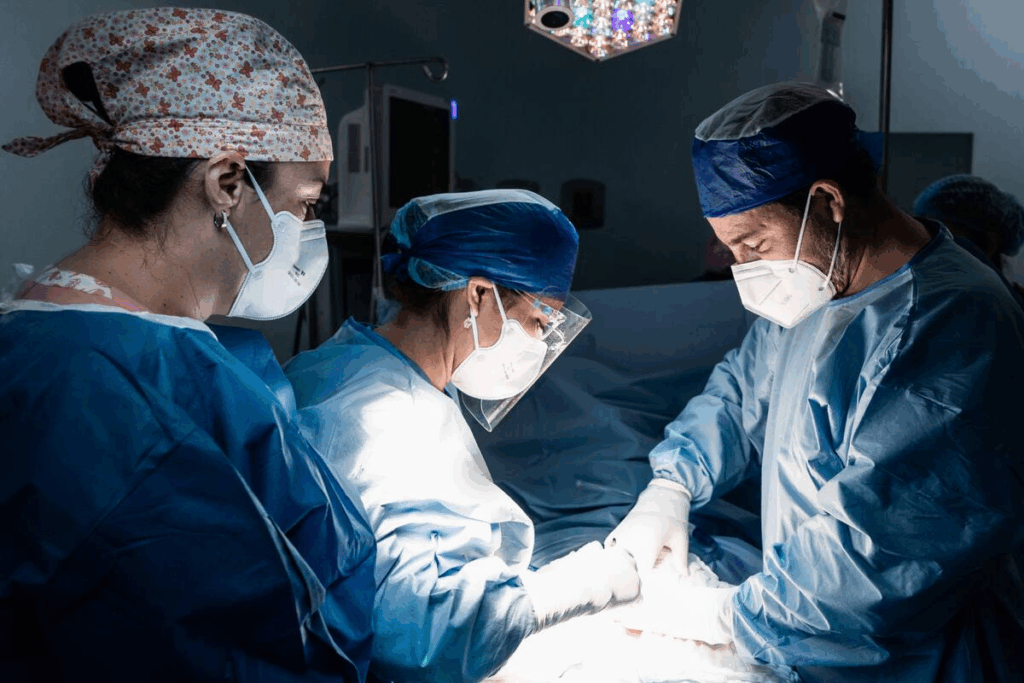
Gastrointestinal surgery encompasses a range of procedures designed to treat conditions affecting the digestive tract. We will explore the various types of gastrointestinal surgery, highlighting their significance in medical practice. Complete guide to the 7 most common types of gastro surgery and their specific indications.
Recent projections show that minimally invasive procedures will make up 70% of all gastrointestinal surgeries by 2025. This change towards less invasive methods shows how gastrointestinal surgery is evolving. It offers patients more effective and efficient treatment options.
Key Takeaways
- Gastrointestinal surgery includes various procedures for treating digestive tract conditions.
- Minimally invasive procedures are becoming increasingly prevalent in gastrointestinal surgery.
- The field is evolving, with a focus on effective and efficient treatment options.
- Gastrointestinal surgery is critical for addressing various digestive health issues.
- Understanding the types of gastrointestinal surgery can help patients make informed decisions.
The Expanding Field of Gastrointestinal Surgery
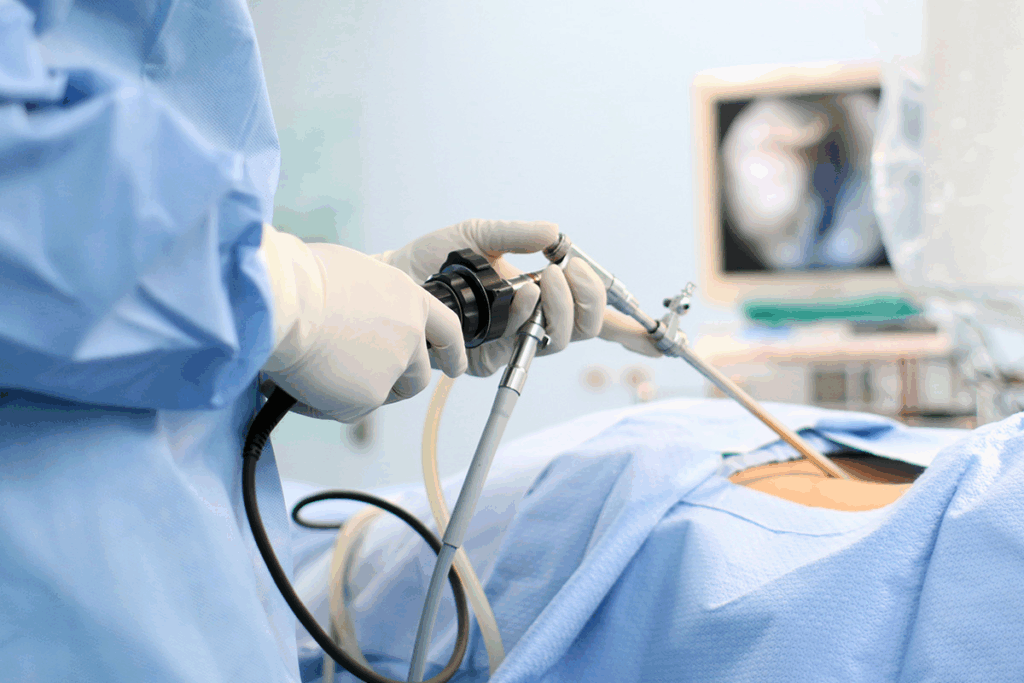
Medical technology keeps getting better, and so does gastrointestinal surgery. This field helps patients all over the world. It includes many procedures for different digestive problems. New techniques, tools, and care methods are making it grow fast.
Definition and Scope of Digestive Tract Procedures
Gastrointestinal surgery deals with the digestive system, from the esophagus to the anus. It also includes organs like the liver and pancreas. The range of surgeries is wide, from simple to very complex.
The Atlas of Gastrointestinal Surgery 2e shows the variety of GI surgeries. These operations help with cancer, inflammation, and other issues. They are key to treating many diseases.
Common Conditions Requiring Surgical Intervention
Many conditions need surgery in the GI tract. These include:
- Gastric cancer and other malignancies
- Inflammatory bowel disease (IBD)
- Gallstones and biliary tract diseases
- Appendicitis
- Diverticulitis and other colonic conditions
The global endoscopy market is growing fast. It was 191.1 million procedures in 2024 and will hit 207.5 million by 2030. This shows more people are using less invasive methods.
Condition | Common Surgical Interventions | Projected Procedures by 2030 |
Gastric Cancer | Gastrectomy, Lymphadenectomy | 1.2 million |
Inflammatory Bowel Disease | Colectomy, Proctocolectomy | 0.8 million |
Gallstones | Cholecystectomy | 2.5 million |
These numbers show surgery’s big role in treating GI diseases. As we keep improving in GI surgery, it’s important to learn about new methods and research. This helps us give our patients the best care.
Gut Surgery: Evolution and Current Trends
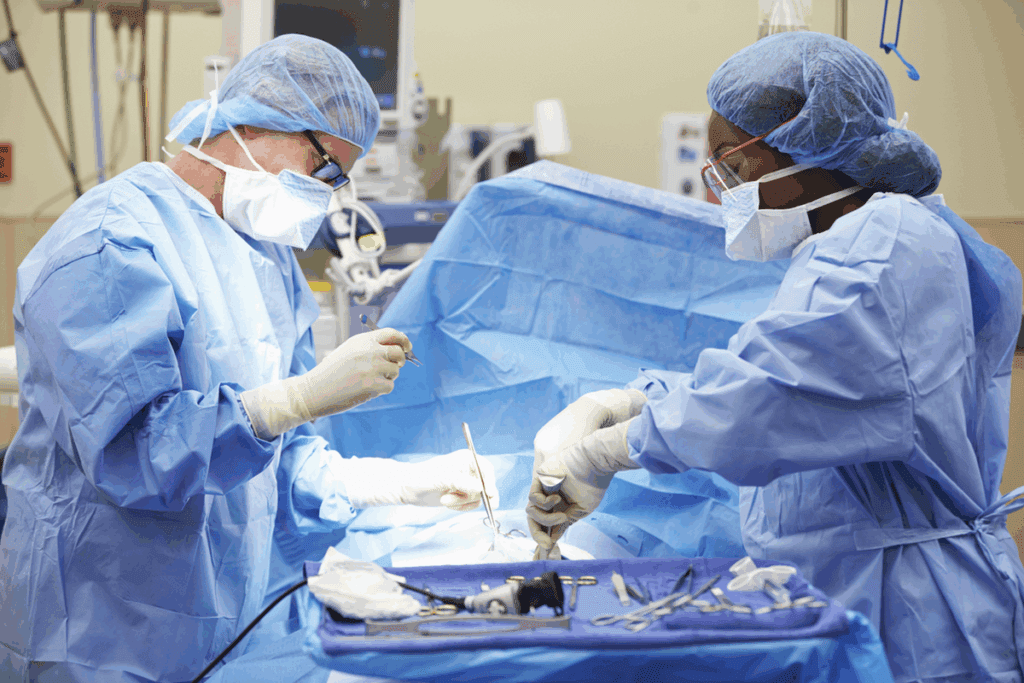
Gastrointestinal surgery has changed a lot, thanks to new technology and methods. Now, we focus more on better patient care and faster recovery times.
Historical Development of GI Surgical Techniques
Gut surgery started in the late 19th century with the first successful surgeries. Over time, we moved from open surgeries to more advanced, minimally invasive ones.
Key milestones include the introduction of laparoscopic surgery in the late 20th century. This made surgeries less invasive and recovery faster. Recently, robotic-assisted surgery has improved precision and control even more.
2024 Statistics and Market Projections
Recent data from 2024 shows a big increase in demand for gastrointestinal surgery. The global market is expected to grow at a 7.5% CAGR from 2024 to 2030.
Segment | 2024 Market Share (%) | 2030 Projected Market Share (%) |
Minimally Invasive Surgery | 60 | 75 |
Open Surgery | 30 | 20 |
Robotic-Assisted Surgery | 10 | 15 |
The Shift Toward Minimally Invasive Approaches
Minimally invasive surgery is becoming more popular. It offers less pain, shorter hospital stays, and quicker recovery.
Minimally invasive procedures are now common in gut surgery. Laparoscopic and robotic-assisted surgeries are at the forefront.
Type 1: Gastrectomy Procedures
Gastrectomy procedures are key in treating gastric cancer and severe stomach issues. They involve removing part or all of the stomach. This depends on the patient’s condition and the disease’s extent.
“The Atlas of Gastrointestinal Surgery 2e” shows how gastrectomy has evolved. Gastrectomy is a complex surgery that requires precision and expertise. It’s tailored to each patient’s needs.
Partial Gastrectomy: Technique and Applications
Partial gastrectomy removes a part of the stomach. It’s used for gastric cancer in a specific stomach area. The surgeon removes the affected stomach part and connects the rest to the small intestine.
The main goal is to remove cancer while keeping stomach function. This improves the patient’s life after surgery.
Total Gastrectomy for Advanced Gastric Cancer
Total gastrectomy removes the whole stomach. It’s for advanced gastric cancer that has spread. The surgeon connects the esophagus to the small intestine for food passage.
“Total gastrectomy is a life-altering surgery that requires careful consideration and planning. Despite its complexity, it offers a chance of survival for patients with advanced gastric cancer.”
Patient Outcomes and Survival Rates
Patient results after gastrectomy depend on several factors. These include cancer stage, patient health, and surgery method. Early-stage cancer patients tend to have better survival rates after surgery.
We watch patient outcomes to improve our surgery and care. Our goal is to increase survival rates and improve life quality for those undergoing gastrectomy.
Type 2: Bariatric Surgical Interventions
For those with severe obesity, bariatric surgery can be a game-changer. This field has made great strides, giving new hope to those dealing with obesity and related health issues.
Sleeve Gastrectomy: Procedure and Benefits
Sleeve gastrectomy, or gastric sleeve surgery, removes a big part of the stomach. This leaves a narrow “sleeve” or tube-like stomach. It reduces the stomach size, limiting how much food you can eat, leading to weight loss. Studies show it’s effective in losing weight and improving health conditions linked to obesity.
The benefits of sleeve gastrectomy include:
- Significant weight loss
- Improvement in obesity-related health conditions, such as type 2 diabetes and hypertension
- Reduced hunger due to the removal of the portion of the stomach that produces the hunger hormone ghrelin
Gastric Bypass Surgery: Technique and Effectiveness
Gastric bypass surgery, or Roux-en-Y gastric bypass, is another common procedure. It creates a small pouch from the stomach and connects it to the small intestine. This reduces food intake and limits nutrient absorption, leading to significant weight loss.
Gastric bypass surgery is highly effective in:
- Achieving and maintaining weight loss
- Improving or resolving obesity-related health conditions
- Enhancing overall quality of life
Patient Selection Criteria and Preparation
Not everyone is a good candidate for bariatric surgery. Criteria include:
- A BMI of 40 or higher, or a BMI of 35 or higher with obesity-related health conditions
- Previous attempts at weight loss through diet and exercise
- A thorough evaluation by a multidisciplinary team, including a surgeon, nutritionist, and psychologist
Preparation for surgery involves a detailed assessment. This includes medical evaluations, nutritional counseling, and psychological support. Patients are also advised to make big lifestyle changes for long-term success.
Understanding bariatric surgery options and their benefits helps individuals make informed decisions. We’re dedicated to providing full care and support to help our patients reach their health goals.
Type 3: Laparoscopic Gastrointestinal Procedures
Laparoscopic gastrointestinal procedures have changed surgery a lot. They use small cuts to insert tools and a camera. This way, doctors can do operations without big cuts.
Laparoscopic Appendectomy and Cholecystectomy
Laparoscopic appendectomy removes the appendix when it’s sick. It’s quick and leaves little scar. Laparoscopic cholecystectomy takes out the gallbladder, often because of stones. Both are safe and let patients go home soon.
- Less pain after surgery
- Stay in the hospital is shorter
- Scars are smaller
- Get back to normal faster
Laparoscopic Colorectal Surgery
Laparoscopic colorectal surgery treats colon and rectum problems. It uses small cuts and a camera. This surgery is for issues like cancer and bowel disease.
It has many benefits. Patients feel less pain and recover faster than with open surgery.
Advantages Over Traditional Open Surgery
Laparoscopic surgery has big advantages over open surgery. These include:
- Smaller cuts mean less scarring
- Less pain after surgery
- Stay in the hospital is shorter
- Less chance of infection and problems
As The Atlas of Gastrointestinal Surgery 2e shows, laparoscopic surgery is getting more popular. It cuts down recovery time and scarring. This makes it a top choice for many.
Type 4: Endoscopic Gastrointestinal Interventions
Gastrointestinal endoscopy is a key part of modern medicine. It helps doctors diagnose and treat digestive tract issues. This method is less invasive than traditional surgery.
Diagnostic Endoscopy Applications
Diagnostic endoscopy lets doctors see inside the digestive tract. They can spot ulcers, inflammation, and tumors. Advanced techniques help get accurate diagnoses for better treatment plans.
The number of endoscopy procedures is rising. By 2024, there will be 191.1 million procedures worldwide. This shows how important endoscopy is for diagnosing and treating GI issues.
Therapeutic Endoscopic Procedures
Therapeutic endoscopy treats various GI disorders. It includes removing polyps, dilating strictures, and stopping bleeding. This method is vital for managing GI conditions without needing surgery.
Endoscopic Retrograde Cholangiopancreatography (ERCP)
ERCP is a special endoscopy for bile and pancreatic ducts. It uses a side-viewing endoscope for detailed views. This allows for stone removal and stent placement.
The table below highlights ERCP’s key points:
Procedure | Indications | Benefits |
ERCP | Diagnosis and treatment of bile and pancreatic duct disorders | Minimally invasive, reduces recovery time, effective for stone removal and stent placement |
Diagnostic ERCP | Visualization of pancreatic and bile ducts | Accurate diagnosis of ductal abnormalities |
Therapeutic ERCP | Treatment of ductal stones, strictures, and leaks | Effective in managing complications related to bile and pancreatic ducts |
In conclusion, endoscopic GI interventions are essential for managing GI diseases. Advances in technology improve patient care and outcomes.
Type 5: Robotic-Assisted Gastrointestinal Surgery
Robotic-assisted gastrointestinal surgery is a new way to do surgery. It gives surgeons better control and vision. This technology is used in many surgeries, making them more precise.
Current Applications in Digestive Tract Surgery
Robotic systems are used in many surgeries. They help with complex operations. Surgeons can do detailed work more easily.
Some key uses are:
- Robotic-assisted colectomies and rectal resections
- Gastric resections for cancer and other conditions
- Hepatobiliary and pancreatic surgeries
Advantages and Limitations of Robotic Systems
The benefits of robotic surgery are:
- More precise and dexterous
- Better vision with 3D high-definition images
- Less blood loss and pain after surgery
- Patients recover faster
But, there are also downsides:
- Expensive to start and maintain
- Surgeons and staff need special training
- Can have technical issues
Latest Innovations and Future Directions
Robotic surgery is getting better fast. New ideas are coming to make surgery better and more available.
Recent advancements include:
Innovation | Description | Potential Impact |
Advanced End Effectors | New wristed instruments for more flexibility | More precise in complex surgeries |
Artificial Intelligence Integration | AI helps with planning and predicting | Better surgery planning and results |
Single-Port Robotics | Robotic systems for single-incision surgery | Less scarring and pain after surgery |
As technology improves, so will surgery. We’ll see better care and more options for patients.
Type 6: Intestinal Resection and Anastomosis
Intestinal resection and anastomosis are key in treating many gut problems. These surgeries help remove sick parts of the intestine. They also help fix the digestive system.
Small Bowel Resection Procedures
Small bowel resection removes a sick part of the small intestine. The steps are:
- Identifying the diseased segment
- Resecting the affected area
- Performing anastomosis to restore intestinal continuity
This surgery is needed for issues like intestinal obstruction, Crohn’s disease, and intestinal tumors.
Colectomy: Partial and Total Approaches
Colectomy removes part or all of the colon. The choice depends on the disease’s location and extent. Partial colectomy is for localized diseases. Total colectomy removes the whole colon.
Anastomosis Techniques and Complications
Anastomosis is a precise step in intestinal surgery. It connects the intestine securely. Different anastomosis techniques are used, like hand-sewn and stapled methods. Yet, problems can happen, such as:
- Leakage at the anastomosis site
- Stricture formation
- Bowel obstruction
Knowing these risks is key to good patient care.
Type 7: Hepatobiliary and Pancreatic Surgery
Hepatobiliary and pancreatic surgeries are very challenging. They need a lot of skill and experience. These surgeries require a deep understanding of the liver and pancreas anatomy and advanced surgical techniques.
Liver Resection for Tumors and Disease
Liver resection is a key surgery for liver problems like tumors and diseases. Precision is key to remove the bad part without harming the healthy liver.
Doctors decide on liver resection after checking with imaging and liver function tests. Advances in surgical techniques and planning have made these surgeries safer and more effective.
Pancreatic Surgery: Whipple Procedure
The Whipple procedure removes tumors or diseased parts of the pancreas. This surgery takes out the head of the pancreas, the duodenum, and sometimes more. It’s a very complex surgery that needs a lot of skill.
Even though it’s hard, the Whipple procedure is a common treatment for some pancreatic problems. It can cure or greatly improve symptoms. Postoperative care is very important to manage risks and ensure a good recovery.
Biliary Tract Interventions
Biliary tract interventions treat problems with the bile ducts, like blockages or cancer. These surgeries can remove the gallbladder or fix the bile ducts. Minimally invasive techniques are used to make recovery faster and leave less scar.
The type of biliary tract intervention depends on the problem, the patient’s health, and other factors. Advances in diagnostic imaging help plan and do these surgeries better.
Conclusion: Advancing Gastrointestinal Surgical Care
The field of gastrointestinal surgery is changing fast. New technologies and methods are making treatments better and more options available. Now, we’re seeing more use of minimally invasive surgeries, which are becoming the norm.
More people need gastrointestinal surgery because of digestive problems. This need is growing. The future looks good with new robotic surgeries, endoscopic treatments, and other advanced tools.
We must keep investing in research to improve gastrointestinal surgery. This way, patients will get better care and live better lives. The future of GI surgery is bright, and we’re dedicated to providing top-notch care.
FAQ
What is gastrointestinal surgery?
Gastrointestinal surgery, or GI surgery, treats problems in the digestive system. This includes the esophagus, stomach, small intestine, and colon.
What are the different types of gastrointestinal surgeries?
GI surgeries include many types. These are gastrectomy, bariatric surgery, and laparoscopic procedures. There’s also endoscopic interventions, robotic-assisted surgery, and intestinal resection. Plus, hepatobiliary and pancreatic surgery.
What is gastrectomy?
Gastrectomy removes part or all of the stomach. It’s done for stomach cancer, severe ulcers, or other issues.
What is bariatric surgery?
Bariatric surgery helps with weight loss. It changes the stomach or intestines. It’s for obesity and related health problems.
What are laparoscopic gastrointestinal procedures?
Laparoscopic GI procedures are small surgeries. They use a laparoscope and small cuts. They’re for appendectomy, cholecystectomy, and colorectal surgery.
What is endoscopic retrograde cholangiopancreatography (ERCP)?
ERCP uses an endoscope to see bile and pancreatic ducts. It treats gallstones, tumors, and duct narrowing.
What is robotic-assisted gastrointestinal surgery?
Robotic-assisted GI surgery uses a robotic system. It helps surgeons with complex procedures. It offers better precision and visualization.
What is intestinal resection and anastomosis?
Intestinal resection removes a part of the intestine. Anastomosis reconnects it. It’s for bowel obstruction, cancer, or inflammatory bowel disease.
What is hepatobiliary and pancreatic surgery?
This surgery treats liver, bile ducts, and pancreas issues. It includes liver resection, Whipple procedure, and biliary tract interventions.
What are the benefits of minimally invasive gastrointestinal surgery?
Minimally invasive GI surgery has many benefits. It has smaller incisions, less pain, and shorter stays. Recovery is faster than traditional surgery.
How do I prepare for gastrointestinal surgery?
Preparing for GI surgery includes a medical check-up and dietary changes. You’ll also make lifestyle changes. Follow your healthcare provider’s instructions.
References
- NICE. (2023). Obesity: identification, assessment and management. NICE guideline [NG189]. https://www.nice.org.uk/guidance/ng189



































