fracture risk a lot. This shows why keeping estrogen levels right is key for bone health.
Bone Quality Changes
Estrogen deficiency also changes bone quality. Bones become weaker and more likely to break. We study these changes to find new ways to help bones.
Correlation Between Estradiol Levels and Bone Health
There’s a strong link between estradiol levels and bone health. Estradiol helps keep bones strong, and low levels increase fracture risk. We’re learning more about how estradiol affects bones.
Estradiol Levels (pg/ml) | Fracture Risk | Bone Mineral Density |
<5 | 2.5-fold increase | Reduced |
5-10 | Moderate risk | Preserved |
>10 | Low risk | Normal |
Understanding estrogen deficiency helps us manage bone health better. We see how important it is to keep estrogen levels up and watch bone health closely.
Diagnostic Approaches for Bone Health Assessment
Diagnostic methods are key in checking bone health and stopping osteoporotic fractures. It’s important to find out who’s at risk early. This way, we can start the right treatments.
Bone Mineral Density Testing
Bone mineral density (BMD) tests are vital for checking bones. They show how strong bones are and how likely they are to break. Dual-energy X-ray absorptiometry (DXA) is the top choice for BMD tests. It’s accurate and safe.
“Bone density testing is a cornerstone in the diagnosis and management of osteoporosis,” as recent guidelines say. We use BMD tests to see if treatments are working. This helps us care for our patients better.
Hormonal Level Evaluation
Checking hormone levels is also key for bone health. Estrogen, in particular, affects bone density. We check hormone levels to find out if they’re causing bone loss.
Testing estradiol levels helps us see how hormones affect bones. This info is important for figuring out the risk of osteoporosis. It helps us decide on treatments.
Risk Assessment Tools
Risk tools are used with BMD tests and hormone checks to fully understand bone health. They help us spot who’s most at risk of fractures and osteoporosis.
- The Fracture Risk Assessment Tool (FRAX) is widely used to calculate the 10-year probability of major osteoporotic fractures.
- Other risk assessment tools consider factors such as age, family history, and lifestyle to determine overall fracture risk.
By using all these methods together, we can create good plans for keeping bones healthy. Experts say, “a complete assessment is essential for managing bone health well.”
Therapeutic Interventions for Maintaining Bone Health
Therapeutic interventions are key to keeping bones strong and preventing fractures. Estrogen is important for bone health, and its drop during menopause can lead to osteoporosis. So, many treatments have been created to help with bone health.
Hormone Replacement Therapy Considerations
Hormone replacement therapy (HRT) is a common treatment for osteoporosis in postmenopausal women. It helps prevent bone loss by reducing osteoclast activity. This keeps bone density stable. A study found that HRT lowers the risk of fractures in postmenopausal women.
“HRT has been shown to reduce the risk of vertebral and non-vertebral fractures in postmenopausal women.”
But, HRT comes with risks. It’s important to weigh its benefits against the risks of breast cancer and heart problems.
Non-Hormonal Medications
For those who can’t or don’t want to use HRT, there are other options. Bisphosphonates, like alendronate and risedronate, are used to treat osteoporosis. They stop bone resorption. SERMs, such as raloxifene, also help by mimicking estrogen’s effects on bones without its risks.
Key non-hormonal medications include:
- Bisphosphonates (e.g., alendronate, risedronate)
- Selective estrogen receptor modulators (SERMs) (e.g., raloxifene)
- Denosumab, a monoclonal antibody that inhibits osteoclast formation
- Teriparatide, an anabolic agent that stimulates bone formation
Lifestyle and Nutritional Approaches
Lifestyle and nutrition are also important for bone health. Eating enough calcium and vitamin D is key. Supplements can help if you’re not getting enough from food.
Eating a diet rich in calcium and vitamin D, along with regular exercise, helps a lot. Exercises that make your bones work harder, like weight-bearing and resistance exercises, are best for bone density.
Other good habits include not smoking and drinking alcohol in moderation. Both can harm your bones.
Conclusion: The Future of Estrogen and Bone Health Research
Research on estrogen and bone health is ongoing and vital. It helps us understand how estrogen affects bones. This knowledge is key to finding new ways to prevent and treat osteoporosis.
New studies suggest we might soon have better ways to deal with estrogen loss. This could lead to new treatments for keeping bones strong. By studying estrogen and bone health, we can find better ways to keep bones healthy for life.
Future studies will likely uncover more about how estrogen and bones interact. This could lead to new treatments for osteoporosis. As we learn more, we can help more people live better lives, free from bone disorders.
FAQ
How does estrogen affect bone density?
Estrogen is key in keeping bones strong by controlling bone cells. When estrogen levels drop, like during menopause, bones can weaken. This makes bones more likely to break.
What is the role of estrogen in bone metabolism?
Estrogen helps bones grow by boosting the activity of bone-building cells. It also slows down bone loss by controlling other cells. This keeps bones healthy.
How does estrogen regulate calcium levels in bones?
Estrogen helps the body absorb calcium, which is good for bones. It also works with other hormones to keep calcium levels right. This is vital for bone health.
What happens to bone health during menopause?
Menopause is tough on bones because estrogen levels drop. This leads to faster bone loss. The exact timing can vary, but bones often lose a lot of density.
What are the clinical consequences of estrogen deficiency on bone health?
Without enough estrogen, bones become weaker and more prone to breaks. The link between estrogen and bone health shows why it’s so important.
How is bone health assessed?
Doctors check bone health with tests like bone density scans and hormone tests. They also use risk tools. These help spot people at risk of bone problems.
What therapeutic interventions are available for maintaining bone health?
To keep bones healthy, treatments include hormone therapy and non-hormonal meds. Lifestyle changes and diet also help. These steps can prevent and treat bone loss.
How does estrogen affect bone mass?
Estrogen keeps bones strong by controlling bone cells. It boosts bone-building cells and slows down bone loss. This helps maintain bone density and lowers osteoporosis risk.
What is the impact of estrogen on vitamin D metabolism?
Estrogen affects how the body uses vitamin D, which is key for calcium and bone health. The connection between estrogen and vitamin D is vital for strong bones.
Why is estrogen important for bone health?
Estrogen is vital for bone health by managing bone cells and metabolism. Without enough estrogen, bones weaken and break more easily. This has serious health effects.
References
National Center for Biotechnology Information. Estrogen’s Impact on Bone Density and Calcium Regulation. Retrieved from https://pubmed.ncbi.nlm.nih.gov/8865143/



































