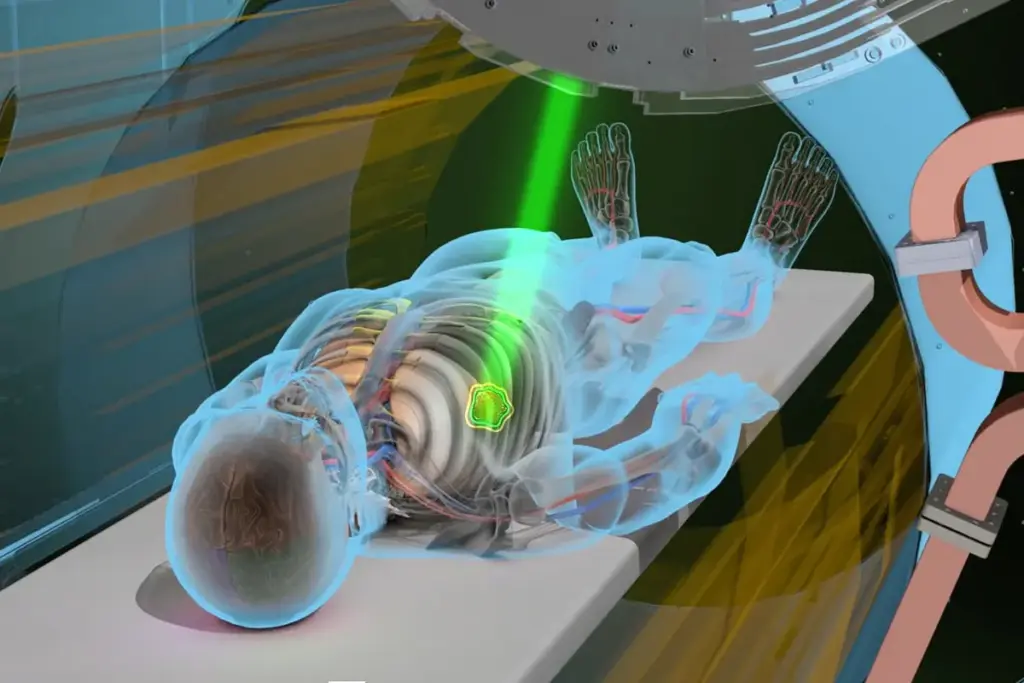
Coronary artery disease is a big problem worldwide, affecting millions each year. Accurate diagnosis and treatment are key to prevent serious issues and improve health outcomes.
Fractional Flow Reserve (FFR) is the top choice for checking if a blockage in the heart’s arteries is serious. But, Resting Full-cycle Ratio (RFR) is becoming a good option too. It doesn’t need the use of adenosine to work. We’ll look into how these two differ and their uses in medicine.
Key Takeaways
- Coronary artery disease is a significant global health issue.
- FFR is the current gold standard for assessing coronary stenoses.
- RFR is a new index that measures the lowest ratio of distal pressure to aortic pressure during the entire cardiac cycle.
- RFR does not require adenosine-induced hyperemia, making it a potentially more convenient alternative to FFR.
- The choice between FFR and RFR depends on various clinical factors.
Coronary Artery Disease and the Need for Functional Assessment
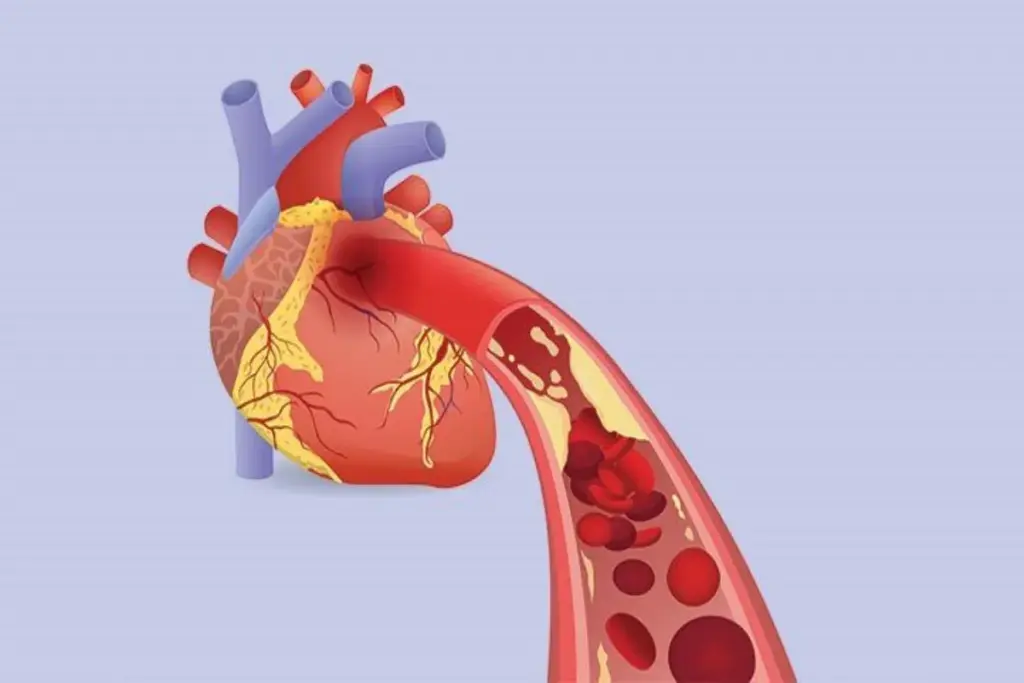
Coronary artery disease (CAD) is a major cause of illness and death worldwide. It’s important to understand how to diagnose and treat it. Knowing the global impact and the limits of current tests is key.
The Global Burden of Coronary Artery Disease
CAD is a big problem for global health, affecting millions. It’s a leading cause of death, making it critical for healthcare to find effective ways to manage it.
Many things can increase the risk of CAD, like lifestyle, genetics, and social status. As more people live longer and lifestyles change, CAD’s impact will grow. This will put more pressure on healthcare systems.
Beyond Anatomy: Why Functional Assessment Matters
Traditional tests for CAD mainly look at the structure of the arteries. But, they don’t always show how much stenoses affect blood flow.
Functional assessment, though, gives vital info on how CAD affects blood flow. This helps doctors decide the best treatment options.
|
Aspect |
Anatomical Assessment |
Functional Assessment |
|---|---|---|
|
Focus |
Visualizes coronary artery structure |
Evaluates coronary blood flow |
|
Method |
Angiography, CT scans |
FFR, RFR measurements |
|
Clinical Decision |
Based on stenosis severity |
Based on functional significance |
Understanding CAD’s global impact and the value of functional assessment is vital. This shift towards functional assessment is a big step forward. It leads to better care for patients.
Understanding FFR (Fractional Flow Reserve) in Depth
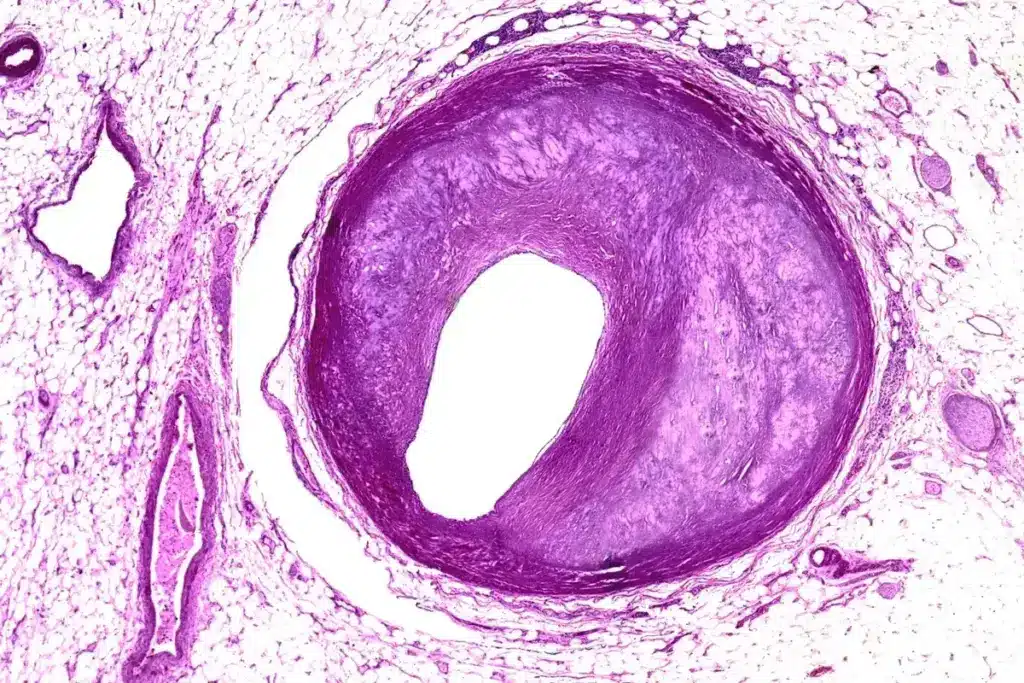
FFR is key in diagnosing and treating coronary artery disease. It gives a detailed look at how severe a blockage is. FFR is the ratio of the pressure in the coronary arteries to the aortic pressure during hyperemia, often caused by adenosine.
Definition and Physiological Basis
FFR measures how severe a blockage is by looking at blood flow to the heart. It uses a pressure wire to compare the pressure before and after a blockage during maximum blood flow. This shows how serious a blockage is, not just its size.
Adenosine is used to increase blood flow for FFR measurements. It makes the arteries wider, allowing more blood to flow. By comparing the pressure before and after a blockage, FFR shows how much a blockage affects blood flow to the heart.
Historical Development and Clinical Adoption
FFR was introduced in the 1990s as a new way to check for heart disease. It has grown a lot and is now used a lot in hospitals. The technology has improved, making it more accurate and useful.
Doctors started using FFR because studies showed it helps decide when to do heart procedures. It helps doctors choose the right treatments, which makes patients better.
The Significance of the 0.80 Threshold
A key part of FFR is the 0.80 threshold. If a blockage’s FFR is 0.80 or less, it’s considered serious and needs treatment. This number comes from studies that show treating these blockages helps patients.
The 0.80 threshold is based on solid evidence. Research shows that treating blockages with an FFR of 0.80 or less improves health. Not treating blockages with higher FFR values is safe and doesn’t harm patients.
How FFR Measurement Works in Clinical Practice
Measuring Fractional Flow Reserve (FFR) is a precise process. It requires a deep understanding of the steps involved. FFR measurement helps doctors assess coronary artery disease by checking pressure drops across lesions.
Catheterization Laboratory Setup
The journey starts with setting up the catheterization lab. This involves getting ready the needed tools like a guiding catheter and a pressure wire. The lab is made sterile and all tools are within reach.
Step-by-Step Procedural Technique
The steps for FFR measurement are critical:
- Access and Guiding Catheter Placement: First, access the coronary arteries through a femoral or radial artery. Then, a guiding catheter is placed.
- Pressure Wire Advancement: Next, a pressure wire is pushed through the guiding catheter to the coronary artery’s end, past the lesion.
- FFR Measurement: With the wire in place, FFR is calculated. It’s the ratio of distal coronary pressure to aortic pressure during peak hyperemia.
Adenosine Administration and Hyperemia
To get maximal hyperemia, adenosine is given. It can be through an IV or directly into the coronary artery. Adenosine makes blood vessels wider, boosting blood flow. This is key for a correct FFR measurement.
Clinical Evidence Supporting FFR-Guided Interventions
FFR-guided interventions have been proven through several key clinical trials. These trials have changed how we approach revascularization. The FAME and FAME2 studies are the most notable, showing the benefits of using Fractional Flow Reserve (FFR) in PCI.
Landmark Clinical Trials: FAME and FAME2
The FAME study was a major trial that showed FFR-guided PCI is better than just using angiography. It included over 1,000 patients and found that FFR-guided intervention lowered MACE rates at one year. The FAME2 trial then compared FFR-guided PCI with just optimal medical therapy in patients with stable coronary artery disease.
These trials have made FFR a key tool in the cath lab. They help doctors make better decisions about when to revascularize.
Impact on Revascularization Decisions
Using FFR-guided interventions has changed how we decide on revascularization. It helps identify which lesions are really important. This means we avoid unnecessary procedures, saving resources and improving patient care.
Our analysis shows that FFR-guided PCI reduces the need for repeat procedures and lowers the risk of heart attacks.
Long-term Clinical Outcomes
The long-term results from FAME and FAME2 trials are promising. Patients who got FFR-guided revascularization had better outcomes. They had lower rates of death, heart attacks, and repeat procedures.
|
Trial |
Primary Endpoint |
FFR-Guided Outcome |
Angiography-Guided Outcome |
|---|---|---|---|
|
FAME |
MACE at 1 year |
13.2% |
18.3% |
|
FAME2 |
MACE at 2 years |
12.7% |
20.8% (medical therapy alone) |
The table above shows the main findings from FAME and FAME2. It highlights the better outcomes with FFR-guided interventions.
Limitations and Challenges of Traditional FFR
FFR is a key tool for diagnosing coronary artery disease. Yet, it faces several challenges. These issues affect its use in traditional settings.
Adenosine-Related Side Effects
Adenosine is used in FFR to induce hyperemia. It can cause chest discomfort, dyspnea, and flushing. These side effects, though temporary, can upset patients.
Adenosine can also cause serious issues. For example, it might lead to bronchospasm in asthma patients or heart block in others. This makes it critical to choose patients carefully and monitor them closely.
Procedural Complexity and Time Constraints
FFR measurement is complex. It needs specialized equipment and trained staff. This can be a hurdle in some places. The process also takes time, straining lab resources.
Getting the pressure wire in the right spot and using adenosine adds to the challenge. It demands a lot of skill and judgment from the team.
Contraindications and Special Populations
FFR isn’t right for everyone. It’s not good for those with severe asthma or allergies to adenosine. Patients with acute coronary syndromes or recent heart attacks need careful thought before FFR.
Dealing with serial lesions or widespread disease makes FFR results tricky. It requires a deep understanding of heart physiology and the test’s limits.
Introduction to RFR (Resting Full-cycle Ratio)
In cardiology, a new tool has been introduced: the Resting Full-cycle Ratio (RFR). It’s changing how we look at coronary artery disease. This new method is easier for patients and more efficient for doctors.
RFR is the lowest ratio of distal pressure to aortic pressure during the whole cardiac cycle. It doesn’t need hyperemia. This makes RFR different from other tests that do need hyperemia.
Definition and Physiological Principles
RFR checks how severe coronary stenosis is when the heart is at rest. It looks at the pressure ratio throughout the heart cycle. This way, it doesn’t need to make the heart work harder like some tests do.
Development History and Validation
RFR has been tested thoroughly to prove its worth. It’s been compared to FFR and iFR, showing it’s reliable and accurate for finding coronary artery disease.
The creation of RFR shows the constant push for better, more patient-focused tests in cardiology. Its success against other tests has made it a key part of doctor’s work.
How RFR Differs from Other Resting Indices
RFR is different from iFR because it looks at the whole heart cycle, not just a part of it. This gives a clearer picture of how blood flows through the heart. It might help doctors make more accurate diagnoses.
Understanding RFR helps us see its importance in diagnosing and treating coronary artery disease. As cardiology keeps evolving, tools like RFR will be vital for better patient care.
The Technical Process of RFR Measurement
The RFR measurement process has several key steps. It helps doctors accurately check for coronary artery disease. RFR, or Resting Full-cycle Ratio, shows how severe the blockage is without using special agents.
Equipment Requirements
To measure RFR, certain equipment is needed. A pressure wire is placed beyond the blockage. It’s connected to a console that records and analyzes the pressure.
- A pressure wire (e.g., a coronary guidewire with pressure-sensing technology)
- A console for recording and analyzing pressure data
- A catheterization laboratory setup for the procedure
Advanced pressure wires are key for precise measurements. They help get high-quality data during the RFR process.
Procedural Workflow
The RFR measurement process is designed to be safe and efficient. It includes several steps:
- Preparation of the catheterization laboratory
- Insertion of the pressure wire into the coronary artery
- Advancement of the pressure wire distal to the stenosis
- Recording of pressure data over the entire cardiac cycle
- Analysis of the recorded data to calculate the RFR value
During the procedure, careful attention to detail is vital. This ensures accurate measurements. It’s important to verify the pressure wire’s correct placement and the quality of the data.
Data Acquisition and Analysis
Recording pressure distal to the stenosis over the entire cardiac cycle is part of data acquisition. The ratio is then calculated from this data.
Specialized software in the console system analyzes the data. It calculates the RFR value. Clinicians use this value to assess coronary artery disease severity.
Understanding the RFR measurement process helps clinicians see its value in managing coronary artery disease. RFR measurement is a big step forward in cardiology. It makes diagnosis more accurate and efficient.
Advantages of Adenosine-Free Assessment with RFR
Adenosine-free assessment with RFR is becoming more popular. It offers better patient comfort and makes procedures more efficient. Let’s look at the main benefits of using RFR for coronary artery disease assessment.
Elimination of Hyperemic Agent
One big plus of RFR is not needing hyperemic agents like adenosine. Using adenosine can lead to side effects like chest pain, shortness of breath, and heart block. RFR makes the procedure more comfortable for patients by avoiding these issues.
Key benefits of eliminating adenosine include:
- Reduced risk of adenosine-related side effects
- Improved patient tolerance and comfort during the procedure
- Simplified procedural workflow due to fewer complications
Improved Patient Comfort and Safety
RFR makes patients more comfortable by not using adenosine. This is key for a good experience and successful procedures.
The focus on patient comfort is reflected in the following aspects:
- Minimizing procedural risks and complications
- Enhancing the overall patient experience through reduced discomfort
- Facilitating a smoother recovery process
Procedural Efficiency and Workflow Benefits
RFR makes the assessment process faster by not needing adenosine. This efficiency can cut down procedural times and improve lab workflow.
Procedural benefits include:
- Reduced time required for the assessment
- Simplified procedural steps due to the absence of adenosine-related protocols
- Potential for increased throughput in catheterization laboratories
Direct Comparison: FFR vs. RFR Methodology
In the world of diagnosing coronary artery disease, FFR and RFR stand out as two distinct approaches. They differ in their underlying principles, how they are done, and what they aim to find.
Physiological Basis Differences
FFR looks at the blood flow in a narrowed artery compared to what it could be without the narrowing. It uses a special drug to make blood flow more. RFR, on the other hand, checks the pressure in the artery at rest, without needing any drugs.
FFR sees the pressure drop in a narrowed artery as a sign of how serious the blockage is. RFR looks at the pressure when the heart is at rest, avoiding the issues that can come with the drugs used in FFR.
Procedural Workflow Comparison
FFR involves giving a drug to increase blood flow, which can be uncomfortable for patients and takes more time. RFR is simpler because it only needs to measure pressure when the heart is at rest. This makes it quicker and more comfortable for patients.
- FFR requires: Pharmacological induction of hyperemia, which can cause side effects like chest pain or dyspnea.
- RFR requires: Simple pressure measurement at rest, making it more comfortable for patients and potentially quicker.
Diagnostic Thresholds and Interpretation
FFR and RFR have different cut-off points for what’s considered a problem. FFR says a value of ≤0.80 is bad, while RFR uses ≤0.89. Knowing these numbers is key for making the right decisions in treatment.
Choosing between FFR and RFR depends on the patient, the blockage, and what the doctors prefer. Both have their good points and bad, and using them right can help treat coronary artery disease better.
Diagnostic Performance of FFR and RFR
FFR and RFR are key in managing coronary artery disease. They have been studied a lot to see how well they work in real-world settings.
Sensitivity and Specificity Comparisons
Studies have looked at how well FFR and RFR spot coronary artery disease. FFR is seen as the top choice for checking if a blockage is serious, with a clear cut-off of 0.80. RFR, without needing extra blood flow, is a good option too. It shows a strong link with FFR, showing both can be trusted in some situations.
When we compare FFR and RFR, we must think about the situation and the patients. Research shows RFR can be just as good as FFR in finding serious blockages, but they might not always agree.
Correlation Between FFR and RFR Measurements
There’s a lot of interest in how FFR and RFR relate to each other. A strong link between them means RFR could be used instead of FFR in some cases. But, it’s also important to know when they don’t match up well.
Studies show FFR and RFR usually agree, but not always. It’s important to know when they don’t match to make the best choices for patients.
Clinical Agreement and Discordance Scenarios
FFR and RFR usually agree, but not always. Disagreements can happen because of the blockage’s type and the patient’s blood flow. Knowing why this happens helps doctors understand the results better.
In summary, both FFR and RFR are good for finding coronary artery disease. Knowing how well they work helps doctors make better choices for their patients.
Patient Preparation and Experience: FFR vs. RFR Procedures
FFR and RFR procedures differ in more than just technology. They also affect how patients prepare, experience the procedure, and recover. Knowing these differences is key to improving patient care.
Pre-procedure Requirements
Before starting FFR or RFR, patients must meet certain requirements. Both procedures start with coronary angiography to find the problem area. But, the preparation steps vary because of the drugs used.
For FFR, patients get adenosine to increase blood flow. This means watching their heart rate and avoiding certain medicines. These steps are important for adenosine to work right.
RFR doesn’t need adenosine, making preparation simpler. Patients get the usual checks before the procedure but don’t worry about adenosine side effects.
|
Pre-procedure Requirement |
FFR |
RFR |
|---|---|---|
|
Adenosine Administration |
Required |
Not Required |
|
Vital Sign Monitoring |
Yes |
Yes |
|
Medication Review |
Yes, with focus on adenosine interaction |
Standard medication review |
Patient Experience During Measurement
The experience during the procedure is different for FFR and RFR. FFR uses adenosine, which can cause chest pain, flushing, and shortness of breath. These symptoms are usually short-lived but can be uncomfortable.
RFR is usually more comfortable because it doesn’t use adenosine. Patients often don’t feel as much discomfort or side effects, making the experience better.
Recovery and Post-procedure Care
After both procedures, patients get standard care after the catheterization. But, FFR patients might need closer watch because of adenosine’s effects. This can include heart rate changes or lasting symptoms.
RFR recovery is often easier, with fewer complications. Patients can usually go back to normal activities quickly, unless there are issues from the catheterization.
Key differences in patient experience between FFR and RFR procedures are summarized as follows:
- FFR requires adenosine, leading to possible side effects and discomfort.
- RFR does not use adenosine, making it a more comfortable experience.
- RFR recovery is simpler and less complicated.
Understanding these differences helps healthcare providers improve patient care. This makes the experience better for those getting tested for coronary artery disease.
Integration with Cardiac MRI and Other Imaging Modalities
Assessing coronary artery disease has changed a lot. Now, we use FFR and RFR with advanced imaging. This mix gives us a clearer view of the disease. It helps doctors make better treatment plans.
Complementary Role of Cardiac MRI in Coronary Assessment
Cardiac MRI shows the heart and its blood vessels in detail. It’s key for seeing how bad coronary artery disease is. When paired with FFR and RFR, it paints a full picture of the heart’s health.
Cardiac MRI is great for looking at heart tissue and checking how well the heart works. It also shows blood vessel details without harmful radiation. Mixing it with FFR and RFR helps doctors understand the heart’s function better.
How FFR and RFR Complement Non-invasive Imaging
FFR and RFR give us important info on heart blockages. They add to what cardiac MRI and other scans show. They help figure out if a blockage needs treatment.
Using these tools together gives a deeper look at heart disease. For example, a patient with a blockage might get FFR or RFR to see if it’s serious. This helps decide if they need surgery or not.
Future of Multimodality Imaging Approaches
The future of heart disease checks is bright. We’ll see better images and ways to mix data from different scans. This will make treatments more precise and effective.
With more advanced scans and tools, doctors can give patients better care. Mixing cardiac MRI, FFR, RFR, and other tests will lead to better health outcomes. It’s all about making treatments more personal and effective.
Clinical Scenarios: When to Choose FFR vs. RFR
When we look at coronary artery disease, picking between FFR and RFR is complex. It depends on many clinical factors.
Patient-Specific Selection Criteria
Choosing between FFR and RFR starts with the patient. For some, RFR is better because it doesn’t need adenosine. RFR’s adenosine-free assessment is a big plus for these patients.
But, FFR might be better for others. This is true for complex cases where FFR’s proven track record is key. The right choice depends on the patient’s health and the specifics of their heart issues.
Lesion Characteristics Considerations
How complex the heart lesions are also matters. FFR is better for tough cases. RFR works well for simpler ones.
When deciding, we look at where the lesions are, how bad they are, and what they look like. For example, RFR might be good for some, but FFR is better for others.
Institutional and Operator Factors
What the hospital prefers and who is doing the test also plays a part. Places that know FFR well might stick with it. They have a lot of data to back it up.
But, some places might choose RFR to make things easier or to use less adenosine. Who is doing the test and how comfortable they are with each method is also important.
In the end, picking between FFR and RFR is about the patient, the heart issues, and who is doing the test. By thinking about these things, doctors can make the best choice for their patients.
Economic and Practical Considerations
Using FFR and RFR technologies in healthcare has many economic and practical sides. As these tools become more common, it’s key to understand their costs and challenges. This helps in using them better for patient care.
Procedural Costs and Resource Utilization
FFR and RFR procedures have costs like equipment, supplies, and training. FFR uses adenosine, which can add to the cost and may cause side effects. RFR, being adenosine-free, could be cheaper by avoiding these costs and simplifying the process.
Here’s a table comparing the costs of FFR and RFR:
|
Cost Component |
FFR |
RFR |
|---|---|---|
|
Equipment Cost |
$1,500 – $2,000 |
$1,000 – $1,500 |
|
Adenosine Cost |
$100 – $300 |
$0 |
|
Personnel Training |
$500 – $1,000 |
$500 – $1,000 |
|
Total Procedural Cost |
$2,100 – $3,300 |
$1,500 – $2,500 |
Training Requirements for Physicians
Doctors need special training for FFR and RFR to use them right. The training covers the science behind them, how to do the procedures, and making decisions based on the results. RFR might be easier to learn because it doesn’t need adenosine and is simpler to do.
Key aspects of training include:
- Understanding the physiological basis of FFR and RFR
- Mastering the procedural techniques for measurement
- Interpreting results and making clinical decisions
Implementation Challenges
Starting FFR and RFR in hospitals faces several hurdles. These include needing the right equipment, trained staff, and fitting them into current workflows. Also, things like hospital policies and how well staff can use these tools can affect their adoption.
It’s important to think about these challenges when deciding to use FFR and RFR. Knowing the economic and practical sides helps us overcome these hurdles and use these tools effectively.
Emerging Technologies and Future Directions
Looking ahead, new technologies will greatly impact how we diagnose and treat coronary artery disease. Advanced methods, artificial intelligence, and new physiological indices will change the game in coronary physiology.
Non-invasive FFR Computation
Non-invasive FFR computation is a big step forward in diagnosing coronary artery disease. It uses advanced imaging and computer models to get FFR values without invasive procedures. This makes it safer and more accessible for more people.
- Improved patient comfort and safety
- Broader accessibility for FFR assessment
- Potential for earlier diagnosis and intervention
Artificial Intelligence Applications
Artificial intelligence (AI) is set to change coronary physiology a lot. AI can sift through lots of data to find insights that doctors might miss. It can predict FFR values from images and spot risky lesions.
Key benefits of AI in coronary physiology include:
- Enhanced predictive capabilities
- Improved diagnostic accuracy
- Personalized treatment planning
Next-Generation Physiological Indices
New physiological indices are being researched. They aim to give more accurate and detailed views of coronary health. These might include new hemodynamic parameters or resting measurements.
As these technologies grow, they promise to enhance coronary artery disease diagnosis and treatment. By adopting these innovations, we can expect better patient care and more efficient healthcare.
Conclusion: The Evolving Role of FFR and RFR in Coronary Assessment
FFR and RFR are key tools in checking coronary artery disease. Ongoing research is changing how we use them in medical care. New tech and a better understanding of heart health are driving these changes.
FFR is now a top choice for checking if heart blockages matter. RFR is a new option that might make things easier for doctors and patients.
Choosing between FFR and RFR depends on many things. These include the patient’s health, the blockage’s complexity, and what doctors prefer. As cardiology gets better, using these tools with other tests like MRI will help us treat heart disease better.
In the end, using FFR and RFR wisely is key. It’s all about following the science and focusing on the patient. This approach will lead to better care for heart patients.
FAQ
What is the difference between FFR and RFR?
FFR and RFR are both used to check how severe coronary artery disease is. FFR uses adenosine to make blood flow increase. RFR checks blood flow at rest without adenosine.
What is coronary artery disease, and why is functional assessment important?
Coronary artery disease happens when arteries narrow or block due to plaque. Functional tests are key because they show how severe the blockage is. They help decide if surgery is needed, more than just looking at pictures of the arteries.
How is FFR measured, and what is the significance of the 0.80 threshold?
FFR is measured with a pressure wire in a lab. Adenosine is used to increase blood flow. A 0.80 reading means the blockage is serious enough to need treatment.
What are the limitations of FFR, and how does RFR address these?
FFR has downsides like adenosine side effects and complex procedures. RFR fixes these by not needing adenosine. It makes patients more comfortable and could make procedures easier.
Can RFR be used in all patients, or are there specific criteria?
RFR is good for many, but FFR might be better for some. It depends on the patient’s health and the blockage’s type. Doctors decide based on each case.
How do FFR and RFR integrate with other imaging modalities like cardiac MRI?
FFR and RFR work well with cardiac MRI and other tests. Together, they give a full picture of heart disease. This helps doctors make better treatment plans.
What are the economic and practical considerations of FFR and RFR?
Choosing FFR or RFR means thinking about cost and how easy they are to use. It also involves training doctors and setting up systems in hospitals. These factors affect how often they are used.
Are there emerging technologies or future directions in coronary physiology?
Yes, new tech like non-invasive FFR tests and AI are coming. They aim to improve how we diagnose and treat heart disease.
How does cardiac MRI contribute to the assessment of coronary artery disease?
Cardiac MRI shows the heart and blood vessels in detail. It helps see how bad heart disease is. It works with FFR and RFR for a complete check.
Can patients with pacemakers undergo an MRI, and is it safe?
MRI safety with a pacemaker varies by pacemaker type and MRI settings. Some newer pacemakers might be safe for MRI under certain conditions. Always check with a doctor first.
What preparation is required for an MRI with contrast?
For an MRI with contrast, you might need to fast, remove metal, and tell about medical implants. Your doctor will give specific instructions.
How long does a cardiac MRI take, and what is the experience like?
A cardiac MRI usually lasts 30 to 60 minutes. You lie in a noisy MRI machine and might need to hold your breath. It’s a bit of an experience.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/37427088/**




































