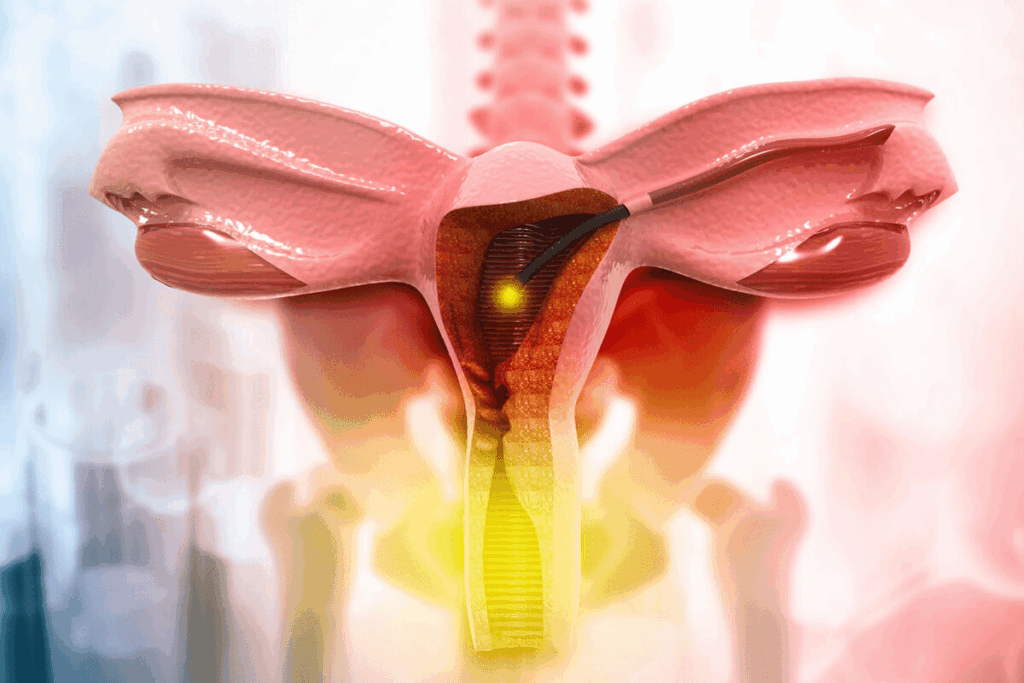
Uterine prolapse happens when the muscles and tissues that hold the uterus get weak. This makes the uterus drop into or through the vagina. It’s a common issue for many women, often those who have had a vaginal birth or gone through menopause. Visual guide and stage-by-stage explanation of uterine prolapse and its effect on the vaginal canal.
As the condition gets worse, how it looks changes a lot. In the early stages, the drop might be small and inside. But in more serious cases, it can cause a noticeable bulge outside.
Understanding the different stages of uterine prolapse is key. It helps women get the medical help they need early on. This can greatly improve their life quality.
Key Takeaways
- Uterine prolapse is a condition where the uterus drops into or through the vagina due to weakened supporting muscles and tissues.
- The condition’s prevalence is higher among women who have had vaginal childbirth or menopause.
- The visual appearance of uterine prolapse varies significantly across different stages.
- Early stages may involve subtle internal displacement, while advanced cases can result in visible external bulging.
- Recognizing the stages and symptoms of uterine prolapse is essential for timely medical intervention.
Understanding Uterine Prolapse

To understand uterine prolapse, we first need to grasp the basics of female pelvic anatomy. Uterine prolapse is a form of pelvic organ prolapse. It happens when the muscles and tissues supporting the pelvic organs weaken. This allows the uterus to slip out of its normal position.
Definition and Basic Anatomy
Uterine prolapse is when the uterus slips into or outside the vaginal canal. This is due to weakened pelvic floor muscles and supportive tissues. The pelvic floor muscles are key in supporting the uterus, bladder, and bowel.
The uterus is normally held in place by a group of muscles and ligaments that form the pelvic floor. When these supportive structures weaken, it can lead to prolapse.
We rely on the pelvic floor muscles to support our internal organs. When these muscles weaken, it can lead to various complications, including uterine prolapse. The condition can range from mild to severe, depending on the degree of displacement.
As stated by the American College of Obstetricians and Gynecologists, “Pelvic organ prolapse is a common condition that can affect women of all ages, but it’s more prevalent among older women.” This highlights the importance of understanding the condition and its prevalence across different age groups.
How Common Is Uterine Prolapse?
Uterine prolapse is a relatively common condition. About half of all women develop mild pelvic floor weakness over their lifetime. A significant portion of these cases may involve some degree of uterine prolapse.
The prevalence increases with age, specially during and after menopause. This is due to the decrease in estrogen levels which further weakens the pelvic muscles.
Age Group | Prevalence of Uterine Prolapse |
20-39 years | Low |
40-59 years | Moderate |
60+ years | High |
Understanding the prevalence and risk factors associated with uterine prolapse can help in early detection and management. It’s important for women, specially those in higher risk categories, to be aware of the symptoms. They should seek medical attention if they experience any discomfort or abnormalities.
Causes of Uterine Prolapse
It’s important to know why uterine prolapse happens. This condition occurs when the muscles and ligaments around the uterus get weak. This weakness lets the uterus slip into or out of the vagina. Many things can cause this problem.
Weakening of Pelvic Floor Muscles
The pelvic floor muscles are key in holding up the uterus, bladder, and bowel. If these muscles get weak, uterine prolapse can happen. Things that can make these muscles weak include:
- Aging
- Childbirth
- Chronic coughing
- Heavy lifting
- Obesity
As we get older, our muscles naturally get weaker. This makes us more likely to have a prolapse. Activities that put strain on the pelvic floor can also make it weaker faster.
Impact of Childbirth
Childbirth is a big risk for uterine prolapse. Vaginal delivery can really strain the muscles and tissues around the uterus. The more vaginal deliveries a woman has, the higher her risk is. Studies show that women with multiple vaginal births are more likely to have a prolapse.
Hormonal Changes During Menopause
Hormonal changes in menopause also affect uterine prolapse. When estrogen levels drop during menopause, the tissues around the uterus get thinner and less elastic. This loss of support can lead to prolapse.
“The decline in estrogen during menopause can significantly affect the health and elasticity of pelvic tissues, increasing the risk of prolapse.”
Knowing the causes helps in finding ways to prevent and treat uterine prolapse. By tackling these causes, women can lower their risk of getting this condition.
Risk Factors for Developing Uterine Prolapse
Uterine prolapse is a complex condition with many risk factors. Knowing these can help prevent and manage it.
Age-Related Factors
Advanced age is a big risk for uterine prolapse. As women get older, the muscles and ligaments that support the pelvic organs weaken. The risk gets much higher after 50.
Pregnancy and Delivery History
Pregnancy and childbirth, and having multiple vaginal deliveries, can strain the pelvic floor muscles. This increases the risk of uterine prolapse. The risk is higher with vaginal deliveries than with cesarean sections.
Delivery Type | Risk Level |
Vaginal Delivery | High |
Cesarean Section | Lower |
Genetic Predisposition
Genetic factors can also play a role. Women with a family history of pelvic floor disorders are at higher risk.
Lifestyle and Environmental Factors
Lifestyle factors like obesity, chronic coughing, and heavy lifting can increase the risk. These activities put strain on the pelvic floor muscles.
Understanding these risk factors helps individuals take steps to lower their risk. This includes staying at a healthy weight, avoiding heavy lifting, and managing chronic coughs.
Common Symptoms of Uterine Prolapse
Uterine prolapse symptoms can vary, affecting physical comfort, bowel and bladder function, and sexual health. Women with this condition often feel discomforts that can greatly lower their quality of life.
Physical Sensations and Discomfort
One main symptom is feeling pelvic heaviness or pressure. This feeling can be constant or get worse when standing for a long time. Some women might also feel:
- a feeling of something “coming down” or bulging into the vagina
- lower back pain or discomfort
- discomfort or pain in the pelvic area
Impact on Urinary and Bowel Function
Uterine prolapse can also affect how you use the bathroom. Common problems include:
- urinary incontinence or leakage, often during activities that increase abdominal pressure like coughing or sneezing
- frequent urination or urgency
- difficulty emptying the bladder completely
- constipation or straining during bowel movements
These issues happen because the prolapsed uterus can press on the bladder and bowel, making it hard for them to work right.
Effects on Sexual Health
Uterine prolapse can also affect your sex life. Women might feel:
- discomfort or pain during sexual intercourse
- decreased sexual satisfaction due to the physical discomfort or emotional distress associated with the condition
Talking to your healthcare provider about these symptoms is important. They can help address any underlying issues.
Knowing the common symptoms of uterine prolapse is key for early treatment. If you’re experiencing any symptoms, we urge you to see a doctor. They can help you find ways to improve your life.
Visual Appearance of Uterine Prolapse
Uterine prolapse shows different signs at each stage. It affects both inside and outside the body. The more it progresses, the more noticeable the signs become.
Internal Appearance Changes
Inside, uterine prolapse means the uterus moves into the vaginal canal. Doctors can see this during an exam.
The cervix might look lower or bulge out. In later stages, the uterus can move even more, changing the pelvic area.
External Visual Indicators
Outside, signs of uterine prolapse become clearer as it gets worse. At first, there might not be many visible signs.
But as it gets worse, a bulge or lump can show at the vaginal opening. In the worst cases, the uterus can stick out of the vagina, changing how it looks outside.
How Appearance Changes Over Time
The look of uterine prolapse changes a lot as it moves from one stage to the next.
Stage | Internal Appearance | External Appearance |
Stage 1 | Uterus descends into upper vagina | No visible external symptoms |
Stage 2 | Cervix reaches lower vagina | Possible bulge at vaginal opening |
Stage 3 | Cervix protrudes outside vagina | Visible bulge outside vagina |
Stage 4 | Uterus completely prolapsed outside vagina | Significant external bulge |
Knowing these changes is key for both patients and doctors. It helps track the condition’s progress and find the right treatment.
The Four Stages of Uterine Prolapse Explained
Uterine prolapse can be divided into four stages. Each stage shows how far the uterus has moved into or through the vagina. Knowing these stages helps doctors understand how severe the condition is and what treatment is best.
Stage One: Initial Descent into Upper Vagina
In stage one, the uterus starts to move into the upper vagina. At this early stage, symptoms are often mild. Women might feel a bit of discomfort or a heaviness in their pelvic area.
Stage Two: Descent into Lower Vagina
By stage two, the uterus has moved further into the lower vagina. Symptoms get worse, including more pelvic pressure and discomfort during activities. Some women might also notice urinary issues.
Stage Three: Cervical Protrusion at Vaginal Opening
In stage three, the cervix starts to show at the vaginal opening. This stage brings more discomfort and noticeable symptoms. Women may find it hard to urinate or have bowel movements, and they feel more pelvic pressure.
Stage Four: Complete Prolapse Outside Vagina
Stage four is the most severe, where the uterus fully prolapses outside the vagina. This can cause a lot of pain, make walking hard, and lead to hygiene problems.
Women progress through these stages at different rates. Their health, past childbirth, and other pelvic issues can affect this.
Stage | Description | Common Symptoms |
Stage One | Initial descent into upper vagina | Minimal symptoms, slight discomfort |
Stage Two | Descent into lower vagina | Increased pelvic pressure, discomfort during activities |
Stage Three | Cervical protrusion at vaginal opening | Significant discomfort, urinary or bowel difficulties |
Stage Four | Complete prolapse outside vagina | Pain, difficulty walking, hygiene issues |
Doctors say knowing the stage of uterine prolapse is key to choosing the right treatment. “Accurate staging is vital for picking the best treatment, whether it’s non-surgical or surgery,” a top gynecologist notes.
Diagnosing Uterine Prolapse
Diagnosing uterine prolapse involves a detailed medical check-up. This includes a pelvic exam and sometimes more tests. We know it can be scary, but it’s a key step in getting the right care.
Medical Examination Process
The first step is talking about your health history. We’ll ask about your symptoms, past pregnancies, and any surgeries or health issues. This helps us understand your situation better.
Then, a pelvic exam is done to see how bad the prolapse is. You might be asked to bear down or cough. This helps us figure out the best way to help you.
Diagnostic Tools and Tests
We might also use special tools and tests to confirm the diagnosis. These could include:
- Pelvic floor strength assessment
- Ultrasound to check the pelvic organs
- Urodynamic tests for bladder function
- Defecography for bowel movements
Differentiating from Other Pelvic Conditions
It’s important to tell uterine prolapse apart from other pelvic issues. We’ll do a detailed exam and might use tests to find out what’s going on. This could include cystocele, rectocele, or vaginal vault prolapse.
Knowing exactly what you have helps us give you the best treatment. We can then tailor our advice to fit your needs.
When to Seek Medical Attention
If you feel a heaviness or bulge in your vagina, have trouble peeing, or feel pain during sex, see a doctor. Early treatment can really improve your life.
If you’re worried about symptoms, talk to a healthcare provider. Quick action can help manage your symptoms and stop things from getting worse.
Treatment Options for Different Stages of Uterine Prolapse
There are many ways to treat uterine prolapse, from simple steps to surgery. The right treatment depends on how bad the prolapse is, your symptoms, and your health.
Conservative Management Approaches
For mild cases, doctors often suggest simple treatments. These include exercises, making lifestyle changes, and using pessaries.
- Pelvic floor exercises, like Kegels, can make the muscles around the uterus stronger.
- Changing your lifestyle, like losing weight or avoiding heavy lifting, can help.
- Pessaries are devices put in the vagina to support the uterus.
Non-Surgical Interventions
For cases that need more than simple treatments, doctors might suggest other non-surgical options. These include:
- Hormone replacement therapy (HRT) to make vaginal tissues stronger and more elastic.
- Estrogen creams to improve vaginal health.
Surgical Solutions
For severe cases or when other treatments don’t work, surgery is considered. Surgery aims to fix or remove the prolapsed uterus.
- Surgical methods like uterine suspension use mesh or sutures to support the uterus.
- In advanced cases, a hysterectomy (removing the uterus) might be needed.
Treatment Effectiveness by Stage
The success of treatments varies with the stage of uterine prolapse. Knowing how treatments work at each stage is key to managing expectations.
Stage of Prolapse | Common Treatments | Effectiveness |
Stage 1 | Conservative management, pelvic floor exercises | Highly effective in managing symptoms |
Stage 2 | Pessaries, non-surgical interventions | Effective in reducing symptoms, improving quality of life |
Stage 3 | Surgical interventions, including uterine suspension | Effective in correcting prolapse, improving symptoms |
Stage 4 | Surgical options, including hysterectomy | Highly effective in resolving prolapse, though with significant lifestyle implications |
Talking to a healthcare provider is important to find the best treatment for you. Your specific situation can influence the best choice.
Prevention and Management Strategies
To prevent uterine prolapse, a mix of pelvic floor exercises, lifestyle changes, and pregnancy and childbirth precautions is needed. These steps can greatly lower the risk of uterine prolapse.
Pelvic Floor Strengthening Exercises
Kegel exercises are key in preventing and managing uterine prolapse. They strengthen the muscles that support the uterus, bladder, and bowel. This reduces the chance of prolapse.
- Identify the correct muscles: The muscles used to stop the flow of urine are the pelvic floor muscles.
- Perform Kegel exercises regularly: Squeeze the pelvic floor muscles, hold for 5 seconds, and release for 5 seconds. Repeat this process 10-15 times, three times a day.
- Engage in other pelvic floor exercises: Squats and lunges can also strengthen the pelvic floor.
Lifestyle Modifications
Making lifestyle changes is important in preventing uterine prolapse. Simple adjustments can greatly improve pelvic health.
Lifestyle Change | Benefit |
Maintaining a healthy weight | Reduces pressure on the pelvic floor |
Avoiding heavy lifting | Decreases strain on pelvic muscles |
Quitting smoking | Reduces chronic coughing, which can strain pelvic muscles |
Preventive Measures During Pregnancy and Childbirth
Pregnancy and childbirth increase the risk of uterine prolapse. Taking preventive steps during these times can help lower this risk.
- Regular prenatal care: Monitoring pelvic health during pregnancy can help identify issues early.
- Pelvic floor exercises during pregnancy: Continuing Kegel exercises during pregnancy can help maintain pelvic floor strength.
- Considering a planned delivery: Discussing delivery options with a healthcare provider can help minimize the risk of prolapse.
By adding these prevention and management strategies to daily life, women can greatly reduce their risk of uterine prolapse. This helps maintain overall pelvic health.
Conclusion
Uterine prolapse is when the uterus slips out of place. This can cause discomfort and affect your life quality. It’s important to know the stages and symptoms to get the right medical care.
There are four stages of uterine prolapse, each showing how far the uterus has slipped. Knowing these signs can help you get help when you need it.
Understanding the stages helps you choose the right treatment. Treatments range from non-surgical options to surgery. The right treatment can greatly improve your symptoms and overall health.
If your symptoms don’t go away or get worse, see a doctor. With the right care, you can manage uterine prolapse and keep living well. Knowing about uterine prolapse is the first step to better health.
FAQ
What is uterine prolapse?
Uterine prolapse is when the uterus falls into the vagina. This happens when the muscles and ligaments that hold it in place get weak.
What are the stages of uterine prolapse?
There are four stages of uterine prolapse. Stage one is when it starts to fall into the upper vagina. Stage two is when it falls into the lower vagina. Stage three is when the cervix shows at the vaginal opening. Stage four is when it completely falls out of the vagina.
What does a prolapsed uterus look like?
A prolapsed uterus looks different at each stage. In the early stages, you might not see or feel anything. As it gets worse, you might see or feel a bulge at the vaginal opening.
What are the common symptoms of uterine prolapse?
Common symptoms include feeling a heaviness or pulling in the pelvis. You might also have trouble urinating or moving your bowels. Some women also find sex uncomfortable. The severity of these symptoms depends on the stage of prolapse.
How is uterine prolapse diagnosed?
Doctors usually diagnose it with a pelvic exam. They might also use ultrasound or urodynamic tests to see how severe it is.
What are the treatment options for uterine prolapse?
Treatment options include pelvic floor exercises and non-surgical methods like pessaries. Surgery, such as hysterectomy or uterine suspension, is also an option.
Can uterine prolapse be prevented?
While not all cases can be prevented, there are ways to reduce the risk. Doing pelvic floor exercises, staying at a healthy weight, and avoiding heavy lifting can help. Getting good prenatal and postnatal care is also important.
How does childbirth affect the risk of uterine prolapse?
Childbirth, and vaginal delivery in particular, can weaken the muscles and ligaments that support the uterus. This increases the risk of uterine prolapse.
Are there lifestyle changes that can help manage uterine prolapse?
Yes, making lifestyle changes can help manage symptoms. Avoiding heavy lifting, managing chronic cough, and staying at a healthy weight can slow the progression of uterine prolapse.
What is the impact of menopause on uterine prolapse?
Menopause can weaken the pelvic floor muscles because of hormonal changes, like the decrease in estrogen. This can contribute to uterine prolapse or make it worse.
When should I seek medical attention for uterine prolapse?
You should see a doctor if you have symptoms like pelvic discomfort, trouble with urination or bowel movements, or if you notice a bulge in the vagina. Early treatment can help determine the best course of action.
References
https://my.clevelandclinic.org/health/diseases/16030-uterine-prolapse

































