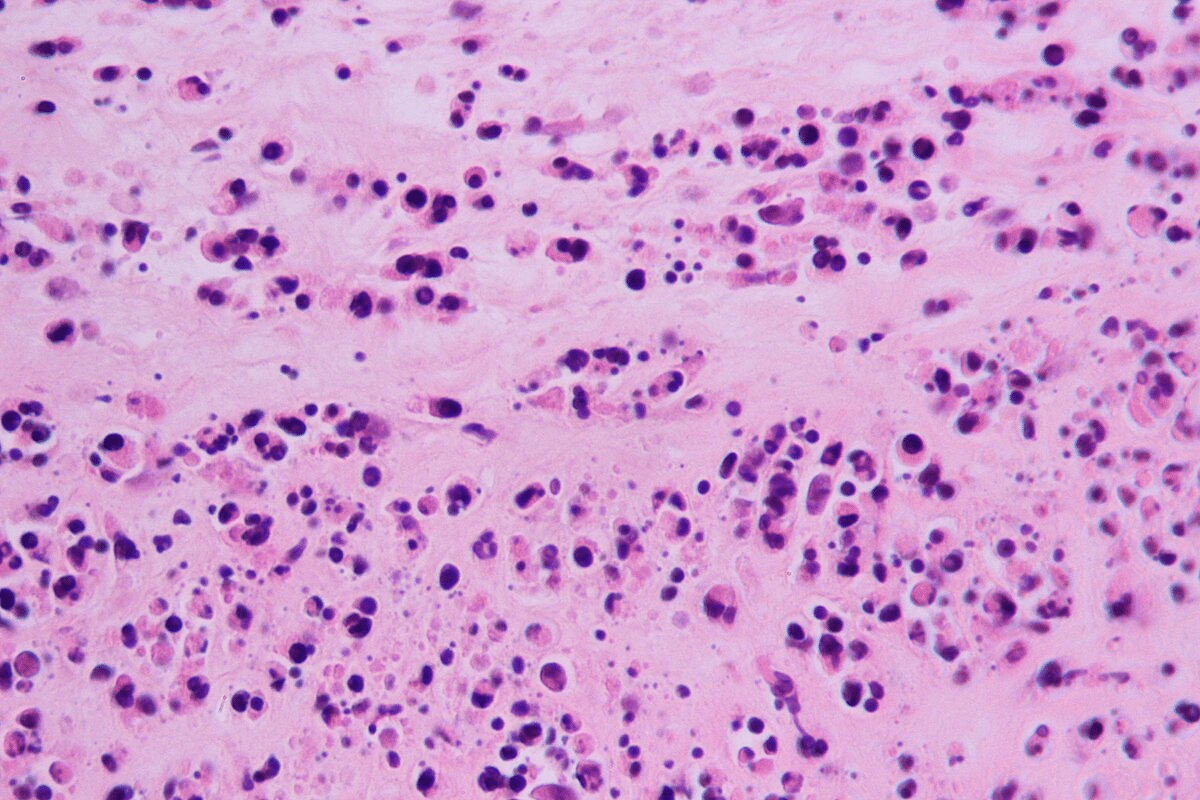
Vasculitis is a group of conditions that cause inflammation of blood vessels. This can lead to minor skin issues or serious illnesses affecting vital organs. Seeing purple bruise-like spots can be scary. But knowing what causes them can help figure out if you need to see a doctor right away.
The inflammation in vasculitis can make blood vessel walls thicker. This can narrow the vessels and harm organs and tissues. At Liv Hospital, we focus on our patients to make sure any vascular inflammation is found and treated correctly.
Key Takeaways
- Vasculitis involves inflammation of blood vessels, potentially causing damage to organs and tissues.
- The condition can range from minor skin issues to serious illnesses affecting vital organs.
- Understanding the causes of vasculitis is key to knowing if you need to see a doctor fast.
- Liv Hospital’s approach ensures proper identification and management of vascular inflammation.
- We use proven treatment plans to avoid serious problems.
Understanding Vasculitis and Vascular Inflammation

Vasculitis is a condition where blood vessels get inflamed. It can happen to anyone, at any age. The most common type, affecting the skin, is seen in about 38 to 55 per million adults each year.
Definition and Prevalence of Blood Vessel Inflammation
Blood vessel inflammation, or vasculitis, happens when the immune system attacks blood vessels by mistake. This can damage the vessel walls. The exact cause is often unknown, but it’s thought to be a mix of genetics and environmental factors.
Studies show vasculitis can be different types, based on the size and location of the affected blood vessels. Some types are more common in certain age groups.
|
Type of Vasculitis |
Prevalence |
Common Age Group |
|---|---|---|
|
Cutaneous Small-Vessel Vasculitis |
38-55 per million adults per year |
Adults of various ages |
|
Giant Cell Arteritis |
20-30 per 100,000 people over 50 |
Older adults |
|
Takayasu Arteritis |
Rare, about 2 per million people per year |
Younger adults |
How Inflamed Capillaries Affect Body Systems
Inflamed capillaries can affect many body systems. When capillaries get inflamed, they can get damaged. This can cause symptoms like rashes or purpura, or even affect organs like the kidneys or lungs.
Understanding vasculitis is important. It’s not just about inflamed blood vessels. It’s about how these inflamed vessels affect the body’s function and the patient’s quality of life. The impact can be significant, ranging from mild discomfort to life-threatening complications.
“Vasculitis is a complex condition that requires a thorough approach to diagnosis and treatment. Knowing its different forms and symptoms is key to managing it well.”
We will keep exploring vasculitis. We will look at its symptoms, causes, and treatment options. This will help us understand this complex condition better.
Identifying Vasculitis Rash on Legs: Characteristic Signs
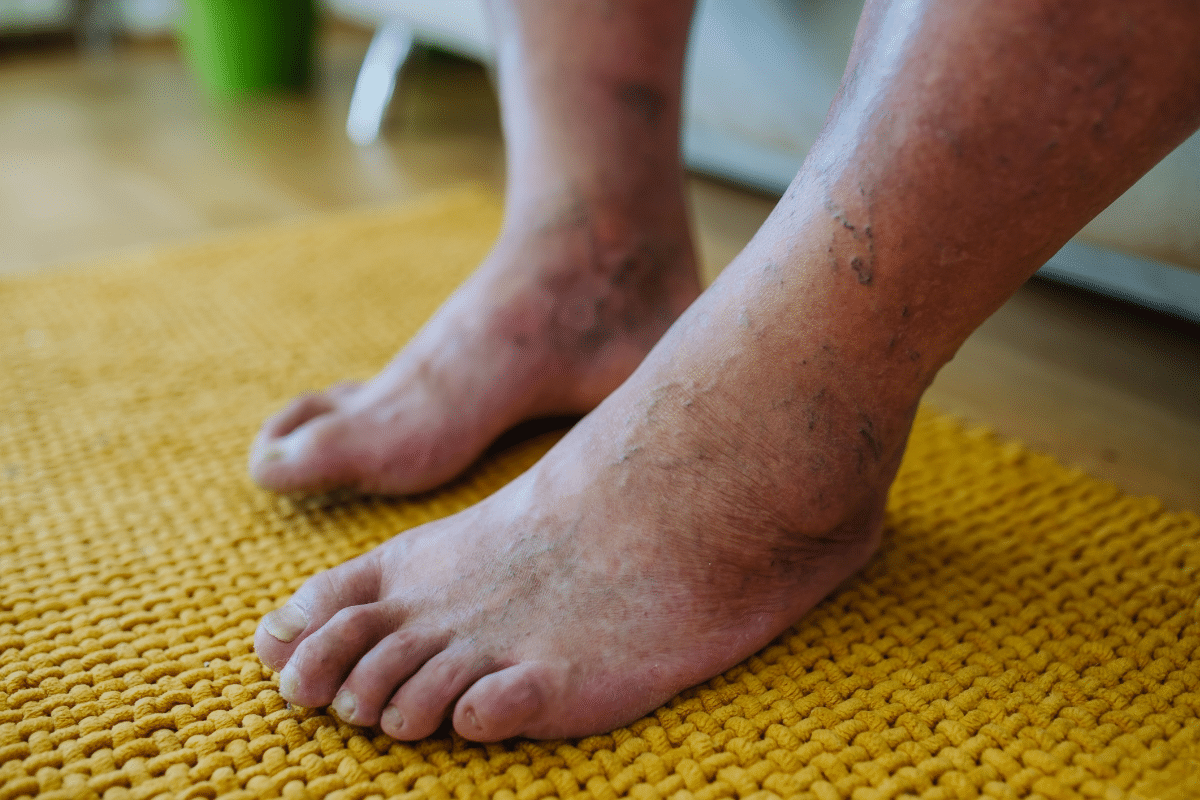
Understanding vasculitis rash on legs means knowing its key signs and symptoms. This condition shows up through specific skin lesions. These are key for diagnosing it.
Palpable purpura is a major sign of vasculitis, mainly in its skin form. “Purpura” means purple spots or patches on the skin. If these spots are palpable (can be felt), it shows blood vessel inflammation.
Palpable Purpura: The Hallmark Symptom
Seeing palpable purpura is a big clue for diagnosis. These spots are usually tender, purple or reddish-brown, and found on legs, buttocks, and trunk. A medical expert says,
“The presence of palpable purpura is highly suggestive of vasculitis, mainly when other symptoms are present.”
Why Vasculitis Commonly Affects the Lower Extremities
Vasculitis often hits the lower legs because of gravity’s impact on blood flow. The skin in these areas is also cooler. This makes the lower legs more likely to have vascular inflammation due to increased pressure and possible vessel damage.
Non-Blanching Spots: What They Indicate
Non-blanching spots, which don’t disappear when pressed, are another sign of vasculitis. These spots show bleeding into the skin because of damaged blood vessels. Seeing non-blanching purpura means there’s serious vascular inflammation and possible damage.
Knowing these signs is key for early diagnosis and treatment of vasculitis rash on legs. Spotting palpable purpura and non-blanching spots helps doctors start the right treatment. This can help lessen symptoms and avoid worse problems.
The Root Causes of Vasculitis
It’s important to know what causes vasculitis to find the right treatment. Vasculitis is when blood vessels get inflamed. It can happen for many reasons.
Immune System Dysfunction and Vessel Damage
In about half of the cases, vasculitis has no clear cause. It often happens when the immune system attacks its own blood vessels. This leads to inflammation and damage.
Immune system dysfunction plays a big role in vasculitis. If the immune system doesn’t work right, it can make antibodies that harm blood vessels. This causes inflammation.
Medications That Can Trigger Vasculitis
Some medicines can cause vasculitis. NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) and antibiotics are examples. Taking these medicines can start an immune reaction that leads to vasculitis.
|
Medication Category |
Examples |
Potential to Trigger Vasculitis |
|---|---|---|
|
NSAIDs |
Ibuprofen, Naproxen |
Yes |
|
Antibiotics |
Penicillin, Minocycline |
Yes |
Infections and Autoimmune Connections
Infections and autoimmune diseases also play a big part in vasculitis. Some infections can start an immune reaction that leads to vasculitis. Autoimmune diseases can make the immune system attack blood vessels directly.
It’s key to understand these connections to manage vasculitis well. By finding and fixing the root causes, doctors can create better treatment plans. This helps reduce inflammation and prevent more damage.
Types of Vasculitis That Manifest as Skin Rashes
It’s important to know about the different vasculitis types that show up as skin rashes. Vasculitis is an inflammation of blood vessels. It can affect various parts of the body, including the skin. Skin rashes from vasculitis can look different and vary in how severe they are.
Cutaneous Small-Vessel Vasculitis: The Most Common Form
Cutaneous small-vessel vasculitis is the most common skin vasculitis. It mainly affects the small blood vessels in the skin. This leads to inflammation and a rash. This condition is usually just in the skin but can sometimes show a bigger problem.
Key features include palpable purpura. These are purple spots that can be felt on the skin, often on the lower legs.
Henoch-Schönlein Purpura and Its Distinctive Features
Henoch-Schönlein purpura (HSP) is a type of vasculitis that mainly hits kids but can also affect adults. It’s known for a specific reddish-purple rash. Other symptoms like belly pain and joint pain often come with it. HSP is marked by IgA immune complexes in the affected vessels.
“HSP is a form of vasculitis that can have significant systemic implications, requiring prompt diagnosis and treatment.”
Systemic Vasculitis with Cutaneous Manifestations
Systemic vasculitis is when vasculitis affects not just the skin but also other organs. When it shows up on the skin, it can cause different rashes. For example, granulomatosis with polyangiitis (GPA) and eosinophilic granulomatosis with polyangiitis (EGPA) can have skin symptoms along with other body issues.
It’s key for doctors to know about these different vasculitis types. Each one has its own signs and can affect the whole body. This makes it important to do a full check-up.
Vasculitis Beyond the Legs: Other Affected Areas
Vasculitis can show up in many parts of the body, not just the legs. It can also affect the hands, feet, and face. Knowing this helps us understand how widespread this condition can be.
Mild Vasculitis in Hands and Feet: What to Look For
Mild vasculitis in the hands and feet might cause unexplained bruising or burst blood vessels. These areas are more likely to get affected because of their location and small blood vessels.
- Numbness or weakness in the hands or feet
- Swelling or hardening of the palms or soles
- Visible signs of bruising or purpura
Unexplained Bruising on Inner Arms: A Warning Sign
Unexplained bruising on the inner arms might signal vasculitis. This happens when blood vessels get inflamed, leading to leakage and bruising.
Watching for such bruising is important, even more so if it’s with pain or swelling.
Nasal Vasculitis and Facial Involvement
Nasal vasculitis means inflammation in the nasal blood vessels, often part of a bigger vasculitis issue. Facial symptoms can include redness, swelling, or lesions.
Spotting nasal vasculitis and facial signs needs a detailed check-up and knowing about vasculitis’s many forms.
Diagnosing Vasculitis: From Symptoms to Confirmation
Diagnosing vasculitis requires checking symptoms, running lab tests, and sometimes doing skin biopsies. We’ll walk you through the steps and tests needed for diagnosis.
Clinical Examination of Vasculitis Spots
The first step in diagnosing vasculitis is a clinical exam. We look at the vasculitis spots’ appearance and where they are. Palpable purpura, a key symptom, is often found during this exam. We also check the spots’ size, color, and tenderness.
We also review the patient’s medical history. This helps us find possible triggers or underlying conditions that might be causing the vasculitis.
Laboratory Tests and Skin Biopsies
Laboratory tests are key in confirming vasculitis. These tests may include:
- Blood tests to check for signs of inflammation or infection
- Urine tests to assess kidney function
- Imaging studies to evaluate the extent of vasculitis
Skin biopsies are often needed to confirm the diagnosis. A skin sample is examined under a microscope for vasculitis signs. This helps us tell vasculitis apart from other conditions with similar symptoms.
Ruling Out Other Conditions with Similar Symptoms
Diagnosing vasculitis can be tricky because it looks like other conditions. We must rule out other possible causes of symptoms, like infections, allergic reactions, or other inflammatory disorders.
A detailed diagnostic approach, including clinical exams, lab tests, and skin biopsies, helps us accurately diagnose vasculitis. This way, we can create an effective treatment plan.
Is Vasculitis Serious or Fatal? Understanding the Risks
Vasculitis can range from mild skin symptoms to serious organ damage. It’s important to know the risks it poses.
Mild Vasculitis: When It’s Limited to the Skin
Often, vasculitis only affects the skin, showing up as rashes or purpura on the legs. This type is usually mild and might not need strong treatment. Yet, it’s key to have a doctor watch it closely to avoid skin damage.
When Vasculitis Affects Internal Organs
Vasculitis can be serious if it hits internal organs. It can harm important areas like the kidneys, lungs, and heart. When organs are involved, the risk of serious problems grows a lot. For example, kidney vasculitis can cause kidney failure if not treated right away.
Can Vasculitis Kill You? Addressing the Mortality Risk
In severe cases, vasculitis can be deadly. The risk of death is higher if vital organs are affected or if treatment is delayed. Quick diagnosis and treatment are key to avoid serious issues and lower death risk. Knowing how serious vasculitis can be is why seeing a doctor is so important if symptoms get worse.
Managing vasculitis, whether it’s mild or severe, is a big task. By understanding the risks and working with doctors, patients can handle its challenges better.
Treatment Options for Vasculitis Rash on Legs
It’s important for patients to know about treatment options for vasculitis rash on legs. The right treatment depends on how severe the rash is and the patient’s health.
Managing Mild Cutaneous Symptoms
For mild vasculitis, treatment aims to manage symptoms and prevent irritation. Topical corticosteroids help reduce inflammation and itching. Patients should avoid scratching and keep their skin moisturized to prevent dryness.
“Early treatment and good skin care are key for mild cutaneous vasculitis,” says Medical Expert, a dermatologist. “By controlling inflammation and preventing infections, we can greatly improve patients’ lives.”
Medications to Control Vascular Inflammation
For more severe cases or when vasculitis affects more than the skin, systemic corticosteroids or immunosuppressive drugs may be needed. These medications can have side effects, so doctors closely monitor their use.
- Corticosteroids: Effective in reducing inflammation but can have long-term side effects.
- Immunosuppressives: Used in severe cases to suppress the immune system’s abnormal response.
- Biologic agents: Target specific parts of the immune system involved in vasculitis.
Addressing Underlying Triggers and Causes
Finding and treating the cause of vasculitis is key. This might mean stopping certain medications, treating infections, or managing autoimmune disorders. Sometimes, vasculitis is a sign of a more complex condition that needs detailed management.
By treating vasculitis holistically, we can reduce symptoms and improve overall health and well-being.
Living with Vasculitis: Self-Care Strategies
Living with vasculitis can be tough, but the right self-care can help. It’s important to manage the condition with both medical treatment and personal care. This approach can improve your life quality.
Skin Care for Affected Areas
Proper skin care is key for those with vasculitis, like a rash on the legs. Gentle cleansing and moisturizing can ease discomfort and aid in healing. Use mild, fragrance-free products to avoid skin irritation.
It’s important to avoid scratching or picking at the rash. This can cause infection or scarring. Keeping the area clean and dry and avoiding tight clothes are also vital.
Lifestyle Modifications to Reduce Flares
Changing your lifestyle can help lessen vasculitis flares. Maintaining a healthy lifestyle is important. This includes a balanced diet, regular exercise, and enough rest.
Identifying and avoiding triggers is also key. Keep a symptom journal to track flares and possible causes. Common triggers include certain medications, infections, or environmental factors.
- Eating a balanced diet rich in fruits, vegetables, and whole grains
- Staying hydrated by drinking plenty of water
- Engaging in regular, gentle exercise to maintain mobility and reduce stress
- Getting enough rest and practicing stress-reducing techniques, such as meditation or deep breathing
When to Seek Emergency Medical Attention
Self-care is important, but knowing when to seek medical help is just as vital. Severe symptoms or signs of complications need immediate care. Look for severe abdominal pain, difficulty breathing, or significant vision changes.
Being aware of complications and knowing when to act is critical. Regular check-ups with your healthcare provider are also important. They help monitor your condition and adjust treatment plans as needed.
Conclusion: The Outlook for People with Vasculitis
The outlook for vasculitis depends on the type and how severe it is. With the right treatment and care, many people can manage their symptoms well. It’s important for patients to understand their condition to make good care choices.
Managing vasculitis means using medicine, changing your lifestyle, and taking care of yourself. Working with your healthcare team is key. This way, you can lower the chance of serious problems and get better results.
Most people with vasculitis see a big improvement with treatment. But, some might keep having symptoms. This shows the need for constant monitoring and care. By being proactive in managing vasculitis, patients can improve their outlook and live better.
FAQ
What is vasculitis and how does it affect the body?
Vasculitis is a condition where blood vessels get inflamed. This can harm different parts of the body. It can cause skin rashes, damage to organs, and other issues.
What are the characteristic signs of vasculitis rash on legs?
Signs of vasculitis rash on legs include palpable purpura and non-blanching spots. These are often seen more on the lower legs. This is because of gravity and higher blood pressure.
What causes vasculitis, and can it be triggered by medications or infections?
Vasculitis can be caused by problems with the immune system or damage to blood vessels. It can also be triggered by certain medicines and infections.
Is vasculitis serious or fatal, and what are the risks associated with it?
Vasculitis can be serious and even fatal in some cases. It’s most dangerous if it affects internal organs or is untreated. The risk of death depends on the type and severity of vasculitis.
How is vasculitis diagnosed, and what tests are used to confirm the condition?
Doctors use a mix of physical exams, lab tests, and skin biopsies to diagnose vasculitis. These help confirm inflammation and rule out other conditions.
What are the treatment options for vasculitis rash on legs, and how can symptoms be managed?
Treatment for vasculitis rash on legs includes managing mild symptoms and using medicines to reduce inflammation. It also involves addressing the underlying causes to prevent further issues.
Can vasculitis affect areas beyond the legs, such as the hands, feet, or face?
Yes, vasculitis can affect many parts of the body, including the hands, feet, and face. It can cause mild symptoms, unexplained bruising, or even affect the nose.
How can I live with vasculitis, and what self-care strategies can help manage the condition?
To live with vasculitis, focus on skin care and making lifestyle changes to reduce flare-ups. Knowing when to seek emergency care is also key to preventing complications.
What is the outlook for people with vasculitis, and can proper treatment improve the prognosis?
With the right treatment, many people with vasculitis can manage their symptoms and avoid complications. The outcome depends on the type and severity of the condition.
Can burst blood vessels in fingers be a sign of vasculitis?
Yes, burst blood vessels in fingers can be a sign of vasculitis. This is often seen with other symptoms like skin rashes or joint pain.
Is mild vasculitis on hands and feet a common manifestation of the condition?
Yes, mild vasculitis on hands and feet is common. It can also be accompanied by other symptoms like unexplained bruising or skin lesions.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3626098/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News






























